Promoting breastfeeding in a modern NICU Uwe Ewald

Promoting breastfeeding in a modern NICU Uwe Ewald, Uppsala, Sweden

Why breastfeeding? • The physiological norm of infant feeding – Optimal nutrient composition • Promotes attachment/bonding and parenting skills – The prefrontal cortex and orbitofrontal area of the brain are interconnected in a more powerful way if a baby is given love and attention (Gerhardt, 2004).

Systematic reviews on effects • Suboptimal breastfeeding results in more than 800 000 child death annually • 11. 6% of all infant death 2011 Black RE et al Lancet 2013; 382: 427 -51 • Association with: • an increase in IQ of about three points, even after adjustment for several confounders • 1 mm reduction in blood pressure • 12% reduction in overweight or obesity • Reduced risk of SIDS Horta BL et al Geneva; WHO 2013

Barriers of breastfeeding preterm infants Infants • Tied to devices • Breathing support • Diseases Mothers • Diseases/complications • Stress • Depression, guilt • Stress/pain • Subtle bf cues Care culture • Separation • Late initiation of breastfeeding • Low muscular tone, fatigue • Small mouth, weak intraoral vacuum

Strategy • Reduce losses – Thermoneutrality – Insensible losses – Minimal handling • Limiting early weight loss – Max 7% (1 SD) initial weight loss

Earlier nutrient intake § Human milk from 2 hours after birth § Colostrum § Gavage and/or cup feeding § § Increase 10 -20 m. L/kg/d up to 150 -250 m. L/kg/d Goal – full enteral at <7 d Early partial parenteral nutrition (<1 h) Amino acids instead of Na. Cl in lines

Human milk – volume tailored for growth rate of term infants • Energy – 130 kcal /kg requires 200 m. L/kg/d from day 0 • Protein – 4. 5 g/kg requires 450 ml/kg/d from day 0 • Fat – 6, 5 g/kg requires 150 ml/kg/d from d 0

Targeted fortification Polberger 1999 If growth failure: Analysis of mothers or donated bank milk (protein fat, carbohydrate) Improve pumping technique Calculating goal intake (GA/PMA) Increase if possible volume to 200 -250 m. L/kg/d If protein deficency: Commercial bovine fortifiers

Problems of lactoengineering • Lack of research evidence (growth, body composition, side effects) • Difficult to reach balanced nutrient intake • Enteral intolerance (higher osmolarity) • Costs • Potentially negative for mothers expression/breastfeeding efforts. . `my milk is not good enough`…

Breastfeeding – not only nutrition and volumes • • Emotions affect everything! Enable closeness Empower the parents to be self-sufficient Emphasize feeding as a relational interplay (for comfort and pleasure)
This promotes breastfeeding Kangaroo mother care Non-separation Family centered care Developmental care

Support • • Adult bed adjacent to the infant Presence possible 24/7 Involvement in care decisions Early breastmilk expression Pumping Breastmilk bank Encouraging staff and context

Facilitating breastfeeding of preterm infants in the clinical setting • Space - place, privacy, environment • Support (parental leave, social network) Thernstrom, Ewald Acta Paediatr 2012 • Dedicated and well trained staff J Hum Lact. 1996; 12: 221 • Avoid separation – Rooming-in J Perinat Neonatal Nurs. 2012; 26: 336 • Early breast milk expression J Perinatol. 2012; 32: 205 • Skin-to skin contact, Kangaroo Mother Care Cochrane Syst Rev. 2012: 16; 5

KMC policy for preterm infants • KMC for infants born ≥ 32 wks – KMC 24/7 the norm • KMC for infants born 28 -31 wks – Early after stabilization within hours, ideally 24/7 • KMC for infants born ≤ 27 wks – Within 3 -5 d, dependant on stability in temperature, fluid and electrolyte balance, Karlsson, J Pedatr. 2012
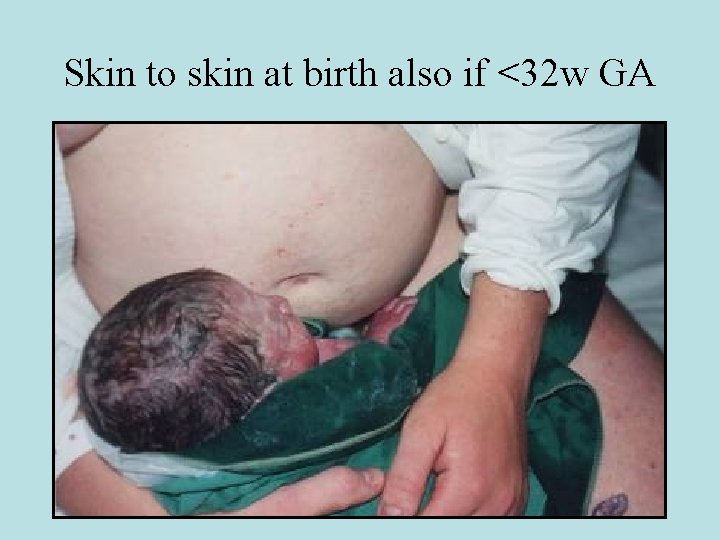
Skin to skin at birth also if <32 w GA

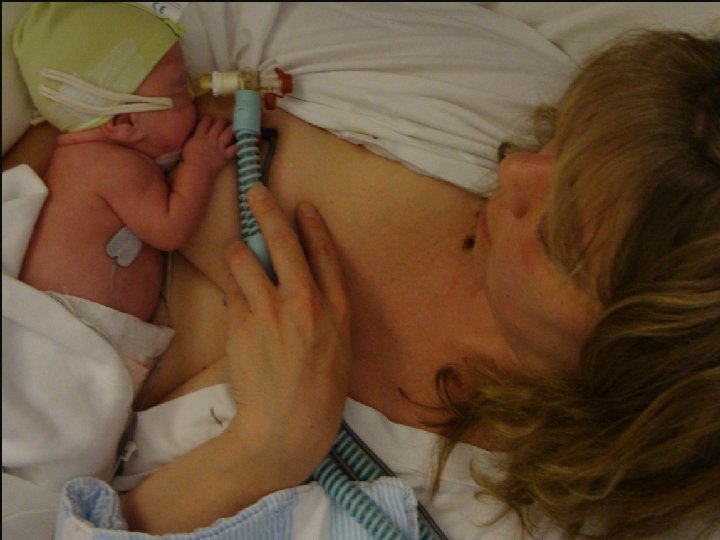
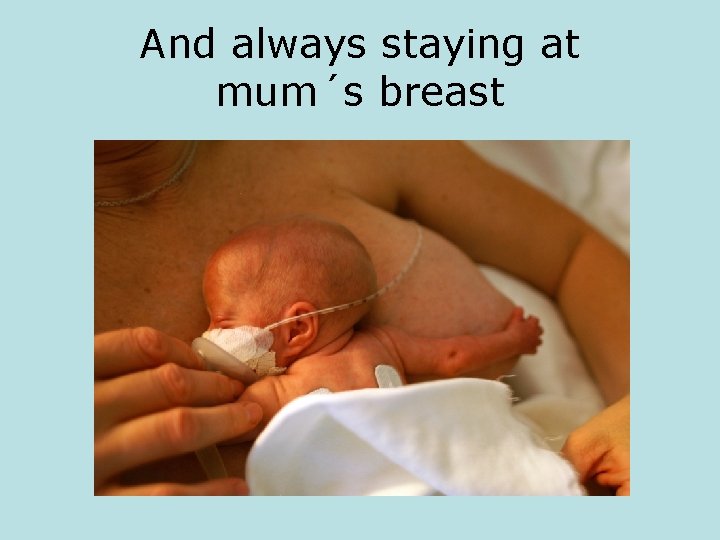
And always staying at mum´s breast
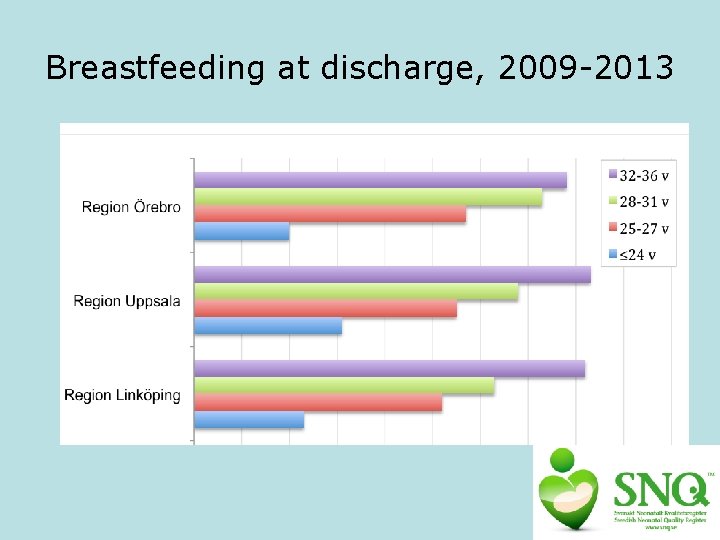
Breastfeeding at discharge, 2009 -2013
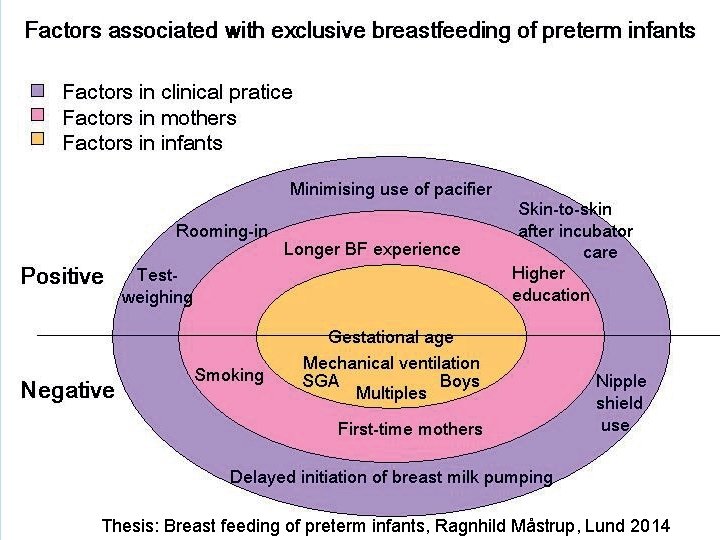
Thesis: Breast feeding of preterm infants, Ragnhild Måstrup, Lund 2014

Thank you!


Routines for breast milk – Encouraged early expression/pumping – Pump 6 -8 times (also nights) – Use double pump technique – Aim for 700 ml/d at 5 -7 d – Colostrum within hours – Fresh milk (kept at +4 o. C) – Surplus frozen at -20 o. C – Donor milk from preterm mothers

Transition to exclusive breastfeeding • Breastfeedning on semi-demand. • Decreasing daily amounts by tube or cup • Day 1 breastfeeding + 250 ml • Day 2 breastfeeding + 200 ml etc • Weight once daily Or • Test-weighing before and after • Adjusting amounts given by tube or cup
- Slides: 24