Project Ghana Emergency Medicine Collaborative Document Title Approach

Project: Ghana Emergency Medicine Collaborative Document Title: Approach to Bradycardias and Tachycardias Author(s): Rockefeller Oteng (University of Michigan), MD 2012 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike-3. 0 License: http: //creativecommons. org/licenses/by-sa/3. 0/ We have reviewed this material in accordance with U. S. Copyright Law and have tried to maximize your ability to use, share, and adapt it. These lectures have been modified in the process of making a publicly shareable version. The citation key on the following slide provides information about how you may share and adapt this material. Copyright holders of content included in this material should contact open. michigan@umich. edu with any questions, corrections, or clarification regarding the use of content. For more information about how to cite these materials visit http: //open. umich. edu/privacy-and-terms-use. Any medical information in this material is intended to inform and educate and is not a tool for self-diagnosis or a replacement for medical evaluation, advice, diagnosis or treatment by a healthcare professional. Please speak to your physician if you have questions about your medical condition. Viewer discretion is advised: Some medical content is graphic and may not be suitable for all viewers. 1

Attribution Key for more information see: http: //open. umich. edu/wiki/Attribution. Policy Use + Share + Adapt { Content the copyright holder, author, or law permits you to use, share and adapt. } Public Domain – Government: Works that are produced by the U. S. Government. (17 USC § 105) Public Domain – Expired: Works that are no longer protected due to an expired copyright term. Public Domain – Self Dedicated: Works that a copyright holder has dedicated to the public domain. Creative Commons – Zero Waiver Creative Commons – Attribution License Creative Commons – Attribution Share Alike License Creative Commons – Attribution Noncommercial Share Alike License GNU – Free Documentation License Make Your Own Assessment { Content Open. Michigan believes can be used, shared, and adapted because it is ineligible for copyright. } Public Domain – Ineligible: Works that are ineligible for copyright protection in the U. S. (17 USC § 102(b)) *laws in your jurisdiction may differ { Content Open. Michigan has used under a Fair Use determination. } Fair Use: Use of works that is determined to be Fair consistent with the U. S. Copyright Act. (17 USC § 107) *laws in your jurisdiction may differ Our determination DOES NOT mean that all uses of this 3 rd-party content are Fair Uses and we DO NOT guarantee that your use of the content is Fair. 2 To use this content you should do your own independent analysis to determine whether or not your use will be Fair.
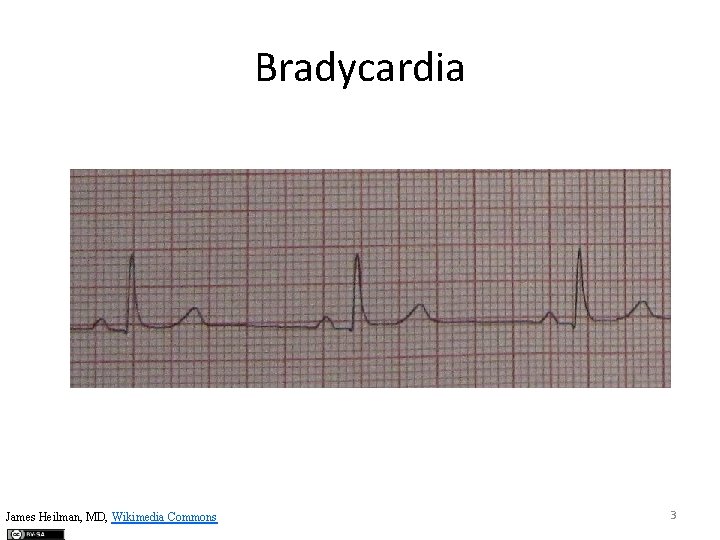
Bradycardia James Heilman, MD, Wikimedia Commons 3
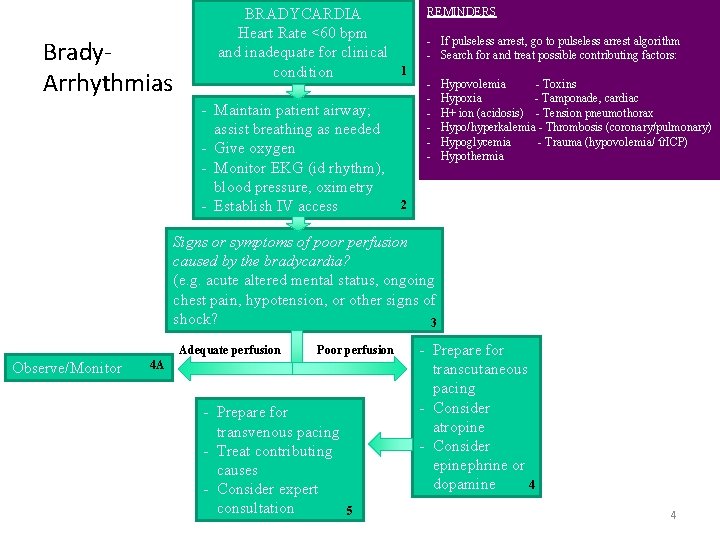
Brady. Arrhythmias BRADYCARDIA Heart Rate <60 bpm and inadequate for clinical condition 1 - Maintain patient airway; assist breathing as needed - Give oxygen - Monitor EKG (id rhythm), blood pressure, oximetry - Establish IV access 2 REMINDERS - If pulseless arrest, go to pulseless arrest algorithm - Search for and treat possible contributing factors: - Hypovolemia - Toxins Hypoxia - Tamponade, cardiac H+ ion (acidosis) - Tension pneumothorax Hypo/hyperkalemia - Thrombosis (coronary/pulmonary) Hypoglycemia - Trauma (hypovolemia/ ICP) Hypothermia Signs or symptoms of poor perfusion caused by the bradycardia? (e. g. acute altered mental status, ongoing chest pain, hypotension, or other signs of shock? 3 Adequate perfusion Observe/Monitor Poor perfusion 4 A - Prepare for transvenous pacing - Treat contributing causes - Consider expert consultation 5 - Prepare for transcutaneous pacing - Consider atropine - Consider epinephrine or 4 dopamine 4
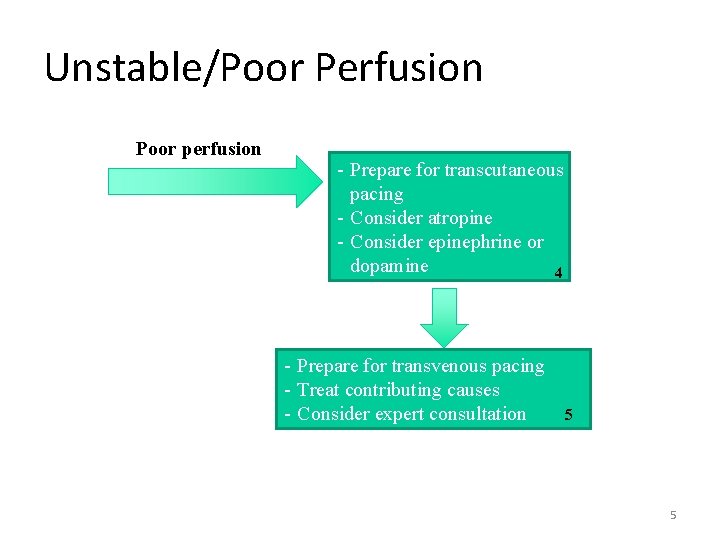
Unstable/Poor Perfusion Poor perfusion - Prepare for transcutaneous pacing - Consider atropine - Consider epinephrine or dopamine 4 - Prepare for transvenous pacing - Treat contributing causes - Consider expert consultation 5 5

Geo Swan, Wikimedia Commons 6

Reminders • If pulseless arrest develops, go to pulseless arrest algorithm • Search for and treat possible contributing factors: Hypovolemia Hypoxia Hydrogen ion (acidosis) Hypo/hyperkalemia Hypoglycemia Toxins (drugs) Tamponade (cardiac) Tension PTX Thrombosis (coronary or pulmonary) Trauma (hypovolemia, increased ICP) Hypothermia 7
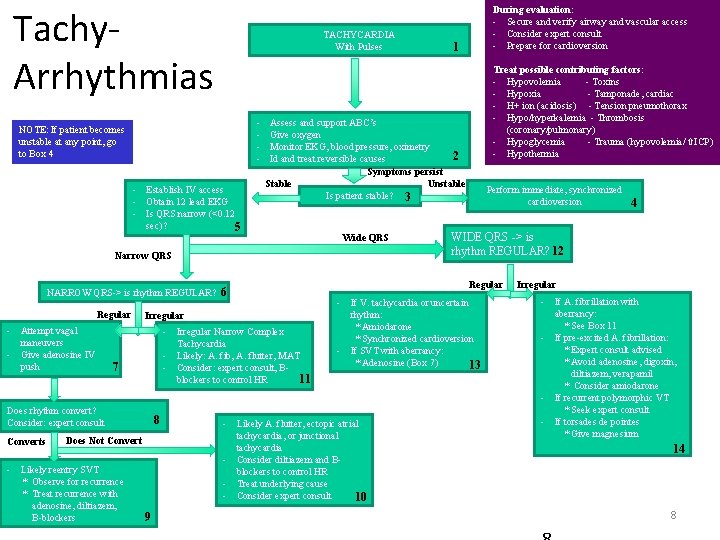
Tachy. Arrhythmias TACHYCARDIA With Pulses - NOTE: If patient becomes unstable at any point, go to Box 4 - Establish IV access - Obtain 12 lead EKG - Is QRS narrow (<0. 12 sec)? 5 Regular - Attempt vagal maneuvers - Give adenosine IV push - Irregular Narrow Complex Tachycardia - Likely: A. fib, A. flutter, MAT - 6 Consider: expert consult, B 11 blockers to control HR Does rhythm convert? Consider: expert consult Converts 8 Does Not Convert - Likely reentry SVT * Observe for recurrence * Treat recurrence with adenosine, diltiazem, B-blockers 6 Irregular 7 9 1 Treat possible contributing factors: - Hypovolemia - Toxins - Hypoxia - Tamponade, cardiac - H+ ion (acidosis) - Tension pneumothorax - Hypo/hyperkalemia - Thrombosis (coronary/pulmonary) - Hypoglycemia - Trauma (hypovolemia/ ICP) - Hypothermia Assess and support ABC’s Give oxygen Monitor EKG, blood pressure, oximetry 2 Id and treat reversible causes Symptoms persist Stable Unstable Is patient stable? 3 Wide QRS Narrow QRS NARROW QRS-> is rhythm REGULAR? During evaluation: - Secure and verify airway and vascular access - Consider expert consult - Prepare for cardioversion Perform immediate, synchronized cardioversion WIDE QRS -> is rhythm REGULAR? 12 Regular - If V. tachycardia or uncertain rhythm: * Amiodarone * Synchronized cardioversion - If SVT with aberrancy: * Adenosine (Box 7) 13 - Likely A. flutter, ectopic atrial tachycardia, or junctional tachycardia - Consider diltiazem and Bblockers to control HR - Treat underlying cause - Consider expert consult 10 4 Irregular - If A. fibrillation with aberrancy: * See Box 11 - If pre-excited A. fibrillation: * Expert consult advised * Avoid adenosine, digoxin, diltiazem, verapamil * Consider amiodarone - If recurrent polymorphic VT * Seek expert consult - If torsades de pointes * Give magnesium 14 8
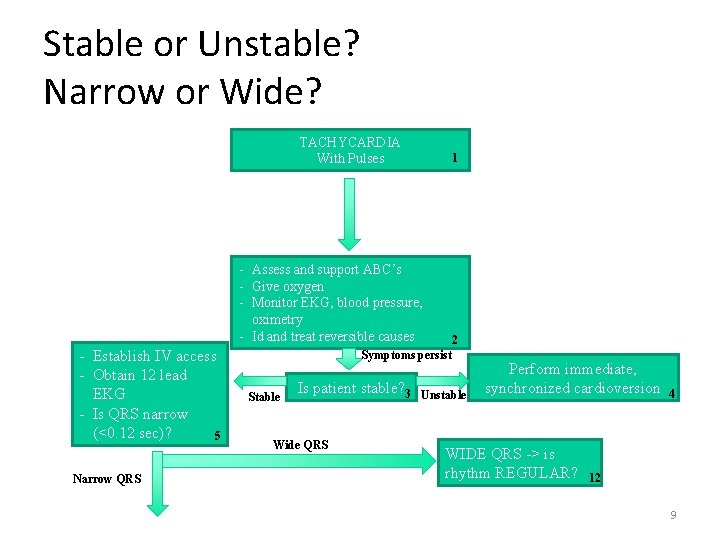
Stable or Unstable? Narrow or Wide? TACHYCARDIA With Pulses 1 - Assess and support ABC’s - Give oxygen - Monitor EKG, blood pressure, oximetry - Id and treat reversible causes - Establish IV access - Obtain 12 lead EKG - Is QRS narrow (<0. 12 sec)? 5 Narrow QRS 2 Symptoms persist Stable Is patient stable? 3 Wide QRS Unstable Perform immediate, synchronized cardioversion WIDE QRS -> is rhythm REGULAR? 4 12 9
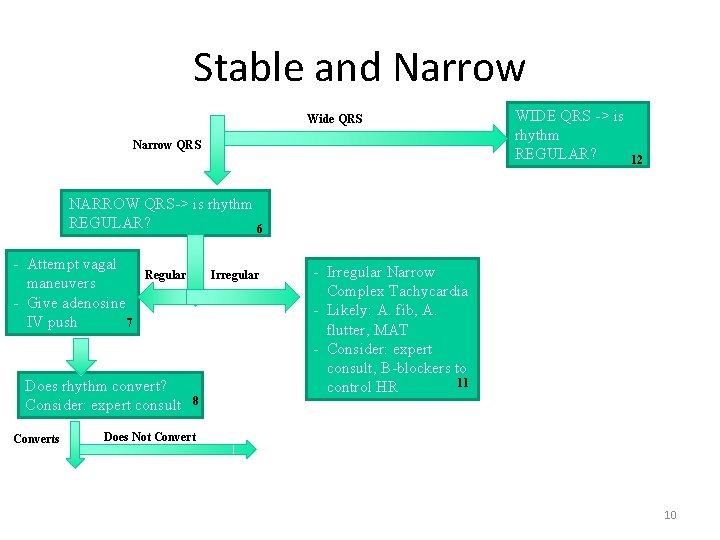
Stable and Narrow Wide QRS Narrow QRS WIDE QRS -> is rhythm REGULAR? 12 NARROW QRS-> is rhythm REGULAR? 6 - Attempt vagal maneuvers - Give adenosine IV push 7 Regular Does rhythm convert? Consider: expert consult Converts Irregular 8 - Irregular Narrow Complex Tachycardia - Likely: A. fib, A. flutter, MAT - Consider: expert consult, B-blockers to 11 control HR Does Not Convert 10

SVT – Mechanism Reentry via accessory pathway A) Normal conduction B) PAC C) Orthodromic reentrant pathway 11

SVT – Mechanism • AV nodal reentrant circuit - 60% • Atrio-ventricular reentrant circuit w/ accessory pathway - 30% • Atrial tachycardia – 10% • Other rare forms: Sinus-node reentrant tachycardia, inappropriate sinus tachycardia, ectopic junctional tachycardia, and non-paroxysmal junctional tachycardia. 12

SVT - Treatment • • Adenosine: – 6 mg - termination in 60 -80% – 12 mg - termination in 90 -95% – Contraindicated in heart transplant, COPD/asthma, and wide complex tachycardia (unless 100% certain is SVT w/ aberrancy) – Avoid with evidence of pre-excitation Beta blockers or Ca++ channel blockers - contraindicated in antidromic WPW Last resort: procainamide, ibutilide, propafenone, or flecainide If unstable - electricity! 13
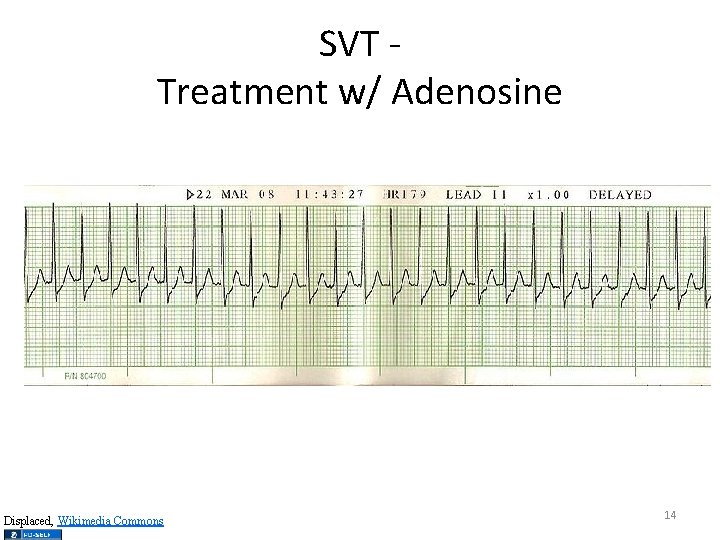
SVT Treatment w/ Adenosine Displaced, Wikimedia Commons 14
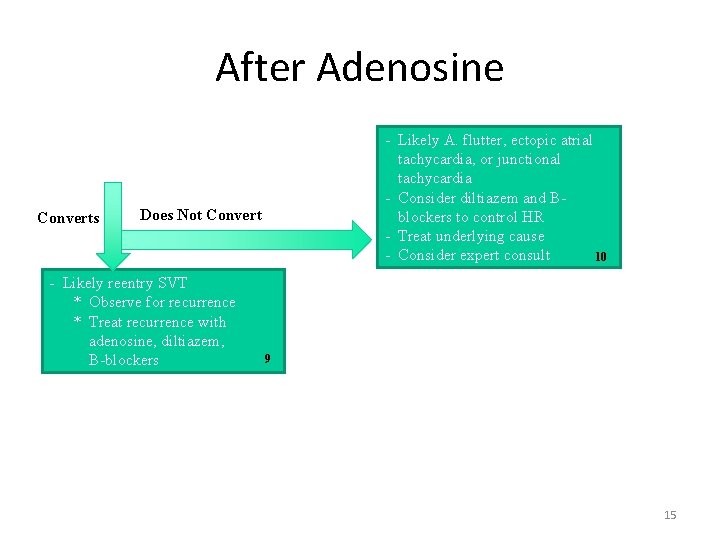
After Adenosine Converts - Likely A. flutter, ectopic atrial tachycardia, or junctional tachycardia - Consider diltiazem and Bblockers to control HR - Treat underlying cause - Consider expert consult 10 Does Not Convert - Likely reentry SVT * Observe for recurrence * Treat recurrence with adenosine, diltiazem, B-blockers 9 15
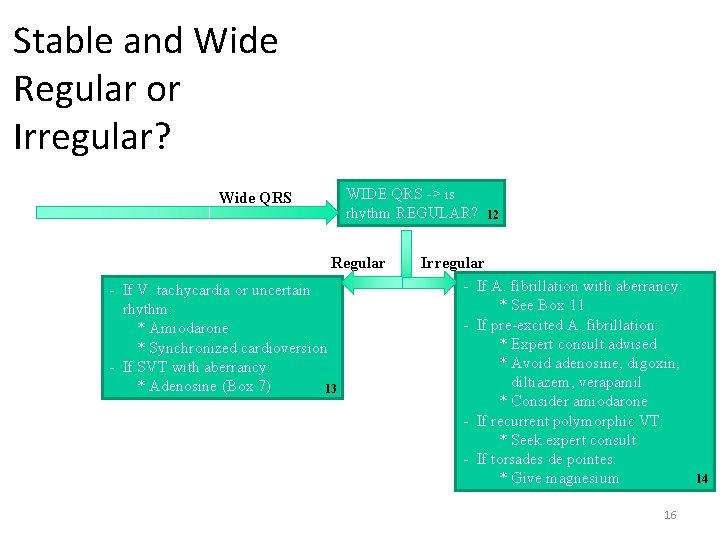
Stable and Wide Regular or Irregular? WIDE QRS -> is rhythm REGULAR? Wide QRS Regular - If V. tachycardia or uncertain rhythm: * Amiodarone * Synchronized cardioversion - If SVT with aberrancy: * Adenosine (Box 7) 13 12 Irregular - If A. fibrillation with aberrancy: * See Box 11 - If pre-excited A. fibrillation: * Expert consult advised * Avoid adenosine, digoxin, diltiazem, verapamil * Consider amiodarone - If recurrent polymorphic VT: * Seek expert consult - If torsades de pointes: * Give magnesium 16 14
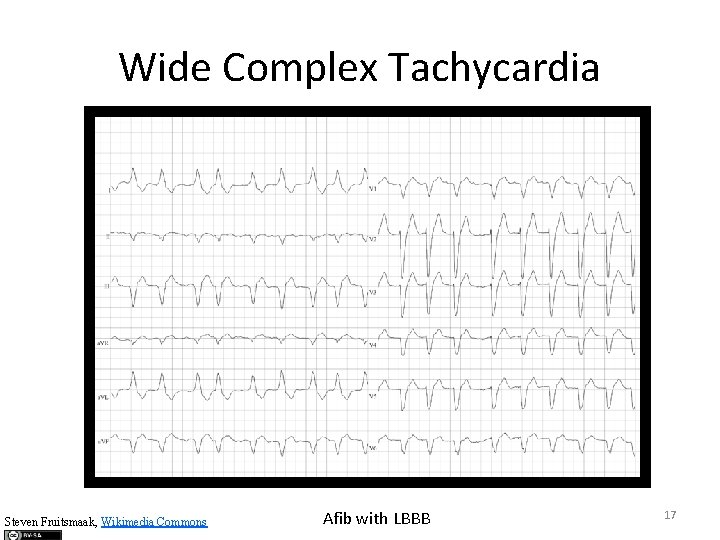
Wide Complex Tachycardia Steven Fruitsmaak, Wikimedia Commons Afib with LBBB 17

Wide Complex Tachycardia • • Stable – Amiodarone 150 mg over 10 min or other anti-arrhythmics – Prepare for synchronized cardioversion Unstable – ABC’s/Call for help/Start CPR – Defibrillate: Biphasic 120 -200 J (When in doubt pick 200 J), monophasic 360 J – Epinephrine 1 mg IV q 3 -5 min – Vasopressin 40 Units IV – May try amiodarone or lidocaine after 3 attempts at defibrillation • Amiodarone 300 mg, may repeat w/ 150 mg x 1 • Lidocaine 1 -1. 5 mg/kg, then 0. 5 -0. 75 mg/kg, max is 3 mg/kg 18

H’s and T’s During Evaluation • Secure, verify airway and vascular access when possible • Consider expert consultation • Prepare for cardioversion Treat contributing factors: Toxins (drugs) Tamponade (cardiac) Hypoxia Tension PTX Hydrogen ion (acidosis) Thrombosis (coronary/pulmonary) Hypo/hyperkalemia Trauma Hypoglycemia Hypovolemia Hypothermia 19

Review 20

Bradycardias Tx of Bradycardias • Stable – MI – Adequate perfusion? – Monitor BP!! • Unstable – Poor perfusion – Immediate transcutaneous pacing – Consider atropine while awaiting pacer, 0. 5 -1. 0 mg – Consider epi or dopamine if pacing ineffective 21

Tachycardia’s Stable vs. Unstable • Stable – MI – 12 lead – Narrow complex – Wide complex – Treat causes • Unstable – Altered MS – CP – Hypotension – Signs of shock • H’s and T’s 22

Tx of Stable Tachycardias • A-fib/flutter – Diltiazem (Ca++ channel blocker) – Consider cardioversion • SVT – Vagal maneuvers – Adenosine • 6 mg then 12 mg • V-Tach (WITH PULSE) – Antiarrhythmic: Lidocaine, Amiodarone, (Mg+ for torsades) 23

Tx of Unstable Tachycardias • Stable – Amiodarone 150 mg over 10 min or other antiarrhythmics – Prepare for synchronized cardioversion • Perform immediate synchronized cardioversion – MI – Sedate if conscious – DO NOT DELAY CARDIOVERSION 24

Contributing Factors H’s and T’s • • • Hypovolemia Hypoxia Hydrogen ion (acidosis) Hypo/hyperkalemia Hypoglycemia Hypothermia Toxins (drugs) Tamponade (cardiac) Tension PTX Thrombosis (coronary or pulmonary) Trauma 25
- Slides: 25