Prognosis of angiosarcoma at different anatomic sites BiingLuen

Prognosis of angiosarcoma at different anatomic sites Biing-Luen Lee, MD. Cheng-Feng Chen Division of Plastic and Reconstructive Surgery, Department of Surgery, Taipei Veterans General Hospital. Koo Foundation Sun Yat-Sen Cancer Center Taipei, Taiwan

Introduction • Angiosarcomas are rare soft-tissue sarcomas of endothelial cell origin that have a poor prognosis • Angiosarcomas are subdivided into cutaneous angiosarcoma, lymphoedema-associated angiosarcoma, radiation-induced angiosarcoma, primary-breast angiosarcoma, and soft-tissue angiosarcoma -Robin J Young et al. Review: Angiosarcoma. Lancet Oncol 2010; 11: 983– 91

Treatment • Surgery with wide excision as the main curative treatment option. Local control is improved with adjuvant radiotherapy. There is no compelling evidence for adjuvant chemotherapy -Robin J Young et al. Lancet Oncol 2010; 11: 983– 91
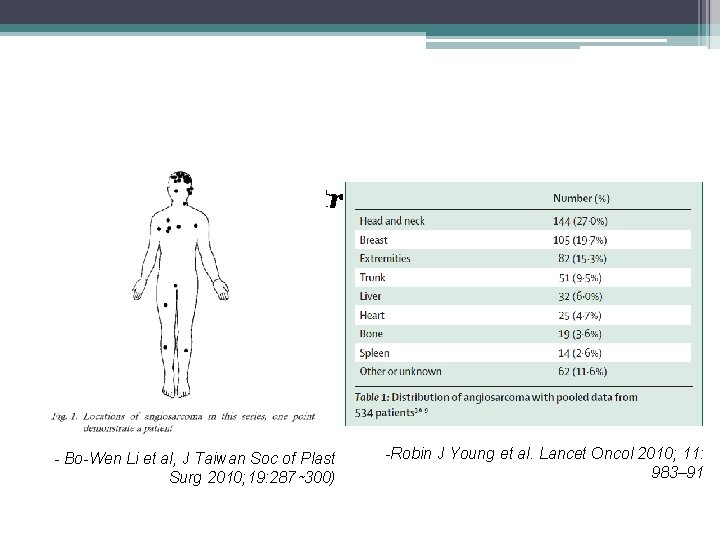
Anatomic sites distribution - Bo-Wen Li et al, J Taiwan Soc of Plast Surg 2010; 19: 287∼ 300) -Robin J Young et al. Lancet Oncol 2010; 11: 983– 91
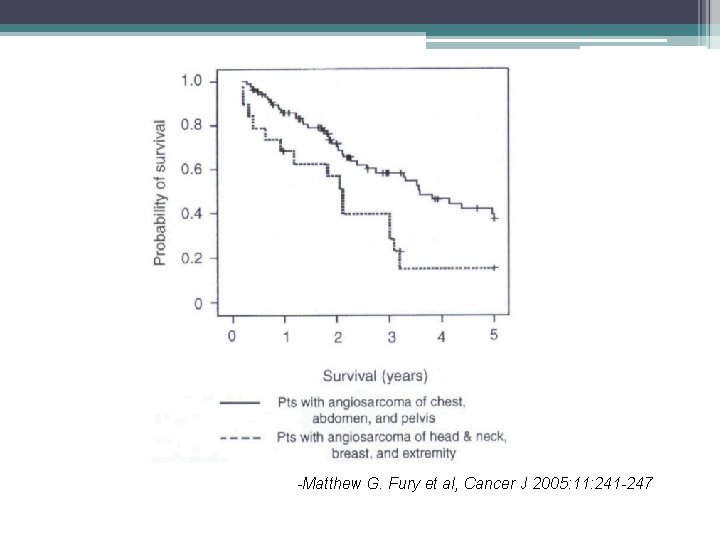
-Matthew G. Fury et al, Cancer J 2005: 11: 241 -247

• Primary site in the liver, presence of metastases and performance status were correlated to poor overall survival, whereas soft tissue primary tumors independently correlated to better survival - J. Fayette et al, Annals of Oncology 18: 2030– 2036, 2007

Material and Method • Retrospective chart review • From 1996 to 2011, pathology reported angiosarcoma from Koo Foundation Sun Yat-Sen Cancer Center and Taipei veteran general hospital • Angiosarcoma at: ▫ Scalp and face ▫ Trunk ▫ Liver

• Patients with incomplete data, concurrent cancer were excluded • Start time: since symptoms appeared • Operation: tumor wide excision/ metastasectomy, excisional biopsies were not included

Results • Total 44 patients • 24 patients had angiosarcoma at scalp and face • 9 at trunk (7 at breast, 1 at lower abdomen and 1 at left supra-scapula region) • 11 at liver
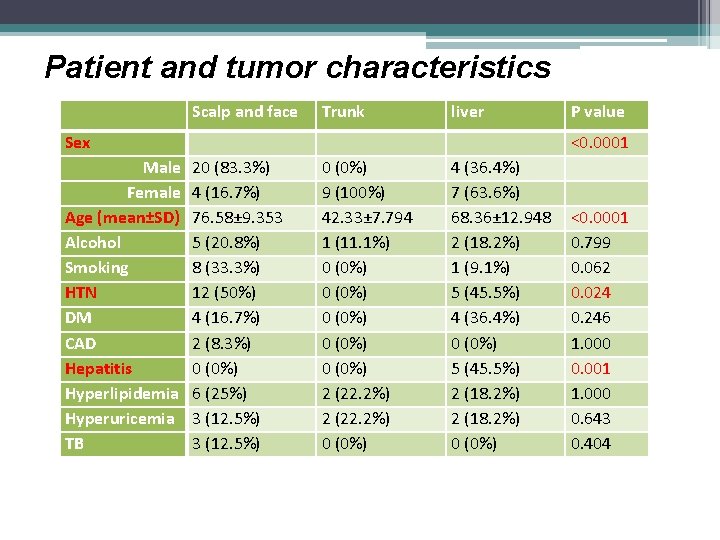
Patient and tumor characteristics Scalp and face Trunk liver Sex Male Female Age (mean±SD) Alcohol Smoking HTN DM CAD Hepatitis Hyperlipidemia Hyperuricemia TB P value <0. 0001 20 (83. 3%) 4 (16. 7%) 76. 58± 9. 353 5 (20. 8%) 8 (33. 3%) 12 (50%) 4 (16. 7%) 2 (8. 3%) 0 (0%) 6 (25%) 3 (12. 5%) 0 (0%) 9 (100%) 42. 33± 7. 794 1 (11. 1%) 0 (0%) 0 (0%) 2 (22. 2%) 0 (0%) 4 (36. 4%) 7 (63. 6%) 68. 36± 12. 948 2 (18. 2%) 1 (9. 1%) 5 (45. 5%) 4 (36. 4%) 0 (0%) 5 (45. 5%) 2 (18. 2%) 0 (0%) <0. 0001 0. 799 0. 062 0. 024 0. 246 1. 000 0. 001 1. 000 0. 643 0. 404
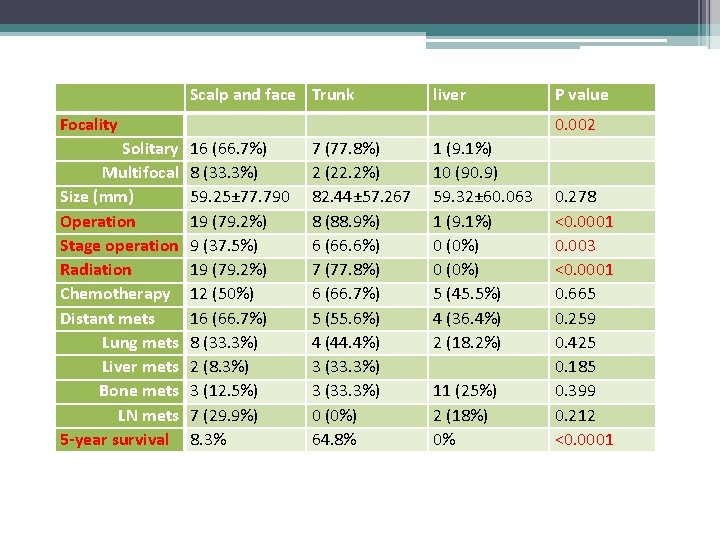
Scalp and face Trunk liver Focality Solitary Multifocal Size (mm) Operation Stage operation Radiation Chemotherapy Distant mets Lung mets Liver mets Bone mets LN mets 5 -year survival P value 0. 002 16 (66. 7%) 8 (33. 3%) 59. 25± 77. 790 19 (79. 2%) 9 (37. 5%) 19 (79. 2%) 12 (50%) 16 (66. 7%) 8 (33. 3%) 2 (8. 3%) 3 (12. 5%) 7 (29. 9%) 8. 3% 7 (77. 8%) 2 (22. 2%) 82. 44± 57. 267 8 (88. 9%) 6 (66. 6%) 7 (77. 8%) 6 (66. 7%) 5 (55. 6%) 4 (44. 4%) 3 (33. 3%) 0 (0%) 64. 8% 1 (9. 1%) 10 (90. 9) 59. 32± 60. 063 1 (9. 1%) 0 (0%) 5 (45. 5%) 4 (36. 4%) 2 (18. 2%) 11 (25%) 2 (18%) 0% 0. 278 <0. 0001 0. 003 <0. 0001 0. 665 0. 259 0. 425 0. 185 0. 399 0. 212 <0. 0001
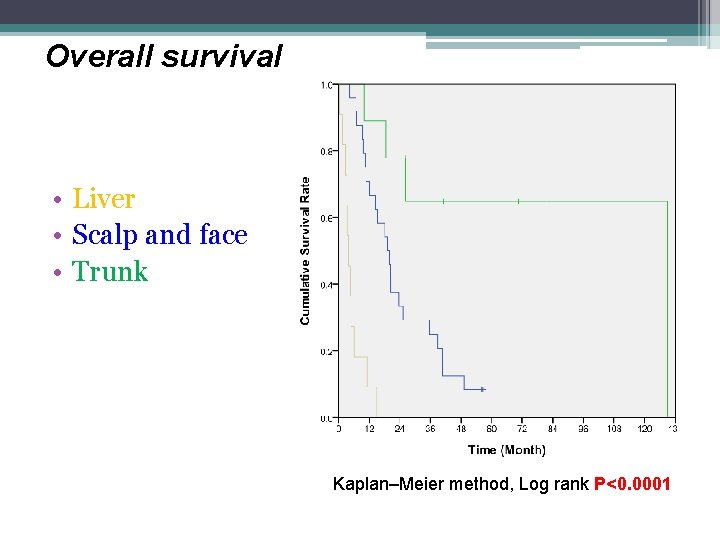
Overall survival • Liver • Scalp and face • Trunk Kaplan–Meier method, Log rank P<0. 0001

Cox regression forward stepwise Variables HR Location (Trunk vs. head) 95% CI of HR P value Lower Upper 0. 040 0. 009 0. 190 <0. 0001 Location (Liver vs. head) 6. 890 2. 261 20. 998 0. 001 Focality (Solitary vs. multifocal) 0. 378 0. 147 0. 970 0. 043 Operation 0. 060 0. 017 0. 207 <0. 0001 Chemotherapy 0. 090 0. 030 0. 272 <0. 0001 Lung mets 4. 213 1. 650 10. 753 0. 003 Liver mets 7. 271 2. 121 24. 919 0. 002 Variables: age, sex, location, focality, size, op, RT, chemo, dis met, lung met, liver met, bone met, LN mets
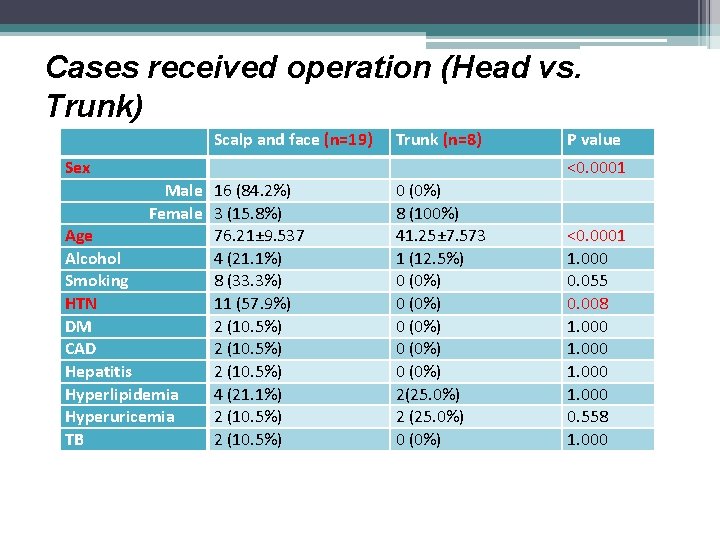
Cases received operation (Head vs. Trunk) Scalp and face (n=19) Trunk (n=8) Sex Male 16 (84. 2%) Female 3 (15. 8%) Age 76. 21± 9. 537 Alcohol 4 (21. 1%) Smoking 8 (33. 3%) HTN 11 (57. 9%) DM 2 (10. 5%) CAD 2 (10. 5%) Hepatitis 2 (10. 5%) Hyperlipidemia 4 (21. 1%) Hyperuricemia 2 (10. 5%) TB 2 (10. 5%) P value <0. 0001 0 (0%) 8 (100%) 41. 25± 7. 573 1 (12. 5%) 0 (0%) 0 (0%) 2(25. 0%) 2 (25. 0%) 0 (0%) <0. 0001 1. 000 0. 055 0. 008 1. 000 0. 558 1. 000
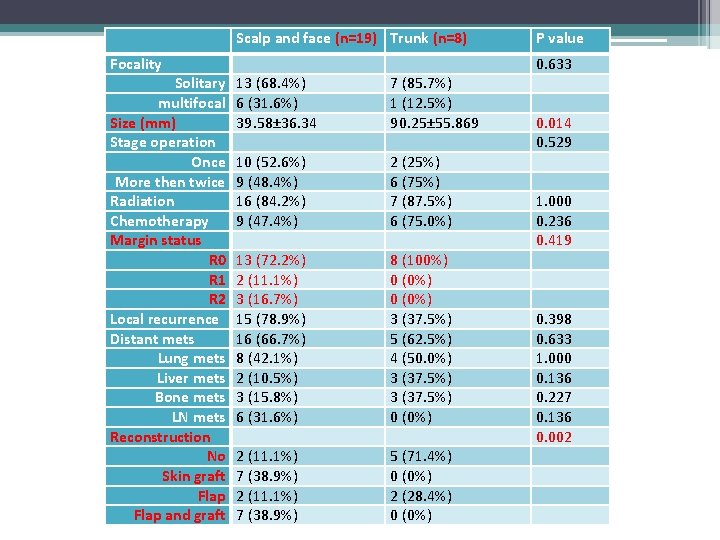
Scalp and face (n=19) Trunk (n=8) Focality Solitary multifocal Size (mm) Stage operation Once More then twice Radiation Chemotherapy Margin status R 0 R 1 R 2 Local recurrence Distant mets Lung mets Liver mets Bone mets LN mets Reconstruction No Skin graft Flap and graft P value 0. 633 13 (68. 4%) 6 (31. 6%) 39. 58± 36. 34 7 (85. 7%) 1 (12. 5%) 90. 25± 55. 869 10 (52. 6%) 9 (48. 4%) 16 (84. 2%) 9 (47. 4%) 2 (25%) 6 (75%) 7 (87. 5%) 6 (75. 0%) 13 (72. 2%) 2 (11. 1%) 3 (16. 7%) 15 (78. 9%) 16 (66. 7%) 8 (42. 1%) 2 (10. 5%) 3 (15. 8%) 6 (31. 6%) 8 (100%) 0 (0%) 3 (37. 5%) 5 (62. 5%) 4 (50. 0%) 3 (37. 5%) 0 (0%) 2 (11. 1%) 7 (38. 9%) 5 (71. 4%) 0 (0%) 2 (28. 4%) 0 (0%) 0. 014 0. 529 1. 000 0. 236 0. 419 0. 398 0. 633 1. 000 0. 136 0. 227 0. 136 0. 002
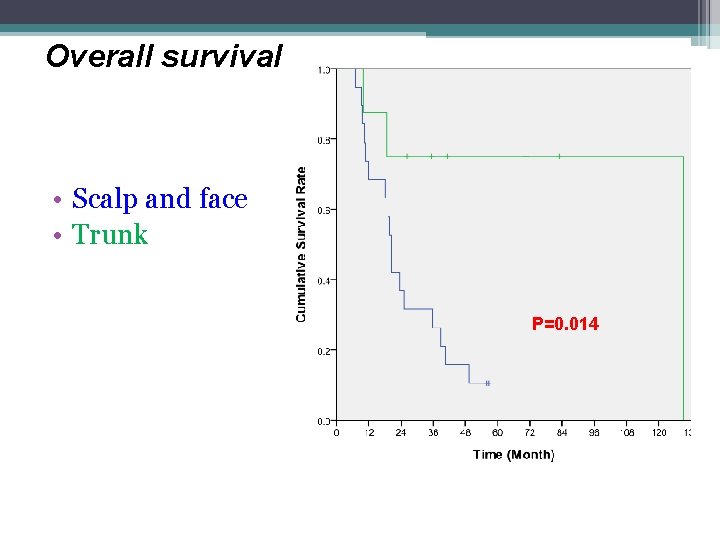
Overall survival • Scalp and face • Trunk P=0. 014
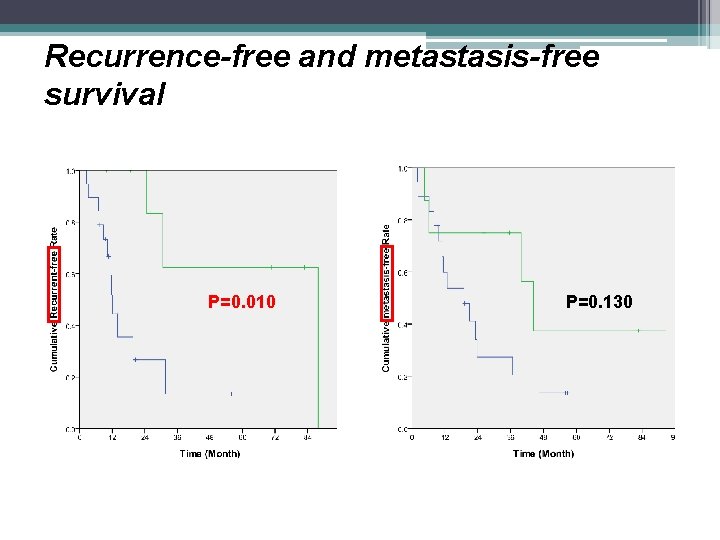
Recurrence-free and metastasis-free survival P=0. 010 P=0. 130

Results • Scalp and face angiosarcomas are more common in old male patients, more difficult to reach free margin status, more likely to recur locally and metastasize distantly with poor prognosis • Usually needs flaps or grafts for reconstruction

• Trunk (breast) angiosarcomas are more common in younger women, usually solitary but bigger in size and easier to reach free margin status, with better prognosis and survival • Patients with liver angiosarcomas often had multifocal lesions, less possible to receive operation with the worst prognosis

Discussion • Represents clinical presentation and treatment of angiosarcoma cases in Taiwan • All 7 cases of breast angiosarcomas in our series didn’t have radiation exposure history, and are primary-breast angiosarcomas • More primary-breast angiosarcoma cases in Taiwan
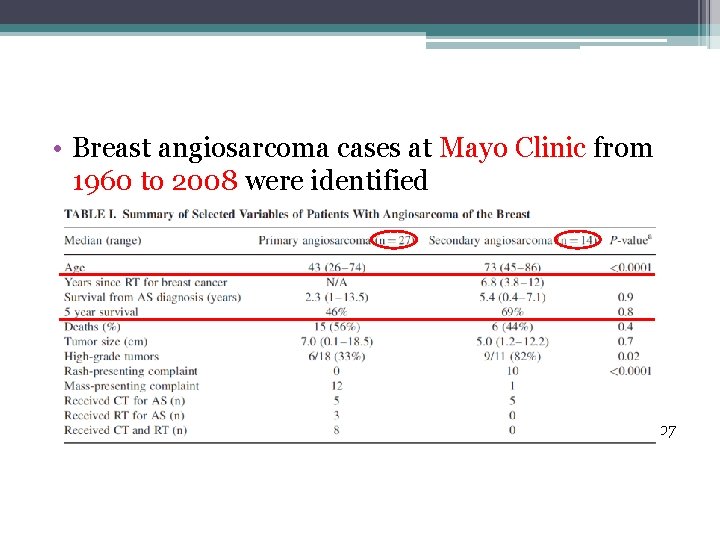
• Breast angiosarcoma cases at Mayo Clinic from 1960 to 2008 were identified - JEFFREY S. SCOW et al, Journal of Surgical Oncology 2010; 101: 401– 407

Limitations • Small sample size • Incomplete patient information • Lack of pathological data
Thank you for your attention!!
- Slides: 23