Professionalism Beauty is in the Eye of the

Professionalism: Beauty is in the Eye of the Beholder CLAUDETTE DALTON, M. D. FALL 2018 CPE WASHINGTON, DC

Objective �To define the un-definable as poorly defined by Boards of Medicine and Osteopathy! �Throw down some gauntlets about possible assessment and remediation

Definition of Professionalism: The Ancients �Hippocrates and Maimonides—a sacred trust to protect and care for the patient and a set of values (2000 BC) �Scribonius--A profession is a commitment to compassion, benevolence and clemency in the relief of suffering. (47 AD)

Louis Brandeis-1914 �Three criteria: A profession is an occupation… where training is intellectual and involves knowledge as distinguished from mere skill pursued largely for others and not merely for one’s self in which the amount of financial return is not the accepted measure of success

Sir William Osler, ACGME and AOA �The practice of medicine is an art; a calling, not a business; a calling which your heart will be exercised equally with your head, a calling which extracts from you at every turn self-sacrifice, devotion, love and tenderness to your fellow man. �ACGME : A commitment to carrying out professional responsibilities, adherence to ethical principles and sensitivity to a diverse patient population. �AOA: An occupation …which is pursued largely for others and not merely for oneself

AOA Professionalism Qualities �Patient first and support of patient rights �Do no harm—at any level �Maintain appropriate relationships with patients and colleagues �No tolerance for lying, cheating, stealing �Commitment to life long learning and improvement and self-assessment �Advocate for improved quality of care and access to care �Work for a just distribution of resources

Common Elements �A social covenant with society �For the benefit of the patient �Sacred trust �Self sacrifice and diligence �Sympathy and empathy �Not about the money or prestige �Ethical codes are part but not all �Requires good communication skills �Situational/context dependent �Part of one’s intrinsic personality—lifelong emotional, cognitive and behavioral qualities. But not intuitive!

Conclusions? �A “Core Pattern of Conduct” �An Identity of Integrity �“Quality isn’t something you lay on top of a subject like a Christmas tree, but is present in the core. ” Zen and the Art of Motorcycle Maintenance �There is no single comprehensive definition �The public equates professionalism as the basis for allowing self-regulation. �“Character is determined by community and vice versa. ” Aristotle �Societal needs lead to regulatory frameworks

State Licensing Boards � Give general, undifferentiated, self-regulated license � Serve the public, not physicians � Complaint driven—”unprofessional conduct” � Look at conduct, not how the physician says they think or feel � Many believe lack of professionalism is the core lesion in most cases and it can usually be identified � Often cannot cite since no regulatory language to support charges. � No access to past issues; no way to monitor going forward � Few assessment options; not sure what to do with them anyway � Difficult to successfully remediate �Licensing boards do not have the tools they need

Professionalism is not Static � State Licensing Boards recognize that there are generational differences �Recognize there are demographic and cultural differences �Recognize that med ed impact is a key factor �And, most importantly, realize that the current changes in how medicine is practiced are influencing professionalism…and the physician’s personal situation that is wrapped around their practice �Every case is multifactorial, situational and individual
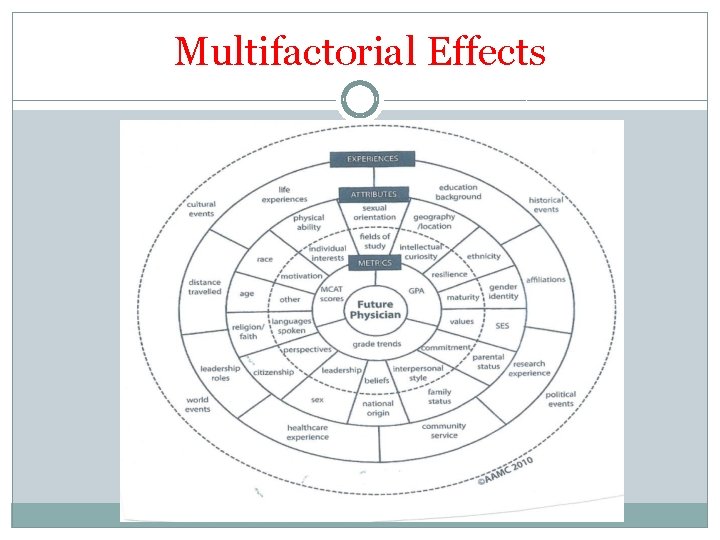
Multifactorial Effects

Other Licensing Board Factors �Failure to report ethical and behavioral lapses early in training and education…and in practice �Complaint driven system precludes active monitoring to ID patterns �Confidentiality often blocks access to data �Lack of a truly reliable way to OBJECTIVELY assess professionalism across populations �Confusion about the line between “ethics” and “professionalism” �Lacking crucial data over time so both prevention and assessment are difficult

Good Assessments �Objective �Trained observers �Valid and reproducible �Cost effective and feasible �Over time/cumulative observations preferable �Needs benchmarks �In context or an equivalent –i. e. focused on the lapse �Have an educational/formative effect �Be a catalytic agent �Use adult learning principles

Adult Learning/Andragogy �Focus on what has utility or need for them. �Context is most important �Integrate new information into established framework �Prefer self-directed learning to groups or classroom �Life changing events often are impetus �Value mentors and expertise �Learn best by doing (Dale’s Cone of Experience)

Existing Assessments �Canadian and other Commonwealth models �Drexel, Vanderbilt, San Diego, other medical school based �CPEP, PACE, other independent �Simulations and Standardized patients �Local psychiatric and other testing modalities �FPPE-like hospital based, peer review driven �Licensing board hearing

Potential Data Sources � 360 degree �Emotional Intelligence instruments �Physical and mental health �Patient satisfaction surveys �Malpractice �Simulations �Mentor/trainer/preceptor longitudinal observations �Case reviews �Access to peer review/hospital credentialing �PLAS
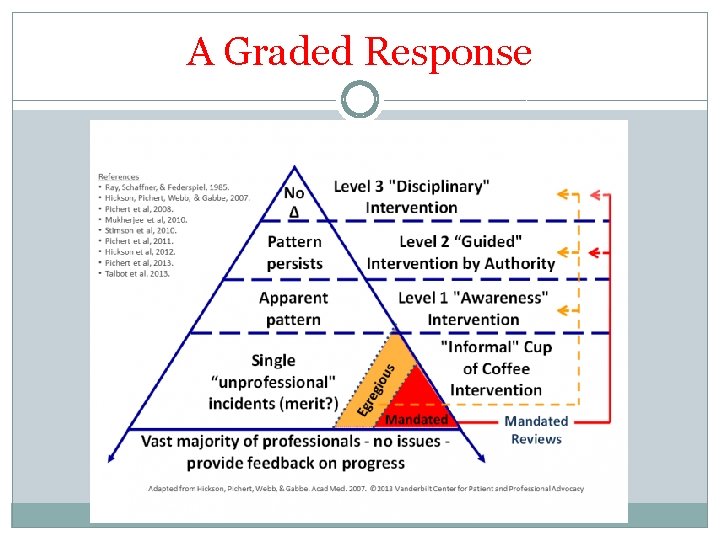
A Graded Response

Successful Remediation Needs �Courses are not enough �Should be done by the profession—and the specialty �Longitudinal surveillance system --for the individual �Graded, situational interventions �Standardized training of mentors, observers and monitors �Definition of success

Remediation Infrastructure Needs �Longitudinal surveillance system --for the individual �Multisource data collection--for the system �Resources for the physician �Resources for those impacted by the physician �On-going monitoring process when needed �Policies and procedures to support reproducibility of the framework �Joint input from medical school to practice �On-going research on causes, assessments and remediation

So, now what? �We need a common sense of what we are trying to regulate: Is it Art or not? �Need better regulatory language that meshes with bylaws language �Communication between undergraduate, graduate and practices on concerns �Need better—and consistent--assessment tools and remediation options �BUT…lacking those, we need the backbone to say— from the beginning and all along the way—that this won’t fly…

Thank you! QUESTIONS? CED 2 T@HOTMAIL. COM
- Slides: 21