PROF MANZUR MORSHED FCPS MRCP ADVISER BTF Overview

PROF. MANZUR MORSHED FCPS, MRCP ADVISER, BTF Overview of the Management of Thalassemia

“Patients with optimally treated thalassemia can now enjoy a nearnormal life and lifestyle, and experience regular physical and emotional development from childhood to adulthood”. – TIF guidelines for TDT; 3 rd edition (2014) p 224

Goal of treatment • To maintain the best possible quality of life with minimum intervention • Regular monitoring/follow up is the key to maintain a good quality life • Treatment of a thalassemia patient – whether TDT or NTDT - needs a serious commitment from treating doctor

Management of b thalassemia • General care and nutrition • Blood transfusion • Iron chelation: s/c Desferioxamine, oral deferasirox/ deferiprone • Drugs aiming at increment of Hb • Splenectomy – indications and precautions • Management of thrombosis, Pul HTN and leg ulcer • Management of endocrine, hepatic and cardiac complications • Management of fertility and pregnancy • Curative treatment • Stem cell transplantation • Gene therapy

Management of b thalassemia • General care and nutrition • Blood transfusion • Iron chelation: s/c Desferioxamine, oral deferasirox/ deferiprone • Drugs aiming at increment of Hb • Splenectomy – indications and precautions • Management of thrombosis, Pul HTN and leg ulcer • Management of endocrine, hepatic and cardiac complications • Management of fertility and pregnancy • Curative treatment • Stem cell transplantation • Gene therapy

Management of b thalassemia • General care and nutrition • Blood transfusion • Iron chelation: s/c Desferioxamine, oral deferasirox/ deferiprone • Drugs aiming at increment of Hb • Splenectomy – indications and precautions • Management of thrombosis, Pul HTN and leg ulcer • Management of endocrine, hepatic and cardiac complications • Management of fertility and pregnancy • Curative treatment • Stem cell transplantation • Gene therapy – Monitoring and follow up plan

General Care and Nutrition • Growth and Qo. L : Observation and supportive care – appetite – activity, schooling, employment and social life • Diet: Poor growth can be due to nutritional factors such as caloric intake and micronutrient deficiencies. – Iron restriction myth – A diet high in calcium is also recommended (milk, fish, cheese etc. ). – A diet rich in high Vitamin E content, ie; eggs and vegetable oils, nuts.

General Care and Nutrition • Calcium & Vitamin D: Recommended for all thalassemics, along with measurements of vitamin D levels every few months. • Folic acid: Apart from Hb synthesis, risk of thrombosis is also reduced. • Vitamin C: 2 -3 mg/kg/day, with DFO infusions, or if deficiency is proven. • L-carnitine: May be beneficial (50 mg/kg/day). • Silymarin: In case of liver involvement. Dose is 140 mg 3 times daily. • Zinc: Not recommended as routine. • Wheat grass: Insufficient evidence for any long term benefits.

General Care and Nutrition • Alcohol, tobacco and substance abuse should be avoided • Physical activity should be encouraged. • Co-morbidities need appropriate evaluation. • Routine dental care: Maxillary deformities may occur in absence of adequate blood transfusions from an early age. Orthodontic interventions may become necessary.

Management of Fever Two major risks during fever • Worsening of anemia • Serious sepsis During the clinic or ER visits • Check hemoglobin, reticulocyte count and bilirubin • Admit for observation or transfusion if the hemoglobin low • Antibiotic treatment may be needed Splenectomized patients with a fever • Should be seen on the same day • Given a dose of intravenous antibiotic, admission recommended

Drugs to reduce the need for transfusion in beta thalassemia

Ways to increase Hb production • Induction of Fetal Hb (α 2γ 2) – – – Hydroxyurea (DNA-binding drug) Thalidomide histone deacetylase inhibitors (azacitidine, decitabine) m. TOR pathway inhibitors : Everolimus Metformin • Targeting IE (ineffective erythropoesis) – – JAK 2 inhibitors Activin receptor trap ligands Iron restriction erythropoisis α-globin synthesis reduction

Induction of Hb. F (α 2γ 2) • Increased production of γ-globin leads to decreased imbalance between β & α-chains resulting in haemolysis reduction. • Also - inherited persistent high levels of Hb. F have a milder clinical course than other patients with Thalassemia. • Therefore, therapeutic approaches reactivating and increasing Hb. F concentration, are attractive. • Accordingly, several studies were done with potential inducers of Hb. F – particularly with hydroxyurea.

Hydroxyurea • Experience from Iran and India – many patients were reported to have become transfusionindependent – in patients who were not transfused, the Hb concentration increased – the combination of hydroxyurea with L-carnitine or magnesium could be more effective in improving hematologic parameters and cardiac status in patients with TI than hydroxyurea alone • Experience from Europe – constant increase of the RBC volume and in Hb. F, but only a modest effect on total Hb concentration Karimi M, et al. J Pediatr Hematol Oncol. 2005; 27: 380 -5. Dixit A, et al. Ann Hematol. 2005; 84: 441 -6. Karimi M, et al. Eur J Haematol. 2010; 84: 52 -8.

Hydroxyurea (Cont’d) • Predictive of good response: – Co-inheritance of α-thalassemia, – the Xmn-1 HBG 2 polymorphism, and – the underlying β-globin genotype – Hb E/β-thalassemia patients • Treatment with hydroxyurea has also shown promising results in decreasing plasma markers of thrombin generation Singer ST, et al. Br J Haematol. 2005; 131: 378 -88. Panigrahi I, et al. Hematology. 2005; 10: 61 -3. Ataga KI, et al. Br J Haematol. 2007; 139: 3 -13.
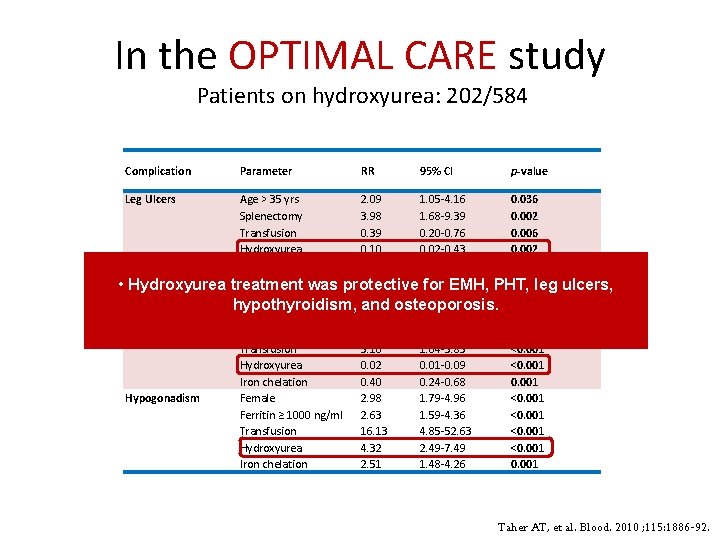
In the OPTIMAL CARE study Patients on hydroxyurea: 202/584 Complication Leg Ulcers Hypothyroidism • Hydroxyurea Osteoporosis Hypogonadism Parameter RR 95% CI p-value Age > 35 yrs 2. 09 1. 05 -4. 16 0. 036 Splenectomy 3. 98 1. 68 -9. 39 0. 002 Transfusion 0. 39 0. 20 -0. 76 0. 006 Hydroxyurea 0. 10 0. 02 -0. 43 0. 002 Splenectomy 6. 04 2. 03 -17. 92 0. 001 Hydroxyurea was protective 0. 05 0. 01 -0. 45 0. 003 leg treatment for EMH, PHT, Age > 35 yrs 3. 51 2. 06 -5. 99 <0. 001 hypothyroidism, and osteoporosis. Female 1. 97 1. 19 -3. 27 0. 009 Splenectomy 4. 73 2. 72 -8. 24 <0. 001 Transfusion 3. 10 1. 64 -5. 85 <0. 001 Hydroxyurea 0. 02 0. 01 -0. 09 <0. 001 Iron chelation 0. 40 0. 24 -0. 68 0. 001 Female 2. 98 1. 79 -4. 96 <0. 001 Ferritin ≥ 1000 ng/ml 2. 63 1. 59 -4. 36 <0. 001 Transfusion 16. 13 4. 85 -52. 63 <0. 001 Hydroxyurea 4. 32 2. 49 -7. 49 <0. 001 Iron chelation 2. 51 1. 48 -4. 26 0. 001 ulcers, Taher AT, et al. Blood. 2010 ; 115: 1886 -92.

Hydroxyurea side effects However, side effects include – cytopenia, – hyperpigmentation, – weight gain, – opportunistic infections, – azoospermia in approximately 80% of men (even years after the end of treatment), and – marked hypomagnesemia. – Teratogenicity.

Safety measures to reduce harm from Hydroxyurea > Not be used in pregnant women or patients with hepatic or renal failure > CBC, Hepatic and renal function studies, q 2 weeks for the first 3 months & then monthly > History and physical examination evaluating for GI, neurologic, or dermatologic side-effects, monthly Ø Gonadal function follow-up • Restrict use in the following groups of NTDT patients: – Patients for which a transfusion course is required but are alloimmunized – Patients with following morbidities – Pulmonary HTN, EMH pseudotumors, Leg ulcers.

Hydroxyurea • Dose: Start at 10 mg/kg/day with escalation q 8 wks to maximal tolerated dose, but not exceeding 20 mg/kg/day. • Response evaluation: – At 3 and 6 months of therapy - Hb increase of >1 g/dl. – Discontinue in patients not showing response. – Re-evaluate at 12, 18, and 24 months to ensure maintenance of response. • Though baseline Hb. F level and it’s response to HU is dependent on genetic factors, criteria for treatment should not be based on genetic characteristics.

Thalidomide • A synthetic glutamic acid derivative, was used as a sedative as well as an anti-emetic. Because of serious teratogenic effects in pregnant women, it was withdrawn. • Relaunched for its anti-angiogenic properties and is now used in various inflammatory disorders and certain malignancies such as MPN, MDS, Multiple Myeloma. • Mechanism of action: – Hb. F production: It is postulated that thalidomide might have effect on the γ-globin gene through ROS-p 38 MAPK signaling pathway as other Hb. F stimulating drugs. Therefore Thalidomide causes an increase in Hb through raising Hb. F. – Downregulation of alpha chain production, thereby reducing alpha: beta ratio.

Are we ready for thalidomide as a routine drug in thalassemia? • The answer is a clear “No”! • Not yet undergone adequate trials for its routine use in thalassemia. • Has significant adverse events including serious life-threatening ones. Thrombosis has already been reported even with a single course of thalidomide in a patient of thalassemia major. • Only anecdotal reports of its use in those patients, in whom transfusions were near impossible due to alloimmunisation and other immunomodulators failed to improve the situation. • It is mandatory to explain to the patients and their families the need for use of a non-approved drug with its inherent life-threatening adverse effects. Only if they then consent, should it be used. • ………. . Presently, therefore, it has no role in routine management of thalassemia syndromes. Management of ß-thalassemia – Consensus and controversies! Mamta V Manglani et al; Pediatric Hematology Oncology Journal 2; 4, 2017, 94 -97

SPLENECTOMY

Splenectomy • Less common than in the past because – – proper transfusion regimen and chelation has brought the disease very well controlled and reduced the incidence of splenomegaly and iron overload – the high disease burden (complications) associated with it. • Main indications include – growth retardation or poor health with increased transfusion demand (to reduce excessive blood consumption and consequent severe iron overload) – Leukopenia/thrombocytopenia (Hypersplenism) – symptomatic splenomegaly vless transfusion requirement

Splenectomy: adverse events • Splenectomy was independently associated with an increased risk of most disease-related complications. • Thromboembolic events– Venous thrombosis – Silent brain infarctions • Pulmonary hypertension • Infection - sepsis – 10 -year follow-up of 221 splenectomized patients, 6 of whom died of sepsis – no need to “wait & see” in such patients with fever Cappellini MD, et al. Br J Haematol. 2000; 111: 467 -73. Atichartakarn V, et al. Int J Hematol. 2003; 78: 139 -45. Pinna AD, et al. Surg Gynecol Obstet. 1988; 167: 109 -13.
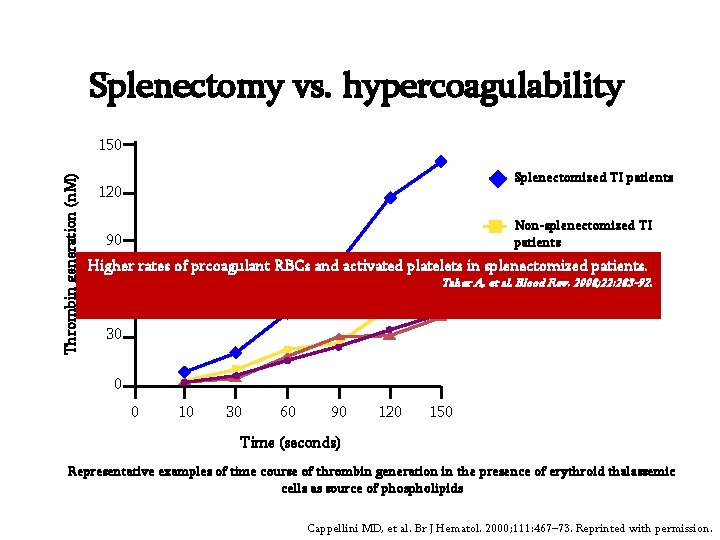
Splenectomy vs. hypercoagulability Thrombin generation (n. M) 150 Splenectomized TI patients 120 Non-splenectomized TI patients 90 Higher rates of prcoagulant RBCs and activated platelets in splenectomized patients. Normal controls Taher A, et al. Blood Rev. 2008; 22: 283 -92. 60 Splenectomized controls 30 0 0 10 30 60 90 120 150 Time (seconds) Representative examples of time course of thrombin generation in the presence of erythroid thalassemic cells as source of phospholipids Cappellini MD, et al. Br J Hematol. 2000; 111: 467– 73. Reprinted with permission.

Splenectomy care • Should be avoided in patients <5 years • If splenectomy is indicated, patients should receive the following vaccines (2 weeks prior to and then 3 to 5 years later): – – Pneumococcal 23 -valent polysaccharide vaccine – (s/c or i/m) H influenzae vaccine - If not administered as childhood immunizations Meningococcal polysaccharide vaccine Influenza vaccine annually • Patients who underwent splenectomy without being given the vaccine may still benefit from vaccination postsplenectomy • Post-splenectomy sepsis remains a risk; therefore, febrile splenectomized patients should undergo rapid evaluation and treatment.

Post-splenectomy prophylaxis • Compliance with prophylactic abx should be stressed while explaining that it does not entirely prevent postsplenectomy sepsis. • Splenectomized patients should receive prophylactic abx for > 2 years following splenectomy (for children until >5 years of age) – P. O. penicillin, 125 mg bid for age <2 yrs, & 250 mg bid for >2 yrs – Alternatives include amoxicillin, TMP-SMZ, and erythromycin • The GB should be inspected and removed during splenectomy if there is evidence of gallstones. Liver biopsy may be considered.

Thrombotic disease

Thrombotic disease • The following subgroups of NTDT patients should be considered at higher risk of thrombosis or CVD, : – – – • • Adult patients Splenectomized patients Never or previously minimally transfused patients Patients with elevated platelet counts (≥ 500 x 109/l) Patients with elevated nucleated RBCs (≥ 300 x 106/l) Patients with a Hb level <9 g/dl Patients with a history of pulmonary hypertension Patients with iron overload Pregnant patients Patients with a personal or family history of thrombosis Patients with other conventional risk factors for thrombosis or CVD Patients developing thrombotic or CVD should be treated as per standard guidelines In high-risk patients prophylactic anticoagulants/antiaggregants should be given. Aspirin should be given in splenectomized NTDT patients with platelets ≥ 500 x 109/l. Transfusion should be considered for prevention of thrombotic or CVD in high-risk patients.

Pulmonary HTN • NTDT patients should undergo yearly echocardiogram for the assessment of Pulmonary HTN • Patients ‘likely’ to have pulmonary HTN on echo should undergo right heart catheterization to confirm the diagnosis. Ventilation/perfusion lung scan is also recommended to rule out pulmonary thromboembolic disease • Patients with ‘possible’, ‘likely’, or confirmed pulmonary hypertension may benefit from the following interventions > Blood transfusion & adequate control of iron overload status > hydroxyurea > Sildeanfil citrate > Anticoagulant therapy

CONCLUSION

The initial clinic visit Review laboratory results • Hematological • Electrophoresis • DNA tests Establish baseline evaluation Counseling • Discuss probable outcome and uncertainties • Stress that close follow up is essential to make informed decisions Introduce the care team • Physician, Nurse, Social Worker etc • Provide support

Montioring/Follow up • Frequency of visits – Initially every month, then 2 months, then 3 -12 months • Growth and development – Height and weight, pubertal development • Nutrition – Folate, vitamin D, avoiding supplemental iron • Endocrine, cardiac, iron status • Counseling for risk during infections • Building relationship – Accessibility, social work assessment.
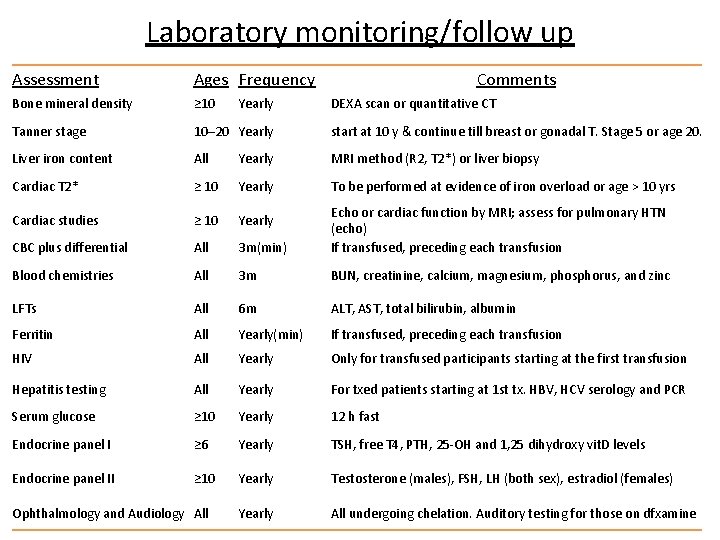

Laboratory monitoring/follow up Assessment Ages Frequency Bone mineral density ≥ 10 Tanner stage 10– 20 Yearly start at 10 y & continue till breast or gonadal T. Stage 5 or age 20. Liver iron content All Yearly MRI method (R 2, T 2*) or liver biopsy Cardiac T 2* ≥ 10 Yearly To be performed at evidence of iron overload or age > 10 yrs Cardiac studies ≥ 10 Yearly CBC plus differential All 3 m(min) Echo or cardiac function by MRI; assess for pulmonary HTN (echo) If transfused, preceding each transfusion Blood chemistries All 3 m BUN, creatinine, calcium, magnesium, phosphorus, and zinc LFTs All 6 m ALT, AST, total bilirubin, albumin Ferritin All Yearly(min) If transfused, preceding each transfusion HIV All Yearly Only for transfused participants starting at the first transfusion Hepatitis testing All Yearly For txed patients starting at 1 st tx. HBV, HCV serology and PCR Serum glucose ≥ 10 Yearly 12 h fast Endocrine panel I ≥ 6 Yearly TSH, free T 4, PTH, 25 -OH and 1, 25 dihydroxy vit. D levels Endocrine panel II ≥ 10 Yearly Testosterone (males), FSH, LH (both sex), estradiol (females) Yearly All undergoing chelation. Auditory testing for those on dfxamine Ophthalmology and Audiology All Yearly Comments DEXA scan or quantitative CT

Challenges for Quality treatment • Noncompliance to treatment – Financial – Education – Lack of support • Intolerance and Complications of drugs • Lack of availability of appropriate blood products and drugs

Last word • Protocol based but individualized plan is needed for appropriate management. • The protocol should be made by a coordinated effort by the dedicated “thalassemia care givers” keeping the real scenario of our patients in mind. • Co-operation and coordination among different specialties (Adult and Pediatric Physicians, Cardiologists, Gynecologists, Endocrinologists, Gastroenterologists etc) is very much needed to manage these patients appropriately.
- Slides: 36