Principles Practice of Evidencebased Medicine Roberto Cardarelli DO

Principles & Practice of Evidence-based Medicine Roberto Cardarelli, DO, MHA, MPH

Outline • Defining Evidence-based medicine (EBM) • Background of EBM • Practicing EBM • Limitations of EBM • How to ask answerable clinical questions

What is EBM? • EBM is the integration of: – Best research evidence • Clinically relevant • Patient oriented • Such as dx tests, prognostic markers, therapy – Clinical expertise • Use of clinical skills and past experiences to identify a patient’s unique health states and needs – Patient values • Unique preferences, concerns, & expectations each patient brings

Why EBM? • “Clinical Epidemiology”. • Current era was established and renamed EBM in 1992 by a group led by Gordon Guyatt at Mc. Master University in Canada. • The spread of EBM arose from 4 realizations: – Our daily need for valid information about dx, prognosis, tx, and prevention – Inadequacy of traditional sources (texts) – Disparity between diagnostic skills and clinical judgment vs. up-to-date knowledge and clinical performance – Inability to afford more than a few second per pt for finding and assimilating the evidence

Why EBM? • Development of these strategies have made practicing EBM possible: – Strategies for efficiently tracking down and appraising evidence – Creation of systematic reviews and concise summaries (i. e. Cochrane Collaboration) – Evidence based journals of secondary publications – ID’ing and applying strategies for lifelong learning and for improving our clinical performance

Why EBM? • Keeping up – knowledge explosion – medical literature • Life-long, self-directed learning • Enhancing clinical practice, resulting in better patient outcomes. • Teaching students/residents based on valid evidence. • What sources do you use?

Practicing EBM • Clinically important evidence - POEMS – therapy – diagnostic tests – harm – prognosis – cost-effectiveness • DOES – molecular biology – pathophysiology

Practicing EBM • Framework of EBM – Are the results of the study valid? – What are the results? – Will the results help with caring for my patients?

Practicing EBM • Step 1: Create an answerable question • Step 2: Track down the best evidence to answer your question • Step 3: Critically appraise that evidence for its validity (closeness to the truth), impact (size of effect), applicability (useful to your pt) • Step 4: Integrate the critical appraisal with our clinical expertise and with our pt’s unique biology, values, and circumstances • Step 5: Evaluate our effectiveness and efficiency in steps 1 -4 and seek ways to improve them for the next time

Types of Clinical Questions • • Therapy -- Is this treatment any good? Diagnostic test -- How good is this test? Harm -- Does this exposure cause harm? Prognosis -- What is the likely clinical course? • Economic Analysis -- Is this intervention cost-effective? • Clinical Guideline -- What should I do for this problem? • Overview -- Is there scientific evidence to guide our decisions?

Information to look for… • Some conditions and their treatments change frequently– What do you do? • YOU find the best current evidence that gives up-to -date protocols that are crucial to medical management. • Conditions that are encountered less often. – What do you do? • You should try to find a review (EBM) that another person may have done. Just make sure that you can apply the evidence to your patient.

Limitations to EBM • Shortage of coherent scientific evidence • Difficulties of applying evidence to an individual pt • Developing new skills to practice EBM (searching EBM, statistics, etc) • Limited time of the busy practitioner • Evidence that “EBM” works is limited.

Step 1: Asking a clinical question • Background questions have 2 components – Question root – Aspect of the disorder – Ex: What causes cyanosis? • Foreground questions w/ 4 components: – – Pt or problem of interest The main intervention (dx, tx, prognostic fx’s) Comparison intervention(s), if relevant Clinical outcome(s) of interest

Step 1: Asking a clinical question • When our experience of a specific condition is limited- we tend to ask more background questions • As our experience grows- we should and tend to ask more foreground questions – EX: In patients with suspected pneumonia, are any clinical findings sufficiently powerful to confirm or exclude pneumonia all by themselves, or is a CXR necessary for the dx?
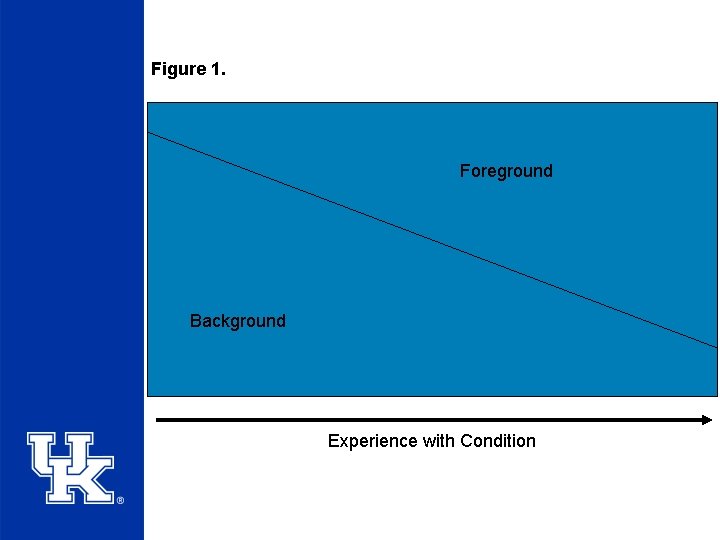
Figure 1. Foreground Background Experience with Condition

Rx Educational Prescription Pt Name: Date: Target Disorder: Intervention (+/- comparison): Outcome: Discuss: Search strategy Search results Validity Importance of the valid results Can you apply this to your pt

Rx Educational Prescription Pt Name: John Doe Date: 8/18/03 Target Disorder: Pneumonia Intervention (+/- comparison): Power of clinical exam vs clinical exam + CXR Outcome: Confirm or exclude pneumonia Discuss: Search strategy Search results Validity Importance of the valid results Can you apply this to your pt

Curriculum for next 5 lectures • • • Diagnosis and screening Prognosis Therapy Harm Applying EBM to your patient
- Slides: 18