Principles of Surgery Evaluation of Abdominal Trauma Anand

Principles of Surgery Evaluation of Abdominal Trauma Anand Pandya MD FRCSC Trauma Surgery and Critical Care Medicine Clinical Associate St. Michael’s Hospital, University of Toronto

Objectives n Evaluation of Abdominal Trauma Mechanisms of Injury n Assessment of Unstable Patients n Assessment of Stable Patients n Case Discussions n n Diagnostic tests n Decision making
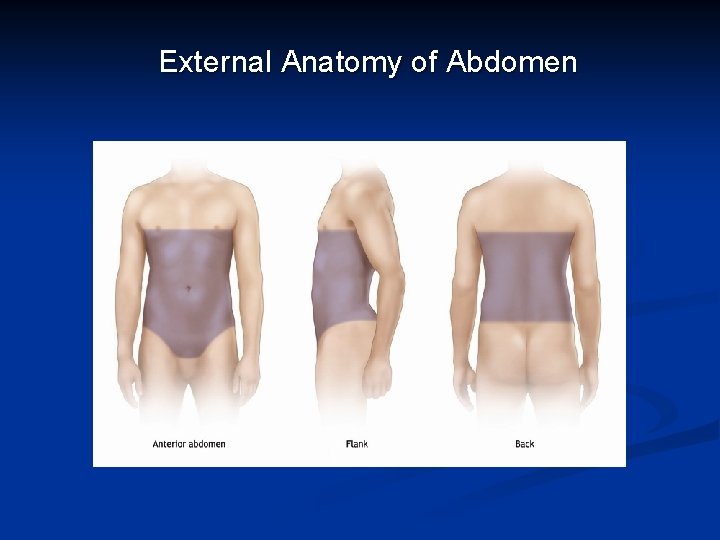
External Anatomy of Abdomen

Mechanism of Injury: Blunt n Compression, crush, or sheer injury to abdominal viscera: deformation of solid or hollow organs, rupture (e. g. small bowel, gravid uterus) n Deceleration injuries: differential movements of fixed and non-fixed structures (e. g. liver and spleen laceration at sites of supporting ligaments)
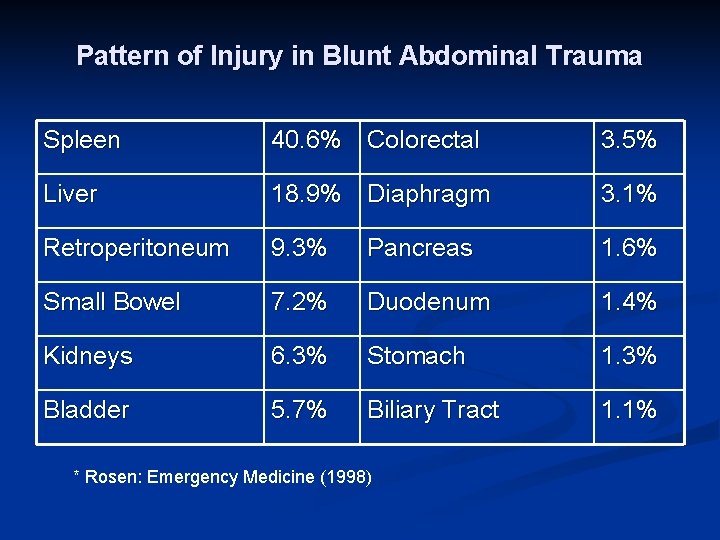
Pattern of Injury in Blunt Abdominal Trauma Spleen 40. 6% Colorectal 3. 5% Liver 18. 9% Diaphragm 3. 1% Retroperitoneum 9. 3% Pancreas 1. 6% Small Bowel 7. 2% Duodenum 1. 4% Kidneys 6. 3% Stomach 1. 3% Bladder 5. 7% Biliary Tract 1. 1% * Rosen: Emergency Medicine (1998)

Mechanism of Injury: Penetrating ● Stab ● Low energy, lacerations ● Gunshot ● Kinetic energy transfer ● Cavitation, tumble ● Fragments

Assessment: History n n n AMPLE Mechanism MVC: n n n Speed Type of collision (frontal, lateral, sideswipe, rear, rollover) Vehicle intrusion into passenger compartment Types of restraints Deployment of air bag Patient's position in vehicle
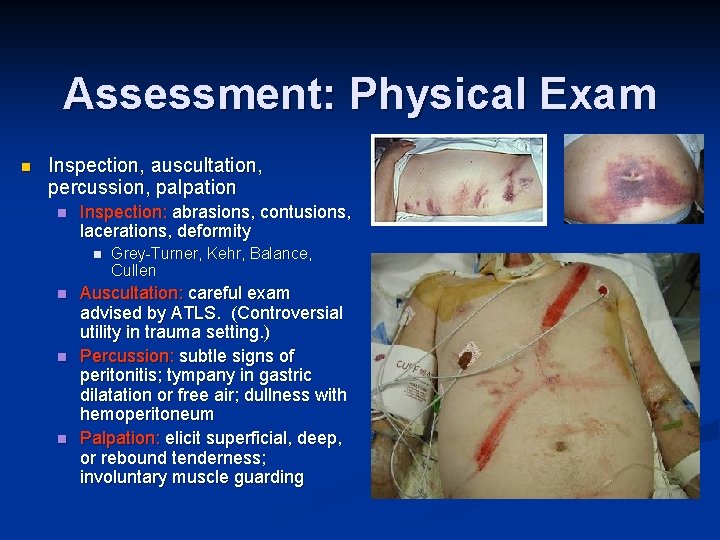
Assessment: Physical Exam n Inspection, auscultation, percussion, palpation n Inspection: abrasions, contusions, lacerations, deformity n n Grey-Turner, Kehr, Balance, Cullen Auscultation: careful exam advised by ATLS. (Controversial utility in trauma setting. ) Percussion: subtle signs of peritonitis; tympany in gastric dilatation or free air; dullness with hemoperitoneum Palpation: elicit superficial, deep, or rebound tenderness; involuntary muscle guarding

Abdominal Injury Factors that Compromise the Exam ● Alcohol and other drugs ● Injury to brain, spinal cord ● Injury to ribs, spine, pelvis Caution A missed abdominal injury can cause a preventable death.

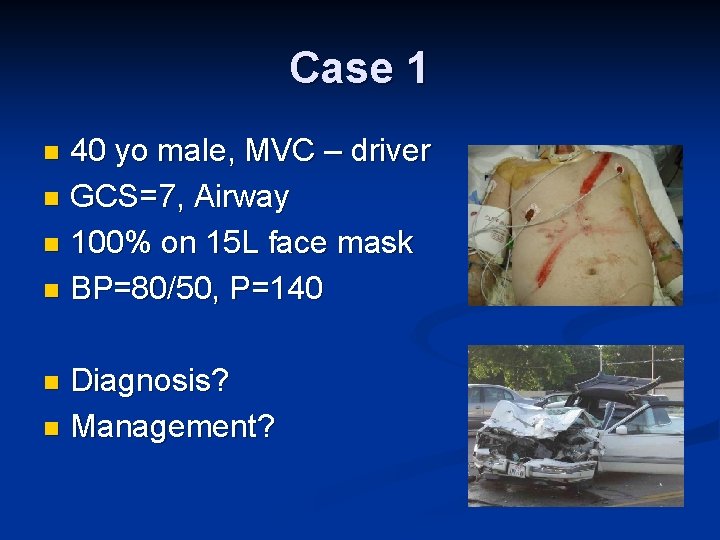
Case 1 40 yo male, MVC – driver n GCS=7, Airway n 100% on 15 L face mask n BP=80/50, P=140 n Diagnosis? n Management? n
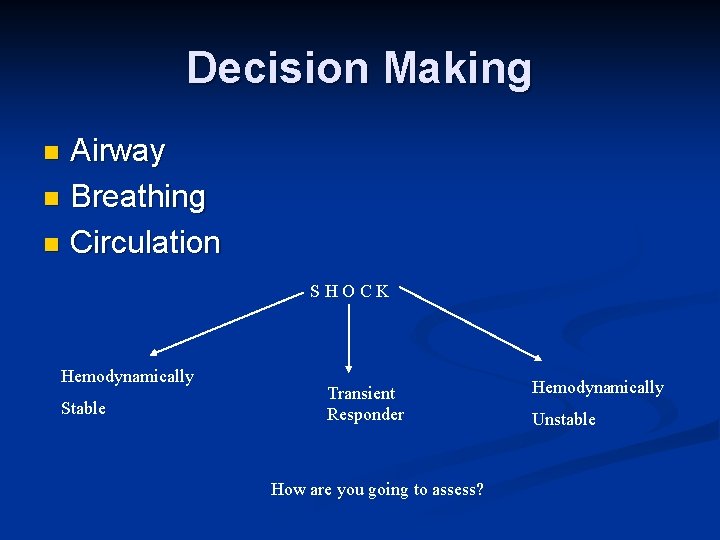
Decision Making Airway n Breathing n Circulation n SHOCK Hemodynamically Stable Transient Responder How are you going to assess? Hemodynamically Unstable

Shock Scalp n Chest – clinically vs. chest x-ray n Abdomen n FAST n DPL n Pelvic X-ray n Extremities – Femur n Other causes of shock – cardiogenic, obstructive, anaphylactic, septic n

FAST

Focused Abdominal Sonography for Trauma (FAST) n Demonstrate presence of free intraperitoneal fluid n Evaluate solid organ hematomas n Advantages n n No risk from contrast media or radiation Rapid results, portability, non-invasive, ability to repeat exams. n Disadvantages n n n Cannot assess hollow visceral perforation Operator dependent Retroperitoneal structures are not visualized
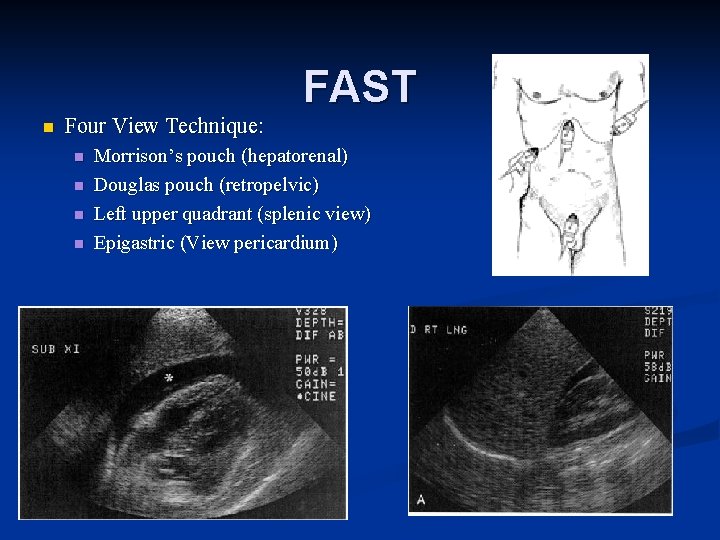
FAST n Four View Technique: n n Morrison’s pouch (hepatorenal) Douglas pouch (retropelvic) Left upper quadrant (splenic view) Epigastric (View pericardium)

Diagnostic Peritoneal Lavage n n Introduced by Root (1965) Indications for DPL in blunt trauma: 1. Hypotension with evidence of abdominal injury 2. Multiple injuries and unexplained shock 3. Potential abdominal injury in patients who are unconscious, intoxicated, or paraplegic 4. Equivocal physical findings in patients who have sustained high-energy forces to the torso 5. Potential abdominal injury in patients who will undergo prolonged general anesthesia for another injury, making continued reevaluation of the abdomen impractical or impossible

Contraindications of DPL n Absolute : n n n Peritonitis Injured diaphragm Extraluminal air by x-ray Significant intraabdominal injury by CT scan Intraperitoneal perforation of the bladder by cystography Relative : n n n Previous abdominal operations (because of adhesions) Morbid obesity Gravid Uterus Advanced cirrhosis (because of portal hypertension and the risk of bleeding) Preexisting coagulopathy

DPL: Procedure

Evaluation of DPL n Fluid is sent for: cell count, amylase, alk phos, presence of bile Aspirate Lavage Negative Index Positive value Blood >10 m. L Fluid Enteric content RBC > 100, 000/m. L WBC > 500/m. L Amylase >175 U/d. L Alk Phos > 3 IU Bile Confirmed RBC < 50, 000/m. L WBC < 100/m. L Amylase < 75 U/d. L

Diagnostic Peritoneal Lavage RBC Count Incidence of visceral damage >100, 000 95% 20, 000 -100, 000 15 -25% Warrant further investigation <20, 000 < 5% n Complications of DPL: Perforation of small bowel, mesentery, bladder and retroperitoneal vascular structures. n Limitation: offers no information about status of retroperitoneal organs nor allow determination of which organ has been injured.
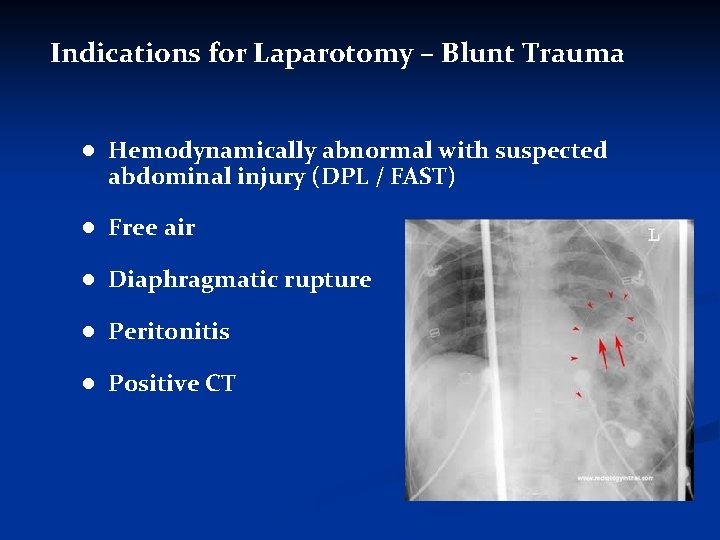
Indications for Laparotomy – Blunt Trauma ● Hemodynamically abnormal with suspected abdominal injury (DPL / FAST) ● Free air ● Diaphragmatic rupture ● Peritonitis ● Positive CT

On Route to OR n n ABC Chest x-ray, Pelvis x-ray IV access Resuscitation n n n What is the goal? Group and Match Notify OR, Surgeon, Anaesthesia Request OR equipment Consent Antibiotics
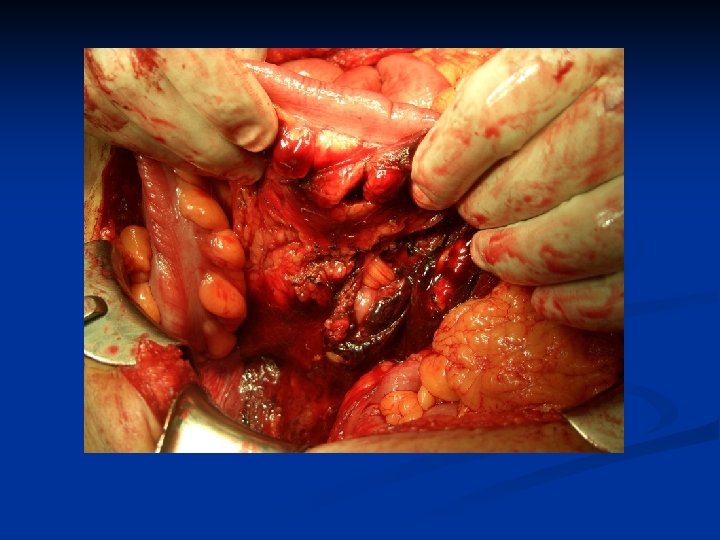

Case 1: Learning Points Recognize Shock n Hemodynamically unstable = OR n Role of FAST, DPL n Permissive hypotension in resuscitation until bleeding controlled n

Case 2: 40 yo male, MVC Driver n Airway n Breathing = 100% on 5 L NP n Circulation = 130/70, P=100 n Disability, GCS=14 n Exposure n n Management?

How do you investigate the Abdomen? n Hemodynamically stable: ABCDE, secondary survey n FAST n CT Scan n Lab work n

Imaging in Blunt Abdominal Trauma – CT Scan n Sensitivity: n Solid organ injury: 97% [II, III] n Identify Contrast extravasation n Guide Operative vs. Non-operative management n Enteric injury: 64 – 94% [III] n Diaphragmatic injury: 61% [III] n Pancreatic injury: 30% [III]

CT Scan
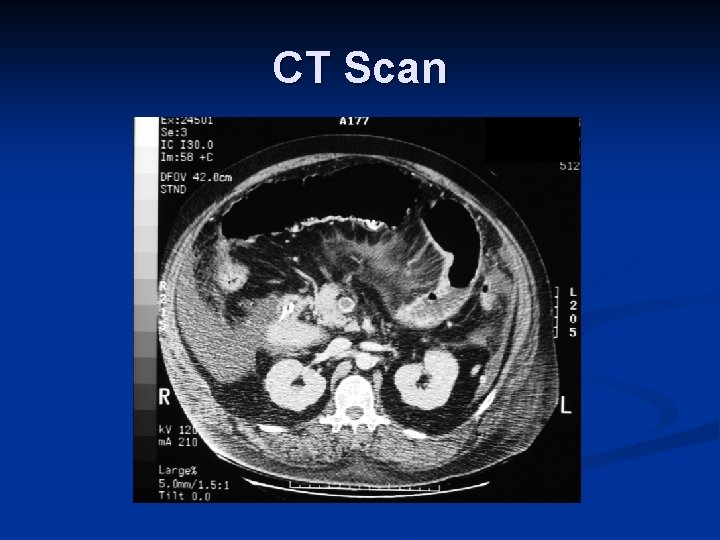
CT Scan
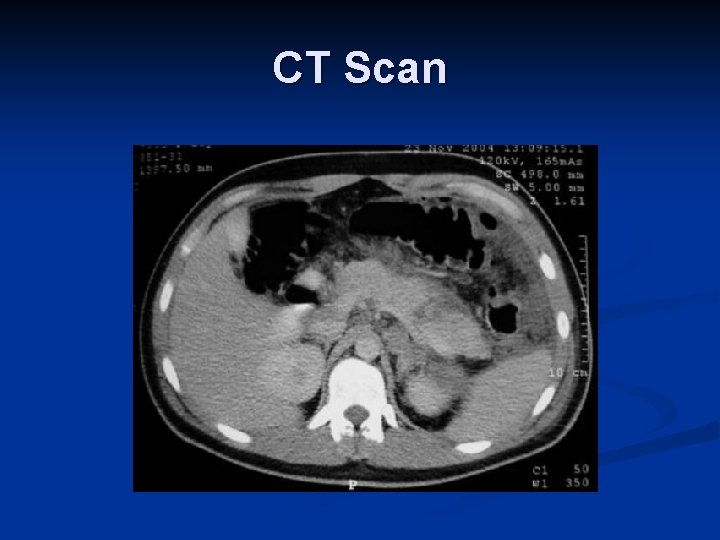
CT Scan

Role of Laboratory Tests Amylase n B-HCG n

In Pregnancy X-rays n Ultrasound n Abdominal n Fetal n Circumferential Lead Shield n Caution with Radiation exposure n

Decision Making n n n Stable patient CT Scan Operative n n n Solid organ injury, hypotensive Hollow viscus organ injury Intraperitoneal bladder injury Diaphragmatic injury Non-operative management n n Observation Interventional Radiology

Learning Points Case #2 CT scan is helpful for decision making in a stable patient n Poor detection of hollow viscus, pancreatic and diaphragmatic injury n Be worried of free fluid in abdomen n Repeat CT Scan and close clinical observation n
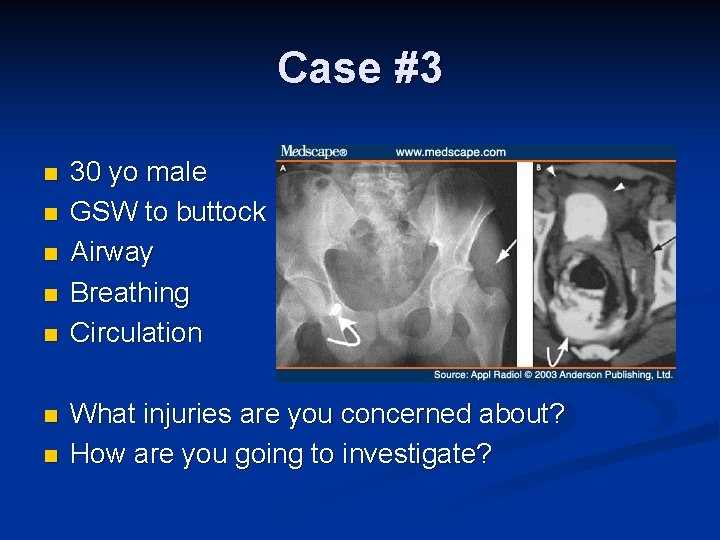
Case #3 n n n n 30 yo male GSW to buttock Airway Breathing Circulation What injuries are you concerned about? How are you going to investigate?

Transpelvic GSW n Rectal injury Extraperitoneal – rigid sigmoidoscopy n Intraperitoneal – CT scan with rectal contrast or laparotomy n n Bladder injury Hematuria n Cystogram n n Urethral injury n Retrograde urethrogram

Transpelvic GSW n Vascular injury FAST n CT Scan n n Pelvic fracture n n X-ray Female – Uterine injuries n CT Scan

Decision Making Low threshold for laparotomy with GSW n Bowel injury = sigmoidoscopy n Intraperitoneal – repair/resect n Extraperitoneal – diversion n n Bladder injury = cystogram Intraperitoneal – surgical repair n Extraperitoneal – foley catheter n

Learning Points Case #3 Think of associated injuries n GSW have blast effect, variable trajectory n Diagnostic tests guide treatment n Early laparotomy n
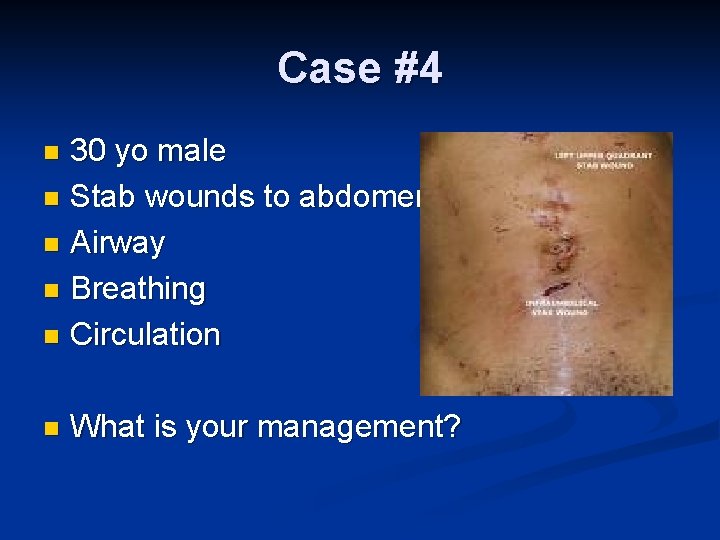
Case #4 30 yo male n Stab wounds to abdomen n Airway n Breathing n Circulation n n What is your management?

Options for Management Diffuse Abdominal Tenderness Yes Laparotomy No Hemodynamic Stability? Indications for Laparotomy – Penetrating Trauma ● ● ● Hemodynamically abnormal Peritonitis Evisceration Positive DPL, FAST, or CT Violation of peritoneum
Options for Management n Hemodynamically stable penetrating injury Serial Observation Wound Exploration DPL CT scan +/- Contrast Laparoscopy Laparotomy Ultrasound/echo – cardiac box Pericardial window – cardiac box

Stab Wounds Shorr RM, Gottlieb MM, et al. Selective management of abdominal stab wounds: Importance of the physical examiantion. Arch Surg 1988, 123(9): 1141 -5. 330 patients over 12 months 154 (47%) acute abdomen, underwent immediate celiotomy Even of these, 31% negative 176 (53%) observed 3 (1. 7%) injuries required celiotomy (no adverse effects)

The Value of Serial Observation

Learning Points Case #4 Injury from stab wounds are different from GSW n Indications for early surgery n Consider diagnostic options n Value of serial exam n
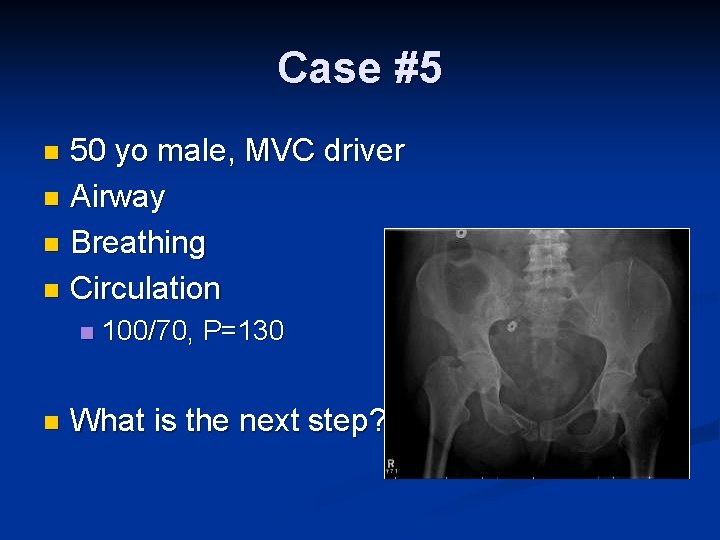
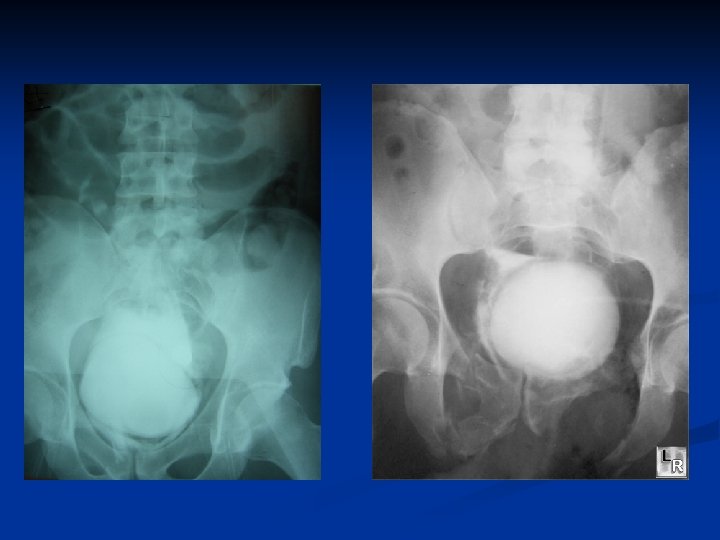
Case #5 50 yo male, MVC driver n Airway n Breathing n Circulation n 100/70, P=130 What is the next step?

Priorities ABC n Consider associated injuries with pelvic trauma n Blood vessels – arterial and venous n Bone n Bladder and urethral n Bowel n Baby (Uterus) n Other Body injuries n
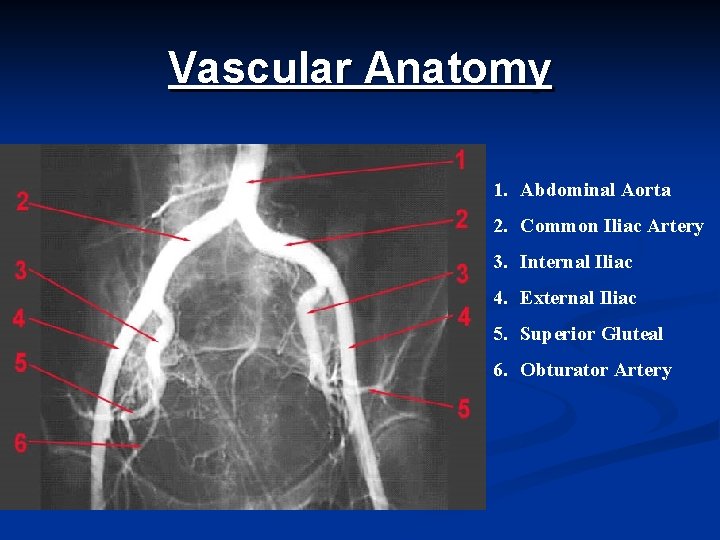
Vascular Anatomy 1. Abdominal Aorta 2. Common Iliac Artery 3. Internal Iliac 4. External Iliac 5. Superior Gluteal 6. Obturator Artery
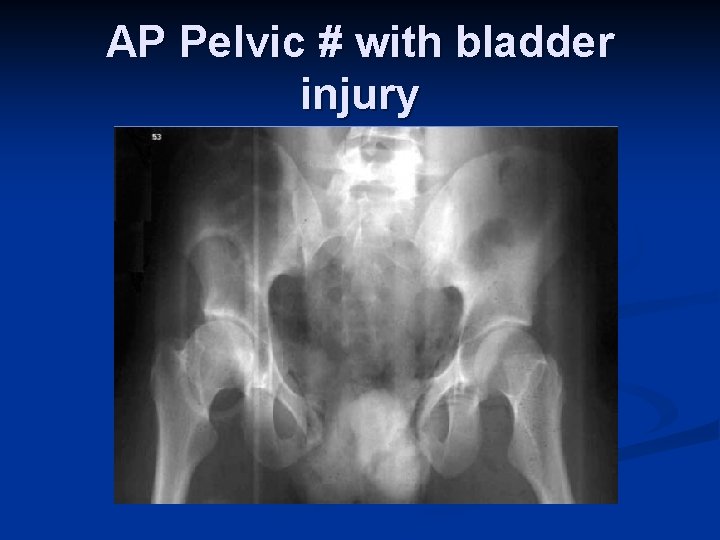
AP Pelvic # with bladder injury

The Pelvic Mantra…. Unstable Fractures Lead to Unstable Patients - stability should be tested by GENTLE manipulation - stability should only be performed ONCE Minimize further hemmorage !
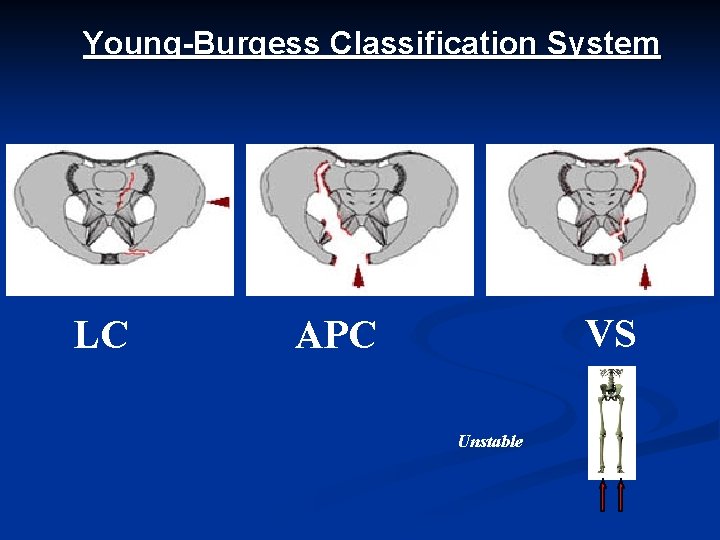
Young-Burgess Classification System LC VS APC Unstable

Decision Making n Hemodynamically Stable CT Scan + cystogram n If blush then observe vs. embolize n n Hemodynamically unstable, Pelvis unstable FAST or DPL to rule out intra-abdominal injury n Bedsheet wrap pelvis, Ex-fix, C-clamp n If intraperitoneal blood = laparotomy n If no intraperitoneal blood = Angiogram n
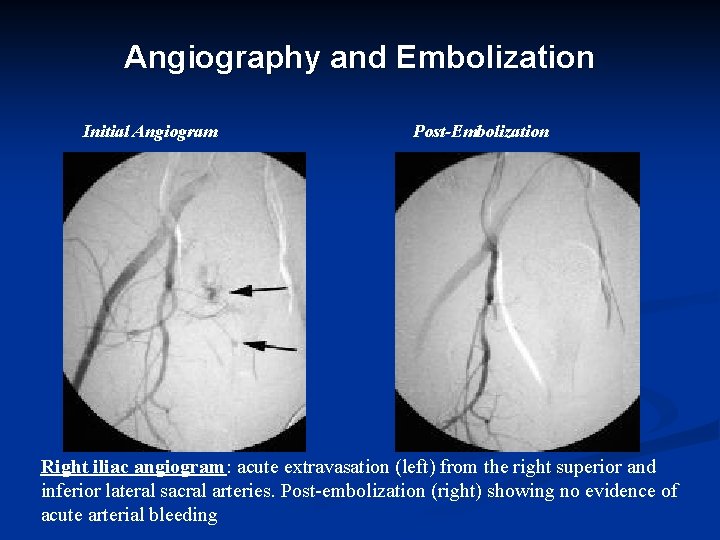
Angiography and Embolization Initial Angiogram Post-Embolization Right iliac angiogram: acute extravasation (left) from the right superior and inferior lateral sacral arteries. Post-embolization (right) showing no evidence of acute arterial bleeding

Learning Points Case #5 Unstable vs. Stable patients n Recognize pelvic fracture n Rule out bladder injuries n Angiogram and emobolization of arterial injuries n

Role of Interventional Radiology n Embolization Spleen n Liver n Pelvis n n Angioplasty + Stent n n Renal artery dissection Stent n Thoracic aortic injuries
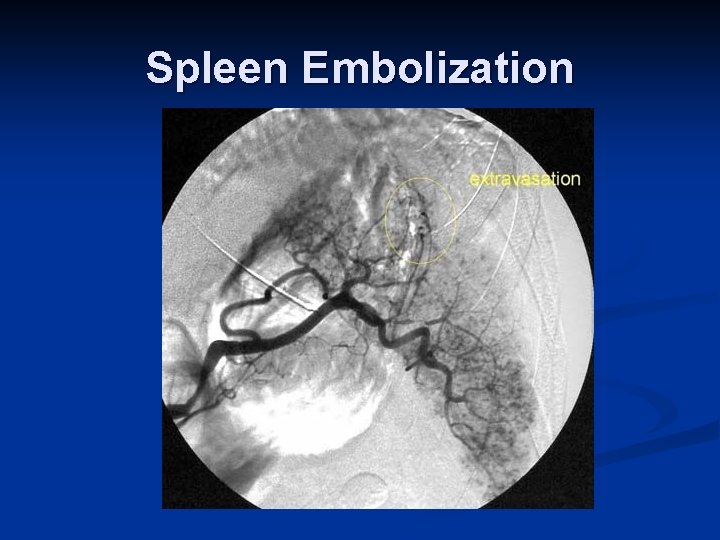
Spleen Embolization
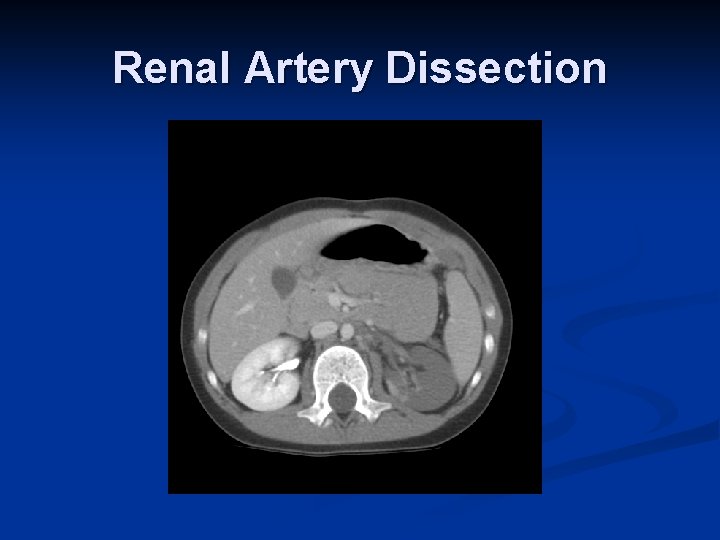
Renal Artery Dissection
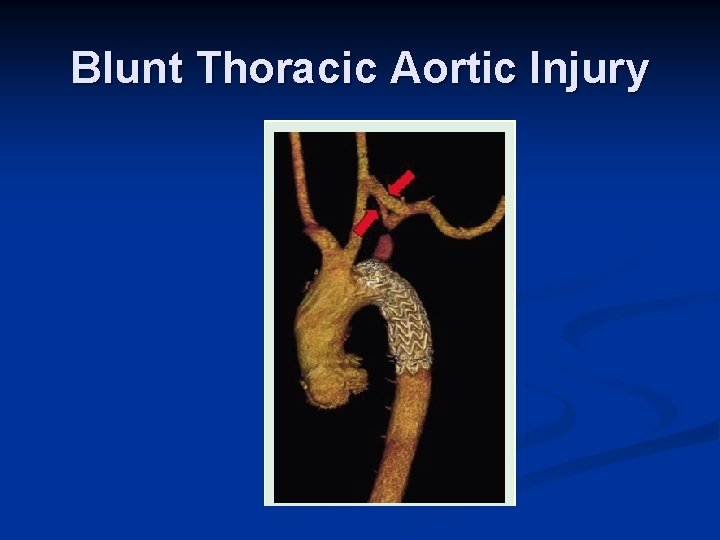
Blunt Thoracic Aortic Injury

Summary n n n Mechanism of injury – Blunt vs. Penetrating ABC Stability of trauma patients Select ppropriate diagnostic imaging Think about associated injuries Multi-modality n n n Clinical FAST CT Scan Interventional Radiology Surgical exploration

Questions
- Slides: 63