Primary Liver Cancer Hepatocellular Carcinoma and Cholangiocarinoma Patrick


























- Slides: 53

Primary Liver Cancer: Hepatocellular Carcinoma and Cholangiocarinoma Patrick M. Horne, MSN, ARNP, FNP-BC Assistant Director of Hepatology Clinical Research Division of Gastroenterology, Hepatology and Nutrition University of Florida Health

Disclosures • Financial relationships to disclose within the past 12 months: • Grant support with Bayer/Onyx

Objectives • Discuss the diagnosis and management of hepatocellular carcinoma (HCC) and cholangiocarinoma • Review current screening and staging of both HCC and cholangiocarinoma • Selection of the optimal, evidence-based surgical and nonsurgical treatment modalities • Review current treatment options

Background of HCC • World wide – 6 th most common cancer – 748, 271 new cases per year – 3 rd leading cause of cancer-related mortality – 695, 843 deaths per year • US incidence has tripled over the last three decades – Estimated new cases: >20, 000 new cases annually – Fastest Growing Death Rate in the US – Dismal 5 -year survival 10% • 80%-90% of HCC cases occur in cirrhotic livers • Leading cause of death in cirrhosis Globocan 2008. Mc. Glynn KA et al. Int J Cancer. 2001; 94: 290 -296; Mc. Glynn KA et al. Cancer Epidemiol Biomarkers Prev. 2006; 15: 1198 -1203; El-Serag HB. Gastroenterology. 2004; 127: S 27 -S 34; Altekruse SF et al. J Clin Oncol. 2009; 27: 1485 -1491

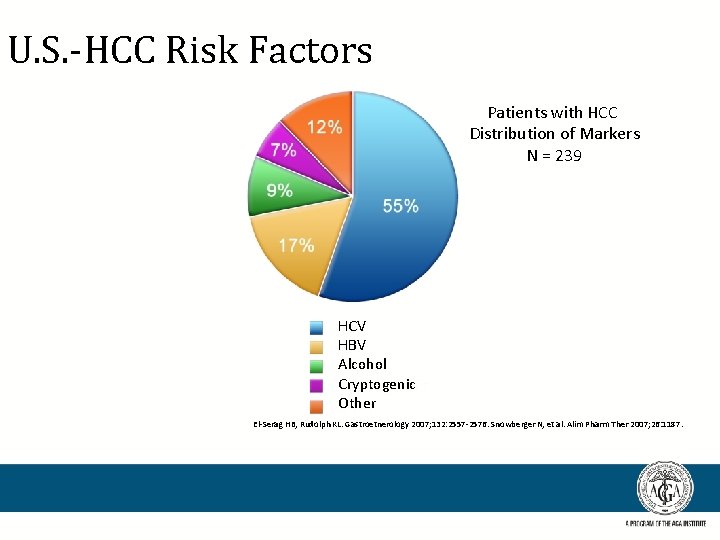
U. S. -HCC Risk Factors Patients with HCC Distribution of Markers N = 239 HCV HBV Alcohol Cryptogenic Other El-Serag HB, Rudolph KL. Gastroetnerology 2007; 132: 2557 -2576. Snowberger N, et al. Alim Pharm Ther 2007; 26: 1187.

Risk Factors for HCC Host Factors • Cirrhosis • HBV, HCV, NASH, Alcohol • Hemachromatosis, • α-1 antitrypsin deficiency • HBV • Male gender • Family history of HCC • Coinfection with HCV, HBV, or HIV • Older age Viral Factors • HBV DNA levels >2, 000 IU/m. L (10, 000 copies/m. L, REVEAL Study) • HBV genotype C* • Basal core promoter mutation • Presence of HBe. Ag • History of reversions from anti-HBe to HBe. Ag Likely Factors • Diabetes • Obesity AASLD practice guidelines. AASLD website. Available at: http: //www. aasld. org/practiceguidelines. Accessed 02/10/11; Keeffe. Clin Gastroenterol Hepatol. 2008; 6: 1315; Mahtab. Hepatobiliary Pancreat Dis Int. 2008; 7: 457; Lin. Hepatology. 2007; 46: 1034.

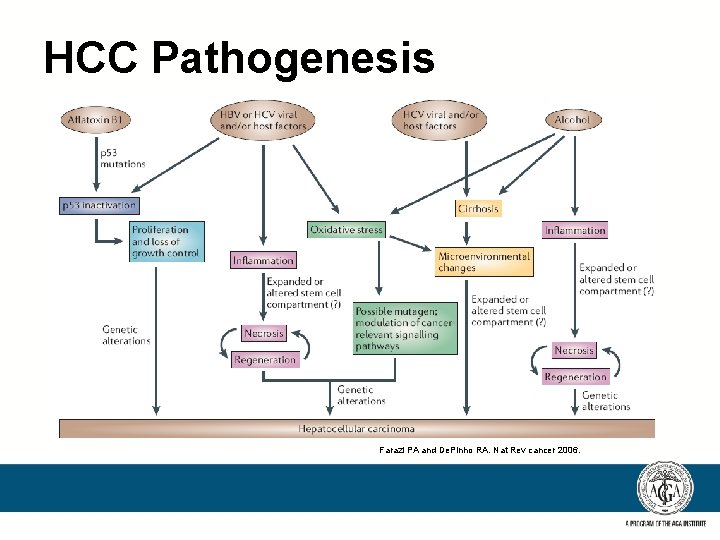
HCC Pathogenesis Farazi PA and De. Pinho RA. Nat Rev cancer 2006.

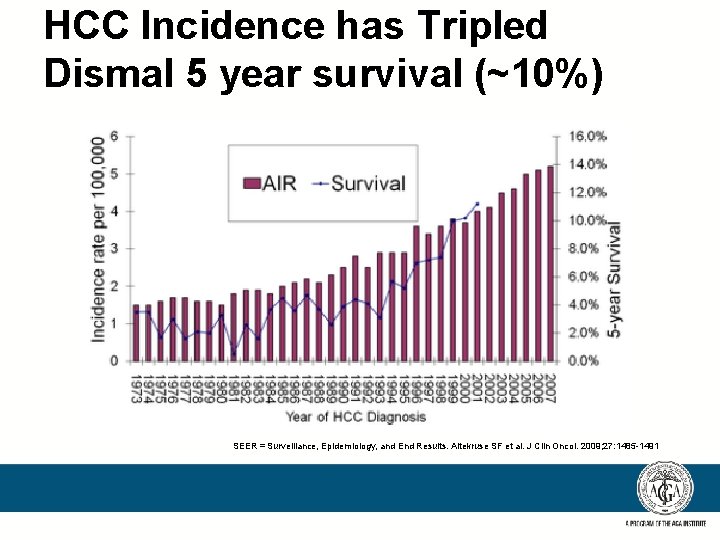
HCC Incidence has Tripled Dismal 5 year survival (~10%) SEER = Surveillance, Epidemiology, and End Results. Altekruse SF et al. J Clin Oncol. 2009; 27: 1485 -1491

Groups for Whom HCC Surveillance is Recommended AASLD Practice Guidelines • • Cirrhosis – Viral hepatitis – HCV, HBV – Non-alcoholic fatty liver/non-alcoholic steatohepatitis (NAFLD/NASH) – Alcohol and other Hepatitis B carriers – Asian males over 40 yrs – Asian females over 50 yrs – All cirrhotic hepatitis B carriers – Positive family history of HC – Non-cirrhotic HBV carriers with high HBV DNA levels or more severe current/past levels of inflammatory activity AASLD=American Association for the Study of Liver Diseases; HBV=hepatitis B virus. Practice guidelines page. AASLD website. Available at: http: //www. aasld. org/practiceguidelines.

Current Recommendation for Surveillance • AASLD practice guidelines – Ultrasound every 6 months • Goal – Detect early tumor and improve survival • AFP – Normal in 40% of patients with HCC – Inadequate sensitivity and specificity in the diagnostic range – normal in small HCC – Values >200 ng/m. L high PPV in cirrhotic patients with a mass El Serag. Gastroenterology. 2008; 134: 1752; Practice guidelines page. AASLD website. Available at: http: //www. aasld. org/practiceguidelines. Accessed 10/12/11; Sheu. Gastroenterology. 1985; 89: 259.

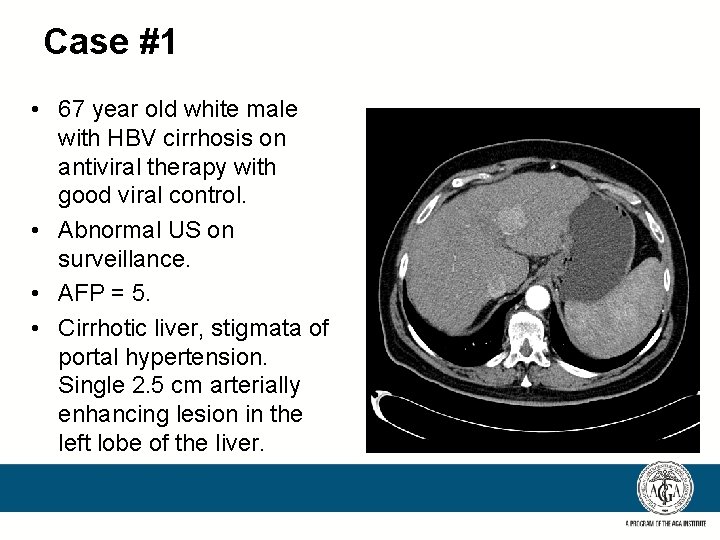
Case #1 • 67 year old white male with HBV cirrhosis on antiviral therapy with good viral control. • Abnormal US on surveillance. • AFP = 5. • Cirrhotic liver, stigmata of portal hypertension. Single 2. 5 cm arterially enhancing lesion in the left lobe of the liver.

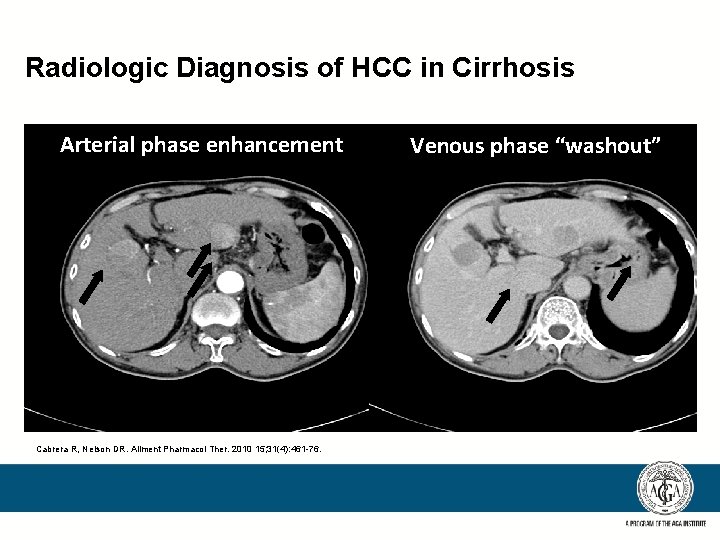
Diagnostic Algorithm for HCC in Cirrhosis New Liver Nodule on US <1 cm >1 cm Repeat US at 3 months Growing/changing character 4 -phase MDCT / dynamic contrast enhanced MRI Arterial hypervascularity AND venous or delayed phase washout Stable Investigate according to size Adapted from Bruix J, Sherman M. Hepatology July, 2010. Available at http: //www. aasld. org/practiceguidelines/Pages /New. Updated. Guidelines. aspx. Accessed 08/03/10. Yes Other contrast enhanced study (CT or MRI) No HCC Arterial hypervascularity AND venous or delayed phase washout Biopsy Yes No

Radiologic Diagnosis of HCC in Cirrhosis Arterial phase enhancement Cabrera R, Nelson DR. Aliment Pharmacol Ther. 2010 15; 31(4): 461 -76. Venous phase “washout”

Radiologic Diagnosis of HCC

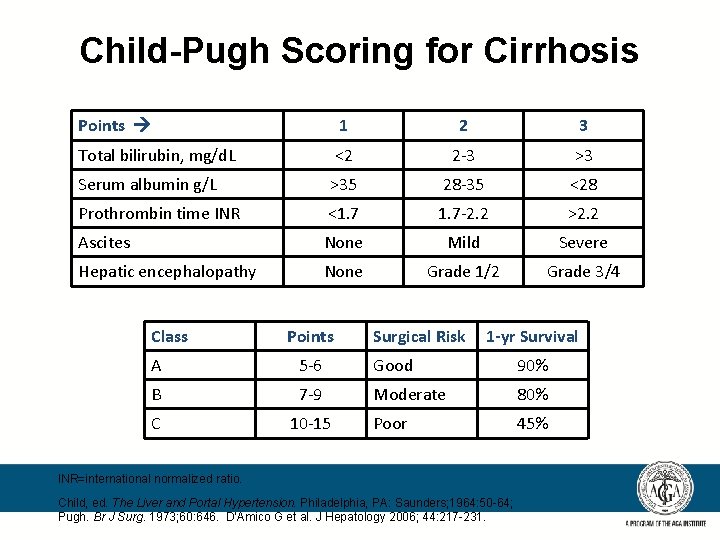
Child-Pugh Scoring for Cirrhosis Points 1 2 3 Total bilirubin, mg/d. L <2 2 -3 >3 Serum albumin g/L >35 28 -35 <28 Prothrombin time INR <1. 7 -2. 2 >2. 2 Ascites None Mild Severe Hepatic encephalopathy None Grade 1/2 Grade 3/4 Class Points Surgical Risk 1 -yr Survival A 5 -6 Good 90% B 7 -9 Moderate 80% C 10 -15 Poor 45% INR=international normalized ratio. Child, ed. The Liver and Portal Hypertension. Philadelphia, PA: Saunders; 1964: 50 -64; Pugh. Br J Surg. 1973; 60: 646. D’Amico G et al. J Hepatology 2006; 44: 217 -231.

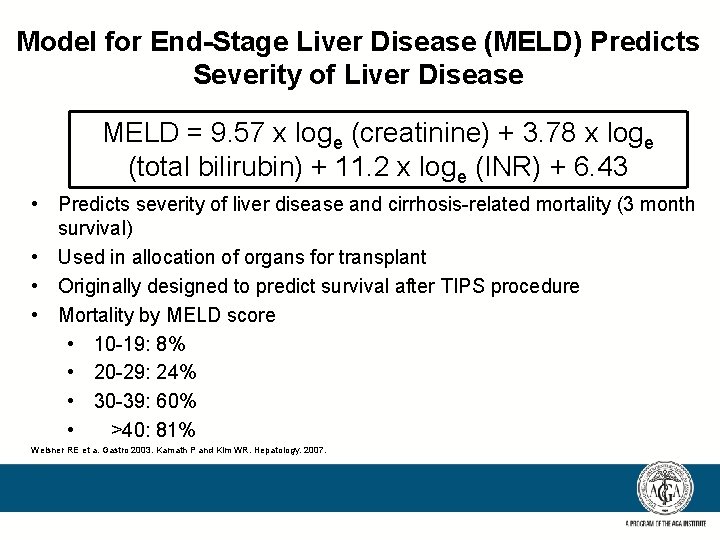
Model for End-Stage Liver Disease (MELD) Predicts Severity of Liver Disease MELD = 9. 57 x loge (creatinine) + 3. 78 x loge (total bilirubin) + 11. 2 x loge (INR) + 6. 43 • Predicts severity of liver disease and cirrhosis-related mortality (3 month survival) • Used in allocation of organs for transplant • Originally designed to predict survival after TIPS procedure • Mortality by MELD score • 10 -19: 8% • 20 -29: 24% • 30 -39: 60% • >40: 81% Weisner RE et a. Gastro 2003. Kamath P and Kim WR. Hepatology. 2007.

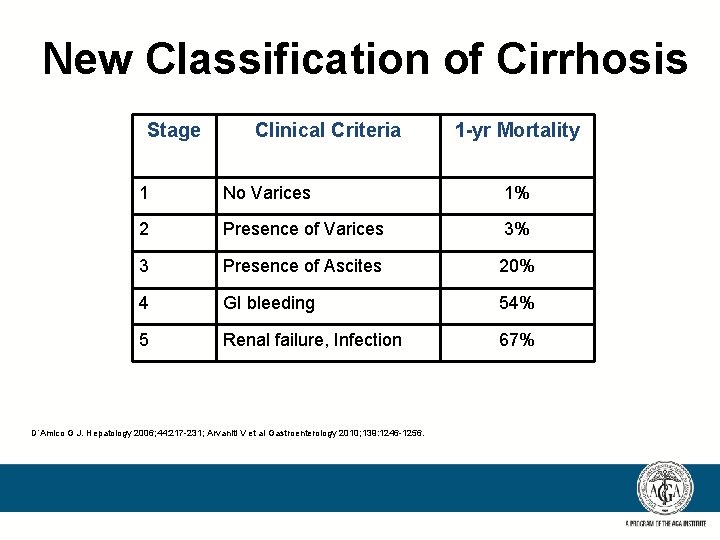
New Classification of Cirrhosis Stage Clinical Criteria 1 -yr Mortality 1 No Varices 1% 2 Presence of Varices 3% 3 Presence of Ascites 20% 4 GI bleeding 54% 5 Renal failure, Infection 67% D’Amico G J. Hepatology 2006; 44: 217 -231; Arvaniti V et al Gastroenterology 2010; 139: 1246 -1256.

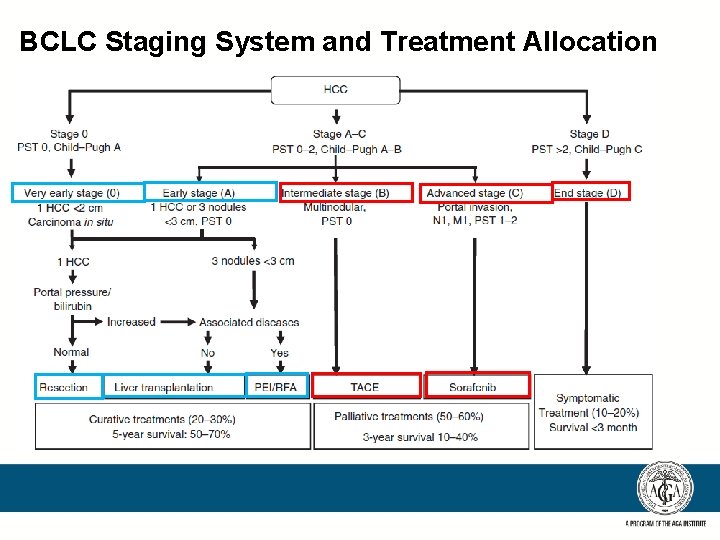
BCLC Staging System and Treatment Allocation

What is the best treatment option for this patient? Surgery: C Liver Transplantation U Liver Resection R A T I V E Ablation: Percutaneous ethanol injection (PEI) Radiofrequency (RFA) P a l l i a t i v e Transarterial: Chemoembolization 90 Y microspheres Systemic Therapies: Sorafenib Clinical Trials

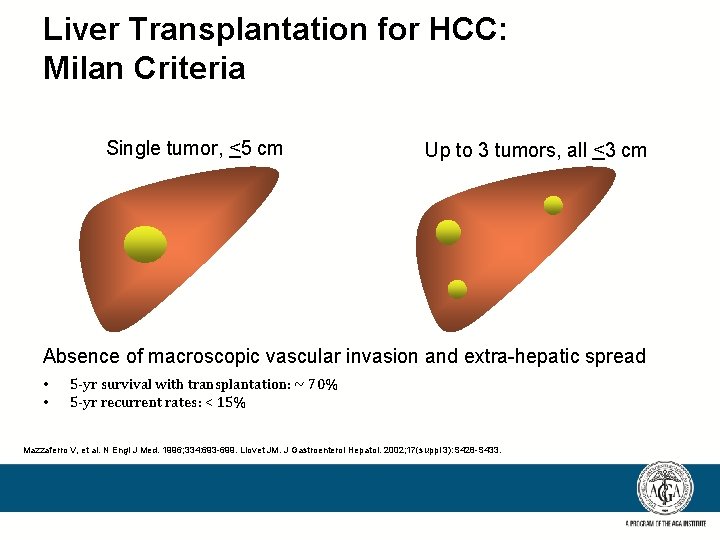
Liver Transplantation for HCC: Milan Criteria Single tumor, <5 cm Up to 3 tumors, all <3 cm Absence of macroscopic vascular invasion and extra-hepatic spread • • 5 -yr survival with transplantation: ~ 70% 5 -yr recurrent rates: < 15% Mazzaferro V, et al. N Engl J Med. 1996; 334: 693 -699. Llovet JM. J Gastroenterol Hepatol. 2002; 17(suppl 3): S 428 -S 433.

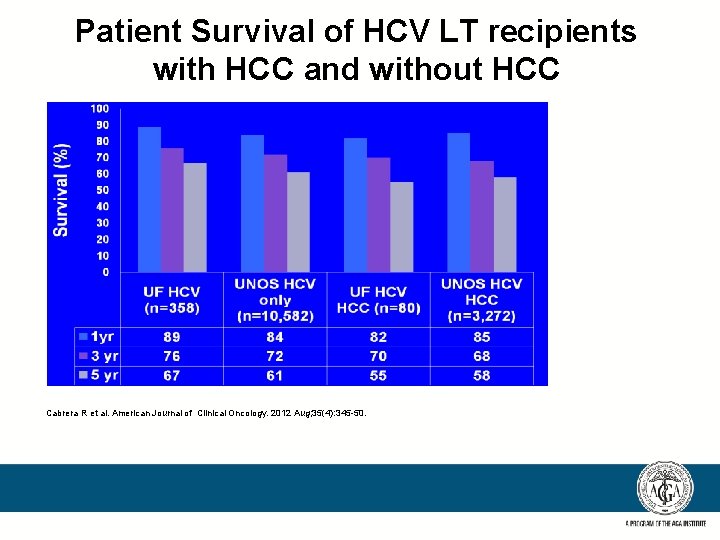
Patient Survival of HCV LT recipients with HCC and without HCC Cabrera R et al. American Journal of Clinical Oncology. 2012 Aug; 35(4): 345 -50.

Candidates for RFA and PEI • Includes individuals who are not candidates for surgery – resection or transplantation • Radiofrequency ablation generally preferred over percutaneous ethanol injection – Necrotic effect more predictable across tumor sizes – Meta-analyses (4 RCTs) suggest better local control and survival benefit with RFA vs PEI Bruix J, et al. AASLD HCC Guidelines. July 2010.

New Trends in Local Ablation • Microwave ablation • Irreversible electroporation • Intravenous heat-sensitive liposomal doxorubicin in combination with RFA • Combination chemoembolization and RFA

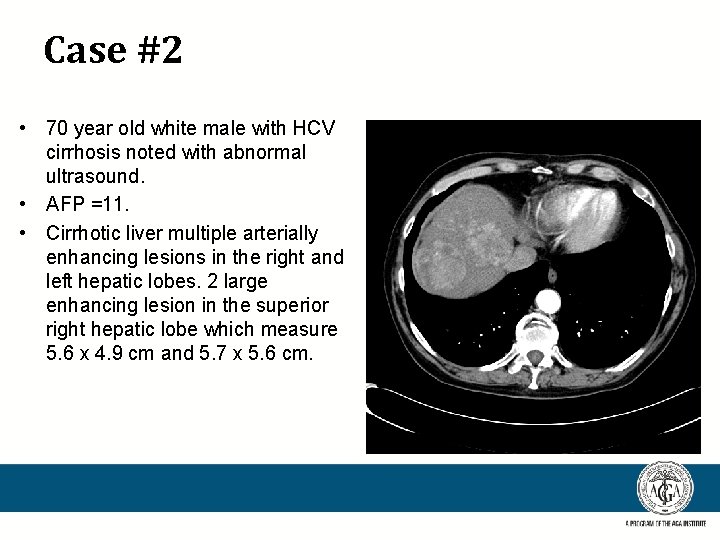
Case #2 • 70 year old white male with HCV cirrhosis noted with abnormal ultrasound. • AFP =11. • Cirrhotic liver multiple arterially enhancing lesions in the right and left hepatic lobes. 2 large enhancing lesion in the superior right hepatic lobe which measure 5. 6 x 4. 9 cm and 5. 7 x 5. 6 cm.

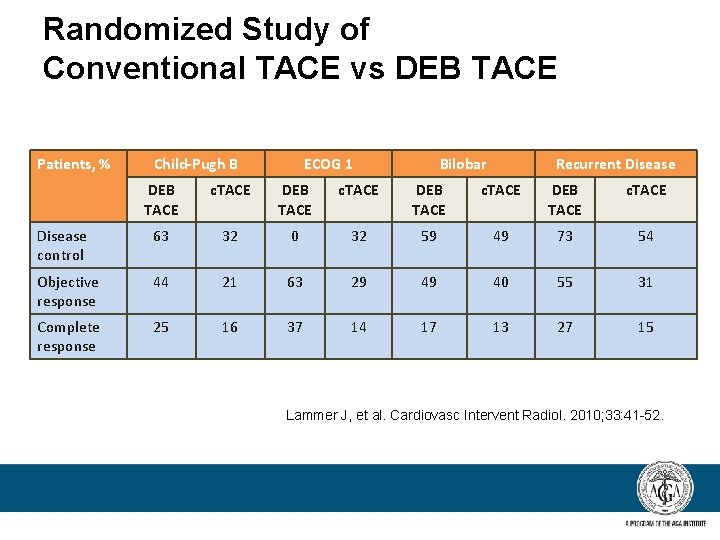
Randomized Study of Conventional TACE vs DEB TACE Patients, % Child-Pugh B ECOG 1 Bilobar Recurrent Disease DEB TACE c. TACE Disease control 63 32 0 32 59 49 73 54 Objective response 44 21 63 29 49 40 55 31 Complete response 25 16 37 14 17 13 27 15 Lammer J, et al. Cardiovasc Intervent Radiol. 2010; 33: 41 -52.

Contraindications to TACE • Extrahepatic tumor spread • Lack of portal blood flow – Portal vein thrombosis, portosystemic anastomoses or hepatofugal flow • Advanced liver disease (Child-Pugh Class B or C) • Clinical symptoms of end-stage cancer

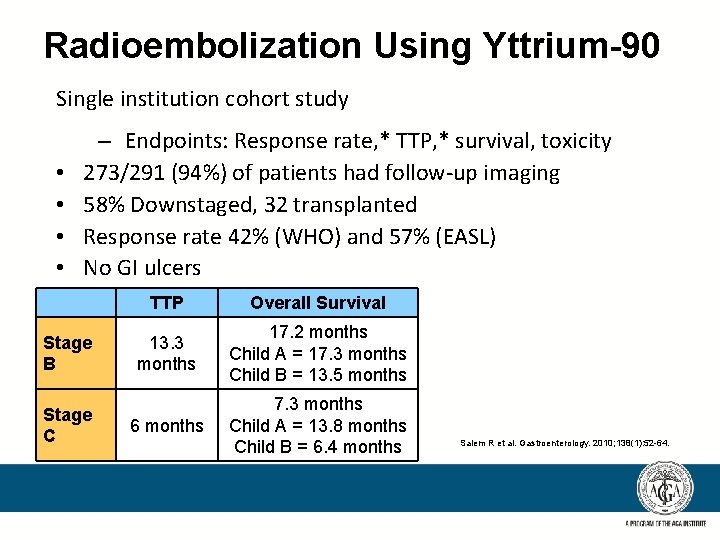
Radioembolization Using Yttrium-90 Single institution cohort study • • – Endpoints: Response rate, * TTP, * survival, toxicity 273/291 (94%) of patients had follow-up imaging 58% Downstaged, 32 transplanted Response rate 42% (WHO) and 57% (EASL) No GI ulcers Stage B Stage C TTP Overall Survival 13. 3 months 17. 2 months Child A = 17. 3 months Child B = 13. 5 months 6 months 7. 3 months Child A = 13. 8 months Child B = 6. 4 months Salem R et al. Gastroenterology. 2010; 138(1): 52 -64.

New Trends in Loco-Regional Therapy • • Doxorubicin-eluting beads Quadraspheres Combination TACE or Y 90 with sorafenib SBRT and Proton beam therapy

Case #3 • 47 year old white male with HCV cirrhosis undergoes a screening abdominal ultrasound. • Ultrasound reveals multiple liver masses. • Innumerable bilobar arterial enhancing lesions and vascular invasion. AFP >50, 000. consistent with diffuse HCC

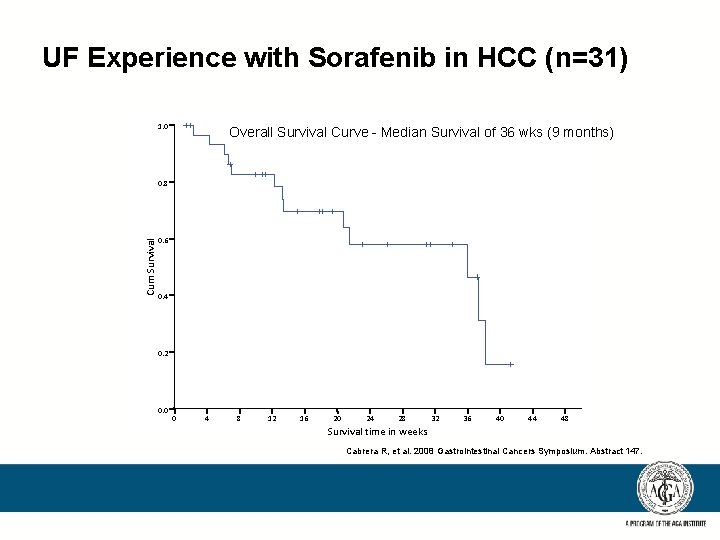
UF Experience with Sorafenib in HCC (n=31) 1. 0 Overall Survival Curve - Median Survival of 36 wks (9 months) Cum Survival 0. 8 0. 6 0. 4 0. 2 0. 0 0 4 8 12 16 20 24 28 32 36 40 44 48 Survival time in weeks Cabrera R, et al. 2008 Gastrointestinal Cancers Symposium. Abstract 147.

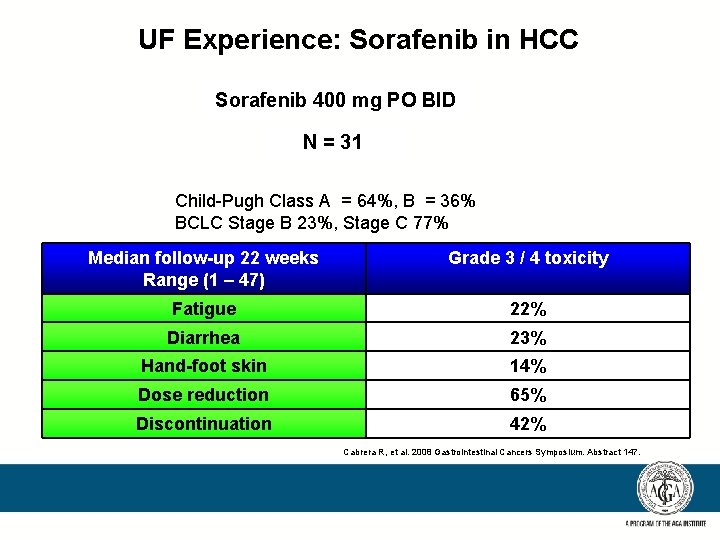
UF Experience: Sorafenib in HCC Sorafenib 400 mg PO BID N = 31 Child-Pugh Class A = 64%, B = 36% BCLC Stage B 23%, Stage C 77% Median follow-up 22 weeks Range (1 – 47) Grade 3 / 4 toxicity Fatigue 22% Diarrhea 23% Hand-foot skin 14% Dose reduction 65% Discontinuation 42% Cabrera R, et al. 2008 Gastrointestinal Cancers Symposium. Abstract 147.

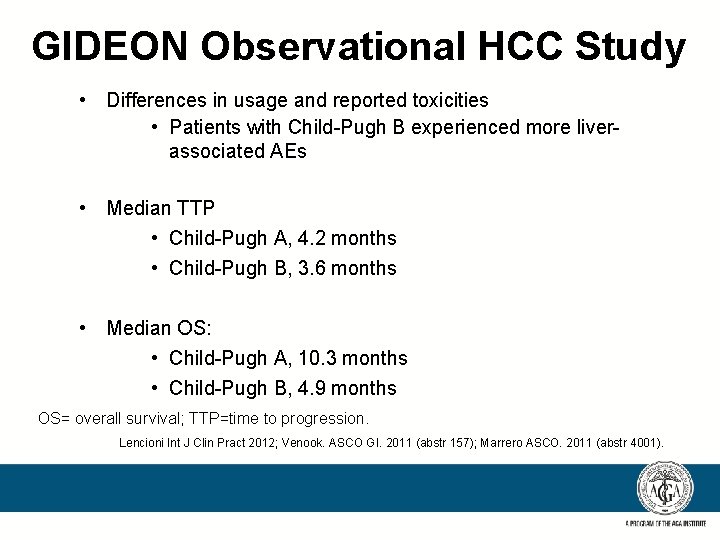
GIDEON Observational HCC Study • Differences in usage and reported toxicities • Patients with Child-Pugh B experienced more liverassociated AEs • Median TTP • Child-Pugh A, 4. 2 months • Child-Pugh B, 3. 6 months • Median OS: • Child-Pugh A, 10. 3 months • Child-Pugh B, 4. 9 months OS= overall survival; TTP=time to progression. Lencioni Int J Clin Pract 2012; Venook. ASCO GI. 2011 (abstr 157); Marrero ASCO. 2011 (abstr 4001).

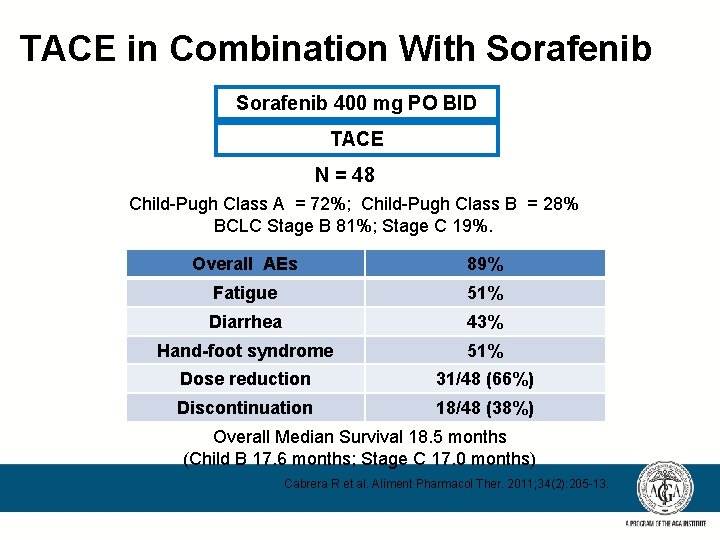
TACE in Combination With Sorafenib 400 mg PO BID TACE N = 48 Child-Pugh Class A = 72%; Child-Pugh Class B = 28% BCLC Stage B 81%; Stage C 19%. Overall AEs 89% Fatigue 51% Diarrhea 43% Hand-foot syndrome 51% Dose reduction 31/48 (66%) Discontinuation 18/48 (38%) Overall Median Survival 18. 5 months (Child B 17. 6 months; Stage C 17. 0 months) Cabrera R et al. Aliment Pharmacol Ther. 2011; 34(2): 205 -13.

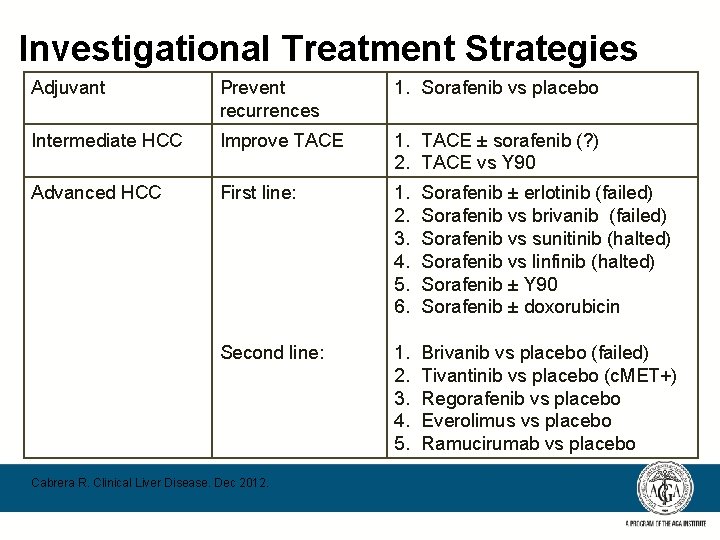
Investigational Treatment Strategies Adjuvant Prevent recurrences 1. Sorafenib vs placebo Intermediate HCC Improve TACE 1. TACE ± sorafenib (? ) 2. TACE vs Y 90 Advanced HCC First line: 1. 2. 3. 4. 5. 6. Sorafenib ± erlotinib (failed) Sorafenib vs brivanib (failed) Sorafenib vs sunitinib (halted) Sorafenib vs linfinib (halted) Sorafenib ± Y 90 Sorafenib ± doxorubicin Second line: 1. 2. 3. 4. 5. Brivanib vs placebo (failed) Tivantinib vs placebo (c. MET+) Regorafenib vs placebo Everolimus vs placebo Ramucirumab vs placebo Cabrera R. Clinical Liver Disease. Dec 2012.

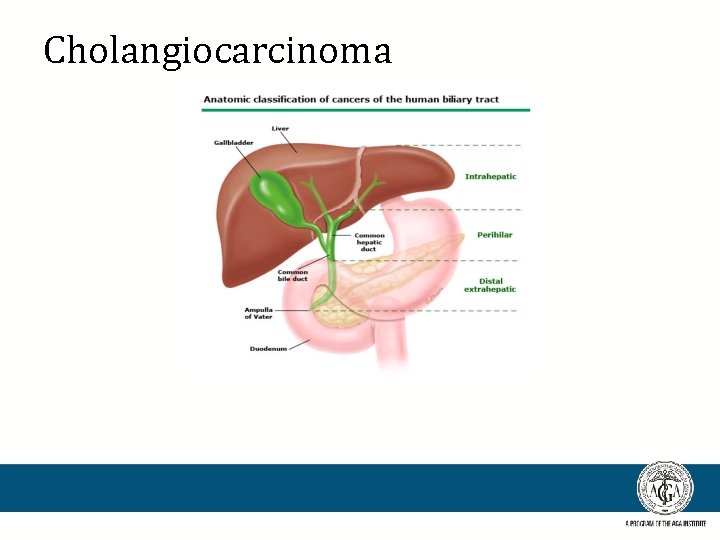
Cholangiocarcinoma (CCA) • Background: – Arises from the epithelial cells of the bile ducts. – Rare in the United States.

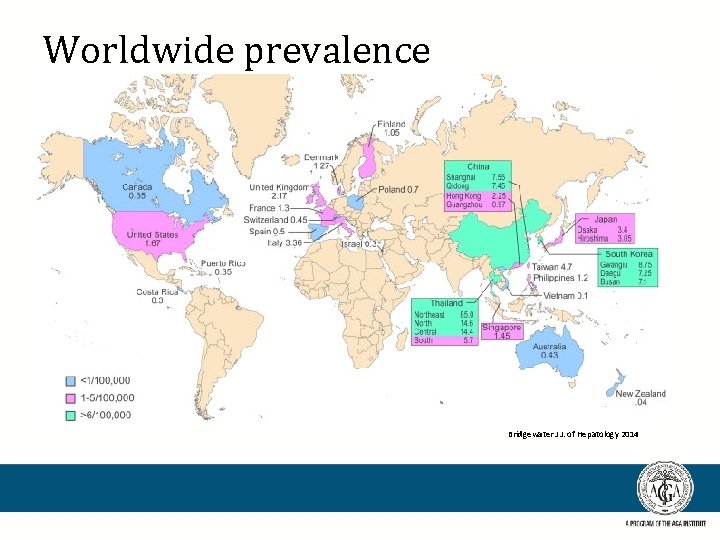
Worldwide prevalence Bridgewater J J. of Hepatology 2014

Cholangiocarcinoma

Risk Factors for Cholangiocarcinoma • Primary sclerosing cholangitis (PSC) – Almost 30% of cholangiocarcinoma case are in the setting of PSC. – Annual incidence is between 0. 6 -1. 5%. – Lifetime risk is 10 -15%. • Fibropolycystic liver disease • Parasitic infection • Viral hepatitis – Though much lower than risk for HCC Burka K. Am J Gastroenoterology 2004

Cumulative incidence of Incidence of Cholangiocarcinoma Years since PSC diagnosis Courtesy of Dr. Keith Linder, MD. , ASU

AASLD guidelines • Risk factors for developing CCA – Elevated serum bilirubin – Variceal bleeding – Proctocolectomy – Chronic UC with colorectal cancer or dysplasia. Practice guidelines page. AASLD website. Available at: http: //www. aasld. org/practiceguidelines.

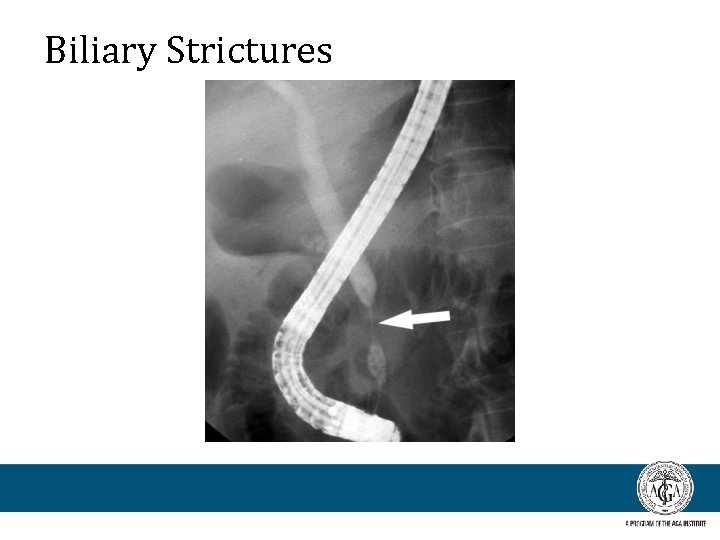
Biliary strictures • Signs and symptoms: – Jaundice, pruritis, abdominal pain, fever, weight loss – Cholangitis is unusual. – Tumor markers? • CEA • CA 19 -9

Biliary Strictures

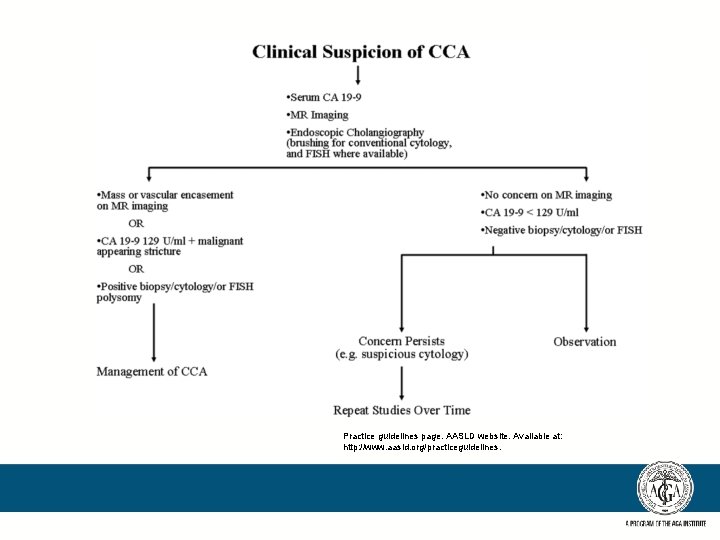
Imaging diagnosis of CCA • Challenging to say the least – Ultrasound – CT scan – MRI with MRCP – ERCP with brushing – No clear guidelines as to best modality to use or frequency

Practice guidelines page. AASLD website. Available at: http: //www. aasld. org/practiceguidelines.

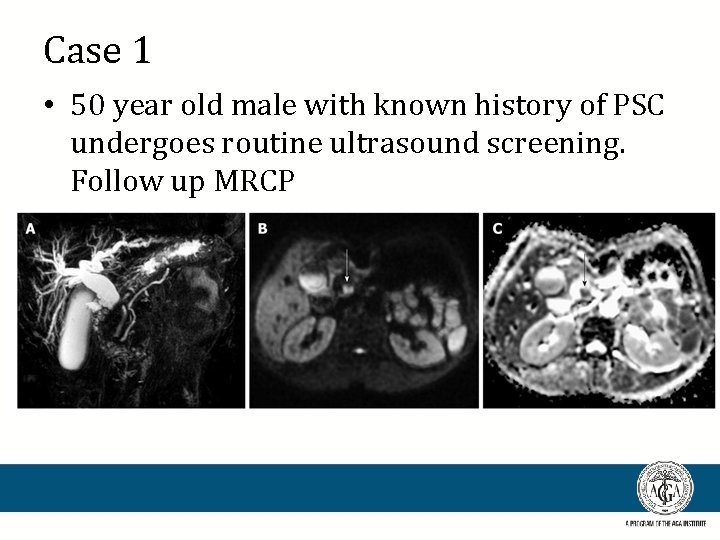
Case 1 • 50 year old male with known history of PSC undergoes routine ultrasound screening. Follow up MRCP

Treatment options • Criteria for surgical resection: – Absence of retropancreatic and paraceliac nodal metatases or distant liver metastases – Absence of invasion of portal vein or main hepatic artery – Absence of extrahepatic adjacent organ invasion – Absence of disseminated disease • Ultimately, candidacy for resection is determined at surgery! Tsao JI et al Ann Surg. 2000 Su CH et al Ann. Surg. 1996

Distal Extrahepatic cholangiocarcinoma • Considered having the highest rate of resection. • Role of adjunct therapy post resection, commonly recommended but lack of data determining if true benefit.

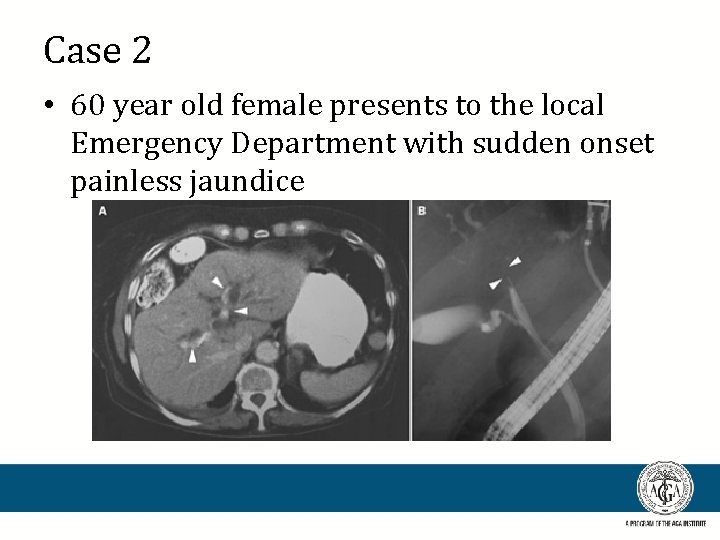
Case 2 • 60 year old female presents to the local Emergency Department with sudden onset painless jaundice

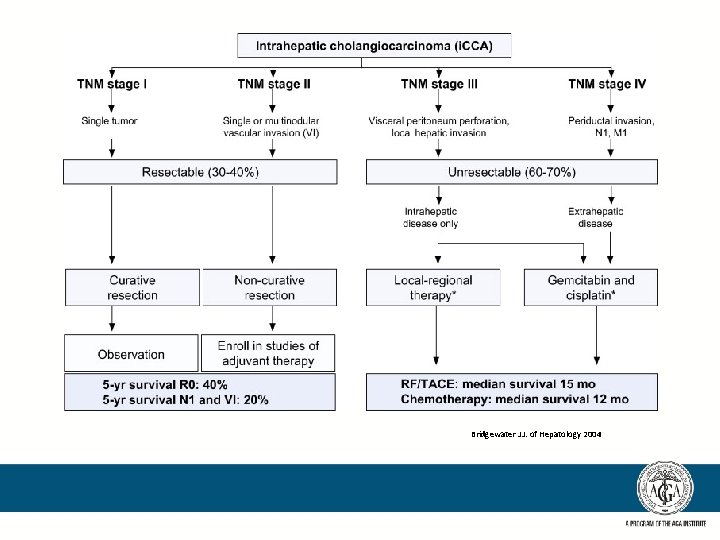
Bridgewater J J. of Hepatology 2004

Role of Radiotherapy with or without chemoradiotherapy • Approaches include external beam irradiation (ERBT) alone or… • In combination with chemoradiotherapy – Most commonly used: • • 5 -FU Gemcitabine Cisplatin oxaliplatin

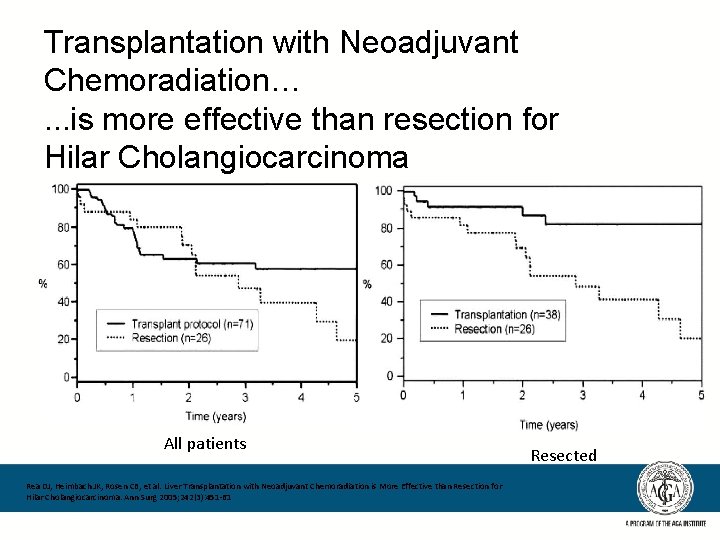
Transplantation with Neoadjuvant Chemoradiation…. . . is more effective than resection for Hilar Cholangiocarcinoma All patients Rea DJ, Heimbach JK, Rosen CB, et al. Liver Transplantation with Neoadjuvant Chemoradiation is More Effective than Resection for Hilar Cholangiocarcinoma. Ann Surg 2005; 242(3): 451 -61 Resected

Summary • HCC has good treatment options, including liver transplantation with diagnosed early. • Clear screening guidelines – US every 6 months – Debate ongoing about role of AFP • Cholangiocarcinoma more difficult and outcomes typically poor • Location of cancer best determination of therapy options and prognosis.

Thank you