Primary Hyperparathyroidism Why Work it Up Rebecca S

Primary Hyperparathyroidism: Why Work it Up? Rebecca S. Sippel, M. D. Chief of Endocrine Surgery Associate Professor of Surgery Endocrine Surgery Fellowship Director

Outline 1. Diagnosis 2. Indications for Surgery 3. Operative management
Primary Hyperparathyroidism Background • 100, 000 new cases/year in US • 0. 5 -1% of general population • More common in elderly (up to 2%) • Females 2: 1 ratio

Primary Hyperparathyroidism Clinical Presentation 10% of patients are “Symptomatic” • Kidney stones and fractures Remainder of patients are labeled as “asymptomatic”

“Asymptomatic? ”

Symptoms and Parathyroid Disease “Asymptomatic” Hyperparathyroidism RARELY exists >95% of patients who are labeled as “asymptomatic” have significant symptoms that are likely related to their hyperparathyroidism
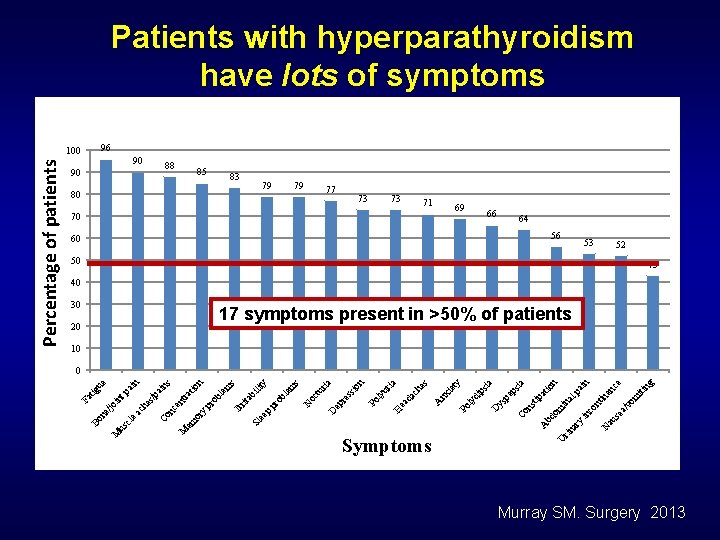
ng iti 53 om ce in pa en in nt /v se a co in al 56 N au y in io n 60 ar rin om at tip ns ps ia 66 bd A Co pe ys D 69 U Symptoms di ps ia 71 ly ty ie 70 Po nx es ia 73 A ch da ea ur 73 H ly n 77 Po ria ss io re ep 79 D tu oc s 79 N m le y 80 ob 83 pr bi lit 20 ee p s n m le ob 30 ita pr tio 85 Irr y tra s 88 Sl or em ai n n ai ue 90 en es /p tp in tig 90 M nc Co ea ch cl us /jo ne Fa 100 M Bo Percentage of patients Patients with hyperparathyroidism have lots of symptoms 96 64 52 50 43 40 17 symptoms present in >50% of patients 10 0 Murray SM. Surgery 2013

Why are we not recognizing the symptoms sooner? 1. Symptoms are non-specific and difficult to quantify 2. We write off the symptoms for other reasons “Primary Hyperparathyroidism is like premature aging. The symptoms are what you expect to happen with older age – it just happens sooner than you think it should. ” Orlo Clark, M. D.

What causes the symptoms? • ? excess calcium or the excess parathyroid hormone or the combination • Symptoms of hyperparathyroidism DO NOT correlate with the labs Higher labs ≠ More symptoms • Some of the most symptomatic patients have very mild lab abnormalities

59 yo female comes in for a routine evaluation, you check a lab panel and her calcium returns 10. 6 mg/d. L What is your Differential Diagnosis of Hypercalcemia? 1. 2. 3. 4. 5. 6. Primary hyperparathyroidism Account for Malignancy majority of cases Vitamin D intoxication Chronic granulomatous disease Medication related (Thiazides, lithium, Vit A) Other rare: hyperthyroidism, immobilization, milk-alkali syndrome, adrenal insufficiency, acromegaly
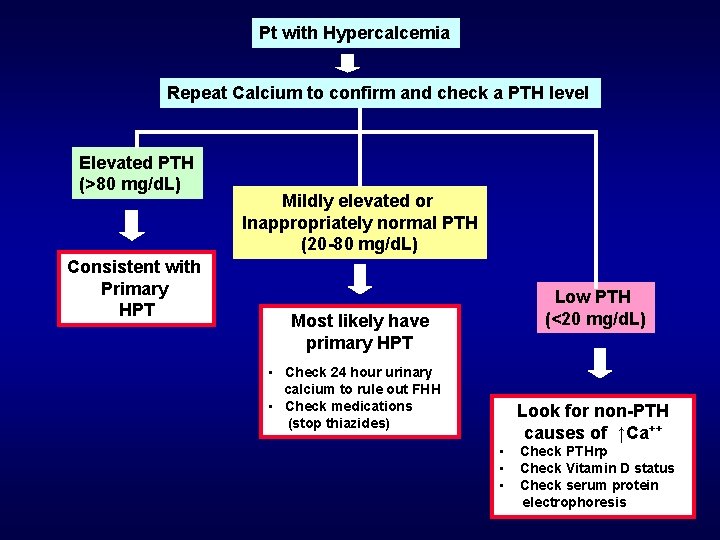
Pt with Hypercalcemia Repeat Calcium to confirm and check a PTH level Elevated PTH (>80 mg/d. L) Consistent with Primary HPT Mildly elevated or Inappropriately normal PTH (20 -80 mg/d. L) Low PTH (<20 mg/d. L) Most likely have primary HPT • Check 24 hour urinary calcium to rule out FHH • Check medications (stop thiazides) Look for non-PTH causes of ↑Ca++ • • • Check PTHrp Check Vitamin D status Check serum protein electrophoresis

65 yo female comes in for a routine evaluation, her DEXA scan shows osteoporosis. You check labs and the calcium is 9. 9 mg/d. L and the PTH is 110. Does she have Primary Hyperparathyroidism? Possibly. • Concurrent Primary HPTH and Vit D deficiency • Secondary cause of elevated PTH (renal failure, malabsorption, vitamin D deficiency, renal calcium loss, bisphonates)
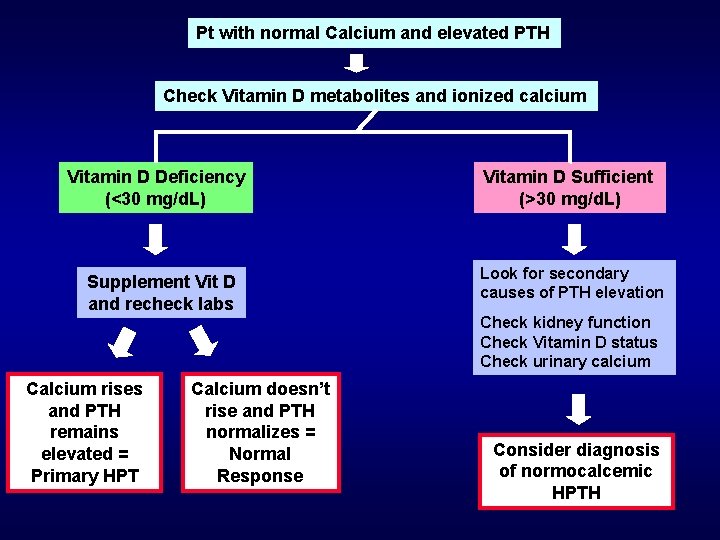
Pt with normal Calcium and elevated PTH Check Vitamin D metabolites and ionized calcium Vitamin D Deficiency (<30 mg/d. L) Supplement Vit D and recheck labs Vitamin D Sufficient (>30 mg/d. L) Look for secondary causes of PTH elevation Check kidney function Check Vitamin D status Check urinary calcium Calcium rises and PTH remains elevated = Primary HPT Calcium doesn’t rise and PTH normalizes = Normal Response Consider diagnosis of normocalcemic HPTH

NIH Consensus Guidelines 2014: Indications for Parathyroidectomy 1. 2. 3. 4. 5. 6. Serum calcium >1 mg/dl above upon limit of normal (>11. 2 -11. 5 mg/d. L) tive h ec e wit j b Presence of Kidney Stones u s os e h r t o d GFR <60 ml/min m n a ith nts, w Bone density > 2. 5 SDsnbelow mass (T score) at any ts apeak ie bone e t s e ati rly p disea site or fragility fracture p e e r r d l e o e d n Age under il Ig 50 ms, m pto Adequatem follow-up not possible or desired y s J Clin Endocrinol Metab. 2014; 99(10)

But I know that patients who don’t meet these guidelines still benefit from surgery! • • • Symptoms Improve Patients “Feel better” Bone Density Improves Lower rates of Fractures Lower risk of Heart Attack Patients Live Longer

Position Statement from US Endocrinology and Endocrine Surgery Organizations “Operative management should be considered and recommended for all asymptomatic patients with primary hyperparathyroidism who have a reasonable life expectancy and suitable operative risk factors. Consultation with an experienced endocrinologist and surgeon can help clarify the patient’s risk/benefit ratio. ” Endocrine Practice 2005 11(1): 49 -54

Symptomatic Improvement after Parathyroidectomy
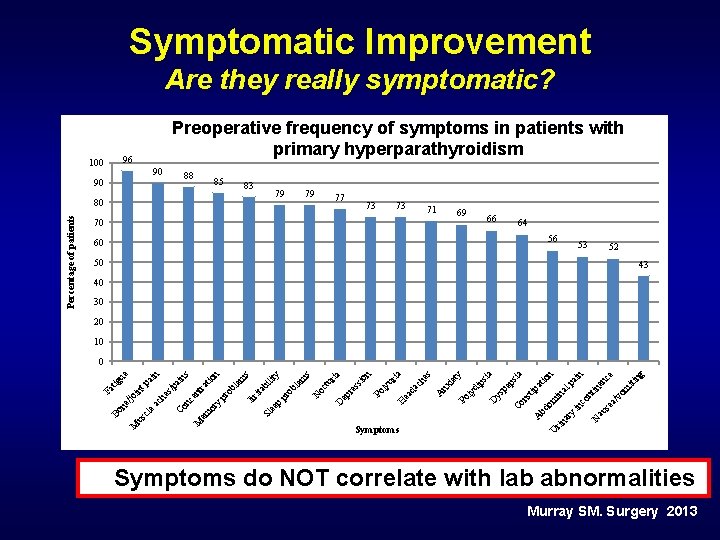
Symptomatic Improvement Are they really symptomatic? Preoperative frequency of symptoms in patients with primary hyperparathyroidism 96 100 90 88 90 85 83 79 79 77 73 73 71 69 70 66 64 56 60 53 52 50 43 40 30 20 10 ng om N au se a /v en in in y ar U rin iti ce n ai co in om bd A Symptoms nt at tip ns Co al p io n ia ps ia ys pe D di ps ty ly ie Po nx A ea da ly ch es ia ur n Po H D ep re ss io tu oc N le m ria s y ob Sl ee p pr bi lit s ita le ob pr y or em Irr tio tra en Co m n s ai n es /p ea ch nc M M us cl ne /jo in Fa tp tig ai ue n 0 Bo Percentage of patients 80 • Symptoms do NOT correlate with lab abnormalities Murray SM. Surgery 2013
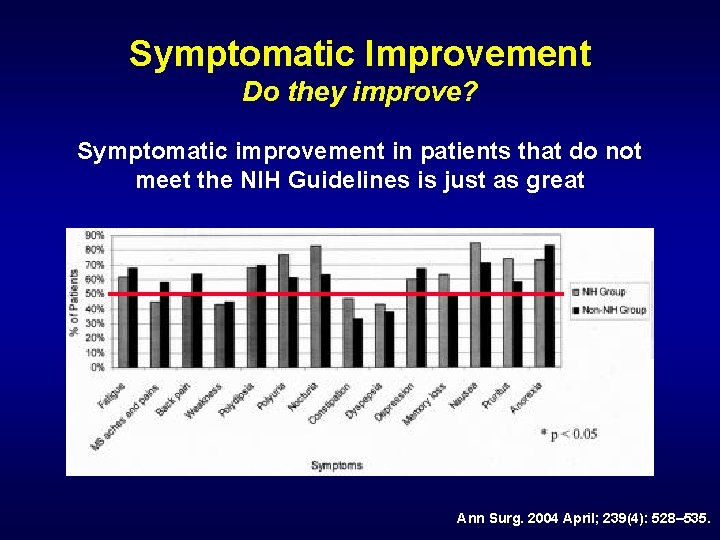
Symptomatic Improvement Do they improve? Symptomatic improvement in patients that do not meet the NIH Guidelines is just as great Ann Surg. 2004 April; 239(4): 528– 535.
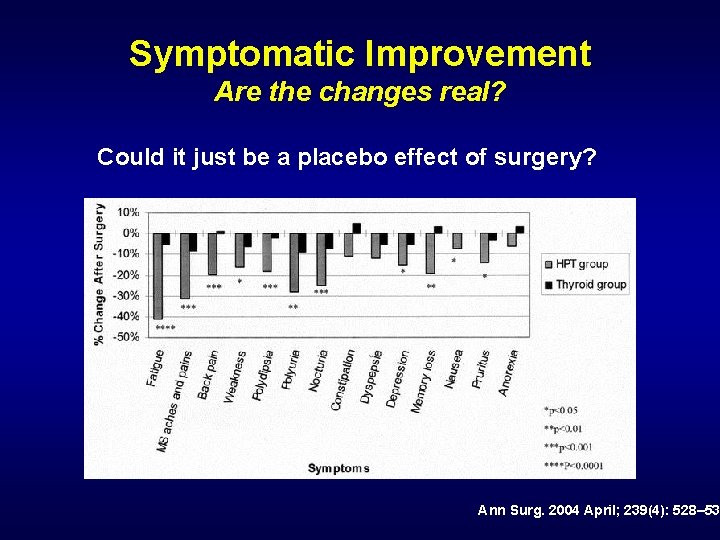
Symptomatic Improvement Are the changes real? Could it just be a placebo effect of surgery? Ann Surg. 2004 April; 239(4): 528– 53

Symptomatic Improvement Heartburn Improves • GERD health-related quality of life (GERD-HROL) • Validated questionnaire – Includes 10 items, Likert scale 0 -5 – Total scores range from 0 -45, with a lower score indicating fewer/less severe symptoms • Overall score improvement – 13. 9± 1. 4 vs. 5. 0± 1. 0 <0. 0001 Reiher, AE et al. Surgery. 2012 Dec.
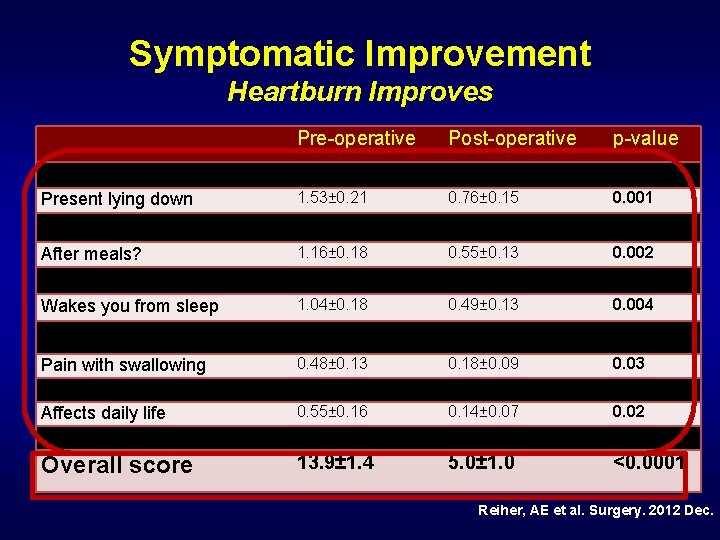
Symptomatic Improvement Heartburn Improves Pre-operative Post-operative p-value Severity Present lying down Present standing up 2. 01± 0. 20 0. 84± 0. 14 <0. 0001 1. 53± 0. 21 0. 76± 0. 15 0. 001 1. 04± 0. 18 0. 49± 0. 13 0. 004 After meals? Affects diet 1. 16± 0. 18 0. 55± 0. 13 0. 002 0. 71± 0. 17 0. 37± 0. 11 0. 03 Wakes you from sleep Difficulty swallowing 1. 04± 0. 18 0. 49± 0. 13 0. 004 1. 03± 0. 21 0. 37± 0. 12 0. 002 Pain with swallowing Gassy/bloated Affects daily life Satisfaction 0. 48± 0. 13 1. 82± 0. 23 0. 55± 0. 16 2. 16± 0. 25 0. 18± 0. 09 0. 49± 0. 14± 0. 07 0. 55± 0. 14 0. 03 <0. 0001 0. 02 <0. 0001 Overall score 13. 9± 1. 4 5. 0± 1. 0 <0. 0001 Reiher, AE et al. Surgery. 2012 Dec.

Impact of Parathyroidectomy on Insomnia • Does Hyperparathyroidism affect sleep quality? • Is this true insomnia? • Does it get better? • Validated insomnia questionnaire • Pre-operatively and post-operatively Murray SE. World Journal of Surgery. Mar 2014
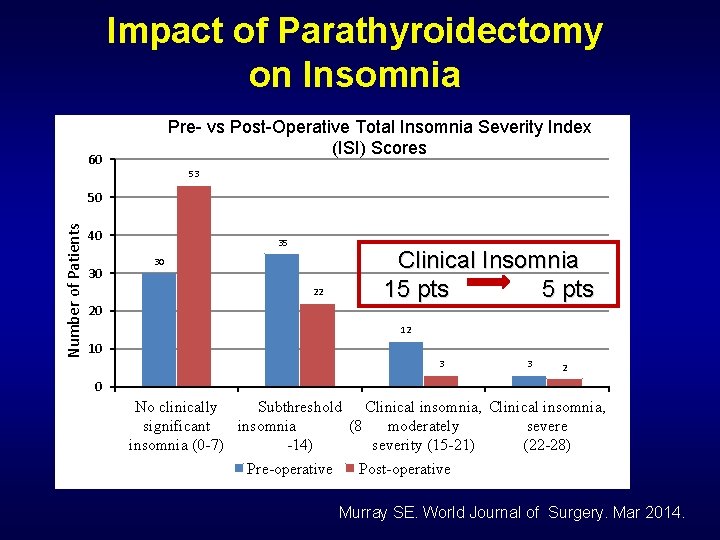
Impact of Parathyroidectomy on Insomnia Pre- vs Post-Operative Total Insomnia Severity Index (ISI) Scores 60 53 Number of Patients 50 40 30 35 30 22 20 Clinical Insomnia 15 pts 12 10 3 3 2 0 No clinically Subthreshold Clinical insomnia, significant insomnia (8 moderately severe insomnia (0 -7) -14) severity (15 -21) (22 -28) Pre-operative Post-operative Murray SE. World Journal of Surgery. Mar 2014.

Quality of Life Improvements after Parathyroidectomy
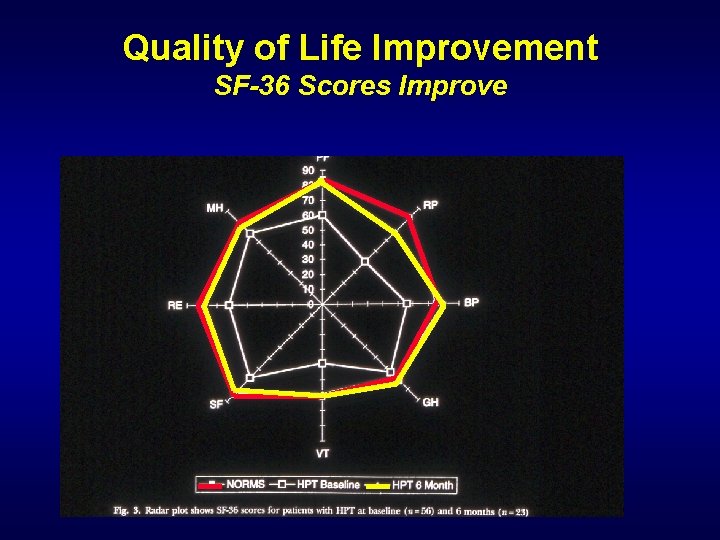
Quality of Life Improvement SF-36 Scores Improve

Quality of Life Improvement Mild Asymptomatic Hyperparathyroidism • RCT: Parathyroidectomy vs. Observation • At 1 yr. surgery patients had significant improvements in four quality of life measures: bodily pain (P = 0. 001), general health (P = 0. 008), vitality (P = 0. 003), and mental health (P = 0. 017) • 150 pts with Primary HPTH undergoing surgery • Improved in all scales on SF-36 • “mild” disease improved more than “classic” J Clin Endocrinol Metab. 2007 Aug; 92(8) Am Journal of Surgery 2009. 197, 284 -290

Bone Improvements after Parathyroidectomy
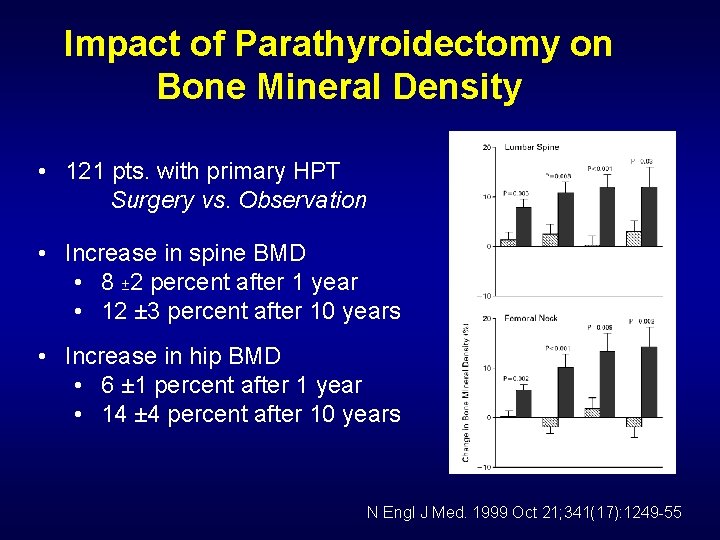
Impact of Parathyroidectomy on Bone Mineral Density • 121 pts. with primary HPT Surgery vs. Observation • Increase in spine BMD • 8 ± 2 percent after 1 year • 12 ± 3 percent after 10 years • Increase in hip BMD • 6 ± 1 percent after 1 year • 14 ± 4 percent after 10 years N Engl J Med. 1999 Oct 21; 341(17): 1249 -55
Impact of Parathyroidectomy on Bone Mineral Density What does this mean for an individual patient? • • Baseline 12% at 1 yr 19% at 3 yr 29% at 5 yr T score = -3. 1 T score = -2. 6 T score = -2. 0 T score = -1. 2 JBMR 2007. 25: 226 -231

Impact of Parathyroidectomy on Fracture Risk • Risk of fracture is increased up to 10 years before surgery • The risk of fracture is not related to the degree of hypercalcemia • The fracture risk returns to normal 1 year after surgery Vestergaard BMJ 321: 598 -602, 2000
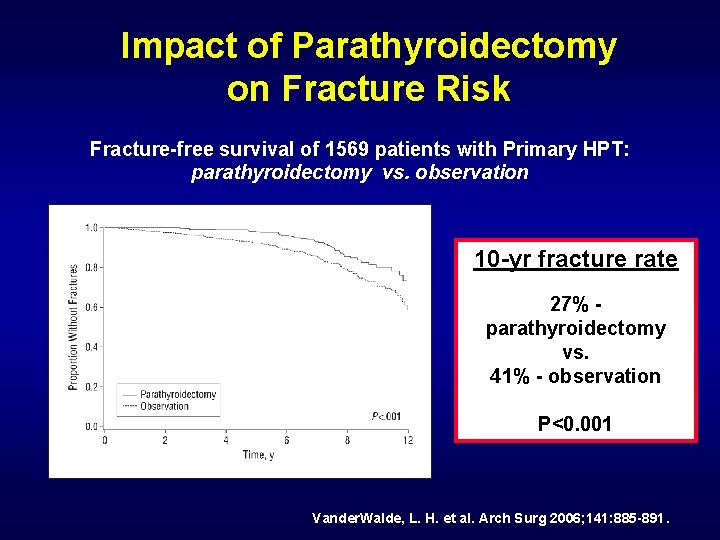
Impact of Parathyroidectomy on Fracture Risk Fracture-free survival of 1569 patients with Primary HPT: parathyroidectomy vs. observation 10 -yr fracture rate 27% parathyroidectomy vs. 41% - observation P<0. 001 Vander. Walde, L. H. et al. Arch Surg 2006; 141: 885 -891.

Bone Effects after Parathyroidectomy Decrease in Fracture Risk What about medical therapy – why not just use bisphonates? 22 elderly patients with primary hyperparathyroidism Surgery Bisphonate Therapy 20% increase in Lumbar BMD 10% increase in Lumbar BMD Gerontology. 2002 48(2): 03 -8.

Cardiac Benefits of Parathyroidectomy
Cardiac Benefits of Parathyroidectomy Decrease in LVH • Left Ventricular Hypertrophy • • • Present in 65% of pts. Correlates with PTH levels Resolves within 6 mo • Blood Pressure • Decreases by an average of 20 mm Hg after surgery Clinical Endocrinology 50: 321 -8, 1999
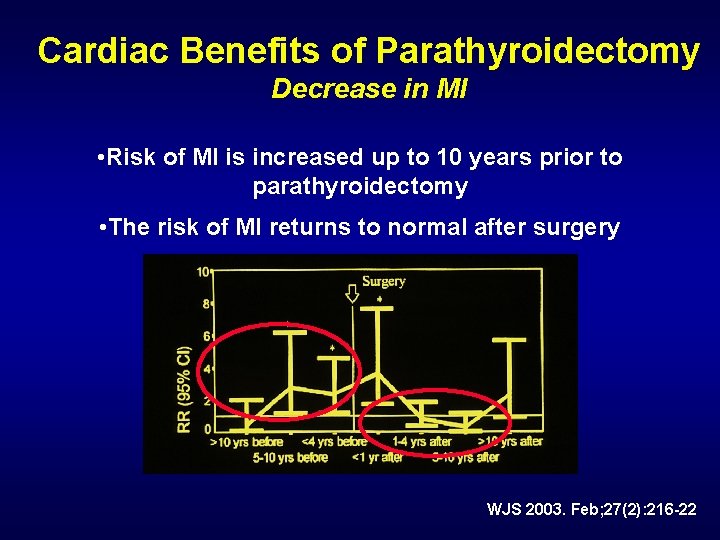
Cardiac Benefits of Parathyroidectomy Decrease in MI • Risk of MI is increased up to 10 years prior to parathyroidectomy • The risk of MI returns to normal after surgery WJS 2003. Feb; 27(2): 216 -22

Improved Mortality after Parathyroidectomy

Impact of Parathyroid Disease on Overall Survival 1578 pts. with 1º Hyperparathyroidism • 15 year follow up – 20% died • Patients with Hyperparathyroidism were 70% more likely to die than the general population • Why did they die? • Heart attacks • Strokes • Cancer World J Surg. 2004 Jan; 28(1): 108 -11

Summary 1. Hyperparathyroidism is a common condition, especially in the elderly 2. While many patients are discovered incidentally, the majority of them are actually symptomatic 3. Parathyroidectomy can: • • Improve symptoms in 2/3 of patients Increase BMD/decrease fracture risk Improve overall QOL Decrease overall and cardiovascular mortality

Treatment of Primary Hyperparathyroidism

Primary Hyperparathyroidism Treatment Options 1. Observation (23 -62% chance of progression at 10 yrs) • • Keep hydrated, avoid thiazides, normal calcium intake Biannual labs 2. Medical Therapy • • • Not recommended Estrogen or Bisphonates for osteoporosis Cinacalcet – Calcium sensing receptor blocker ($$$) 3. Surgery • Only definitive treatment : 95 -98% cure rate

Primary Hyperparathyroidism Surgical Treatment • Diagnosis is Based on Labs • Imaging guides surgical plan it does not make a diagnosis • Negative imaging is seen in about 20 -30% of patients • Goals at Surgery • Distinguish between unilateral (adenoma) vs. multi-gland disease • Clear neck at first operation

Primary Hyperparathyroidism Etiology MULTI-GLAND DISEASE SINGLE ADENOMA PARATHYROID CARCINOMA PARATHYROMATOSIS

Minimally Invasive Parathyroidectomy (MIP) • Advantages • • • Smaller incision size (2 -3 cm) Decreased operative time Can be done with local anesthesia/cervical block Done as an outpatient Less transient hypocalcemia Can examine all 4 glands through the same small incision Bergenfelz A et al. Ann Surg 236: 543 -51, 2002

Technique of MIP 1. Pre-operative localization 2. Intra-operative localization (optional) 3. Intra-operative PTH assay to confirm cure
Pre-operative Localization Nuclear Imaging Tc-99 m Sestamibi
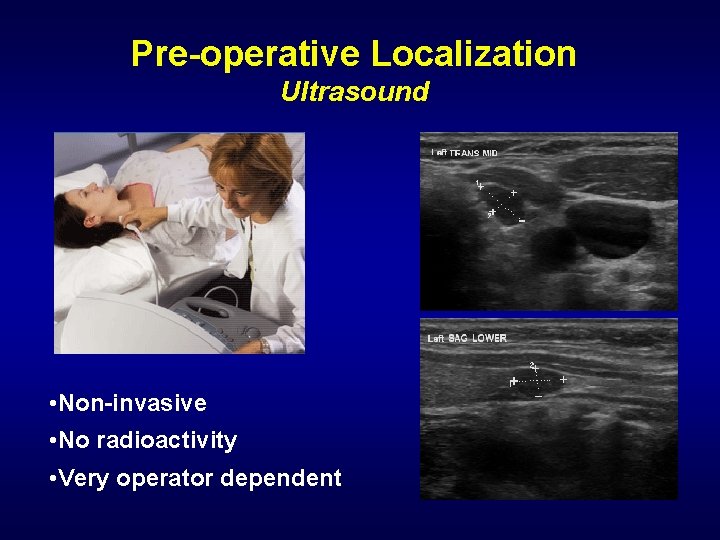
Pre-operative Localization Ultrasound • Non-invasive • No radioactivity • Very operator dependent
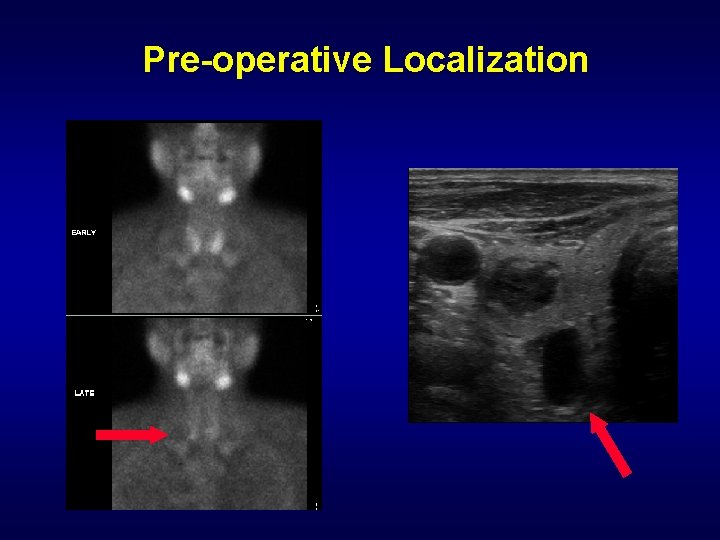
Pre-operative Localization
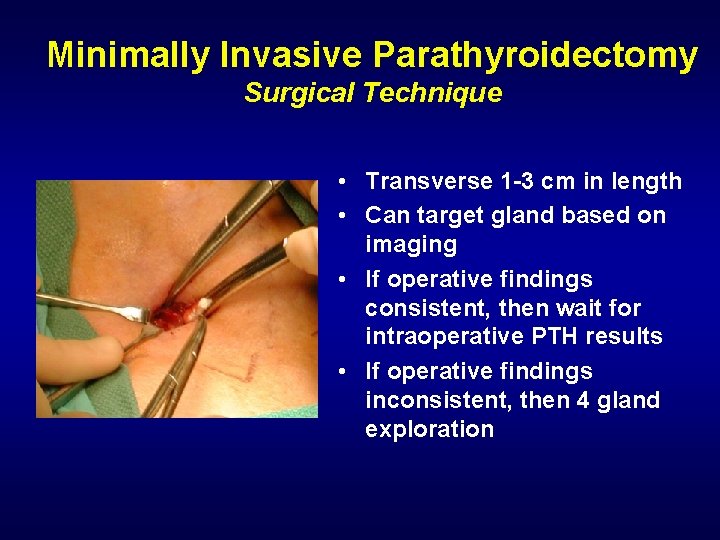
Minimally Invasive Parathyroidectomy Surgical Technique • Transverse 1 -3 cm in length • Can target gland based on imaging • If operative findings consistent, then wait for intraoperative PTH results • If operative findings inconsistent, then 4 gland exploration

Minimally Invasive Parathyroidectomy Intra-operative PTH Monitoring • PTH has a half-life of only 2 -3 minutes • Within 2 -3 half-lives the blood levels should fall by >50% • 95% accurate at predicting cure • Very accurate in patients with single gland disease
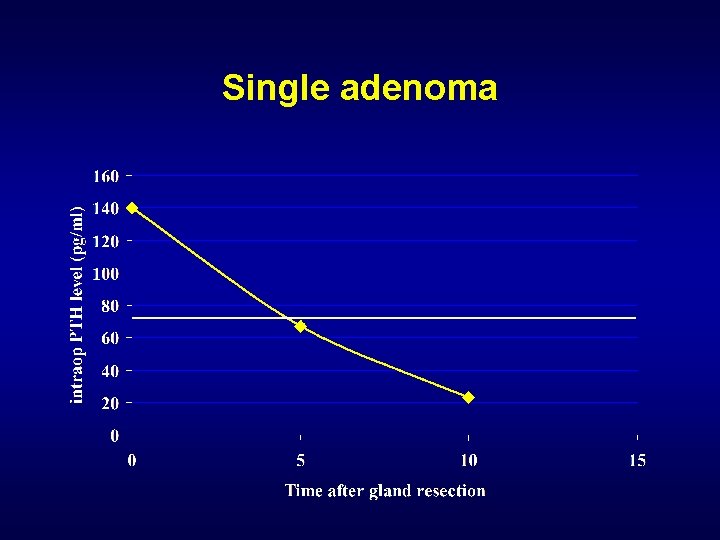
Single adenoma
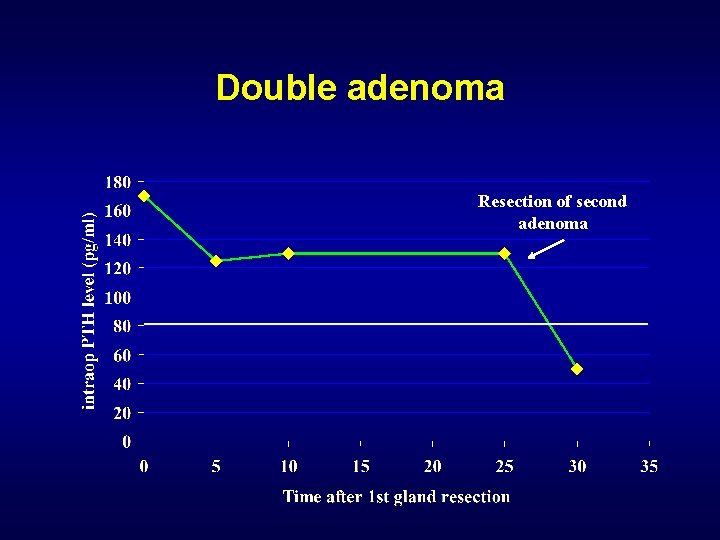
Double adenoma Resection of second adenoma
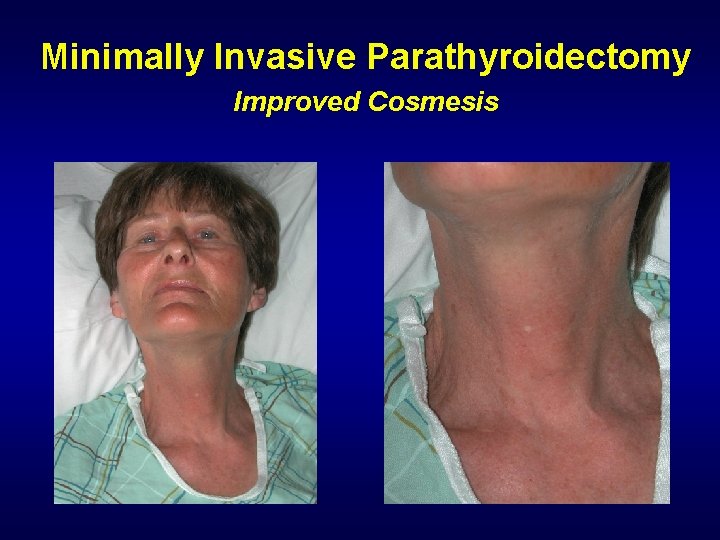
Minimally Invasive Parathyroidectomy Improved Cosmesis
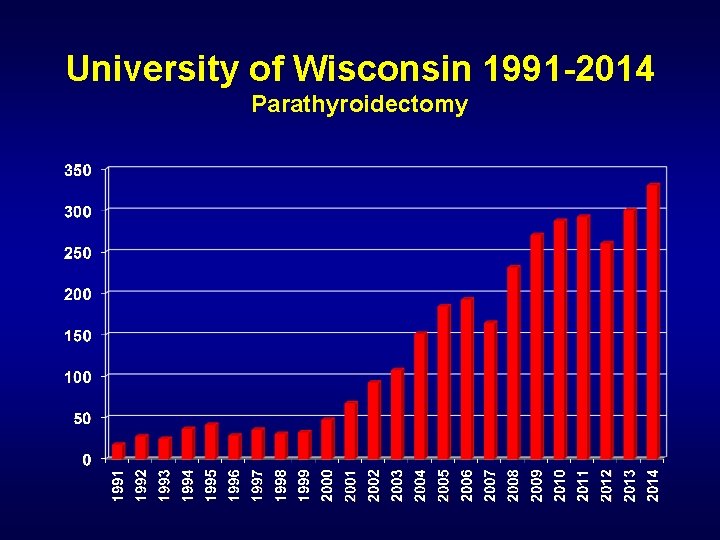
University of Wisconsin 1991 -2014 Parathyroidectomy

Conclusions 1. Virtually all patients with HPT benefit from parathyroidectomy (symptomatically, metabolically, and improved survival) 2. A minimally invasive approach can be used to treat patients with sporadic HPT with about a 97% cure rate and minimal morbidity in experienced hands

Web Resources for Patients AAES Patient Education Website • http: //endocrinediseases. org/index. shtml UW Patient Education Website • http: //www. surgery. wisc. edu/specialties/endocrin e-surgery/conditions-andprocedures/hyperparathyroidism/

Questions? UW Endocrine Surgery Program Dr. David Schneider Dr. Susan Pitt Dr. Rebecca Sippel Dr. Kristin Long 608 -440 -6300 sippel@surgery. wisc. edu Sarah Schaefer, NP
- Slides: 57