Primary craniocerebral vasculitis Takayasus arteritis giant cell arteritis

Primary craniocerebral vasculitis Takayasu’s arteritis, giant cell arteritis and primary CNS angiitis all have granulomatous angiitis Takayasu’s arteritis: – This affects the aortic arch, main arterial trunks and descending aorta including the carotid and subclavian arteries – Incidence in Japan is 1 in 3000, mainly in younger women aged 15 -45 – The affected arteries become fibrotic, rigid and narrowed, which can lead to cerebral ischemia

Giant cell arteritis: – Most common of the three granulomatous arteritides (2 in 10, 000 over age 50) – Targets the extracranial arteries of the head and neck – If the superficial temporal artery is affected it may be thickened and tender – There is an association with polymyalgia rheumatica, very elevated ESR and a risk of blindness from extension to the opthalmic arteries – It responds promptly to steroids – Can also affect the carotid and vertebral arteries leading to cerebral infarcts
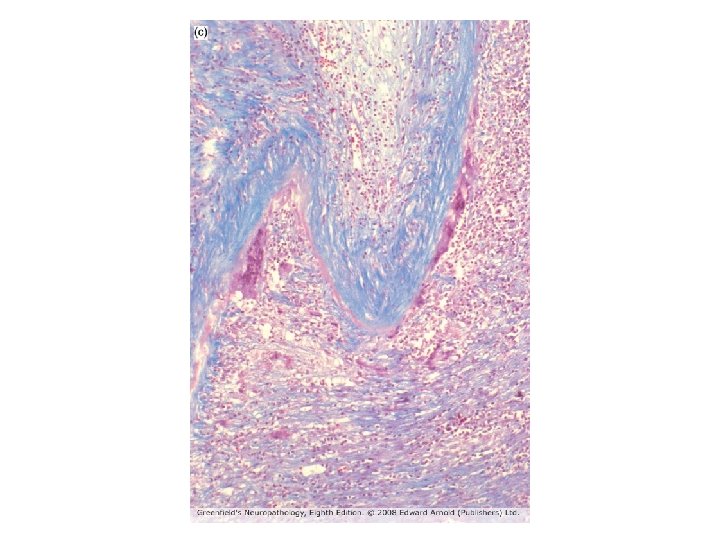

Primary CNS angiitis • Primary CNS angiitis: – Typically affects women aged 30 -50 – Angiography shows narrowed segments in intracerebral arteries – Clinical picture is non-specific (eg headaches, confusion, memory impairment or focal deficits) – Aggressive immunosuppressive therapy can treat the disease effectively
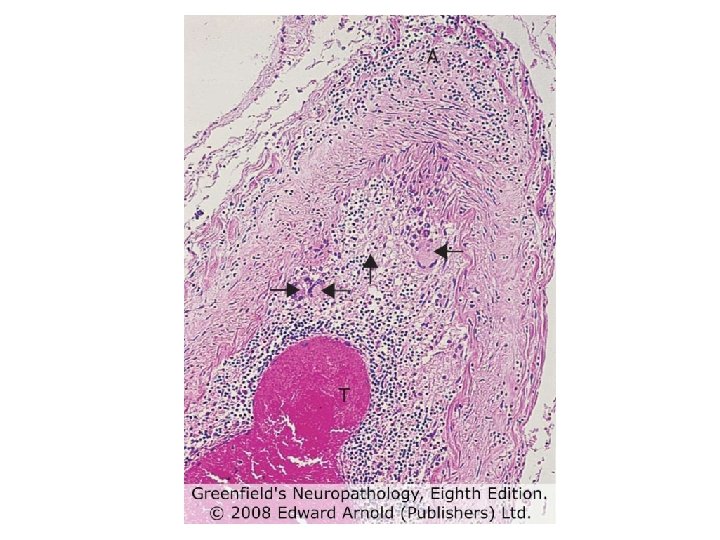

ABRA • Amyloid-beta related angiitis • An unusual complication of Aβ-CAA • 5 cases in the last 3 years

ABRA • ABRA presents at an older age (mean 67) than primary CNS angiitis (mean 43), but younger than non inflammatory Aβ-CAA (mean 76) • Primary angiitis cannot be distinguished from ABRA except by pathology • Biopsies showing vasculitis should be routinely examined for Aβ deposits
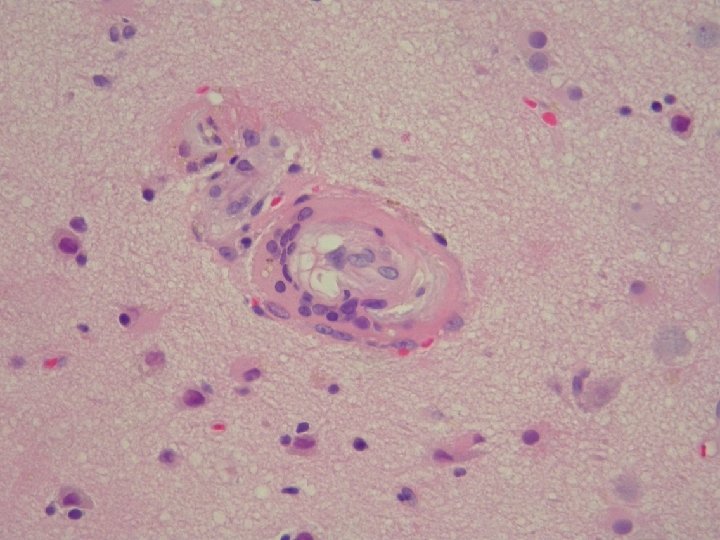

Vasculitis in systemic diseases • Lupus – 50 -75% of patients have CNS involvement – Immune complex mediated vasculitis may lead to infarcts, vessels show fibrinoid necrosis, mononuclear inflammation and fibrosis – However, a predisposition to thrombosis is also advanced as the main cause of the CNS damage, and some authors discount vasculitis entirely • Polyarteritis nodosa – Causes necrotizing lesions in medium sized to small arteries – In systemic PAN the visceral organs are targeted – In limited PAN both skeletal muscle and peripheral nerve are involved with late CNS involvement

Vasculitis in systemic diseases • ANCA associated vasculitides – ANCA stands for anti-neutrophil cytoplasmic antibodies – Wegener’s affects lung and kidney; about 30% develop CNS complications with focal necrotizing or granulomatous vasculitis – Churg-Strauss has an allergic component (with asthma and eosinophilia). There is a necrotizing vasculitis in medium sized to small arteries with extravascular granulomas and abundant eosinophils; 60 -70% develop peripheral neuropathies or CNS involvement

Vasculitis in systemic diseases • Sjögren’s syndrome – Autoimmune disorder that results in Sicca syndrome by involving the exocrine glands (salivary and lacrimal) – Involves peripheral nervous system with varying rates of CNS involvement – Vasculitis/vasculopathy has been described in venous vessels in CNS white matter and/or the leptomeninges • Behçet’s syndrome – Autoimmune disease producing recurrent oro-genital ulcers, uveitis and arthritis – 30 -40% have CNS involvement typically meningoencephalitis of the brain stem (rhombencephalitis) – Vasculitis is reported in venules

Vasculitis in systemic diseases • Rheumatoid arthritis – Vasculitis of the leptomeninges or parenchyma has been reported; this may respond to steroids • Hodgkin’s disease – Paraneoplastic vasculitis of the CNS is rare with the exception of Hodgkin’s disease • Drug induced – Vasculitis has been documented in users of cocaine and amphetamines. There is an association between hepatitis B and C and polyarteritis nodosa, which may link vasculitis to drug use

Infectious causes • Bacterial – Both small and large arteries can be involved in pneumococcal meningitis and tuberculous meningitis, resulting in large infarcts • Spirochetes – Heubner’s arteritis occurs in meningovascular neurosyphilus; typically involves large extracranial arteries; T. pallidum cannot usually be identified in the vessel wall – Lyme disease due to B. burgdorferi which binds to vessel walls and induces vasculitis.

Infectious causes • Viral – Herpes zoster infections in immunosuppressed patients can lead to necrotizing/granulomatous/lymphocytic cerebral vasculitis – Vasculitis also reported in HIV and after retroviral combination therapy • Fungal – Commonest infections due to aspergillus, candida, coccidiodes and mucor species
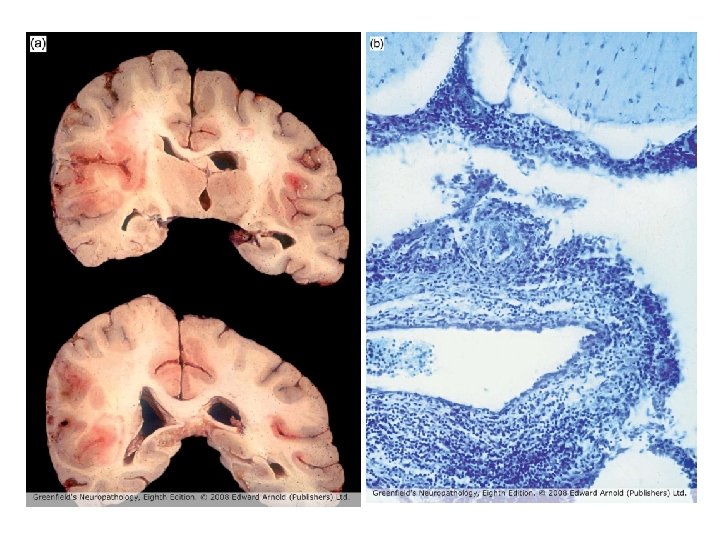
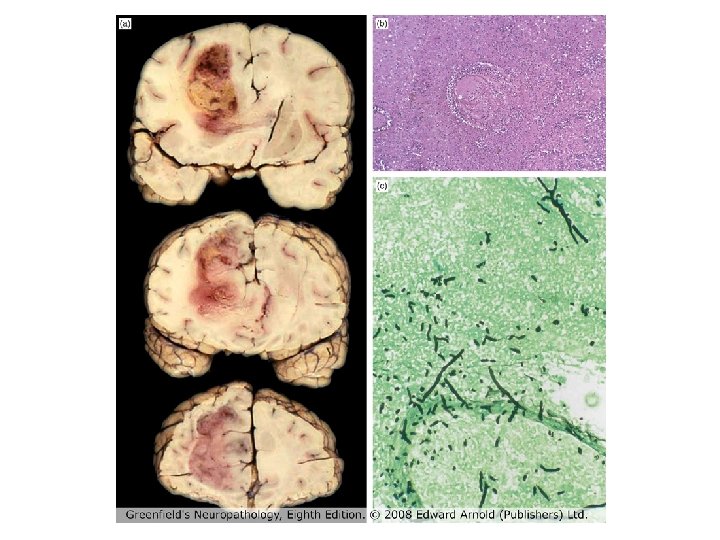

An unusual case of CNS vasculitis • 50 year old female social worker • Past medical history of ulcerative colitis, benign essential hypertension and hypothyroidism • Colitis flared up 3 -4 months before presentation, treated with prednisolone • Flared up 2 weeks before presentation again, treated with prednisolone

Case history • Patient underwent investigative colonoscopy 1 day before presenting • Presented (Oct 2010) with continuous dull headache present during the work day • This had increased in severity by evening • Accompanied by slurred speech, unsteady gait and progressive right sided paralysis

Case history • At a local hospital, she was diagnosed with a right sided stroke • While in hospital, developed sudden reduction in level of conciousness • ‘Grand mal seizure’ lasted 2 minutes • Patient was sedated, intubated and transferred to tertiary care hospital
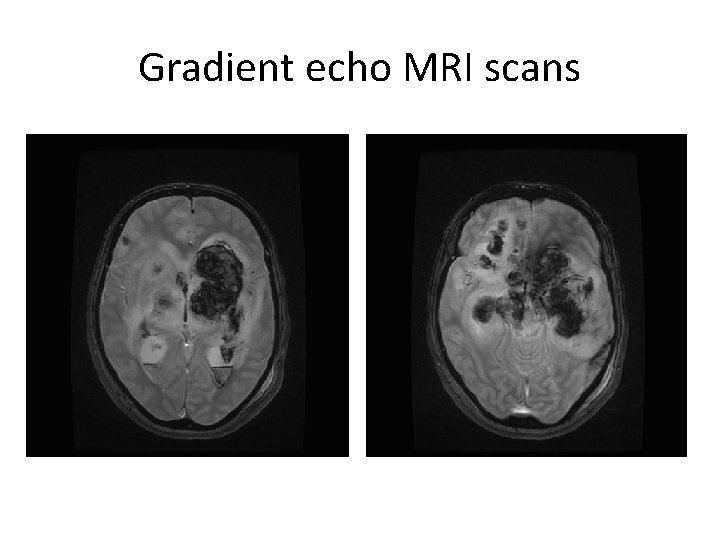
Gradient echo MRI scans
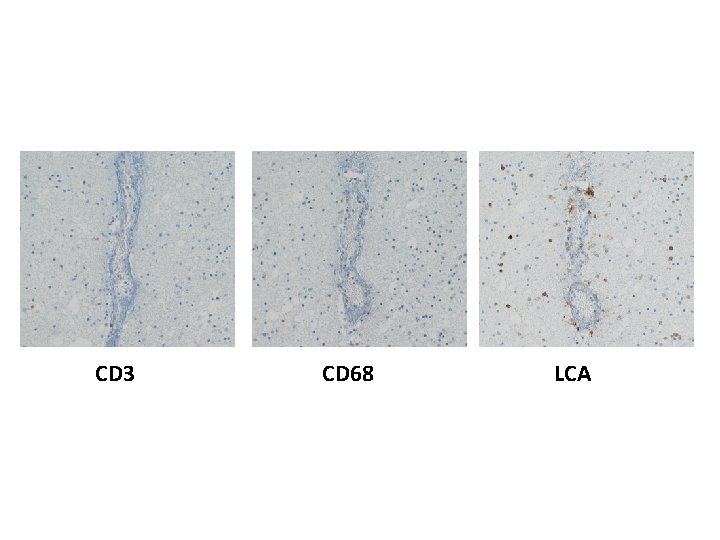
CD 3 CD 68 LCA
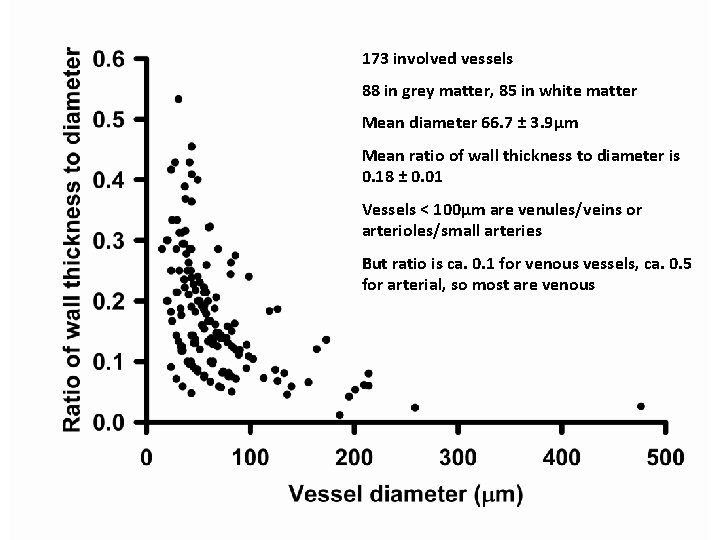
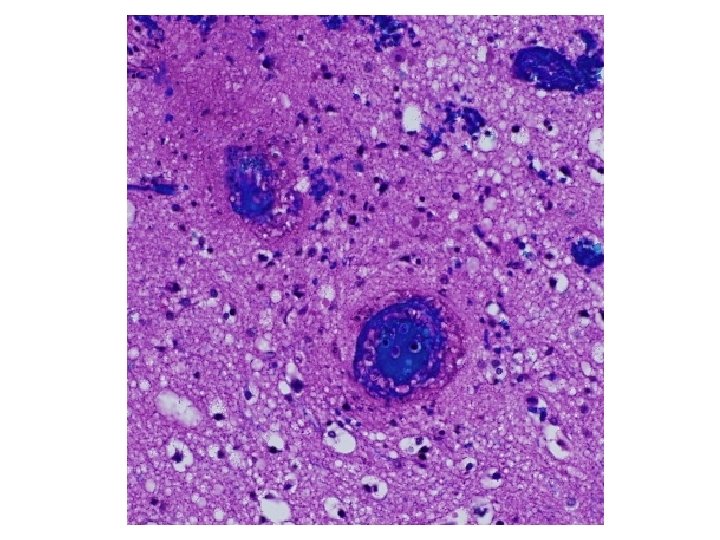
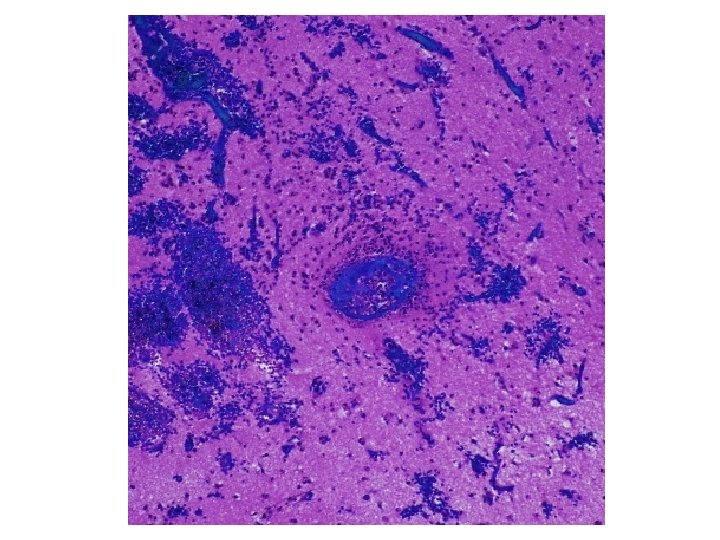
173 involved vessels 88 in grey matter, 85 in white matter Mean diameter 66. 7 ± 3. 9µm Mean ratio of wall thickness to diameter is 0. 18 ± 0. 01 Vessels < 100µm are venules/veins or arterioles/small arteries But ratio is ca. 0. 1 for venous vessels, ca. 0. 5 for arterial, so most are venous

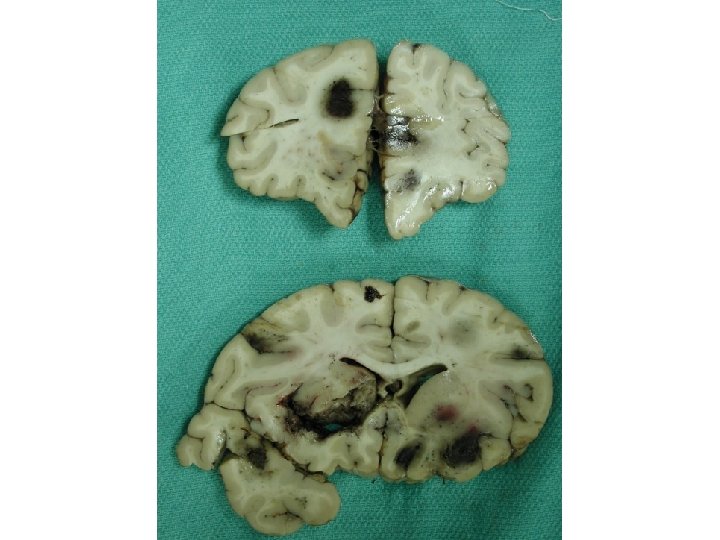
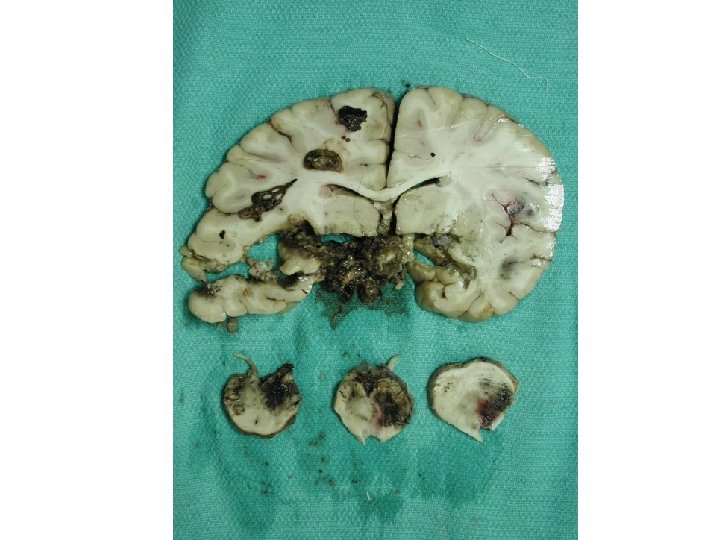
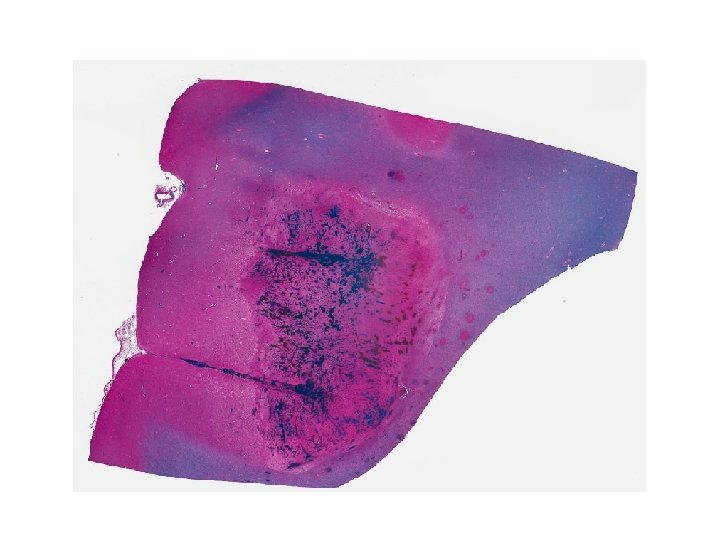
Diagnosis • Acute vasculitis, mostly venous, in association with ulcerative colitis • Predominantly neutrophilic (acute) • Venous involvement explains the extensive hemorrhage since tissue is under arterial perfusion pressure
Thanks! Questions?
- Slides: 29