Primary Care Behavioral Health Fidelity Through Quality Improvement

Primary Care Behavioral Health Fidelity Through Quality Improvement and Assurance Lesley Manson, Psy. D Director of Integrated Training Initiatives Arizona State University, Doctor of Behavioral Health Stacy Ogbeide, Psy. D Assistant Professor Dept. of Family & Community Medicine UTHSCSA Robynne M. Lute, Psy. D Assistant Professor & Assistant Director of Training in Behavioral Medicine, Midwestern University Society for Teachers of Family Medicine December 5, 2015 Dallas, Texas, U. S. A. L 31: Friday, 10: 00 a. m. to 11: 00 a. m.

Disclosures We have not had any relevant financial relationships during the past 12 months.

Please evaluate this presentation using the conference mobile app! Simply click on the "clipboard" icon on the presentation page.

Learning Objectives Learning Objective #1 § Identify clinical and fidelity metrics for PCBH programs related to quality improvement and assurance. Learning Objective #2 § Describe and discuss data mining options for collecting metrics to demonstrate fidelity and quality improvement related to PCBH. Learning Objective #3 § Discuss unique barriers in collecting and assessing metrics for developing and sustaining PCBH programs and for ensuring fidelity.

REFERENCES 1. Robinson, P. & Reiter, J. (2015). Behavioral Consultation and Primary Care: A Guide to Integrating Services (2 nd Edition). Springer International Publishing: Geneva, Switzerland. 1. Savage, A. , Lauby, T. , & Burkard, J. F. (2014) Examining selected patient outcomes and staff satisfaction in a primary care clinic at a military treatment facility after implementation of the patient-centered medical home. Military Medicine, 178(2): 128 134. 2. Goodie, J. L. , Kanzler, K. E. , Hunter, C. L. , Glotfelter, M. A. , & Bodart, J. J. (2013). Ethical and effectiveness considerations with primary care behavioral health research in medical home. Families, Systems, & Health, 31(1), 86 -95. 3. Runyan, C. (2011). Psychology can be indispensable to health care reform and the patient-centered medical home. Psychological Services, 53 -68. doi: 10. 1037/a 0023454

5. Bendix, J. (2014) RVUs: A valuable tool for aiding practice management. Understanding the basics of the RVU can assist physicians and practice managers in a wide variety of finance and management-related tasks. Med Econ, 91(4): 48 -51. 6. Corso, Hunter, Dahl, Kallenberg, and Manson (2016). Integrating behavioral health in the medical home: A rapid implementation guide. Greenbranch: Phoenix, Maryland. 7. Kilbourne, A. M. , Keyser, D. , & Pincus, H. A. (2010). Challenges and opportunities in measuring the quality of mental health care. Canadian Journal of Psychiatry, 55(9), 549 -557. 8. Vannoy, S. D. , Mauer, B. , Kern, J. , Girn, K. , Ingoglia, C. , Campbell, J. , . . . Unutzer, J. (2011). A learning collaborative of CMHCs and CHCs to support integration of behavioral health and general medical care. Psychiatric Services, 62, 753 -758. 9. Goldman, Spaeth-Rublee, Pincus (2015). Quality indicators for physical and behavioral health care indicators. Journal of the American Medical Association. 314(8): 769 -770. doi: 10. 1001/jama. 2015. 6447

RESOURCES • SAMHSA Center for Integrated Care – http: //www. integration. samhsa. gov/ • Agency for Healthcare Research and Quality (AHRQ): “Atlas of Integrated Behavioral Health Care Quality Measures” – http: //integrationacademy. ahrq. gov/atlas • Evaluation Processes – AHRQ: https: //cahps. ahrq. gov/qualityimprovement/improvement-guide/qi-steps/QIMethods_Models/index. html – Institute of Health Improvement (“How to Improve”) • http: //www. ihi. org/resources/Pages/Howto. Improve/defa ult. aspx

Primary Care Behavioral Health (PCBH)…. What is it? • Consultant model • Member of primary care team, work side-by-side • Goal is to improve PCP management of behavioral issues and improve satisfaction o o Wide variety of interventions and goals Brief visits, limited follow-up Immediate feedback to PCP Any behaviorally-based problem, any age • Immediate access, minimal barriers • Population health principles
• Integration is the standard • Not a question of should we integrate, rather how do we integrate? How do we create sustainable integration meeting the triple aim? Ø Identify Barriers to QI Ø Model Fidelity Ø QI Metrics and QI Healthcare Alignment Ø Provider Satisfaction Ø Patient Satisfaction Ø Clinical Quality Indicators

Experience and Satisfaction Objective • Patients experience the PCBH model of care as beneficial. • Patients (or their parents) express overall satisfaction with services provided in the PCBH program. • PCCs experience the PCBH model of care as beneficial and report improved satisfaction. • Increasingly, PCCs report reduced barriers to use of PCBH services. • Increasingly, PCCs indicate a stronger likelihood of working with the PCBH staff to develop and support a behavior change plans for their patients.

Begin at the Beginning • Why integrate…develop metrics…now? • Choose a model (PCBH) • What do we wish to accomplish, demonstrate? – Program Expansion – Patient Driven – Provider/Clinician Driven – Team based care – Financial – Encouraged/Required (PCMH, etc)

Team Based Approach to QI • • • QI is a team process Encourage and seek collaboration Ask questions together Identify barriers Overcome, step side-ways, and leap!

Team Approach • • • Administration Stakeholders Leaders Clinicians Patients Community Members

Barriers to Quality Assurance /Quality Improvement

Barriers to Quality Improvement • Identify the barriers (clinical & administrative) – Time – Resources (workers, workload) – Electronic Health Records – Stakeholders –? Vannoy et al. , 2011

Barriers to Quality Improvement • Poorly defined quality measures • Lack of linked electronic health information • Limited descriptions of behavioral health for program metrics • Limited to MH Kilbourne, Keyser, & Pincus, 2010

Barriers to Quality Improvement • Lacking – Medical linkage – Clinical relevance – Fiscal outcomes Be Proactive in Identifying Barriers! Be Curious, Be a Systems Thinker! Be a Change Agent, Being Reflective! Kilbourne, Keyser, & Pincus, 2010

Reinforce the Whys Ø Promotes organization self-monitoring Ø Promotes improvement Ø Accountability Ø Sustainability

Overcoming Barriers • Need for behavioral health researchers to improve the evidence base for behavioral health treatment • Use of incentives to promote provider accountability for improving care: Start small and celebrate victories! • Refinement of technologies to promote adequate data capture of mental/behavioral health services Kilbourne, Keyser, & Pincus, 2010

Overcoming Barriers • Recognize they always will exist (normalize)! • Standardize a Team-based approach – (Teach It) • Standardize QI in clinical training curriculum! Cross train re QI/QA – (PDSAs, pro formas, PI teams, LEAN, Re. Aim, RIE)

Overcoming Barriers • Monitor and implement strategies to reduce “change fatigue” – use MI – recognize not everyone is ready for change – ambivalence is normal. • Roll with resistance, dance! • Resistance is opportunity! • Listen to other prioritizes!

Start with Standardized Approach

Start with Standardizing üExecutive leadership review and definition of how you are implementing and fostering the culture of integrated care üIdentify expectations from leadership, providers, staff, and patients üMirror the quality management to the medical practice review and consider reviewing the established metrics first üEvery quality indicator MUST be measureable and SMART!

Standard Questions • • What are you going to improve? How will you measure it? By how much? Impact relevance (financial, patient, clinician, system) Who is involved in the change? How will you know change is an improvement? What changes can you make which will lead to the improvement (PDSAs, RIE)? • How will you get reliable data? Adapt, Adopt, or Discard!

How do we evaluate PCBH? Operational and Model Fidelity • • Productivity/Access Session frequency Time spent with patients Penetration rates Top diagnoses Clinical quality indicators Increased early identification • • Care team meetings Huddling Psychosocial wellbeing Chronic illness health improvement • Shared documentation requirements/shared goals • Increased usage of community resources

How do we evaluate PCBH? Operational and Model Fidelity • Team communication expectations • Location of services • Provider satisfaction • Patient satisfaction • Access to BH improves • Cost outcomes • Utilization outcomes – WHO / Provider Use / Consults • Health related quality of life indicators • Wait time of PCC decreases • Reduction in over utilizers in ED / PC

Quality Indicator Focus • Operational – Model fidelity – Culture specific Consider process, structure, workflows, benchmarks, and outcomes • Fiscal – Program sustainability – Program growth • Quality – – – Value based Experience of care Population health Satisfaction Cost Ultimately: Help clinics meet the Triple Aim & providers manage their patients

Examples

Operational / Model Session Specific Metrics • X Number of visits per episode of care – Why important? – Benchmarks • Clinic dependent • • Mean number of visits = 2 - 4 visits Median = 2 visits Mode = 1 visits No more than 10 -15% of patients receiving more than 6 visits in 12 month period with specific justification of care: PHM or group medical visit focus
Increase percentage of patients who are seen for X treatment needs through PCBH by X% • Percentage of clinic patients having a BH consult – Benchmark • Duplicated vs. . unduplicated • 40 -100% for a robust clinic • Clinic dependent • Tracking ability • 25 -30% of clinic • Care team / pod specific • Identify the top diagnosis – Benchmark • Clinic dependent • PHM focus • Quality improvement focus • Provider study

Clinical Quality Metrics Ø Review PCMH NCQA Requirements for IBH. Ø Review NQF, UDS, HEDIS Metrics PCMH 2, Element D, Factor 3: MUST PASS The Practice Team: • Increase frequency by X of utilization of huddle care team / IBH as part of daily primary care team huddles NQF 0710: Depression Remission at Twelve Months: PCMH 3, Element B, Factor 9: • Improve X percentage of depression remission (PHQ-9 score of less than 5) at 12 months for patient’s with PHQ 9 over 9.

Population Health • Improve patient quality of life functioning score on the X measure after X days/weeks. • Improve X percentage of patients screened for X in PC each week/month/quarter. • Improve patient physical health indicators (e. g. , body mass index, waist girth, weight, blood pressure, blood glucose levels, lipid levels, pain level, alcohol use, physical activity, tobacco use) for X patients in X time or through X program.

• Increase the percentage of patients who follow through with their behavioral health referral to X%. • Increase access by X% to integrated behavioral health services through primary care team inclusion and warm handoff/same day service provision. • Increase percentage of patients who are seen for X medical or behavioral health treatment needs by the integrated behavioral health provider by %.

Experience of Care • Improve provider satisfaction with integrated behavioral health and team based primary care through completion of % BH satisfaction surveys at % level. • Improve clinician satisfaction by X% re role, employment, engagement, quality of care. • Improve patient satisfaction with integrated behavioral health and team based primary care through completion of % BH satisfaction surveys at % level. – My care was improved by partnering with a behavioral health provider. – My overall health will improve as a result of this visit. – I feel heard, understood and respected as an active member of my health care team.

Experience of Care • Improve CGCAHPS National Survey Data results by X %. – (29. ) In the last 6 months, how often did this provider involve you in decisions about your care as much as you wanted? – (36. ) Would you recommend this provider's office to your family and friends? – (15. ) In the last 6 months, how often did this provider listen carefully to you?
Cost • Increase X% of patients that were referred to the PC BH staff that kept the appointment (patients with untreated problems have higher overall cost) • X% reduction in ED usage of specific utilization • X% increase/decrease in per capita costs • X cost savings through X per X time for PCBH • X decrease in hospital readmissions for X time/population • X% revenue generation for PCBH appts for X timeline • Increase/decrease X% of patients that were referred for a BH appointment outside of the primary care clinic • Increase/decrease X% of return on investment through PCBH for X timeline

Data Mining Options Collecting metrics to demonstrate quality improvement in PCBH

Where/How do I find the Data? • Claims data • ROI for insurance companies • Joint ventures with insurance companies • Registries • Survey Data • Electronic Health Records • HIE (Health Information Exchanges) • HEDIS, UDS, NQF, Physician Quality Reporting • Self-reporting • Other ways?

Electronic Health Systems and Technology EHR Systems/ HIT – Population identification – Identification of care gaps – Stratification – Patient engagement – Care management – Outcomes measurement

Understand Your Data and Sources • Forms of Data: How to choose? – Claims – Chunking – Small amounts – Analytical vs. Clinical • Volume of Data – How to understand it? – How is it relevant?

Identify the Relevant Data Points • Organizational – Employee wellness – Job satisfaction – employment sustainment – Satisfaction • Model – Length of session – CPT coding – Diagnosis coding – Visit type – Productivity – Huddles – Communication – Documentation

Identify the Relevant Data Points • Clinical Indicators – Mortality – Health status – Biometrics – Disease prevalence – Disability status – Health Maintenance – Health assessments (screening tools) – ED visits – Re-admission – PHM • Standardization – HEDIS – UDS / NQF / CMS – Annual QI Goals – RVUs/Productivity – Fiscal ROI – NCQA PCMH

Quality Improvement/ Evaluation • Plan-Do-Study-Act (PDSA) • RE-AIM Framework (Reach, Effectiveness, Adoption, Implementation, Maintenance): As you design, plan, or evaluate an intervention, there are questions that you should ask yourself: – Reach your intended target population – Efficacy: Intervention effectiveness; negative consequences? – Adoption by target staff, settings, or institutions – Implementation consistency, costs and adaptations made during delivery – Maintenance of intervention effects in individuals and settings over time • Process and Program Evaluations (e. g. , Precede-Proceed): 1) Planning 2) Evaluation

Since time is ticking… • Let’s look at some QI in action – Benchmark provided but unique to each clinic/organization – Recognize how to use data – Create visual representations We will have time for questions!

Productivity / Access to Care • Patient per hour/clinic – Benchmarks • • 1. 5 patients per hour OR • 50% of PCP’s expectations per clinic • PCPs expected to see 10 patients per clinic, BHCs expected to see 5 patients per clinic Initial vs. . Follow-ups – Danger to both sides of the coin – Benchmarks • • 1: 1 or 50% of visits being initials Warm-handoffs/Same-day visits – Benchmark • 50% of all visits
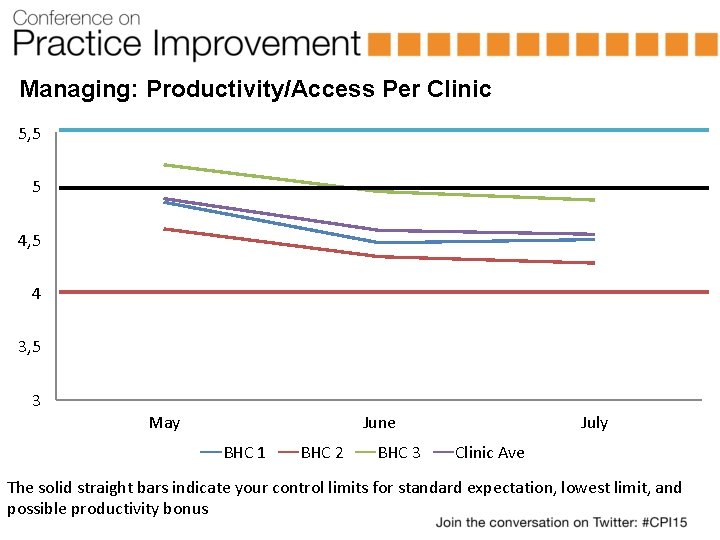
Managing: Productivity/Access Per Clinic 5, 5 5 4, 5 4 3, 5 3 May June BHC 1 BHC 2 BHC 3 July Clinic Ave The solid straight bars indicate your control limits for standard expectation, lowest limit, and possible productivity bonus
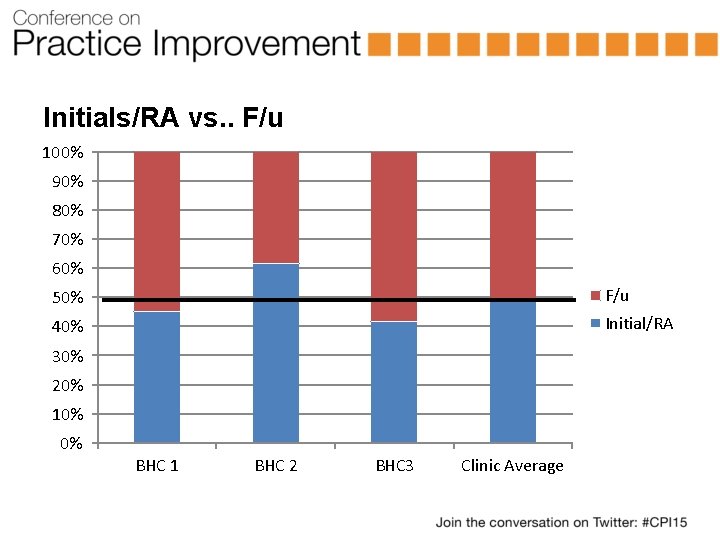
Initials/RA vs. . F/u 100% 90% 80% 70% 60% 50% F/u 40% Initial/RA 30% 20% 10% 0% BHC 1 BHC 2 BHC 3 Clinic Average
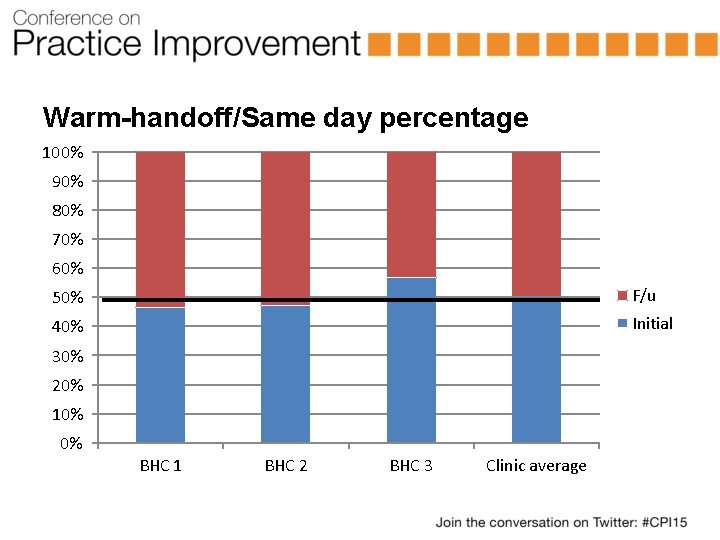
Warm-handoff/Same day percentage 100% 90% 80% 70% 60% 50% F/u 40% Initial 30% 20% 10% 0% BHC 1 BHC 2 BHC 3 Clinic average

Productivity and Access to Care Efforts • Improved patient and family care and satisfaction; early identification; patient centered; enhanced adherence and collaboration; shared decision making • Consultation; self management support, reduced health disparities; improved care team access • Improved cost containment; targeted use of resources; revenue generation; decreased other specialty visits, brief screenings for early identification; increased provider coding

QUESTIONS Lesley Manson, Psy. D. lesley. manson@asu. edu Robynne M. Lute, Psy. D rlute@midwestern. edu Stacy Ogbeide, Psy. D, MS stacy. ogbeide@gmail. com
- Slides: 50