PRIMARY ANGIOPLASTY DR RAJAT GANDHI INTERVENTIONAL CARDIOLOGIST BANKERS

PRIMARY ANGIOPLASTY DR. RAJAT GANDHI, INTERVENTIONAL CARDIOLOGIST , BANKERS HEART INSTITUTE , VADODRA.

RISK FACTORS FOR CAD �HYPERTENSION �DIABETES MELLUTUS �SMOKING �OBESITY �LACK OF EXERCISE �DYSLIPIDAEMIA
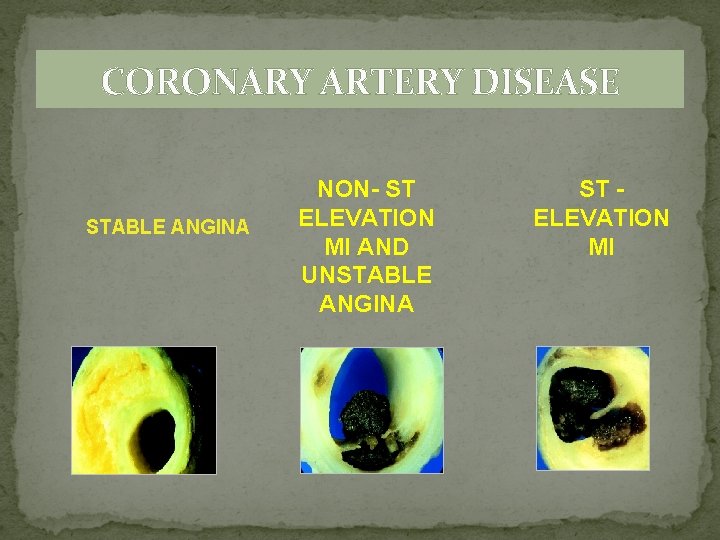
CORONARY ARTERY DISEASE STABLE ANGINA NON- ST ELEVATION MI AND UNSTABLE ANGINA ST ELEVATION MI

CORONARY ARTERY DISEASE �STABLE ANGINA - Chest discomfort precipitated by physical exertion releived by rest or nitrates. �UNSTABLE ANGINA -occurs at rest, last for more than 20 min, severe pain. NSTEMI – evidence of myocardial necrosis with high cardiac enzymes. STEMI - Complete occlusion of one coronary artery.

SYMPTOMS OF ACS -sudden onset of retrosternal CHEST PAIN. -lasting for more then 30 min. -associated with nausea, vomiting, shortness of breath
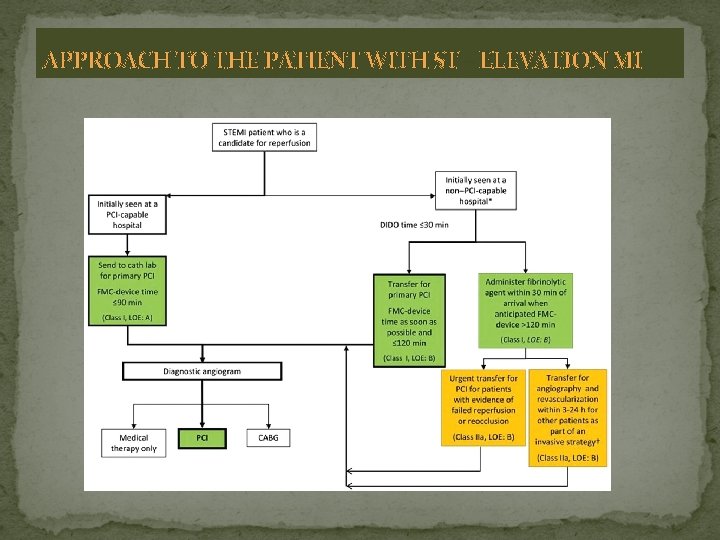
APPROACH TO THE PATIENT WITH ST – ELEVATION MI
TIME

GENERAL TREATMENT MEASURES �ASPIRIN 150 MG �CLOPIDOGREL /PRASUGREL/TICAGRELOR. �STATIN (ATORVA -80 MG, ROSUVA – 40 MG) �NITRATES(IF HAEMODYNAMICALLY STABLE) �OXYGEN

TIMI RISK SCORE FOR STEMI �AGE >75 YRS �SBP<100 MMHG �HEART RATE >100/MIN �LBBB �H/O DM/HTN �AWMI �TIME TO TREATMENT >4 HRS

FIBRINOLYTICS �Streptokinase - 1. 5 MU in 30 – 60 min , allergic reactions, marked fibrinogen depletion , 50 % -90 min patency rate , �Tenectplase – 30 -50 mg bolus , no allergic reaction , 75 % - 90 min patency rate , minimal fibrinogen depletion. �Reteplase – 10 u two bolus , 30 min apart , moderate fibrinogen depletion , 75% - 90 min patency rate. �Alteplase – up to 100 mg in 90 min , mild fibrinogen depletion , 75% - 90 min patency rate.
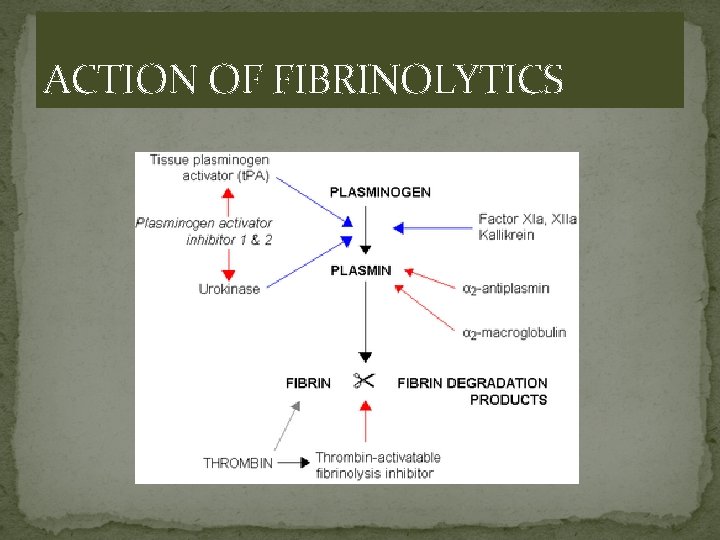
ACTION OF FIBRINOLYTICS

CONTRAINDICATIONS FOR FIBROLYTIC USE IN STEMI � ABSOLUTE – PRIOR ICH , CEREBERAL VASCULAR AV MALFORMATIONS , ISCHEMIC STROKE WITHIN 3 MONTHS , SUSPECTED AORTIC DISSECTION , BLEEDING DISORDERS , INTRACRANIAL NEOPLASMS. RELATIVE – SBP >180 , DBP > 110 MMHG, PREGNANCY , RECENT INTERNAL BLEEDING , RECENT MAJOR SURGERY, ISCHEMIC STROKE MORE THAN 3 MONTHS.

COMPLICATIONS OF FIBRINOLYTICS �FATAL INTRACRANIAL HAEMORRAGE. �INADEQUATE MYOCARDIAL REPERFUSION �CARDIOGENIC SHOCK. �MYOCARDIAL RUPTURE. �ANTIBODY RESISTANCE TO STREPTOKINASE.

ACC 2013 GUIDELINES FOR FIBRINOLYTIC THERAPY IN ACS PATIENTS. I IIa. IIb III Harm In the absence of contraindications, fibrinolytic therapy should be given to patients with STEMI and onset of ischemic symptoms within the previous 12 hours when it is anticipated that primary PCI cannot be performed Within 120 min. In the absence of contraindications and when PCI is not available, fibrinolytic therapy is reasonable for patients with STEMI if there is clinical and/or ECG evidence of ongoing ischemia within 12 to 24 hours of symptom onset and a large area of myocardium at risk or hemodynamic instability. Fibrinolytic therapy should not be administered to patients with ST depression except when a true posterior (inferobasal) MI is suspected or when associated with ST elevation in lead a. VR.

CORONARY ANGIOPLASTY �PRIMARY ANGIOPLASTY – EMERGENCY PERCUTANEOUS CORONARY INTERVENTION (PCI) IN PATIENTS WITH ACUTE ST ELEVATION MYOCARDIAL INFARCTION PRESENTED WITHIN 12 HOURS OF ONSET OF SYMPTOMS. �RESCUE ANGIOPLASTY – PCI IN PATIENTS WITH FAILED THROMBOLYSIS. �FACILITATED ANGIOPLASTY –PCI IN PATIENTS WITH STEMI WHO ARE PRETREATED WITH GP IIBIIIA INHIBITORS OR FIBRINOLYTICS.

ACC 2013 GUIDELINES FOR PRIMARY PCI IN STEMI. I IIa. IIb III Primary PCI should be performed in patients with STEMI and ischemic symptoms of less than 12 hours’ duration who have contraindications to fibrinolytic therapy, irrespective of the time delay from FMC. Primary PCI should be performed in patients with STEMI and cardiogenic shock or acute severe HF, irrespective of time delay from MI onset.

ACC GUIDELINES 2013 FOR PRIMARY PCI in STEMI I IIa. IIb III Harm Primary PCI is reasonable in patients with STEMI if there is clinical and/or ECG evidence of ongoing ischemia between 12 and 24 hours after symptom onset. PCI should not be performed in a noninfarct artery at the time of primary PCI in patients with STEMI who are hemodynamically stable

Antiplatelet Therapy to Support Primary PCI for STEMI I IIa. IIb III A loading dose of a P 2 Y 12 receptor inhibitor should be given as early as possible or at time of primary PCI to patients with STEMI. Options include: • Clopidogrel 600 mg; or • Prasugrel 60 mg; or • Ticagrelor 180 mg

Antiplatelet Therapy to Support Primary PCI for STEMI I IIa. IIb III Aspirin 150 to 300 mg should be given before primary PCI. I IIa. IIb III After PCI, aspirin should be continued indefinitely.

Antiplatelet Therapy to Support Primary PCI for STEMI I IIa. IIb III P 2 Y 12 inhibitor therapy should be given for 1 year to patients with STEMI who receive a stent (BMS or DES) during primary PCI using the following maintenance doses: • Clopidogrel 75 mg daily; or • Prasugrel 10 mg daily; or • Ticagrelor 90 mg twice a day* *The recommended maintenance dose of aspirin to be used with ticagrelor is 81 mg daily.

Antiplatelet Therapy to Support Primary PCI for STEMI I IIa. IIb III Harm Prasugrel should not be administered to patients with a history of prior stroke or transient ischemic attack.

New Inhibitors of the platelet the ADP P 2 Y 12 receptor Receptor Binding Prodrug Half life (requires hepatic activation) Onset of Action Clopidogrel Irreversible Yes Slow Long Prasugrel Irreversible (stronger) Yes More rapid Long Ticagrelor Reversible (stronger) No Rapid Short
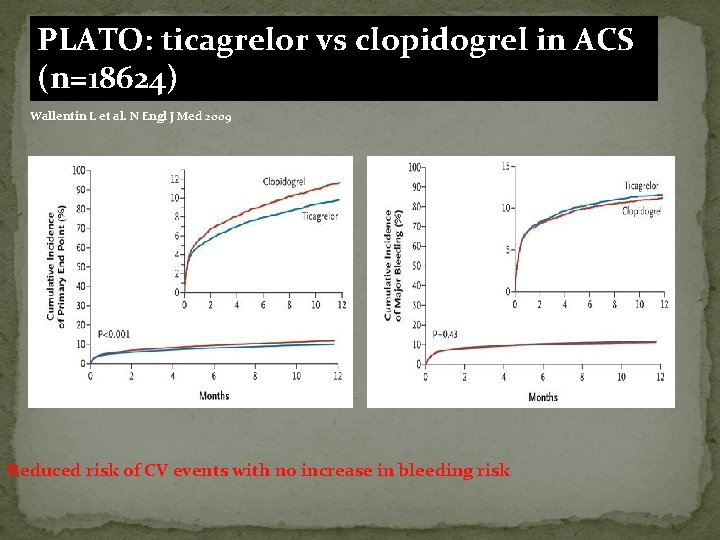
PLATO: ticagrelor vs clopidogrel in ACS (n=18624) Wallentin L et al. N Engl J Med 2009 Reduced risk of CV events with no increase in bleeding risk

NEWER ANTIPLATELETS �PRASUGREL – risk of stent thrombosis is half compared to clopidogrel , side effects ; high risk of bleeding in patients with weight <60 kg and age > 75. TICAGRELOR - reversible platelet inhibitor , safely given in patient with no restriction in age and weight.

Reperfusion at a PCI-Capable Hospital Use of Stents in Patients With STEMI

Use of Stents in Patients With STEMI I IIa. IIb III Harm Placement of a stent (BMS or DES) is useful in primary PCI for patients with STEMI. BMS* should be used in patients with high bleeding risk, inability to comply with 1 year of DAPT, or anticipated invasive or surgical procedures in the next year. DES should not be used in primary PCI for patients with STEMI who are unable to tolerate or comply with a prolonged course of DAPT because of the increased risk of stent thrombosis with premature discontinuation of one or both agents. *Balloon angioplasty without stent placement may be used in selected patients.
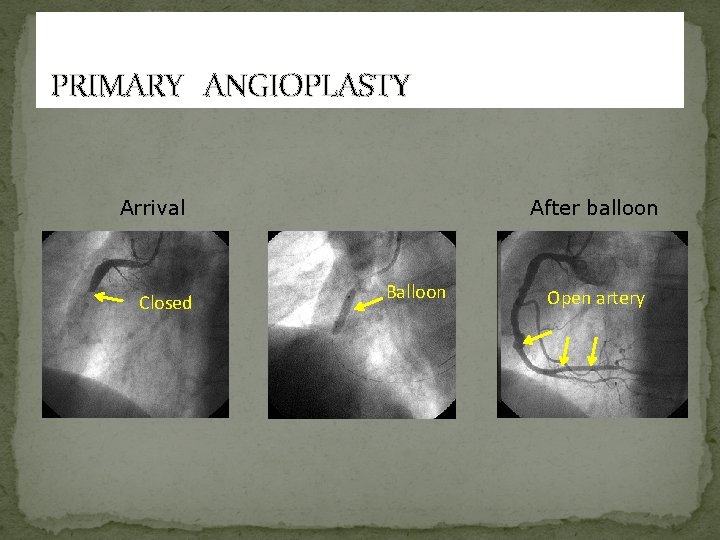
PRIMARY ANGIOPLASTY Arrival Closed After balloon Balloon Open artery
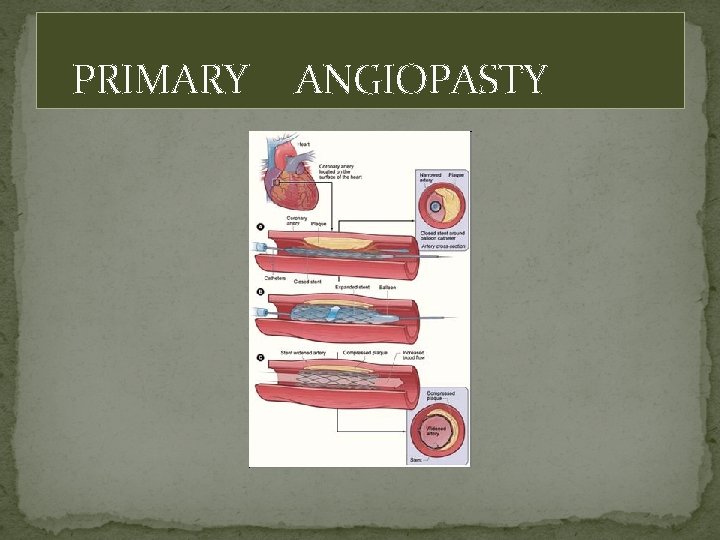
PRIMARY ANGIOPASTY
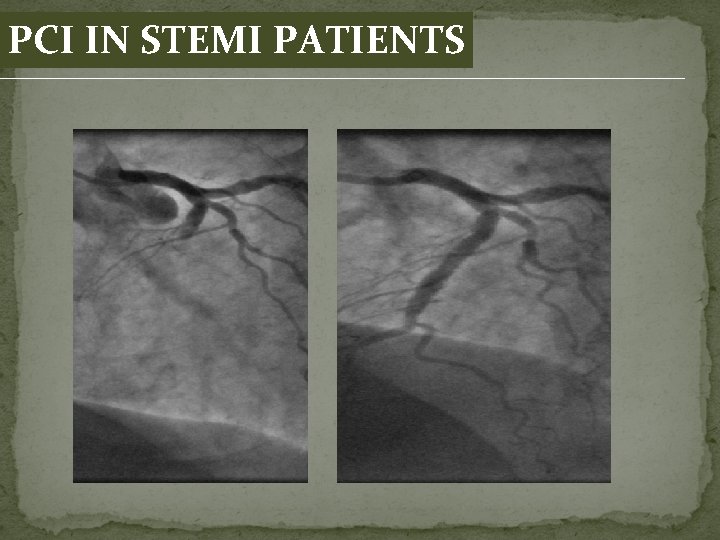
PCI IN STEMI PATIENTS
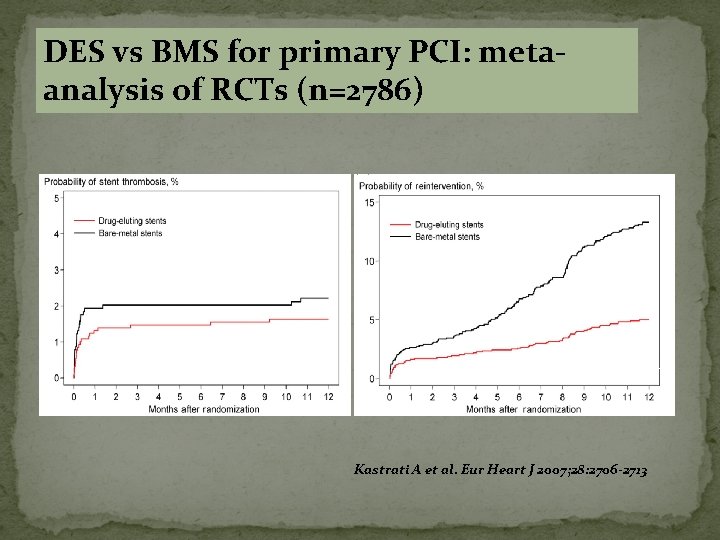
DES vs BMS for primary PCI: metaanalysis of RCTs (n=2786) HR: 0. 80 (0. 48 -1. 39) HR: 0. 38 (0. 29 -0. 50) Kastrati A et al. Eur Heart J 2007; 28: 2706 -2713

BARE METAL STENT �BMS currently used in 10% to 20 % patients. �Large size vessel > 4. 0 mm in diameter. �Restenosis is higher in small size vessel , long lesions and patients with diabetes. �Used in patients where dual antiplatelets cannot be given for longer time.

DRUG ELUTING STENTS �Made up of cobalt chromium. �Coated with durable polymer and drug. �Polymer helps sustained release of drug over 30 days. �Drugs like sirolimus, paclitaxel, everolimus. �Theses drugs are immunosuppressive and antiproliferative which prevent intimal hyperplasia.
PCI IN NSTEMI PATIENTS

Trials of Invasive vs Conservative O’Donoghue, M. et al. JAMA 2008; 300: 71 -80
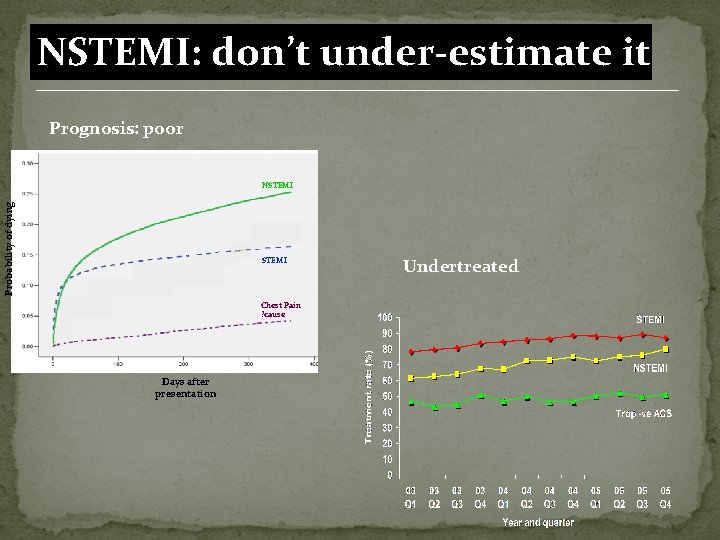
NSTEMI: don’t under-estimate it Prognosis: poor Probability of dying NSTEMI Non-MI ACS STEMI Chest Pain ? cause Days after presentation Undertreated

NSTEMI -etiology and prognosis �Myocyte necrosis – troponin levels �Haemodynamic stress – bnp and nt probnp levels �Vascular damage – microalbuminurea �Inflammation – hs. CRP �Acclerated athersclerosis HBA 1 C LEVELS

CLINICAL INDICATORS OF HIGH RISK IN NSTEMI. �AGE >70 YRS �LBBB �INCREASED TROPONIN LEVELS. �INCRRASED CREATININE , HBA 1 C, BNP LEVELS �HYPOTENSION �HEART FAILURE

Anticoagulant Therapy to Support Primary PCI For patients with STEMI undergoing primary PCI, the following supportive anticoagulant regimens are recommended: I IIa. IIb III • UFH, with additional boluses administered as needed to maintain therapeutic activated clotting time levels, taking into account whether a GP IIb/IIIa receptor antagonist has been administered; or • Bivalirudin with or without prior treatment with UFH.

Antiplatelet Therapy to Support Primary PCI for STEMI I IIa. IIb III It is reasonable to start treatment with an intravenous GP IIb/IIIa receptor antagonist at the time of primary PCI (with or without stenting or clopidogrel pretreatment) in selected patients with STEMI who are receiving UFH. • Abciximab: 0. 25 mg/kg IV bolus, then 0. 125 mcg/kg/min (maximum 10 mcg/min); or I IIa. IIb III • High-bolus-dose tirofiban: 25 mcg/kg IV bolus, then 0. 15 mcg/kg/min; or • Double-bolus eptifibatide: 180 mcg/kg IV bolus, then 2 mcg/kg/min; a 2 nd 180 -mcg/kg bolus is administered 10 min after the 1 st bolus.

CABG in Patients With STEMI I IIa. IIb III Urgent CABG is indicated in patients with STEMI with severe LMCA DISEASE. CABG is recommended in patients with STEMI at time of operative repair of mechanical defects.

Transfer of Patients With STEMI to a PCI-Capable Hospital for Coronary Angiography After Fibrinolytic Therapy I IIa. IIb III Transfer to a PCI-capable hospital for coronary angiography is reasonable for patients with STEMI who have received fibrinolytic therapy even when hemodynamically stable* and with clinical evidence of successful reperfusion. Angiography can be performed as soon as logistically feasible at the receiving hospital, and ideally within 24 hours, but should not be performed within the first 2 to 3 hours after administration of fibrinolytic therapy. *Although individual circumstances will vary, clinical stability is defined by the absence of low output, hypotension, persistent tachycardia, apparent shock, high-grade ventricular or symptomatic supraventricular tachyarrhythmias, and spontaneous recurrent ischemia.

Transfer of Patients With STEMI to a PCI-Capable Hospital for Coronary Angiography After Fibrinolytic Therapy I IIa. IIb III Immediate transfer to a PCI-capable hospital for coronary angiography is recommended for suitable patients with STEMI who develop cardiogenic shock or acute severe HF, irrespective of the time delay from MI onset. Urgent transfer to a PCI-capable hospital for coronary angiography is reasonable for patients with STEMI who demonstrate evidence of failed reperfusion or reocclusion after fibrinolytic therapy.

Importance of Time to Reperfusion Reinfarction Microvascular Reperfusion Myocardial Salvage
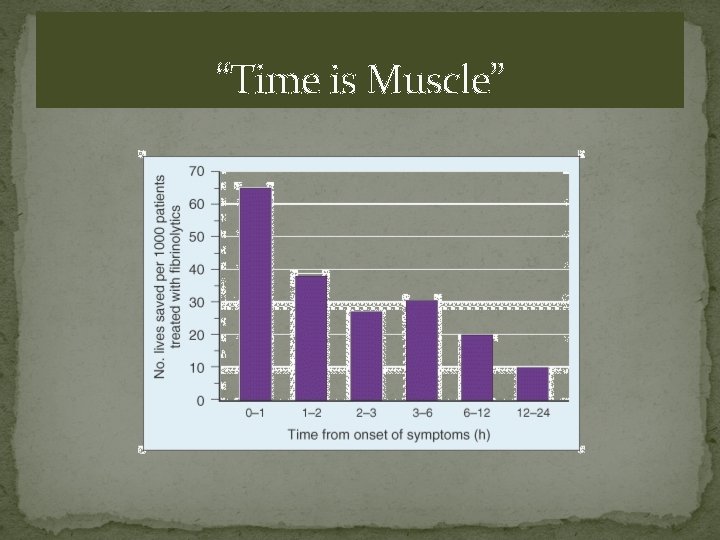
“Time is Muscle”
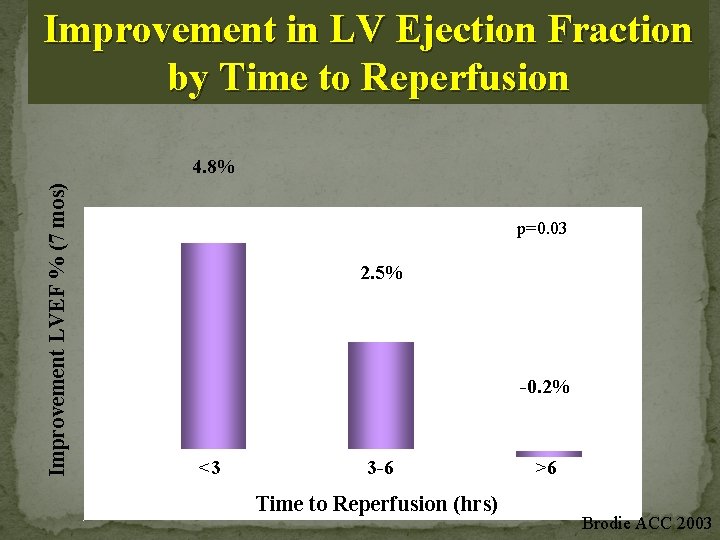
Improvement in LV Ejection Fraction by Time to Reperfusion Improvement LVEF % (7 mos) 4. 8% p=0. 03 5 2. 5% 4 3 2 -0. 2% 1 0 -1 <3 3 -6 Time to Reperfusion (hrs) >6 Brodie ACC 2003
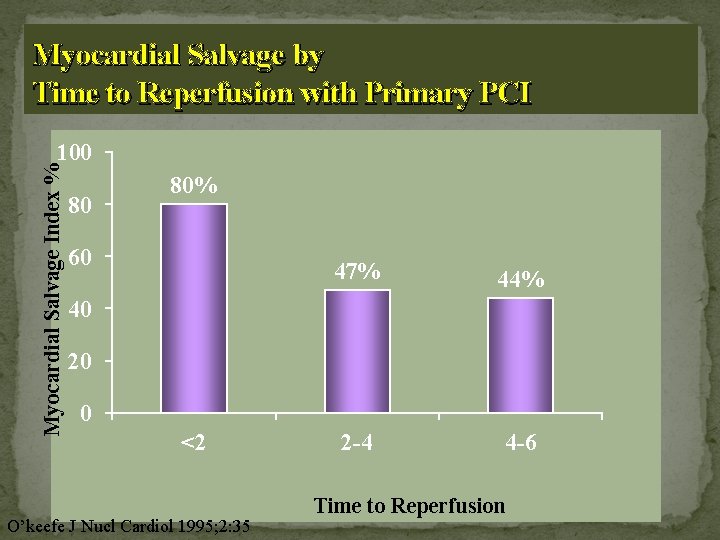
Myocardial Salvage by Time to Reperfusion with Primary PCI Myocardial Salvage Index % 100 80 80% 60 47% 44% 2 -4 4 -6 40 20 0 <2 O’keefe J Nucl Cardiol 1995; 2: 35 Time to Reperfusion
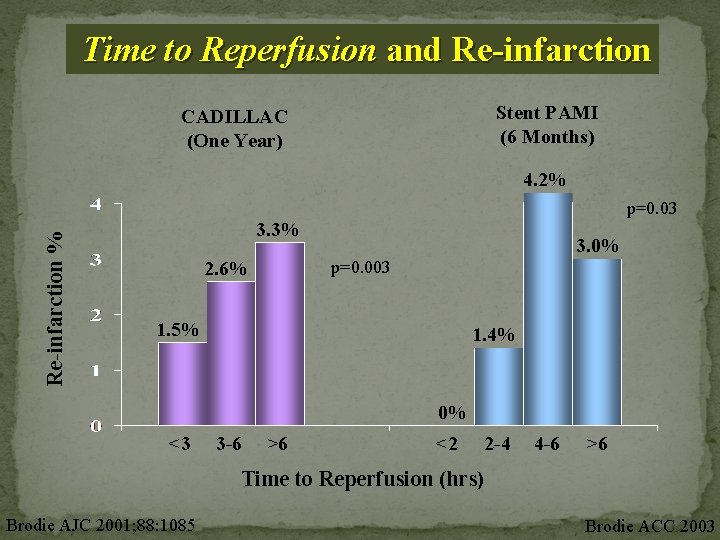
Time to Reperfusion and Re-infarction Stent PAMI (6 Months) CADILLAC (One Year) Re-infarction % 4. 2% p=0. 03 3. 3% 2. 6% 3. 0% p=0. 003 1. 5% 1. 4% 0% <3 3 -6 >6 <2 2 -4 4 -6 >6 Time to Reperfusion (hrs) Brodie AJC 2001; 88: 1085 Brodie ACC 2003
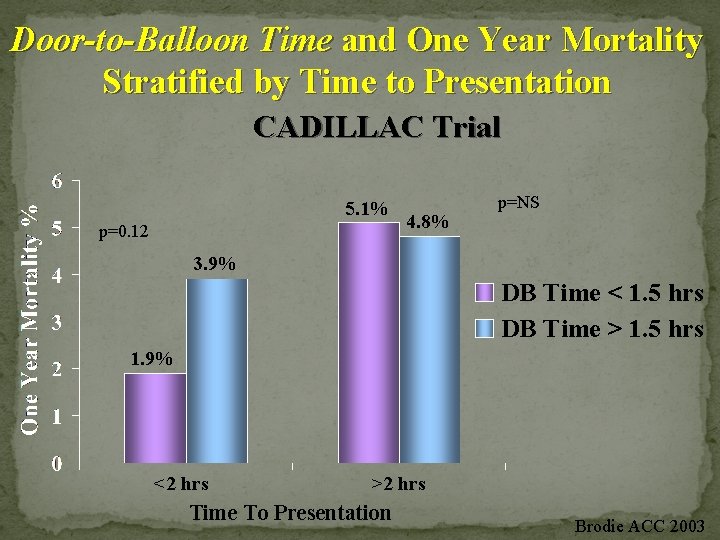
Door-to-Balloon Time and One Year Mortality Stratified by Time to Presentation CADILLAC Trial 5. 1% p=0. 12 4. 8% p=NS 3. 9% DB Time < 1. 5 hrs DB Time > 1. 5 hrs 1. 9% <2 hrs >2 hrs Time To Presentation Brodie ACC 2003
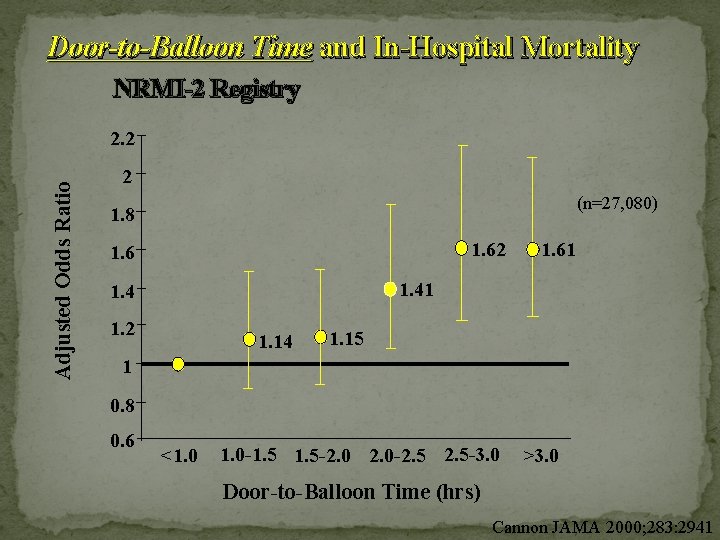
Door-to-Balloon Time and In-Hospital Mortality NRMI-2 Registry Adjusted Odds Ratio 2. 2 2 (n=27, 080) 1. 8 1. 62 1. 61 1. 4 1. 2 1. 14 1. 15 1 0. 8 0. 6 <1. 0 -1. 5 -2. 0 -2. 5 -3. 0 >3. 0 Door-to-Balloon Time (hrs) Cannon JAMA 2000; 283: 2941
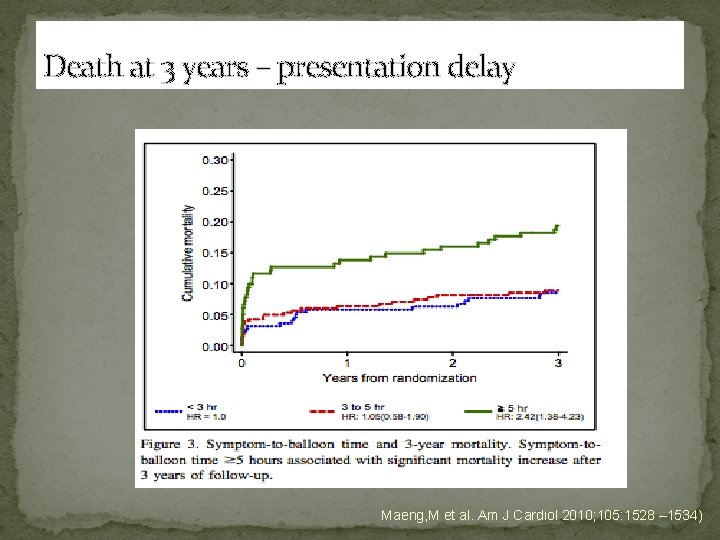
Death at 3 years – presentation delay Maeng, M et al. Am J Cardiol 2010; 105: 1528 – 1534)
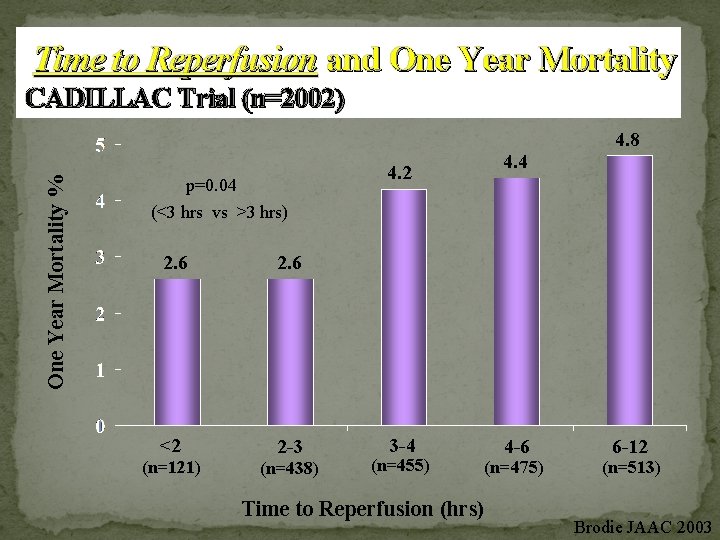
Time to Reperfusion and One Year Mortality % CADILLAC Trial (n=2002) 4. 4 4. 2 p=0. 04 4. 8 (<3 hrs vs >3 hrs) 2. 6 <2 2 -3 (n=121) (n=438) 3 -4 (n=455) 4 -6 (n=475) Time to Reperfusion (hrs) 6 -12 (n=513) Brodie JAAC 2003
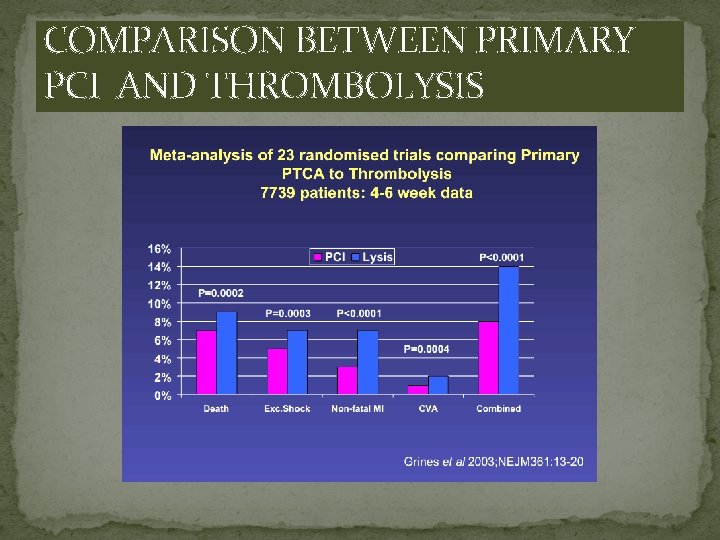
COMPARISON BETWEEN PRIMARY PCI AND THROMBOLYSIS
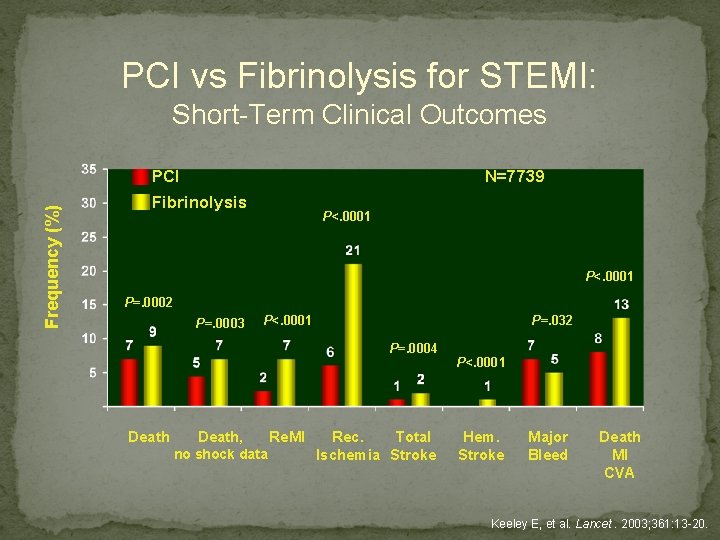
PCI vs Fibrinolysis for STEMI: Short-Term Clinical Outcomes Frequency (%) PCI N=7739 Fibrinolysis P<. 0001 P=. 0002 P=. 0003 P<. 0001 P=. 032 P=. 0004 Death, no shock data Re. MI Rec. Total Ischemia Stroke P<. 0001 Hem. Stroke Major Bleed Death MI CVA Keeley E, et al. Lancet. 2003; 361: 13 -20.
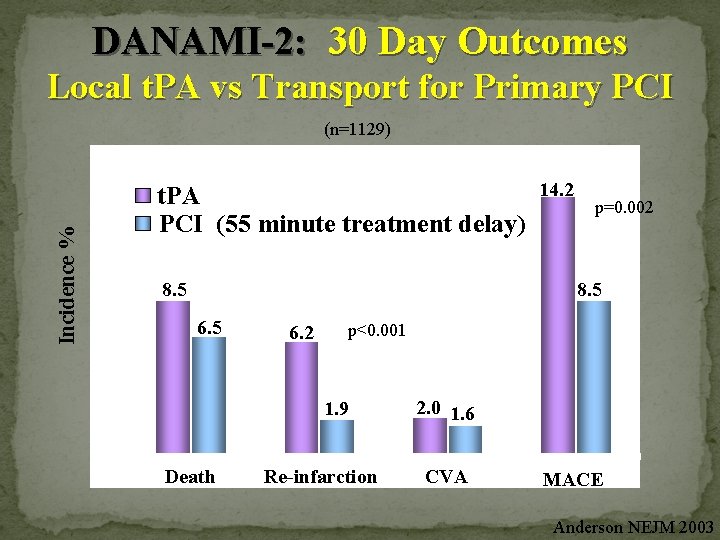
DANAMI-2: 30 Day Outcomes Local t. PA vs Transport for Primary PCI (n=1129) 16 Incidence % 14 12 10 8 6 t. PA PCI (55 minute treatment delay) 8. 5 14. 2 p=0. 002 8. 5 6. 2 p<0. 001 4 1. 9 2 2. 0 1. 6 0 Death Re-infarction CVA MACE Anderson NEJM 2003
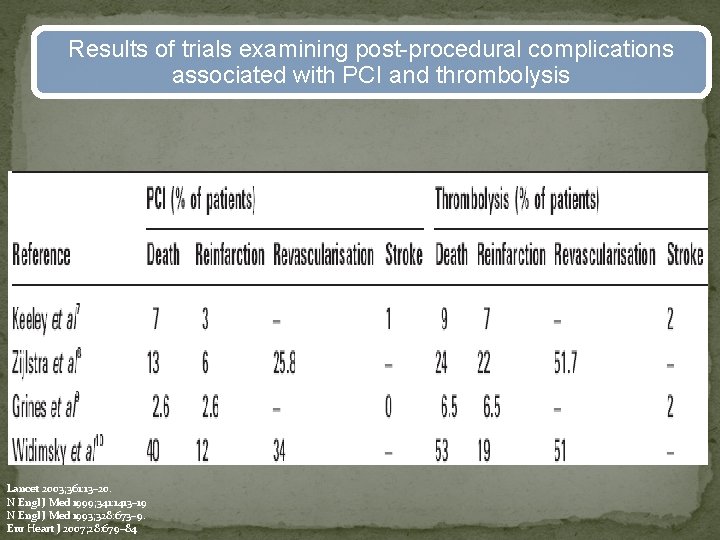
Results of trials examining post-procedural complications associated with PCI and thrombolysis Lancet 2003; 361: 13– 20. N Engl J Med 1999; 341: 1413– 19 N Engl J Med 1993; 328: 673– 9. Eur Heart J 2007; 28: 679– 84
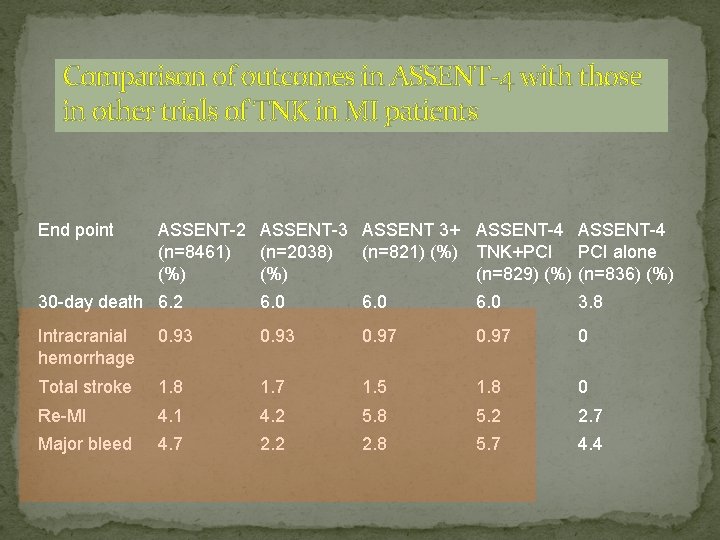
Comparison of outcomes in ASSENT-4 with those in other trials of TNK in MI patients End point ASSENT-2 ASSENT-3 ASSENT 3+ ASSENT-4 (n=8461) (n=2038) (n=821) (%) TNK+PCI alone (%) (n=829) (%) (n=836) (%) 30 -day death 6. 2 6. 0 3. 8 Intracranial hemorrhage 0. 93 0. 97 0 Total stroke 1. 8 1. 7 1. 5 1. 8 0 Re-MI 4. 1 4. 2 5. 8 5. 2 2. 7 Major bleed 4. 7 2. 2 2. 8 5. 7 4. 4

COMPARISON BETWEEN PRIMARY PCI AND FACILITATED PCI Mortality Lytic alone N=2953 IIb/IIIa alone N=1148 Lytic +IIb/IIIa N=399 All (N=4500) 1. 43 (1. 01 -2. 02) 1. 81 (1. 19 -2. 77) 1. 03 (0. 49 -2. 17) 1. 40 (0. 49 -3. 98) 3. 07 (0. 18 -52. 0) Fac. PCI Better Major Bleeding 1. 03 (0. 15 -7. 13) 1. 38 (1. 01 -1. 87) 0. 1 Keeley E, et al. Lancet 2006; 367: 579. Reinfarction 1. 71 (1. 16 - 2. 51) 1 10 0. 1 PPCI Better Fac. PCI Better 1. 51 (1. 10 - 2. 08 ) 1 10 PPCI Better 0. 1 Fac. PCI Better 1 10 PPCI Better
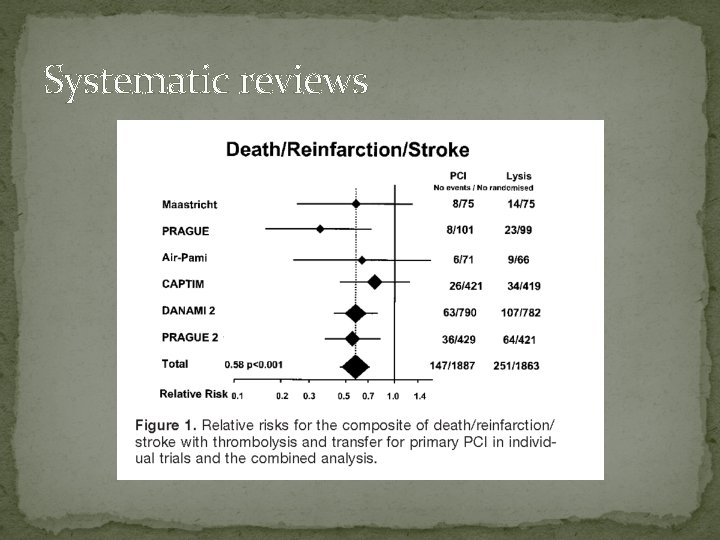
Systematic reviews
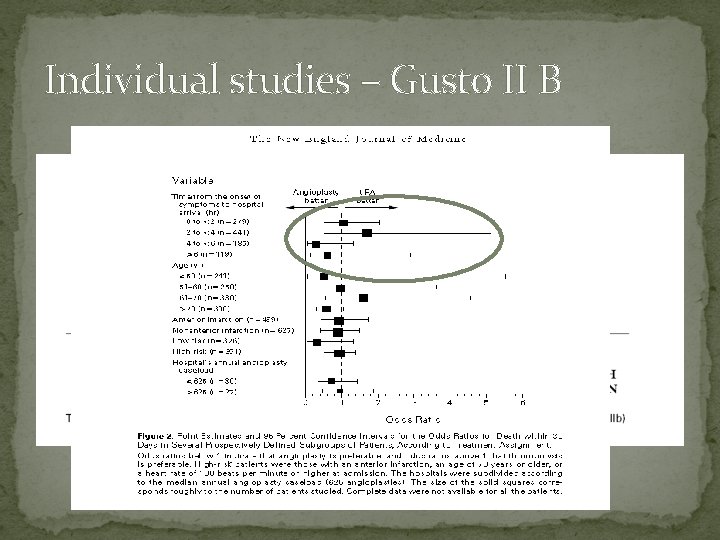
Individual studies – Gusto II B
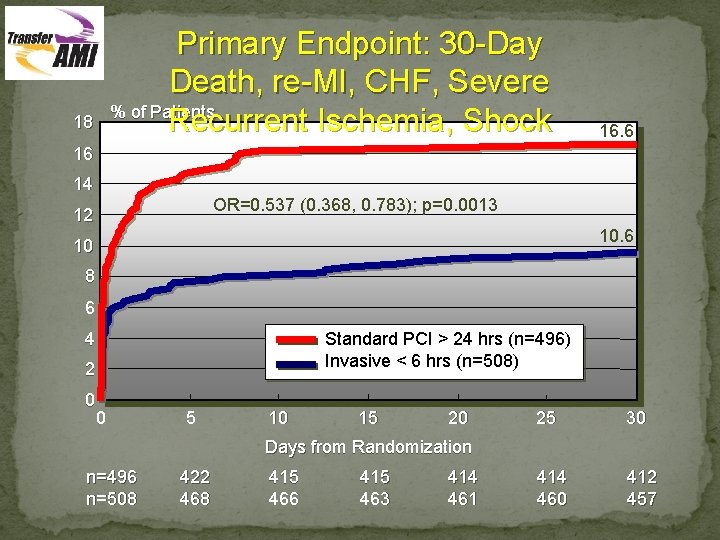
Primary Endpoint: 30 -Day Death, re-MI, CHF, Severe % of Patients Recurrent Ischemia, Shock 18 16. 6 16 14 OR=0. 537 (0. 368, 0. 783); p=0. 0013 12 10. 6 10 8 6 4 Standard PCI > 24 hrs (n=496) Invasive < 6 hrs (n=508) 2 0 0 5 10 15 20 25 30 414 460 412 457 Days from Randomization n=496 n=508 422 468 415 466 415 463 414 461

SUMMARY • PRIMARY PCI IS BETTER THAN THROMBOLYSIS. • DEFINITE MORTALITY BENEFIT WITH PRIMARY PCI. • COMPLICATIONS ARE LESS WITH PRIMARY PCI. • PUBLIC AWARENESS IS REQUIRED TO EXPLAIN THE IMPORTANCE OF PRIMARY PCI. • RESTORATION OF LV FUNCTION AND SALVAGE OF CARDIAC MUSCLE IS BEST WITH PRIMARY PCI.

THANK YOU
- Slides: 62