Primary and secondary prevention of osteoporotic fragility fractures


















- Slides: 21

Primary and secondary prevention of osteoporotic fragility fractures in postmenopausal women Implementing NICE guidance 2008 NICE technology appraisal guidance 160 and 161

What this presentation covers Definitions and scope Background Recommendations Costs and savings Discussion Find out more

Note: updated guidance NICE reviews each piece of guidance it issues. TA 161 replaces NICE technology appraisal guidance 87 issued in January 2005. The review and re-appraisal of alendronate, etidronate, risedronate, raloxifene and teriparatide for secondary prevention of osteoporotic fragility fractures has resulted in changes in the criteria for offering these drugs. In addition, strontium ranelate has also been appraised.

Definitions BMD: bone mineral density DXA: dual-energy X-ray absorptiometry Fragility fracture: a low-trauma fracture T-score: the number of standard deviations (SD) below the mean BMD of young adults at their peak bone mass Osteoporosis: a T-score of − 2. 5 (SD) or below on DXA scanning

Scope For the purposes of this guidance: • Primary prevention refers to opportunistic identification, during visits to a healthcare professional for any reason, of postmenopausal women who are at risk of osteoporotic fragility fractures and who could benefit from drug treatment. It does not imply a dedicated screening programme. • Secondary prevention relates only to treatments for the secondary prevention of fragility fractures in postmenopausal women who have osteoporosis and have sustained a clinically apparent osteoporotic fragility fracture.

Background In England Wales, it is estimated that: • over 2 million women have osteoporosis • 180, 000 osteoporosis-related fractures occur annually • 1 in 3 women over 50 years of age will sustain a vertebral fracture • 2 million bed days annually are a result of fractures • annual social and hospital care costs £ 1. 8 billion

Clinical need Fragility fractures are the clinically apparent outcome of osteoporosis. In the absence of fracture, osteoporosis is asymptomatic. Hip fractures are associated with increased mortality. 50– 70% of vertebral fractures do not come to clinical attention.

Risk factors and risk assessment Independent clinical risk factors for fracture: • parental history of hip fracture • alcohol intake of 4 or more units per day • rheumatoid arthritis. Indicators of low bone mineral density: • low body mass index below 22 kg/m 2 • ankylosing spondylitis • Crohn’s disease • conditions resulting in prolonged immobility • untreated premature menopause.

Technologies Alendronate, etidronate, risedronate (bisphonates) inhibitors of bone resporption and increase BMD by altering osteoclast activation and function. Raloxifene (selective oestrogen receptor modulator) SERMs have selective activity in various organ systems, acting as either a weak oestrogen-receptor agonist or antagonist. Strontium ranelate an element with properties similar to calcium with a dual effect on bone metabolism, increasing formation and decreasing resorption. Teriparatide (parathyroid hormone) a recombinant fragment of human parathyroid hormone which stimulates new formation of bone and increases resistance to fracture.

Adherence to treatment Contraindications Compliance with special instructions for administration Intolerance • • Bisphonates (alendronate, etidronate, risedronate) – persistent upper gastrointestinal disturbance that is sufficiently severe to warrant discontinuation of treatment, where instructions for administration have been followed correctly Strontium ranelate – persistent nausea or diarrhoea, which warrants discontinuation of treatment

Primary prevention: first treatment option Initial treatment offered: alendronate Postmenopausal women aged Independent Indicator of low Osteoporosis confirmed clinical risk factor BMD for fracture younger than 65 years 1 or more and at least one Required additional indicator 65– 69 years 1 or more n/a Required 70 years and older 1 or more or Yes Required In women ≥ 75 years: not required if two or more clinical risk factors or indicators of low BMD

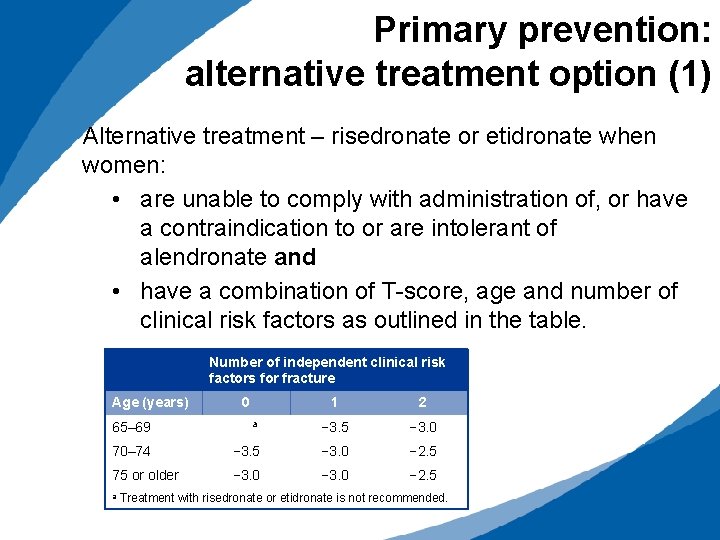
Primary prevention: alternative treatment option (1) Alternative treatment – risedronate or etidronate when women: • are unable to comply with administration of, or have a contraindication to or are intolerant of alendronate and • have a combination of T-score, age and number of clinical risk factors as outlined in the table. Number of independent clinical risk factors for fracture Age (years) 65– 69 0 a 1 2 − 3. 5 − 3. 0 70– 74 − 3. 5 − 3. 0 − 2. 5 75 or older − 3. 0 − 2. 5 a Treatment with risedronate or etidronate is not recommended.

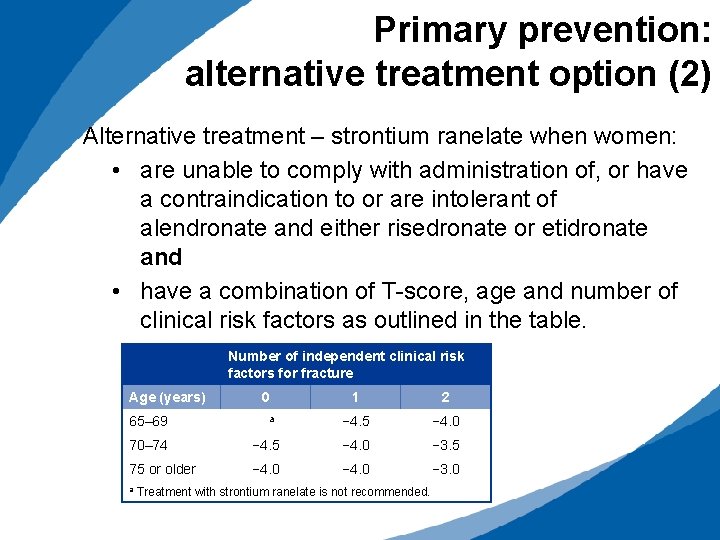
Primary prevention: alternative treatment option (2) Alternative treatment – strontium ranelate when women: • are unable to comply with administration of, or have a contraindication to or are intolerant of alendronate and either risedronate or etidronate and • have a combination of T-score, age and number of clinical risk factors as outlined in the table. Number of independent clinical risk factors for fracture Age (years) 65– 69 0 a 1 2 − 4. 5 − 4. 0 70– 74 − 4. 5 − 4. 0 − 3. 5 75 or older − 4. 0 − 3. 0 a Treatment with strontium ranelate is not recommended.

Secondary prevention: first treatment option Initial treatment offered: alendronate • Postmenopausal women with confirmed osteoporosis • A DXA scan may not be required in women aged 75 or over

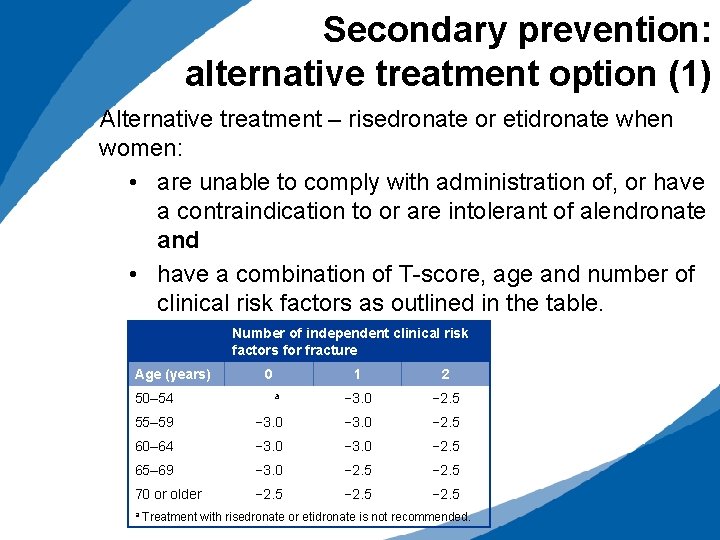
Secondary prevention: alternative treatment option (1) Alternative treatment – risedronate or etidronate when women: • are unable to comply with administration of, or have a contraindication to or are intolerant of alendronate and • have a combination of T-score, age and number of clinical risk factors as outlined in the table. Number of independent clinical risk factors for fracture Age (years) 50– 54 0 a 1 2 − 3. 0 − 2. 5 55– 59 − 3. 0 − 2. 5 60– 64 − 3. 0 − 2. 5 65– 69 − 3. 0 − 2. 5 70 or older − 2. 5 a Treatment with risedronate or etidronate is not recommended.

Secondary prevention: alternative treatment option (2) Alternative treatment – strontium ranelate or raloxifene when women: • are unable to comply with administration of, or have a contraindication to or are intolerant of alendronate and either risedronate or etidronate and • have a combination of T-score, age and number of clinical risk factors as outlined in the table. Age (years) 50– 54 55– 59 60– 64 65– 69 70– 74 75 or older a Number of independent clinical risk factors for fracture 0 1 2 a − 3. 5 − 4. 0 − 3. 5 − 3. 0 − 2. 5 Treatment with raloxifene or strontium ranelate is not recommended.

Secondary prevention: alternative treatment option (3) Alternative treatment – teriparatide when women: • are unable to take, have a contraindication to or are intolerant of alendronate and either risedronate or etidronate, or • have a contraindication to, or are intolerant of strontium ranelate or • have had an unsatisfactory response to treatment with alendronate, risedronate or etidronate and • have a combination of T-score, age and number of fractures as outlined in the table. Age (years) T-score Fractures > 65 years − 4. 0 SD or below – > 65 years − 3. 5 SD or below More than two 55– 64 years − 4 SD or below More than two

Clinical management Women currently receiving treatment that is not recommended in this guidance should have the option to continue treatment. It is assumed women who receive treatment have an adequate calcium intake and are vitamin D replete – consider supplements if needed.

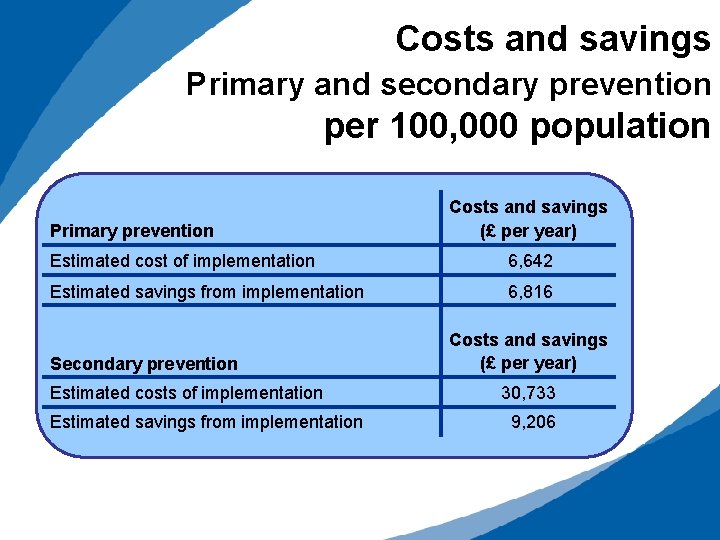
Costs and savings Primary and secondary prevention per 100, 000 population Primary prevention Costs and savings (£ per year) Estimated cost of implementation 6, 642 Estimated savings from implementation 6, 816 Secondary prevention Estimated costs of implementation Estimated savings from implementation Costs and savings (£ per year) 30, 733 9, 206

For discussion How/or will current local prescribing arrangements need to change as a result of this guidance? How can we increase adherence to therapy? What arrangements currently exist regarding access to DXA scanning for this patient group? How can we improve links between primary and secondary care to improve the care of women with osteoporosis?

Find out more Visit www. nice. org. uk/TA 160 and www. nice. org. uk/TA 161 for: • Other guidance formats • Costing report and template • Audit support