Preventing Readmission in the Sepsis Patient A MultiModal


















- Slides: 26

Preventing Readmission in the Sepsis Patient: A Multi-Modal Discharge National Framework (A Quality Improvement Initiative) Ron Yolo, MSN, MBA, RN Mary Ann Camilleri, JD, BSN, RN, FACHE

Introduction/ Problem Statement Sepsis and Sepsis Readmissions • Sepsis is a life threatening blood infection that affects 1 million hospitalized patients each year in the U. S. 1 • Leading cause of readmissions that represent $23. 7 billion of the healthcare spend 2, 3 • Main causes of readmission include re-infection and ineffective discharge coordination 4, 5 • Transitions of care interventions from other chronic diseases have proven effective to reduce readmissions 6 • A significant gap exists in sepsis-specific discharge interventions to prevent readmissions. U. S.

Significance of Addressing the Problem Sepsis Readmissions • #1 cause of hospital readmissions (12. 2%), costing $10, 070 per hospitalization in the U. S. 2 • 1 in 5 sepsis survivors are re-hospitalized within 30 days 5, 7 • Impaired Quality of Life for survivors and long term outcomes 8 • CMS: Hospital Inpatient Quality Reporting Program (HIQRP) • CMS: Hospital Readmissions Reduction Program (HRRP) Penalty Burden on healthcare system: Financial, Societal, and Humanitarian costs

Hospital Readmissions Reduction Program (HRRP) What is a readmission? “An admission to a hospital within 30 days of a discharge from the same or another hospital. ” 10 HRRP Measure Diagnoses: o Heart Attack (AMI) o Heart Failure (HF) o Pneumonia (PN) o Hip/Knee Surgery (THA/TKA) o Chronic Obstructive Pulmonary Disease (COPD) o Coronary Artery Bypass Graft Surgery (CABG) Sepsis is currently not part of the analysis

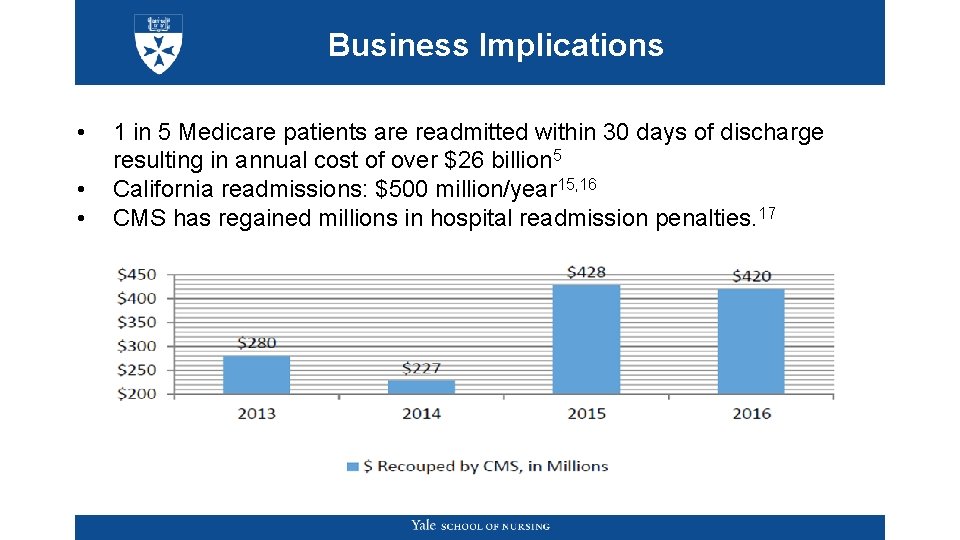
Business Implications • • • 1 in 5 Medicare patients are readmitted within 30 days of discharge resulting in annual cost of over $26 billion 5 California readmissions: $500 million/year 15, 16 CMS has regained millions in hospital readmission penalties. 17

Background/ Literature Review • Cross sectional study of sepsis readmissions 2008 -2011 -One-third of sepsis survivors in the U. S. are readmitted 10 • New emphasis should be directed to sepsis readmissions 11 • Deficiencies in care transition are a major cause of readmission • Effective discharge coordination strategies from other chronic disease proven to reduce readmissions 12 • Hospital driven interventions (education, telehealth, provider follow-up, patient contact) play a vital role in reducing readmissions 13 • No evidence-based comprehensive discharge models or frameworks available for sepsis patients.

Organizational SWOT Analysis Strengths • Merger with Catholic Health Initiatives (CHI); creating economies of scale • Leapfrog ’A’; 5 -Star Medicare Hospital • Improved Quality and Patient Safety/Experience metrics • Engaged clinical and medical staff Weakness • • Opportunities Explore more post-acute care relationships Innovate care delivery to create efficiencies within division hospitals Increase commercial payer mix Merger uncertainties Payer mix (High Medicaid) High acute care length of stays High number of community providers (splitters) Threats Standardization from the national office Increased consolidation the division level COVID-19 pandemic on

Sepsis Readmissions at Glendale Memorial Top 2 Index Admission DRGs for GMHHC Q 1 2018 - Q 4 201815 DRG Code Description N % 871 Septicemia or Severe Sepsis W/O MV >96 Hours W MCC 240 10. 4% 291 Heart Failure & Shock W MCC 150 6. 5% Top 2 Readmission DRGs for GMHHC Q 1 2018 - Q 4 201815 DRG Code Description N % 871 Septicemia or Severe Sepsis W/O MV >96 Hours W MCC 50 12. 0% 291 Heart Failure & Shock W MCC 48 11. 5%

Overall Project Goal Primary Goal: Demonstrate 30 -day reduction of readmitted patients, previously discharged with a primary sepsis diagnosis, through implementation of a multi-modal discharge framework. Aim 1: Developed a Multi-Modal Discharge Framework to Reduce Sepsis Readmissions Aim 2: Implemented and Evaluated the Yolo Framework in Reducing Sepsis Readmissions Aim 3: Recommend for Sustainability and Scalability of the Discharge Framework

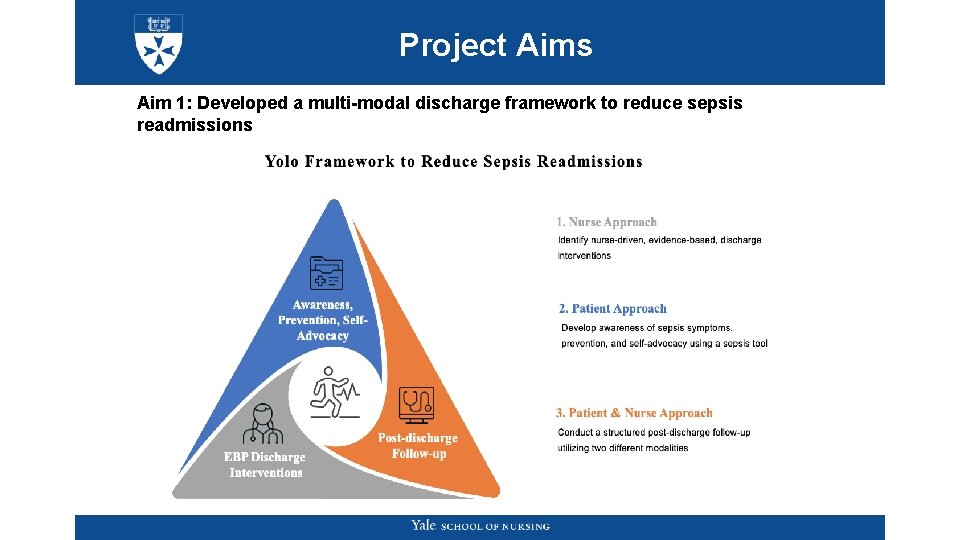
Project Aims Aim 1: Developed a multi-modal discharge framework to reduce sepsis readmissions

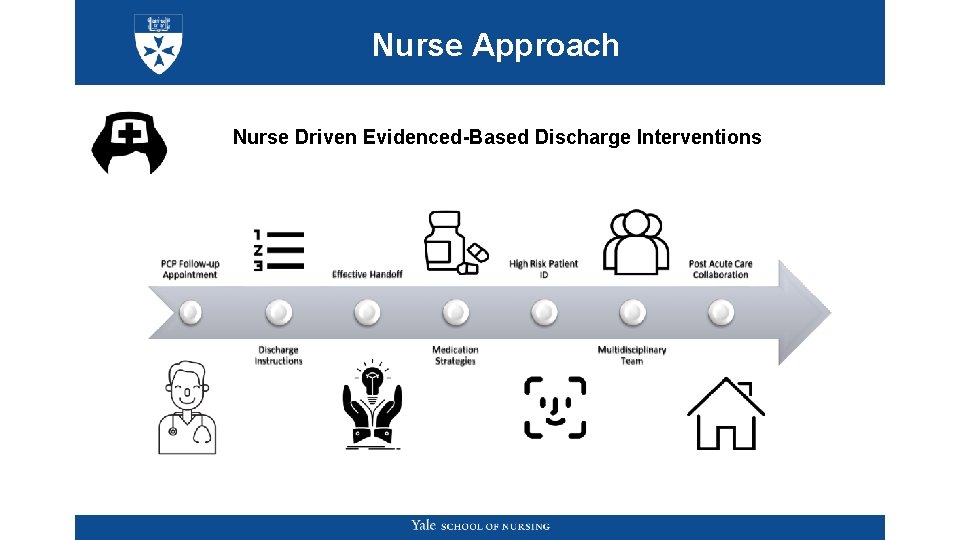
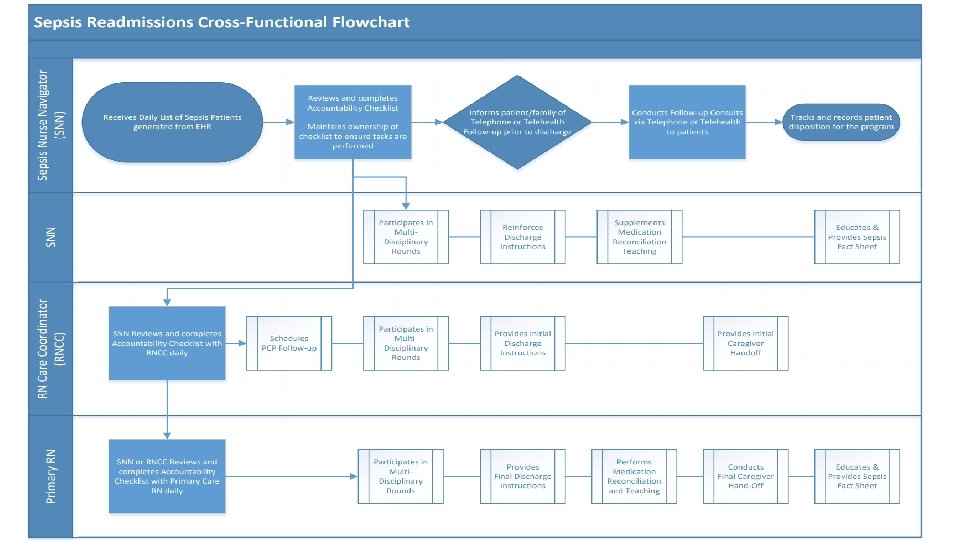
Nurse Approach Nurse Driven Evidenced-Based Discharge Interventions

Patient Approach Developed awareness of sepsis symptoms, prevention, and selfadvocacy using an expert-validated sepsis tool

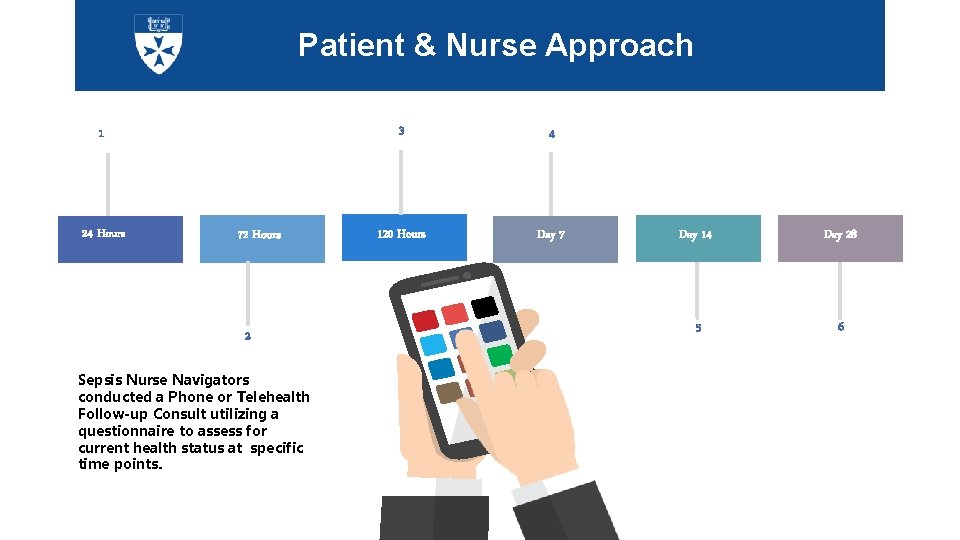
Patient & Nurse Approach 1 24 Hours 72 Hours 2 Sepsis Nurse Navigators conducted a Phone or Telehealth Follow-up Consult utilizing a questionnaire to assess for current health status at specific time points. 3 4 120 Hours Day 7 Day 14 Day 28 5 6

Evaluation

Project Aims Aim 2: Implemented and Evaluated the Yolo Framework in Reducing Readmissions Clinical Group: • Convenience sample of 75 patients with CMS Diagnosis Related Group (870, 871, 872) discharging to home or to an assisted living facility • Observed for 6 months (July-December) • Accessed patient demographics, clinical, and hospitalization data through EHR report Evaluation # 1 Patient and Nurse Satisfaction Survey • Descriptive statistics to determine patient and nurse satisfaction through administration of survey post participation Evaluation # 2 Readmission Data Comparison: • Comparative analysis of baseline and project outcome data • Baseline Data: Retrospective review of the number of sepsis readmissions from 2015 -2019 using DRGs (870 -872) from the same time period (July-December).

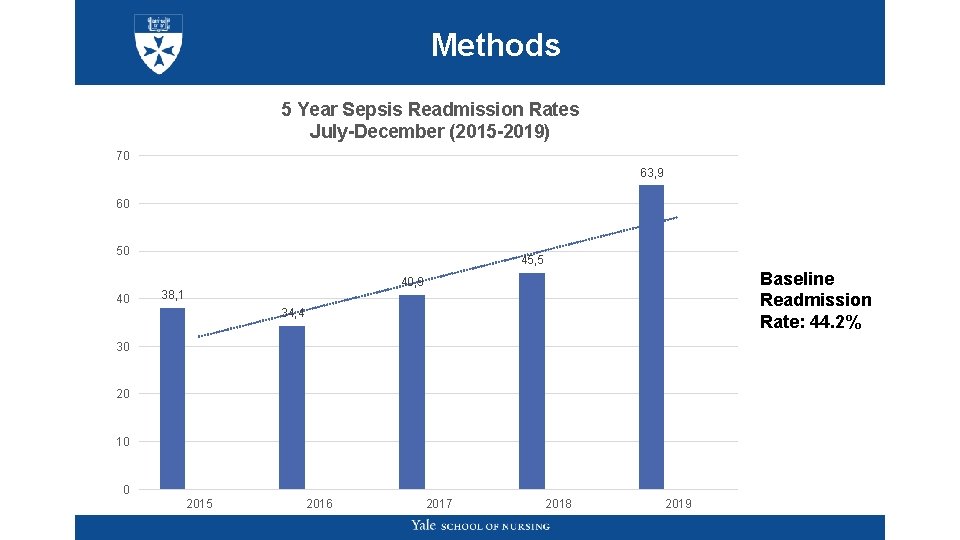
Methods 5 Year Sepsis Readmission Rates July-December (2015 -2019) 70 63, 9 60 50 40 45, 5 Baseline Readmission Rate: 44. 2% 40, 9 38, 1 34, 4 30 20 10 0 2015 2016 2017 2018 2019

Methods Clinical Question: To what extent is there a reduction in the readmission rate of sepsis patients after implementation of a multi-modal framework (that aims to address quality and operational inefficiencies that might occur during care transitions)? Analyzed two variables P 0 = the proportion of sepsis patients who were readmitted within 30 days before implementation of the framework P 1 = the proportion of sepsis patients who were readmitted within 30 days after implementation of the framework P 0 and P 1 = are defined in statistical terms as the number of events of interest (i. e. the number of patients who were readmitted within 30 days) divided by the number of trials (i. e. the total number of patients with sepsis, including those who were not readmitted) P 0 and P 1 = measured over known periods of time, defined as rates of readmission Z-test statistic was utilized; the one-tailed p-value of the Z test statistic was computed.

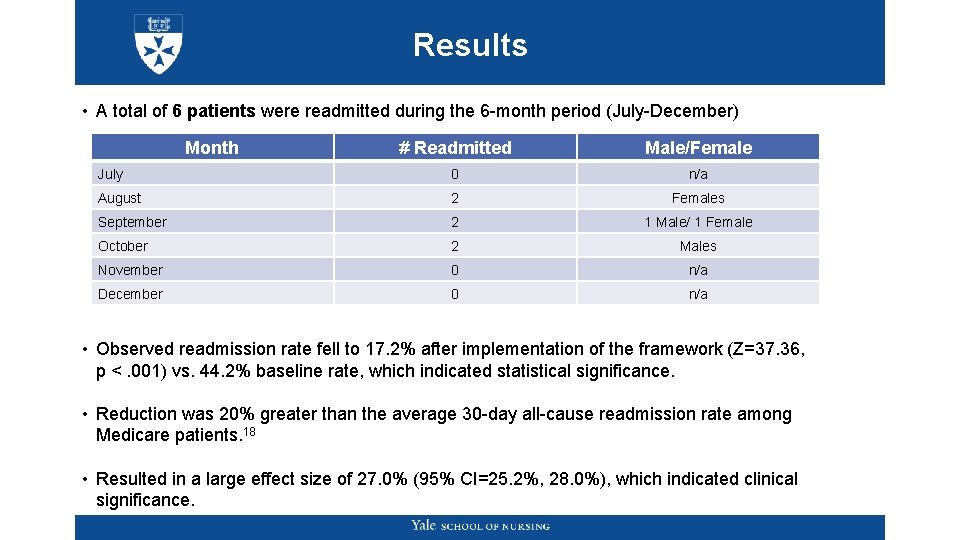
Results • A total of 6 patients were readmitted during the 6 -month period (July-December) Month # Readmitted Male/Female July 0 n/a August 2 Females September 2 1 Male/ 1 Female October 2 Males November 0 n/a December 0 n/a • Observed readmission rate fell to 17. 2% after implementation of the framework (Z=37. 36, p <. 001) vs. 44. 2% baseline rate, which indicated statistical significance. • Reduction was 20% greater than the average 30 -day all-cause readmission rate among Medicare patients. 18 • Resulted in a large effect size of 27. 0% (95% CI=25. 2%, 28. 0%), which indicated clinical significance.

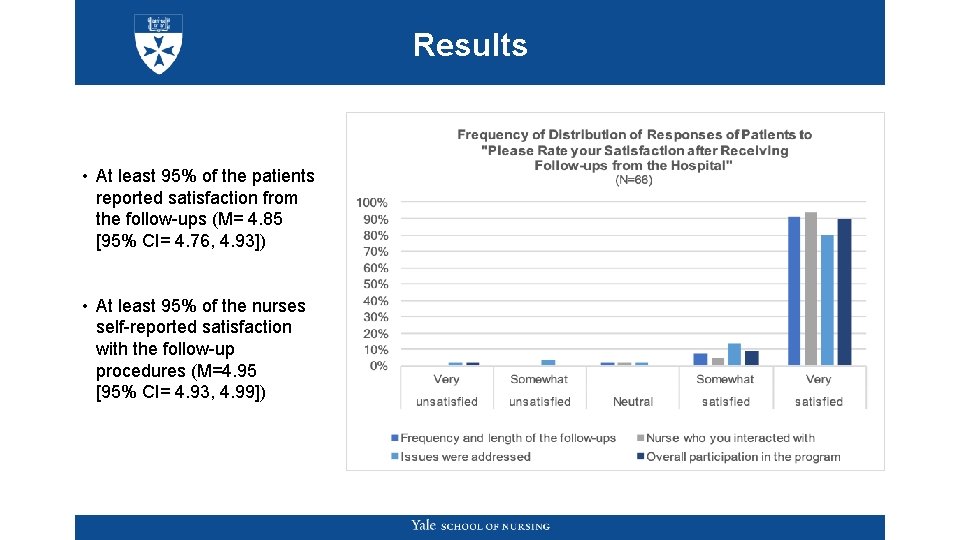
Results • At least 95% of the patients reported satisfaction from the follow-ups (M= 4. 85 [95% CI= 4. 76, 4. 93]) • At least 95% of the nurses self-reported satisfaction with the follow-up procedures (M=4. 95 [95% CI= 4. 93, 4. 99])

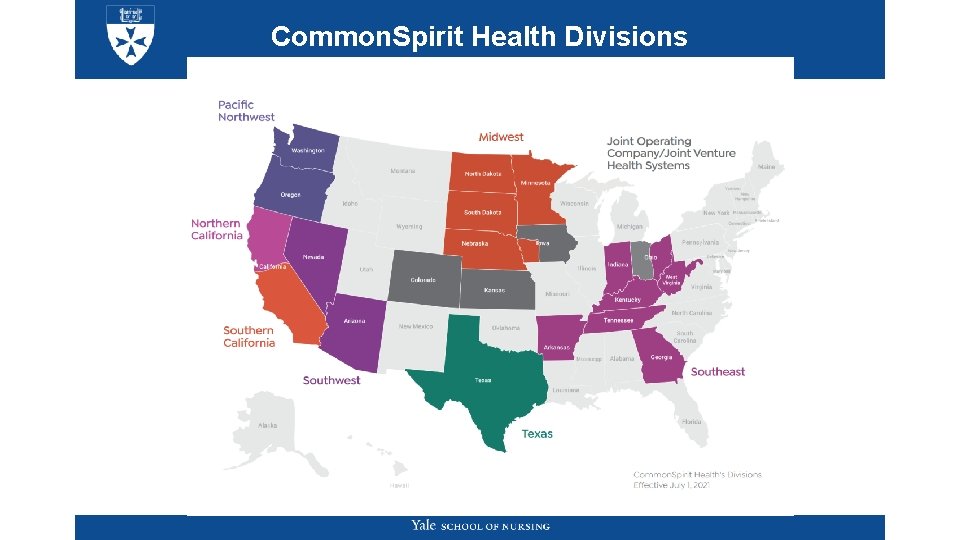
Scaling & Sustainability Plans Aim 3: Recommend for Sustainability and Scalability of the Yolo Framework Successes: • Patients and families extremely receptive towards follow-up activities • Stakeholder engagement Limitations/Opportunities: • Decreased inpatient volume due to COVID-19; readmission rate may be underestimated • Explore inclusion of skilled nursing facility patients to determine framework robustness and applicability • Potential improvements in the sepsis discharge model of care suggested, including COVID 19 education. • Framework refinement for sustainability, integration, resource and time allocation, and program adjustment • Results will be vetted among stakeholders for consideration for scalability in the Southern California hospitals (18 hospitals) and nationally.

Common. Spirit Health Divisions

Implications for Healthcare • An estimated cost savings of $700, 000 was projected for those patients not readmitted during the project phase. This impact extends to significant cost reduction for US healthcare systems • Underscores the importance of allocating resources (Sepsis Nurse Navigators) to address a significant disease process • The high patient and nurse satisfaction rates highlight the magnitude and value of the model. Patient and nurse navigation through the complexities of the healthcare system • DNP project contributes to the body of knowledge in sepsis care, provides an evidencebased discharge framework and interventions to prevent hospital readmissions.

References 1 Martin G. S. (2012). Sepsis, severe sepsis and septic shock: changes in incidence, pathogens and outcomes. Expert review of anti-infective therapy, 10(6), 701– 706. Doi: 10. 1586/eri. 12. 50 2 Mayr F. B. , Talisa V. B. , Balakumar V. , Chang C. H. , Fine M. , Yende S. (2017). Proportion and cost of unplanned 30 -day readmissions after sepsis compared with other medical conditions. Journal of American Medical Association, 317 (5), 530– 531. Doi: 10. 1001/jama. 2016. 20468 3 Torio, C. , Moore, B. (2016). National inpatient hospital costs: The most expensive conditions by payer, 2013. Agency for Healthcare Research and Quality. Retrieved from http: //www. hcup-us. ahrq. gov/reports/statbriefs/sb 204 -Most. Expensive-Hospital -Conditions. pdf. 4 Prescott, H. C. , Langa, K. M. , & Iwashyna, T. J. (2015). Readmission diagnoses after hospitalization for severe sepsis and other acute medical conditions. JAMA, 313(10), 1055– 1057. Doi: 10. 1001/jama. 2015. 1410 5 Shankar-Hari, M. (2020). Rate and risk factors for rehospitalisation in sepsis survivors: Systematic review and meta-analysis. Intensive care medicine, 46, 619 -636. https: //doi. org/10. 1007/s 00134 -019 -05908 -3 6 Kamer Mayer, A. K. , Leasure, A. R. , & Anderson, L. (2017). The effectiveness of transitions-of-care interventions in reducing hospital readmissions and mortality a systematic review. Dimensions of Critical Care Nursing, 36, 311 -316. Doi: 10. 1097/dcc. 0000000266

References 7 Singer, M. , Deutschman, C. S. , Seymour, C. , Shankar-Hari, M. , Annane, D. , Bauer, M. , . . . Angus, D. C. (2016). The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA – Journal of the American Medical Association, 315(8), 801 -810. Doi: 10. 1001/jama. 2016. 0287 8 Winters BD, Eberlein M, Leung J, Needham DM, Pronovost PJ, & Sevransky JE. (2010). Long-term mortality and quality of life in sepsis: a systematic review. Critical Care Medicine, 38(5), 1276– 1283. https: //doi. org/10. 1097/CCM. 0 b 013 e 3181 d 8 cc 1 d 9 Genga K, R, Russell J, A. (2017). Update of sepsis in the intensive care unit. Journal of Innate Immunity. 9, 441 -455. doi: 10. 1159/000477419 10 Centers for Medicare & Medicaid Services. (2019). Hospital Readmissions Reduction Program. Retrieved from https: //www. cms. gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/Value-Based-Programs/HRRP/Hospital. Readmission-Reduction-Program. html 11 Norman, B. , Cooke, C. , Ely, W. , Graves, J. (2017). Sepsis associated 30 -day risk standardized readmissions: Analysis of a nationwide Medicare sample. Critical Care Medicine, 45, 1130 -1137. Doi: 10. 1097/CCM. 0000002476 12 Chang, D. W. , Tseng, C. H. , & Shapiro, M. F. (2015). Rehospitalizations following sepsis: Common and costly. Critical Care Medicine, 43, 2085 -2093. Doi: 10. 1097/ccm. 0000001159 13 Di Palo, K. E. , Patel, K. , Assafin, M. , & Pina, I. L. (2017). Implementation of a patient navigator program to reduce 30 -day heart failure readmission rate. Progress in Cardiovascular Diseases, 60, 259 -266. Doi: 10. 1016/j. pcad. 2017. 004

References 14 Leppin, A. L. , Gionfriddo, M. R. , Kessler, M. , Brito, J. P. , & Mair, F. S. Preventing 30 -day hospital readmissions: A systematic review and meta-analysis of randomized trials. JAMA internal medicine, 174, 1095 -1107. doi: 10. 1001/jamainternmed. 2104. 1608 15 Health Services Advisory Group. (2019). Medicare Fee-For-Service (FFS) Hospital Readmissions: Q 1 2018 - Q 4 2018. State of California. Glendale Memorial Hospital & Health Center. 16 National Inpatient Hospital Costs: The Most Expensive Conditions by Payer, 2013. 17 HCUP Statistical Brief #204. May 2016. Agency for Healthcare Research and Quality, Rockville, MD. Retrieved from http: //www. hcup-us. ahrq. gov/reports/statbriefs/sb 204 -Most. Expensive-Hospital-Conditions. pdf 18 Bailey, et al. (2019). Characteristics of 30 -day all-cause readmissions. Healthcare Cost and Utilization Project.

Questions?