Pretranfusion Compatibility Testing Mr Mohammed A Jaber Blood

Pretranfusion Compatibility Testing Mr. Mohammed A. Jaber
Blood Transfusion Process Pre-transfusion Transfusion Post-transfusion

? What is compatibility testing Also called pretransfusion testing Purpose: To select blood components that will not cause harm to the recipient and will have acceptable survival when transfused If properly performed, compatibility tests will confirm ABO compatibility between the component and the recipient and will detect the most clinically significant unexpected antibodies

? Compatibility testing There are several components of compatibility testing Proper specimen collection Reviewing patient transfusion history ABO, Rh, and antibody testing (screen/ID) Crossmatching Actual transfusion

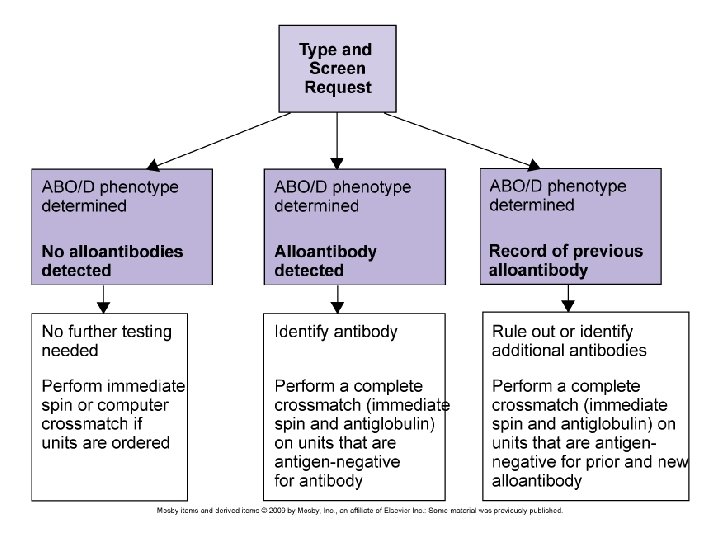
Compatibility testing Can be divided into 3 categories: Preanalytical procedures Serological testing Postanalytical procedures

Pre-analytical phases Patient identification Specimen collection Review of patient history
Patient Identification Must confirm recipient’s ID from bracelet ON the patient Full patient name and hospital number Name of physician

Sample Identification The sample should also have the full patient name, hospital number, and physician Date and time of collection, phlebotomist’s initials All of this should be on the request form and the sample
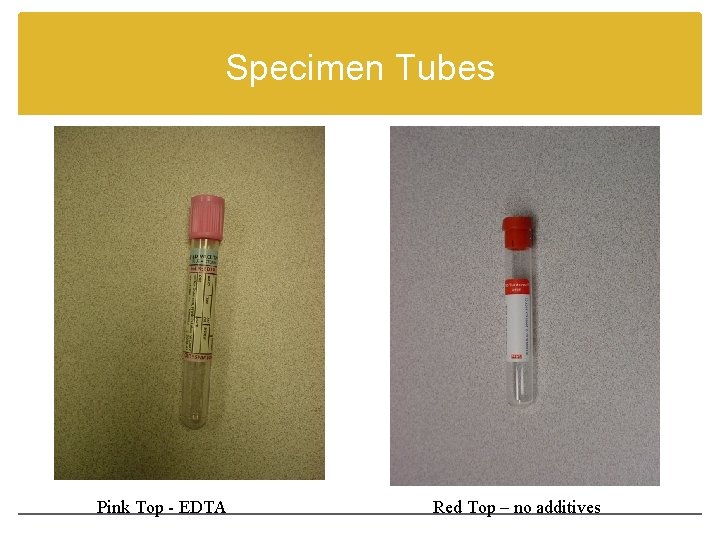
Specimen Tubes Pink Top - EDTA Red Top – no additives

Specimen Collection Collected in tube with EDTA or no additives If the venipuncture causes hemolysis, the sample may be rejected True hemolysis in the patient is the result of complement activation Samples are labeled at the bedside (pre-labeling is not recommended) A record of individuals who collect (or test) the specimens should be documented in order to “backtrack” in case of an error

Specimen Collection If the sample is drawn from an IV line, the IV infusion should be stopped 5 -10 minutes prior to blood drawing and the first 10 m. L discarded Testing should be performed on samples less than 72 hours or else complement dependent antibodies may be missed (complement can become unstable)

Getting the history Look at recipient’s records for any prior unexpected antibodies Previous transfusion reactions

Serological Testing 3 tests: ABO/Rh Antibody detection/identification Crossmatch

ABO/Rh Typing In the ABO typing, the forward and reverse MUST match In the Rh typing, the control must be negative Both of these will indicate what type of blood should be given

Antibody screen and/or ID The antibody screen will detect the presence of any unexpected antibodies in patient serum If antibodies are detected, identification should be performed using panel cells (with an autocontrol) IS 37° (LISS) AHG If an antibody is present, units negative for the antigen must be given Proceed to the crossmatch…

Crossmatching Purpose: Prevent transfusion reactions Increase in vivo survival of red cells Double checks for ABO errors Another method of detecting antibodies

Crossmatch Two types of crossmatches Major – routinely performed in labs Minor – not required by AABB since 1976
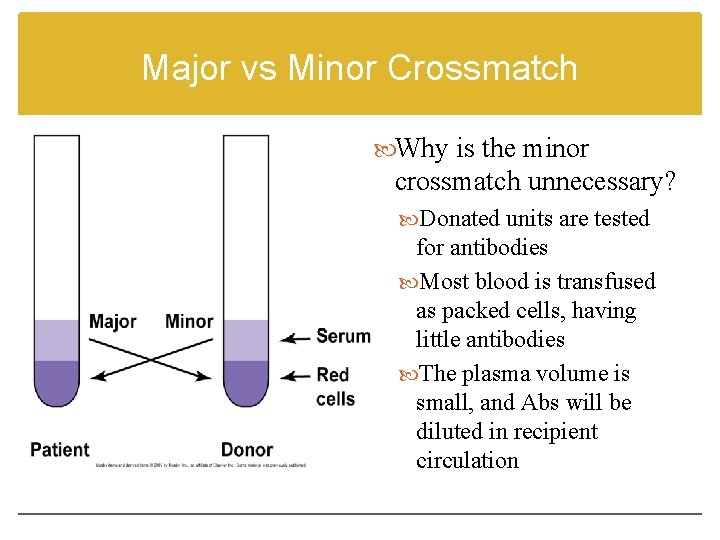
Major vs Minor Crossmatch Why is the minor crossmatch unnecessary? Donated units are tested for antibodies Most blood is transfused as packed cells, having little antibodies The plasma volume is small, and Abs will be diluted in recipient circulation

Crossmatches The crossmatch “shall use methods that demonstrate ABO incompatibility and clinically significant antibodies to red cell antigens and shall include an antiglobulin phase”
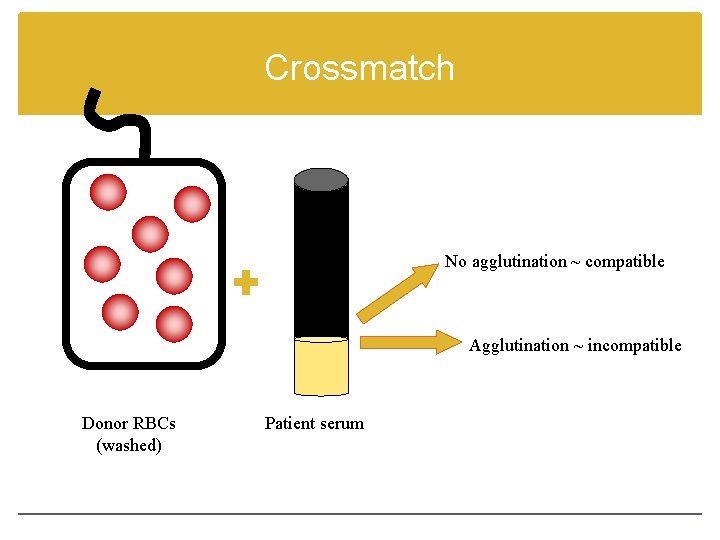
Crossmatch No agglutination ~ compatible Agglutination ~ incompatible Donor RBCs (washed) Patient serum

The procedure Donor cells are taken from segments that are attached to the unit itself Segments are a sampling of the blood and eliminate having to open the actual unit

Units of whole blood with segments attached

Procedure ABO/Rh typing is FIRST performed Antibody Screen is performed next….

Crossmatch Procedure if antibodies are NOT detected: Only immediate spin (IS) is performed using patient serum and donor blood suspension This fulfills the AABB standard for ABO incompatibility This is an INCOMPLETE CROSSMATCH If antibodies ARE detected: Antigen negative units found and X-matched All phases are tested: IS, 37°, AHG This is a COMPLETE CROSSMATCH

…Crossmatches Will Verify donor cell ABO compatibility Detect most antibodies against donor cells Will Not Guarantee normal survival of RBCs Prevent patient from developing an antibody Detect all antibodies Prevent delayed transfusion reactions Detect ABO/Rh errors
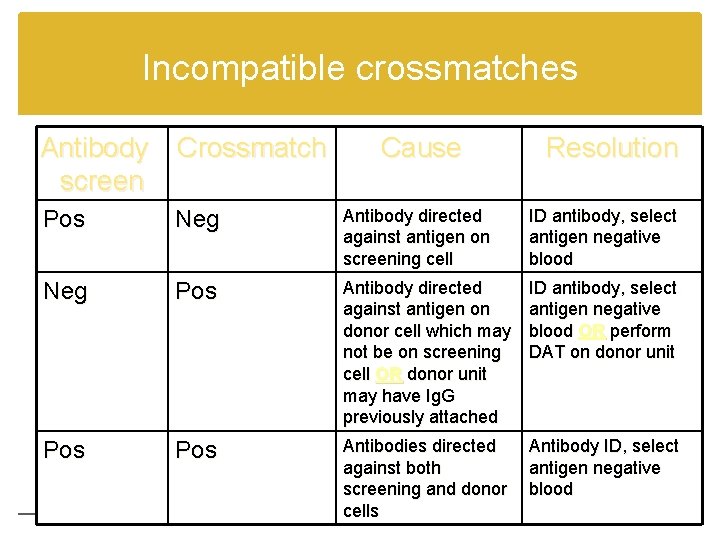
Incompatible crossmatches Antibody Crossmatch screen Cause Resolution Pos Neg Antibody directed against antigen on screening cell ID antibody, select antigen negative blood Neg Pos Antibody directed against antigen on donor cell which may not be on screening cell OR donor unit may have Ig. G previously attached ID antibody, select antigen negative blood OR perform DAT on donor unit Pos Antibodies directed against both screening and donor cells Antibody ID, select antigen negative blood

Additional Information on Types of Compatibility Tests Manual (IS and IAT) Gel Technology Electronic (Computerized) Cross match Red cell Affinity Column Technology (Re. ACT) Solid Phase Adherence Assays (SPAA)
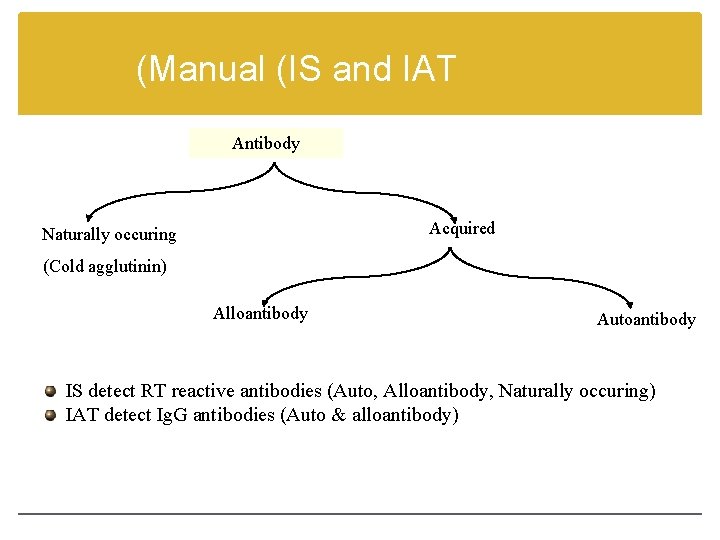
(Manual (IS and IAT Antibody Acquired Naturally occuring (Cold agglutinin) Alloantibody Autoantibody IS detect RT reactive antibodies (Auto, Alloantibody, Naturally occuring) IAT detect Ig. G antibodies (Auto & alloantibody)
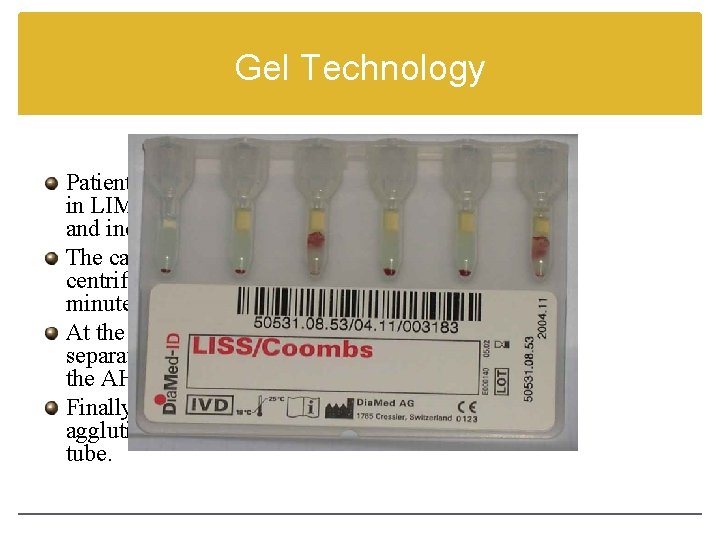
Gel Technology Patient serum, and 1% of suspended RBCs in LIM are dispensed into the microtube o and incubated at 37 C for 15 minutes. The card containing the microtubes is then centrifuged at a controlled speed for 10 minutes. At the start of centrifugation the cells are separated from the serum; then they meet the AHG contained in the microtube. Finally the cells are trapped by the gel (if agglutinated) or pellet to the bottom of the tube.

…New Technologies The electronic crossmatch According to the AABB, the following must be fulfilled: Critical elements of the information system have been validated on-site. No clinically significant antibodies are detected in the current blood sample and there is no record of clinically significant antibodies in the past

(Computer crossmatch (cont’d The patient's ABO group and Rh type has been done twice and entered in the computer The donor ABO/Rh have been confirmed and entered in the computer. The donor unit identification number, component name, and ABO/Rh type must also be entered in the computer The computer system will alert the technologist to ABO & Rh discrepancies between information on the donor label and results of donor confirmatory testing

Red Cell Affinity Column Technology (Re. ACT) Based on affinity adherence of coated red cells in an immunologically active matrix. Antibody- sensitized red cells bind or adsorbed to ligands attached to an agarose matrix. The main ligand is Protein G (prepared from Group C or G Streptococcus or by recombinant technology), which has high affinity for all four Ig. G subclasses. Another Re. ACT ligand is Protein A (from Group A Staphlococcus), which binds to Ig. G 1, 2, and 4.

Red Cell Affinity Column Technology (Re. ACT) Positive reaction: the coated red blood cells with Ig. G are boud to immunoreactive gel particles, occurs mostly at the top of the gel column. Negative reaction: the red blood cells are not coated with antibody and pass through to the bottom of the gel column.

Solid Phase Adherence Assays (SPAA) Uses red cell membrane bound to the surfaces of polystyrene microtitration strip wells, capturing Ig. G antibodies (if present) in patient sera. Patient serum is added to wells coated with screen cells Incubated at 37 o. C for 15 min. Washing anti-Ig. G-coated indicator red cells are added. centrifuge
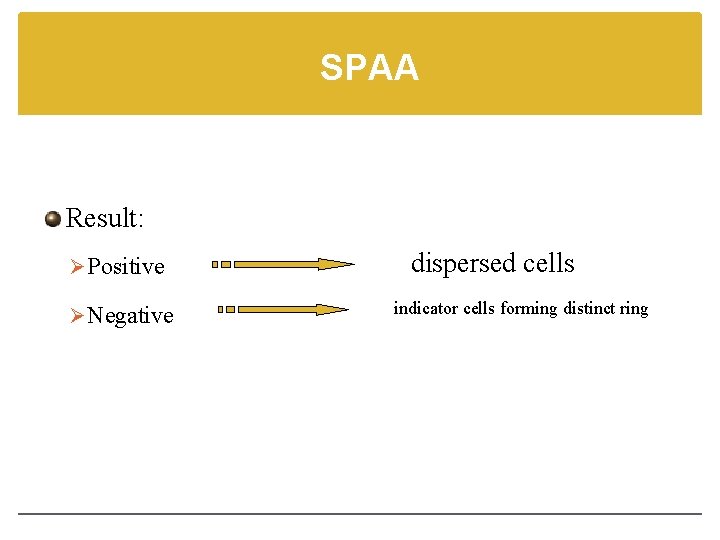
SPAA Result: Ø Positive Ø Negative dispersed cells indicator cells forming distinct ring

Major Crossmatch Tests It is done both for Ig. M and Ig. G antibodies Requirement: 1. Recipient’s serum. 2. Donor’s red cells taken from the tube attached to the bag. A. Saline technique is designed to detect compatibility of Ig. M antibody(ies) in patient’s serum against antigens on donor’s red cells.

Method 1. Label 1 tube for each donor sample to be tested. 2. Put 2 drop of patient’s serum in labeled tube. 3. Add 1 drop of 2 -5% saline suspended red cells of 4. 5. donor Mix and incubate for 5 -10 min. (spin method) or incubate for 30 -60 min (sedimentation method) at RT. Centrifuge at 1000 rpm for 1 min. in spin method (after 5 -10 min. incubation); centrifugation is optional in sedimentation method.

6. Read the result, observe for hemolysis and agglulination. 7. Negative result should be confirmed under microscope. Interpretation Agglutination or hemolysis indicates a positive result (incompatible) Note: In emergency spin technique is acceptable. Saline technique is inadequate as a complete compatibility test because it is inadequate to detect clinically significant Ig. G antibodies.

Crossmatch Test for Ig. G Antibody(ies) B. Anti -Human Globulin Test (IAT) Indirect anti human globulin test (IAT) is the most important and widely used serological procedure in modern blood banking to test the Ig. G compatibility between recipient’s serum and donor’s cells. The majority of incomplete antibodies are Ig. G and are detected by AHG test.

Method 1. Put 2 drops of patient’s serum in a labeled tube. 2. Add 1 drop of 2 -5 % saline suspended red cells of 3. 4. 5. donor. Incubate for 30 -60 min at 37° C Centrifuge at 1000 rpm for 1 min, check for hemolysis/agglutination If there is no hemolysis/agglutination, wash the cells three times with normal saline.

6. Perform IAT test • Add 2 drops of polyspecific AHG serum to washed cells • Centrifuge at 1000 rpm for 1 minute • See for agglutination 7. Add Ig. G coated red cells to negative AHG test. 8. Centrifuge and check for agglutination - if there is no agglutination test is invalid.

Interpretation Hemeolysis or agglutination at any stage indicates incompatibility. Note: Cross-match can be done by two tubes technique for Ig. M and Ig. G separately as described above or by one tubes in which donor’ cell and the patient’s serum after step 5 in saline technique is incubated at 37°C for 20 -30 minutes and then do IAT. In major-cross for Ig. G antibodies albumin or enzyme or LISS can be used with IAT to increase sensitivity. For techniques see chapter on Antiglobulin Test.
- Slides: 43