PRETERM LABOR Overview Definition Diagnosis Management Screening Prevention
PRETERM LABOR § Overview § Definition § Diagnosis § Management § Screening &Prevention
Incomplete development of various organ system PREMATURIT Y REPRESENTS ……… Especially “lungs” Respiratory distress syndrome

DEFINITION §Preterm infant : delivered before 37 completed weeks §≤ 36 6/7 weeks WHO and FIGO

DEFINITION Early preterm : before 33 6/7 weeks Late preterm : between 34 and 36 completed weeks
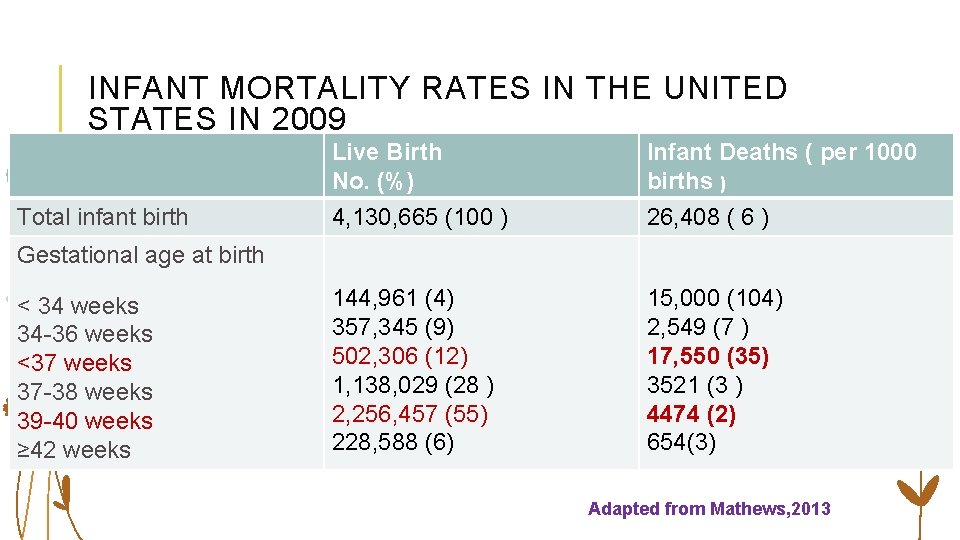
INFANT MORTALITY RATES IN THE UNITED STATES IN 2009 Total infant birth Live Birth No. (%) Infant Deaths ( per 1000 births ) 4, 130, 665 (100 ) 26, 408 ( 6 ) 144, 961 (4) 357, 345 (9) 502, 306 (12) 1, 138, 029 (28 ) 2, 256, 457 (55) 228, 588 (6) 15, 000 (104) 2, 549 (7 ) 17, 550 (35) 3521 (3 ) 4474 (2) 654(3) Gestational age at birth < 34 weeks 34 -36 weeks <37 weeks 37 -38 weeks 39 -40 weeks ≥ 42 weeks Adapted from Mathews, 2013
Unnecessary obstetrical intervention are not occurring before 38 or 39 weeks

TRENDS IN PRETERM BIRTH RATES - The preterm birth rate in the United States 2003 : 12. 3% - In Canada : 7. 7% - 77% of the race/ethnicity-related disparity in infant mortality rate in the United States in 2009 was associated with preterm birth ( Mathews, 2013 )
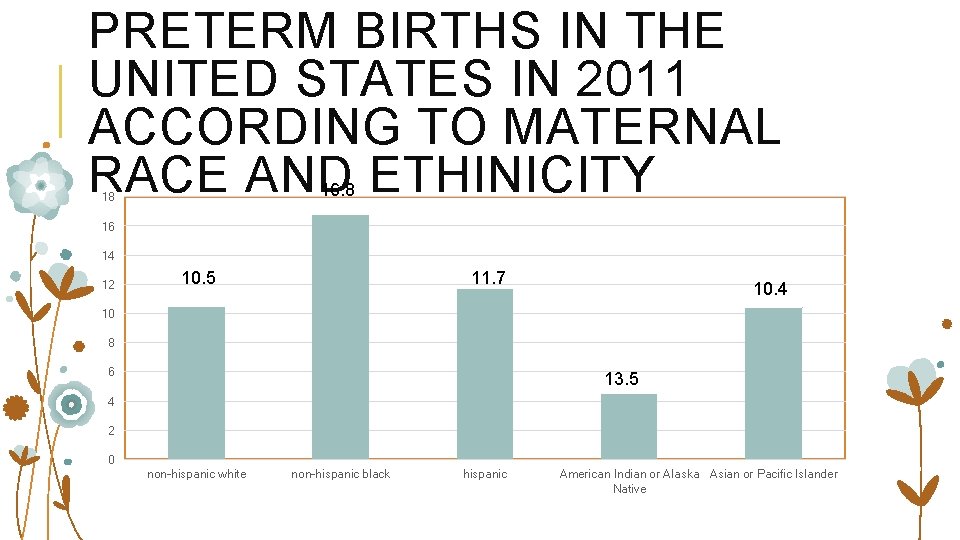
PRETERM BIRTHS IN THE UNITED STATES IN 2011 ACCORDING TO MATERNAL RACE AND ETHINICITY 16. 8 18 16 14 12 10. 5 11. 7 10. 4 10 8 6 13. 5 4 2 0 non-hispanic white non-hispanic black hispanic American Indian or Alaska Asian or Pacific Islander Native
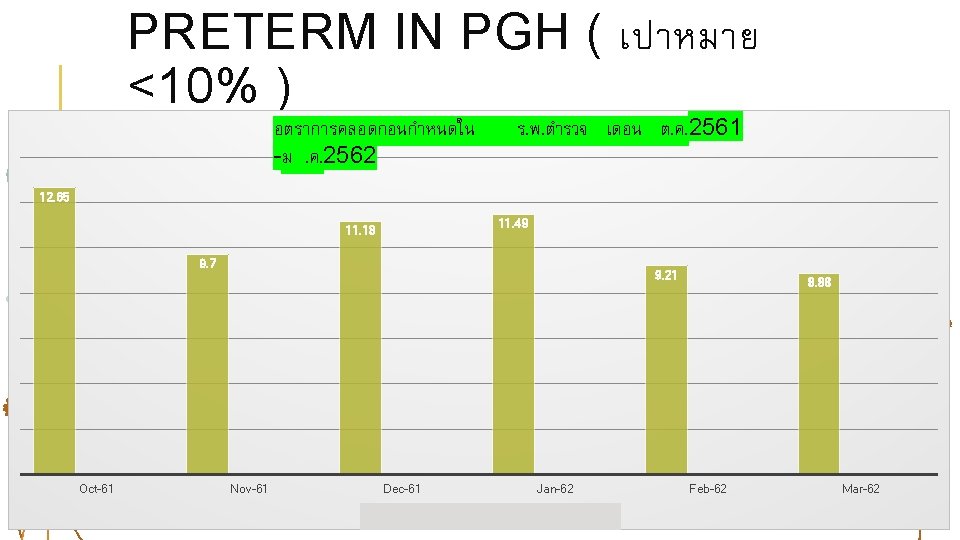
PRETERM IN PGH ( เปาหมาย <10% ) อตราการคลอดกอนกำหนดใน ร. พ. ตำรวจ เดอน ต. ค. 2561 Chart Title -ม. ค. 2562 12. 65 11. 49 11. 18 9. 7 Oct-61 9. 21 Nov-61 Dec-61 Column 3 Jan-62 Column 1 Column 2 8. 88 Feb-62 Mar-62
MORBIDITY IN PRETERM INFANTS Organ system immaturity
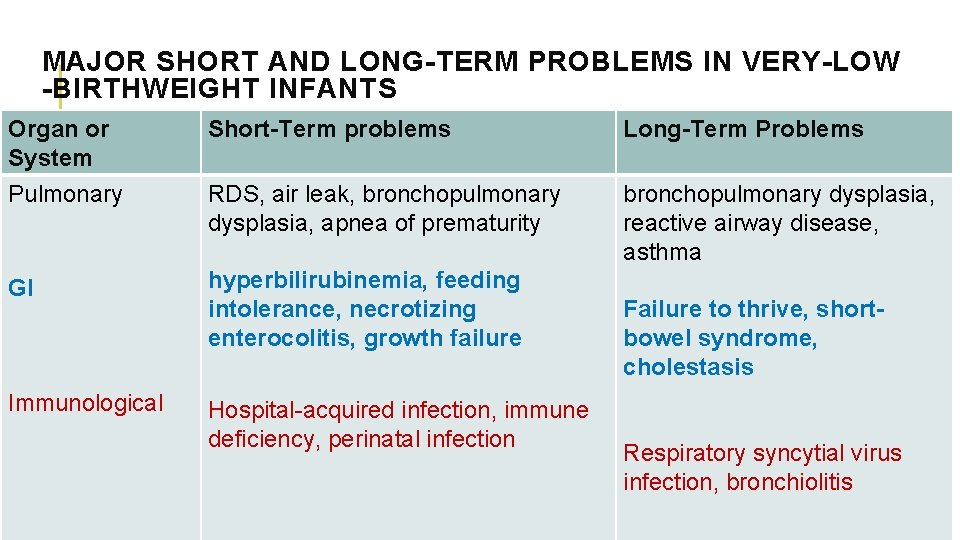
MAJOR SHORT AND LONG-TERM PROBLEMS IN VERY-LOW -BIRTHWEIGHT INFANTS Organ or System Pulmonary Short-Term problems Long-Term Problems RDS, air leak, bronchopulmonary dysplasia, apnea of prematurity bronchopulmonary dysplasia, reactive airway disease, asthma GI hyperbilirubinemia, feeding intolerance, necrotizing enterocolitis, growth failure Immunological Hospital-acquired infection, immune deficiency, perinatal infection Failure to thrive, shortbowel syndrome, cholestasis Respiratory syncytial virus infection, bronchiolitis

Organ or System Short-Term problems Long-Term Problems Central nervous system Intraventricular hemorrhage, periventricular leukomalacia, hydrocephalus Cerebral palsy, hydrocephalus, cerebral atrophy, neurodevelopmental delay, hearling loss Retinopathy of prematurity Blindness, retinal detachment, myopia, strabismus Hypotension, patent ductus arteriosus, pulmonary hypertension Pulmonary hypertension, hypertension in adulthood Opthalmological Cardiovascular Hypertension in adulthood Renal water and electrolyte imbalance, acid-base
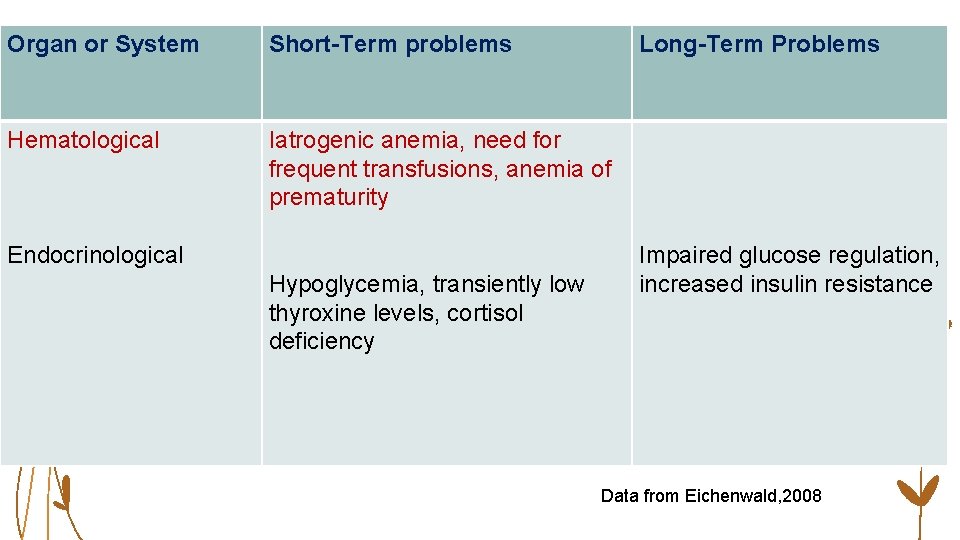

Organ or System Short-Term problems Hematological Iatrogenic anemia, need for frequent transfusions, anemia of prematurity Endocrinological Hypoglycemia, transiently low thyroxine levels, cortisol deficiency Long-Term Problems Impaired glucose regulation, increased insulin resistance Data from Eichenwald, 2008

MORTALITY AND MORBIDITY AT THE EXTREMES OF PREMATURITY § Infants delivered at ≤ 33 weeks : tremendous advances in the perinatal and neonatal care § Survival of increasingly very immature infants in the 1990 s § Uncertainly and controversy as the lower limit of fetal maturation compatible with extrauterine survival

THRESHOLD OF VIABILITY ขดแบงการอยรอด • Birth before 26 weeks : current threshold of viability • Fragile and vulnerable because immature organ system • Brain injury from hypoxic-ischemic injury and sepsis

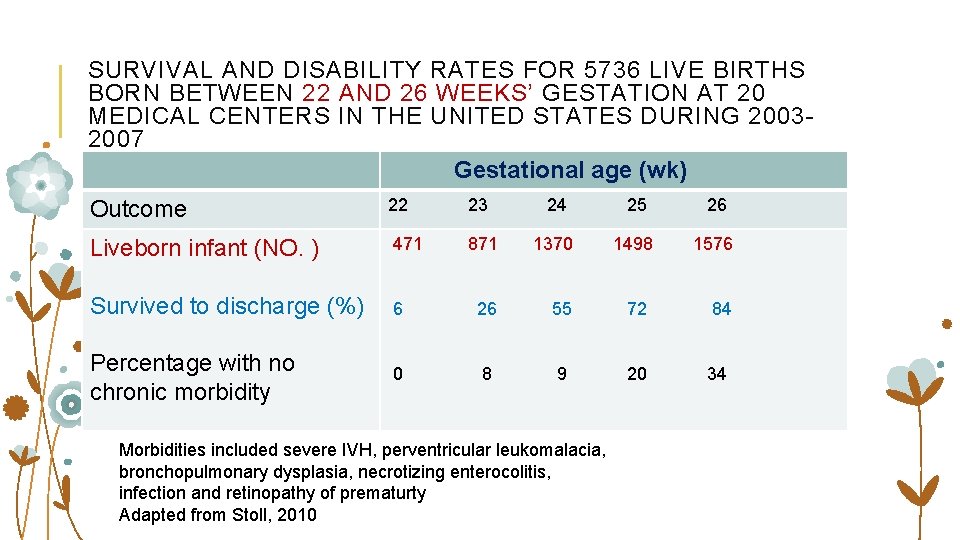
SURVIVAL AND DISABILITY RATES FOR 5736 LIVE BIRTHS BORN BETWEEN 22 AND 26 WEEKS’ GESTATION AT 20 MEDICAL CENTERS IN THE UNITED STATES DURING 20032007 Gestational age (wk) Outcome 22 23 24 25 26 471 871 1370 1498 1576 Survived to discharge (%) 6 26 55 72 84 Liveborn infant (NO. ) Percentage with no chronic morbidity 0 8 9 20 34 Morbidities included severe IVH, perventricular leukomalacia, bronchopulmonary dysplasia, necrotizing enterocolitis, infection and retinopathy of prematurty Adapted from Stoll, 2010

THRESHOLD OF VIABILITY AT PARKLAND HOSPITAL -All fetal indications for cesarean delivery are practiced in women at 25 weeks - At 24 weeks, cesarean delivery is not offered unless fetal weight is estimated at 750 g or greater

LATE PRETERM BIRTH - Infants between 34 and 36 weeks - More than 70% of all preterm births - Respiratory morbidity decreased by approximately 50% per week from 34 to 37 weeks
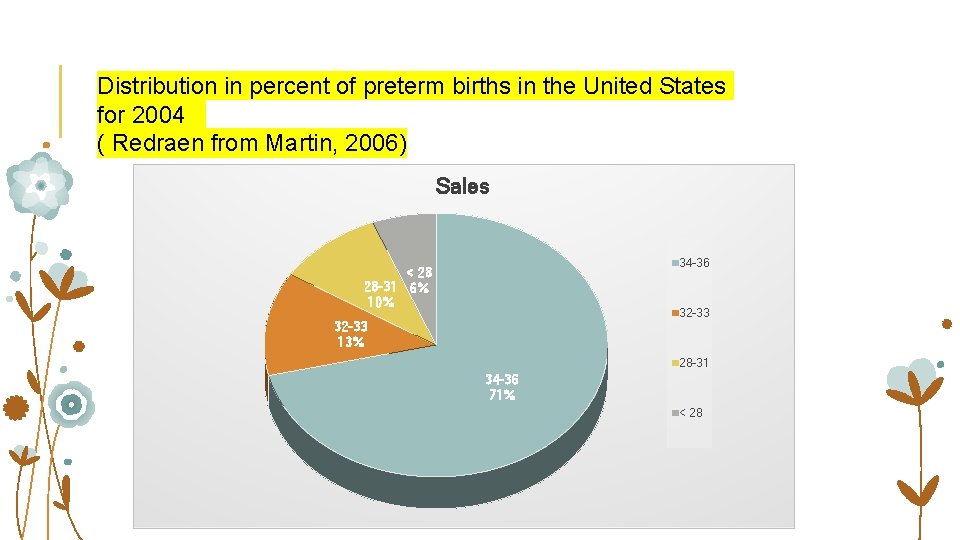
Distribution in percent of preterm births in the United States for 2004 ( Redraen from Martin, 2006) Sales 34 -36 < 28 28 -31 6% 10% 32 -33 13% 28 -31 34 -36 71% < 28
CAUSES OF PRETERM DELIVERY 4 main reasons for preterm births in United States Spontaneous unexplained preterm labor with intact membranes Idiopathic preterm premature rupture of membranes (PPROM) Delivery for maternal or fetal indications Twins and higher-order multifetal births
Interacting, antecedents, contributing factors PPROM and spontaneous preterm labor : 7080% of preterm births REASONS FOR PRETERM BIRTH

UTERINE DISTENTION MATERNAL-FETAL STRESS INFECTION PREMATURE CERVICAL CHANGE BASIC SCIENCE OF SPONTANEOUS PRETERM LABOR
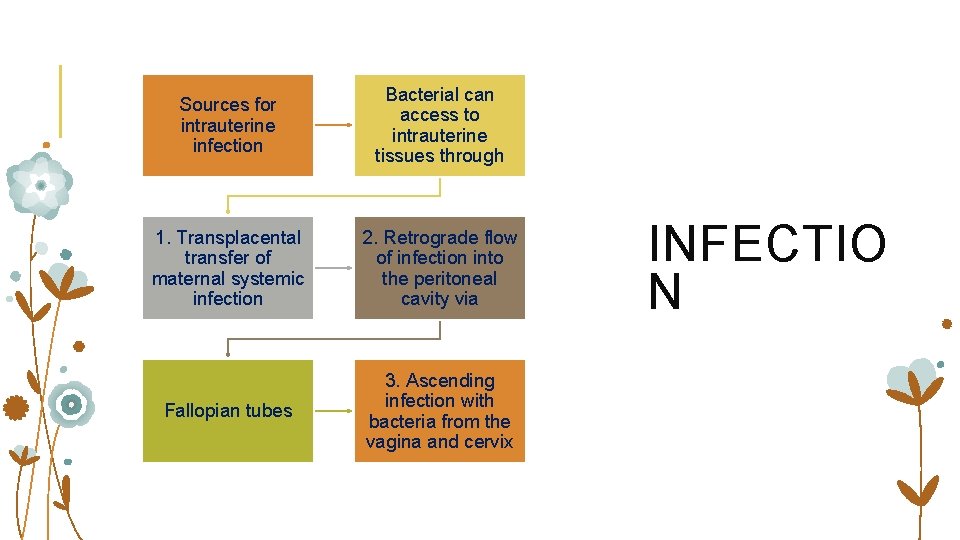
Sources for intrauterine infection Bacterial can access to intrauterine tissues through 1. Transplacental transfer of maternal systemic infection 2. Retrograde flow of infection into the peritoneal cavity via Fallopian tubes 3. Ascending infection with bacteria from the vagina and cervix INFECTIO N

Categorize intrauterine infection into 4 stages of microbial invasion that INFECTIO N Stage 1 : bacterial vaginosis Stage 2 : decidual infection Stage 3 : amnionic infection Stage 4 : fetal systemic infection

PRETERM PREMATURE RUPTURE OF MEMBRANES Major predisposing event : intrauterine infection Associated risk factors v. Low socioeconomic status v. Body mass index ≤ 19. 8 v. Nutritional deficiencies v. Cigarette smoking *****Despite these known risk factors, none is identified in most cases of preterm labor

- Preterm parturition syndrome ( Romero 2006 ) : multiple etiologies SUMMARY OF PRETERM LABOR PATHOPHYS IOLOGY - Intrauterine infection : some cases categorized as idiopathic spontaneous preterm labor - Infection : not explain all causes of preterm birth - Maternal nutrition, genetics, the vaginal microbiome and dynamic regulation of the extracellular matrix

ANTECEDENTS AND CONTRIBUTING FACTORS Threatened abortion : Subsequent preterm labor, placental abruption and subsequent pregnancy loss before 24 weeks ( Weiss 2004 )

ANTECEDENTS AND CONTRIBUTING FACTORS Lifestyle factors §Cigarette smoking §Inadequate maternal weight gain §Illicit drug use §Overweight and obese mothers ( Cnattingius, 2013 ) §Advance maternal age

ANTECEDENTS AND CONTRIBUTING FACTORS Lifestyle factors § Depression, anxiety, and chronic stress § ( Copper, 1996; Li, 2008; Littleton, 2007 ) § Working long hours and hard physical labor ( Luke, 1995 )

ANTECEDENTS AND CONTRIBUTING FACTORS Genetic factors - May play a cause role - Recurrent, familial, and racial nature of preterm birth - Immunoregulatory genes in potentiating chorioamnionitis in case of preterm delivery ( Varner, 2005 )

ANTECEDENTS AND CONTRIBUTING FACTORS Birth defects was associated with preterm birth and low birthweight (Dolan, 2007)

ANTECEDENTS AND CONTRIBUTING FACTORS Periodontal disease - Significantly associated with preterm labor ( Vergnes and Sixou, 2007 ) - The data were not robust enough to recommend screening and treatment of pregnant women (Stamilio, 2007) - Treatment periodontal disease during pregnant : failed to significantly alter preterm birth rate (Michalowictz, 2006)

ANTECEDENTS AND CONTRIBUTING FACTORS Interval between pregnancies Interval < 18 months and > 59 months : associated with increased risks for both preterm birth and SGA newborns

ANTECEDENTS AND CONTRIBUTING FACTORS Prior preterm labor - Major risk factors for preterm labor ******

RECURRENT SPONTANEOUS PRETERM BIRTHS ACCORDING TO PRIOR OUTCOME Birth Outcome Second Birth ≤ 34 weeks (%) First birth ≥ 35 weeks 5 First birth ≤ 34 weeks 16 First and second birth ≤ 34 weeks 41 Data from 15, 863 women delivering their first and subsequent pregnancies at Parkland Hospital. Adapt fro Bloom, 2001

ANTECEDENTS AND CONTRIBUTING FACTORS Bacterial vaginosis BV : associated with spontaneous abortion, preterm labor, PPROM, chorioamnionitis and amnionic fluid infection : Associated with BV : chronic stress, ethnic differences and frequent or recent douching

Admit in LR Notified ����� • • Delivery NPO IV Fluid On external fetal monitoring uterine contraction Vital sign + ���������� ATB prophylaxis Group B Streptococci ����� active phase ������ tocolytic drugs ������ steroid PRETERM LABOR : GA ≥ 34 WEEKS


PRETERM LABOR : GA < 34 WEEKS oหญงตงครรภอาย date มา ร. พ. ดวยอาการเจบครรภถ 18 ป G 1 P 0 GA 32 weeks by 1 ชม. กอนมาร. พ. o. ANC at PGH o. First US at GA 20 weeks , GA = date o. No underlying disease
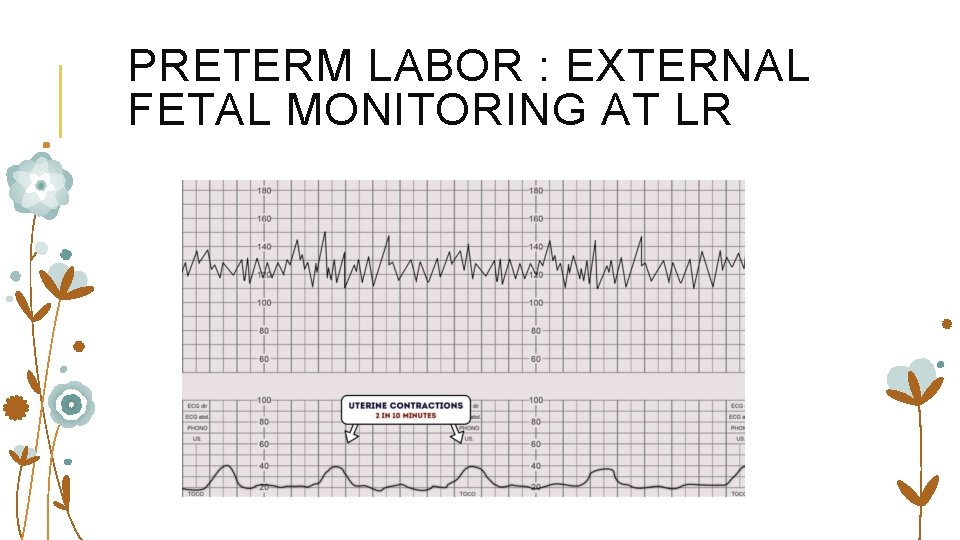
PRETERM LABOR : EXTERNAL FETAL MONITORING AT LR
PV : swab gram stain and culture cervix was opened 2 cm , dilate 100% , station 0 , membrane intact AT LR • Diagnosis : GA 32 weeks with preterm labor

GA 32 WEEKS WITH PRETERM LABOR admit at LR Notified กมารแพทย Expectant management

GA 32 WEEKS WITH PRETERM LABOR Maternal üUnderlying disease : HT, GDM, heart disease, hyperthyroid üVITAL SIGN : Temp, BP, pulse üCause of preterm labor ; Cervical swab gram stain and culture , UA üBiochemistry : CBC, BUN, Cr, electrolyte, BS

GA 32 WEEKS WITH PRETERM LABOR Fetus üConfirm GA, สวนนำของทารก , fetal weight üOn external fetal monitoring

GA < 34 WEEKS WITH PRETERM LABOR § NPO § ยายบยงการหดตวของมดลก ( tocolytic drugs ) § Steroid : Dexamethasone 6 mg im q 12 hours x 4 doses § ATB : prevent Group B Steptococci ( GBS ) when active phase

TOCOL YTIC DRUG S For GA start at viable-336/7 weeks First line 1. calcium channel blockersnifedipine ( Adalat ) 2. beta-adrenergic receptor agonist ( terbutaline/ Bricanyl ) 3. prostaglandin inhibitors : NSAIDs


CONTRAINDI CATION FOR TOCOLYTIC DRUGS v. Severe preeclampsia, eclampsia v. Placental abruption v. Non-reassuring fetal status v. Chorioamnionitis v. Severe anomaly ( incompatible with life ) v. Fetal death in utero

PRETERM PREMATURE RUPTURE OF MEMBRANES Spontaneous rupture of the fetal membranes before 37 completed Weeks and before labor onset ACOG 2013 d

PRETERM PREMATURE RUPTURE OF MEMBRANE : MANAGEMENT ประเมนสาเหตการมนำเดนกอนกำหนด Anovaginal swab culture UA and urine culture ( MUC ) CBC Ultrasound : fetal anomaly, amniotic fluid, placenta Maternal : HT, fever

PRETERM PREMATURE RUPTURE OF MEMBRANE : MANAGEMENT การใหยาปฏชวนะ ตดสนใหคลอด : ATB for prevent group B streptococci ( GBS ) Expectant management : ATB for prolonged latency period กรณทม chorioamnionitis ควรใหคลอด ให Broad spectrum ATB

PRETERM PREMATU RE RUPTURE OF MEMBRA NE : MANAGE MENT GA 24 -33 weeks §expectant management §Steroid for promote lung maturity §เฝาระวง chorioamnionitis : CBC, Vital sign มารดา ( Temp and pulse ), FHR §Fetal monitoring §Ultrasound : AFI §Delivery time : chorioamnionitis, nonreassuring fetal testing, placental abruption, advance labor หรอ อายครรภครบ 34 weeks

PRETERM PREMATU RE RUPTURE OF MEMBRA NE : MANAGE MENT GA 34 -37 weeks แนะนำใหคลอดได ATB for prevent GBS infection Steroid Route of delivery §Normal labor : นมนวล ตดฝเยบใหกวางพอ ลดภาวะเลอดออกในสมอง ) §Cesarean section (
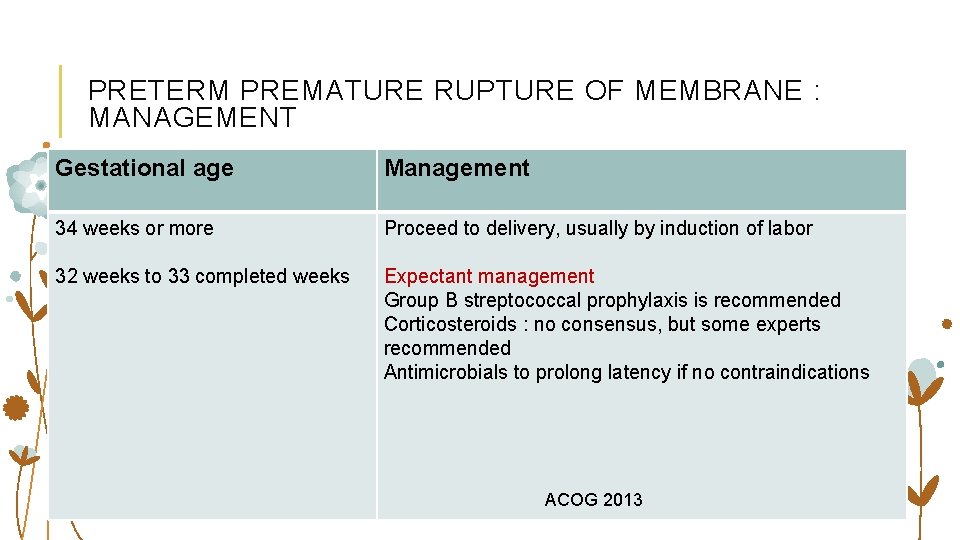
PRETERM PREMATURE RUPTURE OF MEMBRANE : MANAGEMENT Gestational age Management 34 weeks or more Proceed to delivery, usually by induction of labor 32 weeks to 33 completed weeks Expectant management Group B streptococcal prophylaxis is recommended Corticosteroids : no consensus, but some experts recommended Antimicrobials to prolong latency if no contraindications ACOG 2013
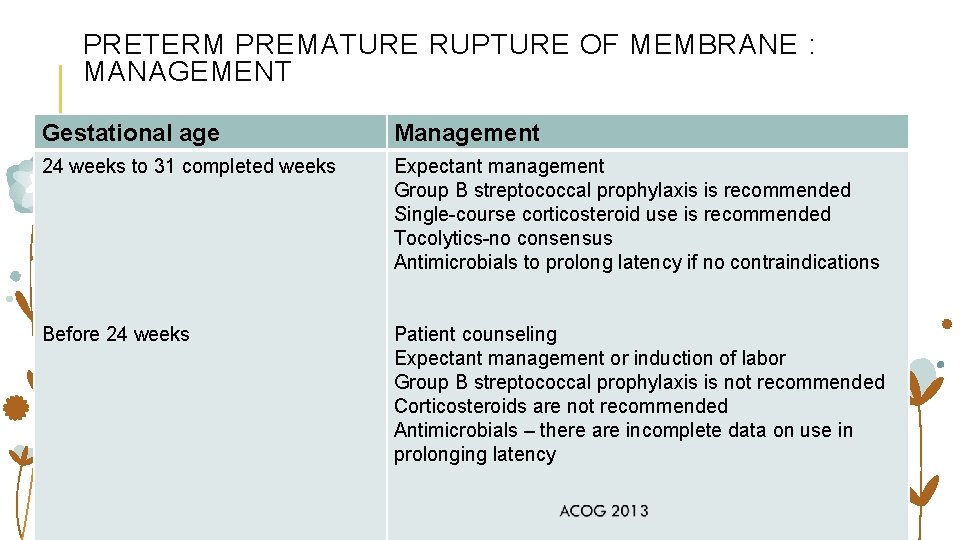
PRETERM PREMATURE RUPTURE OF MEMBRANE : MANAGEMENT Gestational age Management 24 weeks to 31 completed weeks Expectant management Group B streptococcal prophylaxis is recommended Single-course corticosteroid use is recommended Tocolytics-no consensus Antimicrobials to prolong latency if no contraindications Before 24 weeks Patient counseling Expectant management or induction of labor Group B streptococcal prophylaxis is not recommended Corticosteroids are not recommended Antimicrobials – there are incomplete data on use in prolonging latency

SCREENING AND PREVENTION

WHO HAS RISK OF PRETERM LABOR ? 1. History of previous preterm labor 2. Periodontal disease 3. Bacterial vaginitis 4. Genitourinary tract infection 5. Teenage pregnancy 6. ������ 7. smoking 8. Multifetal pregnancy 9. uterine abnormalities






- Slides: 68