PRETERM LABOR Associate Professor Iolanda Elena Blidaru MD

PRETERM LABOR Associate Professor Iolanda Elena Blidaru, MD, Ph. D 11/3/2020 5: 53: 12 Managrement of Preterm Labour 1

PRETERM LABOR • Delivery between 24(20) & 37 weeks gestation • Different from Low birthweight (LBW) – LBW < 2500 gm – Very LBW < 1500 gm – Extremely LBW < 1000 gm • Major cause of fetal, perinatal & Infant death • High cost of survival 11/3/2020 5: 53: 13 Managrement of Preterm Labour 2
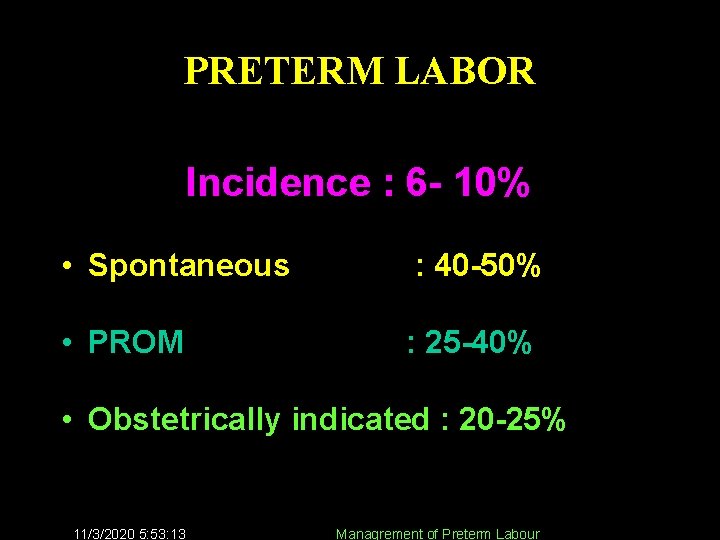

PRETERM LABOR Incidence : 6 - 10% • Spontaneous : 40 -50% • PROM : 25 -40% • Obstetrically indicated : 20 -25% 11/3/2020 5: 53: 13 Managrement of Preterm Labour 3

PRETERM LABOR Most mortality and morbidity is experienced by babies born before 34 weeks. 11/3/2020 5: 53: 13 Managrement of Preterm Labour 4

PRETERM LABOR Major Fetal Risks Of Preterm Delivery • • Death Respiratory distress syndrome Hypothermia Hypoglycemia Necrotising enterocolitis Jaundice Infection Retinopathy of prematurity 11/3/2020 5: 53: 13 Managrement of Preterm Labour 5

PRETERM LABOR ETIOLOGY (I) v Amnionic fluid infection v Cervical incompetence v Placenta praevia v Placental abruption v Uterine anomalies, fibroids v Polyhydramnios 11/3/2020 5: 53: 13 Managrement of Preterm Labour 6

PRETERM LABOR ETIOLOGY (II) v Hypertension v Fetal anomalies v Immunological v Trauma or surgery v IDIOPATHIC - Cause undetectable 11/3/2020 5: 53: 13 Managrement of Preterm Labour 7

PRETERM LABOR CLASSIFICATION 1. Complications of pregnancy that mandate delivery (fetal / maternal risk ) 2. Spontaneous preterm labor with intact membranes – true / false labour 3. Preterm / premature rupture of membranes (PROM) 11/3/2020 5: 53: 13 Managrement of Preterm Labour 8

Prediction 1. Assessment of risk factors 2. Vaginal examination to assess the cervical status 3. Ultrasound visualization of cervical length and dilatation 4. Detection of biological markers 11/3/2020 5: 53: 14 Managrement of Preterm Labour 9

1. Assessment of risk factors 11/3/2020 5: 53: 14 Managrement of Preterm Labour 10

RISK FACTORS OF PRETERM LABOR • Risk assessment - Papiernik • There is strong evidence that intrauterine infection plays a role in preterm labor. • Bacterial vaginosis increases the risk of preterm delivery >2 -fold. 11/3/2020 5: 53: 14 Managrement of Preterm Labour 11

RISK FACTORS OF PRETERM LABOR (I) v Poor socioeconomic/ education/ hygiene/ nutritional status v Young (<16 y. ) or advanced age (>35 y. ) v Nuliparity or grand multiparity v Short stature or low weight (BMI < 19. 0) v Medical or surgical illness in pregnancy v Antiphospholipid syndrome 11/3/2020 5: 53: 14 Managrement of Preterm Labour 12

RISK FACTORS OF PRETERM LABOR (II) v Previous preterm delivery: risk 20 - 40% v Obstetric complications: hypertension in pregnancy, antepartum hemorrhage, infection, polyhydramnios, fetal abnormalities. v Cigarette smoking: risk 20 -30% v Multiple pregnancy: risk >50% v Cervical incompetence v Uterine abnormalities 11/3/2020 5: 53: 14 Managrement of Preterm Labour 13

RISK FACTORS OF PRETERM LABOR (III) v Cervical effacement and/or dilatation > 20 weeks v Pelvic pressure v Low back pain v Uterine contraction 11/3/2020 5: 53: 14 Managrement of Preterm Labour 14

2. Vaginal examination to assess the cervical status 11/3/2020 5: 53: 14 Managrement of Preterm Labour 15
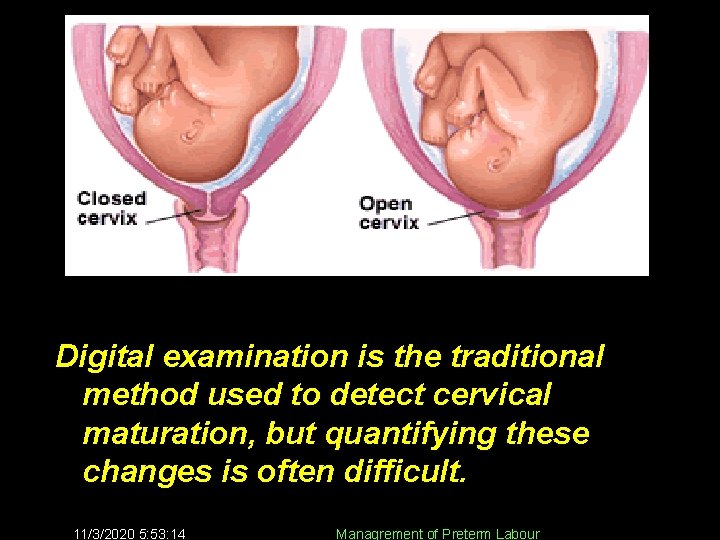
Digital examination is the traditional method used to detect cervical maturation, but quantifying these changes is often difficult. 11/3/2020 5: 53: 14 Managrement of Preterm Labour 16

3. Ultrasound assessment of cervical length and dilatation Vaginal ultrasonography → a more objective examination of the cervix (≈ 35 mm). 11/3/2020 5: 53: 14 Managrement of Preterm Labour 17
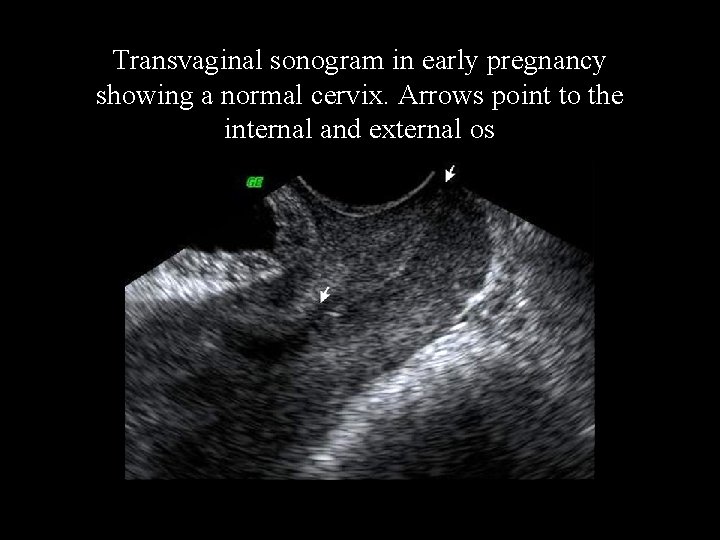
Transvaginal sonogram in early pregnancy showing a normal cervix. Arrows point to the internal and external os
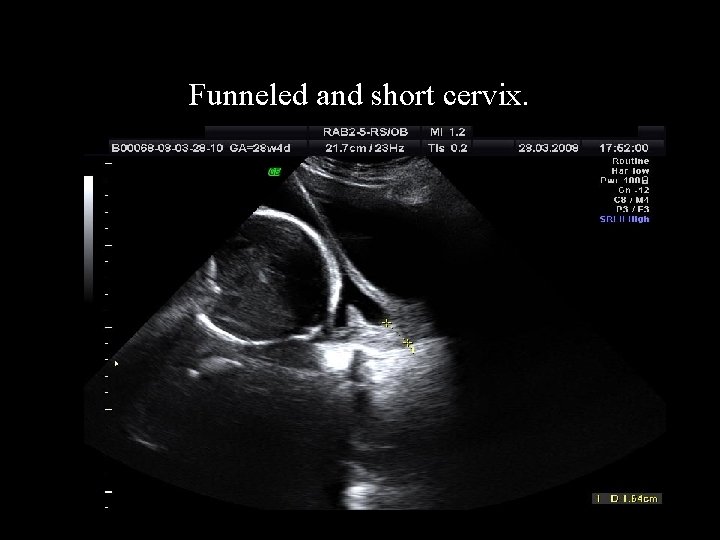
Funneled and short cervix.

4. Detection of biological markers • Testing with biological markers (24 -36 weeks): – Fetal Fibronectin (FFN) - in cervico-vaginal secretions (> 50 ng/m. L) – Salivary estriol (E 3). 11/3/2020 5: 53: 16 Managrement of Preterm Labour 20

DIAGNOSIS OF IMPENDING PRETERM DELIVERY (Active preterm labor) 11/3/2020 5: 53: 16 Managrement of Preterm Labour 21

IMPENDING PRETERM DELIVERY (Active preterm labor) 3 criteria for active preterm labour (20 -36 w): • uterine contractions - 4 in 20 min. or 8 in 1 h. + • cervical changes over time (effacement 80%) or • dilatation ≥ to 2 cm (at least 1) 11/3/2020 5: 53: 17 Managrement of Preterm Labour 22

Prevention 11/3/2020 5: 53: 17 Managrement of Preterm Labour 23

Prevention of Preterm Labor • Antenatal care • Self-monitoring of uterine activity at home: external tocodynamometer • Reduce work, smoking, stress, travel, sexual activity, bed rest, improve nutrition 11/3/2020 5: 53: 17 Managrement of Preterm Labour 24

PREVENTION OF PRETERM LABOR Specific obstetric treatment § Bed rest (in hospital) § Cerclage of the cervix § Antibiotics: urinary infection (asymptomatic bacteriuria), local infection (bacterial vaginosis), occult infection § Progesterone 11/3/2020 5: 53: 17 Managrement of Preterm Labour 25

Treatment of active preterm labor 1. Inhibition of uterine contractions 2. Corticosteroids 3. Antibiotics 11/3/2020 5: 53: 17 Managrement of Preterm Labour 26

Treatment of active preterm labor 1. Inhibition of uterine contractions • • Bed rest - hospitalisation Hydration and sedation ? • Tocolytics • Corticotherapy, Antibiotics 11/3/2020 5: 53: 17 Managrement of Preterm Labour 27

Choice Of Tocolytic Drug 1. Beta –Sympathomimetic agents (Ritodrine, Isoxsuprine, Terbutaline, Salbutamol) 2. Magnesium sulphate 3. Nonsteroidal anti-inflammatory drugs (Indomethacin) 4. Calcium channel blockers (Nifedipine) 5. Nitric Oxide Donors (Nitroglyerin) 6. Oxytocin receptor antagonist (Atosiban = Tractocile) 11/3/2020 5: 53: 17 Managrement of Preterm Labour 28

Choice Of Tocolytic Drug Atosiban: Tractocil • a synthetic peptide, acts as a competitive antagonist of oxytocin at uterine oxytocin receptors. 11/3/2020 5: 53: 17 Managrement of Preterm Labour 29

Choice Of Tocolytic Drug q. Most authorities do not recommend use of tocolytics at or after 34 weeks'. q. Tocolysis should be considered for completing a course of corticosteroids, or in utero transfer. 11/3/2020 5: 53: 17 Managrement of Preterm Labour 30

Corticosteroids • Antenatal corticosteroids are associated with a significant reduction in rates of RDS, neonatal death and intraventricular hemorrhage. • The optimal interval between treatment and delivery is 24 hours. 11/3/2020 5: 53: 17 Managrement of Preterm Labour 31

Treatment of active preterm labor CORTICOSTEROIDS (GA = 24 -34 weeks) • 2 doses of Betamethasone 12 mg i. m. at 24 hours interval or • 4 doses of Dexamethasone 6 mg i. m. /i. v. at 12 hours interval 11/3/2020 5: 53: 17 Managrement of Preterm Labour 32

Treatment of active preterm labor ANTIBIOTICS • Ampicillin / Clindamycin / Erythromycin • Screen All Pregnant Women for GBS All patients in preterm labor are considered at high risk. 11/3/2020 5: 53: 17 Managrement of Preterm Labour 33

Intra Partum Managements of Preterm Labour Minimise Maternal Hypotension and Fetal hypoxia and acidosis < Respiratory Distress Syndrome z Routine use of prophylactic forceps & episiotomy ? z Postpartum uterine control z If Fetal distress - CS? ØBelow 28 weeks - NO CS ØBelow 32 weeks - ? ØAbove 32 weeks - CS ØVertical uterine incision 11/3/2020 5: 53: 17 Managrement of Preterm Labour 34
- Slides: 34