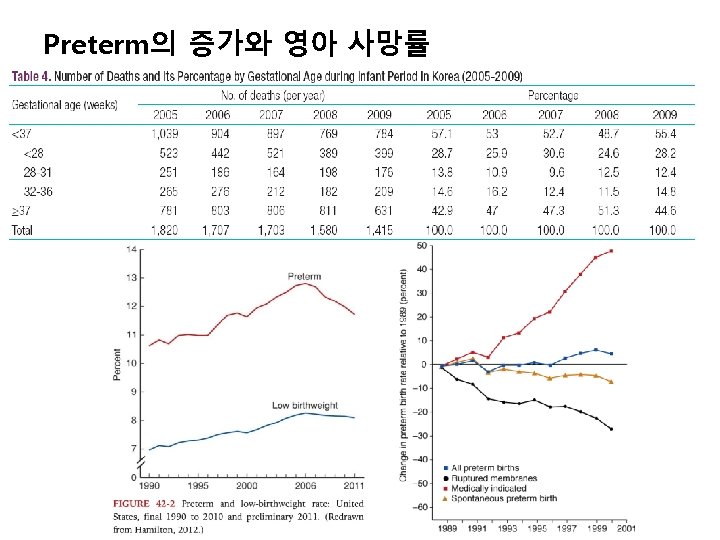
preterm birth 20 37 low birth weight LBW


용어의 정의 조산(preterm birth): 20주부터 37주 이전의 분만 저체중출생아 (low birth weight; LBW): 2, 500 g미만 초저체중출생 (very low birth weight; VLBW): 1, 500 g미만 극저체중출생 (extremely low birth weight; ELBW): 1, 000 g 미만 저체중아 (small for gestational age), 태아발육부전 (fetalgrowth restriction, intrauterine growth restriction): 신 생아 체중 <10% 과체중아 (large for gestational age): 신생아 체중 >90%


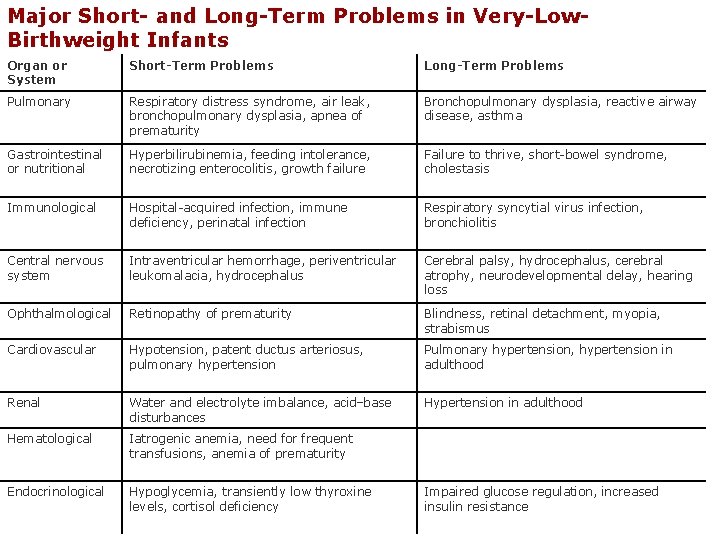
Major Short- and Long-Term Problems in Very-Low. Birthweight Infants Organ or System Short-Term Problems Long-Term Problems Pulmonary Respiratory distress syndrome, air leak, bronchopulmonary dysplasia, apnea of prematurity Bronchopulmonary dysplasia, reactive airway disease, asthma Gastrointestinal or nutritional Hyperbilirubinemia, feeding intolerance, necrotizing enterocolitis, growth failure Failure to thrive, short-bowel syndrome, cholestasis Immunological Hospital-acquired infection, immune deficiency, perinatal infection Respiratory syncytial virus infection, bronchiolitis Central nervous system Intraventricular hemorrhage, periventricular leukomalacia, hydrocephalus Cerebral palsy, hydrocephalus, cerebral atrophy, neurodevelopmental delay, hearing loss Ophthalmological Retinopathy of prematurity Blindness, retinal detachment, myopia, strabismus Cardiovascular Hypotension, patent ductus arteriosus, pulmonary hypertension Pulmonary hypertension, hypertension in adulthood Renal Water and electrolyte imbalance, acid–base disturbances Hypertension in adulthood Hematological Iatrogenic anemia, need for frequent transfusions, anemia of prematurity Endocrinological Hypoglycemia, transiently low thyroxine levels, cortisol deficiency Impaired glucose regulation, increased insulin resistance

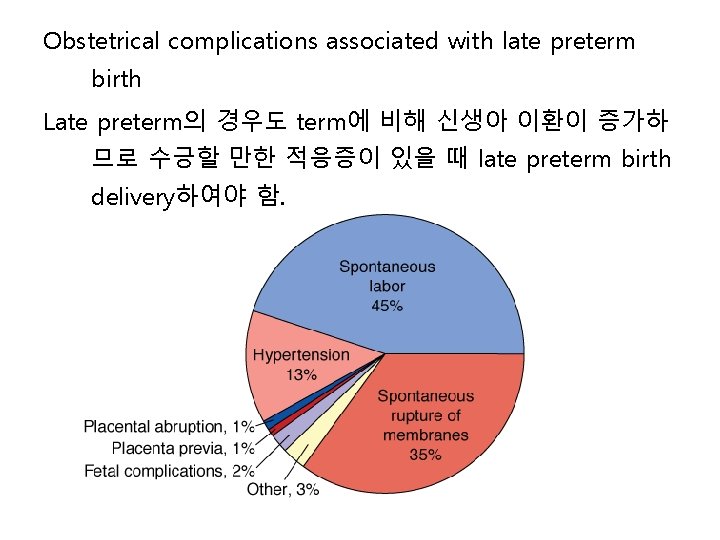
Obstetrical complications associated with late preterm birth Late preterm의 경우도 term에 비해 신생아 이환이 증가하 므로 수긍할 만한 적응증이 있을 때 late preterm birth delivery하여야 함.


조산의 위험인자 ① Threatened abortion ② Lifestyle factors ③ Genetic factors ④ Periodontal disease ⑤ Birth defects ⑥ Interval between pregnancies and preterm birth ⑦ Prior preterm birth ⑧ Infection (Bacterial vaginosis)

Lifestyle factors Cigarette smoking Inadequate weight gain Illicit drug Restricted fetal growth Young or advanced maternal age Poverty Short stature Vitamin C deficiency Occupational factors: prolonged walking or standing, strenuous working condition, long weekly work hours Psychological factors: depression, anxiety, chronic stress

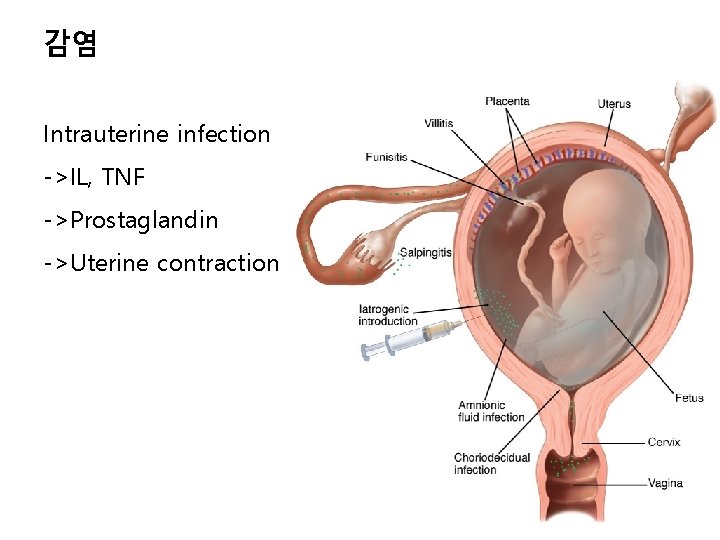
감염 Intrauterine infection ->IL, TNF ->Prostaglandin ->Uterine contraction



Ambulatory uterine monitoring: 권장되지 않음. Fetal fibronectin cervicovaginal fluid reflect stromal remodeling of the cervix prior to labor a possible marker for impending preterm labor 무증상 임신부에서 screening으로 권장되지 않음.

예방 ① 자궁목 원형결찰술(cerclage) -recurrent midtrimester loss with cervical insufficiency -sonographic short cervix of prior preterm birth -rescue op of cervical incompetence ② 프로게스테론 요법 Women with a documented history of a previous spontaneous birth <37 weeks ③ 자궁경관 페사리 (cervical pessaries)
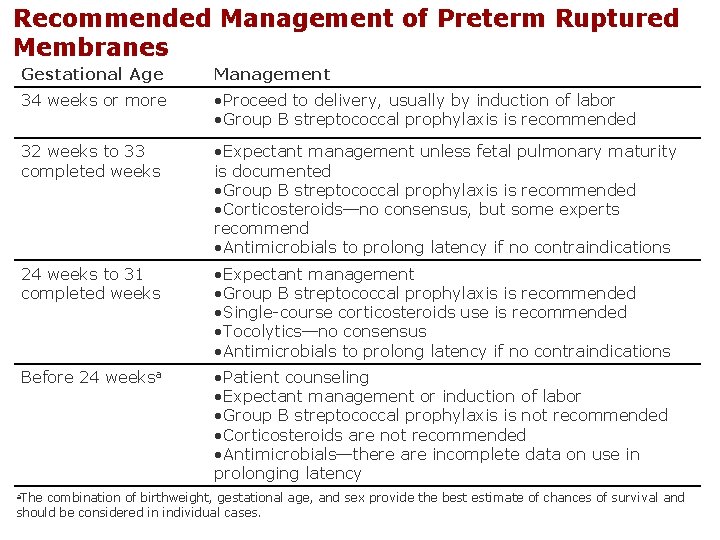





Recommended Management of Preterm Ruptured Membranes Gestational Age Management 34 weeks or more • Proceed to delivery, usually by induction of labor • Group B streptococcal prophylaxis is recommended 32 weeks to 33 completed weeks • Expectant management unless fetal pulmonary maturity is documented • Group B streptococcal prophylaxis is recommended • Corticosteroids—no consensus, but some experts recommend • Antimicrobials to prolong latency if no contraindications 24 weeks to 31 completed weeks • Expectant management • Group B streptococcal prophylaxis is recommended • Single-course corticosteroids use is recommended • Tocolytics—no consensus • Antimicrobials to prolong latency if no contraindications Before 24 weeksa • Patient counseling • Expectant management or induction of labor • Group B streptococcal prophylaxis is not recommended • Corticosteroids are not recommended • Antimicrobials—there are incomplete data on use in prolonging latency a. The combination of birthweight, gestational age, and sex provide the best estimate of chances of survival and should be considered in individual cases.


⑦ 조기진통의 억제-약물 치료 (스테로이드 투여를 위한 48시간 여유를 제공) Tocolytic agents do not markedly prolong gestation but may delivery in some women for up to 48 hours. Maintenance therapy with tocolytics is ineffective for preventing preterm birth and improving neonatal outcome and is not recommended for this purpose. Women with preterm contraction without cervical change, especially those with cervical dilatation of less than 2 cm, genearally should not be treated with tocolytics.


조기진통의 약물적 처치 • 베타 아드레날린성 수용체 작용제 β-adrenergic agonist Ritodrine 부작용: 폐부종 risk factor: tocolytic therapy with β-agonist, multifetal gestation, concurrent corticosteroid therapy, tocolytics more than 24 hours, large IV crystalloid volume infusion • 황산마그네슘 4 g loading followed by 2 g/hr 태아의 bone thinning과 fracture에 대한 우려로 5 -7일 이상 장 기간 사용은 금기.

• Prostaglandin inhibitor Prostaglandin synthesis 억제로 자궁수축 억제시킴. Indomethacin. 태아 및 신생아의 예후 악화에 대하여 논란 이 있음. • 칼슘통로차단제 Acute tocolysis에 대한 RCT가 없음. • Atosiban Competitive antagonist of oxytocin-induced contraction

Prevention of neonatal ICH Magnesium sulfate VLBW에서 maternal magnesium sulfate therapy가 fetal neuroprotective effect가 있음. Neonatal death, cerebral palsy감소한다는 연구가 있었음. VLBW에서 routine 사용은 하지 않으며 specific guideline 이 필요함. Parkland hospital에서는 24 -27+6주까지 6 g loading followed by 2 g/h for at least 2 hrs.


조기진통의 처치 1. Confirmation of preterm labor as detailed in Diagnosis 2. For pregnancies less than 34 weeks in women with no maternal or fetal indications for delivery, close observation with monitoring of uterine contractions and fetal heart rate is appropriate. Serial examinations are done to assess cervical changes 3. For pregnancies less than 34 weeks, corticosteroids are given for enhancement of fetal lung maturation 4. Consideration is given for maternal magnesium sulfate infusion for 12 to 24 hours to afford fetal neuroprotection 5. For pregnancies less than 34 weeks in women who are not in advanced labor, some practitioners believe it is reasonable to attempt inhibition of contractions to delay delivery while the women are given corticosteroid therapy and group B streptococcal prophylaxis. 6. For pregnancies at 34 weeks or beyond, women with preterm labor are monitored for labor progression and fetal well-being 7. For active labor, an antimicrobial is given for prevention of neonatal group B streptococcal infection.

- Slides: 32