Pressure Ulcers in Older Adults Objectives l l

Pressure Ulcers in Older Adults

Objectives l l l Identify how to calculate the incidence and prevalence of pressure ulcers Perform a risk assessment for pressure ulcers, using validated risk assessment scale Define pressure ulcer, including staging Plan care for prevention of pressure ulcers Plan care to include debridement, cleansing, dressing, and pressure relief 2

Prevalence 3
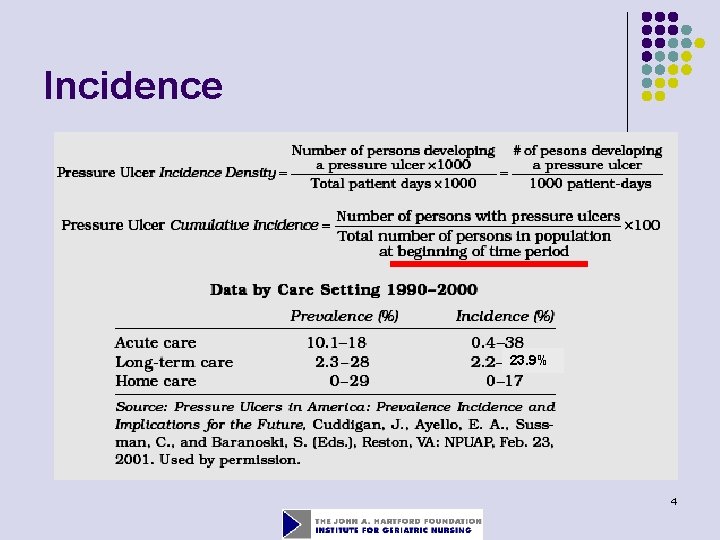

Incidence 23. 9% 4

Healthy People 2010 “Reduce the proportion of nursing home residents with a diagnosis of pressure ulcers to 8 diagnoses per 1, 000 residents. ” 5
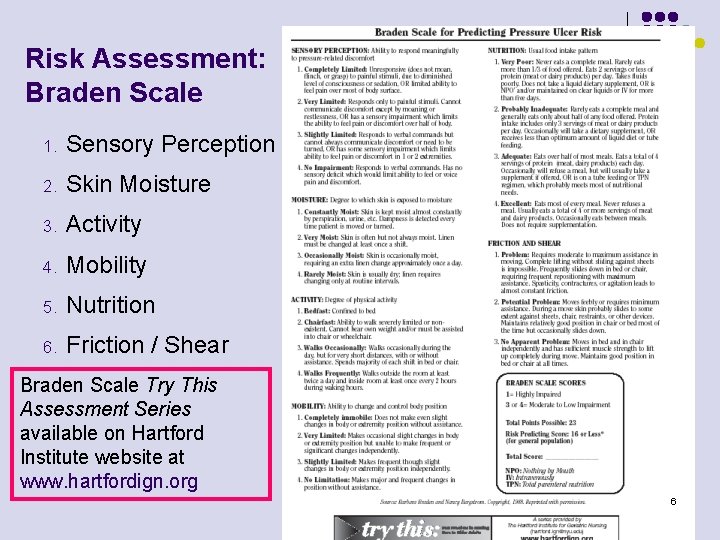

Risk Assessment: Braden Scale 1. Sensory Perception 2. Skin Moisture 3. Activity 4. Mobility 5. Nutrition 6. Friction / Shear Braden Scale Try This Assessment Series available on Hartford Institute website at www. hartfordign. org 6

Risk Assessment: Norton Scale 7
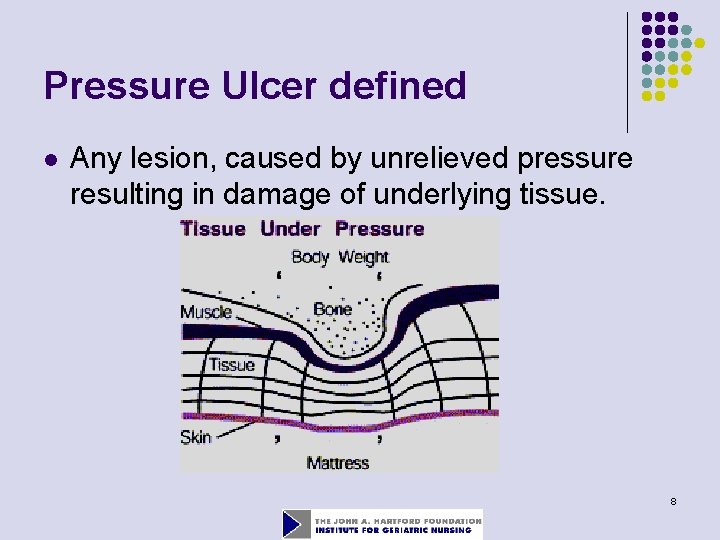
Pressure Ulcer defined l Any lesion, caused by unrelieved pressure resulting in damage of underlying tissue. 8
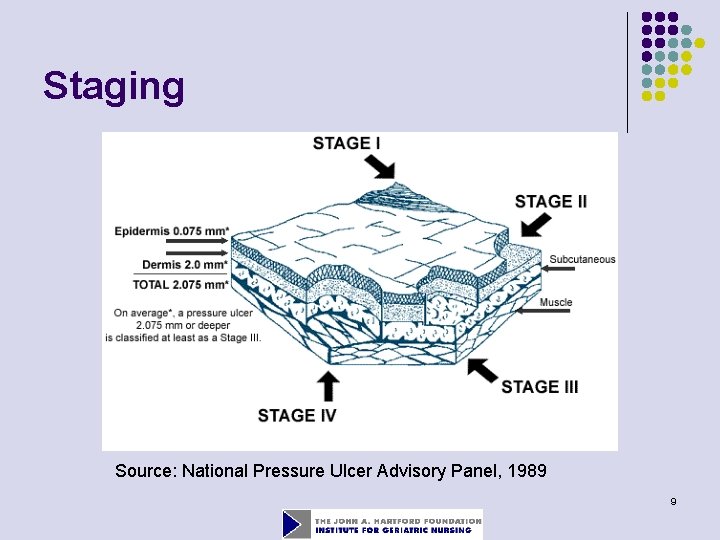
Staging Source: National Pressure Ulcer Advisory Panel, 1989 9

Factors to consider… l Nutritional deficiencies / weight l Aging l Lowered mental status l Immunosuppressant drugs l Infection l Continence 10
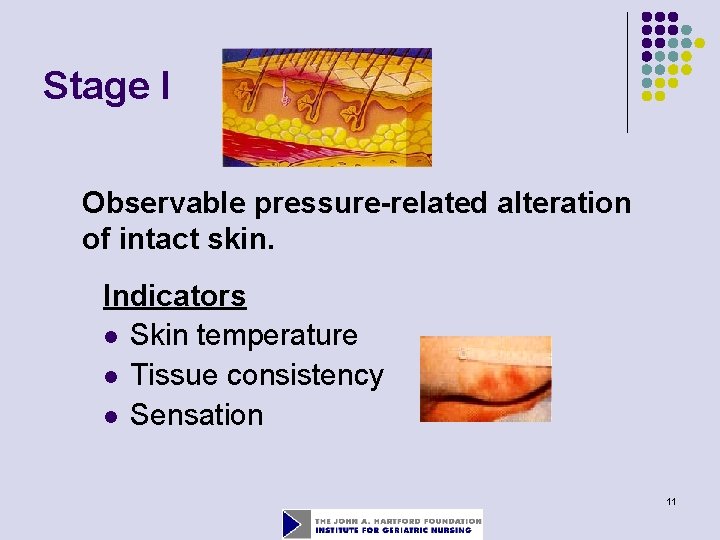
Stage I Observable pressure-related alteration of intact skin. Indicators l Skin temperature l Tissue consistency l Sensation 11
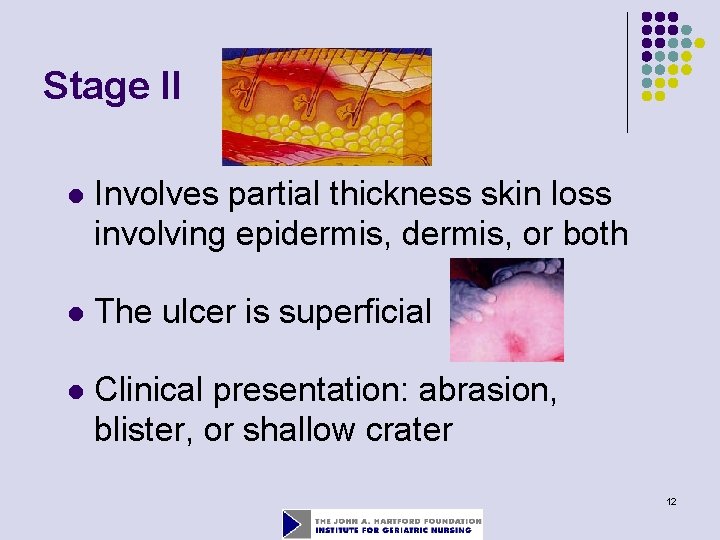
Stage II l Involves partial thickness skin loss involving epidermis, or both l The ulcer is superficial l Clinical presentation: abrasion, blister, or shallow crater 12
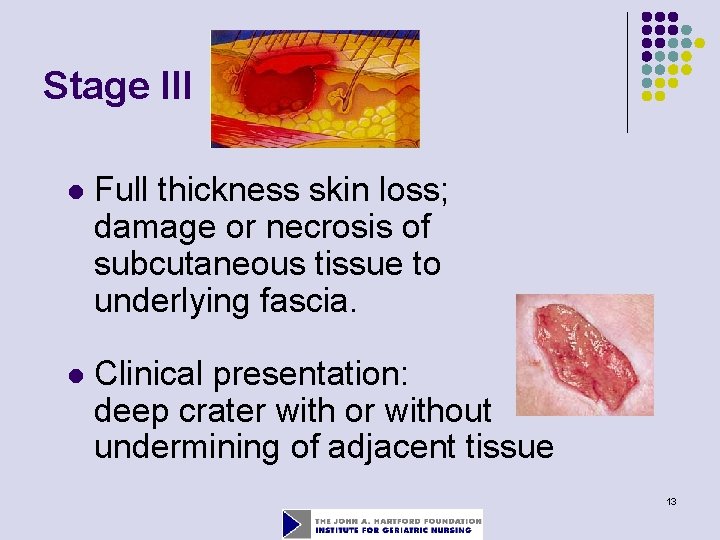
Stage III l Full thickness skin loss; damage or necrosis of subcutaneous tissue to underlying fascia. l Clinical presentation: deep crater with or without undermining of adjacent tissue 13
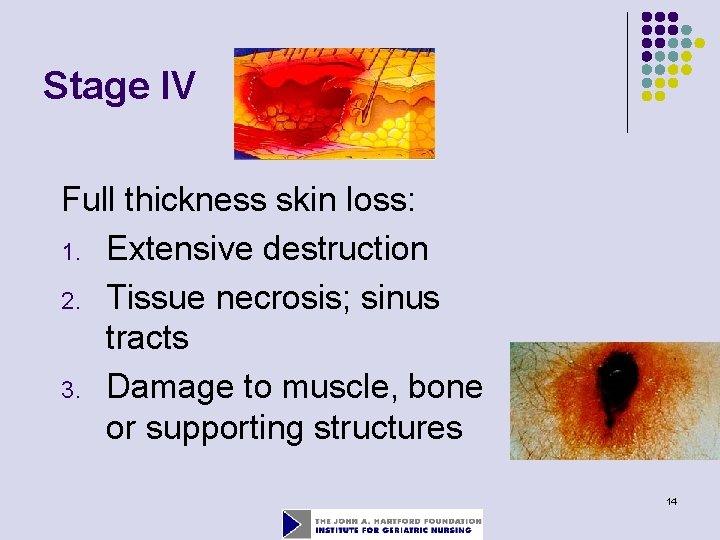
Stage IV Full thickness skin loss: 1. Extensive destruction 2. Tissue necrosis; sinus tracts 3. Damage to muscle, bone or supporting structures 14

Key Staging Points l Only stage once l Stage to maximum anatomic depth of tissue involved l Do not Reverse Stage 15

Limitations of staging system l Difficult to evaluate darkly pigmented skin l Use natural or halogen light, NOT FLOURESCENT l Cannot be staged if with eschar 16

Prevention: Risk Assessment l Bed-or chair-bound persons at risk l Use Braden Scale l Identify ALL risk factors l Assess on admission and regularly 17

Prevention: Skin Care and Early Treatment l l l l Inspect skin daily Individualize bathing frequency Assess / treat incontinence Use moisturizers; avoid massaging bony prominences Proper positioning Dry lubricants Correct nutritional deficiencies 18

Prevention: Mechanical Loading and Support Surfaces l Reposition bed-bound persons every 2 hours l Consider postural alignment l Teach chair-bound persons to shift their weight every 15 minutes l Use lifting devices l Use pillows or foam wedges l Elevate HOB as little as possible l Use repositioning schedule 19

Prevention: Education l Implement educational programs l Include etiology, risk assessment, skin assessment, support surfaces, individualized programs of skin care, demonstration of positioning l Accurate documentation l Mechanism to evaluate 20

Management of Pressure Ulcers AHRQ Guidelines Algorithm 21
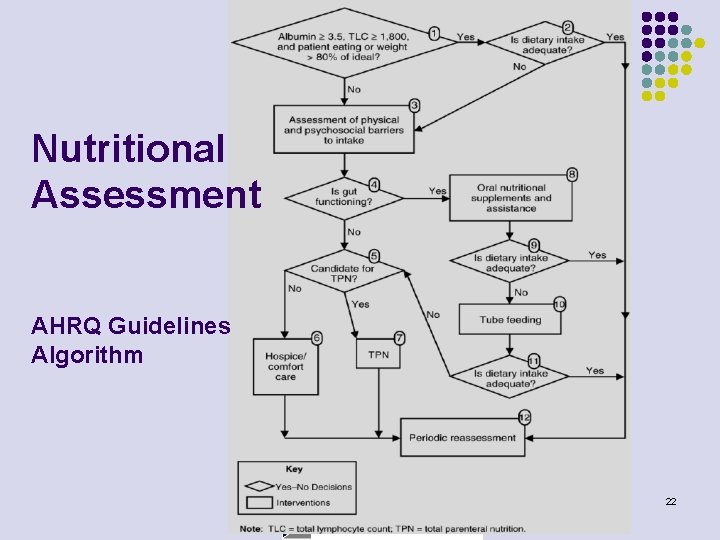
Nutritional Assessment AHRQ Guidelines Algorithm 22

Management of Tissue Loads AHRQ Guidelines Algorithm 23
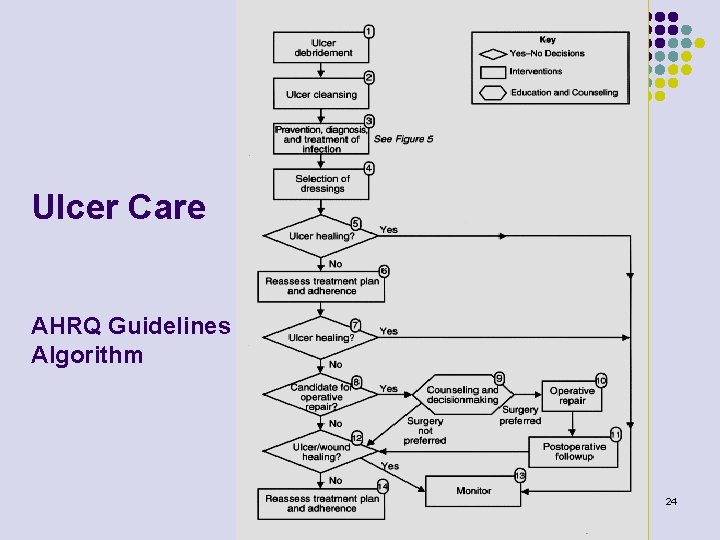
Ulcer Care AHRQ Guidelines Algorithm 24
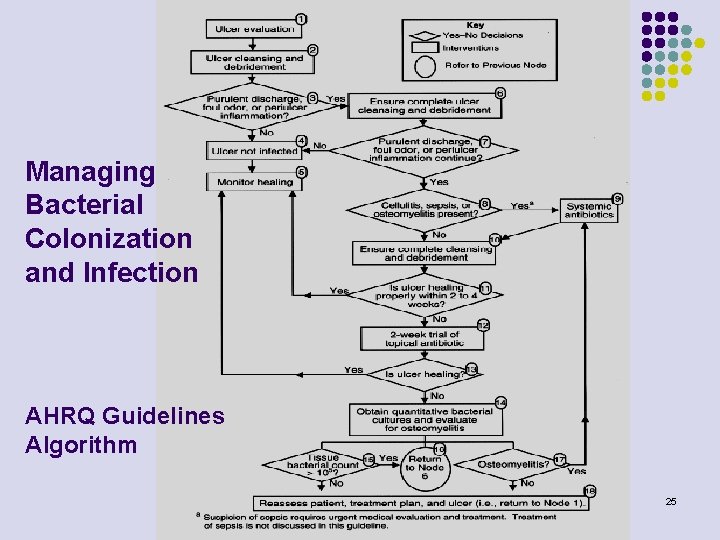
Managing Bacterial Colonization and Infection AHRQ Guidelines Algorithm 25

Questions? 26
- Slides: 26