PRESSURE ULCER AWARENESS TRAINING Eliminating Avoidable Pressure Ulcers

PRESSURE ULCER AWARENESS TRAINING Eliminating Avoidable Pressure Ulcers

The Frightening Statistics • Every year around 700, 000 people are reported as having pressure ulcers, each one costing around £ 4000 in additional care costs. Around 80% of these are avoidable if preventative best practice had been followed.

Pressure Ulcers in Coventry and Warwickshire • Between April 2013 and February 2014 187 pressure ulcers were recorded in Coventry and Warwickshire. This equates to almost £ 750, 000 in additional care costs • Each one of these 187 people may have suffered unnecessarily • Each one of these pressure ulcers could potentially have been prevented with a great amount of knowledge and understanding of preventative best practice

What Are We Trying To Do? • Supported by the CCG, C&WPT, Coventry City Council and UHCW, React to Red Skin is designed to increase education to help prevent avoidable pressure ulcers • This is part of a co-ordinated effort across the area to increase the amount of knowledge around pressure ulcer prevention

The Aim of Training • This training is a basic level of training aimed at staff who care for people who are at risk of pressure ulcers but who are not required to classify or treat pressure damage • It will provide you with basic information about prevention • It will provide you will tools to assessment a person’s level of risk

Introduction • Care professionals have a key role to play in: – The prevention of pressure ulcers – The education of those being cared for – The education of others involved in the care • Clients with impaired mobility are at a higher risk of developing pressure ulcers so carers need to be particularly vigilant • Clients with mental health issues will also present additional challenges where carers may need to take a more proactive role

What Are Pressure Ulcers • A pressure ulcer is a localised injury to the skin and/or tissue usually over a bony prominence as a result of pressure or pressure in combination with shear. • An area of damage to the skin and underlying tissues that is caused by unrelieved pressure, friction or shear forces

Who Is At Risk? • The greatest risk is to those who are immobile • Any person who is unable to change position without help • People unable to feel pain due to nerve damage • Diabetics and people with arterial disease • Elderly people in general are at greater risk because the skin is thinner and more fragile

How Pressure Ulcers Can Affect People’s Lives • • They can be painful Can cause depression and anxiety Stop people taking part in activities Possible hospital admission due to infection • May cause death

Understanding Oxygen and Blood Flow • The human body needs oxygen to survive • Oxygen is carried in the blood supply • The blood supply also carries carbohydrates and amino acids • It removes carbon dioxide • All of this is needed for healthy metabolism

Oxygen Deprivation and the Skin • Skin deprived of oxygen will begin to die if the blood supply is cut off for more than a few hours
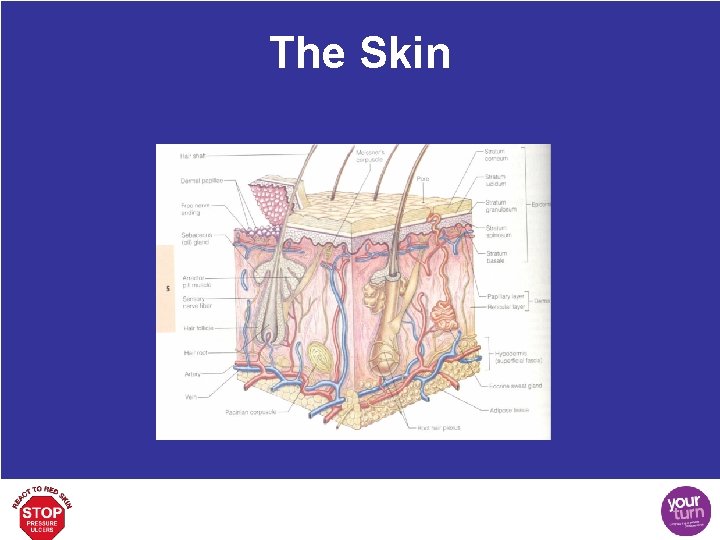
The Skin
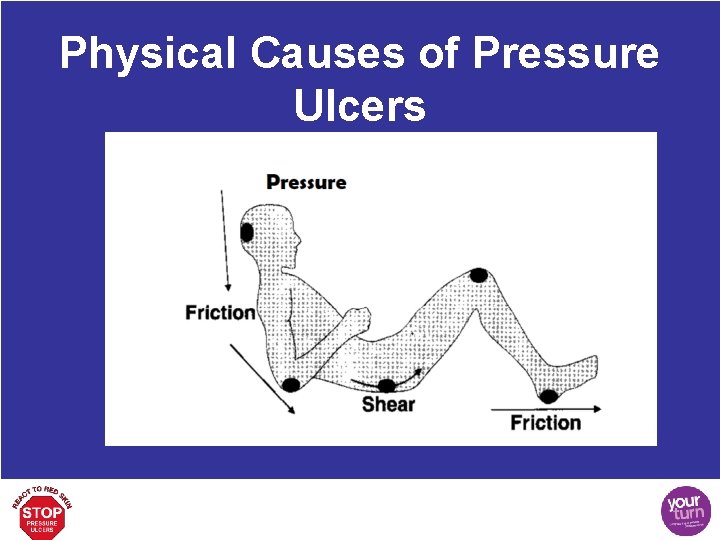
Physical Causes of Pressure Ulcers

Other Causes • Level of mobility – level of consciousness, terminal illness • Extremes of age • Nutrition and hydration status • Moisture to the skin • Sensory – neuropathy, MS, CVA • History of pressure ulcers
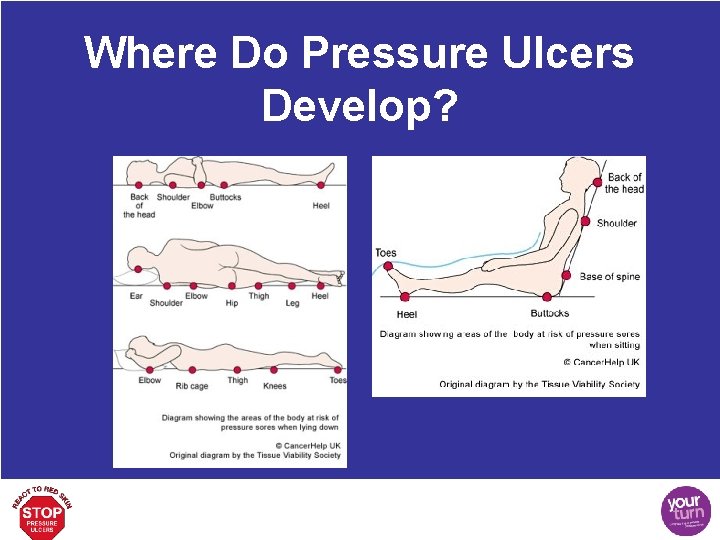
Where Do Pressure Ulcers Develop?

Medication and Pressure Ulcers • Some medication can inadvertently increase the risk of a pressure ulcer if it reduces sensitivity to pain or pressure • Care plans should be clearly noted with details of sedatives or other medication being given in order that correct pressure area care is undertaken

What is NOT a Pressure Ulcer? • • • Burn Skin tear Cut Graze Bruise Corn • • • Leg ulcers Diabetic foot ulcers Surgical wounds Bruise Incontinence

Five Simple Steps S – SURFACE S – SKIN INSPECTION K – KEEP MOVING I – INCONTIENCE N – NUTRITION AND HYDRATION

Surface • Pressure mattresses and cushions are used by people at risk of or who have pressure ulcers – cut foam, memory foam, air alternating (not cushions) • Check covers for damage • Remove slide sheets and hoist slings • Reposition on mattresses • If there is a problem consult the instruction booklet and/or call the engineer

Skin Inspection • Vulnerable areas – bony prominence • Discolouration, blisters, changes in skin temperature, swelling (boggy feel), discomfort (pain, itching, loss of sensation) • Document what is found even if skin is normal • Report any concerns through the PUT form
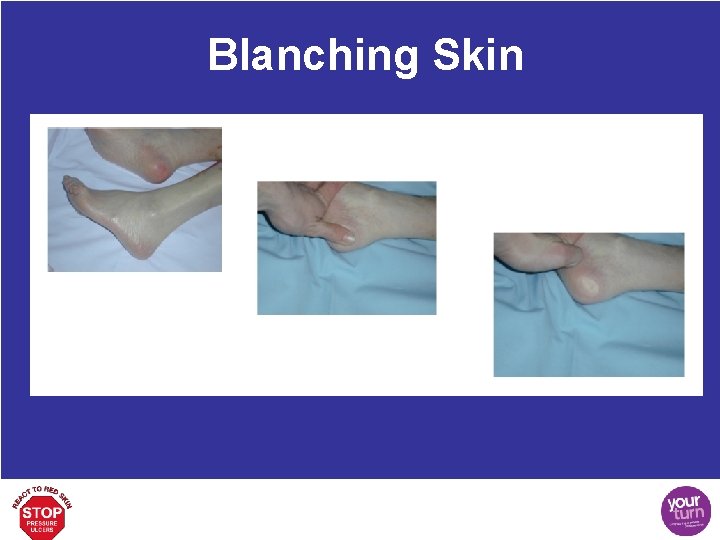
Blanching Skin
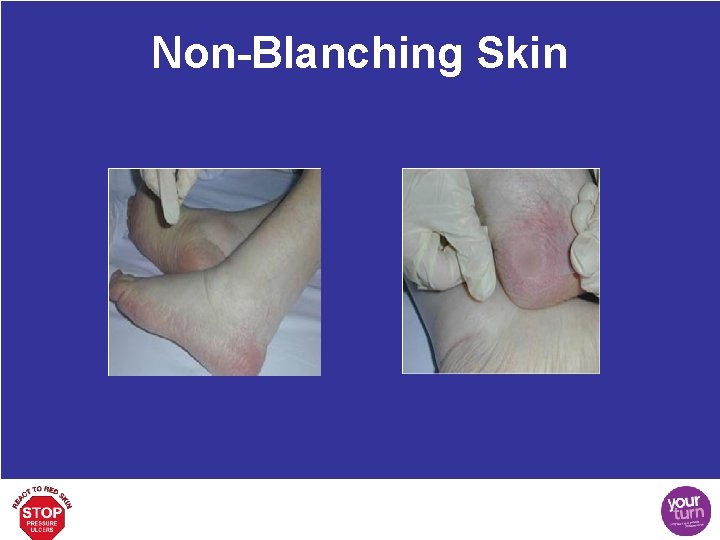
Non-Blanching Skin

Keep Moving • Assist those who cannot reposition/move themselves • Reposition people on mattresses • Limit chair sitting – 2 hours maximum • Encourage regular, gentle movements

• 30 Degree Tilt

Incontinence and Moisture • Ensure people are clean and dry • Limit the use of vigorous movements when washing and drying • If soiled wash using a soap substitute • Apply barrier cream/spray if prescribed • Report any concerns

Nutrition and Hydration • Ensure people are eating and drinking • Monitor intake of food and fluid where possible • Check mouths for any problems such as thrush, ill fitting dentures • Ensure supplements are offered where prescribed

Four Steps of Prevention

Care Homes • Step 1 - Training – Simple advice and knowledge that can improve the outcomes for the people you are caring for – Will be recorded on your employment history (certificates are available) – Demonstrates a commitment and willingness to prevent pressure ulcers with simple techniques

Care Homes • Step 2 – Policy – Agree what is your ‘Policy on Pressure Ulcer prevention’? – Publish your policy for relatives to see – Put it on your website – Gain React to Red Skin Accreditation – Tell the commissioners about your proactivity in this area

Care Homes • Step 3 – Using The New Tools • We have produced some tools to make your jobs easier when it comes to pressure ulcer prevention – Patient information leaflets – – Posters Workbooks Pressure Ulcer Trigger checklists Safety Cross

Care Homes • Step 4 – Keep It Going – Pressure Ulcer Prevention needs to become part of your day to day lives – Get used to using the tools to help record the work that you are doing – Publish your pressure ulcer prevention policy on your website – Get your organisation accredited by React To Red Skin – Keep a log of how many days ‘Pressure Ulcer Free’ you are in your area and communicate it regularly to staff using the Safety Cross

Roles and Responsibilities • Communication is the key • Report concerns – Deterioration – Declining to use prescribed equipment – Breakdown of equipment – Increase in risks to unacceptable levels – 48 of red, non-blanching sking

5 Simple Steps • Incontinence – keep people dry and clean • Sore Skin – early skin inspection means early detection • Unwell – feeling ill can lead to other complications • Reduced Mobility – those who can move less are more at risk • Food and Drink – make sure people have a good diet with plenty of fluids

Mental Illness and Pressure Ulcers • Clients suffering from mental illness are at risk of developing pressure ulcers if their illness affects their motivation • Care professionals should remain vigilant of both client groups with mental illnesses/impairments as well as physical ones

Summary • The care professional has an important part to play in reducing the risks of people developing pressure ulcers • A good understanding of how pressure ulcers develop and client groups at risk means that care professionals are better equipped to: • Reduce the risks • Provide a better standard of care

Conclusion • Only by really working together can we stop pressure ulcers, and stop suffering • We are all responsible for our client's wellbeing • Please help us to prevent pressure ulcer occurring in the first place

PRESSURE ULCER AWARENESS TRAINING Eliminating Avoidable Pressure Ulcers
- Slides: 37