Presented May 2003 Pediatric Anesthesia Abdulaziz Hisham Al

Presented May 2003 Pediatric Anesthesia Abdulaziz Hisham Al Gain

Development: J Organogenesis - 1 st 8 weeks J Organ function - 2 nd trimester J Body mass - 3 rd trimester

Changes in cardiovascular system: J Removal of placenta from circulation J Increasing of systemic vascular resistance J Decreasing of pulmonary vascular resistance J True closure of PDA ~ 2 -3 weeks critical transitional circulation J Myocardial cell mass less developed prone to biventricular failure, volume loading, poor tolerance to afterload, heart ratedependent CO* * True for young infants
Changes in pulmonary system: J Small airway diameter - increased resistance J Little support from the ribs J VO 2 2 x > adults J Diaphragm and intercostal muscles do not achieve type-1 adult muscle fibers until age 2 J Obligate nasal breathers
Airway difference: J Large tongue J Higher located larynx J Epiglottis short and stubby, angled over the inlet J Angled vocal cords we must rotate ETT to correct lodging at anterior comissure J Narrowest portion is cricoid cartilage

Chest wall/Respiratory difference: J Ribs are horizontal in neonates (vertical in adults) J Ribs and cartilages are more pliable J Chest wall collapse more with increased negative intrathoracic pressure J Atelectasis is more common J FRC J number of alveoli J Alveolar ventilation/FRC: Adults = 1. 5: 1 Infants = 5: 1 ( respiratory rate)
Kidney and liver difference: J Low renal perfusion pressure, immature GF, TF, obligate Na loser in the 1 st month of life J Complete maturation @ 2 years of age J Impaired liver enzymes, including conjugation react. J Lower levels of albumen and proteins prone to neonatal coagulopathy, and less drug bound higher drug levels

GI system and thermoregulation: J Full coordination of swallowing ~ 4 -5 months increased risk for GE reflux J Large body surface area/weight J Limited ability to cope stress J Minimal ability to shiver in 1 st 3 months J Heat whole body including the head

Pharmacology/dynamics: J Increased total body water: J Large initial dose required J Less fat longer clinical drugs effect J Redistribution of the drug into muscle will increase duration of clinical effect (fentanyl) J Consider liver and kidney immaturity

Volatile anesthetics Isoflurane: J Less myocardial depression than Halothane J Preservation of heart rate J CMRO 2 reduction rate Desflurane: J Increased incidence of coughing, laryngospasm, secretions J Concern of hypertension and tachycardia from sympathetic activation

Volatile anesthetics (2) Sevoflurane J Less pungent than Isoflurane J Concern of compound A (nephrotoxicity) J Most suitable for induction Remember: MAC for potent volatile anesthetics is increased in neonates, but may be lower for sicker neonates and premies

Induction drugs: Methohexital: J 1 -2 mg/kg i. v. or 25 -30 mg/kg per rectum J Side effects: burning hiccup apnea extrapyramidal syndrome J Contraindication: temporal lobe epilepsy Thiopental: J 5 -6 mg/kg i. v. J Caution in low fat children and malnourished

Induction drugs: Propofol: J 3 mg/kg i. v. (until 6 years of age) J Pain on injection - 0. 2 mg/kg Lidocaine i. v. Ketamine: J 10 mg/kg IM, PR, orally J Increased salivation Contraindications: Increased ICP Open globe injury

Induction drugs: Benzodiazepines: Diazepam: J 0. 1 -0. 3 mg/kg orally J T 1/2 80 hours contraindicated < 6 months Midazolam: J Only FDA benzodiazepine approved in neonates J 0. 1 -0. 15 mg/kg IM J 0. 5 -0. 75 mg/kg orally J 0. 75 -1. 0 mg/kg rectally J Reduce dose in drugs cause Cytochrome P 450 inhibition

Induction drugs: Narcotics: Morphine: J Increased permeability of blood/brain barrier J 50 mcg/kg IV Meperidine: J Less respiratory depression than morphine J Be cautious in long term administration because of its metabolite normeperidine

Induction drugs: Narcotics(2): Fentanyl: J 12. 5 mcg/kg IV during induction provides stable cardiovascular response J 1 -2 mcg/kg adjuvant to anesthesia J Stable cardiovascular response Alfentanyl and Sufentanyl: J More rapid clearance than adults J Can cause parasympatholysis bradycardia, hypotension

Induction drugs: Muscle relaxants: Succinylcholine: J 2. 0 mg/kg IV; 4. 0 mg/kg IM J Consider Atropine 10 -15 mcg/kg given prior SUX J Potential side effects: Rhabdomyolysis Hyperkalemia Masseter spasm MH

Induction drugs: Muscle relaxants(2): J If tachycardia desired - Pancuronium J Mivacurium - brief surgeries, beware of histamine release, bronchospasm J Rocuronium - useful for modified RSI, and can be administered IM (1 mg/kg)
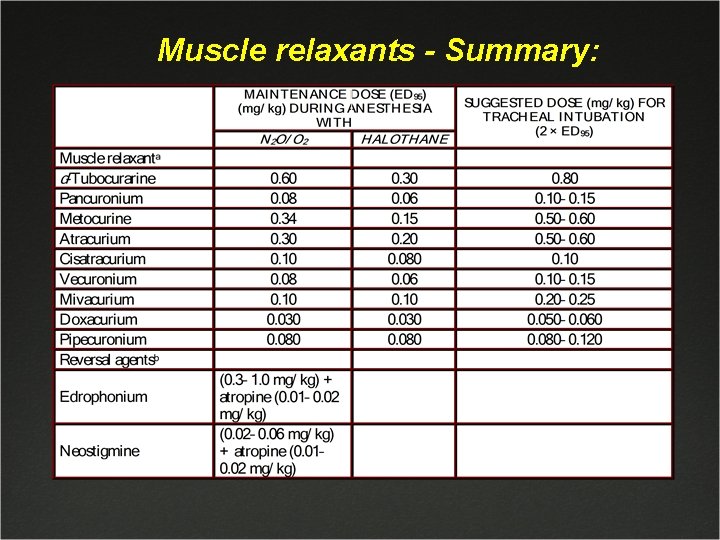
Muscle relaxants - Summary:

Premedication: J Almost all sedatives are effective J Usually not necessary < 6 months J Most common route used is oral J Side effects: Oral - slow onset IM - pain, sterile abscess Rectal - uncomfortable, defecation, burn Nasal -irritating Sublingual -bad taste

Pharmacological premedication options 1. Role when awake separation of child from parent before induction is planned. 2. Its success may be judged by the peacefulness of the separation. 3. Large volume of literature indicates lack of clearly ideal technique http: //metrohealthanesthesia. com/edu/pedspreop 6. htm

Pharmacological premedication options Midazolam (Versed) • • • PO: 0. 5 to 1. 0 mg/kg up to 10 mg max. Bioavailability = 30% Peak serum levels after about 45 minutes Peak sedation by about 30 minutes 85% peaceful separation Mix with grape concentrate or acetaminophen (Tylenol) syrup or elixir or Motrin Suspension (10 mg/kg of the 2% suspension)

Pharmacological premedication options (3) Midazolam (Versed)(2) • • • Nasal: 0. 2 to 0. 6 mg/kg Peak serum level in 10 minutes 0. 2 mg/kg same as 0. 6 mg/kg except 0. 2 mg/kg did not delay recovery 0. 6 mg/kg may delay extubation • Possible concern: animal studies reveal neurotoxicity after topical applicaton.

Pharmacological premedication options (4) Midazolam (Versed)(3) • Sublingual: 0. 2 -0. 3 mg/kg as effective as 0. 2 mg/kg intranasal • Rectal: 0. 35 to 1. 0 mg/kg • Some effect by 10 minutes, peak effect 2030 minutes. • 1. 0 mg/kg did not delay PACU discharge.

Pharmacological premedication options (5) Methohexital (Brevital) • Rectal 25 to 30 mg/kg as 10% solution in warm tap water • 85% sleeping within 10 minutes = rectal induction of GA (very peaceful separation) • Sleep duration: about 45 to 90 minutes • 25 mg/kg did not delay recovery in one study, but some delay may be expected after a short (less than 30 -minute) case.

Pharmacological premedication options (6) Ketamine • PO: 6 to 10 mg/kg • May slightly prolong time to discharge after a short case • IM: 3 to 4 mg/kg sedation; • 2 mg/kg did not delay recovery • 6 to 10 mg/kg = IM induction of general anesthesia • 10 mg/kg: as effective as Midazolam 1 mg/kg but some delay in recovery may be expected

Pharmacological premedication options (7) Midazolam + Ketamine: • PO 0. 4 mg/kg + 4 mg/kg respectively • 100% successful separation • 85% easy mask induction • Doubling dose leads to "oral induction of general anesthesia" in most cases. Lasts 30 to 60 minutes.

Pharmacological premedication options (8) Fentanyl "lollipops" (oral transmucosal Fentanyl) • 15 to 20 mcg/kg • Increased volume of gastric contents • Nausea and vomiting • Pruritus • Hypoventilation (Sp. O 2 <90)

Pharmacological premedication options (9) 1. Metoclopramide (Reglan) PO or IV: 0. 2 mg/kg 2. Ranitidine (Zantac) PO 2. 5 mg/kg 3. EMLA cream: Eutectic mixture of Lidocaine and Prilocaine. For cutaneous application by occlusive dressing one hour preoperative 4. Glycopyrrolate: consider for selected patients for planned airway instrumentation; e. g. : fiberoptic endoscopy, oral or upper airway surgery, cleft palate)5 -10 mcg/kg IV or 10 mcg/kg IM
Preoperative interview: http: //metrohealthanesthesia. com/edu/pedspreop 4. htm

Fasting: J Clear liquids - 2 -3 h before the procedure J If infants are breast fed - 4 h before the procedure J For older patients = the adults rule J Be aware of dehydration

Induction of Anesthesia: Inhalational induction: J Younger than 12 months J After the induction, place the intravenous catheter J Use suggestions in older child (pilot’s mask) J In a case of difficult airway - Fiberoptic intubation

Induction of Anesthesia: Rectal induction: J Methohexital J Thiopental J Ketamine J Midazolam J Technique no more intimidating than rectal temperature measurement J Usual time of onset ~ 10 -15 min

Induction of Anesthesia: Intramuscular induction: J Most common used Ketamine J Disadvantage painful needle insertion J Advantage: reliability

Induction of Anesthesia: Intravenous induction: J The most reliable and rapid technique J Disadvantage - starting intravenous line J If patient is older ask the patient J If you insert IV line: I. Do not allow the patient to see it II. Use EMLA cream III. If use local - ask the patient if there is any sensation on puncture

Patient with full stomach: Treat the same as adult with full stomach: J RSI with ODL using cricoid pressure J Tell the patient that will feel “touching on the neck” J Be aware of VO 2 (desaturation) J 0. 02 mg/kg of Atropine administer before SUX to avoid bradycardia (usually after 2 nd dose) J Use Rocuronium 1. 2 mg/kg J Use Succinylcholine 1 -2 mg/kg if really
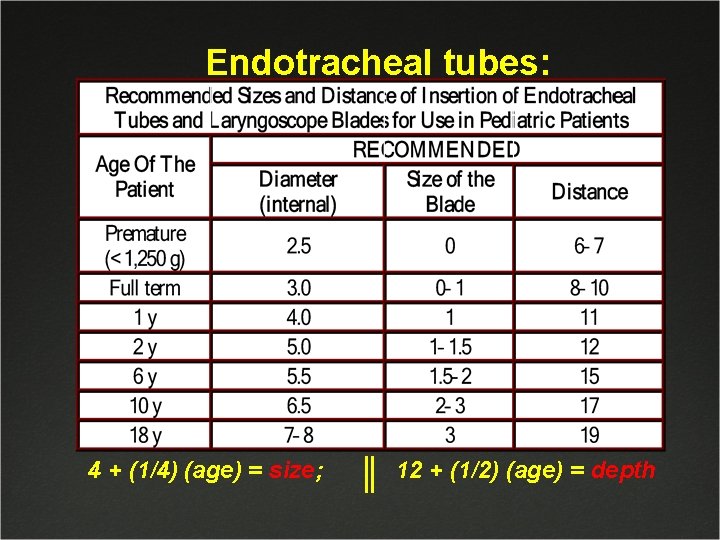
Endotracheal tubes: 4 + (1/4) (age) = size; 12 + (1/2) (age) = depth
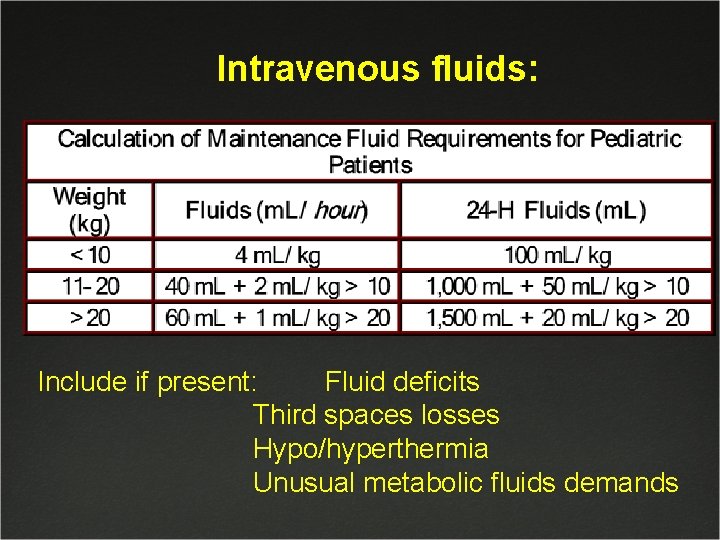
Intravenous fluids: Include if present: Fluid deficits Third spaces losses Hypo/hyperthermia Unusual metabolic fluids demands

Fluid requirements in neonates: During the 1 st week reduced fluid requirements: Day 1 - 70 ml/kg Day 3 - 80 ml/kg Day 5 - 90 ml/kg Day 7 - 120 ml/kg J Concern is immaturity of the neonatal kidney J The volume of extracellular fluids in neonates is large J Consider use of radiant warmers, and heated humidifiers - decrease insensible water loss J Use LR for replacement, D 5% with 0. 45 NS by piggyback
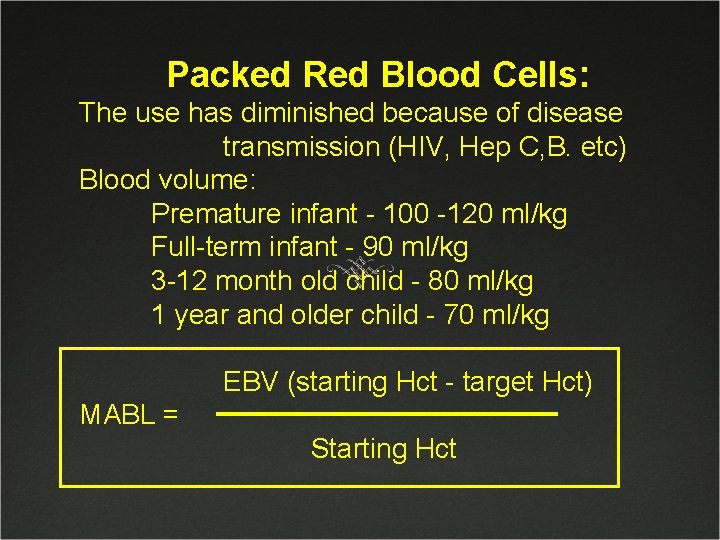
Packed Red Blood Cells: The use has diminished because of disease transmission (HIV, Hep C, B. etc) Blood volume: Premature infant - 100 -120 ml/kg Full-term infant - 90 ml/kg 3 -12 month old child - 80 ml/kg 1 year and older child - 70 ml/kg EBV (starting Hct - target Hct) MABL = Starting Hct
Packed Red Blood Cells (2): J Child usually tolerates Hct ~ 20 in mature children J If: Premature, Cyanotic congenital disease Hct ~ 30 O 2 carrying capacity J No one formula permits a definitive decision J Replace 1 ml blood with 3 ml of LR J Lactic acidosis is a late sing of decreased O 2 carrying capacity J Be aware of blood disorders (sickle cell

Fresh Frozen Plasma: J Use to replenish clotting factors during massive transfusion, DIC, congenital clotting factor deficits J Usually replenished if EBL = 1 -1. 5 TBV J A patient should be never given FFP to replace bleeding that is surgical in nature J If transfused faster than 1. 0 ml/kg/min severe ionized hypocalcemia may occur J If occurs - Rx. with 7. 5 -15 mg/kg Ca++ gluconate J Ionized hypocalcemia can occur in neonates frequently because of decreased ability to mobilize Ca++ and metabolize
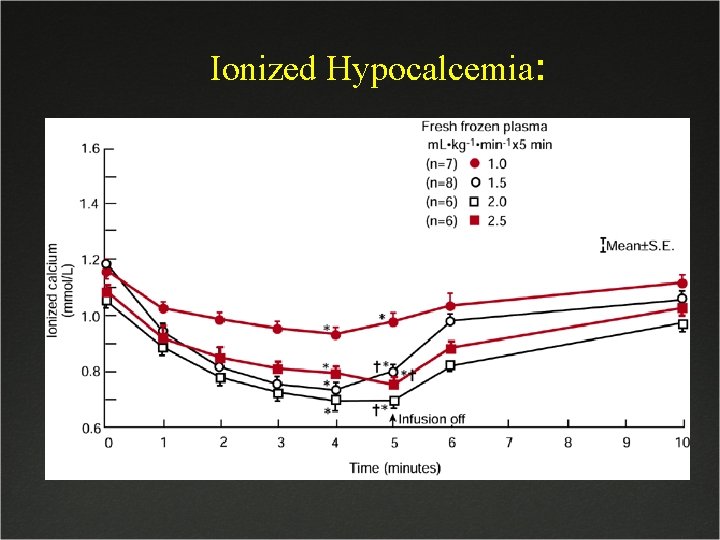
Ionized Hypocalcemia:

Platelets: J Find etiology - TTP, ITP, HIT, DIC, hemodilution after massive blood transfusion J Consider transfusion if Platelets < 50. 000 J In certain hospitals platelet function test is available J If Platelets < 100. 000 and EBL = 1 -2 TBV transfusion more likely J If Platelets > 150. 000 and EBL > 2 TBV

Monitoring the Pediatric Patients: J Must be consistent with the severity of the underlying medical condition J Minimal monitoring: I. 5 ASA monitors II. Precordial stethoscope III. Anesthetic agent analyzer J Use of capnograph and O 2 analyzers is associated with high incidence of false alarms from: movement artifact light interference electrocautery

Special Monitoring the Pediatric Patients: J Intraarterial catheter - most common radial J Pulmonary artery catheters are rarely indicated because equalization of the pressure right/left heart J In a case of severe multisystem organ failure insertion of PAC might be particularly useful J Multilumen catheters are valuable in ICU patients J In a case of rapid fluid replacement peripheral venous catheter might be very useful J Short-term cannulation of

Anesthesia Circuits: J Nonrebreathing circuits: 1. Minimal work of breathing 2. Speeds-up rate of inhalational induction 3. Compression and compliance volumes are less (small circuit volume) J Use of Mapleson D system is recommended in children < 10 kg More sensitive to changes in gas flow More sensitive to humidification Actual delivered volume is greater than other systems

Mapleson D Circuit: Gas disposition at end-expiration during spontaneous ventilation Gas disposition at controlled ventilation

Neonatal Anesthesia: J Understand differences in Physiology Pharmacodynamic response J Most of the complications that arise are attributable to a lack of understanding of these special considerations prior to induction of anesthesia J Be aware of: Sudden changes in hemodynamics Unexpected responses Unknown congenital problem

Neonatal Anesthesia (2): J Children < 1 year old have more complications: I. Oxygenation II. Ventilation III. Airway management IV. Response to volatile agents and medications J Stress response is poorly tolerated J Consider: 1. Organ system immaturity 2. High metabolic rate 3. Large ratio body surface/weight

Neonatal Anesthesia (3): J Prevention of paradoxical air emboli J Fluids instituted with volume-limiting devices J Minimize thermal stress J Use flow-through capnograph if possible J Prevent retinopathy of prematurity by: Lower Fi. O 2 Keep CO 2 within normal range

Neonatal Anesthesia (4): Stress Response: J Poorly tolerated J Use opioid technique (blunt pain response) J Ketamine is excellent choice –stable intraoperative hemodynamics J Potent volatile anesthetics are poorly tolerated J No one should be denied anesthesia because of the age or weight

Special Problems in Neonatal Anesthesia: Meningomyelocele: J Underestimating fluid or blood loss from the defect J High association with hydrocephalus J Possibility of cranial nerve palsy J Potential for brain-stem herniation

Special Problems in Neonatal Anesthesia (2): Pyloric stenosis: J First 3 -6 weeks in life J Anesthesiologist concern: I. Full stomach with barium II. Metabolic alkalosis with Hypochloremia and Hypokalemia III. Severe dehydration J Surgery is never emergency J Metabolic correction mandatory before the surgery J Suction the stomach before induction

Special Problems in Neonatal Anesthesia (3): Omphalocele and Gastroschisis: J Omphalocele occurs because of failure of the gut to return to the abdominal cavity at 10 th week of life J Fine membrane covers intestines and abdominal contents J Gastroschisis develops later in life after gut has returned into abdominal cavity J Abdominal contents and organs are not covered with any membrane – risk of infection

Special Problems in Neonatal Anesthesia (3): Omphalocele

Special Problems in Neonatal Anesthesia (3): Gastroschisis

Special Problems in Neonatal Anesthesia (3): Omphalocele and Gastroschisis(2): J Anesthesiology concern: 1. Dehydration 2. Massive fluid loss (exposed viscera and 3 rd space loss) 3. Heat loss 4. Difficulty of surgical closure 5. High association with prematurity, congenital defects, including cardiac anomalies J Minimize infection, Replenish fluids, be liberal in muscle relaxants, consider hypotension and difficulty ventilation

Special Problems in Neonatal Anesthesia (3): Omphalocele and Gastroschisis(3): J During closure consider * difficulty ventilation * hypotension * abdominal pressure may compromise liver function and alter drug metabolism J During closure of big defects monitoring of the bladder pressures is important: if the pressure is < 20 cm H O attempt is to close, > 20 cm

Special Problems in Neonatal Anesthesia(3): Omphalocele and Gastroschisis (4): J Be aware of Beckwith-Wiedemann syndrome: Profound hypoglycemia Hyperviscosity syndrome Associated visceromegaly

Special Problems in Neonatal Anesthesia(3): Omphalocele and Gastroschisis ddx. (5): 1. Much greater associated defects with Omphalocele 2. More fluid loss associated with Gastroschisis

Special Problems in Neonatal Anesthesia(4): Tracheoesophageal fistula anomaly(1): J 90 % proximal atresia of esophagus with distal fistula J Consider aspiration pneumonitis. Trachea J VATER syndrome: T-type I. Vertebral II. Anal III. Tracheoesophageal IV. Renal J MCC of death – cardiac anomalies

Special Problems in Neonatal Anesthesia(4): Tracheoesophageal fistula anomaly(1): J 90 % proximal atresia of esophagus with distal fistula J Consider aspiration pneumonitis. Trachea J VATER syndrome: T-type I. Vertebral II. Anal III. Tracheoesophageal IV. Renal J MCC of death – cardiac anomalies

Special Problems in Neonatal Anesthesia(4): Tracheoesophageal fistula anomaly(2): J Major issues are: J Aspiration pneumonia Trachea J Overdistention of the stomach T-type J Inability to ventilate J Postoperative intensive care
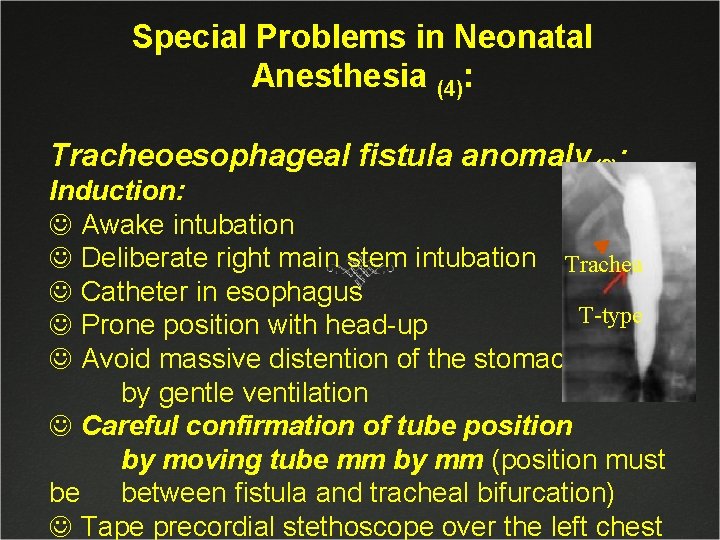
Special Problems in Neonatal Anesthesia (4): Tracheoesophageal fistula anomaly(3): Induction: J Awake intubation J Deliberate right main stem intubation Trachea J Catheter in esophagus T-type J Prone position with head-up J Avoid massive distention of the stomach by gentle ventilation J Careful confirmation of tube position by moving tube mm by mm (position must be between fistula and tracheal bifurcation) J Tape precordial stethoscope over the left chest
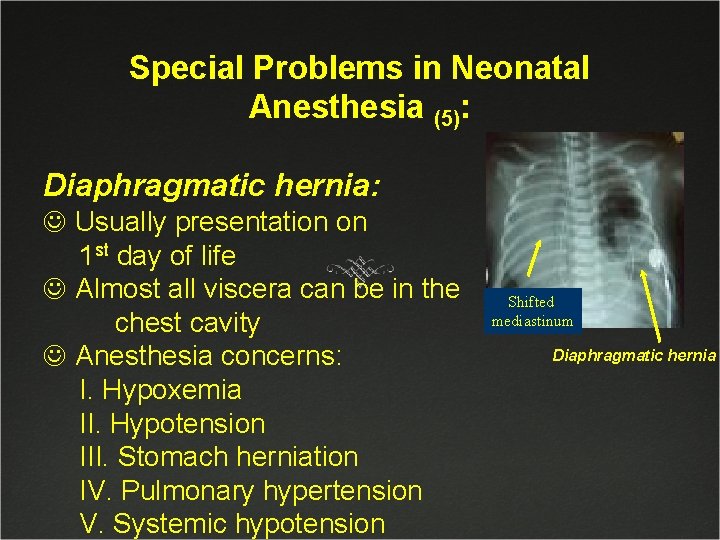
Special Problems in Neonatal Anesthesia (5): Diaphragmatic hernia: J Usually presentation on 1 st day of life J Almost all viscera can be in the chest cavity J Anesthesia concerns: I. Hypoxemia II. Hypotension III. Stomach herniation IV. Pulmonary hypertension V. Systemic hypotension Shifted mediastinum Diaphragmatic hernia

Special Problems in Neonatal Anesthesia (5): Diaphragmatic hernia (2): 1. Awake intubation 2. Intraarterial catheter 3. Use opioids (stress response) Shifted mediastinum 4. Use Pancuronium Diaphragmatic hernia 5. Avoid hypothermia 6. Avoid any myocardial depressant 7. Avoid N 2 O (abdominal distention) 8. Aware of barotrauma-induced pneumothorax 9. Adequate intravenous access 10. Plan postoperative care

Special Problems in Neonatal Anesthesia (6): Former preterm infant (<37 weeks): J High incidence of apnea risk factors: Respiratory distress syndrome Bronchopulmonary dysplasia Neonatal dyspnea Necrotizing enterocolitis Ongoing apnea at the time of surgery Use of narcotics Long acting muscle relaxants Anemia (Hct < 30)

Regional Anesthesia and Anesthesia: (brief overview) J Most regional anesthetics are safe to use J Strict attention to: Dose Route of administration Proper equipment used J Common: Caudal blocks
- Slides: 69