Presented by Katarina Bojani Mentor A mega Horvat

Presented by: Katarina Bojanić Mentor: A. Žmegač Horvat

FACTS & EPIDEMIOLOGY • Most common malignancy in women (25 -30%) • 2 nd leading cause of cancer deaths (after lung c. ) • > 570, 000 new cases worldwide each year • 2, 300 new cases >800 deaths in Croatia (2005)

• One out of eight women will be diagnosed • Strikes a small percentage of men • ≈1, 500 new cases expected to be diagnosed in men next year
Every three minutes a woman in the US is diagnosed with BC Every 12 minutes a woman dies from BC All women are at risk (rare in women <40; 10% of palpable masses malignant)
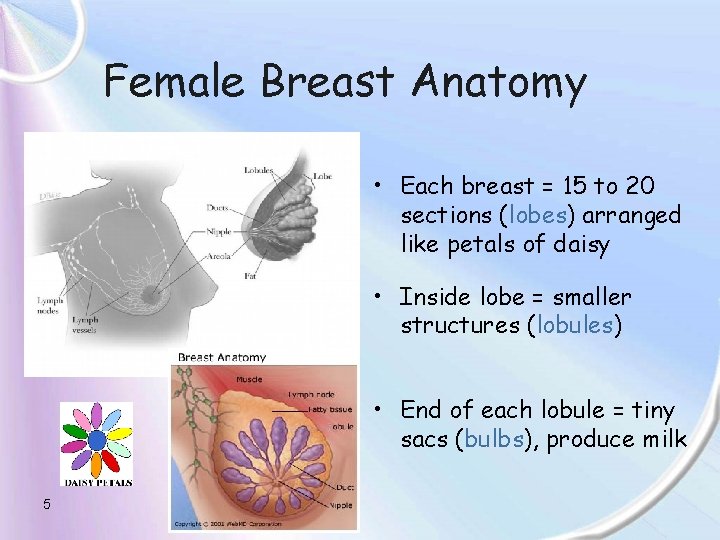
Female Breast Anatomy • Each breast = 15 to 20 sections (lobes) arranged like petals of daisy • Inside lobe = smaller structures (lobules) • End of each lobule = tiny sacs (bulbs), produce milk 5
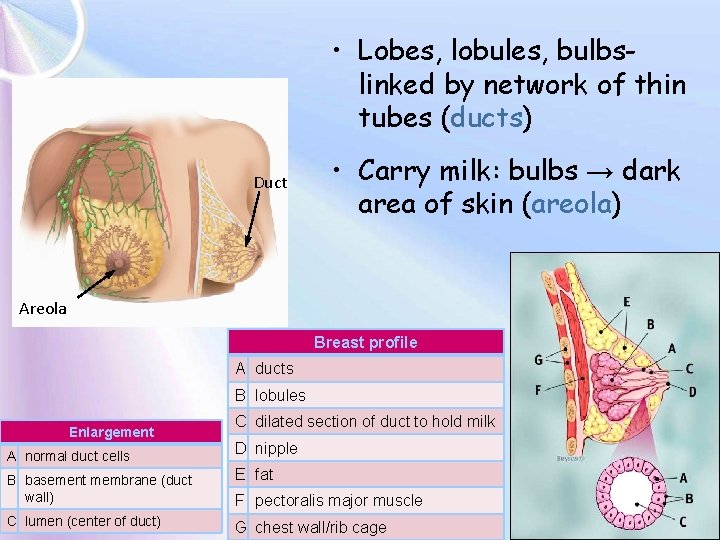
• Lobes, lobules, bulbslinked by network of thin tubes (ducts) Duct • Carry milk: bulbs → dark area of skin (areola) Areola Breast profile A ducts B lobules Enlargement A normal duct cells B basement membrane (duct wall) 6 C lumen (center of duct) C dilated section of duct to hold milk D nipple E fat F pectoralis major muscle G chest wall/rib cage

Risk Factors Nonmodifiable risks Gender Age, Race Family/Personal history of BC Genetic factors Menstrual history Certain types of breast disease Radiation Modifiable risks Weight (obesity) Exercise Alcohol Reproductive history Hormone replacement therapy Oral contraceptive use Breastfeeding

Genetic risk factors → 10 % of BC familial (hereditary) • BRCA 1 & BRCA 2 → tumor suppressor genes (breast cancer gene) →role in cellular DNA repair →mutation increases risk • P 53, RAS, C-MYC, RB gene

Types of Breast Cancer Invasive Cancers spread from ducts or lobes into fatty tissue Noninvasive Cancers (in situ) limited to ducts or lobes & does not spread into fatty tissue
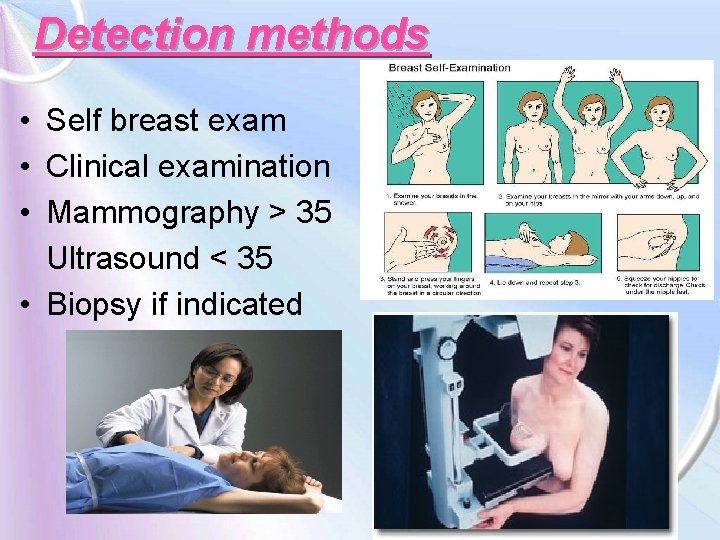
Detection methods • Self breast exam • Clinical examination • Mammography > 35 Ultrasound < 35 • Biopsy if indicated

Mammography X-ray picture of the breast to detect breast cancer Detects a breast lump before it can be felt Age Frequency of Mammogram 40 50 <49 with family hy of breast cancer 1 -2 year Every year Consult health care providers about risks
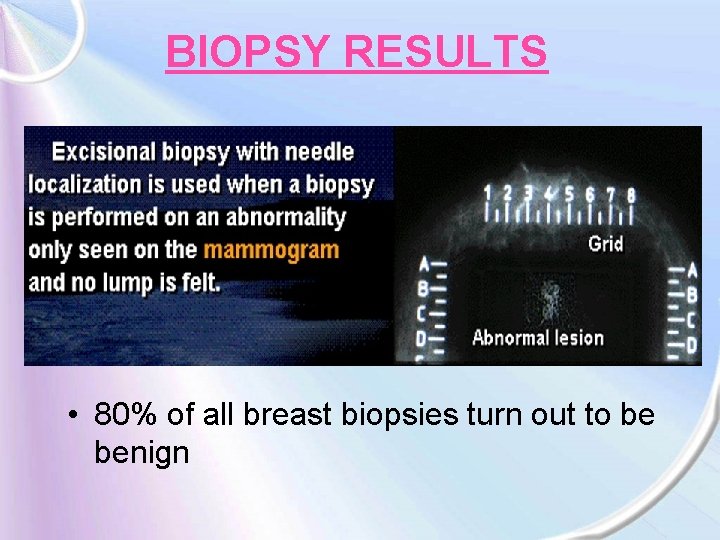
BIOPSY RESULTS • 80% of all breast biopsies turn out to be benign

Clinical Breast Exam Performed by doctor Every 3 y. for women 20 – 39 Yearly for women > 40 yrs of age

Breast Self-Exam Monthly starting at the age of 20! • Still menstruating Ø 2 -3 days after period ends • No longer menstruating Ø same day every month
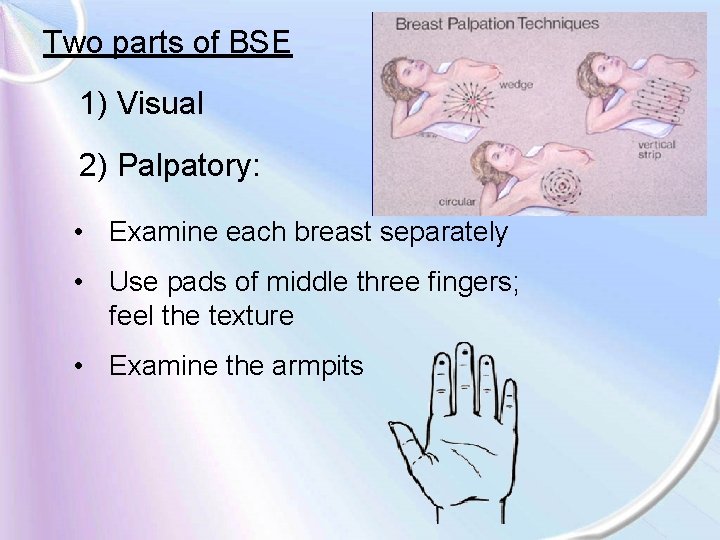
Two parts of BSE 1) Visual 2) Palpatory: • Examine each breast separately • Use pads of middle three fingers; feel the texture • Examine the armpits
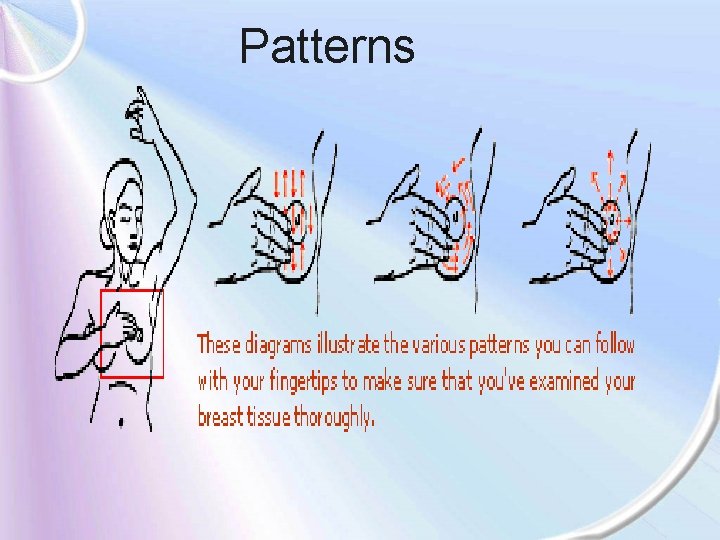
Patterns
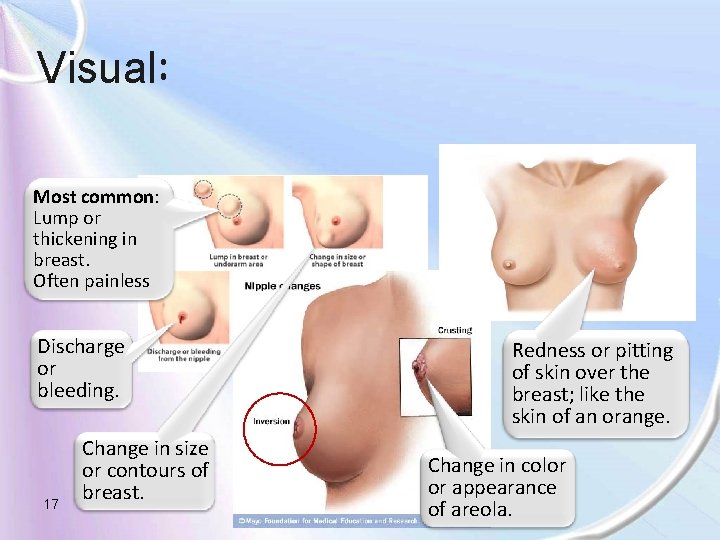
Visual: Most common: Lump or thickening in breast. Often painless Discharge or bleeding. 17 Change in size or contours of breast. Redness or pitting of skin over the breast; like the skin of an orange. Change in color or appearance of areola.

Abnormal Breast Changes Lump in the breast Nipple discharged or tenderness Changes in breast size of shape Changes in the skin of the breast
TREATMENT OPTIONS & PROGNOSIS • Depend on – Size of the tumor – Invasive or in situ SURVIVA L tm size increaseschance decreases – Histologic type - ductal (85%) vs. lobular – Estrogen/progesterone receptors (60 -70%positive) – Her-2/ neu status (receptor for epidermal growth f. )
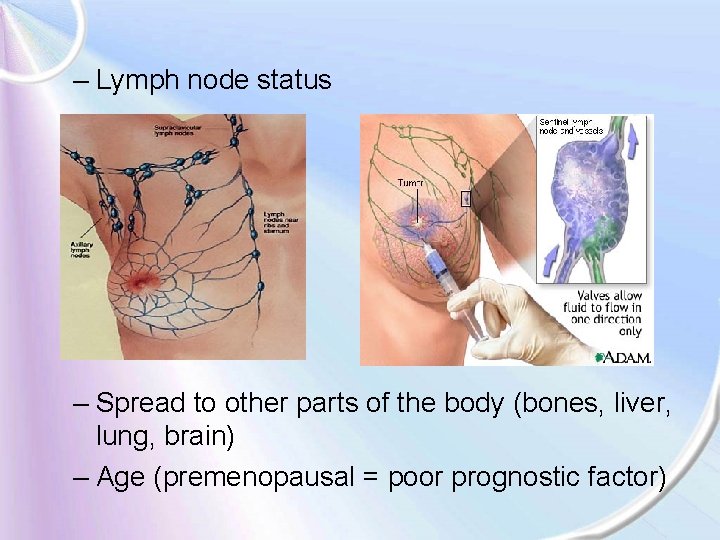
– Lymph node status – Spread to other parts of the body (bones, liver, lung, brain) – Age (premenopausal = poor prognostic factor)

TREATMENT Goals Cure, Control, Palliation • • • Surgery Radiation Therapy (local) Chemotherapy (systemic) Hormonal Therapy (systemic) Immunotherapy �� Therapy is individualized
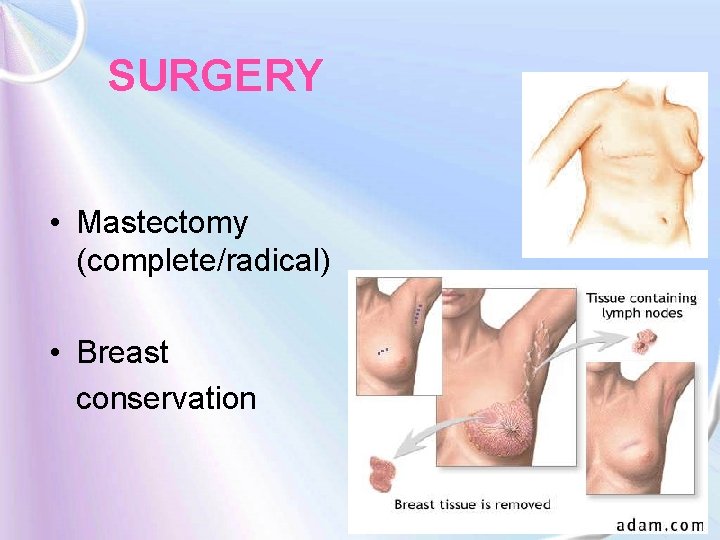
SURGERY • Mastectomy (complete/radical) • Breast conservation (partial)
RECONSTRUCTION

RADIATION THERAPY Local control of disease Indications: • Adjuvant (after partial mastectomy) • Young patients with DCIS • High risk of local recurrence • High energy rays used to kill cancer cells

CHEMOTHERAPY Anticancer drugs = systemic control of disease Indications: • After surgery to reduce risk of recurrence • Large + locally advanced cancer to reduce the size prior to surgery (neoadjuvant) • Metastatic - to reduce cancer that has spread + relieve symptoms & prolong life

HORMONAL THERAPY • Hormones (blood stream) → attach ca. cells, promote their growth • Block the receptor or production of hormones ! • Side effects: hot flashes, depression, ↑ risk of uterine cancer, induced manopause, blood clots • Tamoxifen, aromatase inhibitors. . .
IMMUNOTHERAPY Monoclonal antibodies • Trastuzumab/Herceptin • Patients whose cancer cells over-express Her-2 -neu oncogene as measured by IHC or FISH (25 to 30% of patients)

• Through early detection and improved treatments more women than ever are surviving breast cancer. . .

THANK YOU FOR YOUR ATTENTION! Questions ?

References: • Kusić Z. Onkologija. Zagreb, 2008 • Damjanov I, Jukić S, Nola M. Patologija. Medicinska naklada, Zagreb, 2008 • Kumar P, Clark M. Clinical Medicine. Saunders Elsevier, London, 2007 • www. cancer. org • www. cancer. gov
- Slides: 30