Presented by Coleen Maritz Audiologist 1 Anatomy of

Presented by Coleen Maritz Audiologist
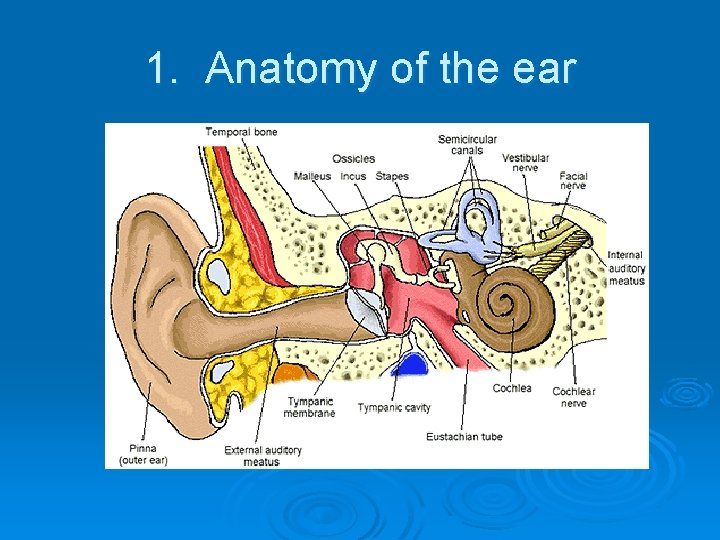
1. Anatomy of the ear
2. Types of Hearing Loss Ø Conductive Hearing Loss - Resultant of outer or middle ear pathology. When the transmission of sound is interrupted in the outer ear or more frequently in the middle ear. - Children: most common cause is otits media. Adults: most common cause is otosclerosis.
Types of Hearing Loss Cont. Ø Sensorineural Hearing Loss - Resultant of inner ear and/or auditory nerve damage. - When the hair cells of the cochlea or the acoustic nerve are damaged.

Types of Hearing Loss Cont. Ø Mixed Hearing Loss - Involves a combination of a conductive and sensorineural hearing loss.
3. Causes of Hearing Loss Ø Causes of Conductive Hearing Loss o Outer and middle ear disorders may cause a conductive hearing loss.

Outer & Middle Ear Disorders DISORDERS DEFINITION Microtia & Atresia Congenital malformations of ear & external auditory canal. Microtia-abnormal smallness of auricle. Atresia-Absence of opening of external auditory meatus. Excessive ear wax obstructing ear canal Impacted Cerum & Foreign Bodies
Outer & Middle Ear Disorders Cont DISORDERS DEFINITION Tympanic membrane perforation Otitis media Hole in the ear drum Middle ear infection. Primary caused by Eustachian tube dysfunction. Increased risk: Craniofacial anomalies, Down’s syndrome, allergiescigarette smoke exposure.
Outer & Middle Ear Disorders Cont DISORDERS DEFINITION Otosclerosis Disorder of bone growth that affects the stapes and the bony labyrinth of the cochlea. Affects sound transduction through middle ear.
Outer & Middle Ear Disorders Cont DISORDERS Cholesteatoma Other Middle ear Disorders: v. Physical trauma DEFINITION Pocket that forms in the ear usually due to Otitis media. Normal shedding of epithelium results in growth of cholesteatoma. Smells bad if it should burst. Gun shot, Blow to head.

Outer & Middle Ear Disorders Cont DISORDERS v. Baro-trauma v. Tumours v. Tympanosclerosis DEFINITION v. Sudden change in atmospheric pressure (Diver, aeroplane). v Neoplasms-Glomus tumor, often causes tinnitus as well. v. Whitish plaques on the tympanic membrane.

Causes of Hearing Loss Cont. Ø Causes of Sensorineural Hearing Loss 1. Prenatal Congenital infections * CMV – viral infection; type of herpes virus transmitted in utero; can cause hearing loss, blindness and seizures * HIV – affinity for CNS; opportunistic infections cause hearing loss eg. Meningitis * Rubella – viral infection

Causes of Hearing Loss Cont. * Syphilis – often causes progressive hearing loss; onset after 2 years of age * Toxoplasmosis – caused by parasite infection transmitted through contaminated food; causes hydrocephalus, mental retardation and hearing loss

Causes of Hearing Loss Cont. 2. Perinatal Causes Ø Ø Ø Hypoxia Birth trauma Hyperbilirubenemia Ototoxic medication Premature infants = increased risk for hearing loss

Causes of Hearing Loss Cont. 3. Acquired hearing loss Ø Ø Ø Herpes zoster oticus (Ramsay Hunt Syndrome) – same virus that causes chickenpox; can cause hearing loss Mumps – acute systemic viral disease; common in childhood over the age of 2 years; often causes unilateral hearing loss Measles Meningitis Serous labyrinthitis (inflammation of labyrinth)
![Causes of Hearing Loss Cont. Ø Ototoxic medication: [Oto=ear. Ototoxic=Toxic to the ear] Ototoxic Causes of Hearing Loss Cont. Ø Ototoxic medication: [Oto=ear. Ototoxic=Toxic to the ear] Ototoxic](http://slidetodoc.com/presentation_image_h2/b25e87013cd739f35525ab0f60f397fb/image-16.jpg)
Causes of Hearing Loss Cont. Ø Ototoxic medication: [Oto=ear. Ototoxic=Toxic to the ear] Ototoxic medications are drugs that have the potential to cause damage to the inner ear structures which may result in temporary or permanent hearing loss or an aggravation of an existing sensorineural hearing loss. Consuming more than one ototoxic medication at a time increases your risk to develop a sensorineural hearing loss.

Causes of Hearing Loss Cont. 1. Aminoglycosides (antibiotics): • • • Amikacin Gentamycin Garamycin Kanamycin Netilmycin Tobramycin Streptomycin Viomycin Neomycin

Causes of Hearing Loss Cont. Ø Aminoglycosides (antibiotics) cont: These medications are toxic when used intravenously in serious life threathening situations. The blood levels of these medications are usually monitored to prevent ototoxicity. Topical preparations and ear drops containing these antibiotics, Neomycin, Gentamycin, have not been demonstrated to be toxic in humans.

Causes of Hearing Loss Cont. 2. Erythromycin (antibiotics): • • • EES Eryc E-mycin Ilosone Pediazole • Biaxin • Zithromax New derivatives of Erythromycin

Causes of Hearing Loss Cont. Ø Erythromycin (antibiotics) cont: These are usually ototoxic when given intravenously in dosages of 2 -4 grams per 24 hours, especially if there is underlying kidney insufficiency. The usual oral dosage of one gram per 24 hours is not toxic. There are no significant reports of ototoxicity with new Erythromycin derivatives, since they are given orally at lower dosages.

Causes of Hearing Loss Cont. 3. Vancomycin – Vancocin (antibiotics) This antibiotic is used in a similar manner as the aminoglycosides; when given intravenously in serious life-threatening infections. It is potentially ototoxic. It is usually used together with the aminoglycosides which enhances the possibility of ototoxicity.

Causes of Hearing Loss Cont. 4. Salicylates (used in treatment of arthritis): Toxic effects usually appear after consuming an average of 6 -8 pills per day. Toxic effects are reversible once medication is discontinued. • Acetylsalicylic acid • Aspirin

Causes of Hearing Loss Cont. 5. Antimalarial medication-Quinine Derivitaves: Quinine ingestion cause a syndrome including tinnitus, sensorineural hearing loss and vertigo. Recent studies suggest that quinine impairs outer hair cell mobility. Ototoxic effects are similar to asprin- reversible once medication is discontinued).

Causes of Hearing Loss Cont. Antimalarial medication-Quinine Derivitaves (cont. ): • • • Quinidex (causes tinnitus) Atrabrine Plaquenil Quinine Sulfate Mefloquine Chloroquine
Causes of Hearing Loss Cont. 6. Loop diuretics: These medications are usually ototoxic when given intravenously for acute kidney failure or acute hypertension. Rare cases have been reported when these medications are taken orally in high doses in people with chronic kidney disease. • Edecrin (Ethacrynic acid) • Lasix (Furosemide) • Bumex (Bumetanide)

Causes of Hearing Loss Cont. 7. Chemotherapeutic Agents: • • • Ciaplatin Nitrogen Mustard Vincristine These medications are ototoxic when given for treatment of cancer. The ototoxic effects of these medications are enhanced in patients who are already taking other ototoxic medications.

Causes of Hearing Loss Cont. 8. Nonsteroidal Anti-Inflammatory Drugs Toxic effects usually appear after consuming an average of 6 -8 pills per day. Toxic effects are usually reversible once medications are discontinued. • • • Advil Aleve Anaprox Clinoril Feldene Lodine Motrin Nalfon Naprosyn Nuprin Poradol Voltarin

Causes of Hearing Loss Cont. Ø Acoustic trauma – temporary or permanent Ø Ménière’s disease – causes vertigo, hearing loss, tinnitus, pressure in ear; can be unilateral, fluctuating or progressive Ø Presbyacusis – age related sensorineural hearing loss Ø Noise exposure- most common cause of HL.

Causes of Hearing Loss Cont. Ø Noise Exposure. Damage risk criteria expressed as the maximum permissible noise exposure for a given duration during a work day. Duration per day (in hours) Sound level (in d. B) 8. 0 6. 0 4. 0 3. 0 2. 0 1. 5 1. 0 0. 5 0. 25 90 92 95 97 100 102 105 110 115 (club)

Causes of Hearing Loss Cont. Syndromes associated with Auditory Dysfunction See handout

4. Prevalence of hearing loss 3/1000 infants are born with congenital severe bilateral hearing loss Ø Additional 3 children acquire hearing loss early in childhood Ø Hearing loss occurs twice as frequently as other congenital abnormalities screened for in newborns combined: congenital hypothyroidism; sickle cell anemia; phenylketonuria; galactosemia Ø Prevalence = 10 -20 times higher in NICU Ø
Prevalence of hearing loss cont. Ø Prevalence in general population: l l 2/1000 = severe-profound HL 5/1000 = moderate-severe HL 8/1000 = mild HL 150/1000 = middle ear infections Ø Prevalence expected to be even higher with increase in HIV/AIDS infection

5. Tinnitus 1. Definition of tinnitus: l l l “…hearing a sound that is not related to any external sound in the environment” Ringing sound in patient’s ears is generated by patient’s own body, and is not present in external environment Most common types of sounds reported by patients: ringing, hissing, buzzing, cricket sounds

Tinnitus cont. 2. Neurophysiological model of Tinnitus Ø Ø Stages of tinnitus emergence: Generation- typically in the periphery Detection – subcortical centers Perception and evaluation – cotical areas Sustained activation of emotional (Limbic) and autonomic nervous systems

Tinnitus cont. 3. Prevalence of tinnitus • 17% of general population (44 million) • Clinically significant problems for approximately 4 -5% of the population 4. Impact on patients’ lives • Ranges from mild irritation to total disability, and in some cases suicide

Tinnitus cont. 5. Causes • May be associated with sensorineural hearing loss (damage to OHC and IHC) • Ionic imbalance in the cochlea • Dysfunction of cochlear neurotransmitter systems • Central • Certain medication may cause tinnitus: eg. antidepressants, benzodiazeptines • Unknown causes in a lot of cases

Tinnitus cont. 6. Treatment l l l Unable to suppress tinnitus source – therefore do not currently have a cure Tinnitus Retraining Therapy – helps patients to adapt to noise, and to change their brain’s perception of the tinnitus; makes use of noise generators to mask tinnitus Success rate of 80%

6. Hearing Tests Ø 1. Audiometry l l Puretone Speech Ø 2. Immittance Testing l l Tympanometry Acoustic Reflexes Ø 3. Electrophysiological Testing l l Otoacoustic Emissions (OAE) Auditory Brainstem Response (ABR)

Hearing Tests cont. Ø 1. Audiometry Ø 1. 1 What is audiometry & how does it work? l l 2 measures: intensity & frequency Intensity: • Loudness, measured in d. B • Human ear: 0 -120 d. B l Frequency: • Pitch/ tone of sound, measured in Hz • Human ear: 20 -20 000 Hz; 125 -8000 Hz

Hearing Tests cont. Ø Air conduction audiometry: l Earphones, outer ear, middle ear, inner ear, n. VIII Ø Bone conduction audiometry: l Bone conductor on mastoid

Hearing Tests cont. Ø 1. 2 Aims of Audiometry: l l Measure degree of HL: minimal, mild, moderate, severe, profound Measure site of lesion in hearing mechanism Determine cause of HL Determine degree of handicap (how HL affects patient’s activities of daily life)

Hearing Tests cont. Ø 1. 2 Aims of Audiometry cont: l Obtain indications for appropriate therapeutic and educational assistance – hearing aids; assistive listening devices; speech-language therapy; school placement
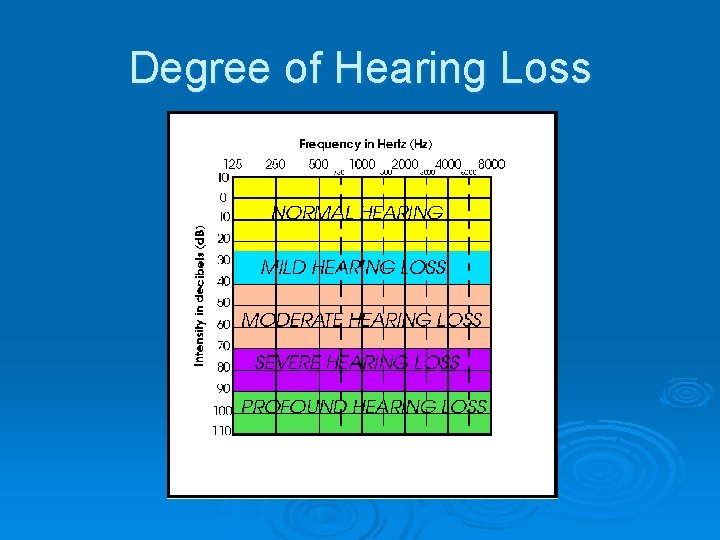
Degree of Hearing Loss
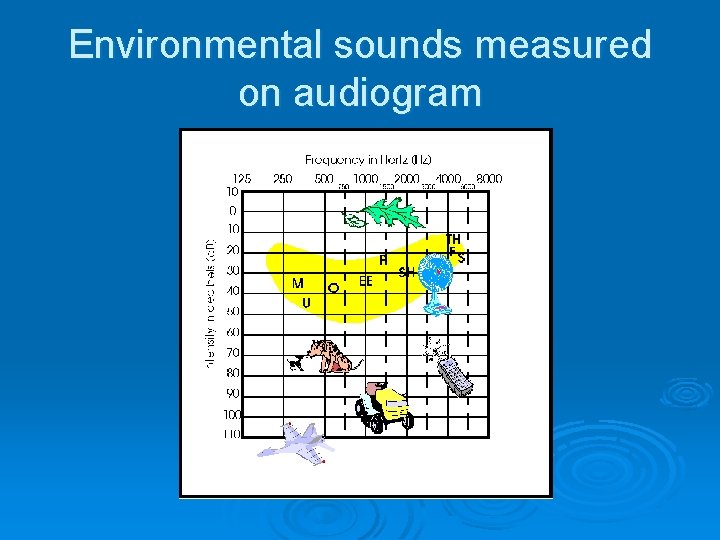
Environmental sounds measured on audiogram

What is an Audiogram? Ø An AUDIOGRAM is a graphic representation of a hearing test.
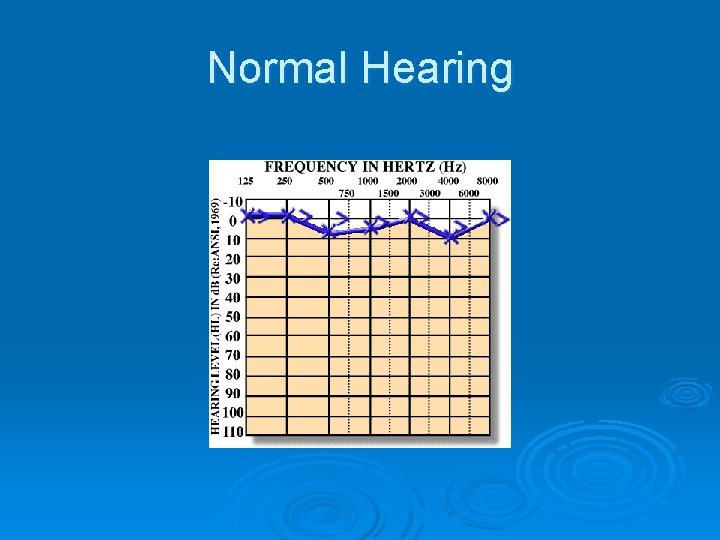
Normal Hearing
7. Types of Hearing Loss. Audiogram Ø 1. Conductive hearing loss l Resultant of external or middle ear pathology l Air conduction abnormal l Bone conduction normal
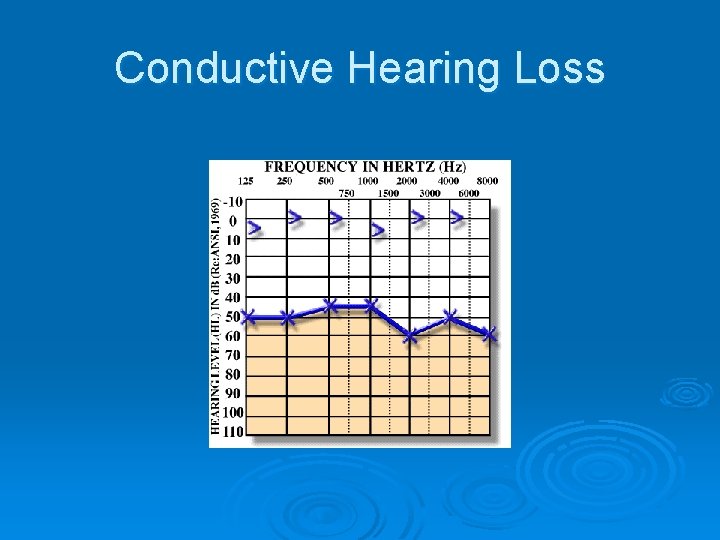
Conductive Hearing Loss
Types of Hearing Loss. Audiogram cont. Ø 2. Sensorineural hearing loss l Resultant of inner ear and/or auditory nerve damage l Air conduction and bone conduction equally abnormal
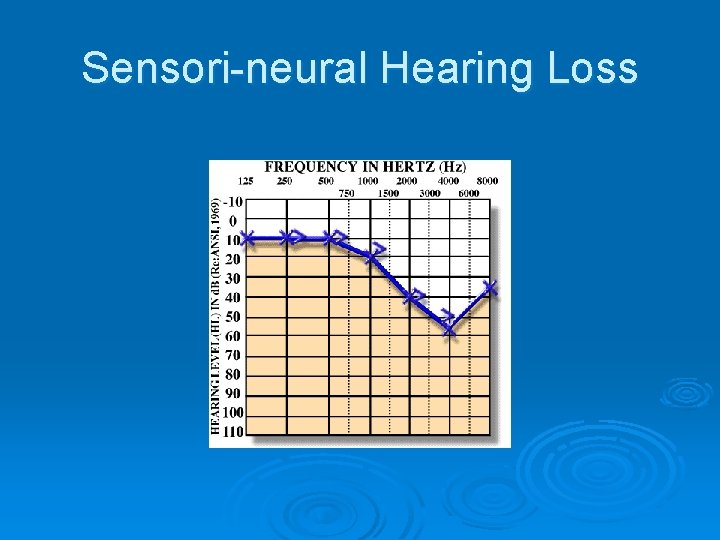
Sensori-neural Hearing Loss

Types of Hearing Loss. Audiogram cont. Ø 3. Mixed hearing loss l Combination of conductive and sensorineural hearing loss l Air conduction and bone conduction abnormal l Air conduction worse than bone conduction (air-bone gap)
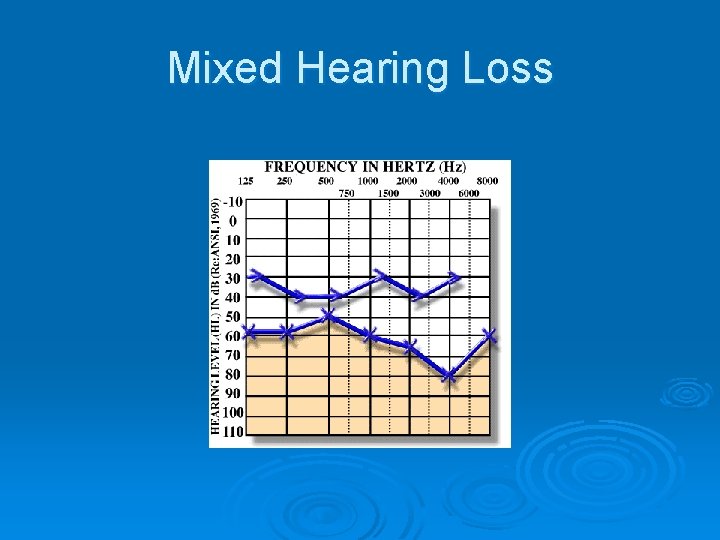
Mixed Hearing Loss

Hearing Tests cont. Ø 2. Immittance Testing Ø 2. 1 Tympanometry l l l Test of middle ear functioning Measures pressure, compliance and volume of middle ear Able to determine if middle ear pathology is present eg. Otitis Media

Hearing Tests cont. Ø 2. 2 Acoustic Reflex Testing l l Measures stapedial muscle reflex (middle ear) in response to loud stimulus Able to estimate hearing thresholds in difficult to test populations, although not always accurately

Hearing Tests cont. Ø 3. Electrophysiological Testing Ø 3. 1 Otoacoustic Emissions (OAE) l l l measure the integrity of the outer hair cells of the cochlea Auditory stimulus is presented to external ear via a probe Cochlea produces “echo” in response to stimulus – measured by probe

Hearing Tests cont. Ø Advantages of OAEs ü ü ü Non-invasive Simple - quick and easy to administer (also used in infant hearing screening) Frequency specific Objective Does not require behavioural cooperation Useful in infants, young children, neurologically compromised

Hearing Tests cont. Ø 3. 2 Auditory Brainstem Response (ABR) v v v Electrophysiological procedure Based on the brainstem’s response to sound Soft click stimuli are presented to the ear, whilst electrodes placed strategically on the head record the brain’s response to the stimuli

Hearing Tests cont. Ø Advantages of ABR: ü ü ü Frequency specific Predicts hearing thresholds No behavioural response required Objective Infants, young children

8. Intervention for Hearing Loss Ø Medical - surgical and/or medicinal treatment Ø Hearing aids (HA) Ø Implantable Devices - Cochlear Implant (CI) - BAHA (Bone anchored hearing aid) - Vibrant Sound Bridge Device

Ø Cochlear Implant - Electronic device for adults and children with a severe to profound hearing loss. - Unlike HA’s, which merely amplify sound, a CI bypasses the damaged hair cells and stimulates the hearing nerve directly. - Implanted directly in the inner ear or cochlea and electronically stimulates the nerves via electrodes.

Ø BAHA - Direct bone conduction - Bypasses conductive element - Creates direct cochlea stimulation - Conductive or mixed HL’s - To close the air-bone gap

Ø Vibrant Sound Bridge Device - Implanted in the middle ear - Device mechanically vibrates the bones in the middle ear. - Moderate to severe SNHL
- Slides: 62