PRESENTATIONS OF MIDDLE EAR DISEASE Elizabeth Rose Royal

PRESENTATIONS OF MIDDLE EAR DISEASE Elizabeth Rose Royal Victorian Eye and Ear Hospital Royal Children’s Hospital

• • Middle-ear conditions Management of otitis media Differential diagnosis of ear pain Clinical cases
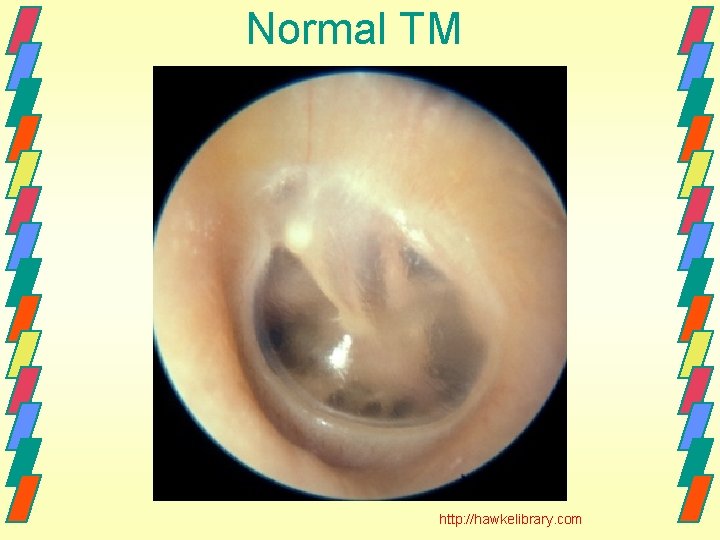
Normal TM http: //hawkelibrary. com
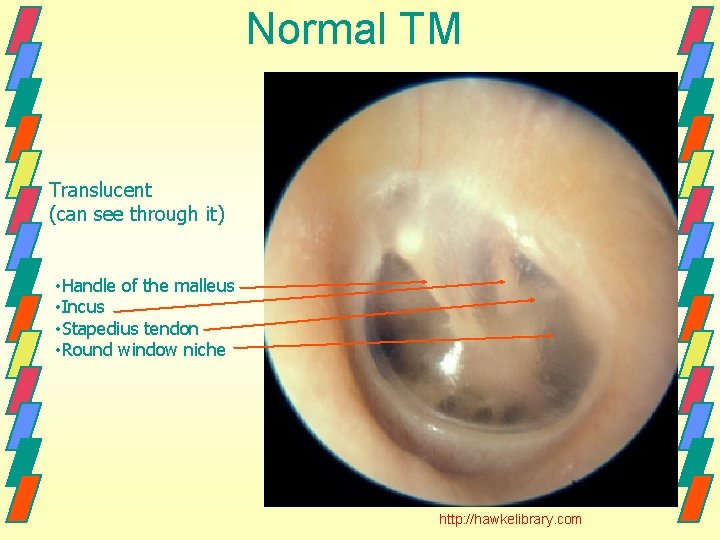
Normal TM Translucent (can see through it) • Handle of the malleus • Incus • Stapedius tendon • Round window niche http: //hawkelibrary. com

OTITIS MEDIA A SPECTRUM OF DISEASE • • • acute otitis media chronic otitis media with effusion atelectasis of the tympanic membrane chronic adhesive otitis media chronic suppurative otitis media – tubotympanic (“safe”) – atticoantral (“unsafe”) and may be a continuum of disease

Diagnosis of acute otitis media (Therapeutic Guidelines) 1. A history of acute onset of symptoms and signs – otalgia, ear pulling, otorrhoea, fever, anorexia, vomiting AND 2. Middle ear effusion (otorrhoea if a TP perforation) AND 3. signs and symptoms of middle ear inflammation, characterised by redness of the tympanic membrane.

Management of AOM • Pain relief Decongestants (oral/topical) and antihistamines – do not make the eustachian tube function better Not recommended

Management of AOM Who should be treated with antibiotics?

Antibiotic therapy • if severe symptoms • pain/fever • perforation • bilateral disease • possible suppurative complication • mastoiditis • Meningitis or other intracranial complication • • • ≤ 2 years old Indigenous (ATSI , Maori and Pacific Islanders) immune deficiency cochlear implant only hearing ear

Antibiotic therapy • Recommended treatment is: amoxicillin 45 mg/kg/day in 3 doses – Can give up to 100 mg/kg/day – Continue for 10 days • If no improvement in 2 days change to amoxicillin/clavulanate

If an allergy to penicillin cefuroxime child 3 months to 2 years: 10 mg/kg up to 125 mg; 2 years or more: 15 mg/kg up to 500 mg orally, 12 -hourly for 5 days

Antibiotic therapy • older children who can be accurate about their symptoms should be treated symptomatically • if no improvement after 2 days consider treatment with antibiotics

CHRONIC OTITIS MEDIA WITH EFFUSION (COME) • the presence of a middle ear effusion • asymptomatic apart from some hearing loss

CHRONIC OTITIS MEDIA WITH EFFUSION Normal OME

AOM COME • TM bulging • TM is retracted • Cannot see lateral process • Lateral process is more prominent of the malleus • Opaque • White from pus in ME • Yellow from effusion • Inflammation/prominent vessels

CHRONIC SUPPURATIVE OTITIS MEDIA (CSOM) “deafness and discharge” • • persistent disease insidious onset severe destruction irreversible sequelae

1. tubotympanic disease (“safe”) central perforation 2. atticoantral disease (“unsafe”) cholesteatoma the presence of keratinising squamous epithelium in the middle ear

Cholesteatoma • A non-neoplastic accumulation of keratinising stratified squamous epithelium in the tympanic cavity (middle ear) or mastoid air cells • Resorbs (damages) underlying bone • Potentially dangerous to the patient

MANAGEMENT OF CHRONIC OTITIS MEDIA WITH EFFUSION (and also retraction/atelectasis of the tympanic membrane)

What are grommets?

AKA • • grommets tubes pressure equalisation tubes middle ear ventilation tubes NOT • a drainage tube (it’s role in life is to ventilate!)

COME Who should have middle ear ventilation tubes? (for OME)

1. COME for 4 months at least, with hearing loss 2. COME in a child ‘at risk’ regardless of the hearing 3. COME and structural damage to the tympanic membrane

1. Hearing loss • median hearing loss is mild but there is a wide range • no data on the criteria for what is a significant hearing loss

2. An ‘at risk’ child has an increased risk of developmental difficulties due to factors not related to the OME: • • physical sensory, e. g. blindness cognitive, e. g. developmental delay behavioural

3. Structural damage to the tympanic membrane

Children with persistent OME who: • Do not have other risk factors • Do not have significant hearing loss • Do not have damage to the tympanic membrane or middle ear Can be evaluated every three months

PRESENTATIONS OF MIDDLE EAR DISEASE

DIFFERENTIAL DIAGNOSIS OF EAR PAIN A. • • • External auditory canal trauma ( e. g. from cotton bud abuse) auricular haematoma foreign body otitis external auditory canal tumour

DIFFERENTIAL DIAGNOSIS OF EAR PAIN B. Middle ear • • acute otitis media bullous myringitis chronic suppurative otitis media middle ear tumour

DIFFERENTIAL DIAGNOSIS OF EAR PAIN C. Referred pain – oropharynx (IXth nerve) • tonsillitis/post-tonsillectomy • carcinoma, including posterior tongue – laryngopharynx (Xth nerve) • pyriform fossa – upper molar teeth, TMJ, parotid gland (Vc) • impacted wisdom teeth • changes to bite from new dentures – cervical spine (C 2, C 3) • pain is often worse at night
- Slides: 31