Presentation of publication National and regional asthma programmes

Presentation of publication National and regional asthma programmes in Europe: a systematic review by Olof Selroos, MD, Ph. D, Emeritus Professor SEMECO AB, Selroos Medical Consulting AB Ängelholm, Sweden

Background • In Europe 10 million people <45 years of age have asthma • Prevalence within EU 8. 2% in adults 9. 4% in children The European Lung White Book, ERS 2013 • Direct costs € 11 billion, indirect costs € 14 billion Lung Health in Europe, Facts and figures, ERS 2013
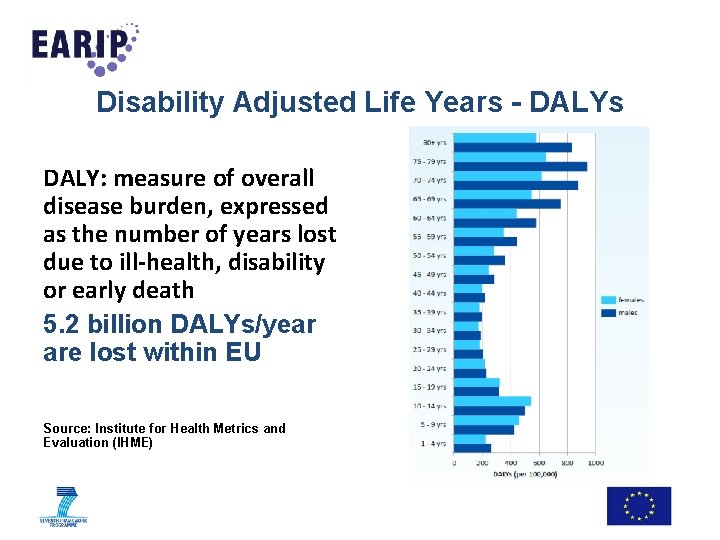
Disability Adjusted Life Years - DALYs DALY: measure of overall disease burden, expressed as the number of years lost due to ill-health, disability or early death 5. 2 billion DALYs/year are lost within EU Source: Institute for Health Metrics and Evaluation (IHME)

Aim of the project • The European Asthma Research and Innovation Partnership (EARIP) aims to build on and harmonise existing asthma activities in order to generate interconnectivities in asthma management, to develop an approach to reduce asthma-related mortality and morbidity across Europe • A systematic review of existing asthma programmes should form a part of the basis for future activities

National and regional asthma programmes in Europe Olof Selroos, Maciej Kupczyk, Piotr Kuna, Piotr Łacwik, Jean Bousquet, David Brennan, Susanna Palkonen, Javier Contreras, Mark Fitz. Gerald, Gunilla Hedlin, Sebastian L. Johnston, Renaud Louis, Leanne Metcalf, Samantha Walker, Antonio Moreno-Galdó, Nikos G. Papadapolous, José Rosado-Pinto, Pippa Powell and Tari Haahtela Eur Respir Rev 2015; 24: 474 -483

Methods • To identify publications on national and regional initiatives in Europe that aimed to improve quality of asthma care in large populations • Only papers published in English were considered

Systematic Search • • Pub. Med Cochrane Database of Systematic Reviews EMBASE Web of Science Citation Index GARD and GAN documents Asthma Health Outcome Project (AHOP) Reference lists of publications

Result of the search • 12 531 citations screened • 732 potentially relevant papers identified for further evaluation • 412 abstracts evaluated • 147 publications found relevant for inclusion • 53 publications (19 European – 10 from Finland) related to national asthma programmes

National and regional asthma programmes identified in Europe Country National Study period Initiator Executor Finland 1994– 2004 Finnish Ministry of Social Affairs and Health and Working group Finnish Lung Health organisation, a nongovernmental organisation France Eight medical specialist societies Ireland 2002– 2005 National Agency for Accreditation and Evaluation of Health on behalf of the French National Health Executive 2014– 2017 Health Service Executives Italy 2013 42 partners The Netherlands 2014– 2018 Lung Alliance Netherlands Poland 2009 –ongoing Portugal 2000– 2011; Directorate General of Health 2012– 2016 Portuguese Ministry of Health Directorate General of Health Turkey 2008 –ongoing Turkish Respiratory Society Regional Poland Global Alliance against Chronic Respiratory Diseases Asthma Society of Ireland Polish Society of Allergology Turkish Ministry of Health 2000– 2003 Dept of International Medicine Asthma and Allergy, Bazlicki University Hospital, Lodz Regional Health Insurance Fund (sponsor)

Based on the Finnish programme we know that: • The asthma burden can be reduced by relatively simple means via: early diagnosis, effective anti-inflammatory medication, guided self-management, and networking • Asthma deaths are avoidable • Hospitalizations can be reduced
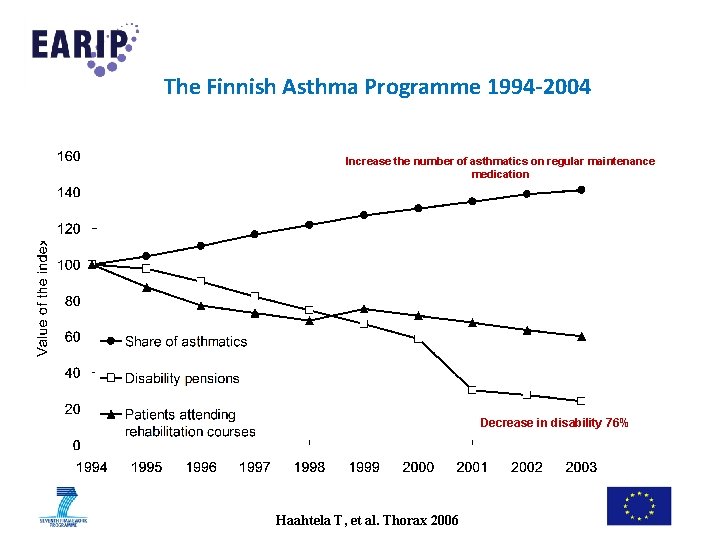
The Finnish Asthma Programme 1994 -2004 Increase the number of asthmatics on regular maintenance medication Decrease in disability 76% Haahtela T, et al. Thorax 2006
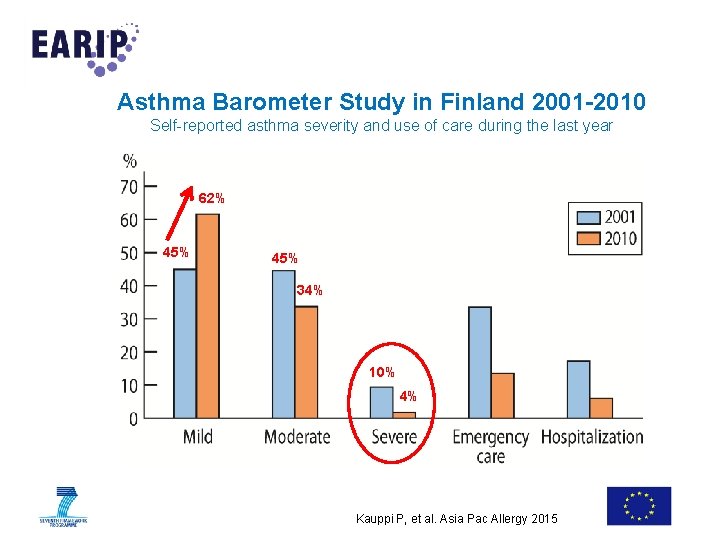
Asthma Barometer Study in Finland 2001 -2010 Self-reported asthma severity and use of care during the last year 62% 45% 34% 10% 4% Kauppi P, et al. Asia Pac Allergy 2015
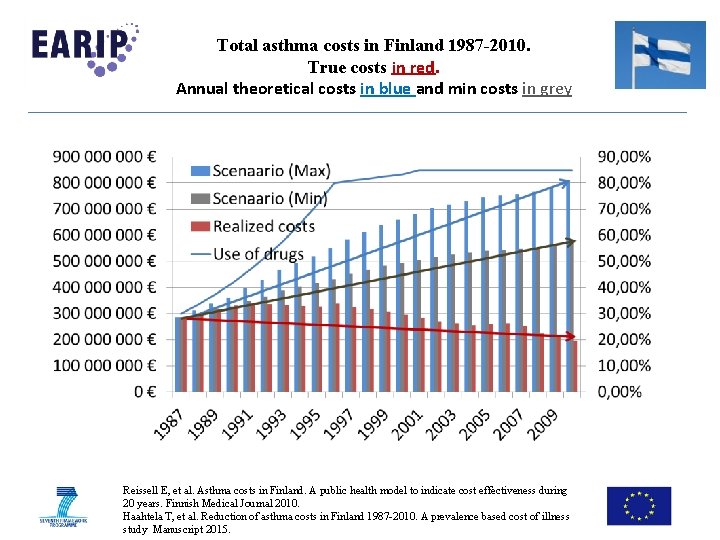
Total asthma costs in Finland 1987 -2010. True costs in red. Annual theoretical costs in blue and min costs in grey Reissell E, et al. Asthma costs in Finland. A public health model to indicate cost effectiveness during 20 years. Finnish Medical Journal 2010. Haahtela T, et al. Reduction of asthma costs in Finland 1987 -2010. A prevalence based cost of illness study Manuscript 2015.

Success factors in the Finnish programme ● Strong public health-care (also good registries) ● Historical reasons to regard asthma as an inflammatory airway disease. ● Generally recognized and accepted need for a change ● Large national consensus (health-care, medical scientific societies, non-governmental organisations and authorities) ● Support from Ministry of Health and Social Affairs and National Public Health Institute ● Simple organizational structure for leadership and implementation of the programme
Generic Action Plan – to be adjusted for local and national needs Example: The Finnish Asthma Programme 1994 -2004 Backgrou nd ► NEW BODY OF KNOWLEDGE • Disability caused by asthma can be prevented ► EPIDEMIOLOGY Morbidity Prevalence ► ECONOMY Costs ►EVIDENCE • Implementation of best practices is highly cost-effective both on the patient and societal level
Generic Action Plan Background ► NEW BODY OF KNOWLEDGE • Disability caused by asthma can be prevented ► EPIDEMIOLOGY Morbidity Prevalence ► ECONOMY Costs ►EVIDENCE • Implementation of best practices is highly cost-effective both on the patient and societal level 4 -Step Action Plan ► CONCLUSIONS • Public health problem • Need for broad consensus • Need for action • Identification of key stakeholders • Focus on patients • Focus on severe asthma to stop exacerbations/atta cks • Focus on effective use of available resources and registers
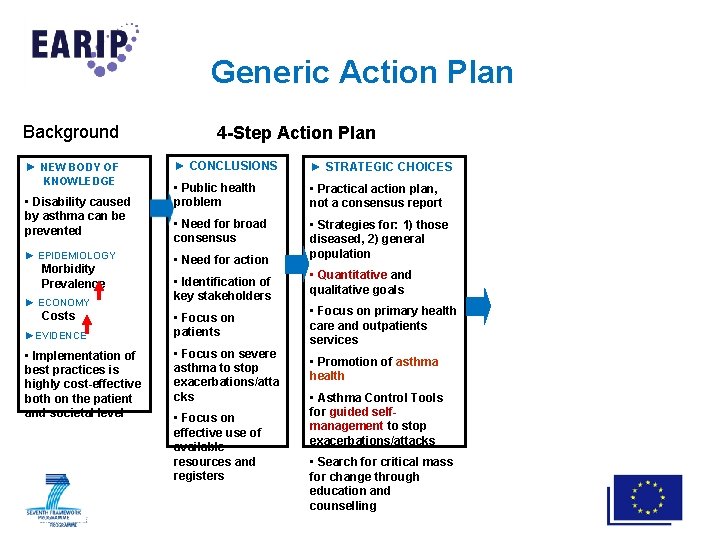
Generic Action Plan Background ► NEW BODY OF KNOWLEDGE • Disability caused by asthma can be prevented ► EPIDEMIOLOGY Morbidity Prevalence ► ECONOMY Costs ►EVIDENCE • Implementation of best practices is highly cost-effective both on the patient and societal level 4 -Step Action Plan ► CONCLUSIONS ► STRATEGIC CHOICES • Public health problem • Practical action plan, not a consensus report • Need for broad consensus • Strategies for: 1) those diseased, 2) general population • Need for action • Identification of key stakeholders • Focus on patients • Focus on severe asthma to stop exacerbations/atta cks • Focus on effective use of available resources and registers • Quantitative and qualitative goals • Focus on primary health care and outpatients services • Promotion of asthma health • Asthma Control Tools for guided selfmanagement to stop exacerbations/attacks • Search for critical mass for change through education and counselling
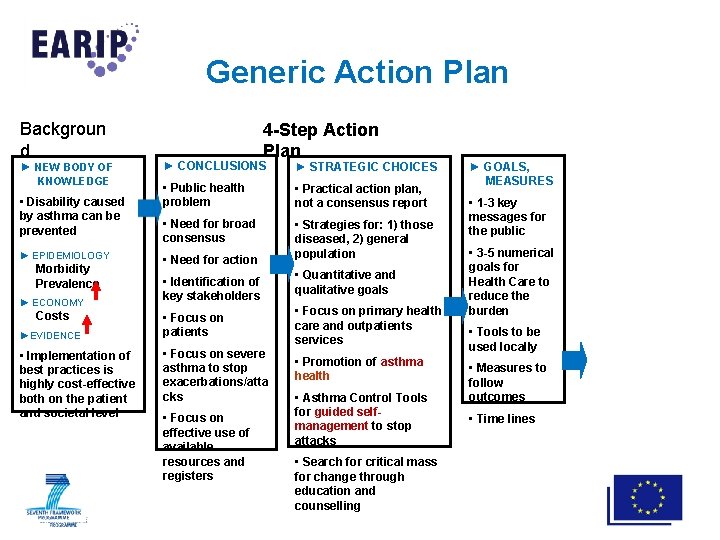
Generic Action Plan Backgroun d ► NEW BODY OF KNOWLEDGE • Disability caused by asthma can be prevented ► EPIDEMIOLOGY Morbidity Prevalence ► ECONOMY Costs ►EVIDENCE • Implementation of best practices is highly cost-effective both on the patient and societal level 4 -Step Action Plan ► CONCLUSIONS ► STRATEGIC CHOICES • Public health problem • Practical action plan, not a consensus report • Need for broad consensus • Strategies for: 1) those diseased, 2) general population • Need for action • Identification of key stakeholders • Focus on patients • Focus on severe asthma to stop exacerbations/atta cks • Focus on effective use of available resources and registers • Quantitative and qualitative goals • Focus on primary health care and outpatients services • Promotion of asthma health • Asthma Control Tools for guided selfmanagement to stop attacks • Search for critical mass for change through education and counselling ► GOALS, MEASURES • 1 -3 key messages for the public • 3 -5 numerical goals for Health Care to reduce the burden • Tools to be used locally • Measures to follow outcomes • Time lines
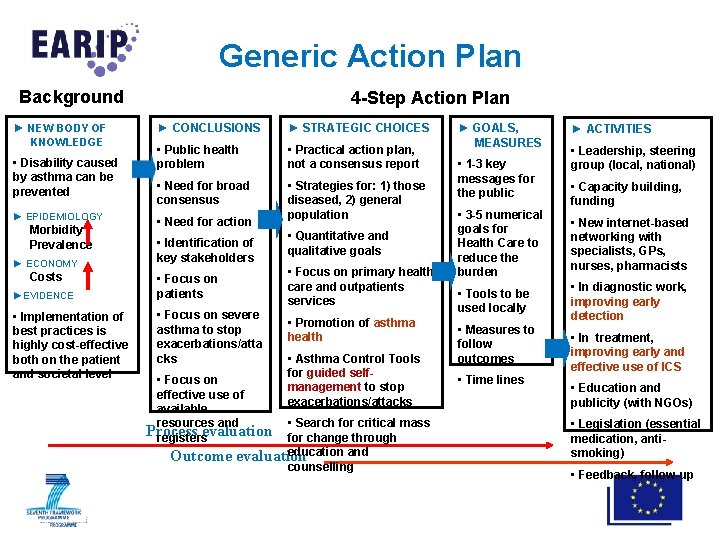
Generic Action Plan Background ► NEW BODY OF KNOWLEDGE • Disability caused by asthma can be prevented ► EPIDEMIOLOGY Morbidity Prevalence ► ECONOMY Costs ►EVIDENCE • Implementation of best practices is highly cost-effective both on the patient and societal level 4 -Step Action Plan ► CONCLUSIONS ► STRATEGIC CHOICES • Public health problem • Practical action plan, not a consensus report • Need for broad consensus • Strategies for: 1) those diseased, 2) general population • Need for action • Identification of key stakeholders • Focus on primary health care and outpatients services • Focus on patients • Focus on severe asthma to stop exacerbations/atta cks • Focus on effective use of available resources and Process evaluation registers Outcome • Quantitative and qualitative goals • Promotion of asthma health • Asthma Control Tools for guided selfmanagement to stop exacerbations/attacks • Search for critical mass for change through education and evaluation counselling ► GOALS, MEASURES • 1 -3 key messages for the public • 3 -5 numerical goals for Health Care to reduce the burden • Tools to be used locally • Measures to follow outcomes • Time lines ► ACTIVITIES • Leadership, steering group (local, national) • Capacity building, funding • New internet-based networking with specialists, GPs, nurses, pharmacists • In diagnostic work, improving early detection • In treatment, improving early and effective use of ICS • Education and publicity (with NGOs) • Legislation (essential medication, antismoking) • Feedback, follow-up
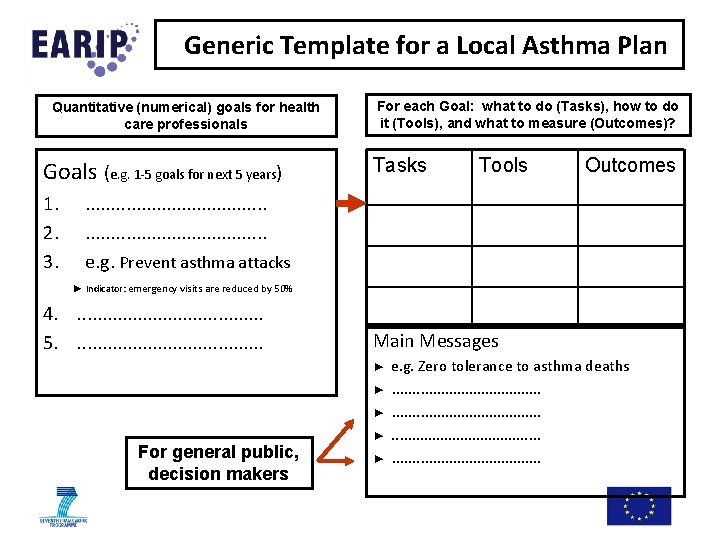
Generic Template for a Local Asthma Plan Quantitative (numerical) goals for health care professionals Goals (e. g. 1 -5 goals for next 5 years) 1. 2. 3. For each Goal: what to do (Tasks), how to do it (Tools), and what to measure (Outcomes)? Tasks Tools Outcomes . . . . e. g. Prevent asthma attacks ► Indicator: emergency visits are reduced by 50% 4. . . . . 5. . . . . Main Messages ► ► ► For general public, decision makers ► ► e. g. Zero tolerance to asthma deaths. . . . . . . . . .

Conclusions Asthma is still seriously neglected This can be changed by § higher awareness of asthma § higher on national priorities § advocacy for change § national asthma strategies § standard case management § more data and monitoring “A community problem needs community solutions” Haahtela et al Thorax 2001; 56: 806 -14
- Slides: 21