Presentation Objectives Optima Nutrition presentation of the tool


Presentation Objectives • Optima Nutrition – presentation of the tool • A preliminary application of Optima Nutrition in Tajikistan • Discussion and the next steps
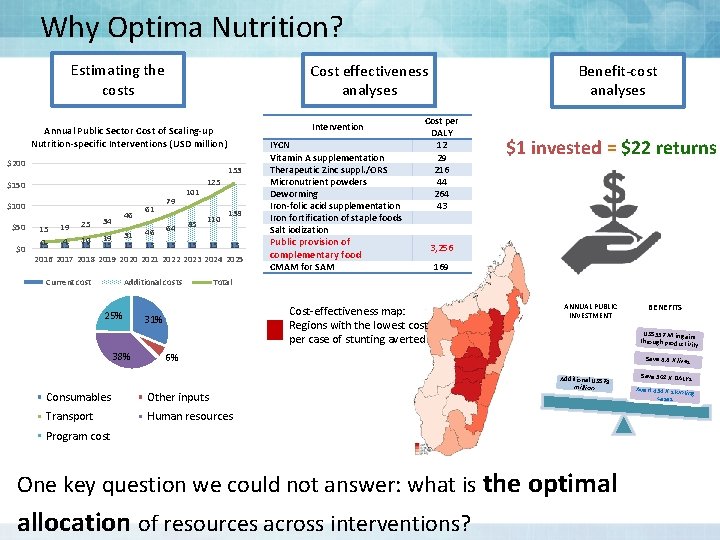
Why Optima Nutrition? Estimating the costs Cost effectiveness analyses Intervention Annual Public Sector Cost of Scaling-up Nutrition-specific Interventions (USD million) $200 153 $150 $100 $50 $0 15 19 25 34 4 15 10 15 19 15 46 31 15 61 46 15 79 64 15 101 85 125 110 15 15 138 15 2016 2017 2018 2019 2020 2021 2022 2023 2024 2025 Current cost Additional costs 25% 38% IYCN Vitamin A supplementation Therapeutic Zinc suppl. /ORS Micronutrient powders Deworming Iron-folic acid supplementation Iron fortification of staple foods Salt iodization Benefit-cost analyses Cost per DALY 12 29 216 44 264 43 Public provision of complementary food CMAM for SAM $1 invested = $22 returns 3, 256 169 Total Cost-effectiveness map: Regions with the lowest cost per case of stunting averted 31% ANNUAL PUBLIC INVESTMENT US$557 M in gains through productiv ity 6% Consumables Other inputs Transport Human resources Save 6. 6 K lives Additional US$79 million Program cost One key question we could not answer: what is the optimal allocation of resources across interventions? BENEFITS Save 302 K DALYs Avert 434 K stunti ng cases
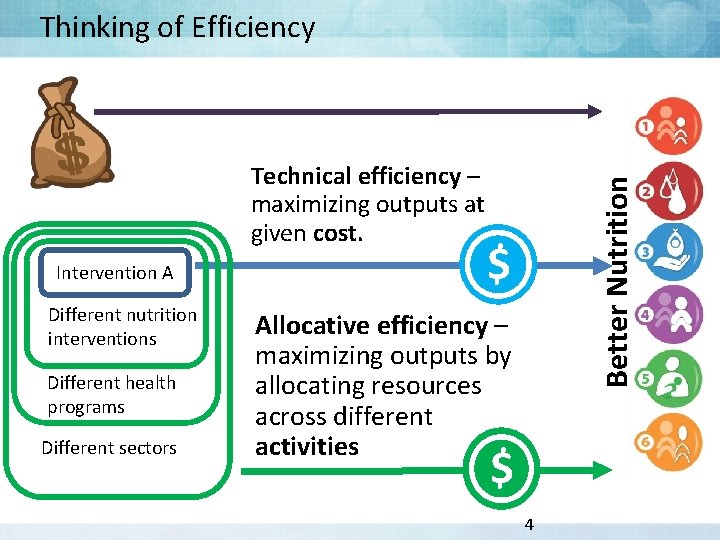
Technical efficiency – maximizing outputs at given cost. Intervention A Different nutrition interventions Different health programs Different sectors Better Nutrition Thinking of Efficiency $ Allocative efficiency – maximizing outputs by allocating resources across different activities $ 4
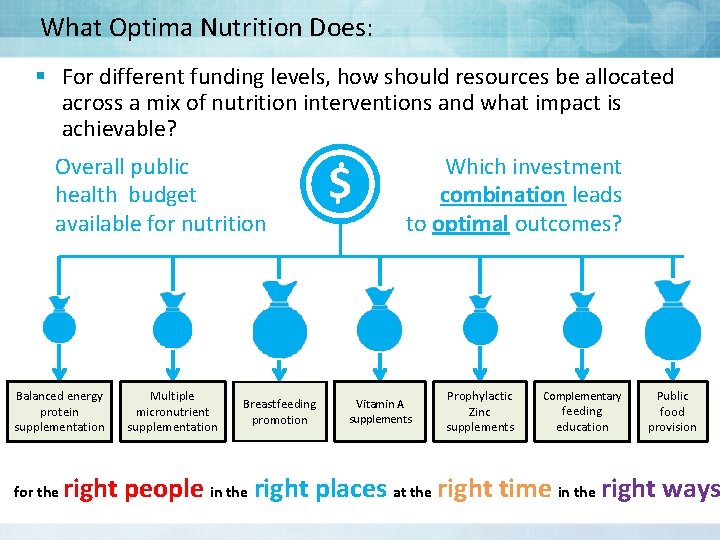
What Optima Nutrition Does: § For different funding levels, how should resources be allocated across a mix of nutrition interventions and what impact is achievable? Overall public health budget available for nutrition Balanced energy protein supplementation for the Multiple micronutrient supplementation Breastfeeding promotion $ Which investment combination leads to optimal outcomes? Vitamin A supplements Prophylactic Zinc supplements Complementary feeding education Public food provision right people in the right places at the right time in the right ways
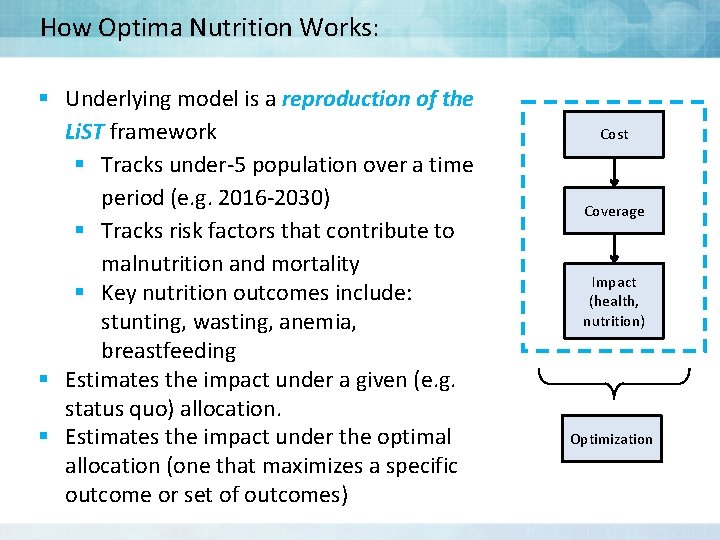
How Optima Nutrition Works: § Underlying model is a reproduction of the Li. ST framework § Tracks under-5 population over a time period (e. g. 2016 -2030) § Tracks risk factors that contribute to malnutrition and mortality § Key nutrition outcomes include: stunting, wasting, anemia, breastfeeding § Estimates the impact under a given (e. g. status quo) allocation. § Estimates the impact under the optimal allocation (one that maximizes a specific outcome or set of outcomes) Cost Coverage Impact (health, nutrition) Optimization

Optimization: consider just two dimensions Objective function: e. g. number of stunted children Funding to Program B Funding to Program A Apply an optimization algorithm to calculate best resource allocation

Optima Nutrition: Application in Tajikistan • One of the first ever applications of the took • Initial presentation of the tool to the national nutrition stakeholders in early 2019 • Data collection: • • Basic demographic and socio-economic data Health and nutrition status data Coverage of the interventions included in the analyses Unit cost data • Data sources: • Government sources (official surveys, data from Mo. HSP) • Supplemental data from partners
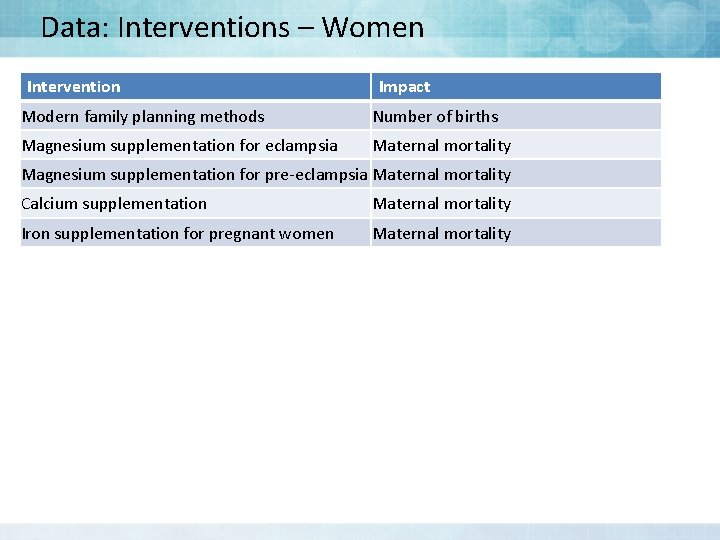

Data: Interventions – Women Intervention Impact Modern family planning methods Number of births Magnesium supplementation for eclampsia Maternal mortality Magnesium supplementation for pre-eclampsia Maternal mortality Calcium supplementation Maternal mortality Iron supplementation for pregnant women Maternal mortality

Data: Interventions – Children Intervention Infant and young child feeding counseling (in health facilities) Micronutrient powder supplementation for children Oral rehydration solution for treatment or diarrhea Oral rehydration solution and zinc for treatment of diarrhea Treatment of severe acute malnutrition (SAM) Vitamin A supplementation Impact Child mortality, linear growth (HAZ) Child mortality, anemia Child mortality, diarrhea incidence

Data: Interventions – General Population Intervention Iron and folic acid (IFA) fortification of maize flour Iron and folic acid (IFA) fortification of wheat flour Impact Child anemia, WRA anemia, child morality (FA’s impact on neural tube defects)
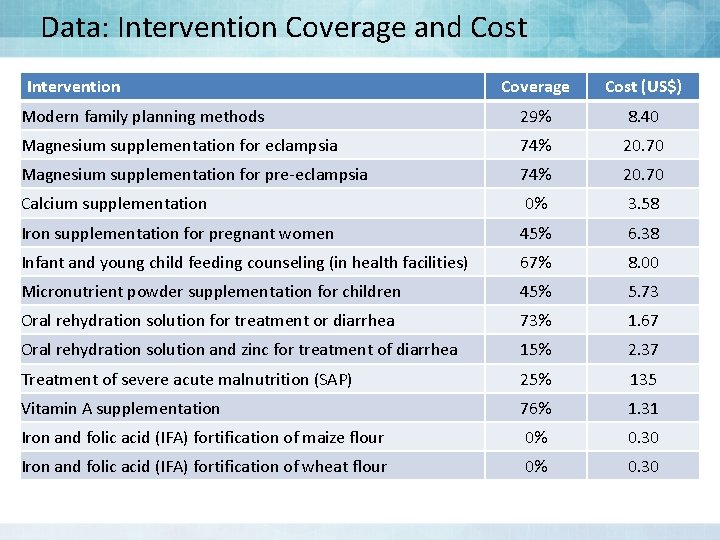
Data: Intervention Coverage and Cost Intervention Coverage Cost (US$) Modern family planning methods 29% 8. 40 Magnesium supplementation for eclampsia 74% 20. 70 Magnesium supplementation for pre-eclampsia 74% 20. 70 Calcium supplementation 0% 3. 58 Iron supplementation for pregnant women 45% 6. 38 Infant and young child feeding counseling (in health facilities) 67% 8. 00 Micronutrient powder supplementation for children 45% 5. 73 Oral rehydration solution for treatment or diarrhea 73% 1. 67 Oral rehydration solution and zinc for treatment of diarrhea 15% 2. 37 Treatment of severe acute malnutrition (SAP) 25% 135 Vitamin A supplementation 76% 1. 31 Iron and folic acid (IFA) fortification of maize flour 0% 0. 30 Iron and folic acid (IFA) fortification of wheat flour 0% 0. 30
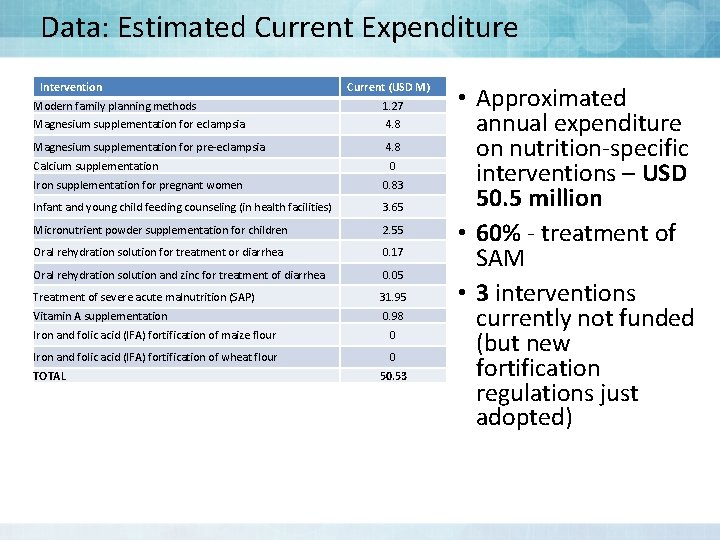
Data: Estimated Current Expenditure Intervention Current (USD M) Modern family planning methods 1. 27 Magnesium supplementation for eclampsia 4. 8 Magnesium supplementation for pre-eclampsia 4. 8 Calcium supplementation 0 Iron supplementation for pregnant women 0. 83 Infant and young child feeding counseling (in health facilities) 3. 65 Micronutrient powder supplementation for children 2. 55 Oral rehydration solution for treatment or diarrhea 0. 17 Oral rehydration solution and zinc for treatment of diarrhea 0. 05 Treatment of severe acute malnutrition (SAP) 31. 95 Vitamin A supplementation 0. 98 Iron and folic acid (IFA) fortification of maize flour 0 Iron and folic acid (IFA) fortification of wheat flour 0 TOTAL 50. 53 • Approximated annual expenditure on nutrition-specific interventions – USD 50. 5 million • 60% - treatment of SAM • 3 interventions currently not funded (but new fortification regulations just adopted)

Preliminary analyses • Analysis question: How to allocate a budget of additional resources, with a possibility of re-allocating current budget, to maximize impact? • Additional resources: • Additional U$ 10 M per year • Can reallocate the exiting budget • Impact: • A combination of reduced: number of stunted children, number of children suffering from anemia, number of child deaths, number of maternal deaths, number of pregnant women suffering form anemia.

Scenarios • Three scenarios are analyzed: • Baseline – no additional funding • Business as usual – additional funding (USD 10 M) allocated proportionally to the currently funded interventions: • USD 10 m (additional funding) = 19. 6% of the current estimated expenditure (USD 50. 5 M); therefore, the coverage of each intervention is expanded by 19. 6% (not percentage points) • Optima allocation • Optima Nutrition software can allocate all funding (the currently spent USD 50. 5 M and the additional USD 10 M) in such a way to achieve the best impact for the complex objective (minimize the number of stunted anemic children, minimize the number of child deaths, minimize the number of anemic pregnant women, minimize the number of maternal deaths).
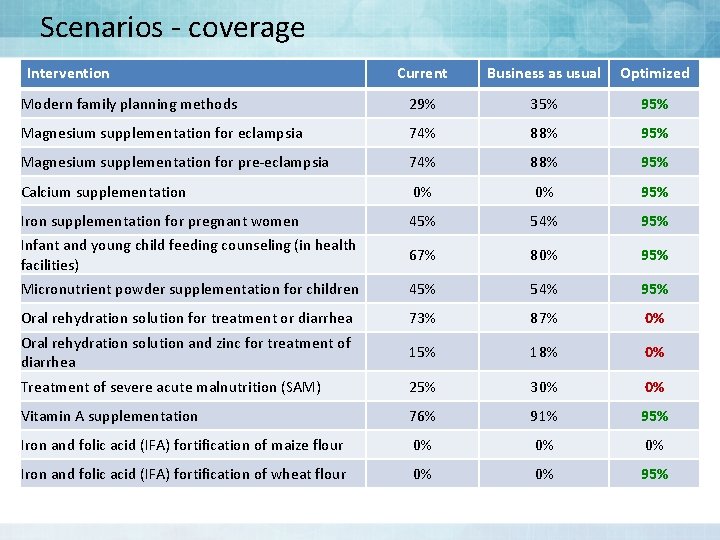
Scenarios - coverage Intervention Current Business as usual Optimized Modern family planning methods 29% 35% 95% Magnesium supplementation for eclampsia 74% 88% 95% Magnesium supplementation for pre-eclampsia 74% 88% 95% Calcium supplementation 0% 0% 95% Iron supplementation for pregnant women 45% 54% 95% Infant and young child feeding counseling (in health facilities) 67% 80% 95% Micronutrient powder supplementation for children 45% 54% 95% Oral rehydration solution for treatment or diarrhea 73% 87% 0% Oral rehydration solution and zinc for treatment of diarrhea 15% 18% 0% Treatment of severe acute malnutrition (SAM) 25% 30% 0% Vitamin A supplementation 76% 91% 95% Iron and folic acid (IFA) fortification of maize flour 0% 0% 0% Iron and folic acid (IFA) fortification of wheat flour 0% 0% 95%
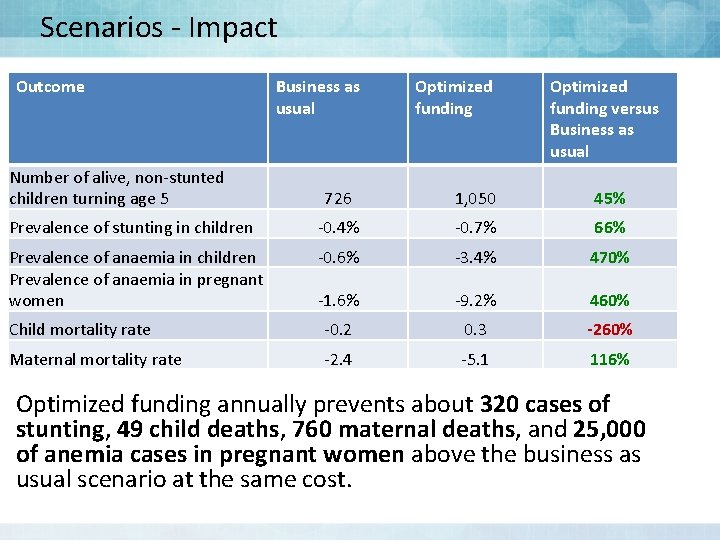

Scenarios - Impact Outcome Number of alive, non-stunted children turning age 5 Business as usual Optimized funding versus Business as usual 726 1, 050 45% Prevalence of stunting in children -0. 4% -0. 7% 66% Prevalence of anaemia in children Prevalence of anaemia in pregnant women -0. 6% -3. 4% 470% -1. 6% -9. 2% 460% Child mortality rate -0. 2 0. 3 -260% Maternal mortality rate -2. 4 -5. 1 116% Optimized funding annually prevents about 320 cases of stunting, 49 child deaths, 760 maternal deaths, and 25, 000 of anemia cases in pregnant women above the business as usual scenario at the same cost.

Conclusions and caveats (so far): • Improving allocative efficiency of nutrition investments can lead to a greater impact. • Shifting funding to more cost-effective interventions can improve key outcomes including stunting prevalence, anemia prevalence, maternal and child mortality, without incurring additional costs. • For the joint objective presented above, the priorities for financing include: • Nutrition interventions preventing maternal mortality • IFA food fortification • Preventing interventions for children under the age of 5 • Caveats: • More accurate data on the actual expenditure on nutrition interventions is needed • Validation of the coverage data (e. g. is 65% really covered by quality IYCF)? • Additional analyses needed at the sub-national level

Next Steps: • EWG validates input data at the national level; • Discussions with the EWG to refine and validate the outcomes and the results at the national level; • Geospatial analyses – optimized allocations across different intervention AND across different oblast’ • Presentation of results and training on the Optima Nutrition tool

Acknowledgements: • The team would like to thank the Optima Working Group chaired Dr. Saida Umarzadova for their support and guidance during the analysis project • The team would also like to thank the all the agencies and technical partners who have shared the data used in the analysis. • Thank you for your continuous collaboration.

THANK YOU FOR YOUR ATTENTION QUESTIONS?
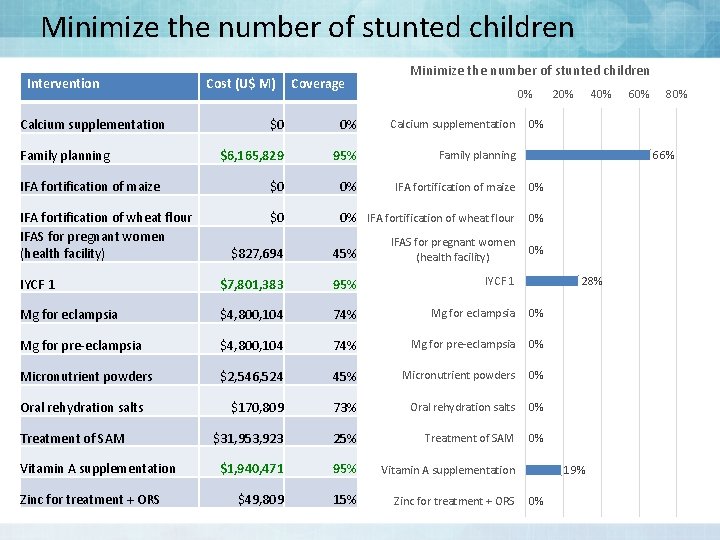
Minimize the number of stunted children Intervention Calcium supplementation Cost (U$ M) Coverage Minimize the number of stunted children 0% $0 0% Calcium supplementation $6, 165, 829 95% Family planning IFA fortification of maize $0 0% IFA fortification of maize IFA fortification of wheat flour IFAS for pregnant women (health facility) $0 0% IFA fortification of wheat flour 0% Family planning 0% IFAS for pregnant women (health facility) IYCF 1 $7, 801, 383 95% IYCF 1 Mg for eclampsia $4, 800, 104 74% Mg for eclampsia 0% Mg for pre-eclampsia $4, 800, 104 74% Mg for pre-eclampsia 0% Micronutrient powders $2, 546, 524 45% Micronutrient powders 0% $170, 809 73% Oral rehydration salts 0% $31, 953, 923 25% Treatment of SAM 0% $1, 940, 471 95% Vitamin A supplementation $49, 809 15% Zinc for treatment + ORS Vitamin A supplementation Zinc for treatment + ORS 60% 80% 66% 45% Treatment of SAM 40% 0% $827, 694 Oral rehydration salts 20% 0% 28% 19% 0%
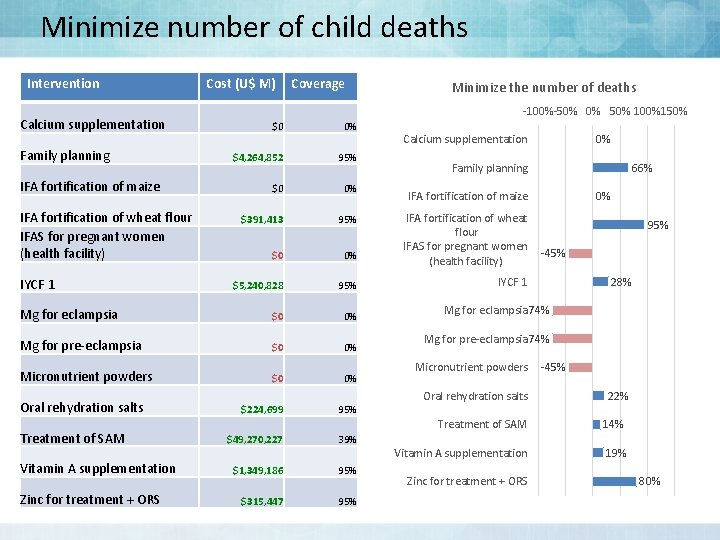
Minimize number of child deaths Intervention Calcium supplementation Cost (U$ M) Coverage -100%-50% 0% 50% 100%150% $0 0% $4, 264, 852 95% $0 0% $391, 413 95% $0 0% $5, 240, 828 95% Mg for eclampsia $0 0% Mg for pre-eclampsia $0 0% Micronutrient powders $0 0% Family planning IFA fortification of maize IFA fortification of wheat flour IFAS for pregnant women (health facility) IYCF 1 Oral rehydration salts Treatment of SAM Vitamin A supplementation Zinc for treatment + ORS Minimize the number of deaths $224, 699 95% $49, 270, 227 39% $1, 349, 186 95% $315, 447 95% Calcium supplementation 0% Family planning 66% IFA fortification of maize IFA fortification of wheat flour IFAS for pregnant women (health facility) 0% 95% -45% 28% IYCF 1 Mg for eclampsia-74% Mg for pre-eclampsia-74% Micronutrient powders Oral rehydration salts -45% 22% Treatment of SAM 14% Vitamin A supplementation 19% Zinc for treatment + ORS 80%
- Slides: 23