Prescribing Teaching 3 Max Roberts max robertsnhs net

Prescribing Teaching 3 Max Roberts max. roberts@nhs. net

Aims & Objectives The basics • Practice prescribing common medications • PSA overview • Controlled Drugs • Anticoagulation
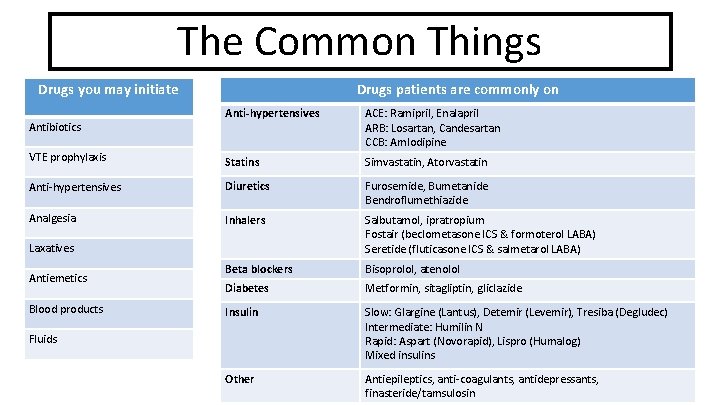
Common things The Common Things Drugs patients are commonly on Drugs you may initiate Anti-hypertensives ACE: Ramipril, Enalapril ARB: Losartan, Candesartan CCB: Amlodipine VTE prophylaxis Statins Simvastatin, Atorvastatin Anti-hypertensives Diuretics Furosemide, Bumetanide Bendroflumethiazide Analgesia Inhalers Salbutamol, ipratropium Fostair (beclometasone ICS & formoterol LABA) Seretide (fluticasone ICS & salmetarol LABA) Beta blockers Bisoprolol, atenolol Diabetes Metformin, sitagliptin, gliclazide Insulin Slow: Glargine (Lantus), Detemir (Levemir), Tresiba (Degludec) Intermediate: Humilin N Rapid: Aspart (Novorapid), Lispro (Humalog) Mixed insulins Other Antiepileptics, anti-coagulants, antidepressants, finasteride/tamsulosin Antibiotics Laxatives Antiemetics Blood products Fluids
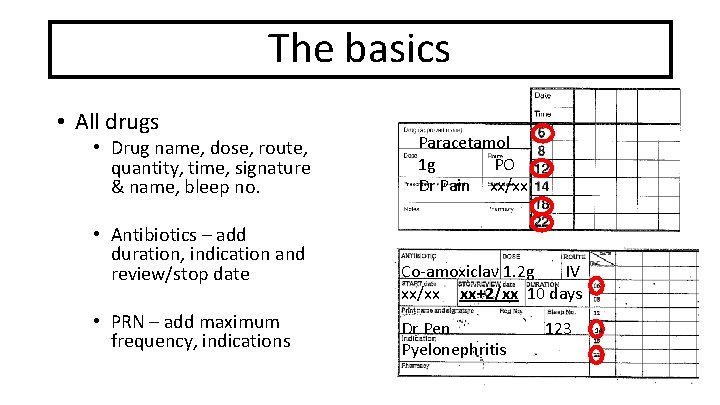

The basics • All drugs • Drug name, dose, route, quantity, time, signature & name, bleep no. • Antibiotics – add duration, indication and review/stop date • PRN – add maximum frequency, indications Paracetamol 1 g PO Dr Pain xx/xx Co-amoxiclav 1. 2 g IV xx/xx xx+2/xx 10 days Dr Pen Pyelonephritis 123 14
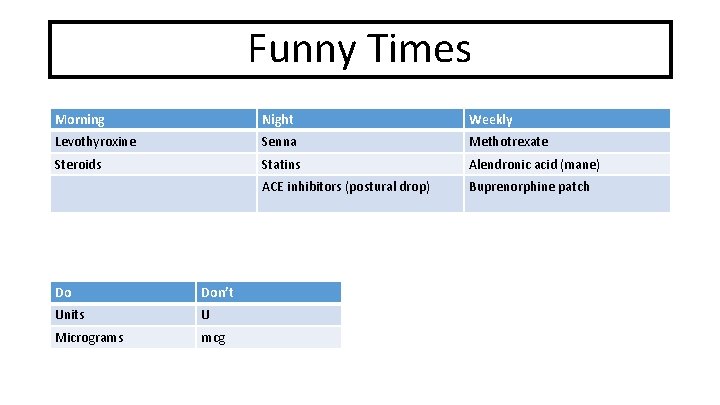
Funny Times Morning Night Weekly Levothyroxine Senna Methotrexate Steroids Statins Alendronic acid (mane) ACE inhibitors (postural drop) Buprenorphine patch Funny times… Do Don’t Units U Micrograms mcg
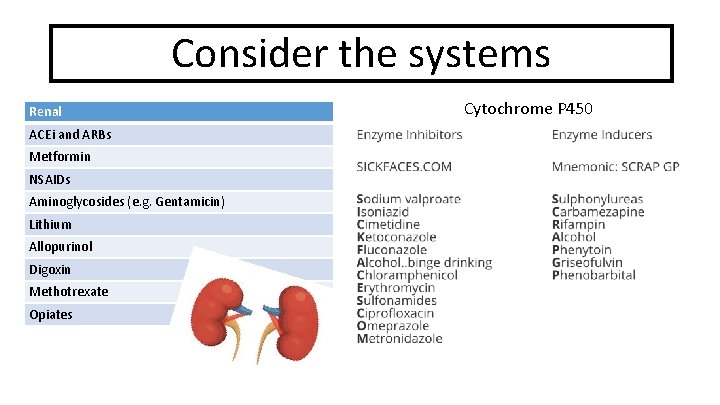
Consider the systems Renal ACEi and ARBs Metformin NSAIDs Aminoglycosides (e. g. Gentamicin) Lithium Allopurinol Digoxin Methotrexate Opiates Cytochrome P 450
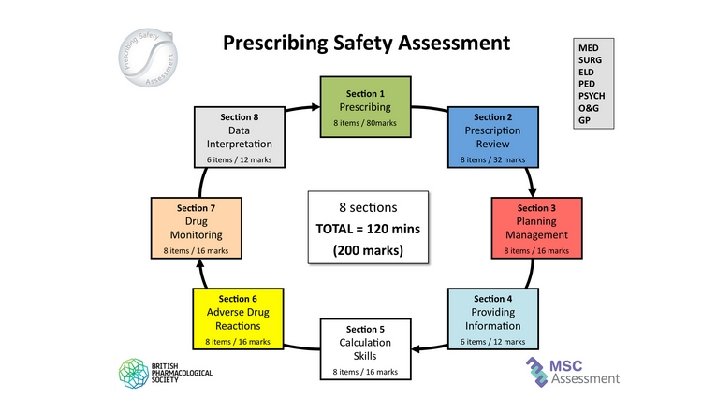
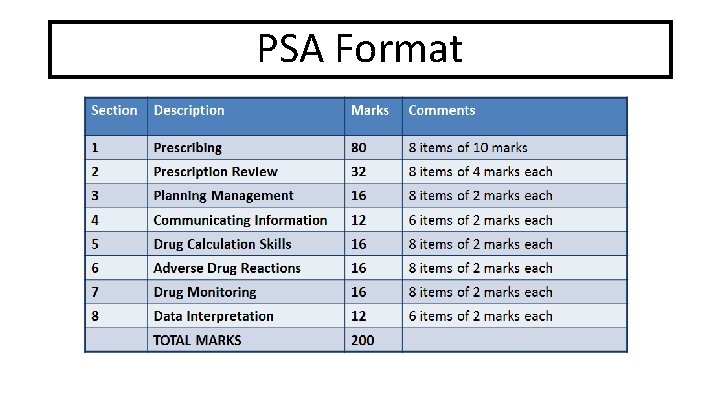
PSA Format

https: //www. amazon. co. uk/Pass-Will-Brown-MBBS-MRCP/dp/0702055182
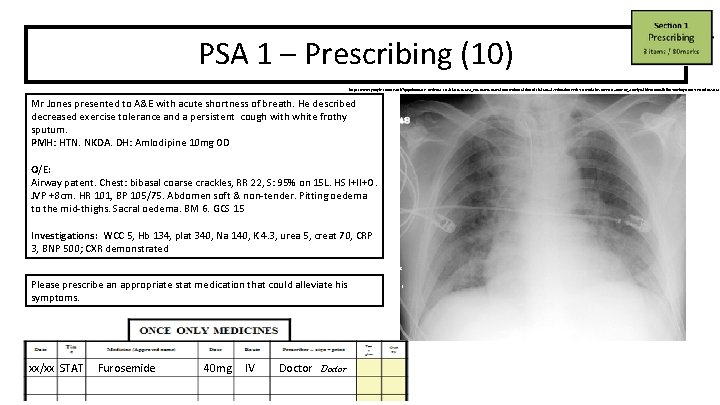
PSA 1 – Prescribing (10) https: //www. google. com/search? q=pulmonary+oedema+cxr&rlz=1 C 1 GCEA_en. GB 869&source=lnms&tbm=isch&sa=X&ved=0 ah. UKEwi. J 7 t. Lso. YDl. Ah. WTo. Fw. KHXJ 6 DRIQ_AUIEig. B&biw=1600&bih=740#imgrc=m 7 x. JYJ-od. U 85 OM: Mr Jones presented to A&E with acute shortness of breath. He described decreased exercise tolerance and a persistent cough with white frothy sputum. PMH: HTN. NKDA. DH: Amlodipine 10 mg OD O/E: Airway patent. Chest: bibasal coarse crackles, RR 22, S: 95% on 15 L. HS I+II+O. JVP +8 cm. HR 101, BP 105/75. Abdomen soft & non-tender. Pitting oedema to the mid-thighs. Sacral oedema. BM 6. GCS 15 Investigations: WCC 5, Hb 134, plat 340, Na 140, K 4. 3, urea 5, creat 70, CRP 3, BNP 500; CXR demonstrated Please prescribe an appropriate stat medication that could alleviate his symptoms. xx/xx STAT Furosemide 40 mg IV Doctor

Controlled drugs What are controlled drugs? • Medicines which are ‘controlled’ under the Misuse of Drugs Act • These include opioids, benzodiazepines, ketamine, THC, Z-drugs, barbiturates, etc • They need to be locked up on the wards • Patients may need proof of identity for their prescriptions • Doctors need to specify exact quantities
Controlled drugs • Drug name and formulation • Words and figures • Strength • Dose • Quantity Please supply 2 (two) patches of buprenorphine 5 (five) microgram/hour, 1 (one) patch once weekly on Fridays, • Frequency, route weekly • Sign, date, bleep
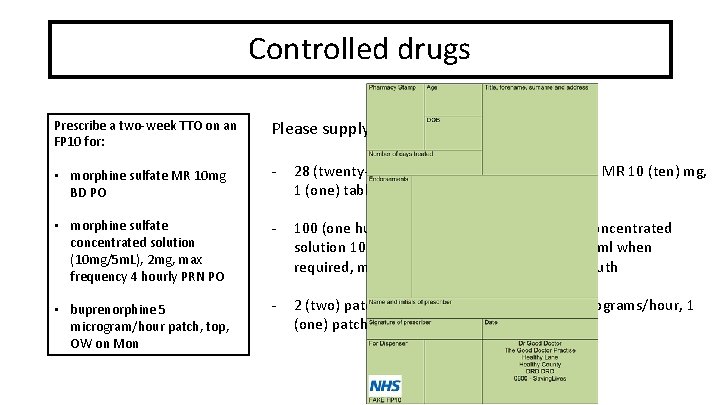
Controlled drugs Prescribe a two-week TTO on an FP 10 for: Please supply: • morphine sulfate MR 10 mg BD PO - 28 (twenty-eight) tablets of morphine sulphate MR 10 (ten) mg, 1 (one) tablet twice a day, by mouth • morphine sulfate concentrated solution (10 mg/5 m. L), 2 mg, max frequency 4 hourly PRN PO - 100 (one hundred) m. L of morphine sulphate concentrated solution 10 mg/5 m. L (ten mg / five m. L), 1 (one) ml when required, maximum frequency 4 hourly, by mouth • buprenorphine 5 microgram/hour patch, top, OW on Mon - 2 (two) patches of buprenorphine 5 (five) micrograms/hour, 1 (one) patch once weekly on Mondays, topical
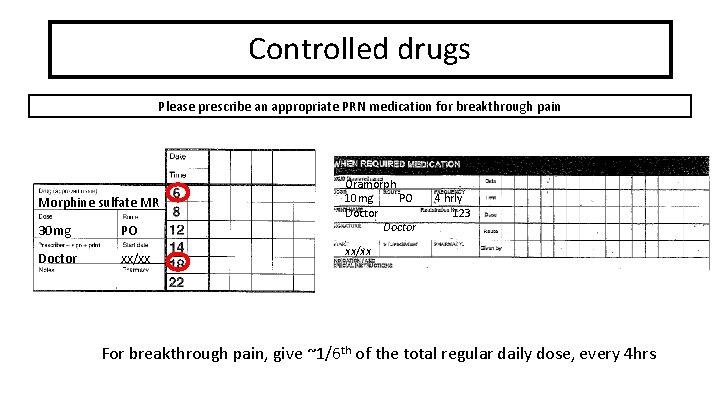

Controlled drugs Please prescribe an appropriate PRN medication for breakthrough pain Morphine sulfate MR 30 mg PO Doctor xx/xx Oramorph 10 mg PO Doctor 4 hrly 123 . xx/xx For breakthrough pain, give ~1/6 th of the total regular daily dose, every 4 hrs
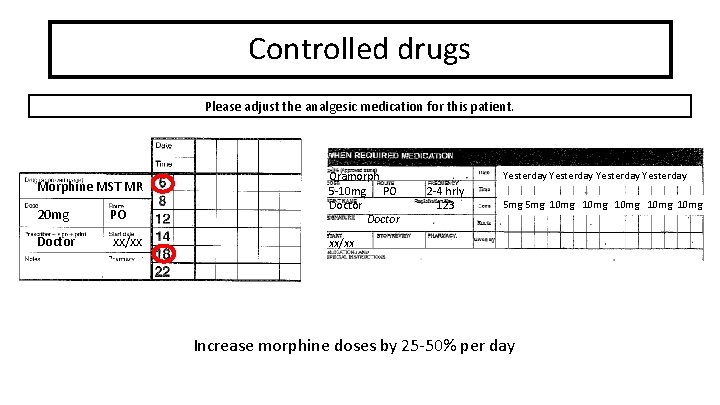
Controlled drugs Please adjust the analgesic medication for this patient. Morphine MST MR 20 mg PO Doctor xx/xx Oramorph 5 -10 mg PO Doctor Yesterday 2 -4 hrly 123 5 mg 10 mg 10 mg . xx/xx Increase morphine doses by 25 -50% per day
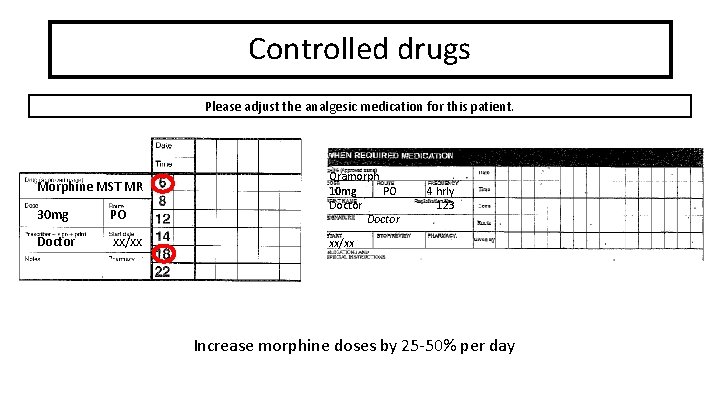
Controlled drugs Please adjust the analgesic medication for this patient. Morphine MST MR 30 mg PO Doctor xx/xx Oramorph 10 mg PO Doctor 4 hrly 123 . xx/xx Increase morphine doses by 25 -50% per day
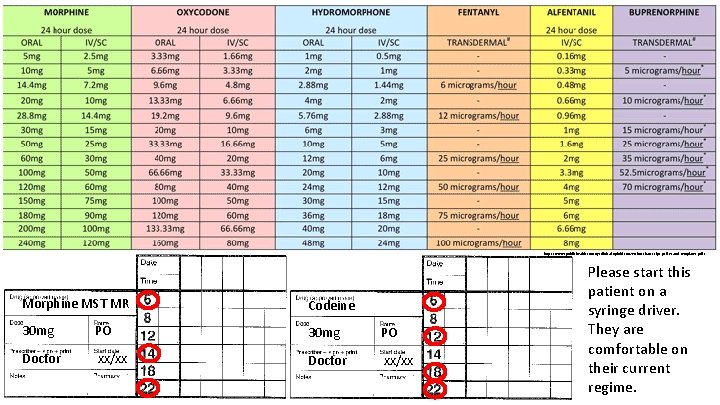
https: //www. publichealth. com. ng/clinical-opioid-conversion-charts-tips-guides-and-templates-pdf/ Morphine MST MR Codeine 30 mg PO Doctor xx/xx Please start this patient on a syringe driver. They are comfortable on their current regime.

Codeine is 3 -methoxymorphine In the body, it gets demethylated to become morphine A dose of codeine is equivalent to 1/10 th the dose of morphine i. e 100 mg codeine = 10 mg morphine 1) Total morphine MR dose = 30 mg TDS = 90 mg over 24 hrs 2) Total codeine dose = 30 mg QDS = 120 mg over 24 hrs = 12 mg morphine over 24 hrs So overall morphine dose = 102 mg oral dose over 24 hrs
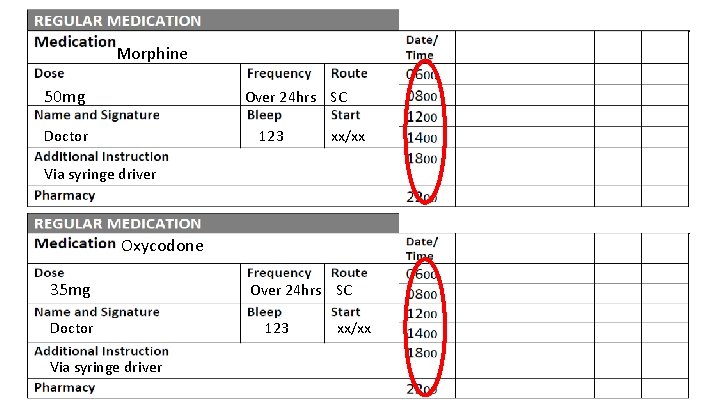

Morphine 50 mg Over 24 hrs SC Doctor 123 xx/xx Via syringe driver Oxycodone 35 mg Doctor Via syringe driver Over 24 hrs SC 123 xx/xx
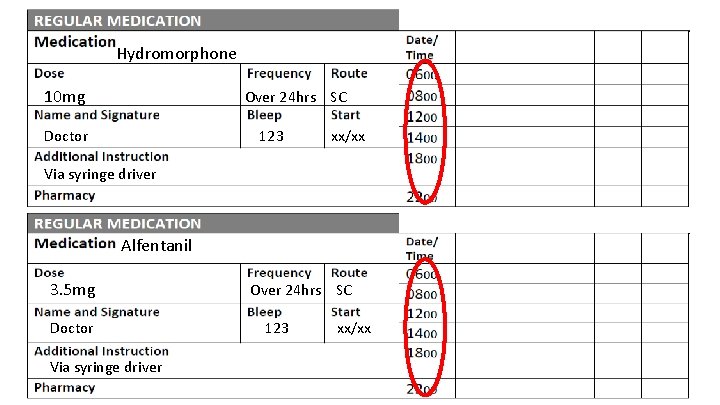
Hydromorphone 10 mg Over 24 hrs SC Doctor 123 xx/xx Via syringe driver Alfentanil 3. 5 mg Doctor Via syringe driver Over 24 hrs SC 123 xx/xx
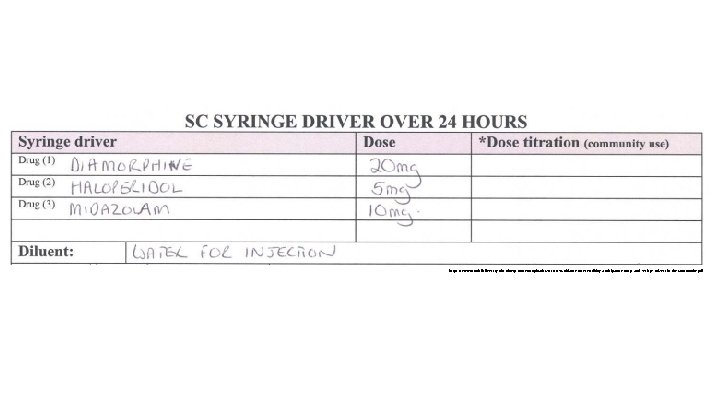

https: //www. northkirkleesccg. nhs. uk/wp-content/uploads/2013/07/Guidance-on-Prescribing-Anticipatory-Drugs-and-Syringe-Drivers-in-the-Community. pdf
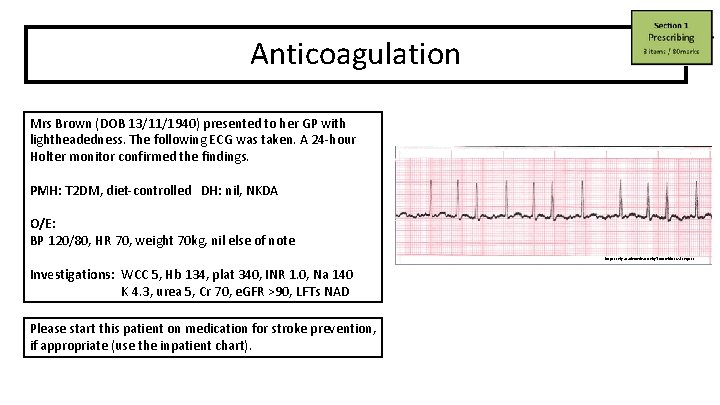
Anticoagulation Mrs Brown (DOB 13/11/1940) presented to her GP with lightheadedness. The following ECG was taken. A 24 -hour Holter monitor confirmed the findings. PMH: T 2 DM, diet-controlled DH: nil, NKDA O/E: BP 120/80, HR 70, weight 70 kg, nil else of note https: //ekg. academy/learn-ekg? courseid=312&seq=13 Investigations: WCC 5, Hb 134, plat 340, INR 1. 0, Na 140 K 4. 3, urea 5, Cr 70, e. GFR >90, LFTs NAD Please start this patient on medication for stroke prevention, if appropriate (use the inpatient chart).

CHA 2 DS 2 -VASc CHF Hypertension HAS-BLED 1 point 1 (>140/90 or on Tx) Age over 75 yr Diabetes Stroke/TIA 2 1 2 Vascular disease 1 (e. g MI, PVD) Age 65 -74 yr Sex category 1 1 if female 1 for each Hypertension >160 sys Abnormal liver/kidney function Stroke Bleeding Labile INRs Elderly: 65 yr or older Drugs (anti-platelets, alcohol >8 units/week) CHA 2 DS 2 -VASc = 4, HAS-BLED = 1
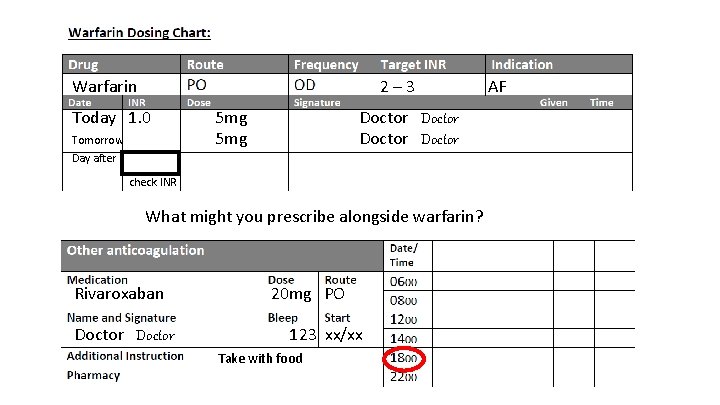
Warfarin 2– 3 Today 1. 0 Tomorrow 5 mg Doctor Day after check INR What might you prescribe alongside warfarin? Rivaroxaban Doctor 20 mg PO 123 xx/xx Take with food AF
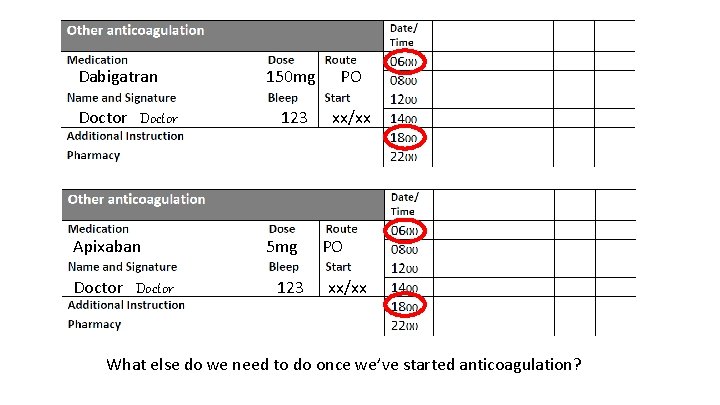
Dabigatran Doctor Apixaban Doctor 150 mg PO 123 xx/xx 5 mg 123 PO xx/xx What else do we need to do once we’ve started anticoagulation?

https: //www. pharmaceutical-journal. com/news-and-analysis/community-pharmacy-plays-its-part-in-making-anticoagulation-therapy-safer/10005896. article? first. Pass=false http: //www. ashfordstpeters. nhs. uk/press-releases-in-2016/203 -anticoagulation-clinic/601 -anticoagulation-clinic
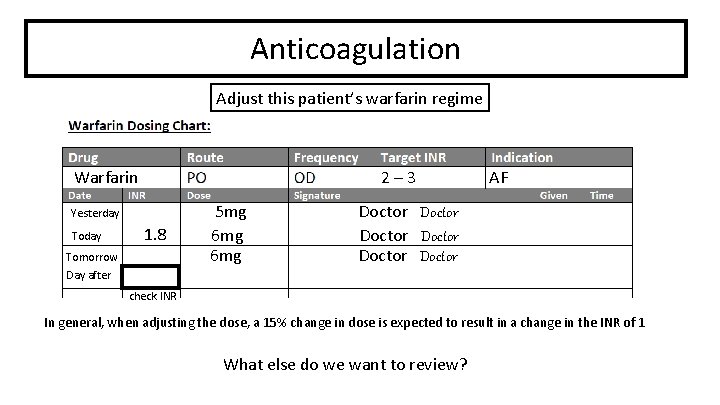
Anticoagulation Adjust this patient’s warfarin regime Warfarin 2– 3 Yesterday Today 1. 8 Tomorrow 5 mg 6 mg AF Doctor Doctor Day after check INR In general, when adjusting the dose, a 15% change in dose is expected to result in a change in the INR of 1 What else do we want to review?


Anticoagulation Prescribe appropriate treatment in the following clinical scenarios for a 70 kg patient: a) INR 6. 5, no bleeding a) INR 8. 5, mild epistaxis b) INR 3. 5, haematemesis with low BP
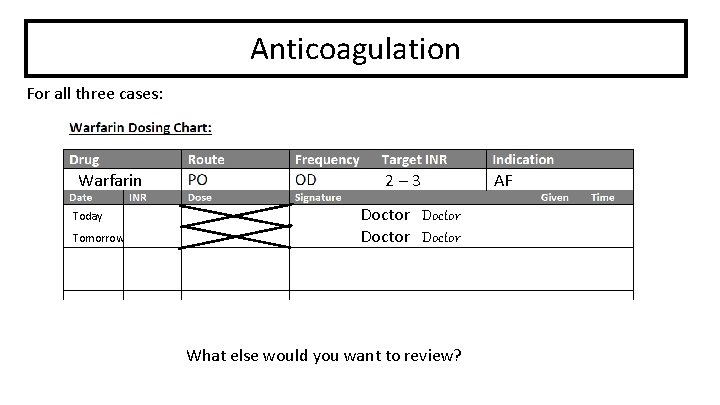

Anticoagulation For all three cases: Warfarin Today Tomorrow 2– 3 Doctor What else would you want to review? AF

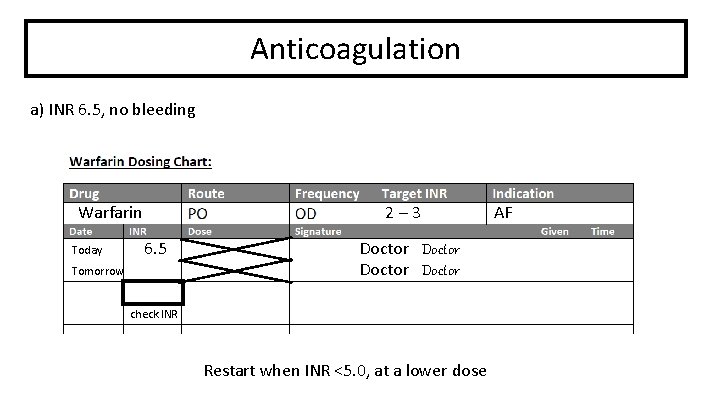
Anticoagulation a) INR 6. 5, no bleeding Warfarin Today 2– 3 6. 5 Tomorrow Doctor check INR Restart when INR <5. 0, at a lower dose AF
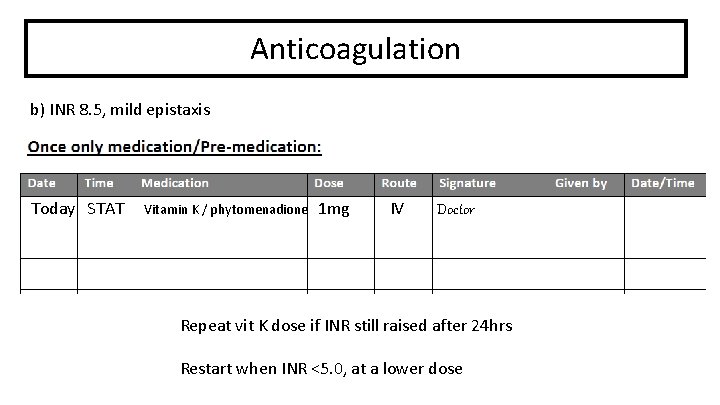

Anticoagulation b) INR 8. 5, mild epistaxis Today STAT Vitamin K / phytomenadione 1 mg IV Doctor Repeat vit K dose if INR still raised after 24 hrs Restart when INR <5. 0, at a lower dose
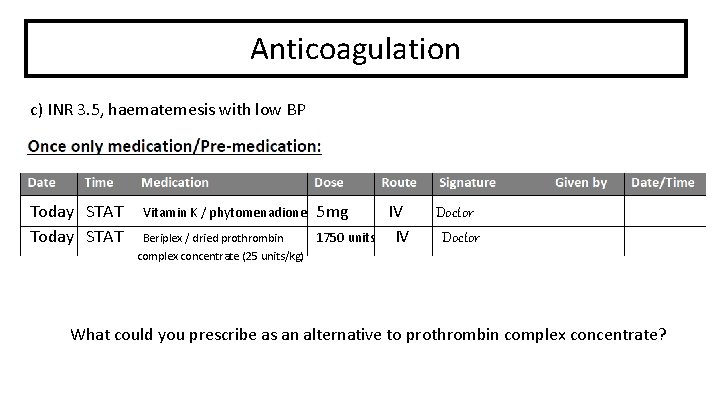
Anticoagulation c) INR 3. 5, haematemesis with low BP Today STAT Vitamin K / phytomenadione 5 mg Beriplex / dried prothrombin 1750 units IV IV Doctor complex concentrate (25 units/kg) What could you prescribe as an alternative to prothrombin complex concentrate?
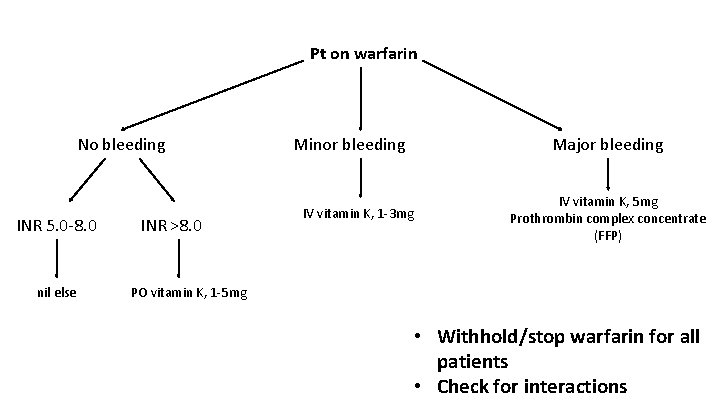
Pt on warfarin No bleeding INR 5. 0 -8. 0 nil else INR >8. 0 Minor bleeding IV vitamin K, 1 -3 mg Major bleeding IV vitamin K, 5 mg Prothrombin complex concentrate (FFP) PO vitamin K, 1 -5 mg • Withhold/stop warfarin for all patients • Check for interactions

Thanks! Any questions? www. surveymonkey. co. uk/r/29 Z 3 VF 5
- Slides: 36