Prescribing in the Elderly Karen Birmingham Pharm D

Prescribing in the Elderly Karen Birmingham, Pharm. D, BCPS Specialty Clinical Pharmacy Services Group Health

“Quote”worthy Definitions Aging Elderly “Progressive accumulation of random changes” “Age nearing or surpassing the average life span” “Time-related loss of functional units” “Age 65 years and older” “Better than the alternative” “Always 15 years older than me”

A Global “Gray Tsunami” • By the year 2006: – almost 500 million people worldwide had reached or exceeded age 65 • By the year 2030: – Total world population estimated to reach over 9 billion – Elderly population in developing countries projected to increase 140% – World population of people ≥ 65 years old expected to reach 1 billion • By the year 2050: – 20% of all elderly patients will be ≥ 80 years old

U. S. Elderly • • • Constitute 13% of the population Consume 34% of all prescription medications Use 40% of all over-the-counter drugs Up to 50% of elderly take multiple medications Medicare population analysis in 1999 (n=1. 2 million) – 82% had at least one chronic condition – 24% had at least four chronic conditions
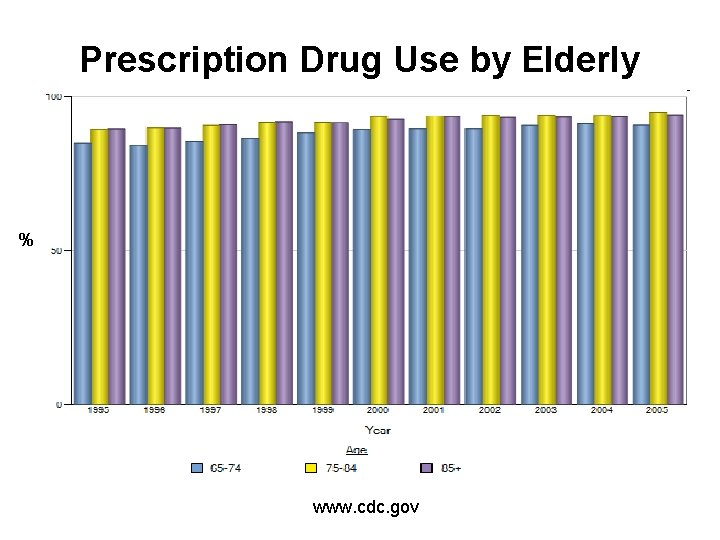
Prescription Drug Use by Elderly % www. cdc. gov
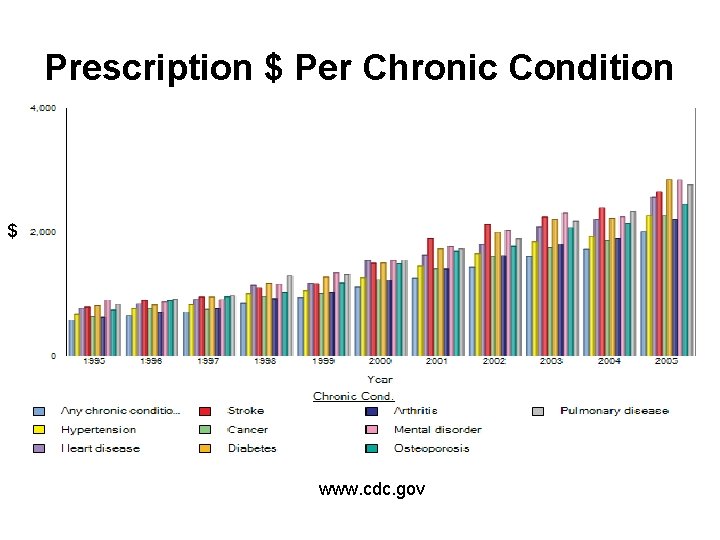
Prescription $ Per Chronic Condition $ www. cdc. gov
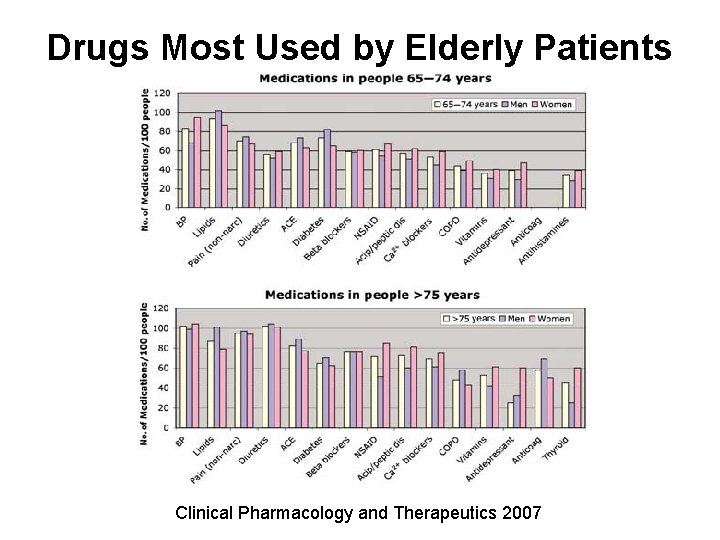
Drugs Most Used by Elderly Patients Clinical Pharmacology and Therapeutics 2007

ADE, ADR and ME Annals of Internal Medicine 2004

Adverse Drug Events • Occur in 20% of elderly patients • Account for 5 -10% of hospitalizations – Nearly 20% ranked as severe – Fatal outcomes in 6% of cases – Repeat hospitalizations in 30% of ADEs • Prevalence of 5 -37% in hospitalized patients – Interventions required in ~30% of patients • Affect ~ 350, 000 long-term care patients annually

Adverse Drug Events and Death “If medication-related problems were ranked as a disease by cause of death, it would be the 5 th leading cause of death in the United States. ” Archives of Internal Medicine 2003

Risk Factors For Adverse Drug Events • • Inappropriate prescribing Polypharmacy Misuse of OTC products Lack of appropriate drug monitoring Complicated dosing instructions Language or educational barriers Nonadherence
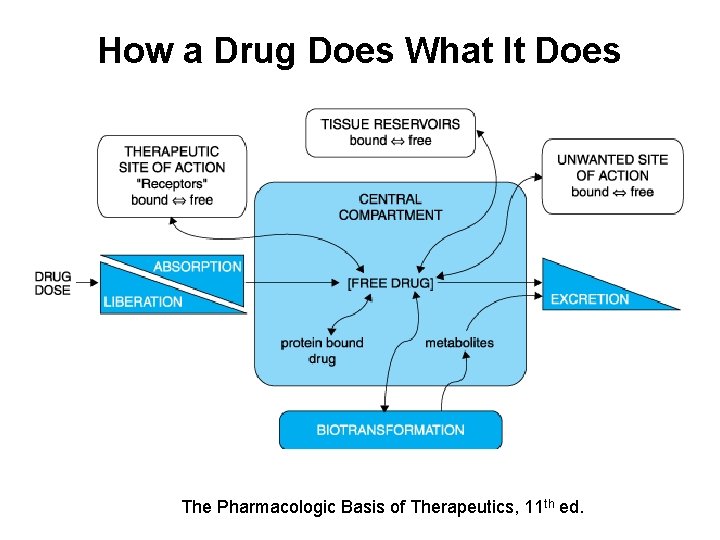
How a Drug Does What It Does The Pharmacologic Basis of Therapeutics, 11 th ed.
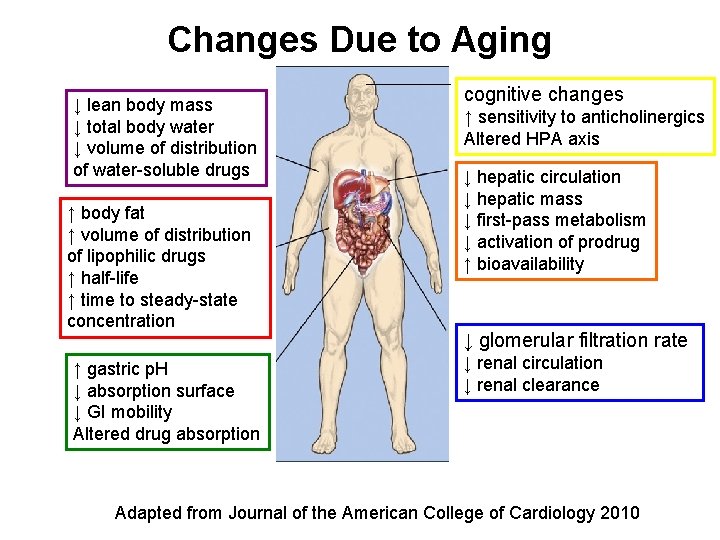
Changes Due to Aging ↓ lean body mass ↓ total body water ↓ volume of distribution of water-soluble drugs ↑ body fat ↑ volume of distribution of lipophilic drugs ↑ half-life ↑ time to steady-state concentration ↑ gastric p. H ↓ absorption surface ↓ GI mobility Altered drug absorption cognitive changes ↑ sensitivity to anticholinergics Altered HPA axis ↓ hepatic circulation ↓ hepatic mass ↓ first-pass metabolism ↓ activation of prodrug ↑ bioavailability ↓ glomerular filtration rate ↓ renal circulation ↓ renal clearance Adapted from Journal of the American College of Cardiology 2010
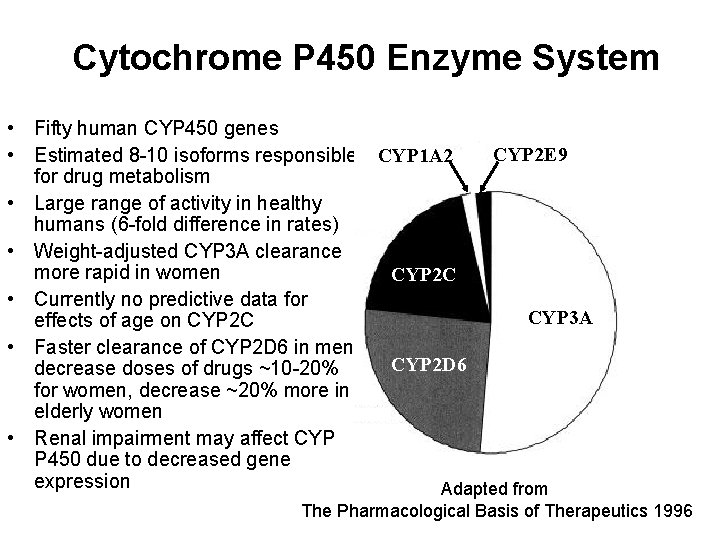
Cytochrome P 450 Enzyme System • Fifty human CYP 450 genes CYP 2 E 9 • Estimated 8 -10 isoforms responsible CYP 1 A 2 for drug metabolism • Large range of activity in healthy humans (6 -fold difference in rates) • Weight-adjusted CYP 3 A clearance more rapid in women CYP 2 C • Currently no predictive data for CYP 3 A effects of age on CYP 2 C • Faster clearance of CYP 2 D 6 in men; CYP 2 D 6 decrease doses of drugs ~10 -20% for women, decrease ~20% more in elderly women • Renal impairment may affect CYP P 450 due to decreased gene expression Adapted from The Pharmacological Basis of Therapeutics 1996
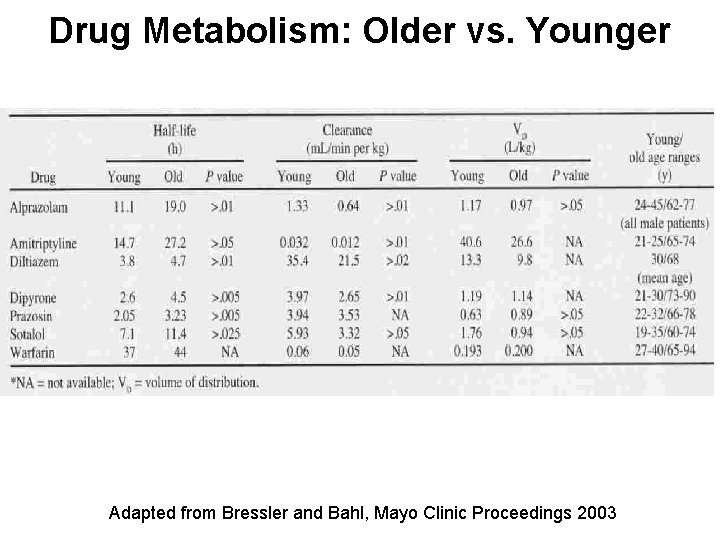
Drug Metabolism: Older vs. Younger Adapted from Bressler and Bahl, Mayo Clinic Proceedings 2003

P-Glycoprotein and Drug Disposition • Efflux transporter • Found in hepatocytes, intestinal mucosal cells, and blood-brain barrier • Conflicting results from small studies: – Animal studies suggest differences between male and female, not yet observed in humans – One study showed no significant difference in leukocyte P-glycoprotein in comparisons of young healthy adults vs. elderly healthy and frail adults – Another study suggested decreased blood-brain barrier P-glycoprotein activity, possibly exposing brain to higher levels of drugs

Age Effects on Hemostasis Coagulation Proteins ↑ Factor VIII ↑ Factor IX ↑ Factor XIII ↑ Fibrinogen ↑ kininogen ↑ prekallikrein Fibrinolytic Proteins ↑ D-dimer ↑ PAI-1 ↓ plasmin Anticoagulant Proteins Antithrombin III Protein C Protein S TFPI ♂↓ ♂↔ ♂↔ ♂↓ Adapted from Journal of the American College of Cardiology 2010 ♀↓ ♀↑ ♀↑ ♀↑
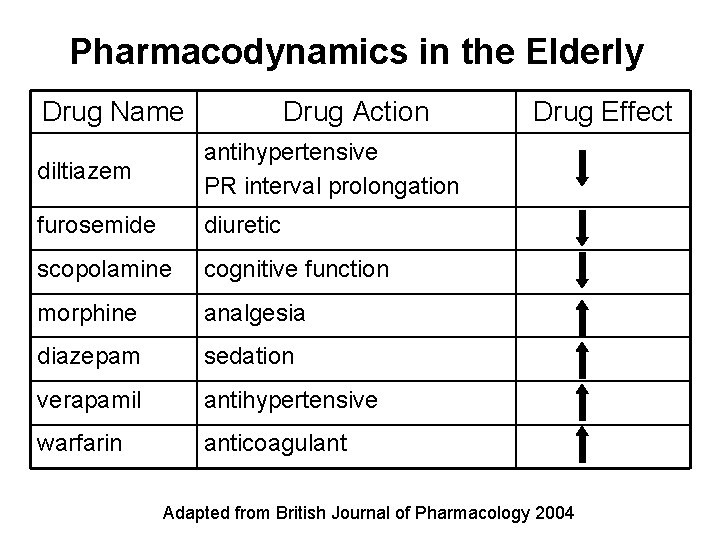
Pharmacodynamics in the Elderly Drug Name Drug Action diltiazem antihypertensive PR interval prolongation furosemide diuretic scopolamine cognitive function morphine analgesia diazepam sedation verapamil antihypertensive warfarin anticoagulant Drug Effect Adapted from British Journal of Pharmacology 2004
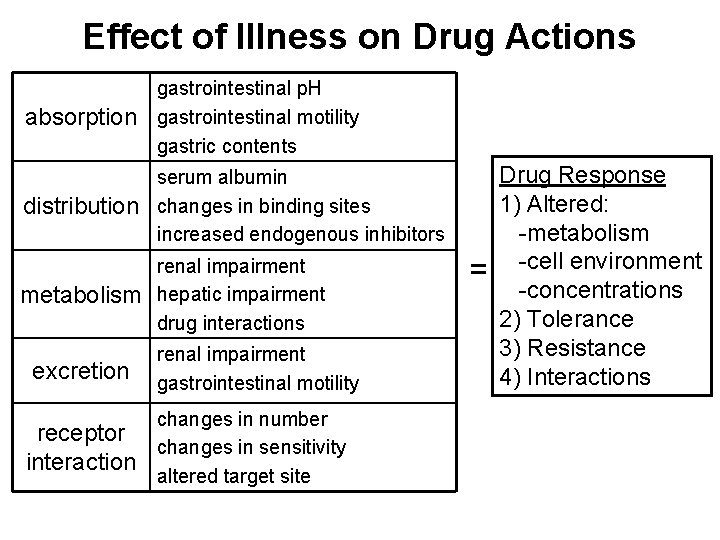
Effect of Illness on Drug Actions absorption gastrointestinal p. H gastrointestinal motility gastric contents distribution serum albumin changes in binding sites increased endogenous inhibitors metabolism renal impairment hepatic impairment drug interactions excretion receptor interaction renal impairment gastrointestinal motility changes in number changes in sensitivity altered target site = Drug Response 1) Altered: -metabolism -cell environment -concentrations 2) Tolerance 3) Resistance 4) Interactions
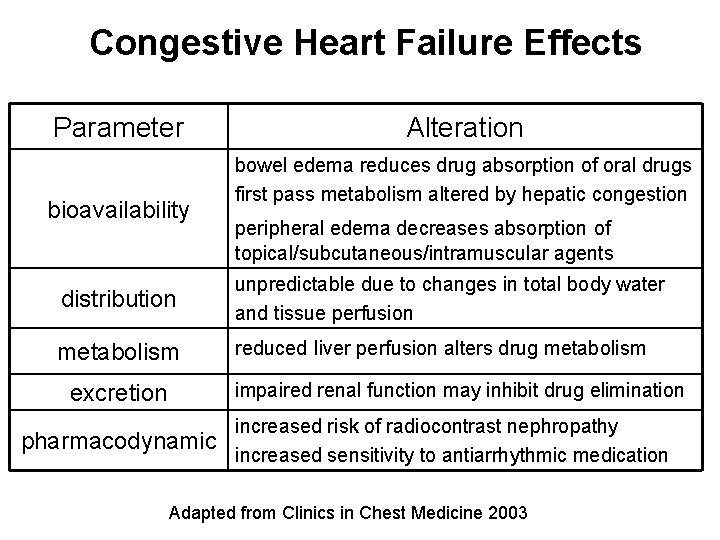

Congestive Heart Failure Effects Parameter bioavailability Alteration bowel edema reduces drug absorption of oral drugs first pass metabolism altered by hepatic congestion peripheral edema decreases absorption of topical/subcutaneous/intramuscular agents distribution unpredictable due to changes in total body water and tissue perfusion metabolism reduced liver perfusion alters drug metabolism impaired renal function may inhibit drug elimination excretion pharmacodynamic increased risk of radiocontrast nephropathy increased sensitivity to antiarrhythmic medication Adapted from Clinics in Chest Medicine 2003
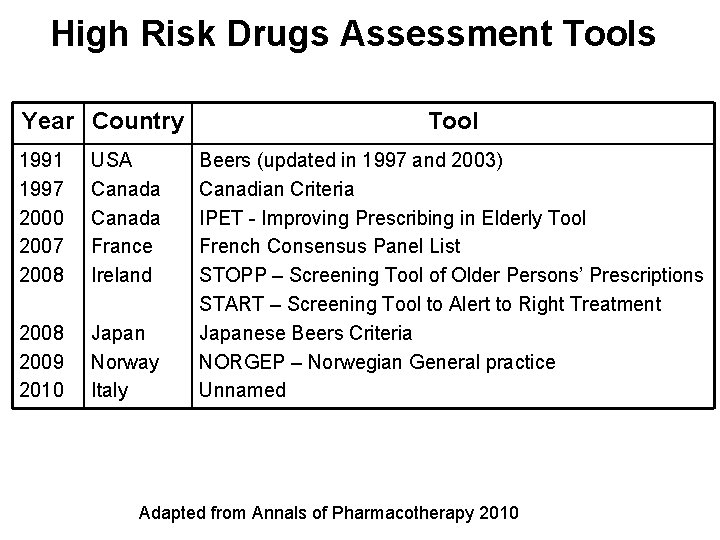
High Risk Drugs Assessment Tools Year Country 1991 1997 2000 2007 2008 USA Canada France Ireland 2008 2009 2010 Japan Norway Italy Tool Beers (updated in 1997 and 2003) Canadian Criteria IPET - Improving Prescribing in Elderly Tool French Consensus Panel List STOPP – Screening Tool of Older Persons’ Prescriptions START – Screening Tool to Alert to Right Treatment Japanese Beers Criteria NORGEP – Norwegian General practice Unnamed Adapted from Annals of Pharmacotherapy 2010
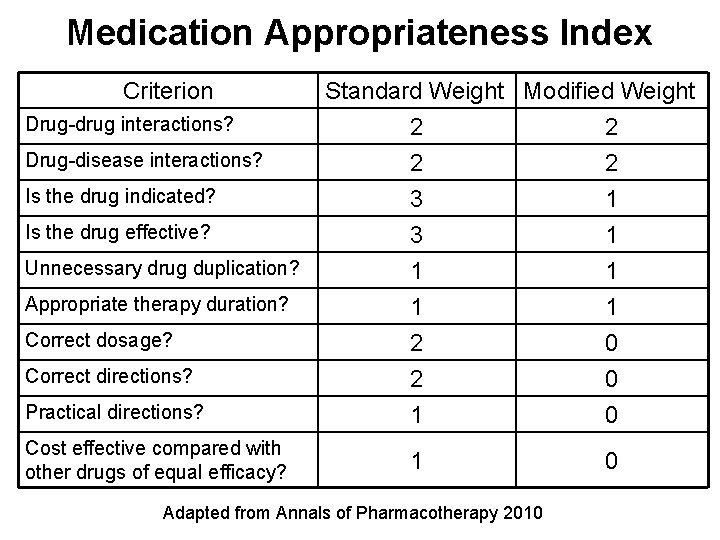
Medication Appropriateness Index Criterion Drug-drug interactions? Drug-disease interactions? Is the drug indicated? Is the drug effective? Standard Weight Modified Weight 2 2 3 1 Practical directions? 3 1 1 2 2 1 1 0 0 0 Cost effective compared with other drugs of equal efficacy? 1 0 Unnecessary drug duplication? Appropriate therapy duration? Correct dosage? Correct directions? Adapted from Annals of Pharmacotherapy 2010

Anticholinergic Risk Scale 3 points 2 points 1 point amitriptyline amantadine carbidopa-levodopa atropine baclofen entacapone carisoprodol cetirizine haloperidol chlorpheniramine cimetidine methocarbamol chlorpromazine clozapine metoclopramide cyproheptadine cyclobenzaprine mirtazapine dicyclomine desipramine paroxetine diphenhydramine loperamide pramipexole hydroxyzine loratadine quetiapine imipramine nortriptyline ranitidine promethazine olanzapine risperidone meclizine prochlorperazine selegiline promethazine tolterodine trazodone Adapted from Archives of Internal Medicine 2008

Drug Burden Index (DBI) Total drug burden = BAC + BS DBI: E = __D__ + D ↑ DBI = ↓ physical performance and cognition Equations from Archives of Internal Medicine 2007

The Big Issues • • • Cognition, sedation, falls GI toxicity Cardiopulmonary effects Bleeding/clotting Renal impairment Liver toxicity

High Risk For Falls Anticholinergics scopolamine atropine belladonna pentobarbital hyoscyamine phenobarbital secobarbital propantheline dicyclomine Muscle Relaxants carisoprodol methocarbamol cyclobenzaprine chlorzoxazone meprobamate metaxalone Tricyclic Antidepressants amoxapine amitriptyline Antihistamines diphenhydramine, hydroxyzine, cyproheptadine Antiemetics promethazine, trimethobenzamide doxepin imipramine protriptyline clomipramine Benzodiazepines diazepam, flurazepam, triazolam, chlordiazepoxide Narcotics meperidine, propoxyphene

Recommendations for Screening Perform fall risk screening on all elderly patients, including: – History of falls or problems with gait/balance – Complete medication review, including prescriptions, over-the-counter drugs, herbal products, nutritional supplements, etc. – Chronic condition risk factors, e. g. osteoporosis, cardiovascular disease, visual impairment, etc. – Assessment of vitamin D deficiency

NSAIDS and GI Risk Relative GI Toxicity of Select NSAIDs Nabumetone Least Etodolac Salsalate Sulindac Diclofenac Ibuprofen Ketoprofen Aspirin Naproxen Flurbiprofen Piroxicam Fenoprofen Indomethacin Meclofenamate Most Adapted from Carman, EBRx Newsletter 2009
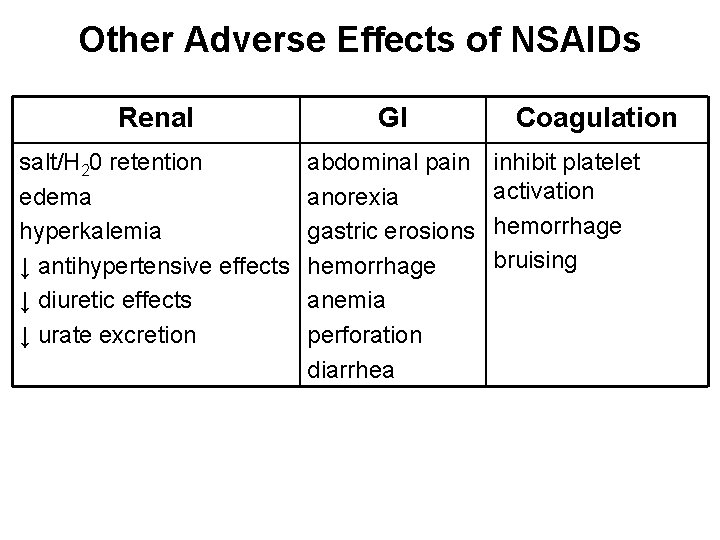
Other Adverse Effects of NSAIDs Renal GI salt/H 20 retention edema hyperkalemia ↓ antihypertensive effects ↓ diuretic effects ↓ urate excretion abdominal pain anorexia gastric erosions hemorrhage anemia perforation diarrhea Coagulation inhibit platelet activation hemorrhage bruising
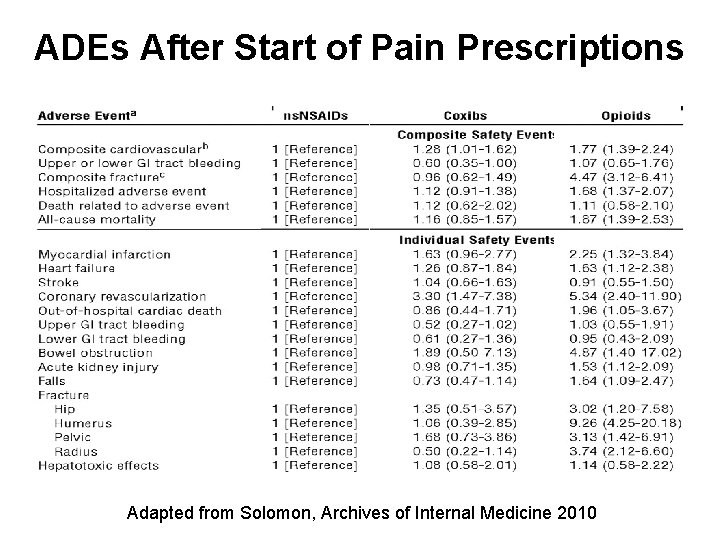
ADEs After Start of Pain Prescriptions Adapted from Solomon, Archives of Internal Medicine 2010

Acetaminophen • Present in multiple OTC products and prescription pain medications • Maximum daily dose often exceeded in community and in hospitals • Increasing reports of severe hepatotoxicity – Higher risk in patients who abuse alcohol and/or exceed dose recommendations • By 2014, all acetaminophen prescription products must have no more than 325 mg acetaminophen per dosage unit – New dose limit set by FDA in January 2011
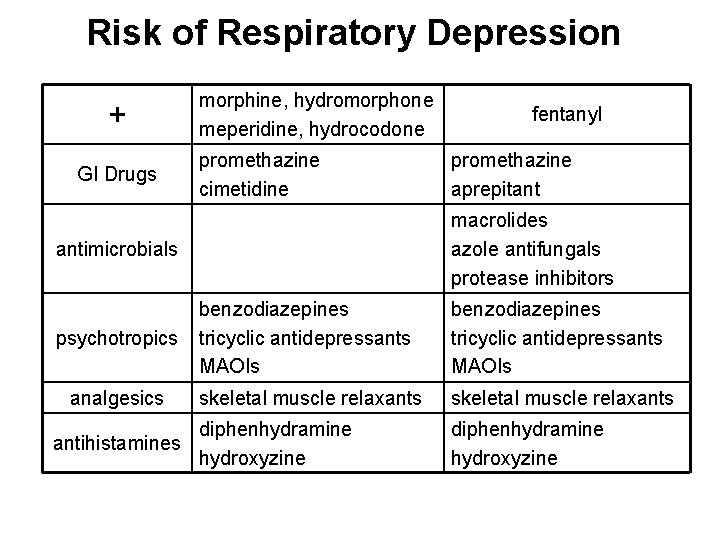
Risk of Respiratory Depression + GI Drugs morphine, hydromorphone meperidine, hydrocodone promethazine cimetidine fentanyl promethazine aprepitant macrolides azole antifungals protease inhibitors antimicrobials psychotropics benzodiazepines tricyclic antidepressants MAOIs analgesics skeletal muscle relaxants diphenhydramine antihistamines hydroxyzine diphenhydramine hydroxyzine
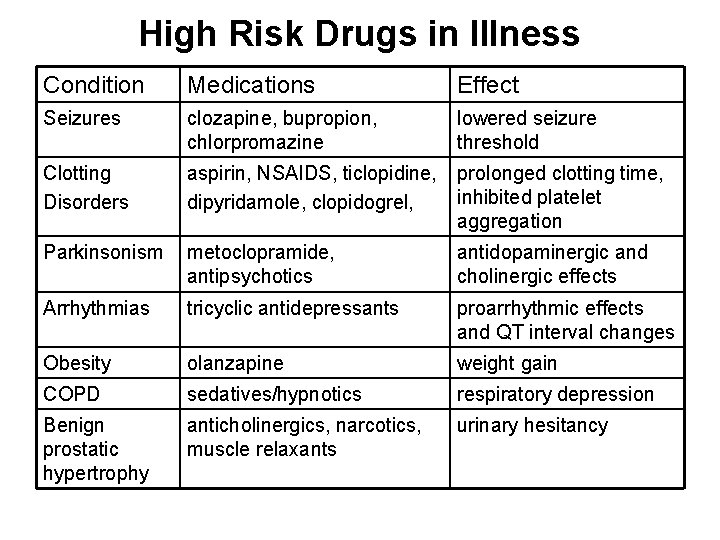
High Risk Drugs in Illness Condition Medications Effect Seizures clozapine, bupropion, chlorpromazine lowered seizure threshold Clotting Disorders aspirin, NSAIDS, ticlopidine, dipyridamole, clopidogrel, prolonged clotting time, inhibited platelet aggregation Parkinsonism metoclopramide, antipsychotics antidopaminergic and cholinergic effects Arrhythmias tricyclic antidepressants proarrhythmic effects and QT interval changes Obesity olanzapine weight gain COPD sedatives/hypnotics respiratory depression Benign prostatic hypertrophy anticholinergics, narcotics, muscle relaxants urinary hesitancy
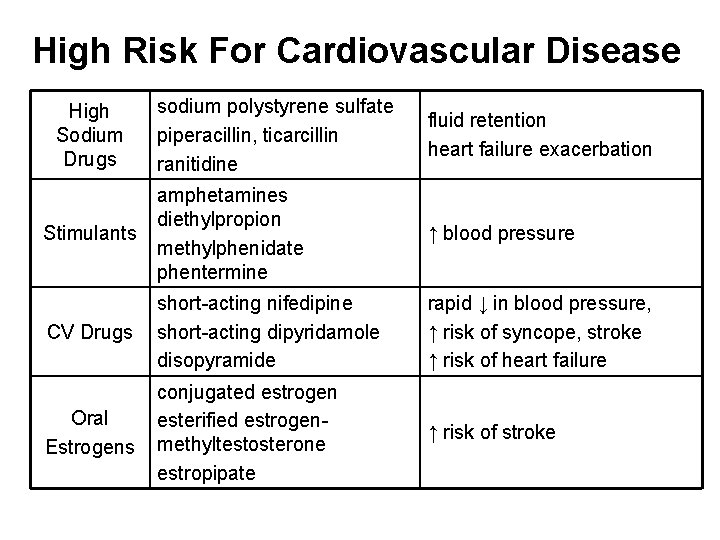
High Risk For Cardiovascular Disease sodium polystyrene sulfate piperacillin, ticarcillin ranitidine fluid retention heart failure exacerbation Stimulants amphetamines diethylpropion methylphenidate phentermine ↑ blood pressure CV Drugs short-acting nifedipine short-acting dipyridamole disopyramide rapid ↓ in blood pressure, ↑ risk of syncope, stroke ↑ risk of heart failure Oral Estrogens conjugated estrogen esterified estrogenmethyltestosterone estropipate ↑ risk of stroke High Sodium Drugs

Drug Interactions • Drug interactions and polypharmacy – Two drugs = DDI occurrence in ~ 13% of patients – Six drugs = DDI occurrence in ~ 80% of patients • Hospitalizations within one week of interactions – Glyburide + cotrimoxazole= 35/909 patients – Digoxin + clarithromycin = 27/1051 patients – ACE inhibitors + diuretics = 43/523 patients • Concomitant alcohol use by 20% of elderly • Many patients report use of nutritional or herbal supplements.
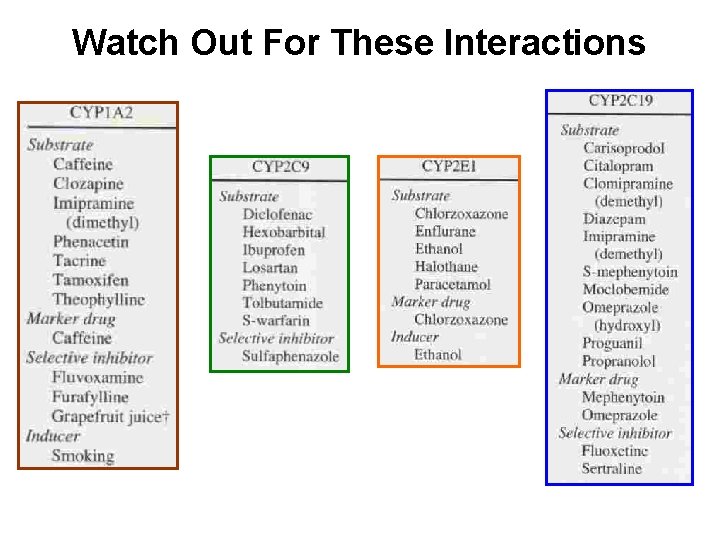
Watch Out For These Interactions

Watch Out For These Interactions
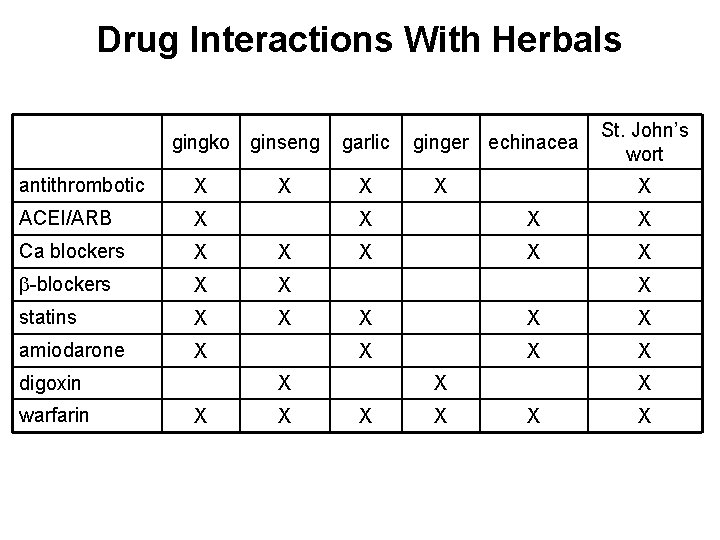
Drug Interactions With Herbals gingko ginseng antithrombotic X ACEI/ARB X Ca blockers X X -blockers X X statins X X amiodarone X digoxin warfarin X garlic X X X St. John’s wort X X X X ginger echinacea X X X

ADEs: Drug Shortages and Recalls Pre-diluted methotrexate was unavailable; a vial of dry powder was reconstituted incorrectly and the patient received less than the prescribed dose Wrong dose of morphine administered after 4 mg/m. L prefilled syringes were replaced with 5 mg/m. L vials Cancellations of surgeries and procedures Chemotherapy treatments delayed in a patient with a high potential for remission while attempting to find a source of the needed drug Unintended intraoperative awareness occurred when a patient was given too little propofol based on weight in an attempt to conserve supplies Shortage of IV sulfamethoxazole/ trimethoprim) led to refractory cases of pneumocystis pneumonia from alternative treatment with clindamycin and primaquine

Prevention of ADEs Frequent medication review and reconciliation Evaluation of indications, benefits, side effects Review of preprinted orders or prescription pads Ensure medication literacy Pharmacologic “debridement” Utilization of online drug evaluation tools Routine pharmacist consultation
- Slides: 40