Prescribing for Palliative Patients a primary care approach

Prescribing for Palliative Patients; a primary care approach Dr Laura Smith GP ST 1

Contents The role of the GP in palliative care – Out of hours – out of ideas? – – Assessment Analgesia Pain Quiz • • • Which one? When? Which Route?

The role of the GP in palliative care Palliative care: 'the active, holistic care of patients with advanced, progressive illness' Why is the GP ideal to facilitate this? long-established relationships with their patients used to dealing with co-morbidity and uncertainty trained to treat patients holistically Care needs to be PROACTIVE

When should we think about palliative care? If a patient is diagnosed with cancer? If a patient needs a syringe driver? If a patient has hours to live? . . . When a patient is in the last year of their life (GSF) Identify GP Assess Plan

Imagine you are a GP. . . How many of your patients are in the last year of their life? 10% 1% 0. 1% On average, each GP has 20 deaths per year: How many of these will be from cancer? How many will be from organ failure? How many from dementia/frailty or MOF? How many will be sudden/unexpected?

Out of hours – out of ideas? Groups of 2 -3 Imagine you are working as the OOH GP: you are called out to a patient who is near the end of life suffering with cancer. His wife is concerned because. . . he won't stop hiccuping doctor, it has been going on for hours! What would you prescribe?
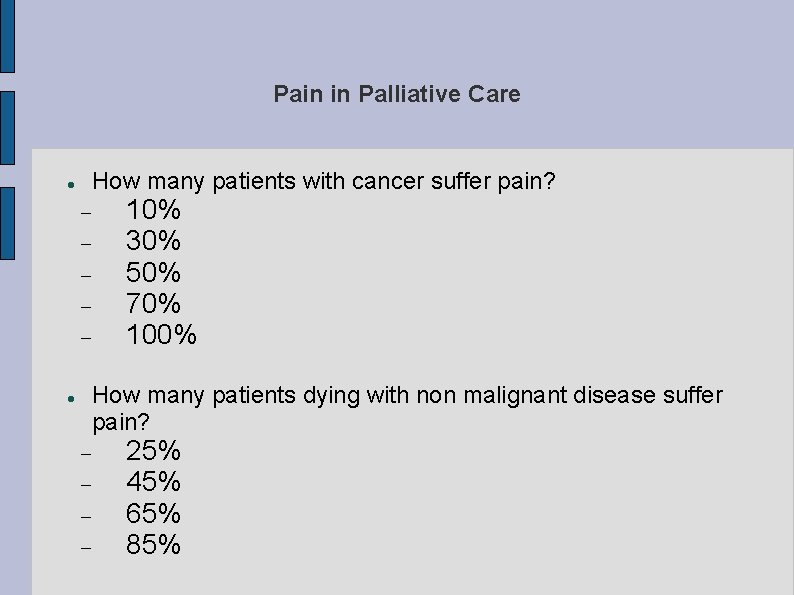
Pain in Palliative Care How many patients with cancer suffer pain? 10% 30% 50% 70% 100% How many patients dying with non malignant disease suffer pain? 25% 45% 65% 85%
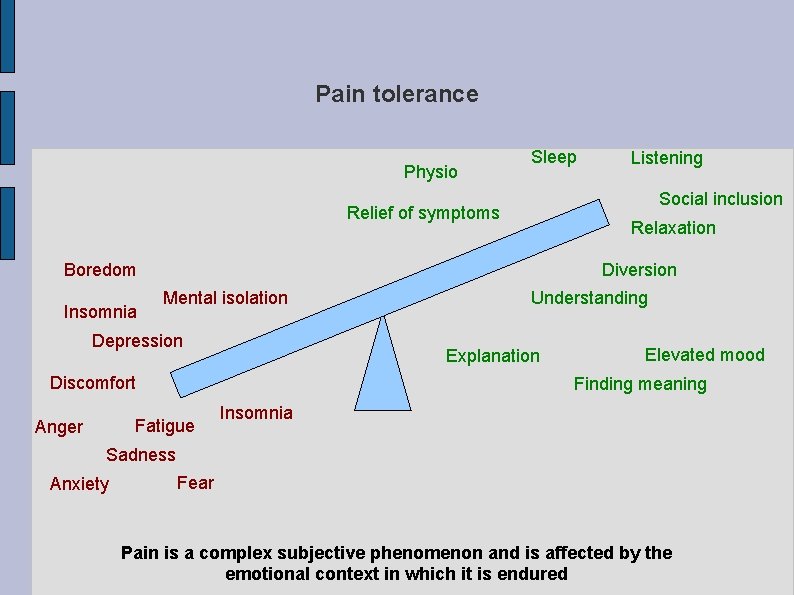
Pain tolerance Physio Sleep Social inclusion Relief of symptoms Relaxation Boredom Insomnia Diversion Mental isolation Depression Understanding Explanation Discomfort Elevated mood Finding meaning Fatigue Anger Listening Insomnia Sadness Anxiety Fear Pain is a complex subjective phenomenon and is affected by the emotional context in which it is endured

History taking SOCRATES Physical effects or manifestations Functional impact of pain Psychosocial factors Spiritual aspects Self assessment important as pain subjective Help patient to actively manage their pain What is causing the pain?

The WHO pain ladder
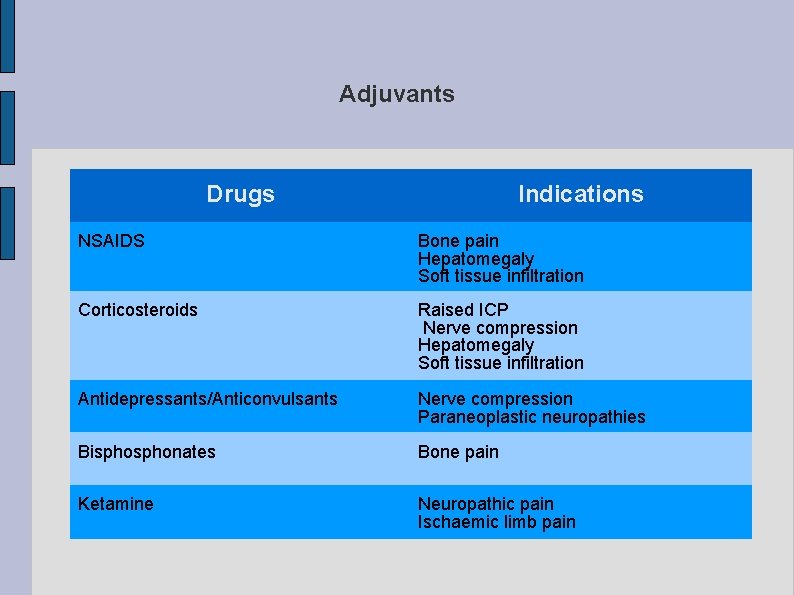
Adjuvants Drugs Indications NSAIDS Bone pain Hepatomegaly Soft tissue infiltration Corticosteroids Raised ICP Nerve compression Hepatomegaly Soft tissue infiltration Antidepressants/Anticonvulsants Nerve compression Paraneoplastic neuropathies Bisphonates Bone pain Ketamine Neuropathic pain Ischaemic limb pain

Non Opiates Paracetamol Weak Few side effects NSAIDS Good for bone pain SE: GI Bleed

Opiates Weak opioids Codiene Tramadol Use with non-opioids Strong opioids Morphine “For patients with no renal or hepatic comorbidities, offer a typical total daily starting dose schedule of 20 -30 mg of oral morphine plus 5 mg oral immediate-release morphine for rescue doses during the titration phase” NICE
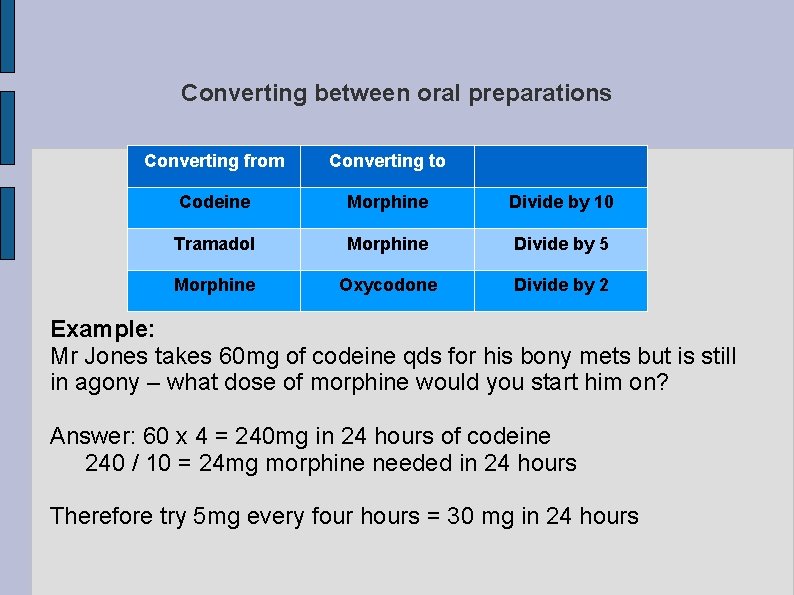

Converting between oral preparations Converting from Converting to Codeine Morphine Divide by 10 Tramadol Morphine Divide by 5 Morphine Oxycodone Divide by 2 Example: Mr Jones takes 60 mg of codeine qds for his bony mets but is still in agony – what dose of morphine would you start him on? Answer: 60 x 4 = 240 mg in 24 hours of codeine 240 / 10 = 24 mg morphine needed in 24 hours Therefore try 5 mg every four hours = 30 mg in 24 hours

Breakthrough pain 1/6 th of total 24 hour dose can be given as a “rescue dose” for pain between doses of regular morphine This can be repeated every 4 hours AIM: Prevent pain, not relieve pain

Parental route of administration When should this be used: Patient unable to swallow, vomiting, weakness, dysphagia IM/SC morphine = ½ oral morphine dose IM/SC diamorphine = 1/3 oral morphine dose

Transdermal route of administration NOT for acute pain, or for patients whose analgesic requirements change rapidly Use if: problems with oral route, constipation, subacute obstruction or morphine intolerance Oral Morphine Dose Patch equivalent 45 mg daily Fentanyl “ 12” patch 90 mg daily Fentanyl “ 25” patch 180 mg daily Fentanyl “ 50” patch 270 mg daily Fentanyl “ 75” patch 360 mg daily Fentanyl “ 100” patch

Poor kidney function: preventing and managing opioid toxicity Consider dose reduction +/- increased dose interval Use immediate-release oral formulation Switch to alfentanil, buprenorphine or fentanyl, which are the opioids of choice where e. GFR <30 ml/minute Frequent monitoring and review Seek specialist advice

Top Tips Continuous pain = regular analgesia NOT prn Take breakthrough analgesia before undertaking a potentially pain-provoking activity KISS: Minimum number of drugs in the most acceptable form and dose intervals possible Written guidance for patients and families Regular review of effectiveness and side effects Adequate prn medications

Quiz Mr Smith comes to see you in your morning surgery. 18 months ago he was diagnosed with bowel cancer. He underwent surgery and chemotherapy but 1 month ago was diagnosed with recurrence with spread to the liver. He comes to see you as he is getting worsening continuous abdominal pain. You take a careful history and you wish to change his pain relief.

Question 1 Mr Smith currently takes: Paracetamol 1 g po qds Ibuprofen 400 mg po tds Codeine 60 mg qds Oral morphine 20 mg immediate release tablets twice daily You wish to convert him to a higher dose of morphine and stop the codeine – what dose of immediate release morphine tablets will you prescribe? A) 10 mg prn B) 10 mg 4 hourly C) 5 mg 4 hourly D) 20 mg 4 hourly

Question 2 What breakthrough dose of oromorph does he need? A)10 mg B) 5 mg C) 6 mg D) 10 ml

Question 3 Mr Smith returns to the surgery later that week. You review his analgesia use: He has taken 10 mg four hourly regularly but most days has needed a breakthrough dose before bed and when taking his dog for a walk (twice a day). How would you alter his morphine dose? A) 45 mg four hourly with 10 mg breakthrough B) 15 mg four hourly with 10 mg breakthrough C) 15 mg four hourly with 15 mg breakthrough D) 20 mg four hourly with 20 mg breakthrough

Question 4 As a good GP what else might you prescribe Mr Smith when you prescribe his morphine? A)Naloxone B)Phosphate enema C)Lactulose and senna D)Ondansetron

Question 5 Mr Smith comes the following week – his pain much better controlled and he is not needing any breakthrough treatment, but is concerned that he feels he is taking medication all the time. What could you do? A)Tell him to skip some doses and see how he feels B)Convert him to a twice daily morphine slow release dose of 45 mg bd C)Convert him to a twice daily morphine slow release dose of 90 mg bd D)Prescribe a fentanyl “ 25” patch

Question 6 2 months later you are asked to see Mr Smith on a home visit. He has been reviewed by your colleagues and is now taking 75 mg bd or MR morphine sulphate tablets. He now describes a burning and tingling type pain in his feet which is making it difficult to walk. It started 14 months ago after the chemotherapy but is now worsening. What would you prescribe? A) MR MST 90 mg bd B) Amitriptiline 10 mg po nocte C) Gabapentin 600 mg tds D) Crutches

Question 7 Unfortunately several weeks later Mr Smith is admitted to hospital overnight unwell with confusion. When discharged home the EDS notes for GP state: “Please alter medication as found to have renal impairment. ” On his last repeat prescription he was on 90 mg bd MR MST, ibuprofen 400 mg tds, amitriptiline 10 mg nocte with 30 mg oromorph as breakthrough prn, lactulose 10 ml bd, senna TT po nocte. Which of his medicines needs to be altered? A)Reduce ibuprofen only B)Stop MST only C)Stop ibuprofen, change MST to fentanyl patch D)Reduce ibupofen, change MST to fentanyl patch

Question 8 What dose of fentanyl patch will you prescribe and when should it be started? A) Fentanyl “ 50” apply at same time as last dose of MR MST given B) Fentanyl “ 25” apply 12 hours after last dose MR MST given C) Fentanyl “ 75” apply at same time as last dose of MR MST given D) Fentanyl “ 12” apply 12 hours after last dose MR MST given

Question 8 Luckily whilst you are working this out the receptionist receives a phone call from the oncall FY 1 – who sent the EDS in error: the patient does not have renal failure – but has deteriorated so could you do a home visit to check on him? On visiting the patient you confirm that he has quickly deteriorated, but he wishes to die at home, with his family supporting him. He is too weak to swallow tablets, and seems in pain. You wish to convert his 90 mg bd MR MST to subcut diamorphine - what is the daily dose? A) 45 mg B) 30 mg C) 90 mg D) 60 mg
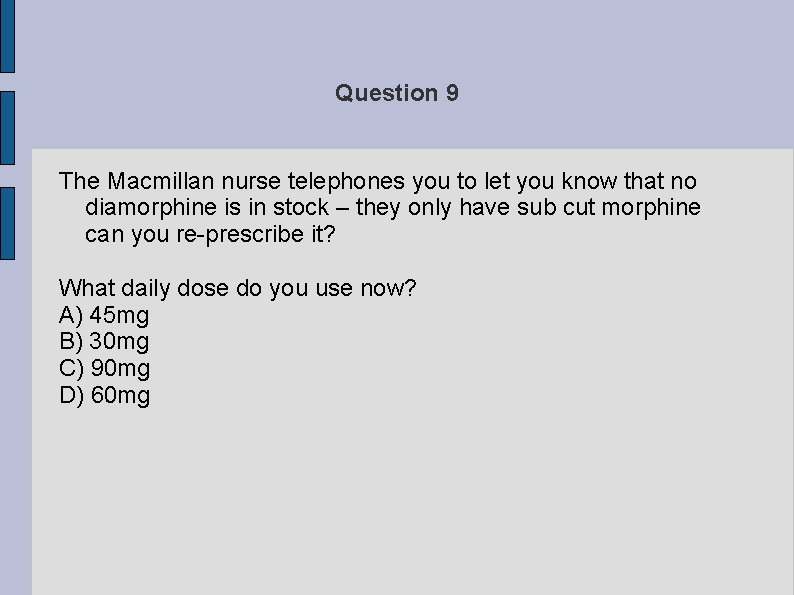
Question 9 The Macmillan nurse telephones you to let you know that no diamorphine is in stock – they only have sub cut morphine can you re-prescribe it? What daily dose do you use now? A) 45 mg B) 30 mg C) 90 mg D) 60 mg

Question 10 You visit Mr Smith on a home visit 3 days later. He is in bed, and is asleep. His breathing has slowed but is very noisy due to secretions. His wife is upset thinking that he is in distress. You think he may be entering the last few hours of life. What might you prescribe? A) Increase his morphine to speed up his death and lessen the agony for his wife. B) Hyoscine hydrobromide 400 microgram subcut C) Midazolam 2. 5 -5 mg subcut D) Cyclizine 50 mg subcut

Summary The role of the GP in palliative care Pain – – Assessment Analgesia • • • Which one? When? Which Route?

References Pain Control in Palliative Care: Patient. co. uk Liverpool Care Pathway for the Dying Patient (LCP) Palliative Care Guidelines: NHS Scotland Opioids in palliative care: safe and effective prescribing of strong opioids for pain in palliative care of adults: NICE guidelines
Final thoughts Mr Smith passes away peacefully that night. His family are happy with the care he has received and thank you for not putting him on that awful death pathway like they do in Liverpool! How do you respond?
- Slides: 34