Prescribing Controlled Substances Problematic Use of Opioids and

"Prescribing Controlled Substances: Problematic Use of Opioids and Benzodiazepines in Clinical Care" Daryl Shorter, MD Staff Psychiatrist Michael E. De. Bakey VA Medical Center March 2, 2017

Objectives - By the completion of the presentation, learners will be able to: (1) List risk factors for misuse, diversion, and/or dependence upon opioid medications and benzodiazepines (2) Identify clinical scenarios in which there is problematic use/prescribing of opioid medications and benzodiazepines (3) Employ treatment algorithms to successfully taper opioid medications and benzodiazepines (4) Discuss strategies for patient monitoring and mitigating risk factors for opioid and benzodiazepine misuse

Definitions • Misuse • Diversion • Dependence

Definitions • Misuse • Diversion • Dependence

Misuse (1) • Any medication use that occurs without prescription (therapeutic benefit v intoxication? ) • Legitimately prescribed medication used for intoxication/euphoria • Medication use in context of dependence (methadone, buprenorphine)

Misuse (2) • Motives for Non-Prescribed Medication Use – Intoxication • High dose, intravenous • Combined with alcohol or other drugs – Therapeutic use • Bona fide condition/appropriate indication • Correct dosing pattern Barrett SP et al. What constitutes prescription drug misuse? Problems and current conceptualizations. Curr Drug Abuse Reviews. 2008; 1: 255 -62.

Misuse (3) • Group differences – Adolescents • Sedative/hypnotics, opiates = therapeutic > recreation • Stimulant medications = recreation – College students • Therapeutic benefit > recreation – Older adults • Withdrawal, dependence

Misuse (4) • Quasi-legitimate Reasons? – Immediate/acute need – Unable to seek formal medical consultation – Barriers to access • Socioeconomic • Geographic • Temporal – Provider reluctance to prescribe – Under-medication

Misuse (5) • Clinical implications of different forms of misuse – Increased risk of overdose – Mitigation of other substance effects

Definitions • Misuse • Diversion • Dependence

Diversion • Exchange of prescription medications • Leads to drug use by unintended persons • Under conditions associated with – “Doctor shopping” – Misrepresentation of medical problems – Theft – Trading, selling, loaning, giving away

Diversion (2) • Gender differences in diversion patterns – 20% of girls, 13% of boys borrow and/or share medications – Of the girls • 16% borrowed • 15% shared • 7% shared meds more than 3 times

Diversion (3) • Motivations for sharing drugs & gender – Receiving person ran out of drug: 40% of girls, 27% of boys – Received from family: 33% of girls, 27% of boys Daniel KL et al. Sharing prescription medication among teenage girls: potential danger to unplanned/undiagnosed pregnancies. Pediatrics 2003; 111: 1167 -70.

Definitions • Misuse • Diversion • Dependence

Dependence • Physiological and/or psychological • Compulsive • Use despite negative consequences

Risk Factors - Opioids • Personal Hx of Substance Abuse – Rx drugs > Illegal drugs > Alcohol • Family Hx of Substance Abuse – Rx drugs > Illegal drugs > Alcohol – Equivalent danger of illegal drugs and Et. OH in men

Risk Factors - Opioids • Age between 16 -45 years • History of preadolescent sexual abuse • Psychological/mental health concerns – ADD, OCD, Bipolar disorder, Schizophrenia – Depression

Naturally occurring - Opium - Morphine - Codeine Opium poppy, Papaver somniferum

Opioid Formulations Morphine Hydromorphone Oxycodone Oxymorphone Oral immediate-release: MSIR® Oral extended-release: MS Contin®, Oramorph®, Avinza®, Kadian® Others: solution, suppositories, intravenous Oral immediate-release: Dilaudid® Others: solution, suppositories, intravenous Oral immediate-release: Oxy IR®, Roxicodone Oral extended-release: Oxycontin® Others: solution Oral immediate-release: Opana® Oral extended-release: Opana ER® Others: intravenous
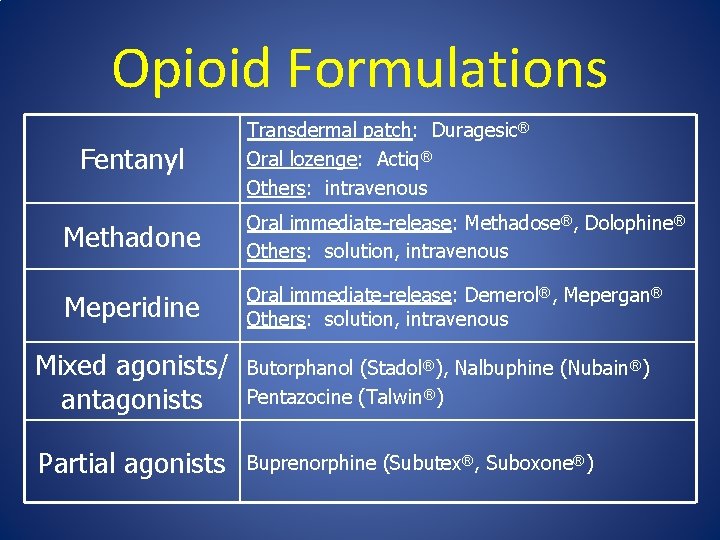

Opioid Formulations Fentanyl Transdermal patch: Duragesic® Oral lozenge: Actiq® Others: intravenous Methadone Oral immediate-release: Methadose®, Dolophine® Others: solution, intravenous Meperidine Oral immediate-release: Demerol®, Mepergan® Others: solution, intravenous Mixed agonists/ antagonists Butorphanol (Stadol®), Nalbuphine (Nubain®) Pentazocine (Talwin®) Partial agonists Buprenorphine (Subutex®, Suboxone®)

Opioid Formulations • Combination Products Hydrocodone Lortab®, Lorcet®, Vicodin®, Norco® Oxycodone Percocet®, Endocet®, Roxicet®, Combunox® Codeine Tylenol #3®, Tylenol #4® Propoxyphene Darvocet®
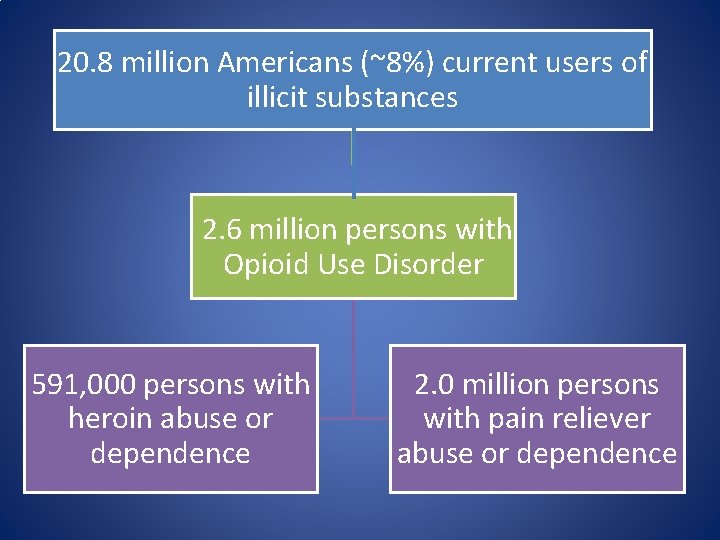
20. 8 million Americans (~8%) current users of illicit substances 2. 6 million persons with Opioid Use Disorder 591, 000 persons with heroin abuse or dependence 2. 0 million persons with pain reliever abuse or dependence
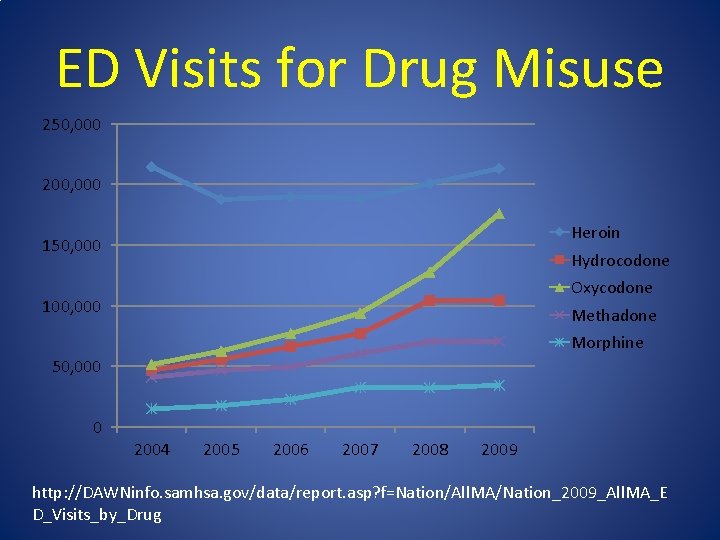
ED Visits for Drug Misuse 250, 000 200, 000 Heroin 150, 000 Hydrocodone Oxycodone 100, 000 Methadone Morphine 50, 000 0 2004 2005 2006 2007 2008 2009 http: //DAWNinfo. samhsa. gov/data/report. asp? f=Nation/All. MA/Nation_2009_All. MA_E D_Visits_by_Drug

DAWN (2009) 1. 2 million ED visits involving nonmedical use of pharmaceutical or dietary supplement Hydrocodone (alone or in combination) 104, 490 ED visits Oxycodone (alone or in combination) 175, 949 ED visits Methadone (alone or in combination) 70, 637 ED visits These 3 medications account for roughly 30% of the ED visits involving nonmedical use of pharmaceuticals/dietary supplements http: //www. nida. nih. gov/infofacts/hospitalvisits. html

CASE – Steve • 62 y Vietnam Era male veteran presents to PCP • PMHx – HTN – Hypercholesterolemia – Gout – Chronic shoulder pain ─ GERD ─ Obesity ─ Chronic back pain • PSHx – Right knee arthroscopy x 2 – Left shoulder – rotator cuff repair

CASE – Steve • PΨHx – Major Depression ─ Generalized Anxiety • Medications – Lisinopril – HCTZ – Allopurinol – Citalopram – Sildenafil PRN ─ Gemfibrozil ─ Simvastatin ─ Omeprazole ─ Trazodone ─ Hydrocodone 10 mg Q 4 H

CASE – Steve • Family Hx – Dad – CAD, MI, Alcohol Use Disorder – Mom – HTN, DM, Dementia – Brother – CAD, Obesity, Alcohol Use Disorder • Substance Use Hx – “Social” alcohol – two 6 pks of beers on weekends – Denies tobacco or illicit substance use

CASE – Steve • Exam (pertinent findings) – Appearance: Older than stated age, but NAD – Gastrointestinal: protuberant abdomen, no TTP, HSM – Musculoskeletal: TTP R shoulder (subscapular region); ↓(? ) ROM with lateral arm raise; no ROM deficits for trunk/lower back; gait WNL – Mental Status: Mild dysphoric mood, anxiety

Strategic Focus • Accurate diagnosis • Appropriate pharmacotherapy • Referral to specialty services 29

Three Common Scenarios… 1. Patient presents with previous or self-diagnosis of Opioid Use Disorder (OUD) 2. Suspicion of OUD a) Self b) Referring provider c) Family 3. Incidental finding of OUD 30

DSM-5 Opioid Use Disorder • • Opioid Use Disorder Opioid Intoxication Opioid Withdrawal Opioid Delirium (Intoxication/Withdrawal) Opioid Depressive Disorder (I/W) Opioid Panic and Anxiety Disorder (W) Opioid Induced Sexual Dysfunction (I/W) Opioid Sleep Disorder (I/W)

DSM-5 Opioid Use Disorder • Tolerance • Hazardous use • Withdrawal • Physical/psychological problems from use • Attempts to cut down • Much time spent using • Social/interpersonal problems from use • Use larger amounts • Activities given up • Neglecting roles • Craving 32

OUD Specifiers • In early remission – none of the criteria met for at least 3 months, but less than 12 months • In sustained remission – none of the criteria met for 12 months or longer – Note: Craving may be present!

OUD Specifiers • On maintenance therapy – Methadone – Buprenorphine – Naltrexone (oral or depot) • In a controlled environment

OUD Caveats • Symptoms of tolerance and withdrawal occurring during appropriate medical treatment are not counted when diagnosing SUD • Opiates are not listed in DSM-5 as causative agent for substance-induced psychosis

Opioid Intoxication • Small, constricted pupils • Slowed breathing • Decreased alertness • Decreased HR, BP • Reports of fatigue

Opioid Withdrawal • Dysphoric (sad) mood • Nausea/vomiting • Muscle aches • Diarrhea • Lacrimation (tearing) or rhinorrhea (runny nose) • Yawning • Pupillary dilation, piloerection (goose flesh), or sweating • Fever • Insomnia 37

Assessment Clinical Opiate Withdrawal Scale • • • Resting heart rate Sweating Restlessness Pupil size (dilation) Bone/Joint aches Runny nose or tearing Score • GI upset • Tremor (outstretched hands) • Yawning • Anxiety • Gooseflesh skin 5 -12 = Mild 13 -24 = Moderate 25 -36 = Moderately Severe More than 36 = Severe

Assessment • “Has a family member ever expressed concern about your Rx opioid use? ” • “Has a physician ever expressed concern about your Rx opioid use? ” • “Have you ever used your Rx opioid to treat other symptoms (e. g. , sleep, irritability, sadness) Adapted from Prescription Drug Use Questionnaire (PDUQ) 39

DSM-5 Opioid Use Disorder • • Opioid Use Disorder Opioid Intoxication Opioid Withdrawal Opioid Delirium (Intoxication/Withdrawal) Opioid Depressive Disorder (I/W) Opioid Panic and Anxiety Disorder (W) Opioid Induced Sexual Dysfunction (I/W) Opioid Sleep Disorder (I/W)

Assessment • Aberrant drug related behaviors – Multiple prescribers – Early prescription refills – Dose/frequency escalation – ER visits for analgesics – Use of alcohol/psychoactive drugs – Taking a family member’s medication • Personal history of opioid detox 41

Assessment • PMP AWARx. E – Prescription drug monitoring program through Texas State Board of Pharmacy – www. pharmacy. texas. gov/PMP • Urine drug screening 42

CASE – Steve • You are concerned that Steve may have OUD, but decide a short-term prescription for opioids is appropriate while laboratory studies and imaging are obtained – You decrease from Hydrocodone 10 mg Q 4 H PRN to Hydrocodone 10 mg Q 6 H PRN

CASE – Steve • Lab WNL • UDS +opiates; negative MJ, bzdp, coc • Imaging – Previous right shoulder procedure – Mild osseous changes in lower spine

CASE – Steve • Visit #2 – Reports ↓ hydrocodone ↑ shoulder/lower back pain – Diminished activity, functioning – ↑ Depression/anxiety

Strategic Focus • Accurate diagnosis • Appropriate pharmacotherapy • Referral to specialty services 46
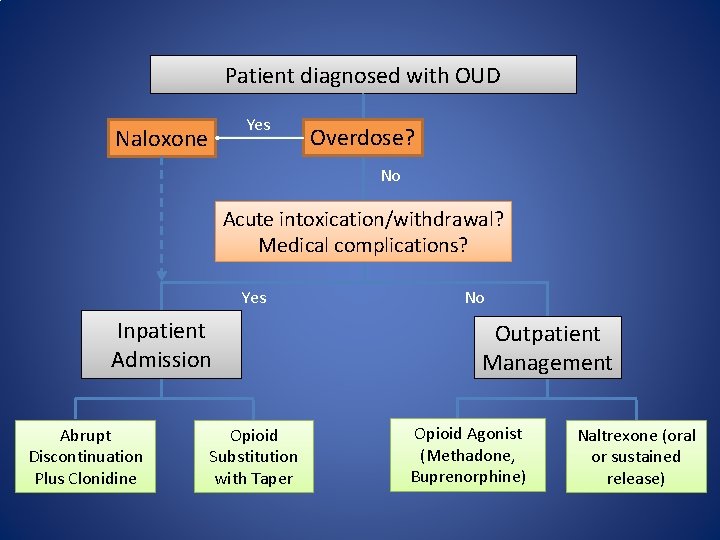
Patient diagnosed with OUD Yes Naloxone Overdose? No Acute intoxication/withdrawal? Medical complications? Yes Inpatient Admission Abrupt Discontinuation Plus Clonidine Opioid Substitution with Taper No Outpatient Management Opioid Agonist (Methadone, Buprenorphine) Naltrexone (oral or sustained release)
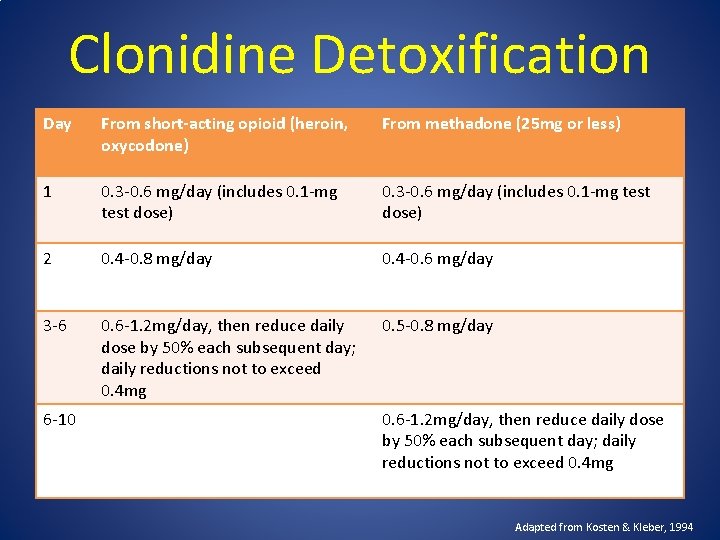
Clonidine Detoxification Day From short-acting opioid (heroin, oxycodone) From methadone (25 mg or less) 1 0. 3 -0. 6 mg/day (includes 0. 1 -mg test dose) 2 0. 4 -0. 8 mg/day 0. 4 -0. 6 mg/day 3 -6 0. 6 -1. 2 mg/day, then reduce daily dose by 50% each subsequent day; daily reductions not to exceed 0. 4 mg 0. 5 -0. 8 mg/day 6 -10 0. 6 -1. 2 mg/day, then reduce daily dose by 50% each subsequent day; daily reductions not to exceed 0. 4 mg Adapted from Kosten & Kleber, 1994

Clonidine Most effective in suppressing autonomic signs of withdrawal, less effective for subjective symptoms Lethargy, restlessness, insomnia, craving are likely to persist Adjuvant therapy may be needed • NSAIDs (for myalgia) • Trazodone (for insomnia) • Antiemetics (for GI distress) • Propranolol (for restlessness)

Withdrawal Management (1) • Symptom-triggered clonidine Rx – For COWS > 8, give 0. 1 -0. 2 mg clonidine – On day 1, target dose of 0. 3 -0. 6 mg – May to 0. 6 -1. 2 mg/day, as necessary – Once stabilized, reduce daily dose by 50% per day 50
• Clonidine Opioid Withdrawal • Agonist Long term • Antagonist Rx of OUD • Agonist 51

Withdrawal Management (2) Use opioid agonist to symptoms • Methadone – Up to 30 mg/day – 10 -20% every 1 -2 days over 2 -3 weeks – Better than α 2 -adrenergic agonist based Rx • Buprenorphine – Up to 8 mg/day – ↓ by 2 mg every 1 -2 days over 7 -10 days 52
• Clonidine Opioid Withdrawal • Agonist Long term • Antagonist Rx of OUD • Agonist 53

Long-term Rx of OUD • Opioid Antagonist Therapy – Intramuscular naltrexone (Vivitrol) • Administer every 30 days • Prevents opioid high • Low compliance – No other FDA-approved medications 54

Long-term Rx of OUD (2) • Methadone maintenance treatment (MMT) – Taken daily by mouth – Obtained through federally-regulated program – Optimal dose varies (target = 80 mg/day) -- Must ↑ dose slowly to avoid OD 55

MMT Drawbacks • Overdose common in early treatment • Cannot be prescribed from general practice • Strict government control and paperwork • Stigma of daily clinic attendance 56

Office-Based Buprenorphine • Taken daily, sublingually • Rx in offices of physicians with special training • Individual dose varies (target = 16 -24 mg/day) • Daily visits not necessary Alcohol Medical Scholars Program 57

Buprenorphine Pharmacology • Partial agonist at μ-opioid receptor • Slow dissociation from receptor • Half-life = 24 -36 hrs • Metabolizes quickly, if give orally • So Rx is sublingual or buccal Alcohol Medical Scholars Program 58

Buprenorphine Pharmacology (2) • Clinical impact – Less subjective euphoria than methadone – Long-lasting clinical action – Partially blocks intoxication – Reduced overdose risk Alcohol Medical Scholars Program 59

Formulations • Buprenorphine alone (Subutex) • Buprenorphine + naloxone (Suboxone) – Naloxone = antagonist – risk of diversion and IV misuse – Combined in 4 mg bup: 1 mg naloxone • Combo in sublingual or buccal film Alcohol Medical Scholars Program 60

More Buprenorphine Info • Side effects – Neuro: Sedation, dizziness, headache – GI: Constipation, nausea/vomiting – Respiratory depression • Availability and cost – Prescribed by MDs with special training – Reimbursed by Medicaid, health insurances ─ But costs more than methadone Alcohol Medical Scholars Program 61

Buprenorphine Treatment • Initiation – Goal: avoid precipitated withdrawal & OD – Patient stops opioid misuse 12 -36 hrs prior – Patient demonstrates early withdrawal • COWS rating > 8 Alcohol Medical Scholars Program 62


CASE – Alfred • 57 y Vietnam Era male veteran presents to PCP • PMHx – HTN ─ Migraine HAs – Chronic pain ─ Gastritis – Gastric neoplasm (benign) • PSHx – Tonsillectomy – childhood – Multiple EGDs

CASE – Alfred • PΨHx – Major Depression • Medications – Lisinopril ─ Omeprazole – ASA ─ Sumatriptan PRN – Loratadine ─ Alprazolam (Xanax) 2 mg TID – Hydrocodone 5 mg Q 6 H PRN

CASE – Alfred • Family Hx – Dad – CVA, DM – Mom – Depression, HTN, obesity • Substance Use Hx – Alcohol – 3 -4 12 oz. beers/session ~1 -2 x/week – Occasional marijuana (<1 joint/use) – H/o cocaine use in 20 s and 30 s

CASE – Alfred • Vague report – “Do I have to answer that? ” – 6 -year history of Alprazolam use – Obtained from both providers and illicit sources – Anxious between dosages – Insomnia if he runs out

CASE – Alfred • Exam (pertinent findings) – Appearance: Older than stated age, fidgety – Gastrointestinal: protuberant abdomen mild TTP, no HSM – Mental Status: Mildly dysphoric, anxious appearing and irritable

BZD Formulations Diazepam Oral immediate-release: Valium®, Diastat® Others: intramuscular, intravenous, suppository Alprazolam Oral immediate-release: Xanax® Oral extended-release: Xanax-XR® Others: solution Clonazepam Oral: Klonopin®, Klonopin wafer® Others: orally disintegrating tablet Lorazepam Oral immediate-release: Ativan® Others: intramuscular, intravenous, sublingual, solution

Indications (FDA) • Alcohol withdrawal • Muscle relaxant • Insomnia • Antiepileptic • Anxiety disorders • Anesthesia adjunct • Panic disorder

Clinical use (non FDA) • Catatonia • Agitation • Abnormal movements • Tourette’s syndrome • Delirium

Epidemiology (1) • 2011: Alprazolam, Lorazepam, Diazepam were the most common prescribed • 2011: 47. 8 million Alprazolam prescriptions written (137 million Hydrocodone Rx) • 2. 3% of adults in US report nonmedical use of sedatives – 10% of those meet criteria for abuse or dependence From SAMHSA NSDUH (2012), DAWN (2010)

Epidemiology (2) • 2011: 345, 528 ER visits related non illicit drugs – 25% related with non medical use of BZD • • 10% Alprazolam 5% Clonazepam 3. 5% Lorazepam 2% Diazepam • 41, 257 (3. 3%) ER visits related non medical use of SSRIs From SAMHSA NSDUH (2012), DAWN (2011)

BZD & Mental Health (1) • 30% of psychiatry pts receive BZD – Affective disorders – Long duration of illness – High utilizers of psychiatric services

BZD & Mental Health (2) • High risk patients – Personal AUD history (15 -20% misuse BZD) – Family h/o of alcohol use disorder – Personal h/o of opioid use disorder – Methadone maintenance (47%)

BZD and Suicide • 2009: 2 nd most common class of drug used in suicide attempt • Alprazolam most commonly used BZD in SA (12%) • Clonazepam second most common (8%) • Zolpidem third most common (6%) From SAMHA 2011.


CASE – Alfred • You are concerned about Alfred’s combined use of BZD and opiates as well as his patterns of BZD use. – You decide a taper off the BZD is appropriate

Assessment “Legitimate” Prescription BZD Use Disorder • GOAL: Treat underlying illness • GOAL: Confirm SUD dx • FOCUS: Assess risk of SUD • FOCUS: Safe discontinuation

Clinical Approach (1) • Identify risk factors – Co-occurring SUD or psychiatric d/o – Highest abuse: diazepam, lorazepam, alprazolam – Prior BZD treatment > 8 wks

Clinical Approach (1) • Minimize potential harms – Aggressive short-term treatment • Use high dose over few weeks while SSRI/SNRI take effect – Short-term treatment • PRN versus continuous schedule – Drug holiday implementation • Intermittent use of medication • Only during high demand situations

Clinical Approach (2) • Recognize TYPES of Bz. UD • Underlying (anxiety) disorder; tolerant • Recreational user • Complicated – High-dose – Poly-BZD use

Clinical Approach (2) • DSM V Criteria for SUD • Aberrant drug related behaviors – Early refills, ER visits – Multiple providers – Taking the medication as prescribed – UDS + for illicit substances
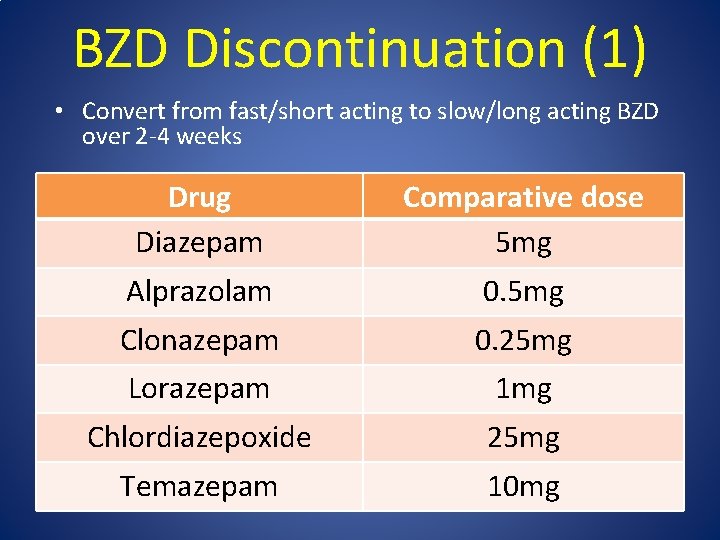
BZD Discontinuation (1) • Convert from fast/short acting to slow/long acting BZD over 2 -4 weeks Drug Diazepam Comparative dose 5 mg Alprazolam 0. 5 mg Clonazepam 0. 25 mg Lorazepam 1 mg Chlordiazepoxide 25 mg Temazepam 10 mg

BZD Discontinuation (2) • Cross taper with alternative agent – GABAergic • Buspirone • Valproate** • Carbamazepine • Gabapentin • Pregabalin – Serotonergic • TCA (Imipramine) **indicates improved rates of long-term abstinence

BZD Discontinuation (3) • Cross taper with medication for anxiety reduction – Hydroxyzine – Quetiapine – Trazodone** • Inpatient management – Flumazenil
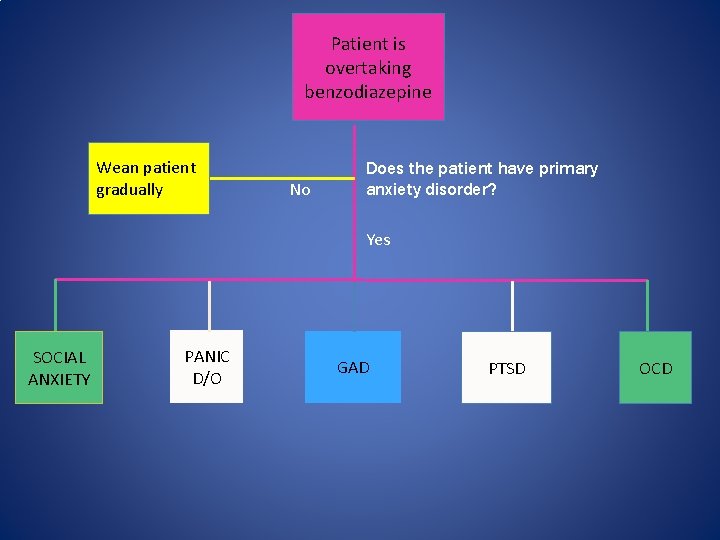
Patient is overtaking benzodiazepine Wean patient gradually No Does the patient have primary anxiety disorder? Yes SOCIAL ANXIETY PANIC D/O GAD PTSD OCD
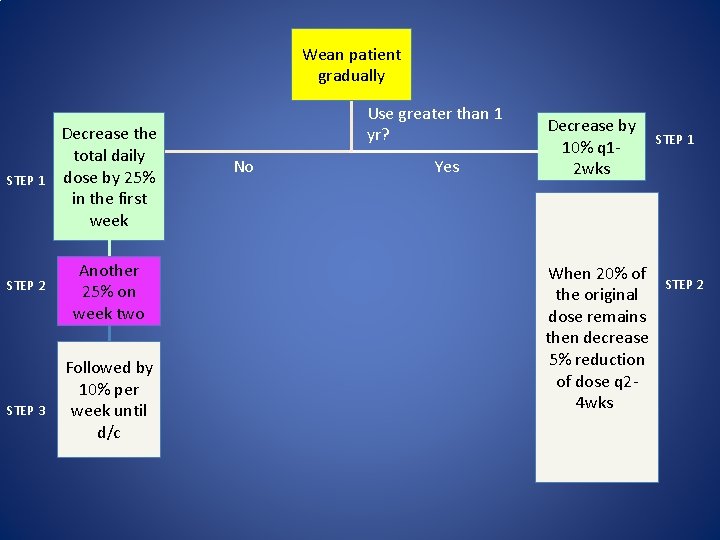
Wean patient gradually STEP 1 Decrease the total daily dose by 25% in the first week STEP 2 Another 25% on week two STEP 3 Followed by 10% per week until d/c Use greater than 1 yr? No Yes Decrease by 10% q 12 wks When 20% of the original dose remains then decrease 5% reduction of dose q 24 wks. STEP 1 STEP 2
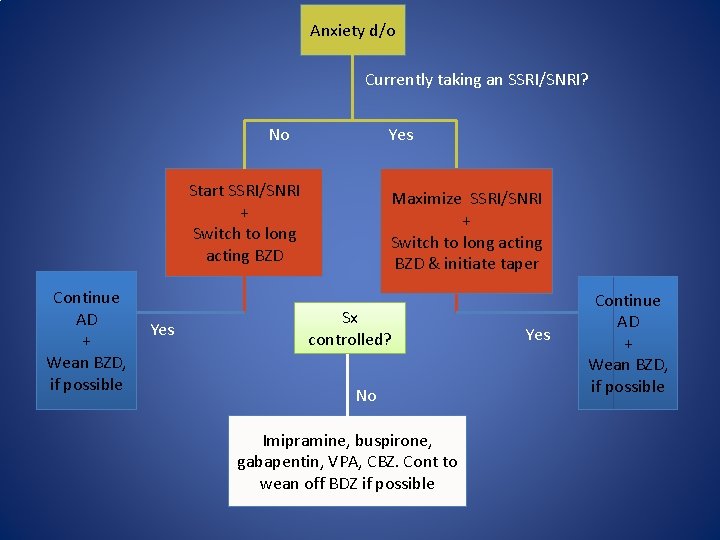
Anxiety d/o Currently taking an SSRI/SNRI? No Yes Start SSRI/SNRI + Switch to long acting BZD Continue AD + Wean BZD, if possible Yes Maximize SSRI/SNRI + Switch to long acting BZD & initiate taper Sx controlled? No Imipramine, buspirone, gabapentin, VPA, CBZ. Cont to wean off BDZ if possible Yes Continue AD + Wean BZD, if possible

Take Home Points • Risk Factors for Opioid Misuse – Personal or family h/o substance use – Age (16 -45 y) – Psychiatric conditions (such as MDD, OCD, SCZ) – Preadolescent sexual abuse (women)

Take Home Points • Risk Factors for BZD Use Disorder – Personal h/o substance use – Long term BZD use – High dose BZD use – Concomitant opioid use (esp. Methadone)

Take Home Points • Screening and assessment should include urine drug screening • Initiation of taper should take into consideration length of time patient has been on medication and may require patience
- Slides: 92