Preoperative Evaluation of the Bariatric Surgery Patient Eric

Preoperative Evaluation of the Bariatric Surgery Patient Eric I. Rosenberg, MD, MSPH, FACP

Case #1 “. . . evaluate for metabolic disorder”

“Super” Morbid Obesity • 53 year-old woman • 399 lbs, 4’ 10”, BMI 83. 3 • Bariatric surgeon notes central obesity, abdominal bruises, buffalo hump

History PMHx: Catatonic schizophrenia Bipolar Disorder PGyn. Hx: G 2 P 2 Meds: Fluoxetine, Risperidone Allergies: Ø FH: Ø SH: Disabled; some Et. OH ROS: Venous stasis, cellulitis

Exam • BP 147/73, P 83 • Flat affect • Moon facies • Buffalo hump • No muscle wasting, no striae, no bruising
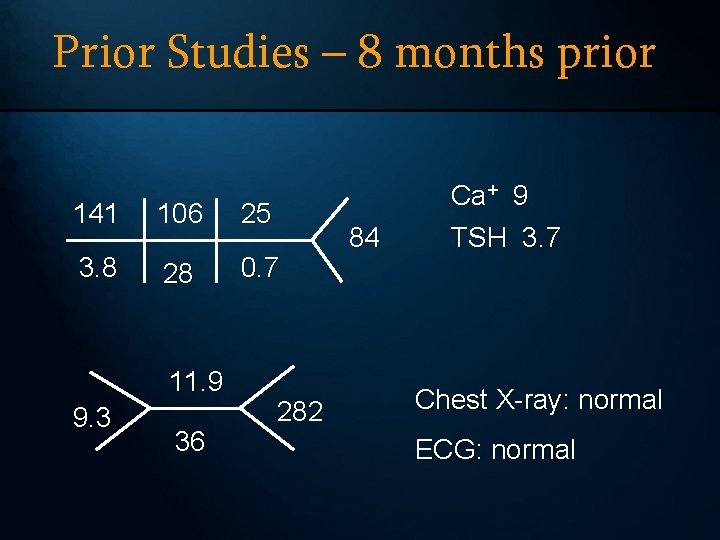
Prior Studies – 8 months prior 141 106 25 3. 8 28 0. 7 11. 9 9. 3 36 282 84 Ca+ 9 TSH 3. 7 Chest X-ray: normal ECG: normal

Differential Dx for Severe Obesity • Dietary • Social/Behavioral • Inactivity • Iatrogenic • Neuro-endocrine

What would you do next?

Key Issues for Bariatric Pre-Operative Evaluation • When should you suspect a non-lifestyle associated etiology for morbid obesity? • What is the most efficient diagnostic strategy to evaluate for a neuro-hormonal cause? • What are the most important medical risks to this patient if she undergoes bariatric surgery?

Key Issues for Bariatric Pre-Operative Evaluation • When should you suspect a non-lifestyle associated etiology for morbid obesity? • What is the most efficient diagnostic strategy to evaluate for a neuro-hormonal cause? • What are the most important medical risks to this patient if she undergoes bariatric surgery?

Severe Obesity = BMI 40 NHLBI 2000
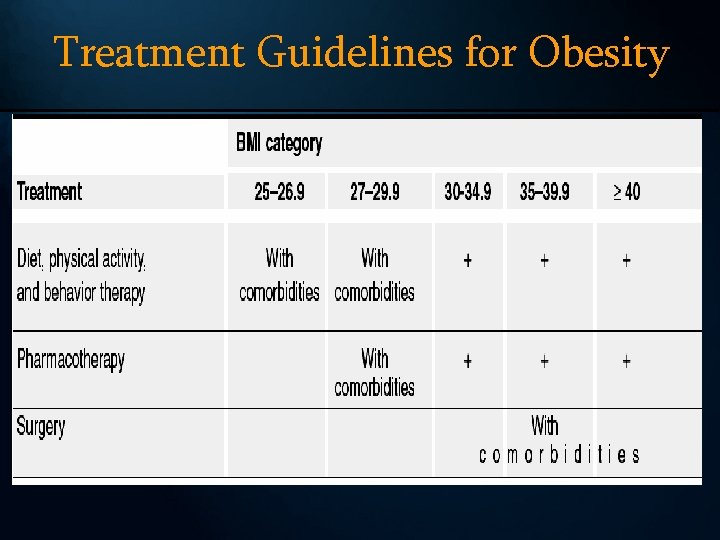
Treatment Guidelines for Obesity
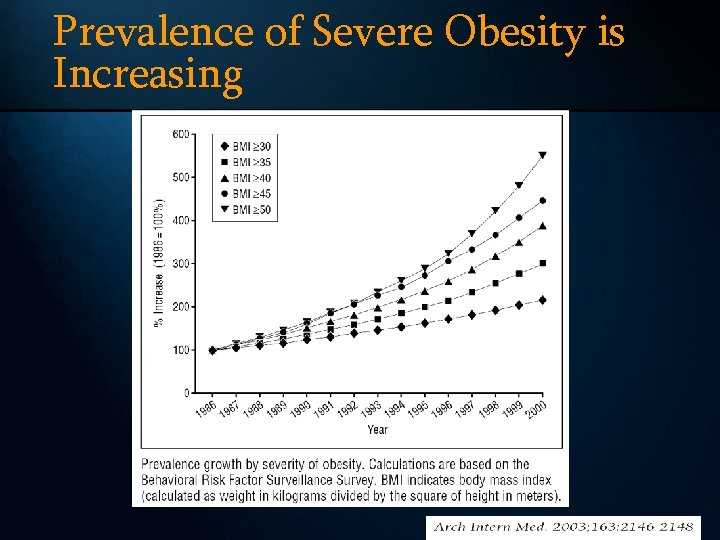
Prevalence of Severe Obesity is Increasing
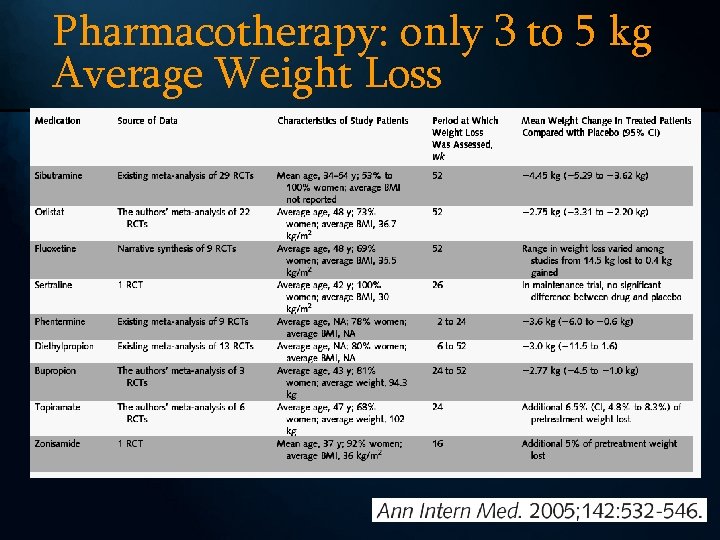
Pharmacotherapy: only 3 to 5 kg Average Weight Loss
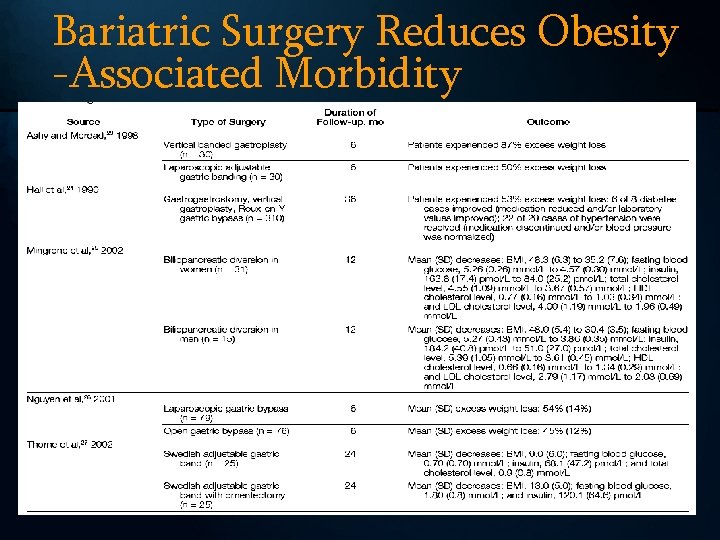
Bariatric Surgery Reduces Obesity -Associated Morbidity

Surgery May Improve Longevity

“Ideal” Bariatric Surgery Candidates Cleve Clin J Med 2006; 73(11).

HMO/Medicare Payment for Bariatric Surgery • BMI > 40 for 2 to 5 years – BMI > 35 if CAD, DM, HTN, sleep apnea • Repeated failures of supervised weight loss (6 months duration) • Letter of medical necessity • “Treatable metabolic causes ruled out” – “Thyroid panel” – “adrenal disorders”
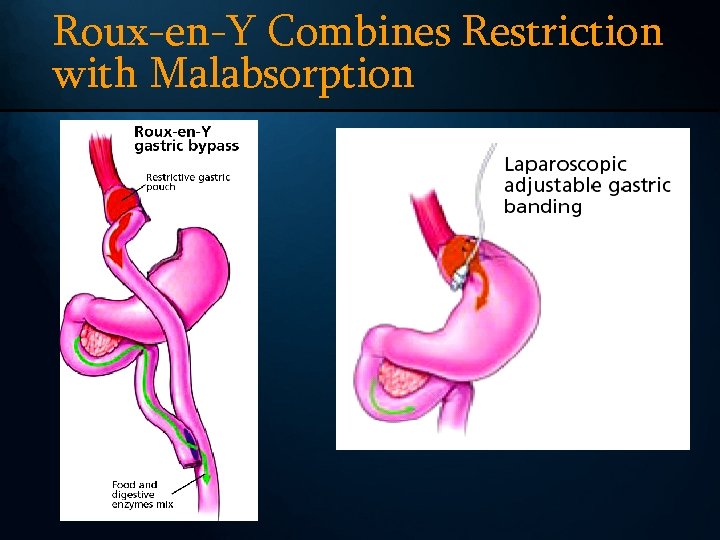
Roux-en-Y Combines Restriction with Malabsorption

Acute Complication Rates for Bariatric Surgery

Long Term Complications • Anastomotic Stricture • Marginal ulcers • Bowel obstruction • Cholelithiasis • Nutritional Deficiencies

Nutritional Deficiencies are Common after Malabsorptive Procedures • Iron • Vitamin B-12 • Calcium • Vitamin D Multitamins will not adequately treat iron and B-12 deficiencies

Key Issues for Bariatric Pre-Operative Evaluation • When should you suspect a non-lifestyle associated etiology for morbid obesity? • What is the most efficient diagnostic strategy to evaluate for a neuro-hormonal cause? • What are the most important medical risks to this patient if she undergoes bariatric surgery?

Possible Metabolic Causes of Obesity in Our Patient • Hypothyroidism • Hypothalamic condition • Cushing’s Syndrome • Polycystic Ovarian Syndrome • Pseudohypoparathyroidism

This was my “non-clearance”… IMPRESSION: A 53 -year-old white female without any history of cardiopulmonary disease. Given her lifelong history of morbid obesity in association with and lack of history of diabetes and hypertension, I think it is unlikely that she has Cushing disease or other underlying metabolic disorder…. I think she is at high risk for perioperative delirium given her significant psychiatric history. I think that the surgical team will need to be cautious with administration of narcotics or hypnotics/sedatives.

But Could She Have Cushing’s Syndrome? • Physical exam suggestive of hypercortisolism – From severe obesity? – From psychiatric distress? – From alcoholism? • No history of glucocorticoid use

Prevalence of Clinical Features of Cushing’s Syndrome • Obesity (90%) • Neuropsychiatric (85%) • Hirsutism (75%) • Bruising (35%) • Hypertension (85%) • Diabetes (20%) Greenspan’s Basic and Clinical Endocrinology, 8 th Edition.

Validity of Standard Screening Tests for Cushing’s Syndrome • Elevated midnight serum cortisol – 96 -100% sensitivity, 100% specificity • Overnight Dexamethasone Suppression – 90 -100% sensitivity, 40% specificity • Elevated 24 -hour urinary cortisol excretion – 100% sensitivity, 98% specificity
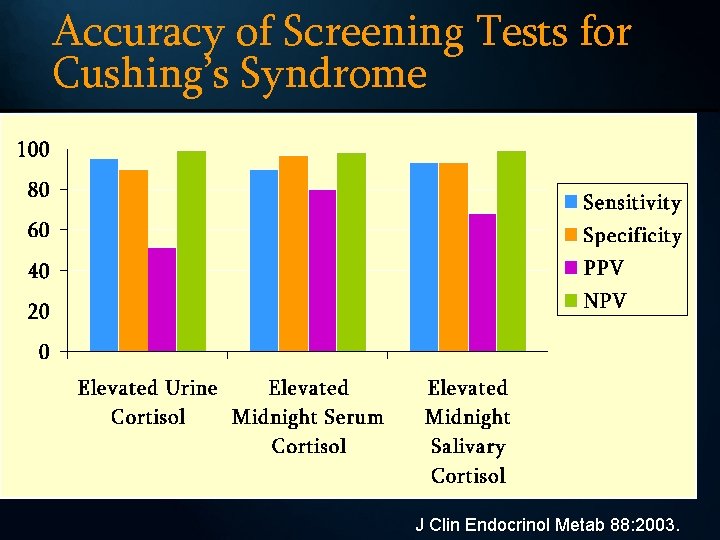
Accuracy of Screening Tests for Cushing’s Syndrome J Clin Endocrinol Metab 88: 2003.

My Clinical Suspicion was High Enough to Screen for Cushing’s RECOMMENDATIONS: 1) “I ordered a midnight salivary cortisol test which is very sensitive and has high negative predictive value. ”

Recommended Preoperative Testing for Bariatric Surgery • Hematocrit • Baseline Iron, B-12 levels • TSH • A 1 c (if diabetic control in doubt) • Creatinine if appropriate • Baseline ECG and other cardiopulmonary testing if suspect undiagnosed disease

8 Months later… • Test #1: 0. 155 ug/d. L (normal <0. 112) • Test #2: quantity not sufficient • Test #3: quantity not sufficient • Test #4: quantity not sufficient • Endocrine referral

Dexamethasone Suppression Test Rules-Out Cushing’s • 1 mg Dexamethasone at 11 PM to 12 AM • 8 AM Cortisol level – 1 mcg/d. L • <8% of patients with Cushing’s show suppression to < 2 mcg/d. L • 100% sensitivity if suppress to less than 1. 2 mcg/d. L

Take-Home Points • Severe Obesity is increasingly prevalent • Bariatric Surgery will increase in popularity • Prospective Bariatric Surgery Patients need careful risk assessment and long-term followup for complications • Consider appropriate screening for secondary causes if patient presents with characteristic history, signs
- Slides: 34