Preoperative Evaluation and Clearance for Surgery Joshua Steinberg

Preoperative Evaluation and Clearance for Surgery Joshua Steinberg MD Wilson Family Medicine Residency Binghamton, New York
Your pt, 72 y. o. Symptomatic gallstones Going for lap chole

Special Kind of Visit Family Physician usually serves just one person at a visit At a Preoperative Evaluation visit, we serve three parties

Whom We Serve

Goal of Pre-Op Eval At VERY LEAST, what does surgeon want to hear from you? CNY Cardiology 1234 Main St. Wherever, NY 67890 Dear Bill the Orthopedist, I had the pleasure of seeing Mrs. Mabel Jones at your kind request. You may proceed to surgery. Yours Truly, Fred the Cardiologist

Let’s do better than minimum! What should we do at the preoperative evaluation of a patient? What would the surgeon and anesthesiologist like us to do? How could we help a patient endure the challenges of surgery and recovery? How could we help surgeon & anesthesiologist give good care?

Organize the Activities Report medical issues 1 Optimize medical issues 2 Consider cardiac status 3 Suggest/implement periop interventions 4

Report medical issues Full History 1 HPI: “asked by Dr. Aronis to evaluate pt prior to cholecystectomy for gallstones” Past Medical History: everything Past Surgical Hx (note problems bleeding or anesthesia) Allergies & Reactions, Meds Fam. Hx (note problems anesthesia, bleeding) Soc. Hx: Et. OH, tobacco, drugs ROS: cardiac, those pertinent to PMHx, functional capacity

Report medical issues Physical Exam 1 Vitals Cardiocirculatory Pulmonary Abdominal anything else you think is pertinent and helpful (neuro exam, mental status exam, skin exam, etc. )

Report medical issues Assessment & Plan 1 10/27/11, 8: 15 am Samantha Smith S: Asked by Dr. Aronis to evaluate pt with cholecystitis prior to lap chole. PMHx, PSHx, All, Meds, Soc. Hx, Fam. Hx, ROS etc. O: vitals, lungs, heart, abd, ext, etc. A/P: 1. Preop clearance: clear to proceed to surgery (more later) 2. Asthma: mild, stable, continue Flovent MDI 3. Chronic Renal Insufficiency: creat stable at 1. 5 baseline 4. Anemia: chronic, from malabsorption after bariatric surgery, recommend check Hct post-op 5. Please note anaphylactic Cefazolin allergy signed, JP Intern

Optimize medical issues Not so rosy 2 after nausea and vomiting of cholecystitis, dehydrated, creat bumped to 2. 1 asthma not controlled HTN uncontrolled Diabetes uncontrolled COPD or CHF exacerbated

Optimize medical issues Not so rosy 2 10/27/11, 8: 15 am Samantha Smith S: Asked by Dr. Aronis to evaluate pt with cholecystitis prior to lap chole. PMHx, PSHx, All, Meds, Soc. Hx, Fam. Hx, ROS O: vitals, lungs, heart, abd, ext, etc. A/P: 1. Preop clearance: pending items 2 -4, I anticipate pt will be clear to proceed to surgery 2. Dehydration: giving 2 L NS 3. Chronic Renal Insufficiency: recheck after IVF, aim to get back to baseline creat 1. 5 4. HTN: SBP 197/98 unsafe for surgery, will resume Amlodipine and Coreg 5. Severe O 2 dept COPD: it’s awful, horrendous, 115. 3 pack-year smoking hx, but optimized on meds and at baseline signed, JP Intern

Check for sub-optimal stuff Optimize medical issues 2 All kinds of labs & workup you could do preop checking if anything is suboptimal BUT, every guideline recognizes that the yield of useful results that influence care is VANISHINGLY LOW. Over -testing is rampant n n n many preop tests already ordered by surgeon if you choose tests, order only ones indicated avoid cost, risk of false positives, unnecessary delay surgery K+ or BMP: certainly digoxin, diuretics, ACE/ARB, ok for others CBC: anything suggests anemia or blood loss

Check for sub-optimal stuff Optimize medical issues 2 CXR: only for s/sx new or unstable cardiopulm disease, 4 organizations beg you to stop routine CXR Coags: known hx coag d/o, hx suggests new coag d/o, on anticoagulant, needs anticoagulant post-op, otherwise don’t do UA: urologic surgery, prosthetic implants, otherwise don’t do EKG: most patients (ICSI vs ACC) n any cardiovasc risk factors, age 65+, any cardiovascular s/sx, surgery of intermediate or high risk anything else you can justify, i. e. renal fxn for known/suspected kidney disease, LFT’s for known/suspected liver disease, HCG, etc. Never do any testing before cataract surgery

Consider cardiac status Cardiac Eval Algorithm 3 American College of Cardiology (ACC) guideline for stepwise consideration of cardiac status revised 1997, 2002, 2007, 2014 always gets easier since evidence shows that pts simply do well!
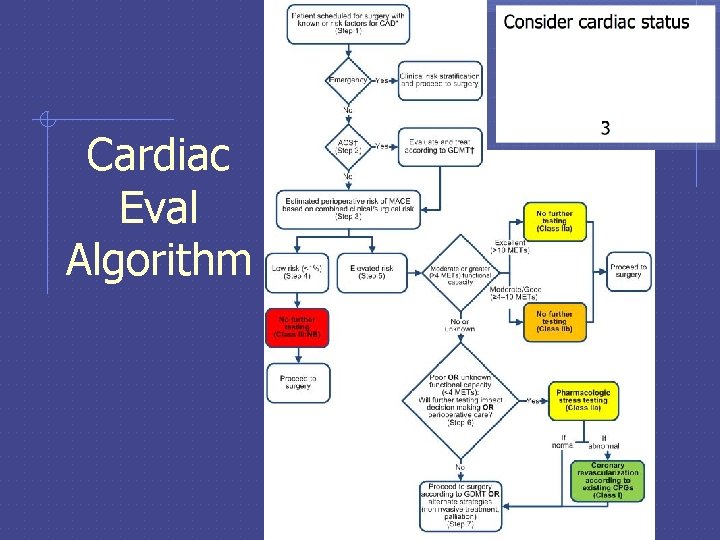
Cardiac Eval Algorithm Consider cardiac status 3
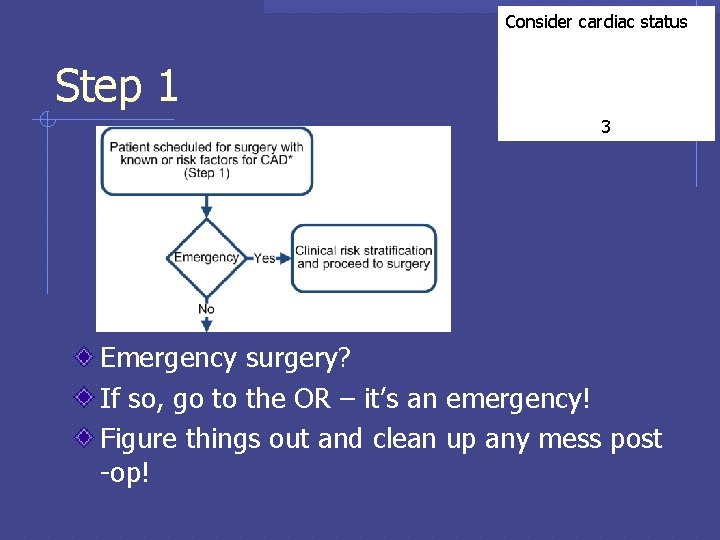
Consider cardiac status Step 1 3 Emergency surgery? If so, go to the OR – it’s an emergency! Figure things out and clean up any mess post -op!

Consider cardiac status Step 2 3 Acute Coronary Syndrome current or recent? n clinical syndromes of acute coronary ischemia including unstable angina, STEMI, NSTEMI If so, evaluate, treat, recover, optimize, and then reconsider OR
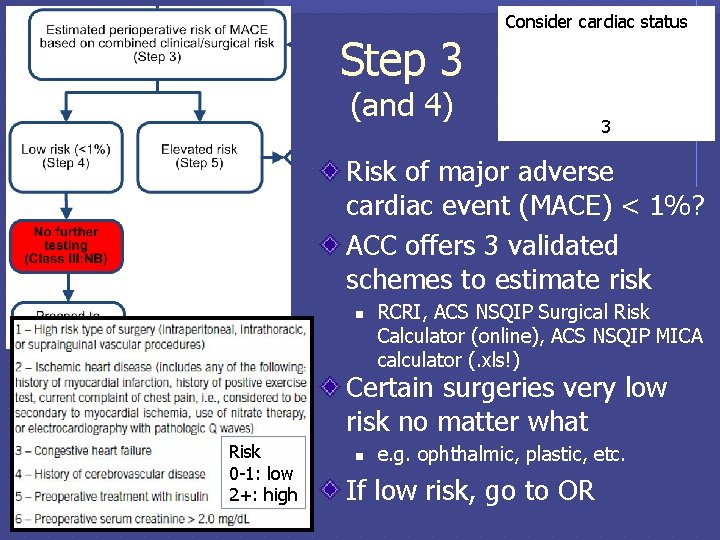
Step 3 Consider cardiac status (and 4) 3 Risk of major adverse cardiac event (MACE) < 1%? ACC offers 3 validated schemes to estimate risk n RCRI, ACS NSQIP Surgical Risk Calculator (online), ACS NSQIP MICA calculator (. xls!) Certain surgeries very low risk no matter what Risk 0 -1: low 2+: high n e. g. ophthalmic, plastic, etc. If low risk, go to OR
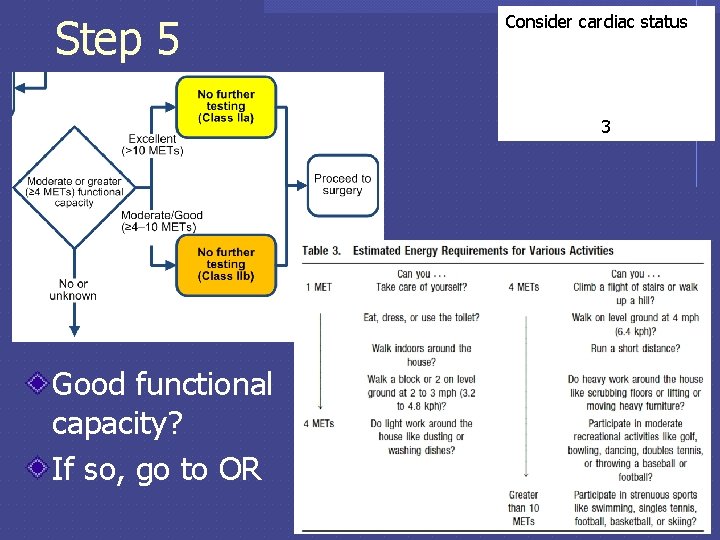
Step 5 Consider cardiac status 3 Good functional capacity? If so, go to OR
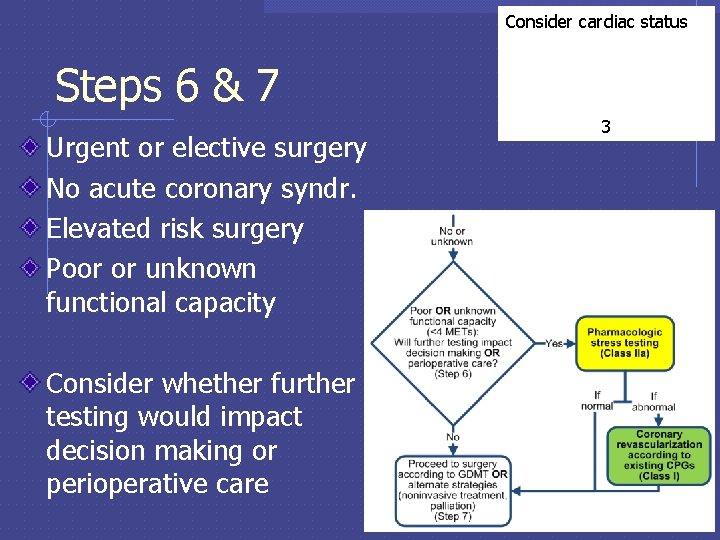
Consider cardiac status Steps 6 & 7 Urgent or elective surgery No acute coronary syndr. Elevated risk surgery Poor or unknown functional capacity Consider whether further testing would impact decision making or perioperative care 3
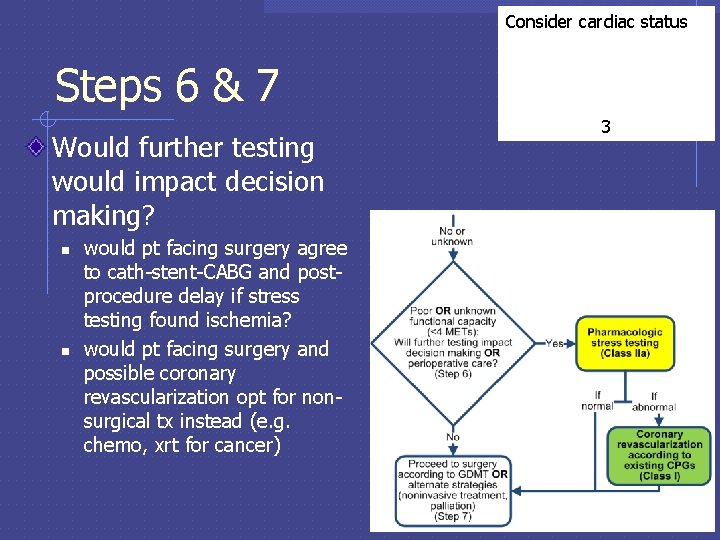
Consider cardiac status Steps 6 & 7 Would further testing would impact decision making? n n would pt facing surgery agree to cath-stent-CABG and postprocedure delay if stress testing found ischemia? would pt facing surgery and possible coronary revascularization opt for nonsurgical tx instead (e. g. chemo, xrt for cancer) 3

Consider cardiac status Cardiac Eval Algorithm 3 10/27/11, 8: 15 am Samantha Smith S: Asked by Dr. Aronis to evaluate pt with cholecystitis prior to lap chole. PMHx, PSHx, All, Meds, Soc. Hx, Fam. Hx ROS: no cardiac sx, good functional capacity O: vitals, lungs, heart, abd, ext, etc. A/P: 1. Preop clearance: according to 2014 ACC guideline, pt is clear to proceed to surgery 2. Asthma: mild, stable, continue Flovent MDI 3. Chronic Renal Insufficiency: creat stable at 1. 5 baseline 4. Anemia: chronic, from malabsorption after bariatric surgery, recommend check Hct post-op 5. Please note anaphylactic Cefazolin allergy signed, JP Intern

Suggest/implement periop interventions Periop interventions 4 Lots of useful things you could do before and after surgery n n n smoking cessation alcohol cessation/detox get the Foley catheter out early mainly medication management n n beta blockers insulin warfarin & bridging heparins aspirin & plavix

Suggest/implement periop interventions Beta-blockers 4 if on one, stay on it add beta-blocker periop? numerous trials show reduced MI’s for pts with significant MI risk then one showing MI benefit, CVA harm n Metoprolol high dose and no titration ACC has softened recommendation but still says offer beta-blockade for higher risk cardiovascular pts with higher risk surgeries and take time to titrate

Suggest/implement periop interventions Diabetes & Insulin 4 Mild hyperglycemia is preferable to hypoglycemia Don’t take oral hypoglycemics on day of procedure Don’t take short-acting insulin morning of procedure Long-acting or intermediate insulin may be used to cover basal insulin needs; 50%-100% of usual dose is often reasonable Insulin pumps should be continued but only to provide basal insulin coverage Details of insulin recommendations influenced by insulin sensitivity of patient, timing of procedure, length of procedure, and how long patient will need to be NPO following the procedure.

Warfarin & bridging Heparins Suggest/implement periop interventions 4 WARFARIN ---> // day preop 5 ? ? ? bridging Heparin ? ? ? ---> // 4 3 2 1 WARFARIN +/- Heparin ---> surgery 1 2 day postop ACCP guideline recommends you handle this based upon risk of thromboembolism during non-anticoagulated time Basically stop Warfarin 5 days before surgery, resume when surgical wounds hemostatic and clinical situation favorable Depending on level of risk of thromboembolic event, cover pt with a Heparin product up until time of surgery and as soon after surgery as pt deemed safe for anticoagulation

Suggest/implement periop interventions Aspirin 4 ACC points out that evidence does not clearly support benefit of Aspirin to prevent peri/post-operative MI’s (in non post-stent pts). Aspirin causes more bleeding during surgery. Thus much weaker recommendation on continuing Aspirin during surgery for high ischemia-risk pts and much more permission to stop aspirin in anyone Should be discussed and negotiated with the surgeon Strong recommendation to continue Aspirin if pt was on Aspirin-Clopidogrel combination (“dual antiplatelet therapy” or DAPT) and both cannot be continued during surgery when highly necessary…

Suggest/implement periop interventions Aspirin & Clopidogrel or the other P 2 Y 12 inhibitors 4 Most patients on Clopidogrel are on it with Aspirin (DAPT) in the 12 months after stent Stent thrombosis rates super-high 1 st 4 -6 wks, somewhat high therafter, especially for DES Try not to do surgery 4 -6 wks after stent at all and not for 365 days after DES If must operate, try to go to OR on DAPT, and if DAPT too dangerous, try to go to OR on Aspirin alone, restarting Clopidogrel ASAP after This stuff should be discussed and negotiated with the surgeon

Periop Med Mgmt Suggest/implement periop interventions 4 10/27/11, 8: 15 am Samantha Smith S: Asked by Dr. Aronis to evaluate pt with cholecystitis prior to lap chole. PMHx, PSHx, All, Meds, Soc. Hx, Fam. Hx ROS: no cardiac sx, good functional capacity O: vitals, lungs, heart, abd, ext, preop labs, EKG A/P: 1. Preop clearance: according to 2014 ACC guideline, pt is clear to proceed to surgery 2. A-fib/Anticoag: as pt is low risk, will stop Coumadin 5 days before surgery and recommend resume when hemostasis achieved 3. DM II: stop Humalog & Metformin, give half dose Lantus night before surgery, resume each when taking PO post-op 4. Please note anaphylactic Cefazolin allergy signed, JP Intern

Agenda for Preop Eval Report medical issues 1 Optimize medical issues 2 Consider cardiac status 3 Suggest/implement periop interventions 4

Preoperative Evaluation So you’ve got it all memorized now? Big Important Med School 1234 Main St. Wherever, NY 67890 Dear Dr. Steinberg, That’s a crazy amount o’ stuff to keep straight! Yours Truly, Bob the Med Student

There’s an App for That…
- Slides: 33