Prenatal Screening Developed by Dr June Carroll Dr

Prenatal Screening Developed by Dr. June Carroll, Dr. Judith Allanson, Ms. Shawna Morrison and Ms. Safa Yusuf Last updated June 2018

Disclaimer • This presentation is for educational purposes only and should not be used as a substitute for clinical judgement. GEC-KO aims to aid the practicing clinician by providing informed opinions regarding genetic services that have been developed in a rigorous and evidence-based manner. Physicians must use their own clinical judgement in addition to published articles and the information presented herein. GEC-KO assumes no responsibility or liability resulting from the use of information contained herein.

Objectives • Following this session the learner will be able to: – Refer to their local genetics centre and/or order appropriately order non-invasive prenatal testing (NIPT) and enhanced first trimester screening (e. FTS) – Discuss and address patient concerns regarding NIPT – Find high quality genomics educational resources appropriate for primary care

The latest in prenatal genetic screening for fetal aneuploidy 1. Cell-free fetal DNA testing (NIPT) 2. Enhanced first trimester screening

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) Two companies have contracts with the Ministry of Health to provide cf. DNA screening to Ontarians § Dyna. Care: Harmony. TM Prenatal Test § Life. Labs Genetics: Panorama. TM

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at ~11+ weeks gestation Down syndrome (trisomy 21) ~1 in 1, 000 live births Edward syndrome (trisomy 18) ~1 in 6, 000 live births Patau syndrome (trisomy 13) ~1 in 8 -15, 000 live births Increased risk associated with increased maternal age at delivery

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation Sex chromosome differences Klinefelter syndrome (47, XXY) Turner syndrome (45, X) Features are variable and depend on which chromosome is extra or missing Triple X syndrome (47, XXX) tall or short stature Jacob syndrome (47, XYY) Occur in about 1 in 500 live births delayed speech or learning differences health issues involving puberty or the heart Panorama/Lifelabs: always report sex chromosome aneuploidies Harmony/Dyna. Care: patient has option to choose monosomy x or full SCA panel - Adding sex chromosome panel increases false +ve rate

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation 3. Is available as a self-pay option to average and low risk women and with MOHLTC coverage for women at increased risk Under age 40 at expected birth No conventional screen or screen negative Normal ultrasound No significant history ~ 500$

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation 3. Is available as a self-pay option to average and low risk women and with MOHLTC coverage for women at increased risk In primary care, where there is a singleton pregnancy: Positive conventional prenatal screen (e. g. FTS/IPS/Quad) ≥ 40 years at expected date of birth Confirmed history of aneuploidy (e. g. previous pregnancy or child) Fetal nuchal translucency (NT) ≥ 3. 5 mm**

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation 3. Is available as a self-pay option to average and low risk women and with provincial funding in some provinces for women at increased risk (+/- specialist involvement) Fetal congenital anomalies on ultrasound which are suggestive of trisomy 21, 18, or 13 Increased risk of aneuploidy including combination of risk indicators including soft markers, biochemistry, maternal age, etc. At risk for male with an X-linked disorder

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation 3. Is available as a self-pay option to average and low risk women and with MOHLTC coverage for women at increased risk 4. Has a very high detection rate, positive predictive value and low false positive rate, for most conditions screened

cf. DNA vs conventional prenatal screening Screening test Detection rate / Sensitivity for T 211, 4 False Positive Rate Positive predictive for T 211, 4 value for T 212, 3 FTS 80 -85% 3 -9% IPS 85 -90% 2 -4% Quad/MMS 75 -85% 5 -10% SIPS 80 -90% 2 -7% >99% <0. 1% cf. DNA 1 Prenatal Screening Ontario 2 Bianchi et al 2014 N Engl J Med 370: 9 3 Norton et al 2015 N Engl J Med 372: 17 4 Gil et al 2015 Ultrasound Obstet Gynecol 45 ~4% ~80% for all populations (high and low risk women)

Five facts about prenatal screening by cell-free DNA 1. Is also known as non-invasive prenatal testing (NIPT) 2. Uses circulating cf. DNA derived from the placenta present in maternal blood to assess aneuploidy risk at 9 -10 weeks gestation 3. Is available as a self-pay option to average and low risk women and with MOHLTC coverage for women at increased risk 4. Has a very high detection rate, positive predictive value and very low false positive rate, for most conditions screened 5. Is a very sophisticated screen, however there are important limitations

cf. DNA limitations Diagnostic testing is recommended before any irrevocable action Chorionic Villus Sampling (CVS), 11 -13 weeks Amniocentesis, 15+weeks Why? Confined placental mosaicism: where the genetic make up of the placenta does not represent that of the fetus. cf. DNA
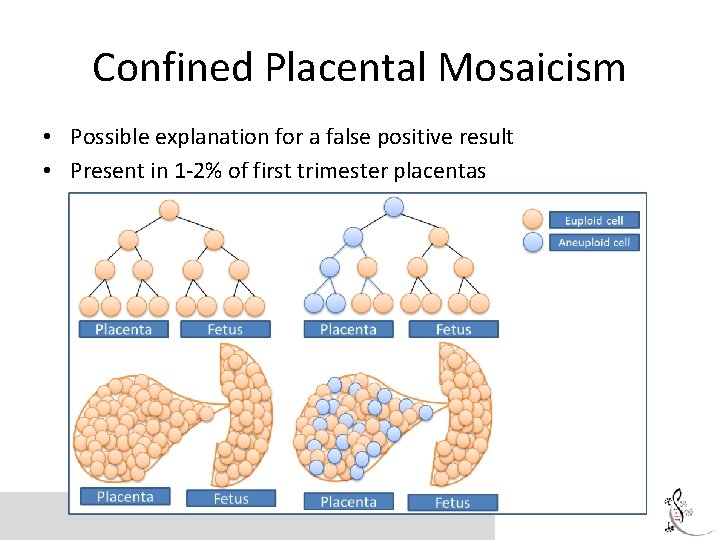
Confined Placental Mosaicism • Possible explanation for a false positive result • Present in 1 -2% of first trimester placentas

cf. DNA limitations Diagnostic testing is recommended before any irrevocable action Chorionic Villus Sampling (CVS), 11 -13 weeks Amniocentesis, 15+weeks Why? Confined placental mosaicism: where the genetic make up of the placenta does not represent that of the fetus. Fetal mosaicism Vanishing twin cf. DNA

cf. DNA limitations Diagnostic testing is recommended before any irrevocable action Not every genetic condition or congenital anomaly is screened for A late first trimester ultrasound at 11 to 14 weeks may be offered, where available An ultrasound at 18 -20 weeks gestation is recommended for all pregnancies, regardless of screening results Family history is the gold standard for risk assessment of heritable conditions cff. DNA

cf. DNA limitations Diagnostic testing is recommended before any irrevocable action Not every genetic condition nor congenital anomaly is screened for Risk of need for repeat test or test failure with no results 1 -6% of women will need a second blood draw ~1/2 – 3/4 will then receive a result Why? Technical issues Low fetal fraction (not enough fetal cf. DNA relative to mother’s) Refer to genetics for all NIPT results that are anything but “low risk” cff. DNA

cf. DNA limitations Diagnostic testing is recommended before any irrevocable action Not every genetic condition nor congenital anomaly is screened for Risk of need for repeat test or test failure with no results Twins There is limited evidence about the performance of cf. DNA screening in twin (or triplet) pregnancies cf. DNA

Enhanced First Trimester Screening What is e. FTS? Improved screening with (3 -4) serum markers NT (where available) AFP PAPP-A bh. CG Placental growth factor (Pl. GF) (Not always included)
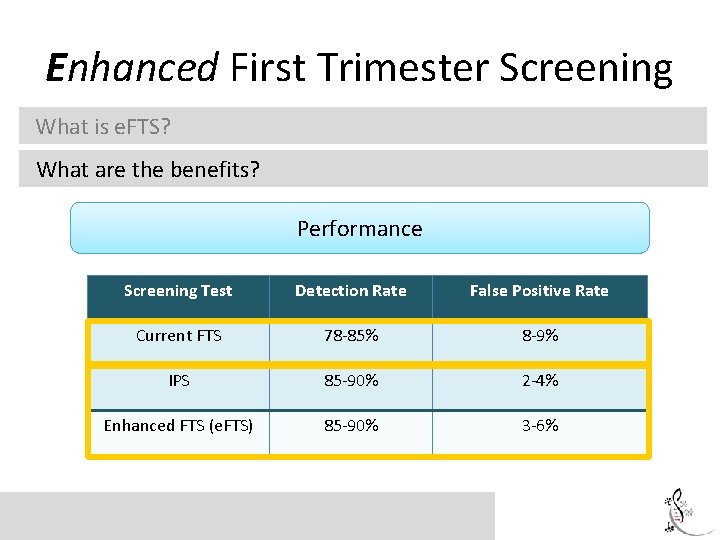
Enhanced First Trimester Screening What is e. FTS? What are the benefits? Performance Screening Test Detection Rate False Positive Rate Current FTS 78 -85% 8 -9% IPS 85 -90% 2 -4% Enhanced FTS (e. FTS) 85 -90% 3 -6%

Enhanced First Trimester Screening What is e. FTS? What are the benefits? Performance Earlier results with access to more options IPS results at about 17 weeks Vs. e. FTS results at about 12+ weeks

Enhanced First Trimester Screening What is e. FTS? What are the benefits? What are the limitations? Screening test not diagnostic Intended to screen for Down syndrome and trisomy 18 only Does not screen for open neural tube defects The primary screening test for the detection of fetal structural abnormalities including open/closed neural tube defects is a second trimester anatomical ultrasound SOGC 2017

What’s new in cell-free DNA screening? - Screening for microdeletion syndromes Microdeletion syndrome Incidence (at birth) Clinical features Babies born with this syndrome often have: 22 q 11. 2 deletion syndrome/ 1 in 4, 000 -2, 000 Di. George heart defects, immune system problems, and mild-to moderate intellectual disability. They may also have kidney problems, feeding problems, and/or seizures. 1 p 36 deletion syndrome 1 in 10, 000 -5, 000 weak muscle tone, heart and other birth defects, intellectual disabilities, and behavior problems. About half will have seizures. 1 in 12, 000 delayed milestones (like sitting, crawling and walking), seizures, and problems with balance and walking. They also have severe intellectual disability and most do not develop speech. Prader-Willi syndrome 1 in 25, 000 - 10, 000 low muscle tone and problems with feeding and gaining weight. They also have intellectual disability. As children and adults, they have rapid weight gain and often develop obesity related medical problems. Cri-du-chat syndrome (5 p-) 1 in 50, 000 - 20, 000 low birth weight, small head size, and decreased muscle tone. Feeding and breathing difficulties are also common. They have moderate-to-severe intellectual disability. Angelman syndrome • Harmony offers 22 q deletion only (~$175) • Panorama offers 22 q only or microdeletion panel (~$245) ‒ Requires confirmatory diagnostic testing

Expansion of non-invasive prenatal testing Arguments for offering cf. DNA with microdeletions • Cumulatively these disorders are common – The combined at-birth incidence of the 5 commonly offered microdeletion syndromes is approximately 1 in 1, 000 • Incidence is independent of maternal age

Expansion of non-invasive prenatal testing Arguments against offering cf. DNA with microdeletions • Because these are low-prevalence disorders, false positive results are inevitable and the positive predictive value will be low --- leading to more diagnostic invasive testing • No published clinical validation studies • There are no recommended guidelines – not considered standard of care • Provinces are not currently funding/ most geneticists not recommending
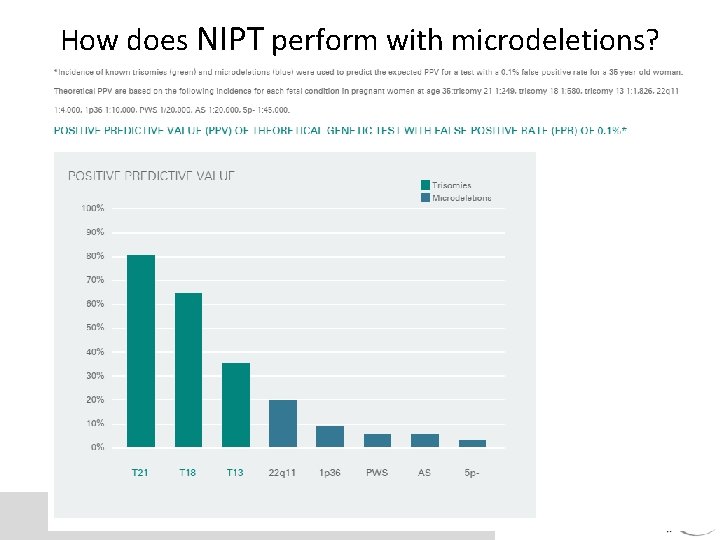
How does NIPT perform with microdeletions?

Case 1 38 yo woman, G 2 P 1 She and her partner are undecided about self-pay non-invasive prenatal testing or first trimester prenatal screening. They are provided with paper work for both screening tests. Your patient proceeds with both tests cf. DNA/NIPT results are reported first and are low risk (<1 in 10, 000 for all aneuploidies T 21, T 18, T 13) e. FTS is reported 4 days later and is screen positive (1 in 75 risk for Down syndrome) What is your next step? A. B. C. D. E. You refer to genetics to discuss diagnostic testing You reassure the patient, offer 18 -22 week scan You repeat cf. DNA/NIPT You order Quad screening None of the above

Case 1 38 yo woman, G 2 P 1: Your patient proceeds with both tests cf. DNA/NIPT results are reported first and are low risk (<1 in 10, 000 for all aneuploidies T 21, T 18, T 13) e. FTS is reported 4 days later and is screen positive (1 in 75 risk for Down syndrome) What is your next step? A. B. C. D. E. You refer to genetics to discuss diagnostic testing You reassure the patient, offer 18 -22 week scan You repeat cf. DNA/NIPT You order Quad screening None of the above Bottom line: If NIPT is being done as primary screen, do NT only and don’t do FTS to avoid discordant results

Case 2 29 year old woman with an NT of 4. 4 mm at 12+5 weeks gestation You offer NIPT and she accepts. NIPT results are normal. She is now 14+2 weeks gestation. You offer genetic counselling and she accepts. What is likely to be offered to this patient? A. Chromosomal microarray B. Genetic testing for other single gene conditions C. Detailed ultrasound D. Fetal echocardiogram E. All of the above

Case 2 29 year old woman with an NT of 4. 4 mm at 12+5 weeks gestation You offer NIPT and she accepts. NIPT results are normal. She is now 14+2 weeks gestation. You offer genetic counselling and she accepts. What is likely to be offered to this patient? A. Chromosomal microarray B. Genetic testing for other single gene conditions C. Detailed ultrasound D. Fetal echocardiogram E. All of the above

Where do I find more for my patients? www. geneticseducation. ca > Public Resources > Prenatal and Preconception

Where do I find more information? www. geneticseducation. ca

List of Screening Centres • Alberta – Calgary Early Risk Assessment Program Prenatal Genetics Clinic Suite 100, 3280 Hospital Dr NW – Edmonton Northern and Central Alberta Maternal – Fetal Medicine Centre Lois Hole Hospital for Women, Ground level 10240 Kingsway Avenue

List of Screening Centres • British Columbia – Vancouver Pregnancy Assessment Medical Genetics BC Women’s Hospital and Health Centre 4500 Oak Street, Room C 234 – Victoria Island Department of Medical Genetics Referral Form Victoria General Hospital 1 Hospital Way
List of Screening Centres • Manitoba – Winnipeg Prenatal Genetic Screening and Diagnosis Service WRHA Genetics and Metabolism Program Health Sciences Centre FE-229 Community Services Bldg, 820 Sherbrook Street • Newfoundland Labrador – St. John’s Provincial Medical Genetics Program – Eastern Health Genetics Janeway Children’s Health and Rehabilitation Centre Rm. 2088, 300 Prince Philip Drive

List of Screening Centres • Nova Scotia, New Brunswick, and Prince Edward Island – Halifax Fetal Assessment and Treatment Centre IWK Health Centre 7 th floor, Women’s Building

List of Screening Centres • Ontario – Hamilton Prenatal Diagnosis Clinic Mc. Master Children’s Hospital 2 F, 1200 Main Street West – Kingston Medical Genetics Program Kingston General Hospital Armstrong 4, 76 Stuart Street – Orillia North Simcoe Muskoka Regional Genetics Program Orillia Soldiers’ Memorial Hospital 170 Colborne Street West – London Prenatal Genetics Clinic London Health Sciences Centre Victoria Hospital Zone B, Level 5 (North Tower), 800 Commissioners Road East – Ottawa Regional Genetics Program CHEO Clinic WC– 2, 3 rd floor of the Max Keeping Wing, 401 Smyth Road – Sudbury Genetic Counselling Services Health Sciences North 865 sud, rue Regent St. South

List of Screening Centres • Ontario – Timmins Genetics Services Porcupine Health Unit 273 Third Avenue, Suite 103 – North Bay Genetic Counselling North Bay Parry Sound District Health Unit 681 Commercial Street – Sault Ste. Marie Genetics Program Algoma Public Health 294 Willow Avenue – Richmond Hill Genetics Clinic Mackenzie Richmond Hill Hospital B-Wing, Level 2, 10 Trench Street – Oshawa Genetics Clinic Lakeridge Health Oshawa 1 Hospital Court

List of Screening Centres • Ontario – Toronto Prenatal Diagnosis and Medical Genetics Program Mount Sinai Hospital 700 University Avenue, 3 rd Floor, Room 3298 Prenatal Genetic Counseling Sunnybrook Health Sciences Centre 2075 Bayview Avenue, M-wing, 4 th floor – Peterborough Genetics Program Peterborough Regional Health Centre 1 Hospital Drive – Mississauga Clinical Genetics Program Credit Valley Hospital Room 2 G 500, 2200 Eglinton Avenue West – Scarborough Regional Genetics Clinic Rouge Valley Centenary 4 th Floor, 2867 Ellesmere Road – Thunder Bay Genetics Program Thunder Bay Regional Health Sciences Centre 980 Oliver Road

List of Screening Centres • Quebec – Montreal Department of Medical Genetics Montreal Children’s Hospital A 04. 3140. 2 - 1001 Boulevard Décarie – Quebec City Departement de Médecine Génétique Centre hospitalier universitaire de Québec (CHUQ) Local H 1336, 2705 Boulevard Laurier

List of Screening Centres • Saskatchewan – Saskatoon Division of Medical Genetics Royal University Hospital Rm 515 Ellis Hall, 103 Hospital Drive
- Slides: 42