Premature progesterone rise negatively correlated with live birth

Premature progesterone rise negatively correlated with live birth rate in IVF cycles with Gn. RH agonist: An analysis of 2, 566 cycles Fertility and Sterility Vol. 98, No. 3, September 2012 30 th October 2012 Tuesday Infertility Journal reading R 4 孫怡虹/Dr. 蔡永杰

Serum P level in IVF cycles • ↑ On the day of h. CG administration: Not uncommon – Associated with: poor oocyte quality, low fertilization rate, adverse pregnancy outcome – Induced by inappropriate LH elevation (premature luteinization) • After the introduction of Gn. RH analogue – Inhibit LH elevation P level rise would be rare – Subtle rise is still about 5%– 71%: Premature progesterone rise (PPR)

Premature progesterone rise • The influence on pregnancy outcomes: controversial • ↑ Published papers since the 1990 s: – Negative effect vs. Positive correlation – Systematic review and meta-analysis (2007, Venetis et al. ): No correlation – Retrospective study (N > 4000, 2010, Bosch et al. ): • P level >1. 5 ng/Ml • In both Gn. RH agonist & antagonist cycles • Associated with ↓ ongoing pregnancy rate

Premature progesterone rise • Underlying mechanism to influences clinical outcomes: elusive – Premature of endometrium a detrimental factor to the endometrial receptivity – Compromised quality of oocytes

Premature progesterone rise • Pathogenesis and etiology: poorly understood 1) During controlled ovarian stimulation (COS) multiple follicles (each one producing a normal amount of P) Accumulated P production 2) Overdose of exogenous gonadotropin to promote: cholesterol P (Acting on granulosa cells) 3) Premature luteinization, as the consequence of subtle LH rise (Even with Gn. RHa) 4) Poor ovarian response with increased LH sensitivity

Hypothesis If PPR is harmful to clinical outcomes, either triggering h. CG in advance or freezing all embryos should be recommended to avoid the adverse consequences

Aim • Retrospective analysis • To quantify the incidence of PPR – In a large cohort of patients (n = 2, 566) – Undergoing COS with Gn. RH agonist long or short protocol ? To investigate the relationship: Serum P level Probability of live birth ? Possible mechanism: PPR affects live birth rate ? Possible factor(s) related to the occurrence of PPR

MATERIALS AND METHODS

Non-interventional retrospective analysis • Reproductive Medicine Center of the Women and Children Hospital of Guangdong Province • January 1, 2002 ~ December 30, 2007 – Women who started their first IVF/ICSI cycles with Gn. RH agonist treatment: All IVF/intra-cytoplasmic sperm injection (ICSI) cycles – All with Controlled Ovarian Stimulation – In the case of P level rise No fresh ET canceled • F/u through December 2011 – For clinical data of frozen ET

• 3, 034 patients Excluded: 468 cycles (No embryo formed or all embryos were frozen owing to OHSS or other personal reasons) • Long protocol (n = 1, 719) Short protocol (n = 847) – 2002 ~ 2004, Short protocol: protocol prevalent (650/733, 88. 7%) Long protocol: PCOS patients or some potential high responders – 2005 ~ 2007, Long protocol: protocol dominant (1, 636/1, 833, 89. 3%) Short protocol: potential poor responders or patients refusing long protocol for personal reasons
Controlled Ovarian Stimulation Protocol • Long protocol: – Triptorelin depot 1. 875 mg or 1. 3 mg Down regulation – Recombinant FSH Ovarian stimulation • Short protocol: – Triptorelin 0. 1 mg In cycle day 2 – r. FSH From day 3

Controlled Ovarian Stimulation Protocol • Follicle growth monitoring: – Serum E 2, P, and LH level measurements – Vaginal ultrasound investigation è≥ 2 follicles: size of ≥ 18 mm 35 hours later 10, 000 IU h. CG for the oocyte retrieval

Embryo Culture, Transfer, Freezing and Thawing • Cultured in Quinnes sequential culture media – Transferred on day 3: ≤ 3 Embryos èLuteal support: 20– 40 mg P in oil – Surplus embryos frozen: ≥ 4 cells, < 25% fragmentation • For frozen ET: – Transferred: ≤ 3 frozen-thawed survival embryos – In a natural or hormonal replacement cycle

Hormone Assays • Serum: 8– 9 a. m. at each time point • FSH, LH, E 2, P analyzed by radioimmunoassay • Intra- vs. inter-assay coefficients of variation: – LH = 5. 8% vs. 9. 1% – FSH = 5. 6% vs. 7. 8% – E 2 = 8. 2% vs. 9. 3% – P = 7. 0% vs. 9. 6% • Progesterone: – Sensitivity = 0. 1 ng/ml – Range of measurement = 0. 1– 40 ng/m. L

Outcome Variables • Primary outcome variable: Live birth rate • Secondary outcome variables: – Clinical pregnancy rate: Presence of FHB on ultrasound at 7 weeks' pregnancy – Implantation rate: Number (Gestational sacs seen on the ultrasound) Total number (Embryos transferred)
![Statistical Analysis • Patients divided into 6 groups: – According to Serum [P] (ng/m. Statistical Analysis • Patients divided into 6 groups: – According to Serum [P] (ng/m.](http://slidetodoc.com/presentation_image/a0b8612f1ac9d5968eb04cf2dc79bd5b/image-16.jpg)
Statistical Analysis • Patients divided into 6 groups: – According to Serum [P] (ng/m. L) on the day of h. CG administration: – ≤ 0. 9, 1. 0– 1. 2, 1. 3– 1. 5, 1. 6– 1. 8, 1. 9– 2. 0, >2. 00 • Bosch method (Trend analysis) To determine the cutoff value of PPR • Odds ratio (OR) of live birth rate (each P interval preceding interval)

• Logistic regression analysis: – Parameters possibly related to live birth rate ( x 14) – In which P level, age, and the number of highquality embryos transferred were categorized • Multivariate analysis: for assessing Factors related to PPR

RESULTS
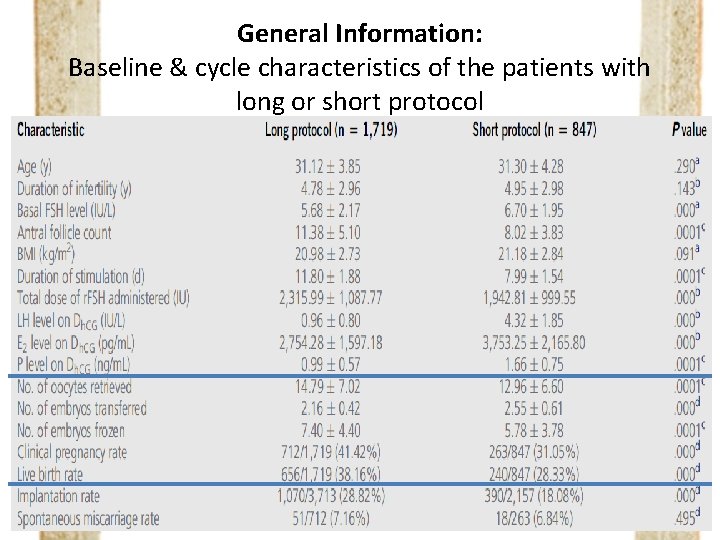
General Information: Baseline & cycle characteristics of the patients with long or short protocol
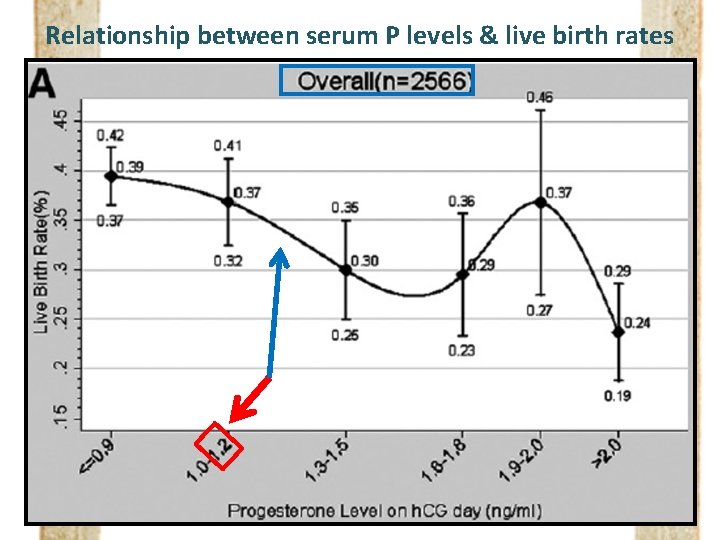
Relationship between serum P levels & live birth rates
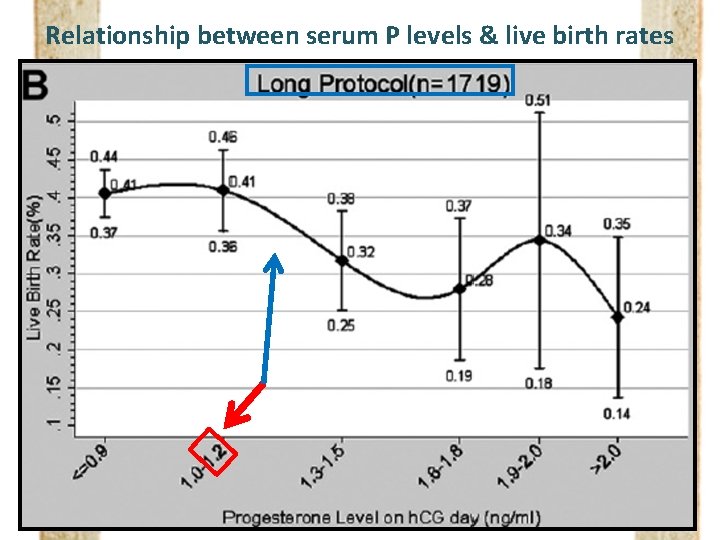
Relationship between serum P levels & live birth rates
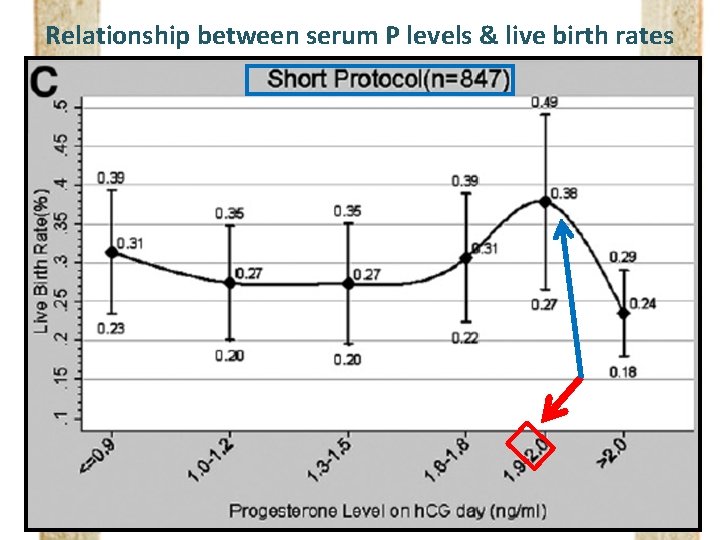
Relationship between serum P levels & live birth rates
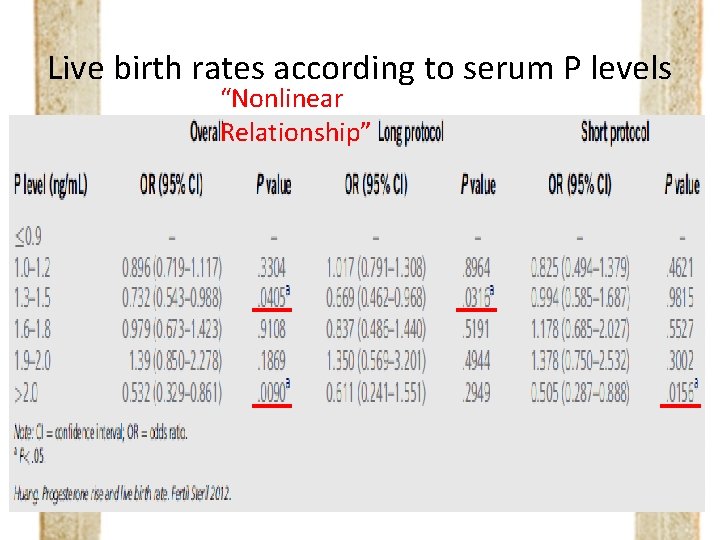
Live birth rates according to serum P levels “Nonlinear Relationship”
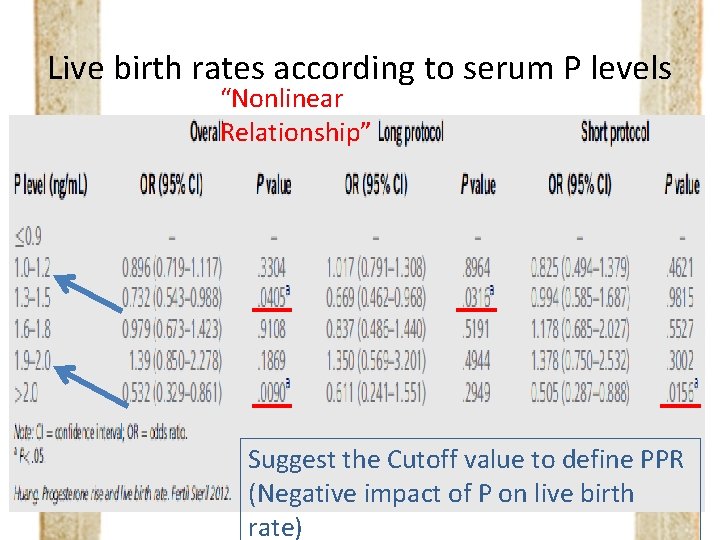

Live birth rates according to serum P levels “Nonlinear Relationship” Suggest the Cutoff value to define PPR (Negative impact of P on live birth rate)

Incidence of PPR • Long protocol: 22. 86% (393/1719) • Short protocol: 27. 63% (234/847)
Clinical outcomes (With Without PPR) • Clinical pregnancy rate – Long protocol: OR 0. 74, P=0. 004 – Short protocol: OR 0. 84, P=0. 002 • Implantation rate – Long protocol: OR 0. 73, P=0. 000 – Short protocol: OR 0. 71, P=0. 005 • Live birth rate – Long protocol: 40. 65/29. 77(%), OR 0. 73; P=. 004 – Short protocol: 30. 18/23. 50(%), OR 0. 78; P=. 083

Logistic regression analysis • For potential factors (might influence live birth rate) • Confirmed: P level did have a negative effect on live birth rate in both (long/short) protocols
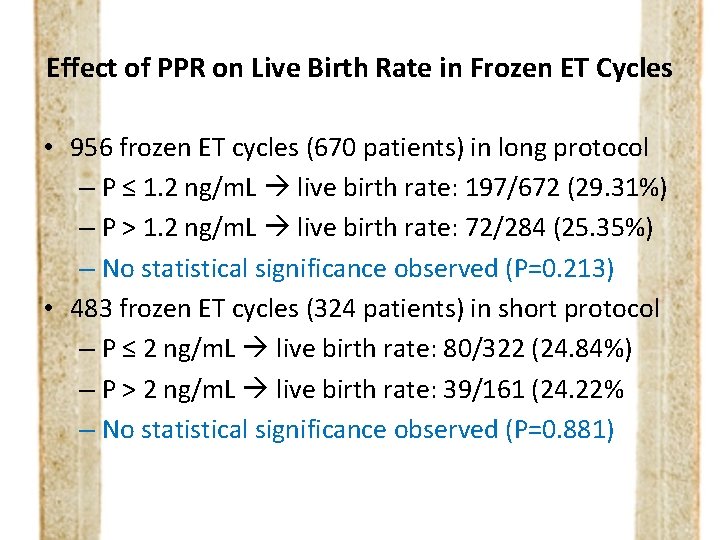

Effect of PPR on Live Birth Rate in Frozen ET Cycles • 956 frozen ET cycles (670 patients) in long protocol – P ≤ 1. 2 ng/m. L live birth rate: 197/672 (29. 31%) – P > 1. 2 ng/m. L live birth rate: 72/284 (25. 35%) – No statistical significance observed (P=0. 213) • 483 frozen ET cycles (324 patients) in short protocol – P ≤ 2 ng/m. L live birth rate: 80/322 (24. 84%) – P > 2 ng/m. L live birth rate: 39/161 (24. 22% – No statistical significance observed (P=0. 881)
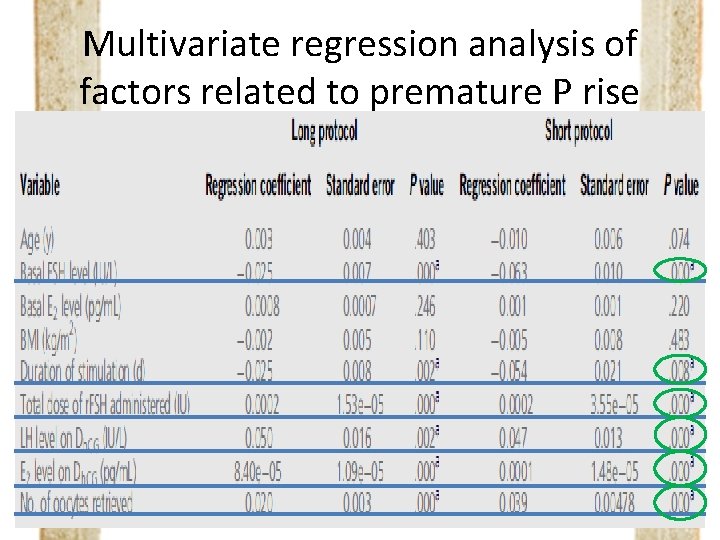
Multivariate regression analysis of factors related to premature P rise

DISCUSSION

Relationship between PPR and clinical outcomes • Controversy – Distinct definition of PPR (0. 9 ~ 2. 0 ng/m. L) – Different statistic methods used – Different characteristics of patients recruited – Retrospective nature of studies analyzing the relationship between PPR and clinical outcomes

Relationship between PPR and clinical outcomes • Not linear in this study (consistent with Bosch et al. 's report) Trend analysis Negative relationship: PPR live birth rate Cutoff value: 1. 2 ng/m. L in long protocol & 2. 0 ng/m. L in short protocol ( 1. 5 ng/m. L) Analyse Live birth rate ( Ongoing pregnancy rate) Patients were much younger (31. 1 vs. 35. 3 years) Different methods of progesterone measurement

Relationship of PPR and clinical outcomes in Gn. RH agonist long protocol • Some studies failed to observe negative correlation: – Limited number of patients recruited – Relatively low threshold used to define PPR • Present study: Largest number of patients (n = 1, 719) with long protocol strengthening the conclusion

Relationship of PPR and clinical outcomes in short protocol • In this study: 1) P level: Short protocol > Long protocol – Flare-up effect of Gn. RH agonist relatively ↑ LH – LH might also be involved in the occurrence of PPR 2) Clinical pregnancy rate (P=. 002) & Live birth rate (P=. 083) ↓ when P level >2 ng/m. L 3) Normal & poor responders (former predominant) 4) ↑ Number of patients involved 5) Cutoff value to define PPR: 2. 0 ng/Ml

The distinct cutoff values determined in the present study 1) The characteristics of patients in long or short protocol were different from each other, more poor responders being included in short protocol 2) The cycle properties of the two protocols are different, with the LH level in the follicle phase being much higher in short protocol 3) The number of patients included in short protocol was relatively few, which might have introduced a bias

Logistic regression analysis in the present study • To exclude interference from confounding factors – Difficult in retrospective study & Prospective studies • 13 confounding factors èConfirmed: PPR was a negative predictor of live birth rate èLow pre ovulatory serum P A dominant predictor of clinical pregnancy

How PPR affects live birth rate ? • Compromised oocyte quality ? èIf it’s the main reason Triggering h. CG in advance would be the first choice (avoid the adverse effects of PPR on the quality of oocytes) • Decreased endometrial receptivity ? èIf it plays a key role freezing embryos would be a better choice (triggering h. CG in advance: would compromise the overall quality of the oocyte cohort when most of the trailing follicles are still small)

How PPR affects live birth rate ? • Frozen ET cycles: long protocol (n = 956) and short protocol (n = 483) èLive birth rates: Not significantly different between the groups with or without PPR èPPR may negatively affect live birth rate through decreased endometrial receptivity • Based on a donor oocyte IVF model, Melo et al. èPregnancy rates of recipients: Not influenced by the P levels of donors è↑ P did not deteriorate the quality of oocytes

Gene expression profile of endometrium • P level >1. 5 ng/m. L vs. normal obviously different van Vaerenberg et al. • Difference maintained until implantation occurred Labarta et al. è↓ Endometrial receptivity may be a cause of ↓ live birth rate èFor Case of P rise on the day of h. CG administration: (The most appropriate choice to avoid the negative effect): cancel fresh ET & freeze all embryos (rather than triggering h. CG in advance)

Underlying mechanism of the occurrence of PPR • Compare multiple variables: Groups without PPR – Factors showing difference the reason of PPR – Simple/weak to distinguish causal/non-causal correlation – Can’t reflect the interaction among variables • Logistic regression in this stidy Analyze which factors were involved in PPR P level (continuous variable) be categorized into 2 groups minify the influence of some factors

Possible explanations of the occurrence of PPR 1. Multiple follicle growth 2. Overdose of exogenous gonadotropin 3. Premature lutineization èPartly explain the reasons from limited facets èMultivariate regression analysis in this study: all contributed to PPR ( Hugues et al. 's conclusion) 4. Poor ovarian response èNot that convincing (women with lower basal FSH level inclined to have PPR)

Multivariate regression analysis • Included Baseline characteristics – (Basal FSH, E 2 level, BMI, Age) – Dose of gonadotropin administered Influence – Patients' ovarian response (Number of oocytes retrieved, E 2 level on the day of h. CG administration) Make the conclusion more reliable & comprehensive

Summary In these 2, 566 patients undergoing their first IVF/ICSI cycles treated with Gn. RH agonist long/short protocol… • PPR Negatively correlated with live birth rate in fresh ET cycles No adverse impact on frozen ET observed èPPR may have deleterious effects on endometrial receptivity

THANK YOU FOR LISTENING
- Slides: 44