Prehospital NSTEMI Patient Assessment and Treatment Paul A










- Slides: 17

Prehospital NSTEMI Patient Assessment and Treatment Paul A. Berlin, MS, NRP

Presenter Disclosure Information Paul A. Berlin Prehospital Non-STEMI Assessment and Treatment FINANCIAL DISCLOSURE: § None UNLABELED/UNAPPROVED USES DISCLOSURE: § None

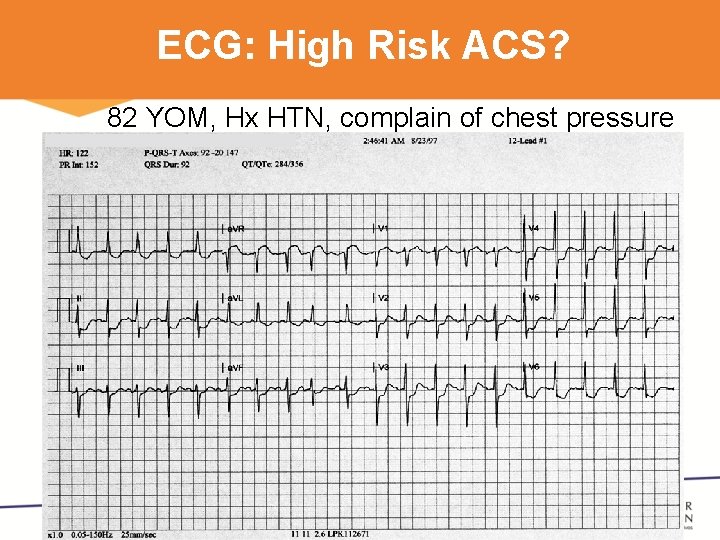
ECG: High Risk ACS? 82 YOM, Hx HTN, complain of chest pressure 3

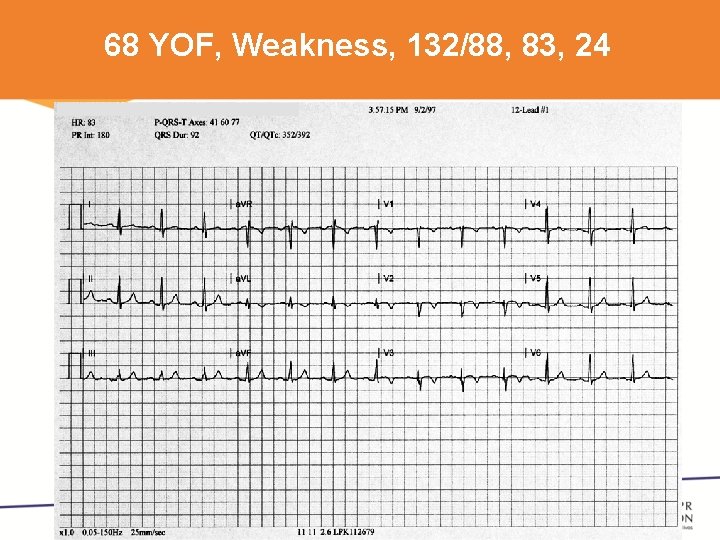
68 YOF, Weakness, 132/88, 83, 24

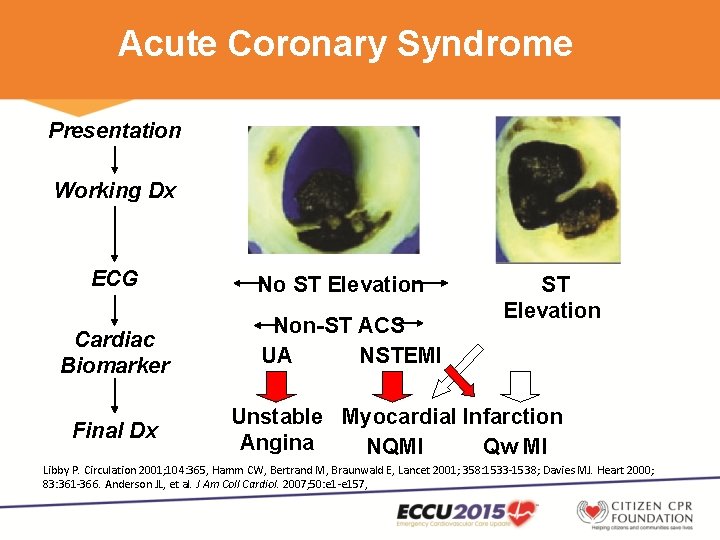
Acute Coronary Syndrome Presentation Working Dx ECG Cardiac Biomarker Final Dx No ST Elevation Non-ST ACS UA NSTEMI ST Elevation Unstable Myocardial Infarction Angina NQMI Qw MI Libby P. Circulation 2001; 104: 365, Hamm CW, Bertrand M, Braunwald E, Lancet 2001; 358: 1533 -1538; Davies MJ. Heart 2000; 83: 361 -366. Anderson JL, et al. J Am Coll Cardiol. 2007; 50: e 1 -e 157,

Myocardial Infarction • Non-ST – Segment Elevation (NSTEMI) (30% - 45%) • ST – Segment Elevation (STEMI) (55% - 70%) How do we find the 30% - 45% of MI patients we are missing?

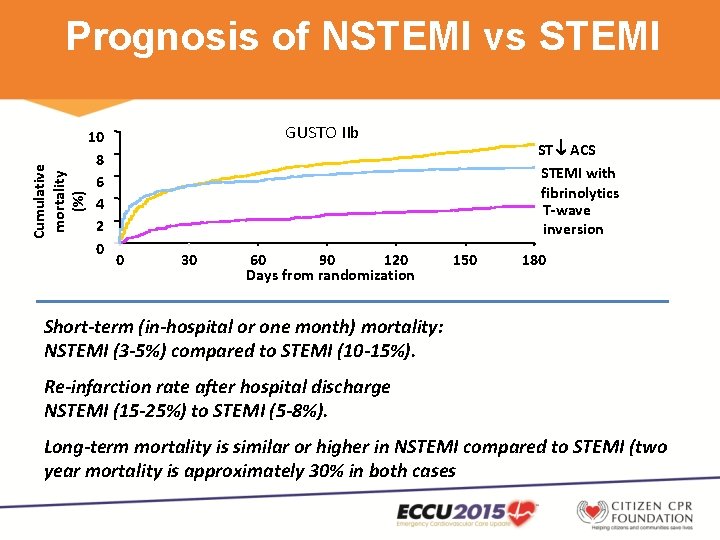
Cumulative mortality (%) Prognosis of NSTEMI vs STEMI 10 8 6 4 2 0 GUSTO IIb 0 30 60 90 120 Days from randomization ST ACS STEMI with fibrinolytics T-wave inversion 150 180 Short-term (in-hospital or one month) mortality: NSTEMI (3 -5%) compared to STEMI (10 -15%). Re-infarction rate after hospital discharge NSTEMI (15 -25%) to STEMI (5 -8%). Long-term mortality is similar or higher in NSTEMI compared to STEMI (two year mortality is approximately 30% in both cases

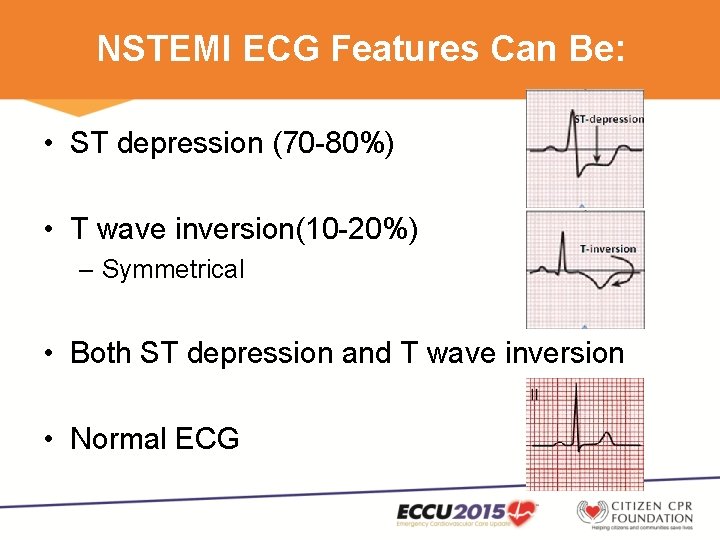
NSTEMI ECG Features Can Be: • ST depression (70 -80%) • T wave inversion(10 -20%) – Symmetrical • Both ST depression and T wave inversion • Normal ECG

Assess Applicability for ACS Triage WA State EMS ≥ 21 years of age with symptoms lasting more than 10 minutes but less than 12 hours suspected to be caused by coronary artery disease: q Chest discomfort, pressure, crushing pain, tightness, heaviness, cramping, burning, aching sensation, usually in the center of the chest lasting more than a few minutes, or that goes away and comes back. q Epigastric (stomach) discomfort, such as unexplained indigestion, belching, or pain. q Shortness of breath with or without chest discomfort. q Radiating pain or discomfort in 1 or both arms, neck, jaws, shoulders, or back. q Other symptoms may include sweating, nausea, vomiting. q Women, diabetics, and geriatric patients might not have chest discomfort or pain. Instead they might have nausea/vomiting, back or jaw pain, fatigue/weakness, or generalized complaints.

Assess High Risk Criteria Based on TIMI (Three or more checked, High risk for NSTEMI) q Age ≥ 55* q 3 or more CAD risk factors: q q q Family history of CAD High BP High cholesterol Diabetes Current smoker q Aspirin use in last 7 days q Angina in last 24 hours q ST-segment deviation on ECG q Known coronary disease q Elevated cardiac biomarkers

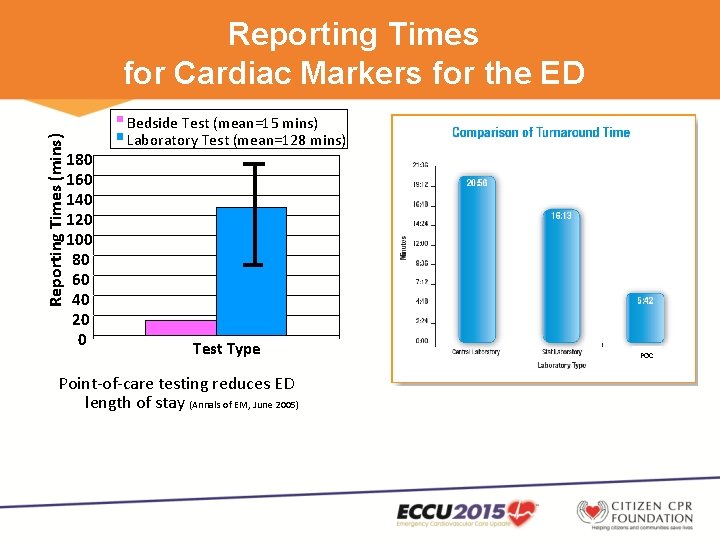
Reporting Times (mins) Reporting Times for Cardiac Markers for the ED 180 160 140 120 100 80 60 40 20 0 Bedside Test (mean=15 mins) Laboratory Test (mean=128 mins) Test Type Point-of-care testing reduces ED length of stay (Annals of EM, June 2005) POC

High-sensitivity cardiac troponin I at presentation in patients with suspected ACS • Low plasma troponin concentrations identify two –thirds of patients at very low risk of cardiac events who could be discharged from hospital. • Implementation of this approach could substantially reduce hospital admissions and have major benefits for both patients and health –care providers. The Lancet, 10/27/2015 Shah ASV, et al.

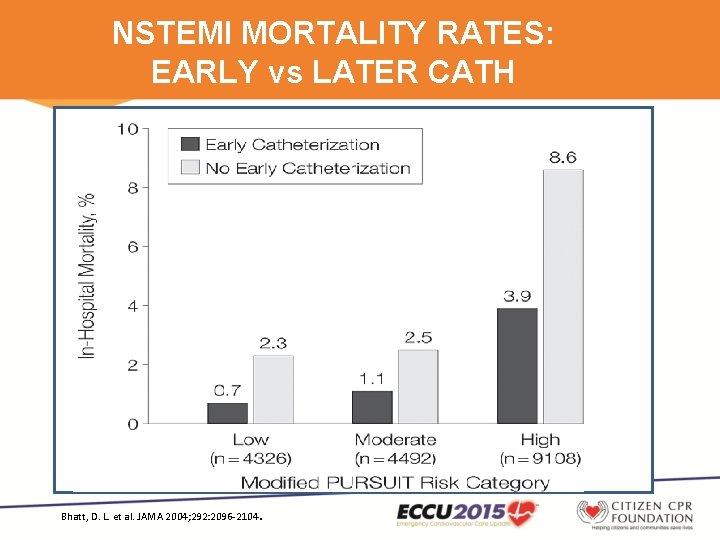
NSTEMI MORTALITY RATES: EARLY vs LATER CATH Bhatt, D. L. et al. JAMA 2004; 292: 2096 -2104.

Treatment Options • • Limit scene time Transport patient to the right facility Follow AHA or local protocols Communicate with receiving facility – Transmit ECG if available • Fibrinolytic check sheet PRN

Challenges • ECG quality • Acceptance of POC – Establishing POC • Risk Assessment Training • Acceptance by Receiving Centers

Questions? • NSTEMI recognition programs are the next step in ACS care following the implementation of strong Prehospital STEMI care programs. • Early recognition of NSTEMI using ECG findings, risk stratification and early biomarkers by prehospital care providers can direct patients to appropriate receiving facilities and reduce morbidity and mortality.

Contact Info: Paul A. Berlin Irondoc. paul@gmail. com