Pregnancy and Drug Abuse Eva JanecekRucker Learning Objectives

Pregnancy and Drug Abuse Eva Janecek-Rucker

Learning Objectives 1. To develop a knowledge base of the effects of substances of abuse (e. g. , alcohol, cocaine, nicotine et al. ) during pregnancy. 2. To examine the pharmacist’s role and develop a comfort level with respect to prevention, counselling and referral of women planning pregnancy as well as those who are pregnant and using psychoactive substances.

Drugs in Pregnancy • CNS depressants – alcohol – benzodiazepines – barbiturates – inhalants (toluene; often combined with alcohol) • CNS stimulants –cocaine –caffeine –nicotine

Drugs in Pregnancy • Hallucinogens – cannabis – LSD • Opioids – codeine, morphine – heroin

Interpretation of Results • Animal studies • Prenatal drug exposure (dose, timing, duration) • Withdrawal • Breastfeeding

Issues with Illicit Drug Use During Pregnancy • Drug – authenticity – dose – additives • Pharmacological effects • Multiple drug use • Injection drug use • Effect of father’s drug use

Issues (cont’d) • Lack of prenatal care • Poor diet • Smoking • Drinking • Violence

Alcohol Fetal Alcohol Spectrum Disorder (FASD) • High risk: woman drinking 6 standard drinks/day during the first trimester • Signs of FAS: – prenatal and postnatal growth retardation – CNS dysfunction (often including mental retardation) • Facial dysmorphology • Other congenital abnormalities • Fetal alcohol effects (FAE)
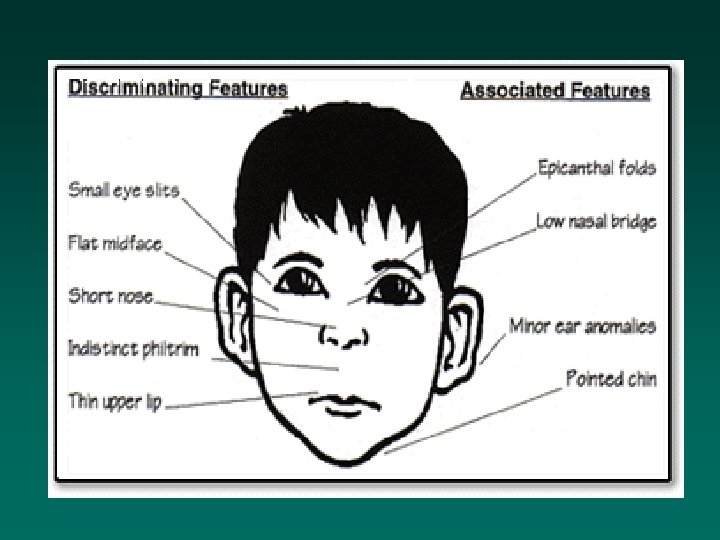
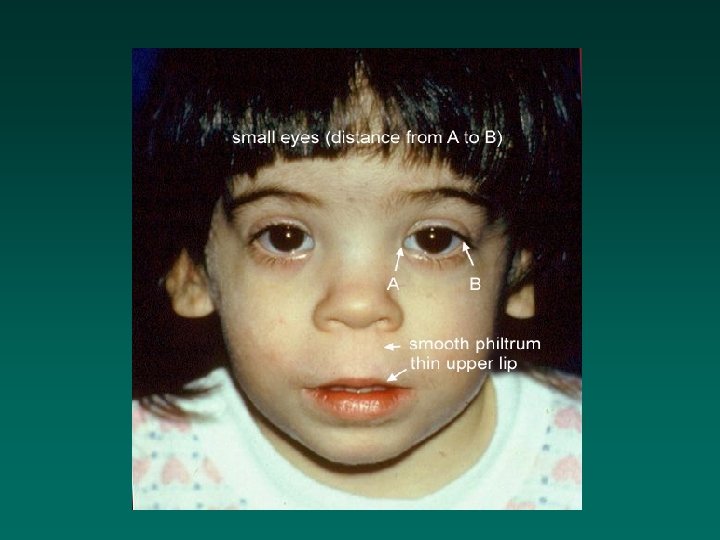
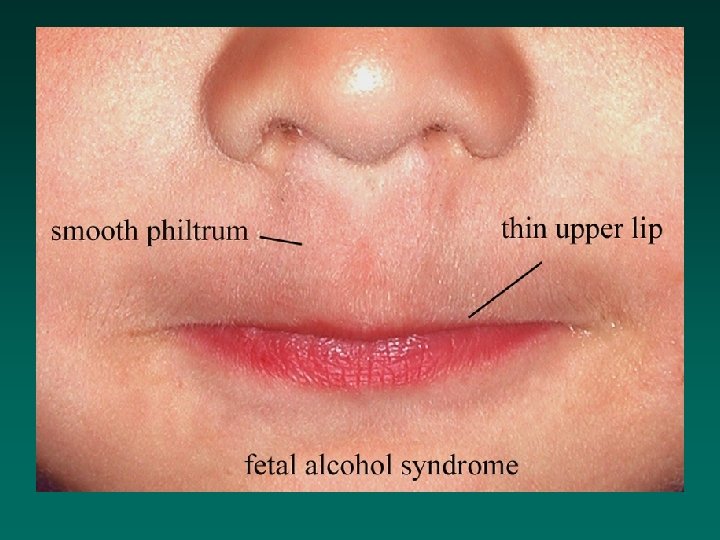

Alcohol (cont’d) • No safe level established – a Canadian committee recommended abstinence ‘or at least to limit consumption to less than 4 drinks per week’

Alcohol (cont’d) • Treatment of a pregnant alcoholic – diazepam loading for alcohol withdrawal • Disulfiram -contraindicated in pregnancy • Naltrexone ?

Solvents • Effects similar to FAS: – CNS dysfunction – Attentional deficits – Growth deficiency – Development delay – Facial dysmorphology

Benzodiazepines • Likely not teratogenic; cleft lip/palate? ? ? • Neonatal withdrawal symptoms

Barbiturates and other hypno-sedatives • No evidence of teratogenicity • Neonatal withdrawal syndrome • Treatment: phenobarbital

Cocaine • • Spontaneous abortion Prematurity Intrauterine growth retardation Abruptio placentae Perinatal cerebral infarction Structural CNS abnormalities Urogenital abnormalities Concomitant use of other drugs (alcohol and benzodiazepines)

Nicotine • Spontaneous abortion • Low birth weight • Perinatal mortality • Prematurity • Abruptio placentae • Congenital malformations (most studies show lack of) • Sudden infant death syndrome (SIDS)

Caffeine • Low dose - no effect • High dose: – in animals - adverse effects – in humans - ?

Heroin • Fetal distress or death during withdrawal in utero • Decreased birth weight • Higher incidence of Ø Infections Ø medical complications Ø obstetrical complications • Neonatal withdrawal • SIDS

Heroin (cont’d) Treatment of pregnant woman • methadone

Cannabis • Decreased birth weight • Prematurity • Effect of tar • No congenital abnormalities

LSD • Limb defects • CNS abnormalities • Ocular abnormalities

Pharmacist’s Role • Identification • Information • Referral

Resources • Alcohol and Drug Assessment and Treatment Services • Motherisk: www. motherisk. org (416) 813 -6780 • www. pregnets. org • Information sources –Textbooks ØDrugs in Pregnancy and Lactation 6 th Edition, GG Briggs, RK Freeman, SJ Yaffe (eds), 2001 ØMaternal-Fetal Toxicology: A Clinician’s Guide 2 nd Edition, G Koren (ed), 1994 –Journals
- Slides: 25