Predictive Modeling 2008 The Blue Cross Blue Shield

Predictive Modeling 2008: The Blue. Cross Blue. Shield of Tennessee Experience Soyal Momin MS, MBA September 23, 2008

Outline • Maximizing the Value of Predictive Modeling: A Health Plan Perspective – Care Management Challenges: • Understand Population Care Management Needs • Identify • Stratify • Triage – Care Management Model, Implementation, Process Efficiencies • Intervene – Care Management Programs • Evaluate – Conclusions

Care Management Challenges: Understand Population Care Management Needs • Cost distribution and trend over time – Quantitative assessment • Population assessment – Qualitative assessment – clinical cost drivers based on healthcare cost (direct cost) • Total cost assessment – direct & indirect costs – Qualitative assessment – clinical cost drivers based on healthcare cost and personnel cost (indirect cost)
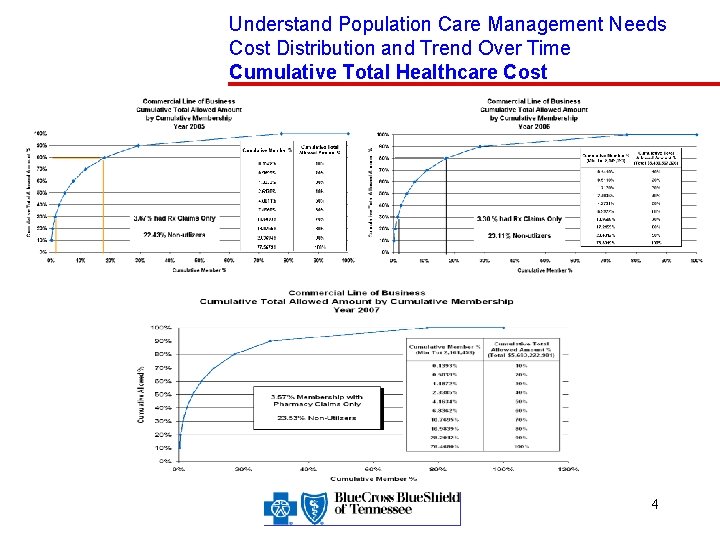
Understand Population Care Management Needs Cost Distribution and Trend Over Time Cumulative Total Healthcare Cost 4
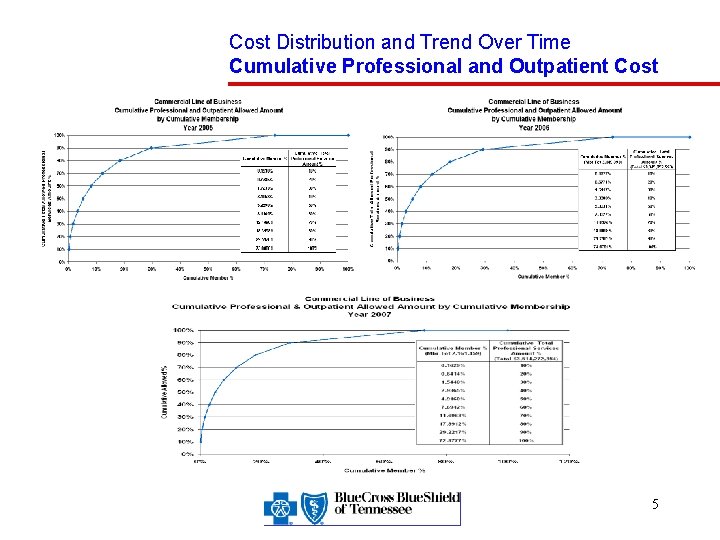
Cost Distribution and Trend Over Time Cumulative Professional and Outpatient Cost 5
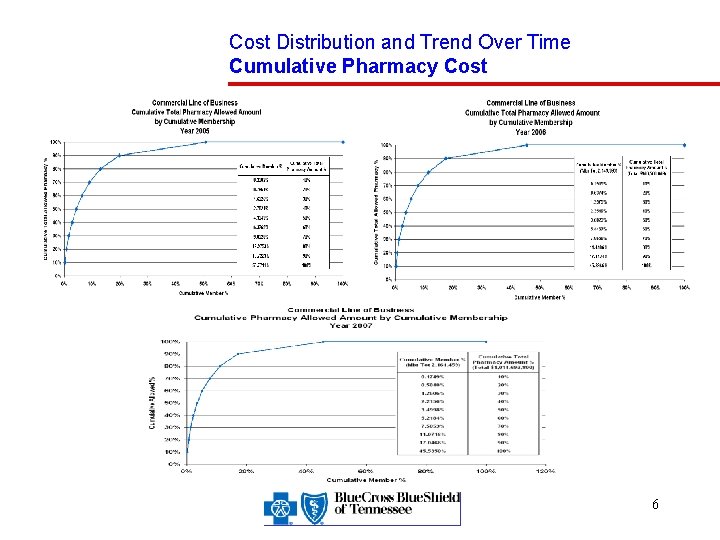
Cost Distribution and Trend Over Time Cumulative Pharmacy Cost 6
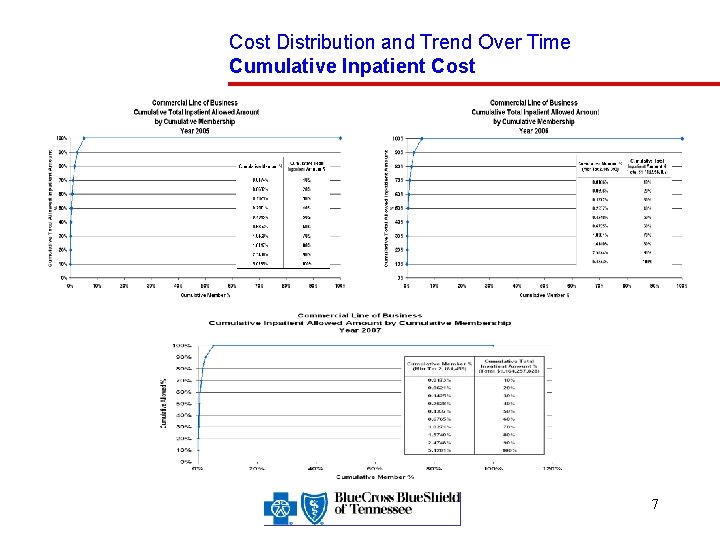
Cost Distribution and Trend Over Time Cumulative Inpatient Cost 7

Understand Population Care Management Needs Population Assessment is an analysis of claims and membership data to determine characteristics of a given population (Network, Region, Group) that might affect the population’s interaction with the health care system 8

Population Assessment Major Analysis Variables Propensity to Utilize Index – The average number of episodes of illness for a member month Episode Seriousness Index – A measure of the average cost to treat the categories of illness experienced by a population Illness Burden – A measure of the level of illness within a group determined by multiplying the propensity to utilize index by the Episode Seriousness Index 9

Population Assessment Major Analysis Variables, Continued Provider Efficiency Index – A measure of the efficiency to treat a specific episode of illness determined by dividing the cost to treat the specific episode by the average cost for the category of illness PMPM Cost Index – An index that measures the PMPM submitted costs for a population determined by multiplying the Illness Burden by the Provider Efficiency Index 10
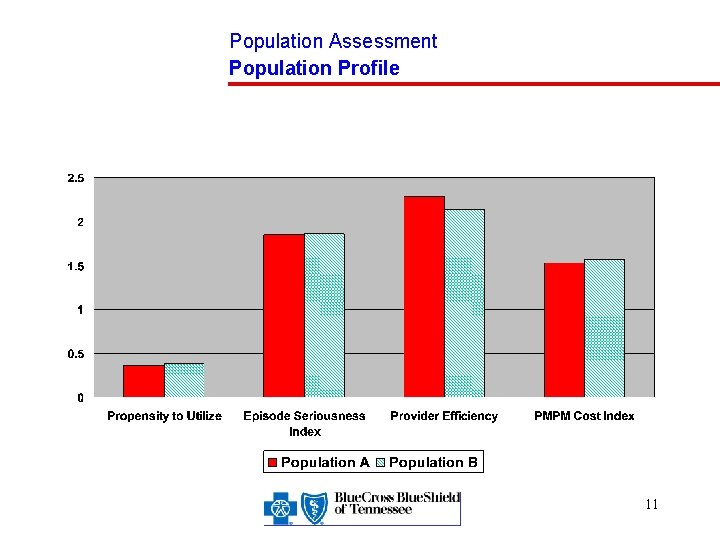
Population Assessment Population Profile 11
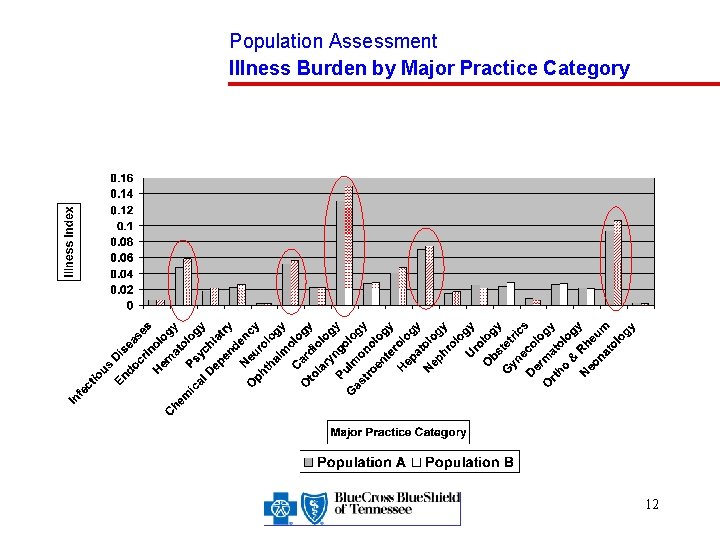
Population Assessment Illness Burden by Major Practice Category 12
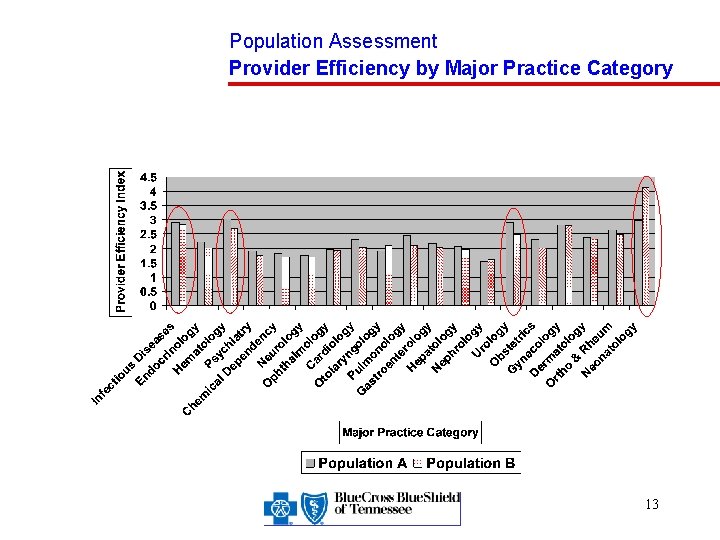
Population Assessment Provider Efficiency by Major Practice Category 13
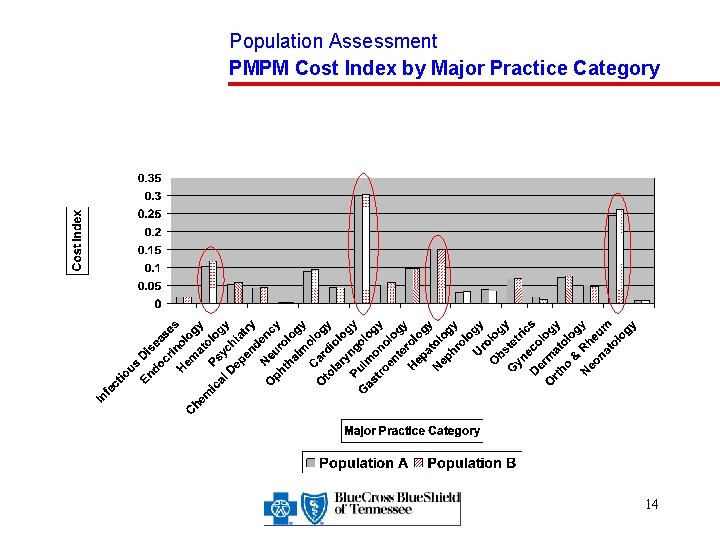
Population Assessment PMPM Cost Index by Major Practice Category 14

Understand Population Care Management Needs Total Cost Assessment Direct costs are dollars paid out for medical treatment § Indirect costs are labor resources lost due to illness § Direct Costs = Inpatient + Professional/Outpatient + Pharmacy Indirect Costs = Sick Leave + Presenteeism + Family & Medical Leave + Turnover Short Term Disability + Long Term Disability + + Worker’s Compensation 15
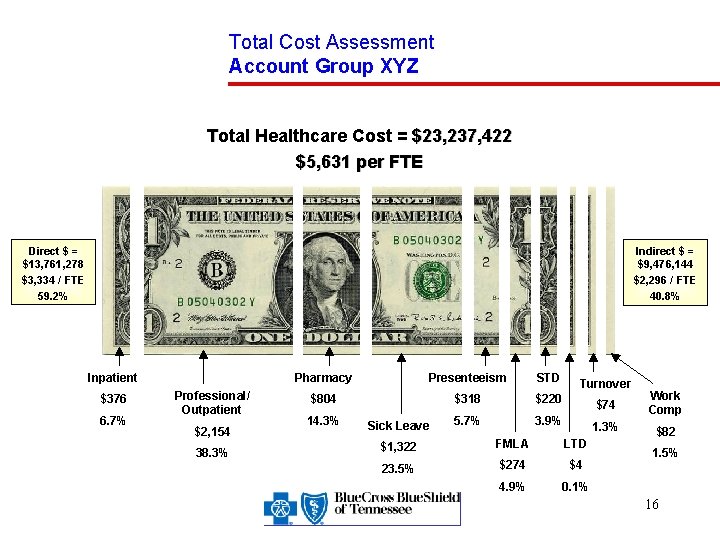
Total Cost Assessment Account Group XYZ Total Healthcare Cost = $23, 237, 422 $5, 631 per FTE Direct $ = $13, 761, 278 $3, 334 / FTE 59. 2% Indirect $ = $9, 476, 144 $2, 296 / FTE 40. 8% Inpatient $376 6. 7% Professional/ Outpatient $2, 154 38. 3% Pharmacy Presenteeism STD Turnover $804 $318 $220 $74 5. 7% 3. 9% Work Comp 1. 3% $82 14. 3% Sick Leave $1, 322 FMLA LTD 23. 5% $274 $4 4. 9% 0. 1% 1. 5% 16
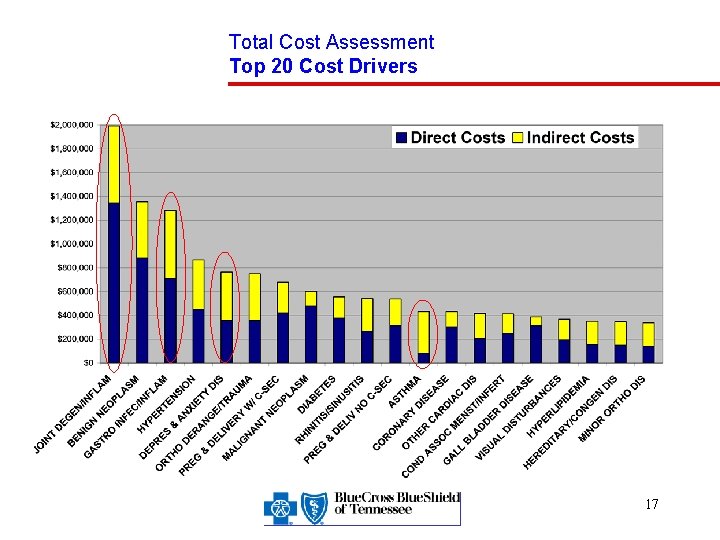
Total Cost Assessment Top 20 Cost Drivers 17

Care Management Challenges: Identify & Stratify Members for Care Management • Identifying Members for Care Management – Referrals from • Internal Sources • External Sources • An internally developed ICD 9 Trigger list – The ICD 9 Trigger list included Asthma, Diabetes, High Risk OB, AIDs, Cancer, CHF, COPD etc – High cost member report • Case managers workload • 103/CM/Month • High predicted cost member report • Stratification index report
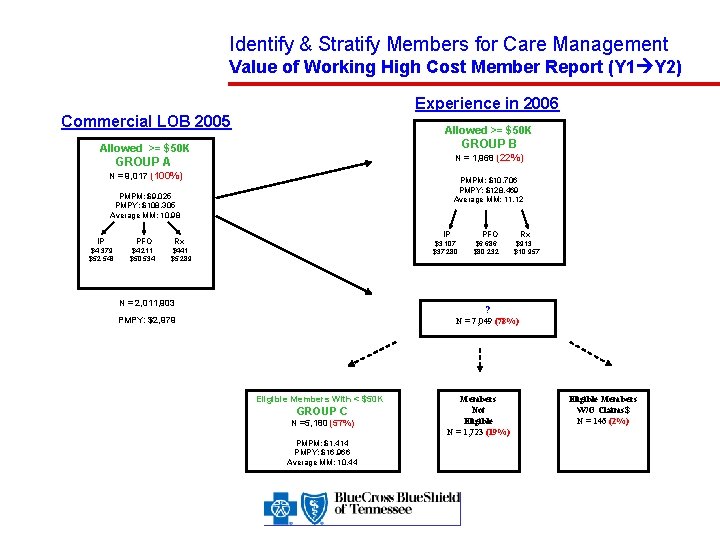
Identify & Stratify Members for Care Management Value of Working High Cost Member Report (Y 1 Y 2) Experience in 2006 Commercial LOB 2005 Allowed >= $50 K GROUP B Allowed >= $50 K N = 1, 968 (22%) GROUP A N = 9, 017 (100%) PMPM: $10, 706 PMPY: $128, 469 Average MM: 11. 12 PMPM: $9, 025 PMPY: $108, 305 Average MM: 10. 98 IP PFO Rx $4, 379 $52, 543 $4, 211 $50, 534 $441 $5, 289 IP PFO $3, 107 $37, 280 N = 2, 011, 903 $6, 686 $80, 232 Rx $913 $10, 957 ? PMPY: $2, 979 N = 7, 049 (78%) Eligible Members With < $50 K GROUP C N =5, 180 (57%) PMPM: $1, 414 PMPY: $16, 966 Average MM: 10. 44 Members Not Eligible N = 1, 723 (19%) Eligible Members W/O Claims$ N = 146 (2%)
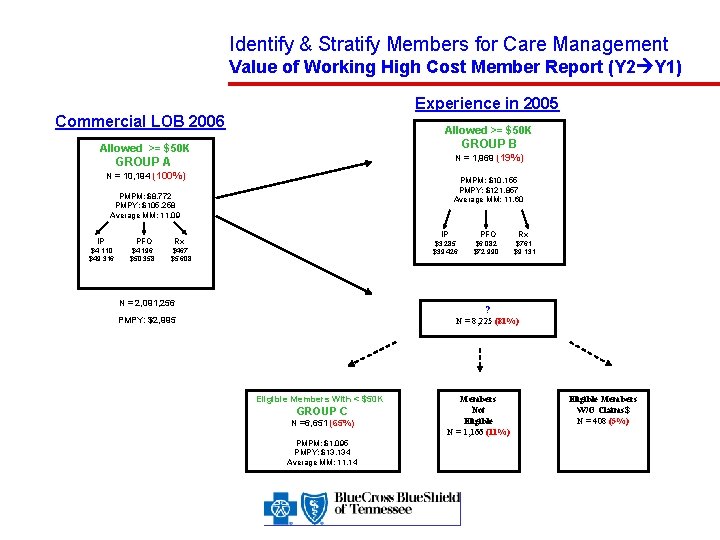
Identify & Stratify Members for Care Management Value of Working High Cost Member Report (Y 2 Y 1) Experience in 2005 Commercial LOB 2006 Allowed >= $50 K GROUP B Allowed >= $50 K N = 1, 969 (19%) GROUP A N = 10, 194 (100%) PMPM: $10, 155 PMPY: $121, 857 Average MM: 11. 60 PMPM: $8, 772 PMPY: $105, 258 Average MM: 11. 09 IP PFO Rx $4, 110 $49, 316 $4, 196 $50, 358 $467 $5, 608 N = 2, 091, 256 IP PFO Rx $3, 285 $39, 426 $6, 082 $72, 990 $761 $9, 131 ? PMPY: $2, 995 N = 8, 225 (81%) Eligible Members With < $50 K GROUP C N =6, 651 (65%) PMPM: $1, 095 PMPY: $13, 134 Average MM: 11. 14 Members Not Eligible N = 1, 166 (11%) Eligible Members W/O Claims$ N = 408 (5%)
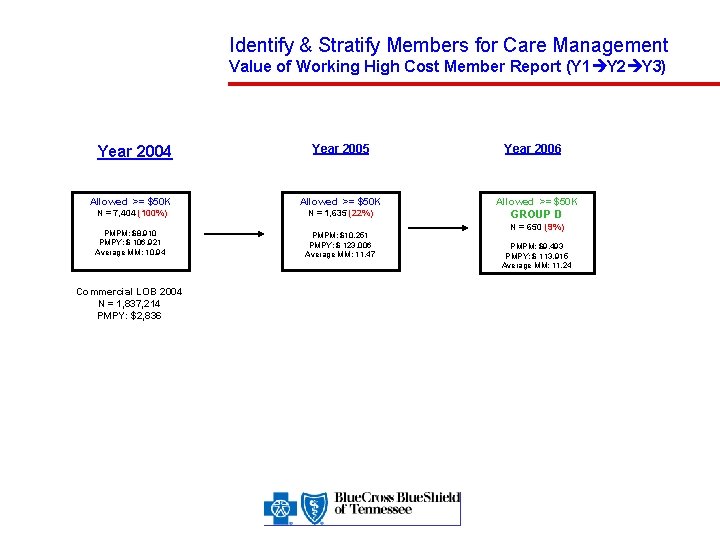
Identify & Stratify Members for Care Management Value of Working High Cost Member Report (Y 1 Y 2 Y 3) Year 2004 Year 2005 Allowed >= $50 K N = 7, 404 (100%) N = 1, 635 (22%) PMPM: $8, 910 PMPY: $ 106, 921 Average MM: 10. 94 Commercial LOB 2004 N = 1, 837, 214 PMPY: $2, 836 PMPM: $10, 251 PMPY: $ 123, 006 Average MM: 11. 47 Year 2006 Allowed >= $50 K GROUP D N = 650 (9%) PMPM: $9, 493 PMPY: $ 113, 915 Average MM: 11. 24
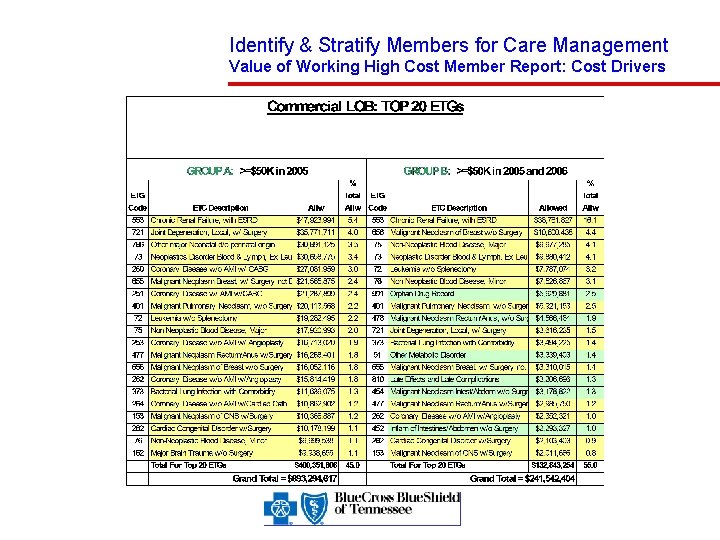
Identify & Stratify Members for Care Management Value of Working High Cost Member Report: Cost Drivers
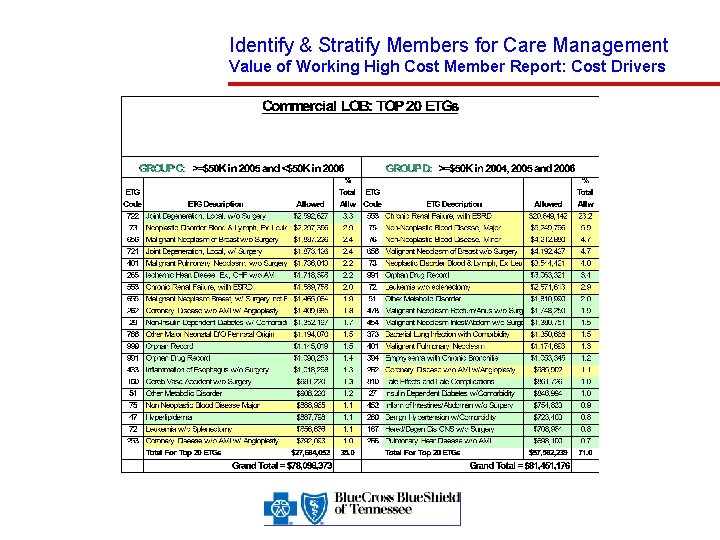
Identify & Stratify Members for Care Management Value of Working High Cost Member Report: Cost Drivers

Identify & Stratify Members for Care Management Developing a Stratification Index (SI) • Why? • 1) To reliably identify higher cost, highly impactable members • 2) To enhance prioritization of members for nurse-intervention management • How? • Use predictive output from MEDai • Select key MEDai measures to construct a composite score • Use the composite score as an index to stratify members Focus on members with the highest index scores
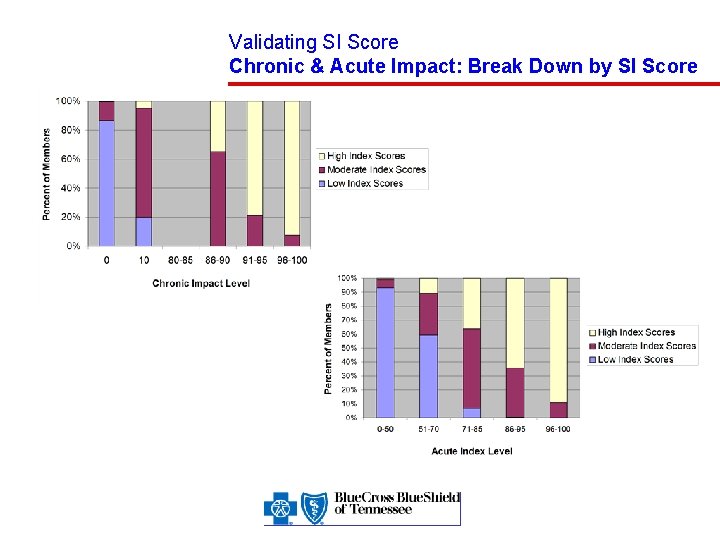
Validating SI Score Chronic & Acute Impact: Break Down by SI Score
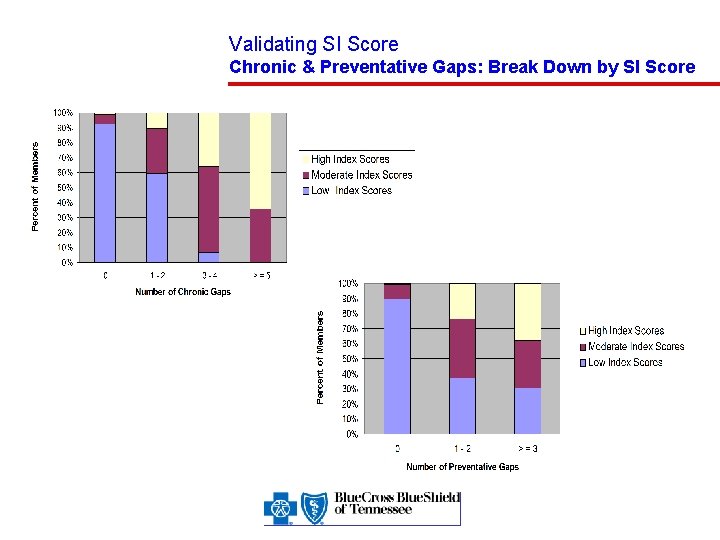
Validating SI Score Chronic & Preventative Gaps: Break Down by SI Score
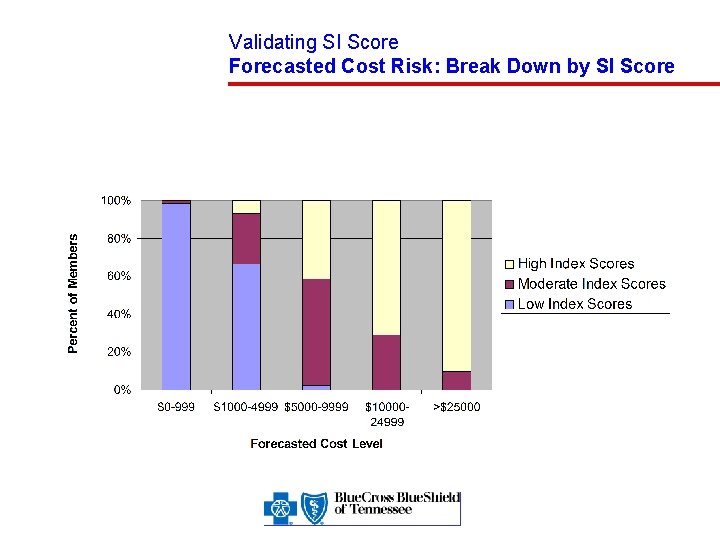
Validating SI Score Forecasted Cost Risk: Break Down by SI Score

Validating SI Score Mover Identification • Movers are members who are likely to make the transition from low or moderate to high risk • Movers can be identified by comparing current vs. forecasted cost risk level • if a member’s current cost is less than $1, 000 (Risk Level I) and is predicted to cost more than $25, 000 (Risk Level V) • Do movers have higher index scores?
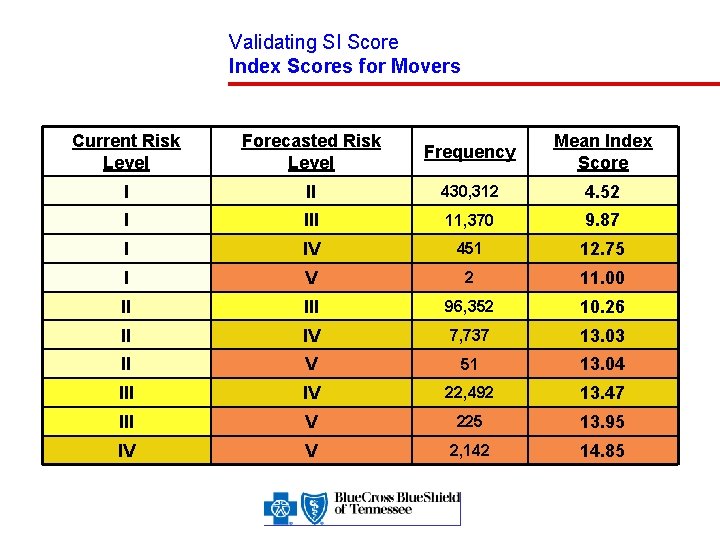
Validating SI Score Index Scores for Movers Current Risk Level Forecasted Risk Level Frequency Mean Index Score I II 430, 312 4. 52 I III 11, 370 9. 87 I IV 451 12. 75 I V 2 11. 00 II III 96, 352 10. 26 II IV 7, 737 13. 03 II V 51 13. 04 III IV 22, 492 13. 47 III V 225 13. 95 IV V 2, 142 14. 85
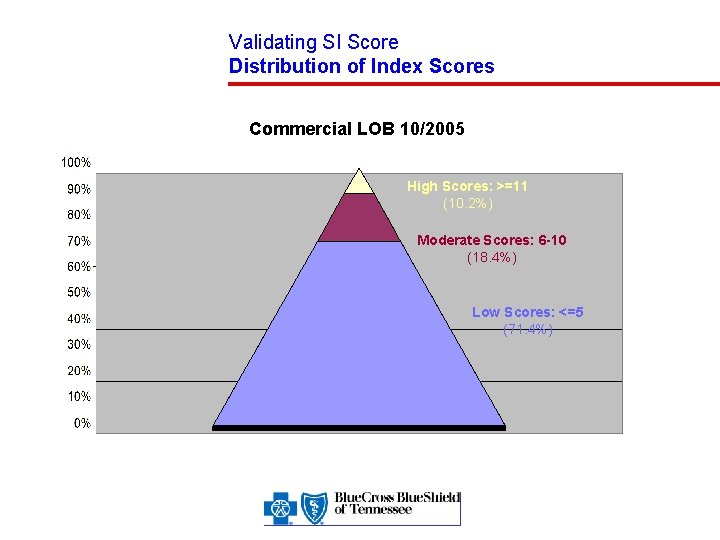
Validating SI Score Distribution of Index Scores Commercial LOB 10/2005 High Scores: >=11 (10. 2%) Moderate Scores: 6 -10 (18. 4%) Low Scores: <=5 (71. 4%)

Care Management Challenges: Triage & Intervene Members for Care Management Needs Care Management Model

Care Management Model Lifestyle/Health Counseling for Healthy and Worried Well • Information on disease/condition – Web resources – Pamphlets – Telephonic health library – 24/7 Nurse Line – HRA/PHR • Encouragement to take more active role/accountability

Care Management Model Care Coordination for Chronically Ill • Telephonic coordination with members and their providers • Ensures appropriate treatments and pharmaceuticals • Five different programs included in this model

Care Management Model Care Coordination Programs • Pharmacy Care Management • Emergency Room (ER) Visits Mgmt. • Transition of Care • Condition Specific Care Coordination • Disease Management

Care Management Model Catastrophic Case Management • Directed to members with – – – Terminal illness (HOPE) Major trauma Cognitive/physical disability High-risk condition Complicated care needs • Systematic process of assessing, planning, coordinating, implementing, and evaluation of care

Triage & Intervene Members for Care Management Needs Implementation • Predictive modeling using – MEDai, DCG, ETG • Rolling 12 months DCG explanation prospective model • ETG cost to supplement MEDai prediction • Developed SQL database containing MEDai, DCG, and ETG information • Improved processes/workflow • Easy and continuous access • Better documentation
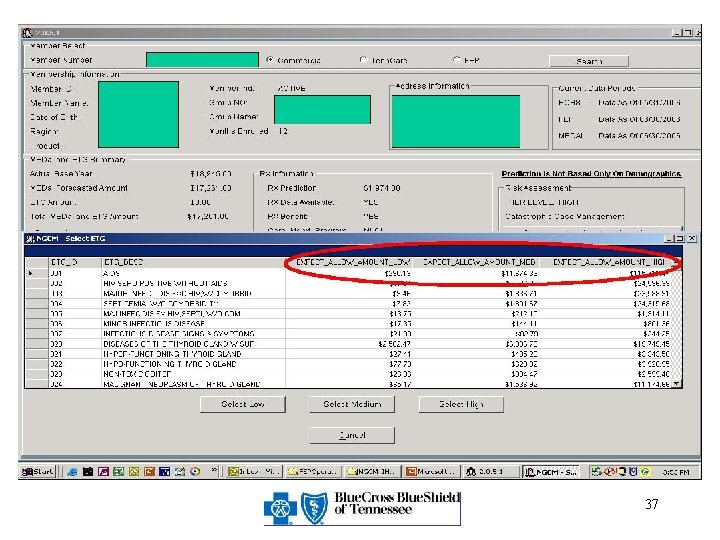
37
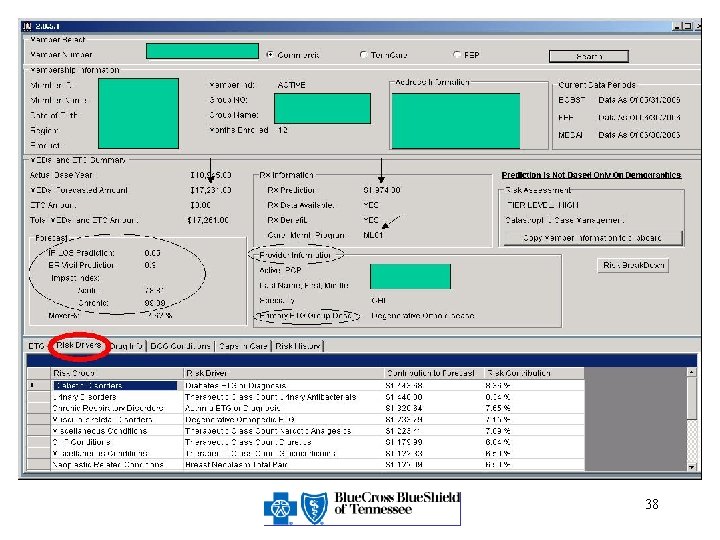
38
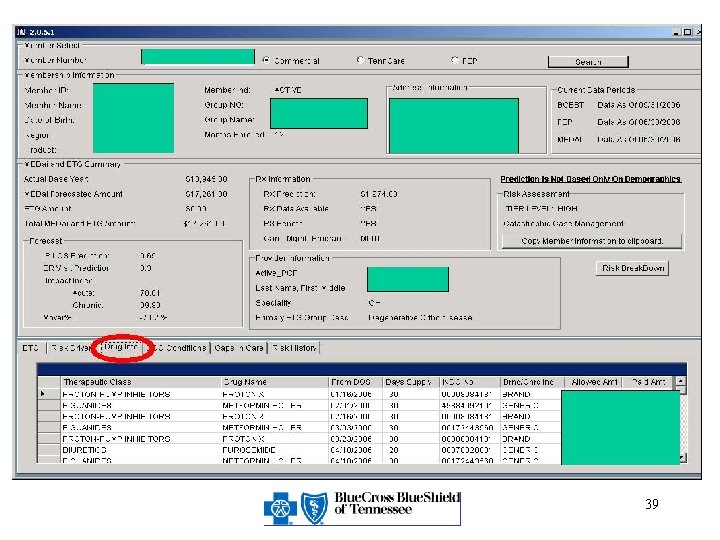
39
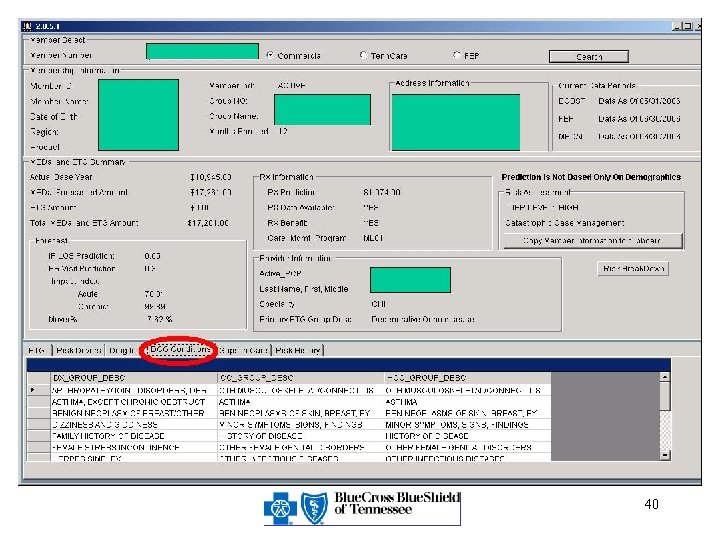
40
41
42
43

Triage & Intervene Members for Care Management Needs Implementation: Future Enhancements • Accreditation Analytics • Member non-compliance for HEDIS measures • Satisfaction profile • Geo-spatial Analytics (imputed race, vicinity to Centers of Excellence (COE) or efficient/quality providers) • Data Mining Analytics • Probability of engagement, segmentation profile • Psychosocial Profile • Speech Analytics • Indirect Cost Profile

Care Management Challenges: Evaluate Care Management Interventions • Basic research problem: measuring what would have happened vs. what actually happened • Methodologies: • Randomized Control Group • Population-Based Pre-Post Methodology • Predictive Modeling • Control Group Matching • Combination

Evaluate Care Management Interventions Predictive Modeling Group's Inflation Factor CM Mbrs Actual PMPM CM Mbrs Predictive Modeling PMPM 5% 7% $ $ $ 574 629 659 $ $ $ 542 638 682 CM Savings PMPM $ 85 $ 140 Total CM Savings Admin Cost $ $ 42, 005 29, 399 Inflated CM Mbrs Predictive Modeling PMPM $ 99, 560 $ 26, 749

Evaluate Care Management Interventions Predictive Modeling w/Adjustments Non CM Mbrs Actual PMPM Non CM Mbrs PMPM Predictive Modeling Inflation Adjusted Non CM Mbrs PMPM Predictive Modeling Adjustment for Actual to Predictive Modeling $ $ $ 225 205 214 5% $ $ $ 217 232 248 -13% CM Mbrs Actual PMPM CM Mbrs Predictive Modeling PMPM Inflated CM Mbrs Predictive Modeling PMPM Adjusted Predictive Model $ $ 574 629 659 692 $ $ 542 638 682 597 Adjusted CM Savings PMPM Adjusted CM Savings Admin Cost Adjusted Net Savings Adjusted ROI $ $ 117 57, 819 29, 399 28, 296 1. 96 $ $ 55 39, 113 26, 749 12, 364 1. 46
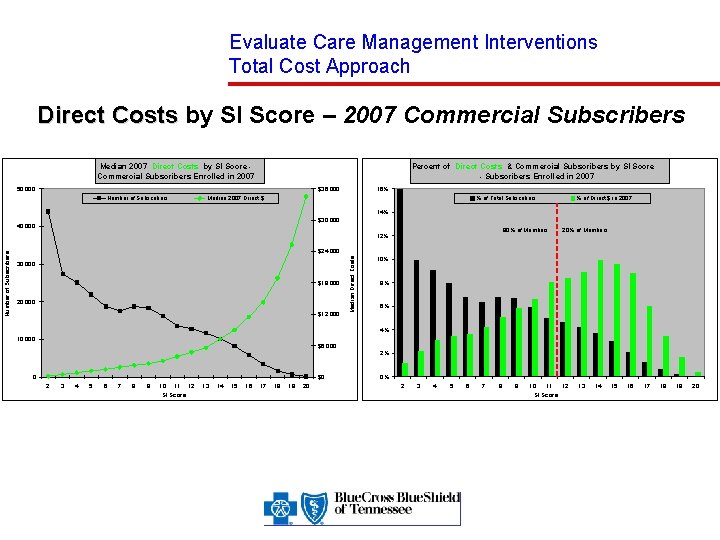
Evaluate Care Management Interventions Total Cost Approach Direct Costs by SI Score – 2007 Commercial Subscribers Percent of Direct Costs & Commercial Subscribers by SI Score - Subscribers Enrolled in 2007 Median 2007 Direct Costs by SI Score Commercial Subscribers Enrolled in 2007 50, 000 $36, 000 Number of Subscribers 16% Median 2007 Direct $ % of Total Subscribers % of Direct $ in 2007 14% $30, 000 40, 000 80% of Members 20% of Members $24, 000 30, 000 $18, 000 20, 000 $12, 000 Median Direct Costs Number of Subscribers 12% 10% 8% 6% 4% 10, 000 $6, 000 2% 0 $0 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20 0% 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20
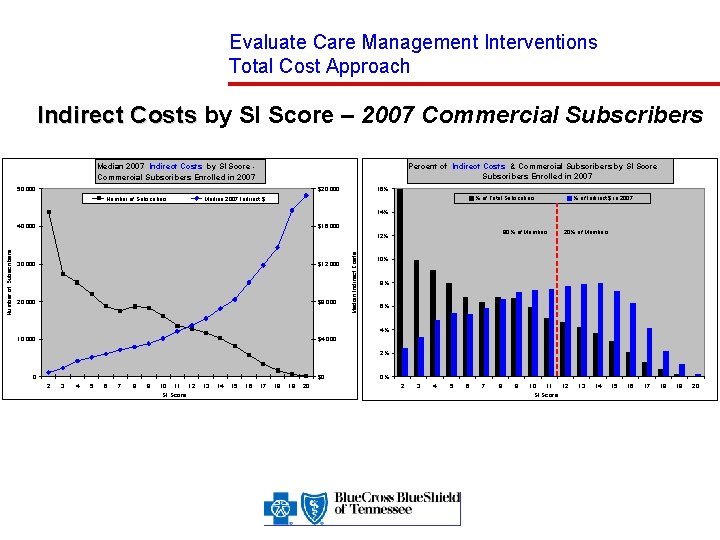
Evaluate Care Management Interventions Total Cost Approach Indirect Costs by SI Score – 2007 Commercial Subscribers Percent of Indirect Costs & Commercial Subscribers by SI Score Subscribers Enrolled in 2007 Median 2007 Indirect Costs by SI Score Commercial Subscribers Enrolled in 2007 50, 000 16% $20, 000 Number of Subscribers % of Total Subscribers Median 2007 Indirect $ % of Indirect $ in 2007 14% 40, 000 $16, 000 80% of Members 30, 000 $12, 000 20, 000 $8, 000 10, 000 $4, 000 Median Indirect Costs Number of Subscribers 12% 20% of Members 10% 8% 6% 4% 2% 0 $0 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20 0% 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20
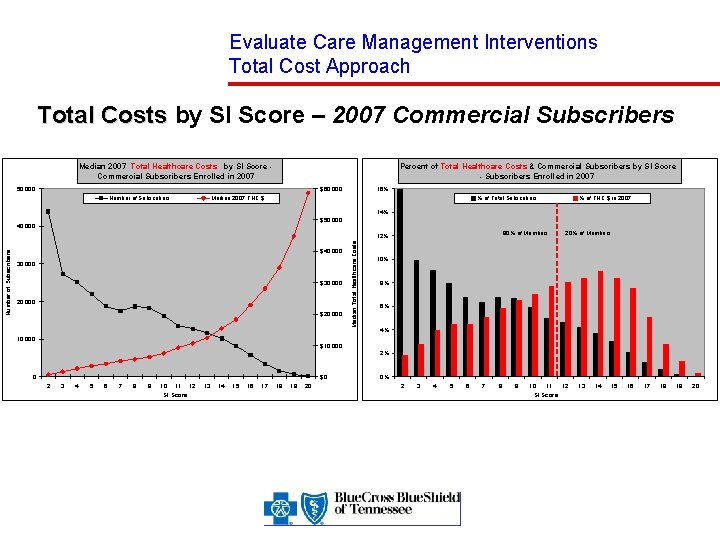
Evaluate Care Management Interventions Total Cost Approach Total Costs by SI Score – 2007 Commercial Subscribers Median 2007 Total Healthcare Costs by SI Score Commercial Subscribers Enrolled in 2007 Percent of Total Healthcare Costs & Commercial Subscribers by SI Score - Subscribers Enrolled in 2007 50, 000 $60, 000 Number of Subscribers 16% Median 2007 THC $ % of Total Subscribers % of THC $ in 2007 14% $50, 000 40, 000 80% of Members $40, 000 30, 000 $30, 000 20, 000 $20, 000 10, 000 Median Total Healthcare Costs Number of Subscribers 12% 20% of Members 10% 8% 6% 4% $10, 000 2% 0 $0 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20 0% 2 3 4 5 6 7 8 9 10 11 12 SI Score 13 14 15 16 17 18 19 20
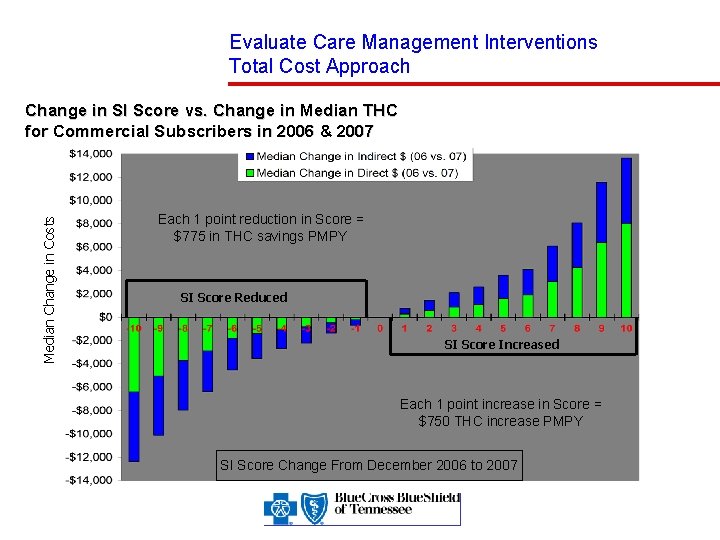
Evaluate Care Management Interventions Total Cost Approach Median Change in Costs Change in SI Score vs. Change in Median THC for Commercial Subscribers in 2006 & 2007 Each 1 point reduction in Score = $775 in THC savings PMPY SI Score Reduced SI Score Increased Each 1 point increase in Score = $750 THC increase PMPY SI Score Change From December 2006 to 2007

Conclusions • • More scientific/standardized approach Able to touch more lives efficiently Well accepted by our care managers PM approach has helped – Streamline our processes – Better manage case managers case load • Provide “Peace of Mind” to our members and clients
- Slides: 52