Precocious Puberty Insights in Management Katrina L Parker

Precocious Puberty Insights in Management Katrina L. Parker, MD Pediatric Endocrinology Morehouse School of Medicine


Precocious Puberty l At the end of the presentation participants: l Will be able to define puberty l Will be able to define precocious puberty and its causes l Be able to describe types of treatment for precocious puberty l Describe problems associated with precocious puberty


Landmark Case of Precocious Puberty l 5 year old Lina Medina of Peru – Menses onset age 8 months – Breast development age 4 – Advanced bone maturation age 5 – Was evaluated for abdominal tumor due to increasing abdominal size at age 5 – On 5/14/1939 gave birth to a 2. 9 kg baby boy

Puberty l The process of physical maturation manifested by an increase in growth rate and the appearance of secondary sexual characteristics l Results in the individual having the capacity to reproduce l Changes are a result of ↑gonadotropin & sex steroid secretion

Mechanism of Puberty Gn. RH stimulates pituitary gonadotropins (LH & FSH) l During childhood pubertal Gn secretion is initially low due to downregulation l Negative feedback of hypothalamic-pituitarygonadal axis l As puberty progresses, episodic release of LH l – Increased amplitude & frequency – Progressive secretion extends over the 24 hr period l Mechanism of why puberty occurs is unknown
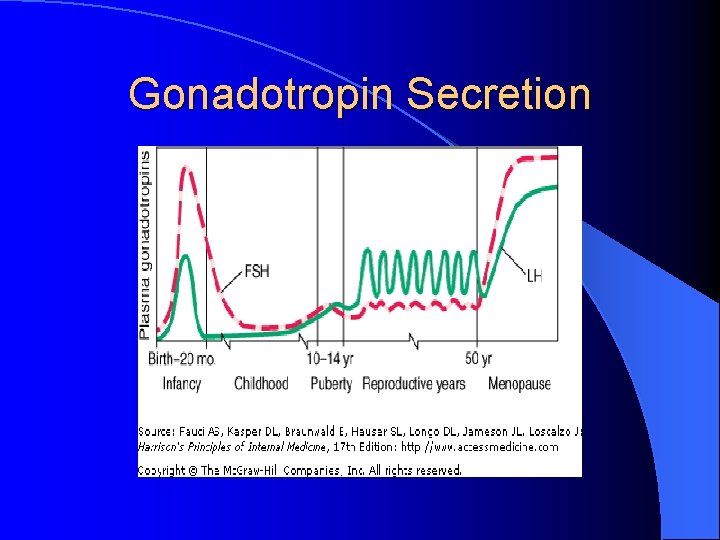
Gonadotropin Secretion
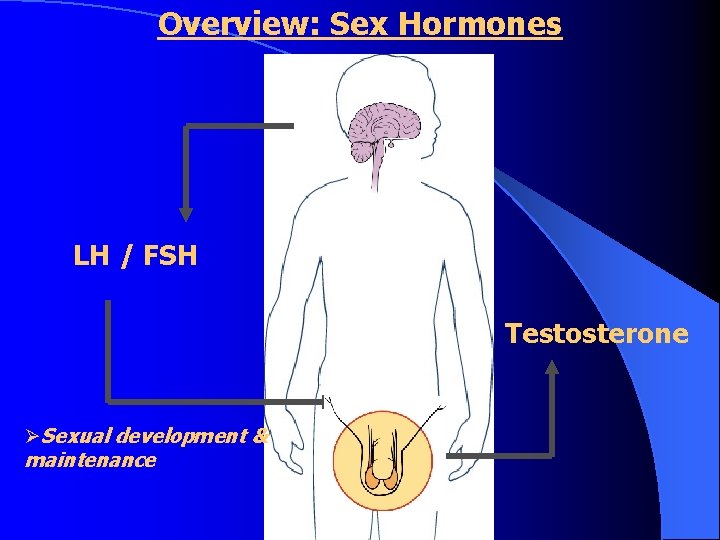
Overview: Sex Hormones LH / FSH Testosterone ØSexual development & maintenance
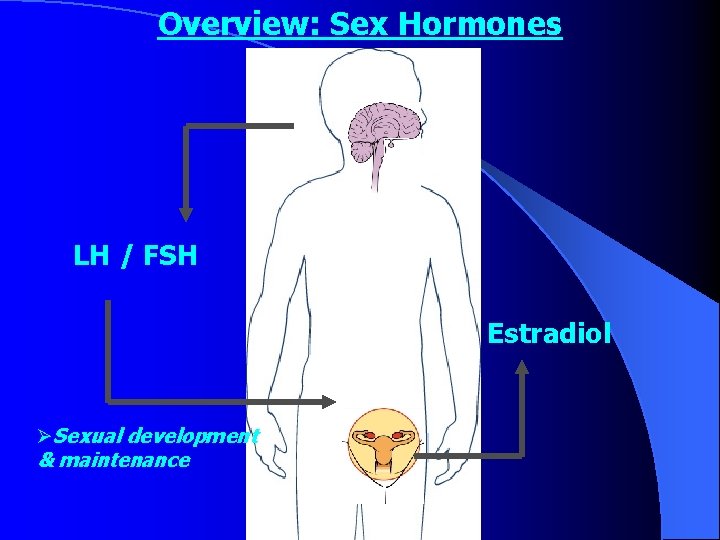
Overview: Sex Hormones LH / FSH Estradiol ØSexual development & maintenance

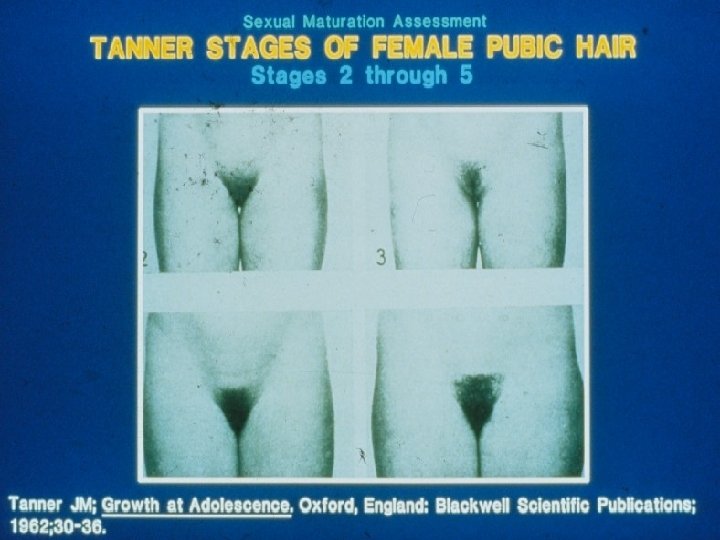
Pubertal Development l Puberty is divided into five Tanner Stages – Each stage represents the extent of testicular enlargement and pubic hair growth in males l The appearance of thelarche and pubic hair growth in girls l

Normal Puberty l Traditionally had been defined as the appearance of any secondary sexual maturation after the age of 8 in girls and 9 years in boys

Progression of Puberty l May progress very slowly l In short burst with no visible change in overall l The earlier the onset, the slower the tempo

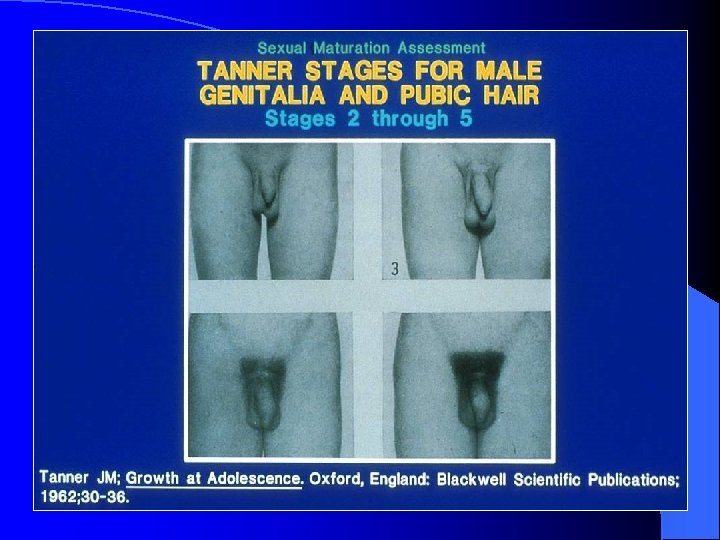
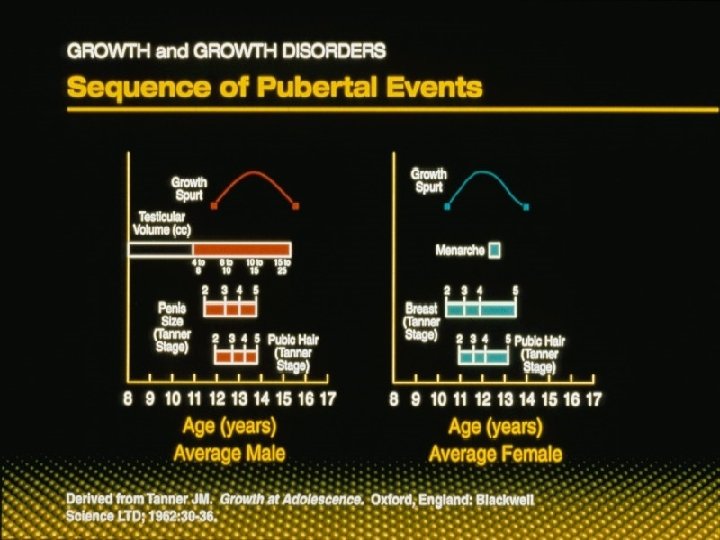
Normal puberty l In males – First sign of puberty is enlargement of testicular volume – Followed by the appearance of pubic hair and accumulation of lean body mass – Growth spurt is noted toward the end of their sexual maturation (late TS III or early TS IV)

PUBERTY AVERAGE of ONSET: 1. GIRLS 10 to 11 years (range 8 to 13 years) 2. BOYS 11 to 12 years (range 9 to 14 years)

PUBERTY INITIAL SIGNS OF PUBERTY: 1. GIRLS – Breast Development 2. BOYS – Testicular Enlargement § Volume > 3. 0 cm³ § Length > 2. 5 cm

Problems with The Definition of Puberty l In girls – Breast development maybe difficult to assess using visual inspection – Discerning breast from fat tissue is a key concern in overweight girls – Key- palpate under the aerolar

Problems with The Definition of Puberty (cont) l In boys – First sign of puberty is noticed – Need to compare testicular volume with orchidometer
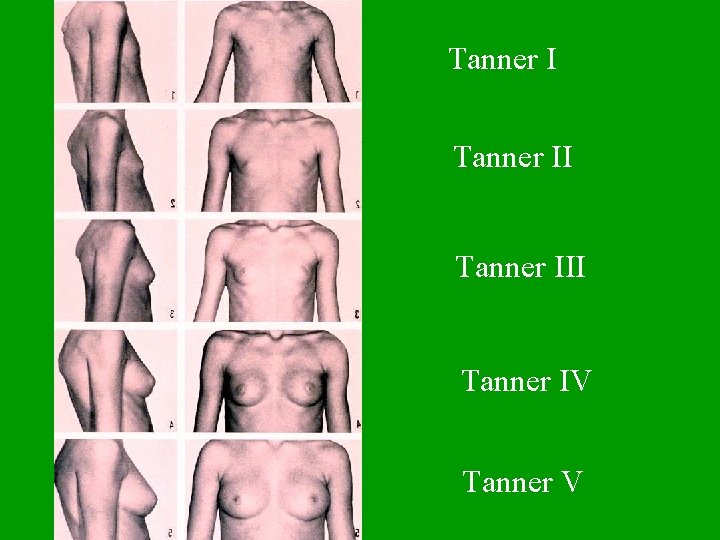
Tanner III Tanner IV Tanner V
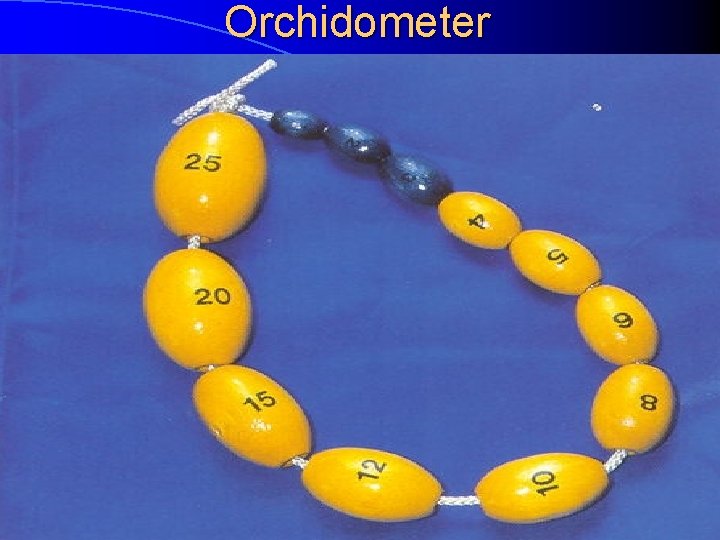
Orchidometer

Factor That Affect Puberty l Genetics l Race/Ethnicity l Previous nutrition l Subcutaneous fat l Birth weight

Factors That Affect Puberty l Exposure – PCB in utero l Girls started puberty earlier – Elevated levels of phthalates l Puerto Rico outbreak in the 1980 s & 1990 s l Obesity – Increased leptin and estrogen production – Insulin stimulation of ovaries & uterus
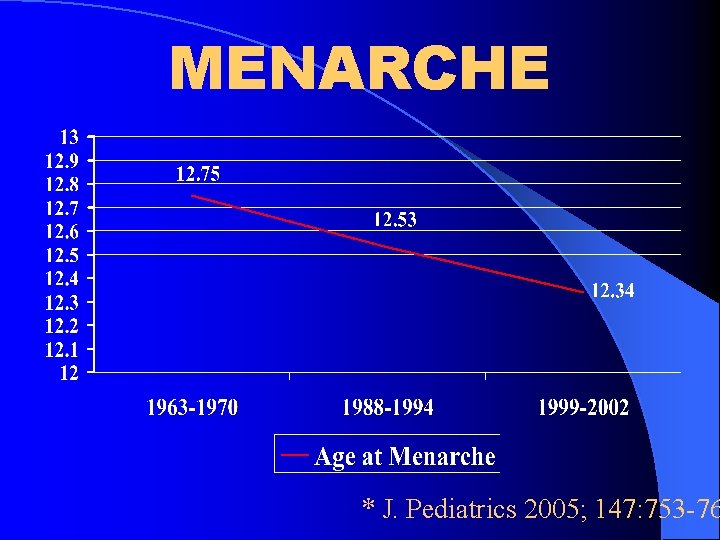
MENARCHE * J. Pediatrics 2005; 147: 753 -76

Are Children Entering Puberty Earlier? l Expert panel convened to settle a debate l Are data sufficient to establish or suggest a secular trend in the timing of puberty onset and/or progression? l Data from 1940 -1994 was evaluated

l Conclusions from data analysis have not been consistent – Limited data comparability among studies – Different populations – Different time periods – Studies used different methods

Pediatric Research In Office Setting l In 1997, a survey was conducted in 225 clinicians in pediatric practices l Pediatricians rated the amount of sexual maturation on girls undergoing complete physical examinations

Results l Data was analyzed on 17, 077 girls 9. 6% were AAF – 90. 4% were CF – l Results: 1% of CF & 3% of AAF are TS II pubic hair by age 3 – 6. 7% of CF & 27. 2% of AAF are TS II by age 7 – 14. 7% of CF & 48. 3% of AAF are TS II by age 8 –

Results (cont. ) l The mean age for onset of pubic hair development was – 8. 78 years for AAF and 10. 51 years for CF l The mean age for menses was – 12. 16 years for AAF and 12. 88 years for CF l The mean age of onset of breast development was age – 8. 87 years for AAF and 9. 96 years for CF
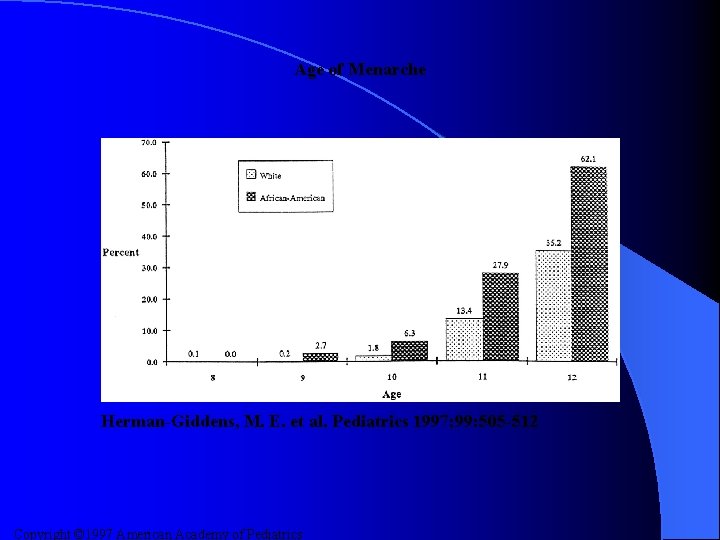
Age of Menarche Herman-Giddens, M. E. et al. Pediatrics 1997; 99: 505 -512 Copyright © 1997 American Academy of Pediatrics
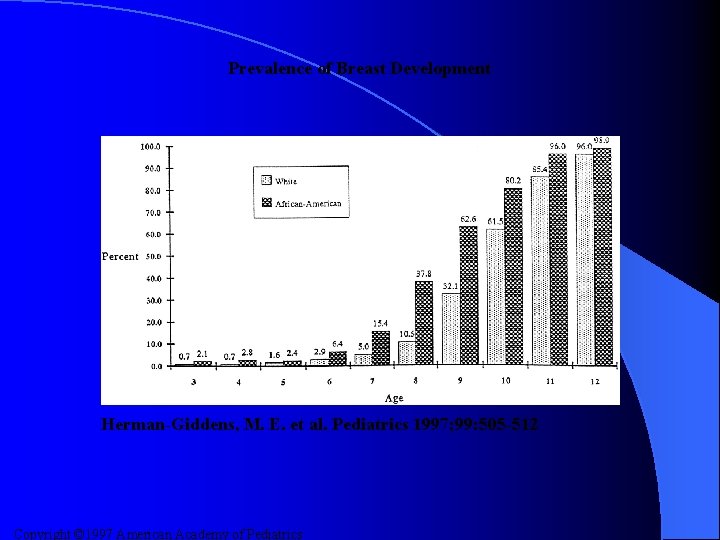
Prevalence of Breast Development Herman-Giddens, M. E. et al. Pediatrics 1997; 99: 505 -512 Copyright © 1997 American Academy of Pediatrics
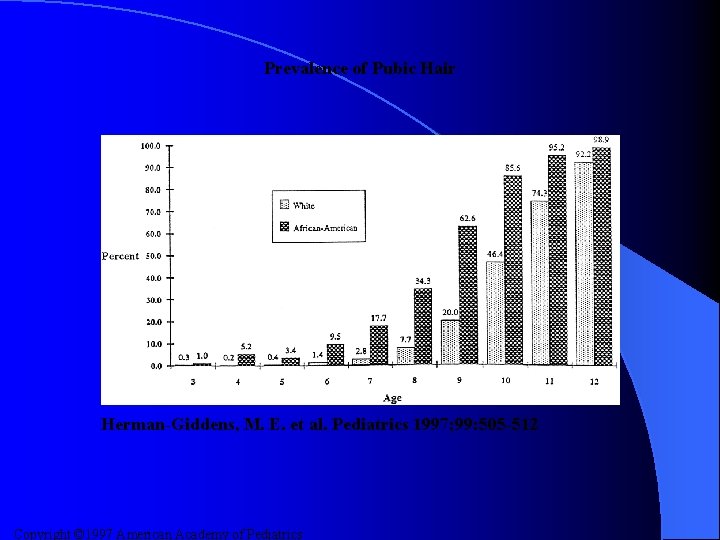
Prevalence of Pubic Hair Herman-Giddens, M. E. et al. Pediatrics 1997; 99: 505 -512 Copyright © 1997 American Academy of Pediatrics

Conclusions l Lead to new guidelines that changed the definition of precocious puberty l Breast development and pubic hair are occurring significantly earlier than suggested

Lawson Wilkins Pediatric Endocrine Society l Recommendations: – Breast development before 7 years in Caucasians and age 6 in African-Americans is considered precocious – Warrants evaluation There are no comparable data published in boys l No change in the recommended age that boys be evaluated l

LWPES Guidelines l Use these guidelines ONLY in healthy girls with no signs of neurological or other disease that may pathologically advance puberty.

LWPES Recommendations l In boys – Fewer data are available on ages and patterns of pubertal development – ? Lower interest in studying male puberty – ? May reflect less cultural awareness


Precocious Puberty l When puberty begins early & progresses early l Onset is occurring earlier l Traditional definition – Onset < age 8 in girls – Onset < age 9 in boys Idiopathic type is the most common l Height age, weight age and bone age all advanced l Early closure of epiphyseal growth plates results in adult short stature below genetic potential l

Precocious Puberty l Gonadotropin-dependent – Involves the premature activation of the hypothalamic- pituitary-gonadal axis l Gonadotropin-independent – Secretion of sex steroids is independent of pituitary gonadotropin release l The prevalence – is estimated to be between one in 5, 000 to 10, 000 children annually in the United States.

Precocious Puberty l Isosexual – Appropriate for sex l Contrasexual or heterosexual – Appropriate sex for the opposite sex l This terminology is cumbersome l Use of feminization in males & masculinization in females should adequately designate these conditions

Differential Diagnosis of Gn. RHdependent precocious puberty Idiopathic l Constitutional l CNS lesions l – Hypothalamic hamartoma – Malignancies l l Astrocytoma Ependymoma Glioma (maybe assoc with NF Type 1) Pineal tumors

Differential Diagnosis (cont) l Miscellaneous – – – – l Significant head trauma CNS infections (meningitis, encephalitis, abscess) Empty sella syndrome Ventricular cysts Granulomas Prior CNS irradiation Congenital hydrocephalus De Morsier syndrome Secondary to Gn. RH-independent precocious puberty

Incomplete Gn. RH independent precocious puberty l Males – Gonadotropin secreting tumors – Excessive androgen production – Testicular tumors (choriocarcinoma) – Virilizing congenital adrenal hyperplasia – Premature Leydig and germinal cell maturation – Extragonadal (i. e hepatoblastoma, germ cell tumors) l Activating mutation of LH receptor

Incomplete Gn. RH independent precocious puberty (cont) l Females – Severe hypothyroidism – Ovarian cysts – Estrogen secreting neoplasm – Exposure to exogenous estrogen l Males and females – Mc. Cune Albright Syndrome

Incomplete Sexual Precocity l Females – Androgen secreting tumors – Virilizing congenital adrenal hyperplasia l Males – Estrogen secreting tumor
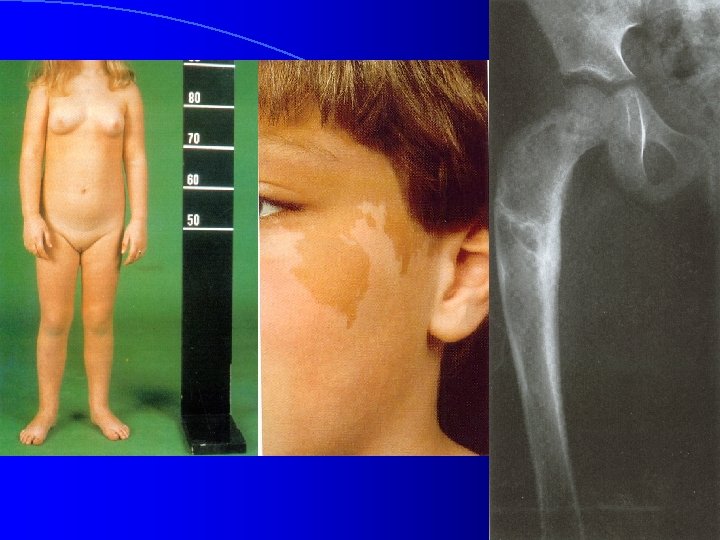
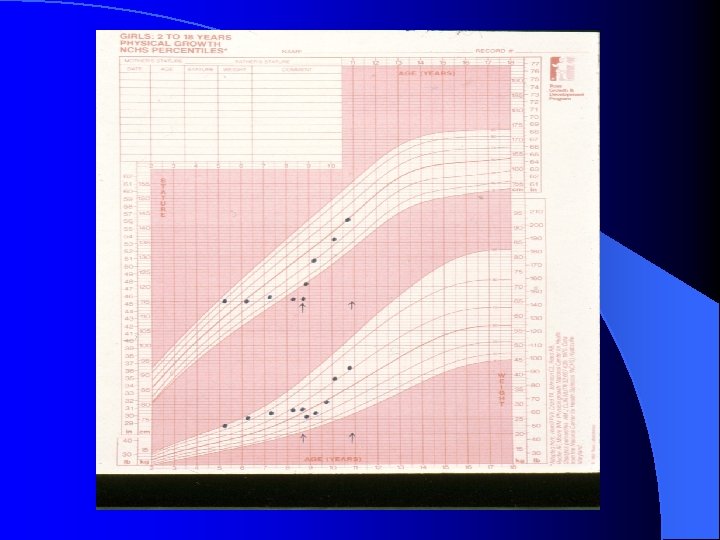
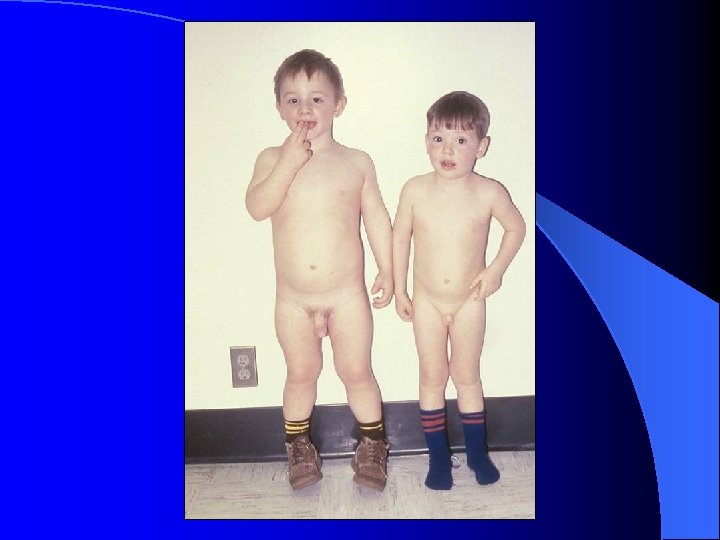

History l Age at onset of signs and symptoms Rate of progression l Growth velocity l l Family history l Hormone exposure l Previous or current CNS abnormalities l Gelastic seizures

Diagnostic Evaluation l History & physical exam – Height, weight, arm span, U/L ratio – Skin, hair, thyroid and neurological findings – Breast/pubic hair staging – Inspection of vaginal mucosa – Testicular/phallus size

Hormonal Testing l Baseline elevation of FSH and FSH response to Gn. RH provocative testing l LH levels are consistent with early puberty – LH/FSH ratio > 1. 0 l Estradiol/testosterone early pubertal range levels may rise to the

Testing (cont. ) l TSH l Plasma 17 -OH Progesterone, DHEAS l Other testing: – Bone age, skeletal survey – Pelvic ultrasound – MRI of the brain

In males l Same evaluation in females, except also obtain: – Testosterone – Beta hcg – Specialized testing for LH receptor mutation

Therapy l Treat the underlying cause l Gn. RH analogue – Lupron depot ped, leuprolide acetate – Histrelin acetete l Monitor therapy – Plasma estradiol/testosterone levels – Growth velocity – Breast/testicular size regression

Variations of Pubertal Puberty l Premature Adrenarche l Premature Thelarche l Premature menarche

Premature Adrenarche l Development of pubic hair before age of 7 years in Caucasian girls and age 6 in African American girls l ? Early maturation of the adrenal zona reticularis l Higher levels of basal and stimulated DHEA levels when compared to prepubertal children

Premature Adrenarche l Linear growth velocity and skeletal maturation is slightly advanced l Maybe associated acne and axillary odor l No evidence of systemic virilization l Exclude adrenal neoplasm and enzymatic defects

Premature adrenarche l History – Racial and ethnic background – History of IUGR, FH of NIDDM, HTN, PCOS higher risk group l 20% of patients with precocious puberty present with premature adrenarche l Obtain baseline bone age, androgens (DHEAS, androstenedione, 17 OH-P, free testosterone, fasting lipid panel, SHBG) l Radiographic imaging R/O CNS or adrenal pathology should be reserved in minority of cases

Premature adrenarche l Independent of the hypothalamic pituitary gonadal axis l Biochemical evidence is found as early as 6 years in normal children – Increased basal dehydroepiandrosterone sulfate (DHEAS) – Relative increase in ACTH l Mechanism is not known

Adrenarche l Adrenal androgens – Begin to rise at about 6 -8 years of age – Occurs approximately 2 years prior to an increase in pubertal gonadotropin pulses and increased pituitary Gn. RH sensitivity – Increase in DHEA and DHEAS production continues until age 14 -16

Premature Thelarche l Has been diagnosed during two age periods – During the first two years of life l caused by the persistent increased infant gonadotropin secretion l Development almost always regress before 24 months of age

Premature Thelarche (cont. ) l Second period – After 6 years of age – May be symmetric or asymmetric l Maybe a consequence of temporarily increased ovarian steroid secretion

Premature Thelarche l May be symmetrical or unilateral l Is not accompanied by other signs of puberty l Normal estrogen levels, and height l Bone age is normal or slightly advanced l Rare ovarian cyst l May be first sign of precocious puberty

Evaluation l Correct diagnosis – Idiopathic or pathologic l History – Any neurological diseases? Personality changes l Headaches or visual symptoms l – Drug exposure

Problems in Girls With Precocious Puberty Are taller than peers initially l Compared to their peers: l – Maybe more likely to have psychological problems – Unintended pregnancies – Higher rates of substance abuse Increased incidence of PCOS l ? Increased breast cancer risk l Unsure of the long term effects on bone mineral density l

l In Gn. RH dependent precocious puberty – Characterized by an acceleration of growth and bone maturation l Early growth manifests as tall stature for age l As bones continue to be exposed to sex steroids, growth plates mature and fuse – Result in overall decreased adult height

Physical examination l Findings on exam can further direct your evaluation – effects of androgens (acne, hirsuitism, increased muscle mass and clitromegaly)

l Minimum bone age determination – If advanced, pursue further evaluation l Gn. RH stimulation test

Treatment Options

Treatment l Gn. RH agonist – Desensitizes the pituitary – Blocks LH and FSH secretion – Prevents continued sexual development for the duration of the treatment l Growth may almost stop while on therapy l ± addition of growth hormone remains controversy

Gn. RH Agonist l Nona- or deca peptides that are structurally similar to endogenous Gn. RH l Are available as subcutaneous and intranasal preparations – Are given as daily or monthly depot injections – Lupron depot Ped, leuprolide acetate, or histrelin

Side effects of Gn. RH Agonist Usually mild l Therapy has been available for greater than 20 years l – Not possible to say there will be no long term complications in some patients l During therapy – Hot flashes, skin rashes – Pain at the injection site – Sterile abscess at the injection site in 10% of patients
Histrelin Implant Therapy for Precocious Puberty l 11 girls with CPP l Age at diagnosis: 6. 5 years (range 2 -9 years) l Gn. RH Stimulation Test – Peak LH 23 ± 28 miu/ml – Peak FSH 20 ± 25 miu/ml l All girls underwent implant placement

Histrelin Implant Study l Girls were divided into 2 Groups: – Group A: 6 girls were followed for 15 months after implant insertion – Group B: 5 girls had their implant removed after 9 months l Gn. RH Stimulation test were performed – Group A 6, 9, 12 & 15 months – Group B 6 & 9 months

Results l In all girls – Breast development regressed – Growth velocity decreased – Bone age advancement slowed – Basal Gn and stimulated response and estradiol levels were suppressed
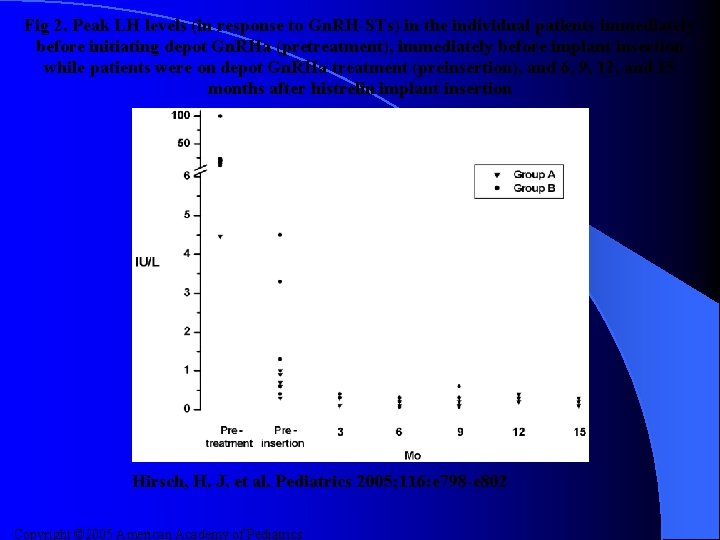
Fig 2. Peak LH levels (in response to Gn. RH-STs) in the individual patients immediately before initiating depot Gn. RHa (pretreatment), immediately before implant insertion while patients were on depot Gn. RHa treatment (preinsertion), and 6, 9, 12, and 15 months after histrelin implant insertion Hirsch, H. J. et al. Pediatrics 2005; 116: e 798 -e 802 Copyright © 2005 American Academy of Pediatrics
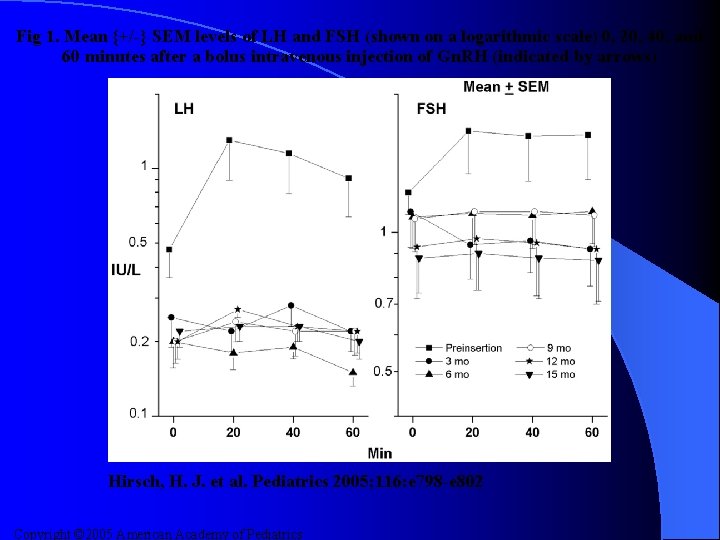
Fig 1. Mean {+/-} SEM levels of LH and FSH (shown on a logarithmic scale) 0, 20, 40, and 60 minutes after a bolus intravenous injection of Gn. RH (indicated by arrows) Hirsch, H. J. et al. Pediatrics 2005; 116: e 798 -e 802 Copyright © 2005 American Academy of Pediatrics

Supprelin® LA l SUPPRELIN® LA – Is 12 -month implant for treating central precocious puberty (CPP) – Was approved by the FDA in May, 2007 – Is inserted on the inner aspect of the upper arm

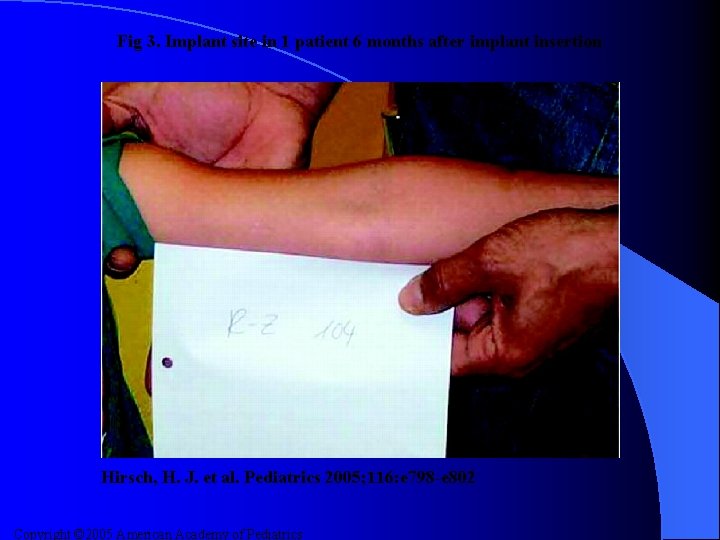
Fig 3. Implant site in 1 patient 6 months after implant insertion Hirsch, H. J. et al. Pediatrics 2005; 116: e 798 -e 802 Copyright © 2005 American Academy of Pediatrics

Side Effects of Histrelin Acetete l At the insertion site – Bruising – Pain – Swelling – Erythema – Soreness – in clinical signs of puberty during the first month

Contraindications of Histrelin Acetate l Not recommended – for usage < age 2 – Women who are pregnant or who become pregnant

Discontinuation of Therapy l l l l Age to discontinue therapy must be individualized Resumption of the hypothalamic-pituitary-gonadal axis begins promptly Menses resumes within 12 -18 months, up to 4. 5 yr Spermatogenesis resumes Documented pregnancy Little or no growth spurt Hyperandrogenism

Summary l Pubertal development is occurring earlier in children l Precocious puberty occurs more commonly in girls l The exact incidence of precocious puberty in males is unknown l Various treatment modalities are available to arrest pubertal development

QUESTIONS
- Slides: 87