Precocious Puberty H Delshad M D Endocrinologist PUBERTY


Precocious Puberty H. Delshad M. D Endocrinologist

PUBERTY It is a physiological phase lasting 2 to 5 years during which the genital organs mature

Precocious Puberty Is the onset of pubertal development at an earlier age than is expected based upon established normal standard Early onset of puberty before ► 8 years of age in girls ► 9 years of age in boys Several factors affect the age of onset of puberty: Familial pattern, environmental factors, ethnicity, chronic disease.
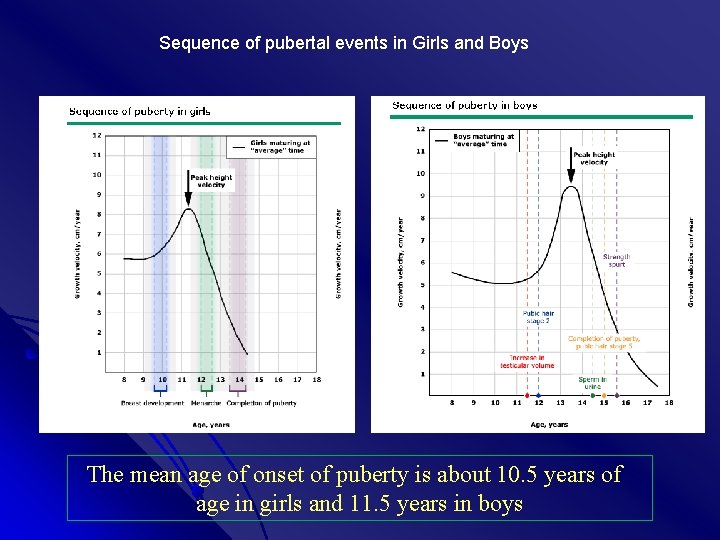
Sequence of pubertal events in Girls and Boys The mean age of onset of puberty is about 10. 5 years of age in girls and 11. 5 years in boys

Difficult to ascertain the early age limit because In a population-based study, breast and/or pubic hair development was present at age 8 in: l 48 percent of African-American l 15 percent of White girls. l At 7 years of age, the proportions were 27 and 7 percent, respectively. l 127. 0. 0. 1/contents/mobipreview. htm? 17/21/17756/abstract/7

Epidemiology The prevalence is difficult to estimate l It has been reported at 1 in 5000 children l In a population-based study that reviewed data from Danish national registries from 1993 to 2001, the incidence of precocious puberty was: ○ 20 per 10, 000 girls ○ < 5 per 10, 000 boys. l Teilmann G, et al. An epidemiologic study based on national registries. Pediatrics 2005; 116: 1323.

Epidemiology In the US: the number of girls diagnosed with precocious puberty is rising and its onset is decreasing: □Over the past 40 years: 0. 5 to 1. 0 years □With black girls maturing 0. 5 to 1. 0 year earlier than white girls. l Kaplowitz P. Pubertal development in girls: secular trends. Curr Opin Obstet Gynecol 2006; 18(5): 487 -91.
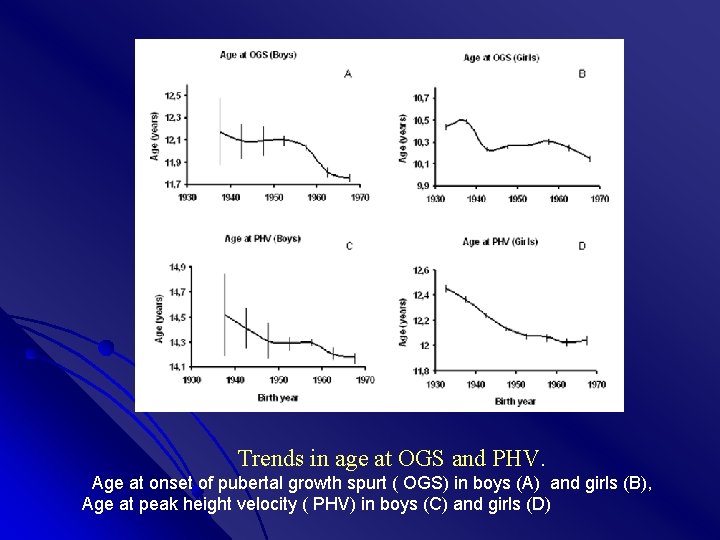
Trends in age at OGS and PHV. Age at onset of pubertal growth spurt ( OGS) in boys (A) and girls (B), Age at peak height velocity ( PHV) in boys (C) and girls (D)

Epidemiology l There is a strong female predominance of precocious puberty. Pescovitz OH , et al. The NIH experience with precocious puberty: Pediatr 1986; 108: 47. l In a retrospective review from a tertiary care l l center the female to male ratio was 23: 1. About half of the 197 girls and one quarter of the boys had GDPP. An etiology was found in all 16 boys and only in 6 girls (3 percent). Bridges NA, et al . Sexual precocity: sex incidence and aetiology. Arch Dis Child 1994; 70: 116.

Types: 1 - True precocious puberty 2 - Pseudo precocious puberty 3 - Incomplete precocious puberty

Central Precocious Puberty Idiopathic (90%) l Organic brain lesions: l Inflamation, Malformation Trauma Chemotherapy Radiotherapy Brain tumor: Hamartomas, Astrocytoma, Ependymoma, Pinealomas, Gliomas Hypothyroidism l Gain-of-function mutations in GPR 54 l

Gain-of-function mutations in GPR 54 The pathogenesis of ICPP is currently unclear. The kisspeptin/G protein‑coupled receptor 54 (GPR 54) signaling pathway initiates the onset of puberty, which is probably closely associated with the occurrence and development of ICPP. The early diagnosis of PP and evaluation of therapeutic effects is very important. Plasma kisspeptin levels rise at the initiation of pubertal development, and the kisspeptin levels of girls with PP decline following treatment with Gn. RH. Detection of kisspeptin can contribute to the early diagnosis of ICPP and may be used as an indicator of therapeutic effects in the treatment of precocious puberty.

Pseudo -Precocious puberty in Female l. Isosexual A girl who feminizes early is defined as having isosexual precocious puberty. l Heterosexual A girl who virilize early is defined as having heterosexual precocious puberty.

Pseudo -Precocious puberty in Female l Iso sexual ( feminizing ) conditions Mc cune – Albrightsyndrome Autonomous ovarian cyst Ovarian tumors Feminizing adrenocortical tumor Exogenous estrogens l Hetrosexual (masculinizing) Congenital adrenal hyperplasia Adrenal tumor Ovarian tumor Glucocorticoid receptor defect Exogenous androgens.

Pseudo -Precocious puberty in Male l. Isosexual A boy who virilize early is defined as having isosexual precocious puberty. l Heterosexual A boy who feminizes early is defined as having heterosexual precocious puberty.

Pseudo -Precocious puberty in Male l Isosexual Congenital adrenal hyperplasia Adrenocortical tumor Leydig cell tumor Familial male precocious puberty HCG secreting tumor Teratoma Glucocorticoid receptor defect Exogenous androgen l Hertrosexual Feminizing adrenocortical tumor Exogenous estrogens
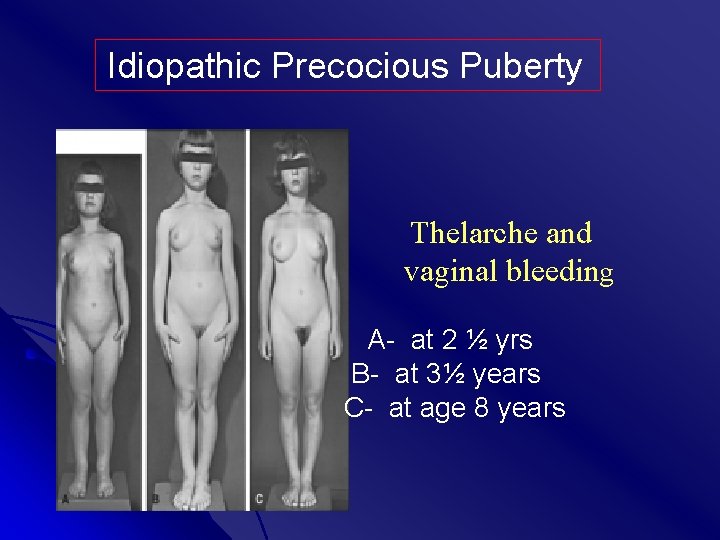
Idiopathic Precocious Puberty Thelarche and vaginal bleeding A- at 2 ½ yrs B- at 3½ years C- at age 8 years
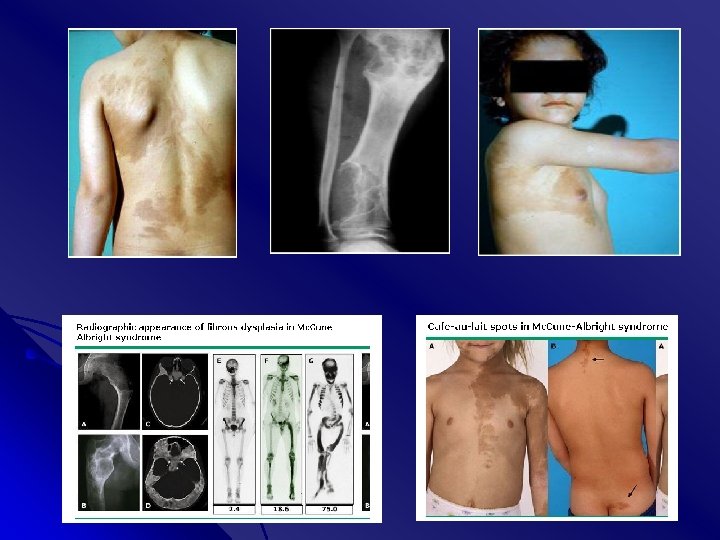
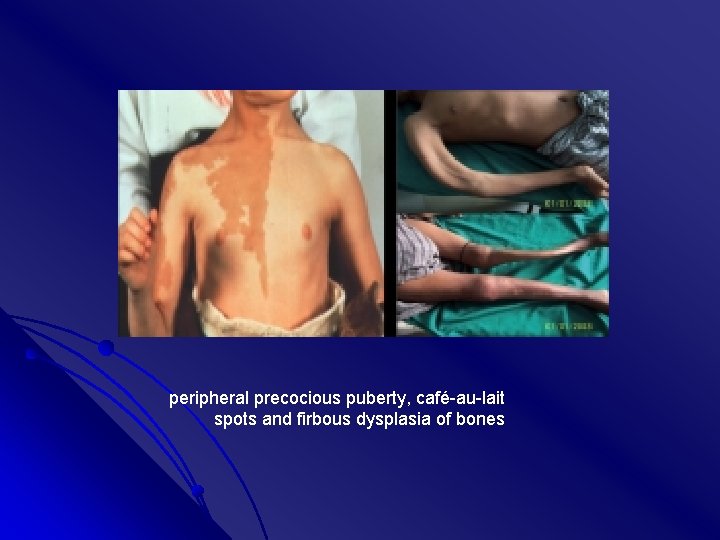
peripheral precocious puberty, café-au-lait spots and firbous dysplasia of bones
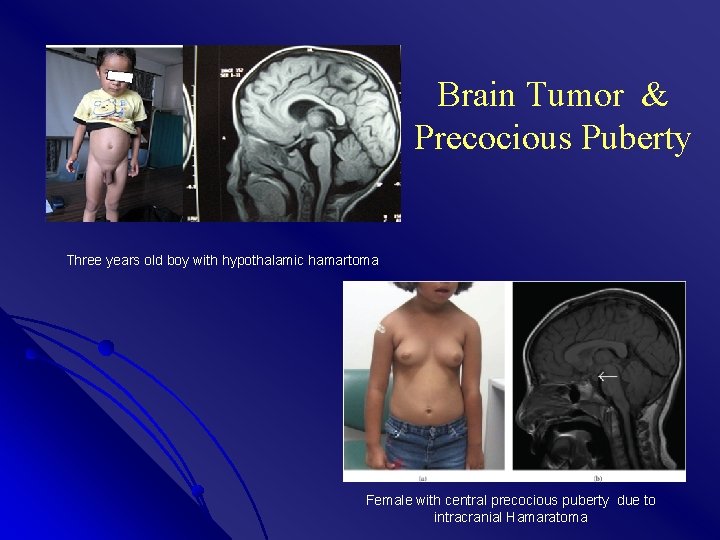
Brain Tumor & Precocious Puberty Three years old boy with hypothalamic hamartoma Female with central precocious puberty due to intracranial Hamaratoma
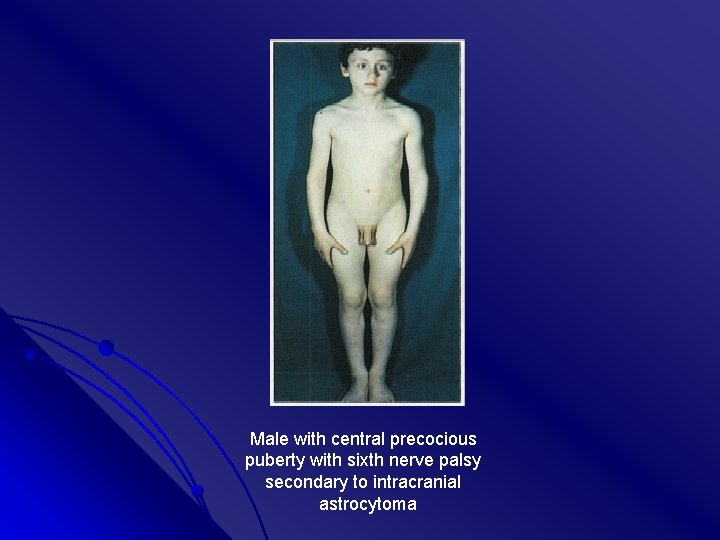
Male with central precocious puberty with sixth nerve palsy secondary to intracranial astrocytoma
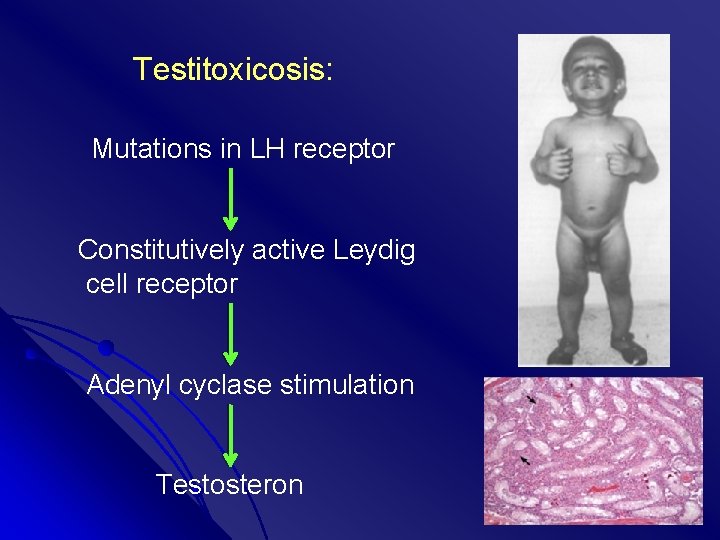
Testitoxicosis: Mutations in LH receptor Constitutively active Leydig cell receptor Adenyl cyclase stimulation Testosteron
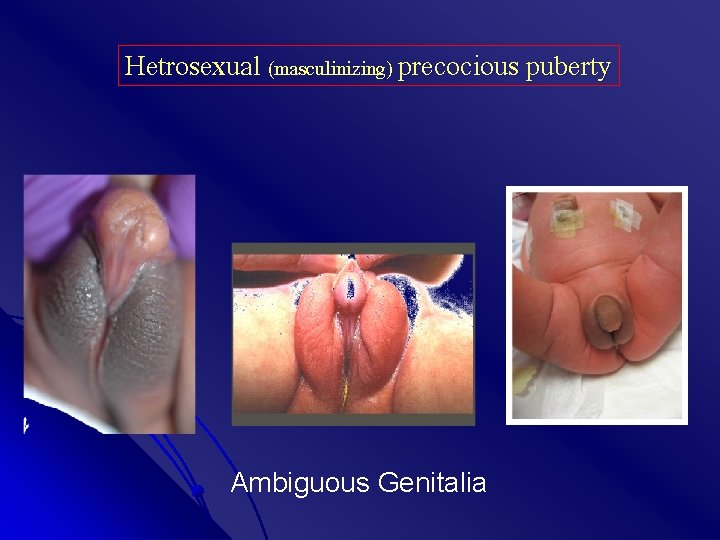
Hetrosexual (masculinizing) precocious puberty Ambiguous Genitalia

Incomplete Precocious Puberty Premature Thelarche Premature Pubarche Premature Adrenarche

Premature Pubarche l 50% of pt. with premature pubarche progress to PCOD l Late onset CAH may have a similar presentation l CPP can occur secondry to late Dx or inadequate Rx of CAH

Premature Menarche l Uncommon l Role out serious cause of bleeding l Neonatal period : withdrawal of estrogen produced by the fetoplacental unit l Childhood l Vulvovaginitis l Foreign body in the vagina l Trauma l Sexual abuse l Vaginal tumors

Approach to precocious puberty l. History l. Physical examination l. Laboratory l. Bone age l. Sonography l. MRI of brain

Diagnosis of precocious puberty 1. History: ● It excludes iatrogenic source of estrogen or androgen. ● It differentiates between isosexual and heterosexual precocious puberty. ● Onset & progression of symptom (N tempo CPP, Abrupt & rapid estrogen sec Tr) ● Hx of CNS trauma or infection ● Symptoms associated with neurological dysfunction ● Symptoms associated with endocrine dysfunction ● Exposure to exogenous steroids ● Hx of abdominal pain or swelling ● Family Hx early puberty, short stature

Diagnosis of precocious puberty 2. Physical examination: ● It diagnoses Mc. Cune-Albright syndrome. ● Neurologic and ophthalmologic examinations exclude organic lesions of the brain. ● Boys: Testes > 4 ml ● Girls: Breast development ● Pubic/axillary hair

Diagnosis of precocious puberty 3. Hormonal assay ●FSH, LH : Pubertal level in GDPP , Low in GIPP ●Sex hormones : Pubertal level in GDPP and in GIPP - Estradiol > 9 pg/ml -Testosterone : 20 – 1200 ng/dl ● Kisspeptin level ● 17α-hydroxy progesterone : elevates in CAH ●TSH : elevated in hypothyroidism ●h. CG : elevated in Germ cell tumors ●LHRH Test : pubertal response, LH > 7 IU/L in GDPP
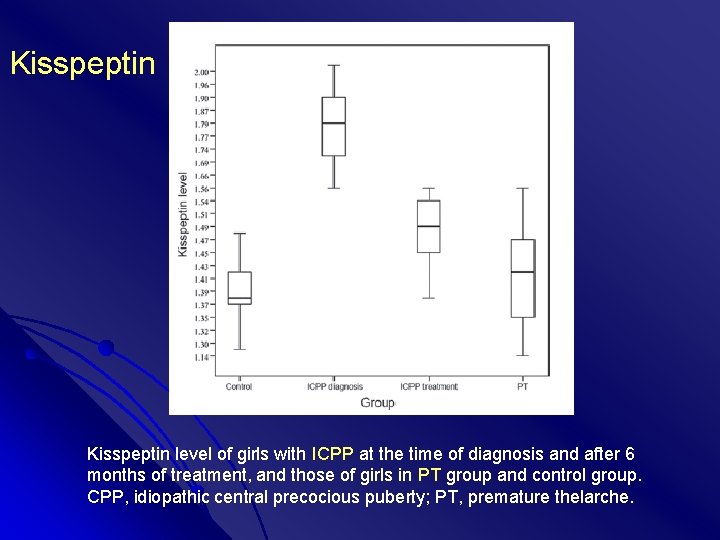
Kisspeptin level of girls with ICPP at the time of diagnosis and after 6 months of treatment, and those of girls in PT group and control group. CPP, idiopathic central precocious puberty; PT, premature thelarche.
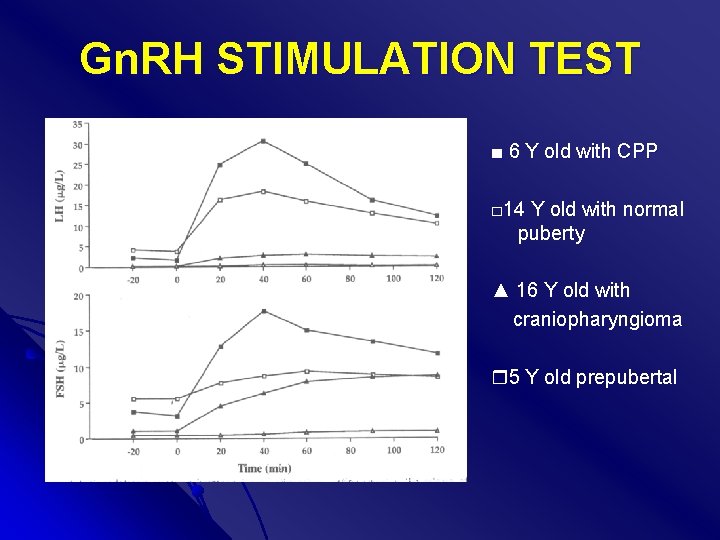
Gn. RH STIMULATION TEST ■ 6 Y old with CPP □ 14 Y old with normal puberty ▲ 16 Y old with craniopharyngioma 5 Y old prepubertal

Diagnosis of precocious puberty 4. X-ray examination To determine bone age : bone age> height age> chronological age Estrogen stimulates growth of bone but causes early fusion of the epiphysis. So the child is taller than her peers during childhood, but is short during adult life. Hypothyroidism is the only condition of precocious puberty in which bone age is retarded 5. Ultrasonography To diagnose ovarian or adrenal tumor. 6. CT or MRI To diagnose an organic lesion of the brain, or adrenal tumor.
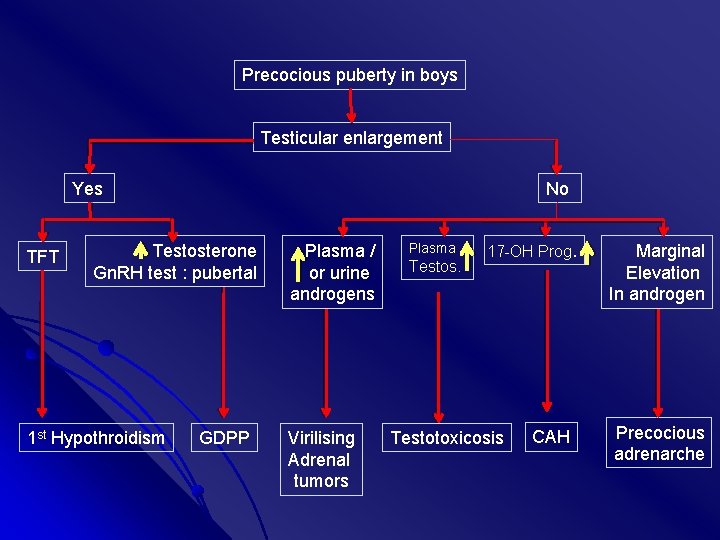
Precocious puberty in boys Testicular enlargement Yes TFT No Testosterone Gn. RH test : pubertal 1 st Hypothroidism GDPP Plasma / or urine androgens Virilising Adrenal tumors Plasma Testos. 17 -OH Prog. Testotoxicosis CAH Marginal Elevation In androgen Precocious adrenarche

Idiopathic precocious puberty: Is diagnosed after excluding all other causes.


Consensus Statement on the Use of Gn. RH Analogs in Children ESPE – LWPES Gn. RH Analogs Consensus Conference Group European Society for Pediatric Endocrinology(ESPE) Lawson Wilkins Pediatric Endocrine Society( LWPES) • 3 - days conference in Nov. 2007 • 30 participants from North America and Europe • Articles written in English with long-term outcome data published between 1990 and 2007 Pediatrics 2009; 123: e 752 -e 762

Use of Gn. RH for conditions other than CPP l Gonadal Protection for Children Undergoing Chemotherapy Routine use of Gn. RH as for gonadal protection in children undergoing chemotherapy cannot be suggested.

Use of Gn. RH for conditions other than CPP Increasing AH of Children With Idiopathic Short Stature Gn. RH therapy alone in children with ISS and normally timed puberty is minimally effective in increasing AH, may compromise BMD, and cannot be suggested for routine use. Combined Gn. RH and GH therapy leads to a significant height gain but may have adverse effects. Routine use of Gn. RH in children with ISS being treated with GH cannot be suggested. l

Use of Gn. RH for conditions other than CPP Increasing AH of Children Born Small for Gestational Age Routine use of the combination of Gn. RH and GH in children born SGA cannot be suggested. l Increasing AH of Children With Severe Hypothyroidism Routine use of combined therapy with Gn. RH and Levothyroxine cannot be suggested. l

Use of Gn. RH for conditions other than CPP Increasing AH of Children With GH Deficiency Routine use of combined therapy with Gn. RH and GH in GH-deficient children with low predicted AH at onset of puberty cannot be suggested. l Increasing AH of Children With Congenital Adrenal Hyperplasia Additional studies are needed to determine if Gn. RH therapy alone or in combination with GH should be used in children with CAH and low predicted AH. Routine use of Gn. RH for CAH cannot be suggested l
- Slides: 42