Prague Hepatology September 20 22 Prague Czech Republic

Prague Hepatology September 20 -22 Prague Czech Republic Critically ill patients with cirrhosis Professor Andrew K Burroughs FRCP FMed. Sci The Royal Free Sheila Sherlock Liver Centre and UCL Institute of Liver and Digestive Health

“CRITICALLY ILL PATIENTS with CIRRHOSIS” (CIC) v Clinical picture v Terminology v Sepsis v Heart and Circulation v Bleeding v Adrenal dysfunction v Renal failure v “Liver support devices” v Outcomes ITU v Prevention v Conclusions

CLINICAL PICTURE
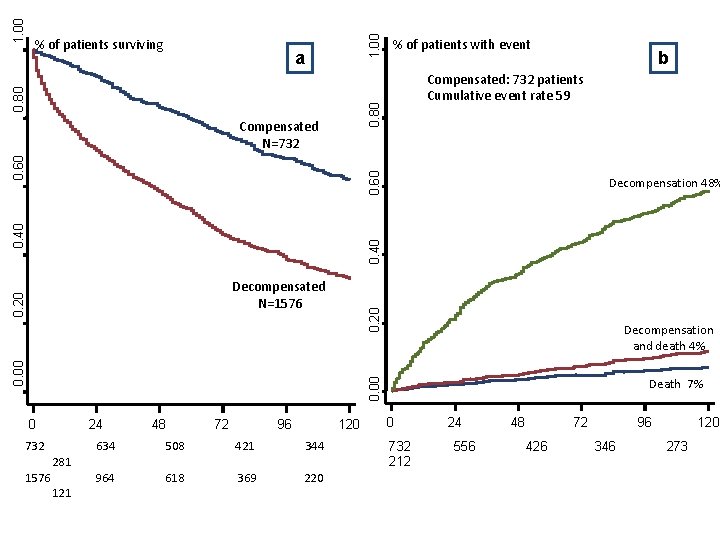
1. 00 a % of patients with event Decompensation 48% 0. 40 0. 60 Compensated N=732 b Compensated: 732 patients Cumulative event rate 59 0. 80 1. 00 % of patients surviving 0. 20 Decompensation and death 4% Death 7% 0. 00 0. 20 Decompensated N=1576 0 732 1576 24 281 121 48 72 96 120 634 508 421 344 964 618 369 220 0 732 212 24 556 48 72 426 96 346 120 273
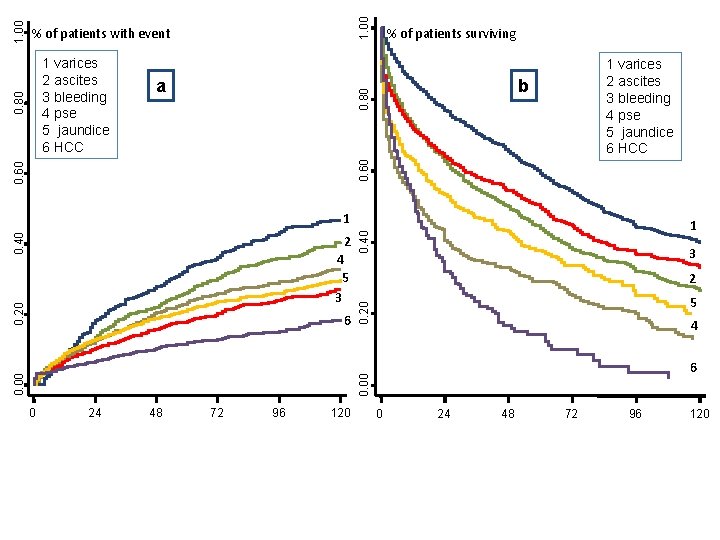
1. 00 a % of patients surviving 1 varices 2 ascites 3 bleeding 4 pse 5 jaundice 6 HCC b 0. 60 0. 80 1 varices 2 ascites 3 bleeding 4 pse 5 jaundice 6 HCC 0. 80 1. 00 % of patients with event 0. 20 3 2 5 4 6 0. 00 6 0. 40 2 4 5 3 1 0. 20 0. 40 1 0 24 48 72 96 120
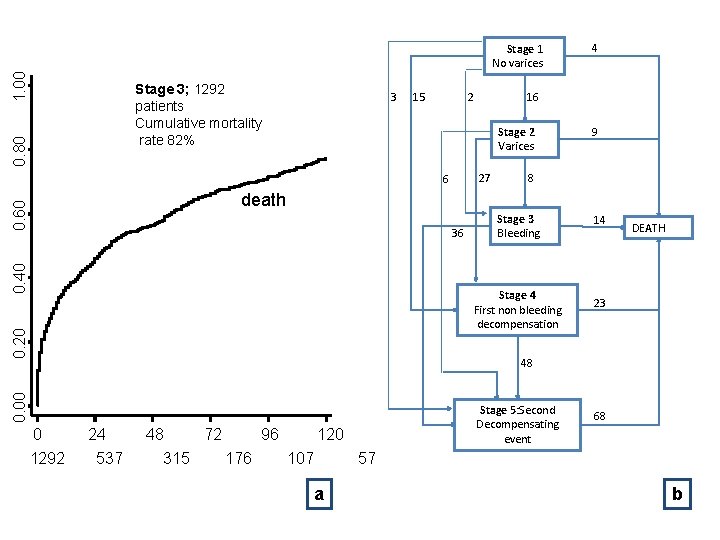
1. 00 Stage 1 No varices 0. 80 Stage 3; 1292 patients Cumulative mortality rate 82% 3 15 16 2 Stage 2 Varices 27 6 4 9 8 0. 60 death 0. 40 36 Stage 3 Bleeding 0. 20 Stage 4 First non bleeding decompensation 14 DEATH 23 0. 00 48 0 1292 24 537 48 315 72 96 176 Stage 5: Second Decompensating event 120 107 68 57 a D'Amico AASLD 2011 b 9
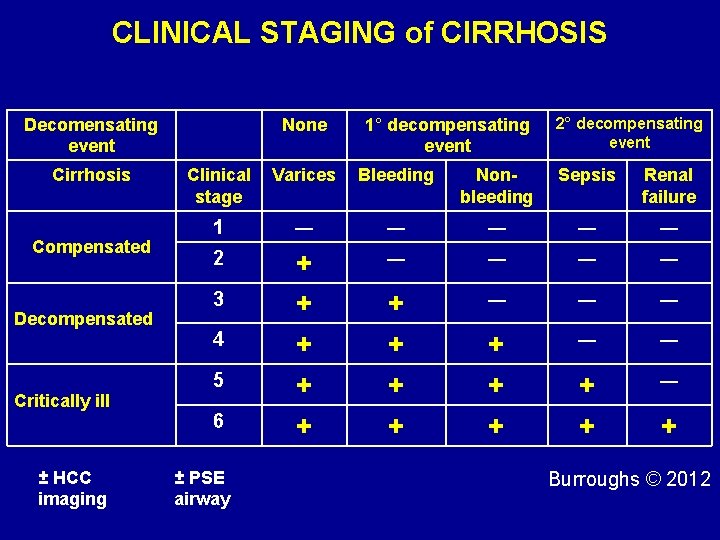
CLINICAL STAGING of CIRRHOSIS Decomensating event Cirrhosis Compensated Decompensated Critically ill ± HCC imaging None 1° decompensating event 2° decompensating event Clinical stage Varices Bleeding Nonbleeding Sepsis Renal failure 1 ― ― ― 2 + + + ― ― ― + + + ― ― + + ― 3 4 5 6 ± PSE airway + Burroughs © 2012

CLINICAL PRESENTATION of CIC v Jaundice v Ascites v Altered mental state v Hypotension v Malnutrition v Oliguria / anuria v Sepsis v Bleeding Any combination
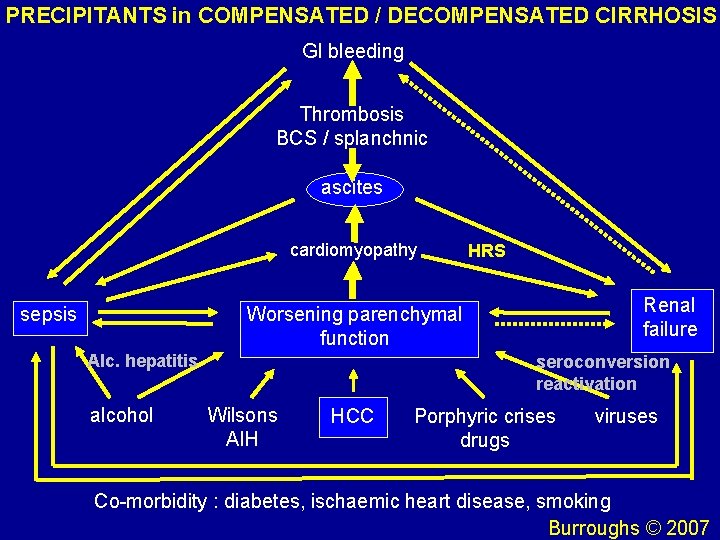
PRECIPITANTS in COMPENSATED / DECOMPENSATED CIRRHOSIS GI bleeding Thrombosis BCS / splanchnic ascites cardiomyopathy HRS Renal failure Worsening parenchymal function sepsis Alc. hepatitis alcohol seroconversion reactivation Wilsons AIH HCC Porphyric crises drugs viruses Co-morbidity : diabetes, ischaemic heart disease, smoking Burroughs © 2007
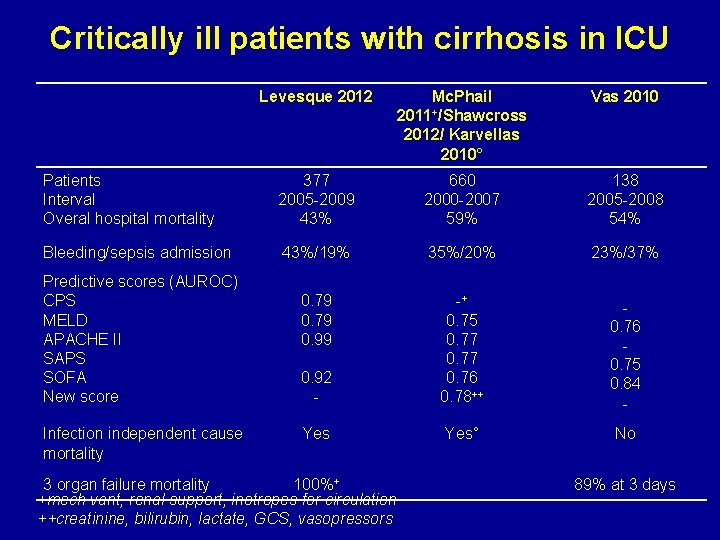
Critically ill patients with cirrhosis in ICU Levesque 2012 Mc. Phail 2011+/Shawcross 2012/ Karvellas 2010° Vas 2010 Patients Interval Overal hospital mortality 377 2005 -2009 43% 660 2000 -2007 59% 138 2005 -2008 54% Bleeding/sepsis admission 43%/19% 35%/20% 23%/37% 0. 79 0. 99 0. 92 - -+ 0. 75 0. 77 0. 76 0. 78++ 0. 76 0. 75 0. 84 - Yes° No Predictive scores (AUROC) CPS MELD APACHE II SAPS SOFA New score Infection independent cause mortality 3 organ failure mortality 100%+ +mech vant, renal support, inotropes for circulation ++creatinine, bilirubin, lactate, GCS, vasopressors 89% at 3 days

Cost of treating critically ill patients with cirrhosis • Simplified therapeutic scoring system (TISS) – estimation of resource cost ITU – TISS – One TISS point 28 (audit nurses) £ 47, 50 (55 Euro) • 473 (from 363) for cost analysis – Median TISS – Median cost 261 (98 -574) £ 12, 403 (4, 636 -27, 283) c. 14, 200 Euro • Survivors cheaper – Median TISS 158 – Cost of survivor episode £ 51, 376 c. 60, 000 Euro • Prediction cost – Admission variceal bleeding , ventilation , low PO 2/Fi. O 2 admission , lactate – More accurate in survivors

TERMINOLOGY

Tentative (“consensus”) definitions of a possible syndrome “acute on chronic liver failure” • Acute hepatic insult manifesting as jaundice and coagulapthy complicated within 4 weeks by ascites and/or encephalopathy (Sarin 2009 – APASL) • Acute deterioration of pre-existing chronic liver disease, usually related to a precipitating event and associated with increased mortality at 3 months due to multisystem organ failure (Olson 2011) • Why not make it simple? Onset of an organ failure other than the liver in a patient with cirrhosis

“Acute on Chronic” Liver Failure – Hypothesis (Malik 2009; Jalan 2012) • The response to injury is an inappropriate inflammatory response and immune dysfunction – leading to an increased susceptibility to infection • Why inappropriate – may be “homeostatic” – Suppressing TNF in alcoholic hepatitis led to increased mortality (Naveau 2004; Boetticher 2008) – Difficulrty in determining culture positive infections • Not clear if there are difference from sepsi in noncirrhotics

CANONIC Study: diagnosis, prevalence and prognosis of “Acute on Chronic liver failure” • First 920 cases • Prevalence of organ failure – – – Liver Renal Coagulation Circulation Brain Lung 15. 2% (bilirbin >12 mg/d. L) 12. 8% (creatinine >2 mg/d. L) 7. 7% 7% 4. 7% grade 3/4 PSE 2. 2%

DIAGNOSTIC CRITERIA AND GRADES OF ACLF NO ACLF: 1. Patients with no organ failure; 2. Patients with hepatic, coagulation, circulation or respiratory failure, serum creatinine < 1. 5 mg/dl and no hepatic encephalopathy; 3. Patient with cerebral failure and serum creatinine < 1. 5 mg/d. L ACLF Grade 1: 1. Patients with renal failure; 2. Patients with other single organ failure with serum creatinine ≥ 1. 5 mg mg/d. L and/or hepatic encephalopathy grade 1 -2. ACLF Grade 2: Patients with 2 organ failures ACLF Grade 3: Patients with 3 organ failures ACLF Grade 4: Patients with 4 -6 organ failures
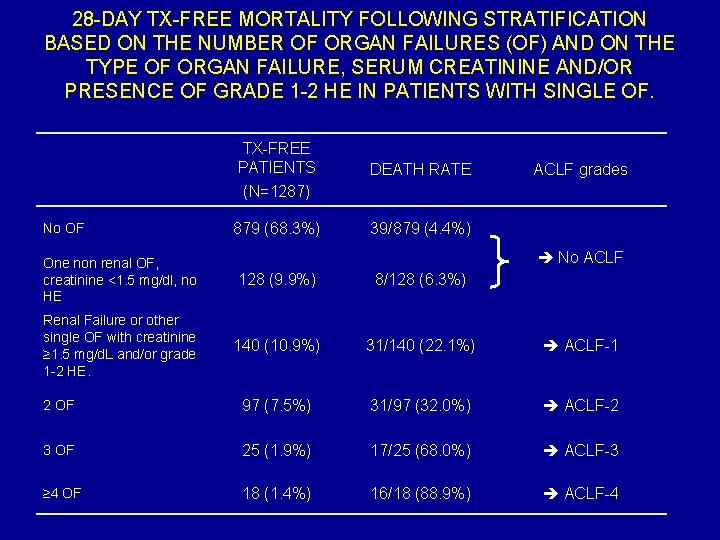
28 -DAY TX-FREE MORTALITY FOLLOWING STRATIFICATION BASED ON THE NUMBER OF ORGAN FAILURES (OF) AND ON THE TYPE OF ORGAN FAILURE, SERUM CREATININE AND/OR PRESENCE OF GRADE 1 -2 HE IN PATIENTS WITH SINGLE OF. No OF TX-FREE PATIENTS (N=1287) DEATH RATE 879 (68. 3%) 39/879 (4. 4%) ACLF grades No ACLF One non renal OF, creatinine <1. 5 mg/dl, no HE 128 (9. 9%) 8/128 (6. 3%) Renal Failure or other single OF with creatinine ≥ 1. 5 mg/d. L and/or grade 1 -2 HE. 140 (10. 9%) 31/140 (22. 1%) ACLF-1 2 OF 97 (7. 5%) 31/97 (32. 0%) ACLF-2 3 OF 25 (1. 9%) 17/25 (68. 0%) ACLF-3 ≥ 4 OF 18 (1. 4%) 16/18 (88. 9%) ACLF-4
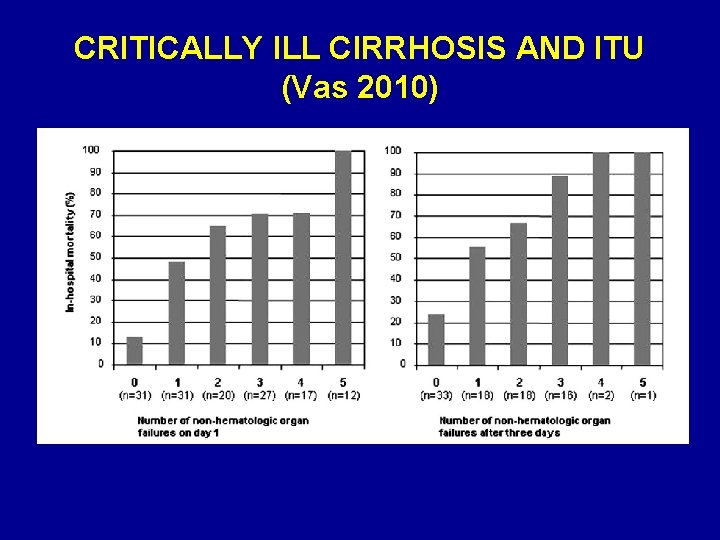
CRITICALLY ILL CIRRHOSIS AND ITU (Vas 2010)

SEPSIS
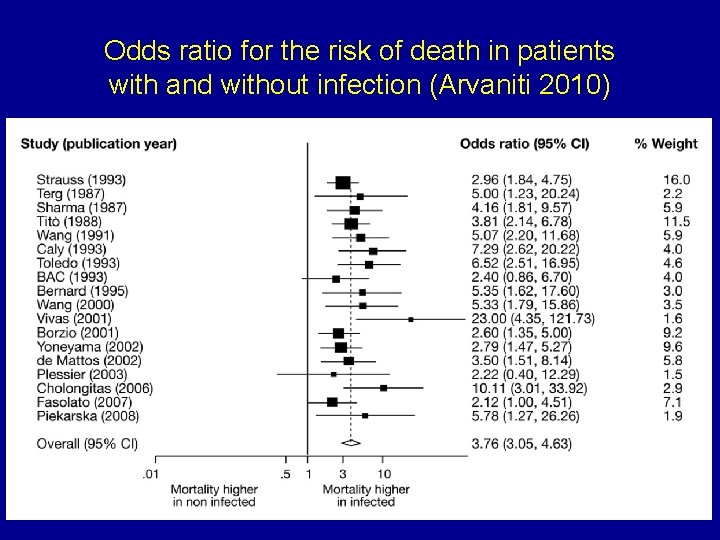
Odds ratio for the risk of death in patients with and without infection (Arvaniti 2010)
Frequency of bacterial infection in cirrhosis prospective study (Borzio 2001) In hospital mortality 15% v 7% non infected % 28 55 19 148 34 27 108
BACTERIAL INFECTIONS in CIRRHOTICS with ASCITES Fasolato 2007 104 consecutive admissions 24% 42. 3% 16. 3% 2. 9% 4. 8% 5. 8%

SEPSIS and CIRRHOSIS v Golden rule always suspect sepsis as precipitant cause v Empirical IV antibiotics – cephalosporins / tazocin v Colloid for spontaneous bacterial peritonitis (Sort 1999) and probably other sepsis v Short ACTH test – hydrocortisone v Oral antifungal prophylaxis
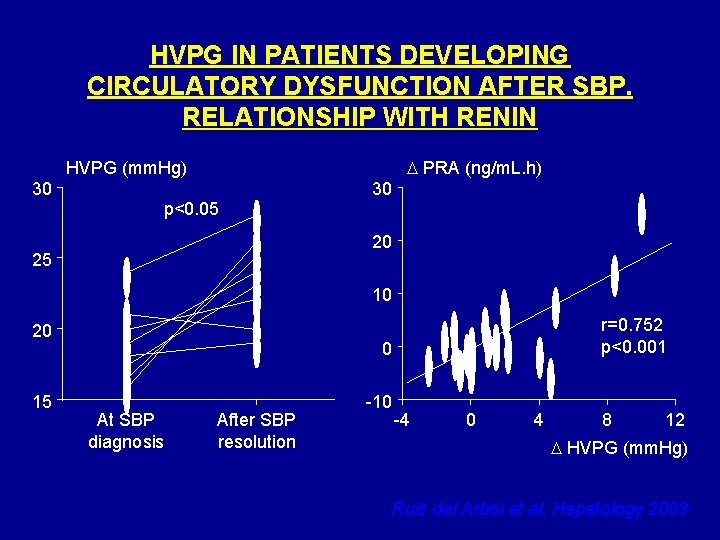
HVPG IN PATIENTS DEVELOPING CIRCULATORY DYSFUNCTION AFTER SBP. RELATIONSHIP WITH RENIN D PRA (ng/m. L. h) HVPG (mm. Hg) 30 30 p<0. 05 20 25 10 20 15 r=0. 752 p<0. 001 0 At SBP diagnosis After SBP resolution -10 -4 0 4 8 12 D HVPG (mm. Hg) Ruiz del Arbol et al. Hepatology 2003
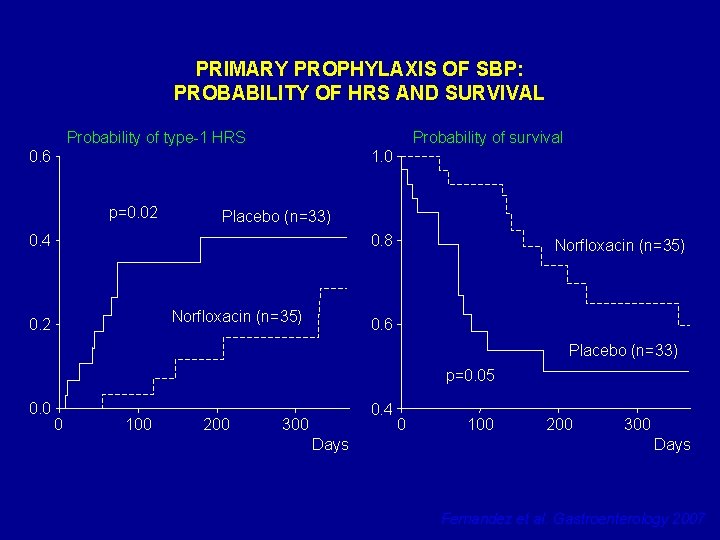
PRIMARY PROPHYLAXIS OF SBP: PROBABILITY OF HRS AND SURVIVAL Probability of type-1 HRS Probability of survival 0. 6 1. 0 p=0. 02 Placebo (n=33) 0. 4 0. 8 Norfloxacin (n=35) 0. 2 Norfloxacin (n=35) 0. 6 Placebo (n=33) p=0. 05 0. 0 0 100 200 0. 4 300 Days 0 100 200 300 Days Fernandez et al. Gastroenterology 2007

POTENTIAL REDUCTION OF BACTERIAL TRANSLOCATION BY PROPRANOLOL • Reduction splanchnic blood flow thus mucosa oedema/congestion - ? permeability • Increase intestinal transit rats (Perez-Paramo 2000) - cisapride (Parado 2000) • Enhance immune system - inhibition stress related c. AMP-PKA pathway (Peuschel 2005) Thalheimer 2005, 2007

Prevention SBP and bactaeremia by propranolol administered in cirrhotic patients in RCT and non-RCT (Senzolo 2009)

Prevention of SBP and bactaeremia by propranolol in haemodynamic responders vs non responders in RCT for the prevention of variceal bleeding and rebleeding comparing propranolol vs. controls and in 2 studies for the prevention of SBP (Senzolo 2009).
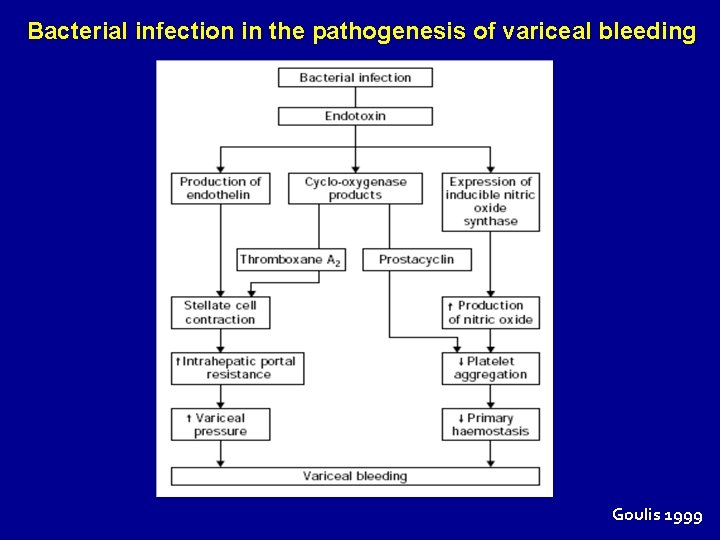
Bacterial infection in the pathogenesis of variceal bleeding Goulis 1999

EARLY REBLEEDING in RANDOMIZED TRIALS of PROPHYLACTIC vs ON DEMAND ANTIBIOTICS Frequency of bleeding 7 days 6 weeks
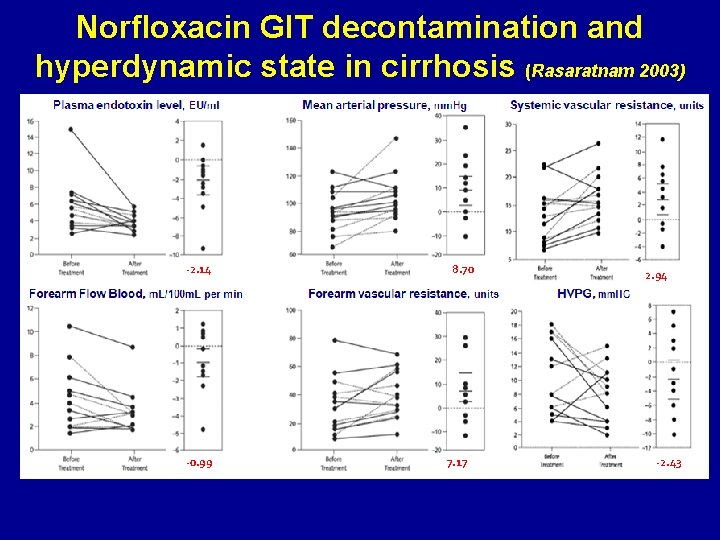
Norfloxacin GIT decontamination and hyperdynamic state in cirrhosis (Rasaratnam 2003) -2. 14 -0. 99 8. 70 7. 17 2. 94 -2. 43

Intestinal decontamination improves liver haemodynamics in patients with alcohol/related decompensated cirrhosis Individual changes in HVPG before and after 4 weeks of rifaximin administration -30 patients with alcohol-related cirrhosis and ascites. -Rifaximin 1200 mg daily p<0. 001 Vlachogiannakos 2009
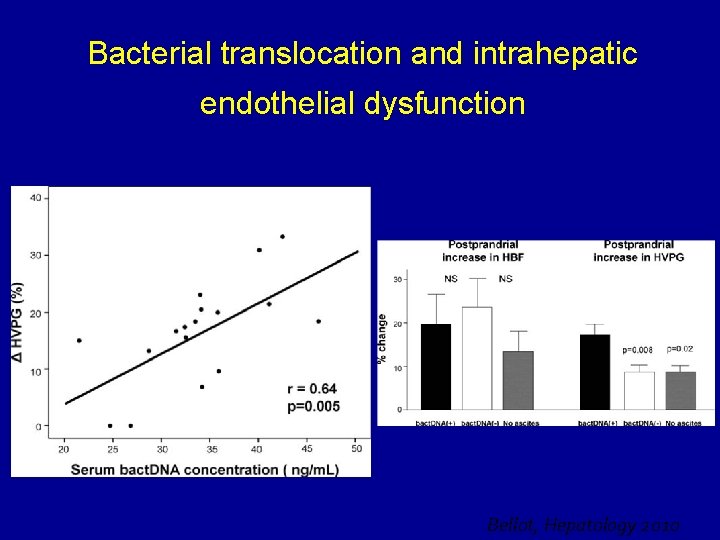
Bacterial translocation and intrahepatic endothelial dysfunction Bellot, Hepatology 2010
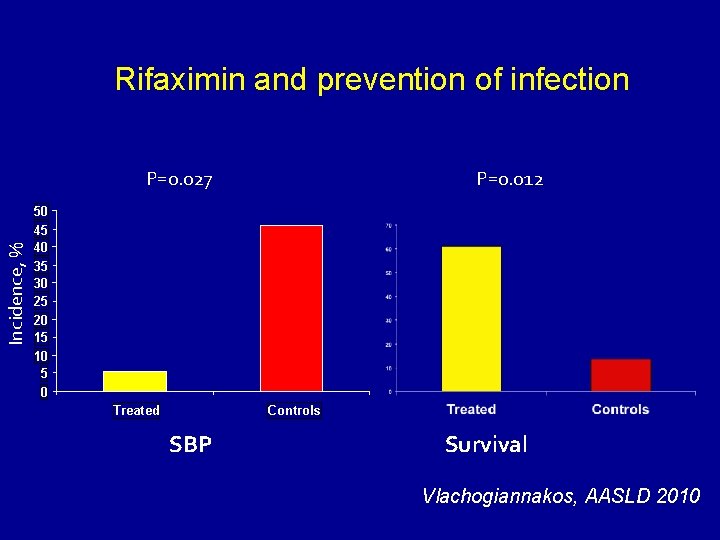
Rifaximin and prevention of infection Incidence, % P=0. 027 P=0. 012 50 45 40 35 30 25 20 15 10 5 0 Treated Controls SBP Survival Vlachogiannakos, AASLD 2010

HEART and CIRCULATION in CIC v systemic (and splanchnic) vasodilatation v “cirrhotic” cardiomyopathy – in end stage cirrhosis ― Inappropriate C. O. with respect to SVR v regional renal vasoconstriction

CIRRHOTIC CARDIOMYOPATHY : CONSTELLATION of FEATURES (Baik 2007) v Baseline increased cardiac output v Blunted verticular response to stimuli v Systolic and / or diastolic dysfunction v Absence left ventricular failure at rest v Electrophysiological abnormalities (QT prolongation) v Chronotropic incompetence Kowalski 1953, Kelbaek 1984, Pozzi 1997, Bernardi 1998, Henriksen 2002, Ramond 1986
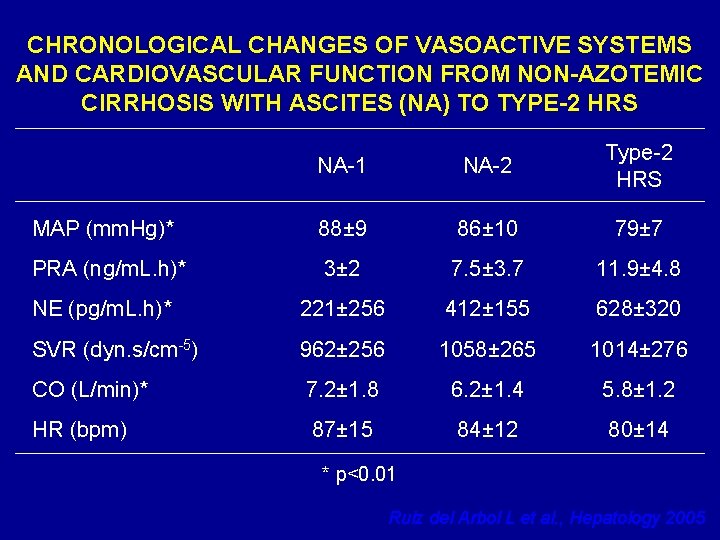
CHRONOLOGICAL CHANGES OF VASOACTIVE SYSTEMS AND CARDIOVASCULAR FUNCTION FROM NON-AZOTEMIC CIRRHOSIS WITH ASCITES (NA) TO TYPE-2 HRS NA-1 NA-2 Type-2 HRS MAP (mm. Hg)* 88± 9 86± 10 79± 7 PRA (ng/m. L. h)* 3± 2 7. 5± 3. 7 11. 9± 4. 8 NE (pg/m. L. h)* 221± 256 412± 155 628± 320 SVR (dyn. s/cm-5) 962± 256 1058± 265 1014± 276 CO (L/min)* 7. 2± 1. 8 6. 2± 1. 4 5. 8± 1. 2 HR (bpm) 87± 15 84± 12 80± 14 * p<0. 01 Ruiz del Arbol L et al. , Hepatology 2005

Does adrenal insufficiency contribute to cirrhotic cardiomyopathy? (Theocharidou 2012)

HEART and CIRCULATION in CIC - ALBUMIN v Albumin debate may not be applicable to cirrhosis v SAFE (RCT) and SOAP (observational) studies v Reduced morbidity with albumin in hypoalbuminaemic patients – RCT (Vincent 2004) v Goal directed fluid resuscitation v Vasopressors v Steroids if vasopressor non-responsive

Early resuscitation – the importance of goal directed therapy (Rivers 2001) Dellinger 2008 – Survive Sepsis Campaign – 1 hr delay /mortality 8% (Kumar 2006)
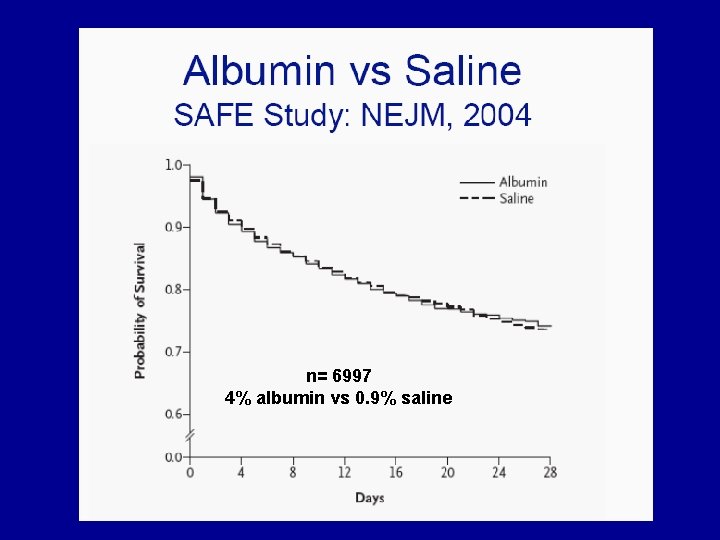
n= 6997 4% albumin vs 0. 9% saline
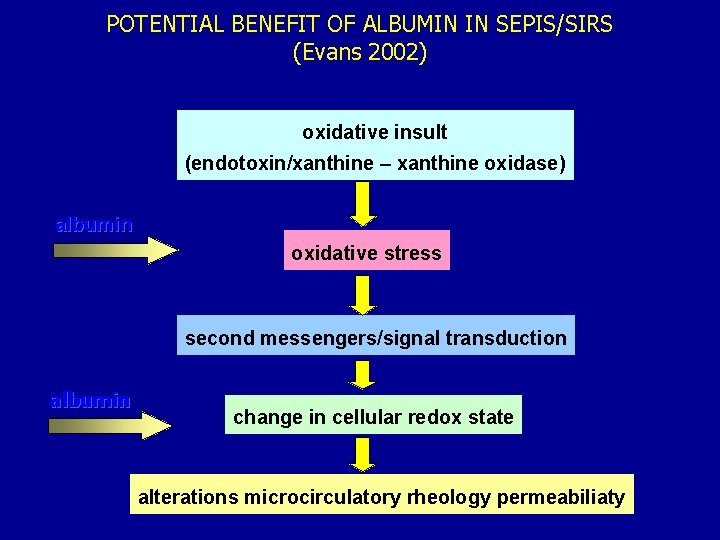
POTENTIAL BENEFIT OF ALBUMIN IN SEPIS/SIRS (Evans 2002) oxidative insult (endotoxin/xanthine – xanthine oxidase) albumin oxidative stress second messengers/signal transduction albumin change in cellular redox state alterations microcirculatory rheology permeabiliaty


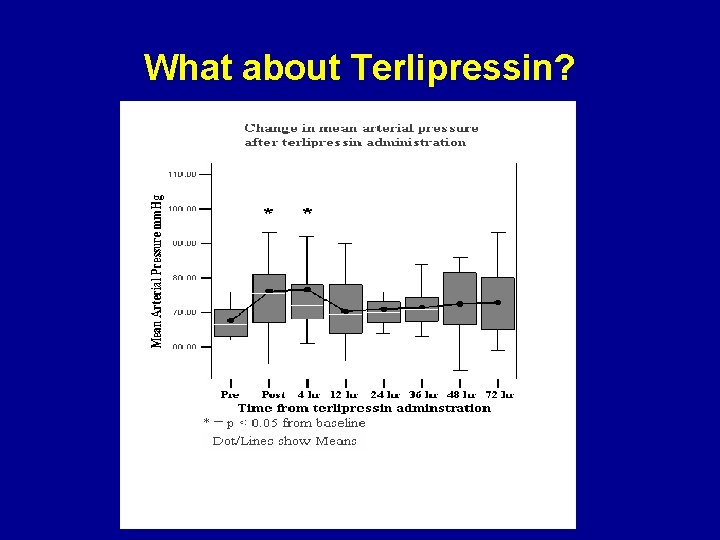
What about Terlipressin?

HEPATIC ENCEPHALOPATHY in CIRRHOSIS v Rarely spontaneous - usually precipitating factor v. Hyponataemia strong inducer v In absence sepsis and renal dysfunction / failure resolves rapidly with standard measures v. Protection of airway intubate grade 3 or more PSE / GCS 8 or less

BLEEDING and CIRRHOSIS

HVPG PREDICTION of 5 DAY FAILURE in ACUTE VARICEAL BLEEDING (Albraldes 2006) § 117 patients – HVPG measured ≤ 48 h ( 4 centres) § 18 (15%) – failure at 5 days (vasoactive drugs, endoscopic therapy, antibiotics) § HVPG ≥ 20 mm. Hg § Systolic BP ≤ 100 mm. Hg § Non-alcoholic cirrhosis OR 5. 2 (1. 3 – 21. 2) OR 3. 6 (1. 2 – 10. 9) OR 4. 0 (1. 3 – 12. 8) § HVPG ≥ 20 mm. Hg strongly related to CP (p=0. 0002) Child A 33% Child B 57% Child C 84% § Without HVPG c statistic 0. 8 c statistic 0. 79

HVPG PREDICTION of 5 DAY FAILURE in ACUTE VARICEAL BLEEDING (Albraldes 2006) Allocation points score % failure Systolic B ≤ 100 mm Hg Systolic B > 100 mm Hg 1 0 Non-alcoholic cirrhosis Alcoholic cirrhosis 1 0 Child B Child C 1 2 0 – 2 points 8 % 3 – 4 points 39 % p = 0. 00006

Diagnosis of upper GI bleeding in cirrhosis Ø Endoscopy as soon as resuscitation adequate Ø It is a high risk endoscopy - adequate support staff (suction) - assess risk of aspiration - pulse oximetry - nasal oxygen - will need endotracheal intubation/GA in several cases Ø Look at fundus, other lesions Ø NB 50% DGH do not have an adequately supported on call system

Timing of endoscopy in Acute Variceal Bleeding in cirrhosis (Hsu 2009) Ø 311 consecutive cirrhotics Ø 25 deaths in hospital (8%) – multivariate analysis adjusted OR p value haematemesis 8. 66 0. 044 MELD score/point 1. 16 <0. 001 endoscopy >15 h 3. 67 0. 016 failure first endoscopy 4. 36 0. 00
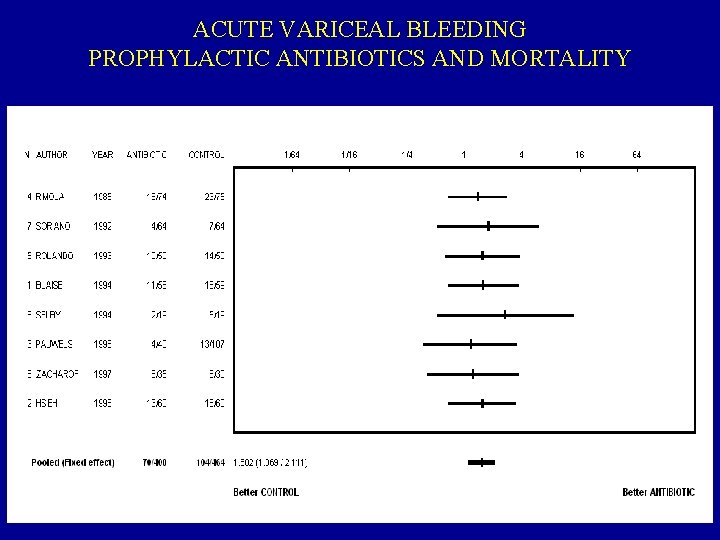
ACUTE VARICEAL BLEEDING PROPHYLACTIC ANTIBIOTICS AND MORTALITY

EARLY REBLEEDING in RANDOMIZED TRIALS of PROPHYLACTIC vs ON DEMAND ANTIBIOTICS Frequency of bleeding 7 days 6 weeks

QUINOLONES VERSUS CEPHALOSPORINS FOR MANAGEMENT OF UPPER GI BLEEDING IN CIRRHOSIS Failure to control bleeding < 5 days <24 hours nes lo ino nes o qu l ± o e n xon qui a i r t cef Sabat 1998 ne nes o o x l no tria f e qui c Fernandez 2006

WHICH ANTIBIOTIC FOR “PROPHYLAXIS” IN UPPER GI BLEEDING IN CIRRHOSIS? Ø IV 3 rd generation cephalosporins Start at admission before endoscopy Ø Active against quinolone resistant bacteria gram negative bacteria non enterococcal streptococci Ø No issue of poor absorption due to bleeding, pseudo-ileus etc. Ø Many cirrhotics receive quinolone prophylaxis Ø Will treat infections already present 20% culture positive at admission 50% of infections in cirrhotics are culture negative

RCT OF TRANSFUSION STRATEGY IN ACUTE VARICEAL BLEEDING (Colomo 2009) Transfusion policy Restrictive (7 -8 g/d. L) Liberal (9 -10 g/d. L) 7 g/d. L 9 g/d. L Patients 74 73 Therapeutic failure + ++ 42 day survival free of failure + ++ Unchanged Increased* Threshold HVPG *p<0. 03 (20. 6 mm. Hg to 21. 3 mm. Hg) Transfusion policy, HVPG, and bacterial infection independent predictors 42 d survival without failure
Transfusion Airway/Adrenals Kidneys Electrolytes TAKE CARE IN BLEEDING OGV Coagulation Alcohol withdrawal Resuscitation Encephalopathy Infection Nutrition Blood transfusion © 2011 Oxygen Gastric Varices
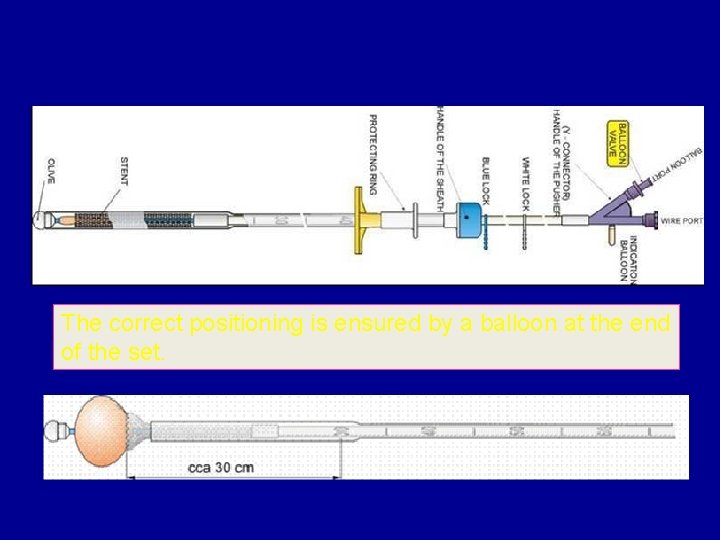
The correct positioning is ensured by a balloon at the end of the set.
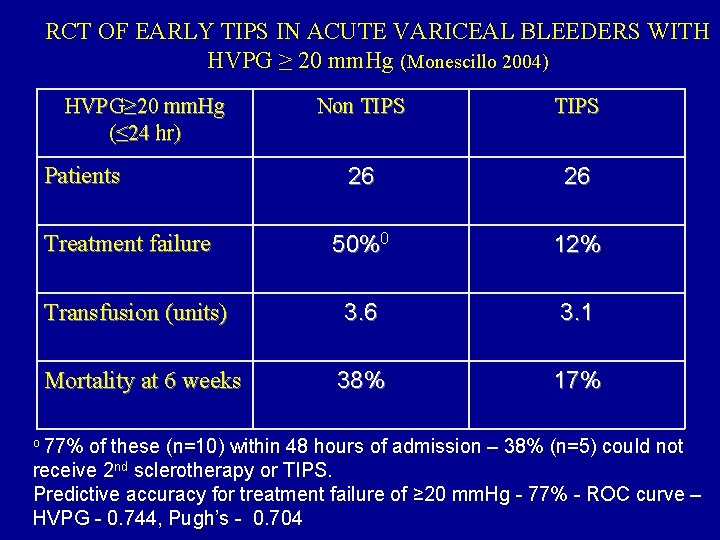
RCT OF EARLY TIPS IN ACUTE VARICEAL BLEEDERS WITH HVPG ≥ 20 mm. Hg (Monescillo 2004) HVPG≥ 20 mm. Hg (≤ 24 hr) Patients Treatment failure Transfusion (units) Mortality at 6 weeks o 77% Non TIPS 26 26 50%0 12% 3. 6 3. 1 38% 17% of these (n=10) within 48 hours of admission – 38% (n=5) could not receive 2 nd sclerotherapy or TIPS. Predictive accuracy for treatment failure of ≥ 20 mm. Hg - 77% - ROC curve – HVPG - 0. 744, Pugh’s - 0. 704

Early TIPS for cirrhosis and variceal bleeding (Garcia-Pagan 2010) • • 9 centres – 34 months – 63 patients (from 359) Vasoactive drugs and endoscopic therapy and antibiotics Randomized ≤ 24 hours from admission Child C (10 -13 points); Child B and active bleeding TIPS (PTFE) performed ≤ 72 hours of diagnostic endoscopy Following 5 days – non TIPS group – NSBB + banding Rescue TIPS (PTFE) if necessary End-point: – – 1° - failure to control acute bleeding 1° - failure to prevent clinically significant rebleeding ≤ 1 year 2° - death ≤ 6 weeks 2° - death ≤ 1 year
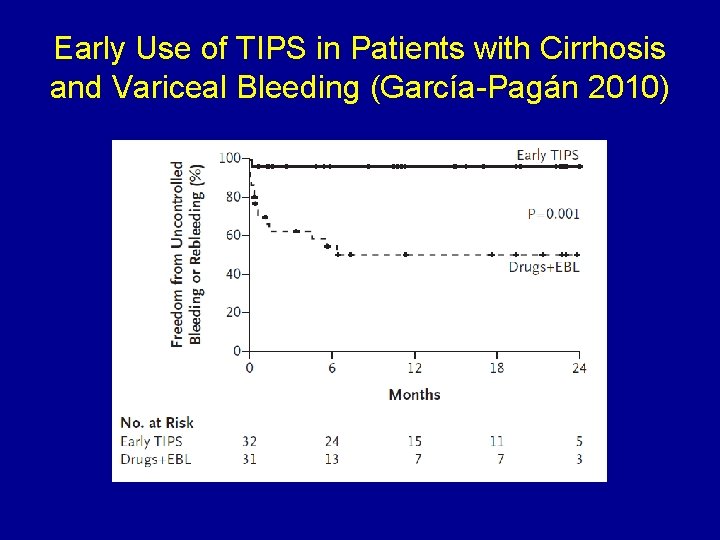
Early Use of TIPS in Patients with Cirrhosis and Variceal Bleeding (García-Pagán 2010)

Early Use of TIPS in Patients with Cirrhosis and Variceal Bleeding (García-Pagán 2010)

ADRENAL DYSFUNCTION

SURVIVAL OF PATIENTS WITH SEVERE SEPSIS WITH (GROUP 1) AND WITHOUT (GROUP 2) ASSESSMENT OF ADRENAL FUNCTION AND EVENTUAL TREATMENT WITH HYDROCORTISONE(50 mg/4 h) Fernandez et al. , Hepatology 2006
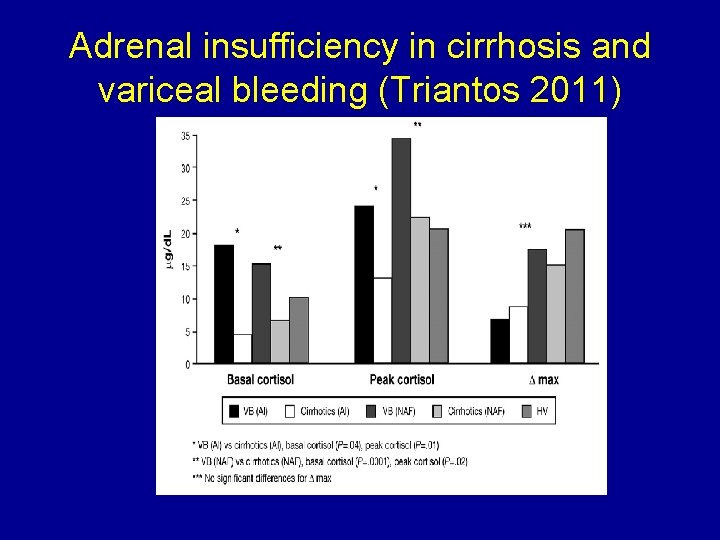
Adrenal insufficiency in cirrhosis and variceal bleeding (Triantos 2011)
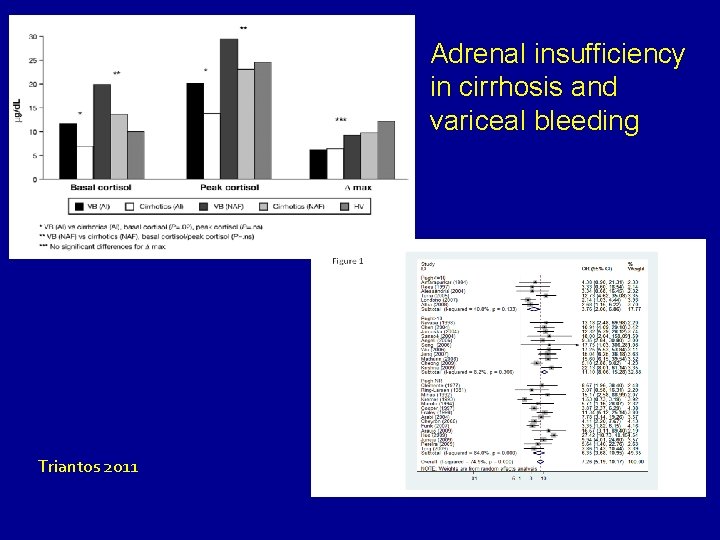
Adrenal insufficiency in cirrhosis and variceal bleeding Triantos 2011

RENAL FAILURE
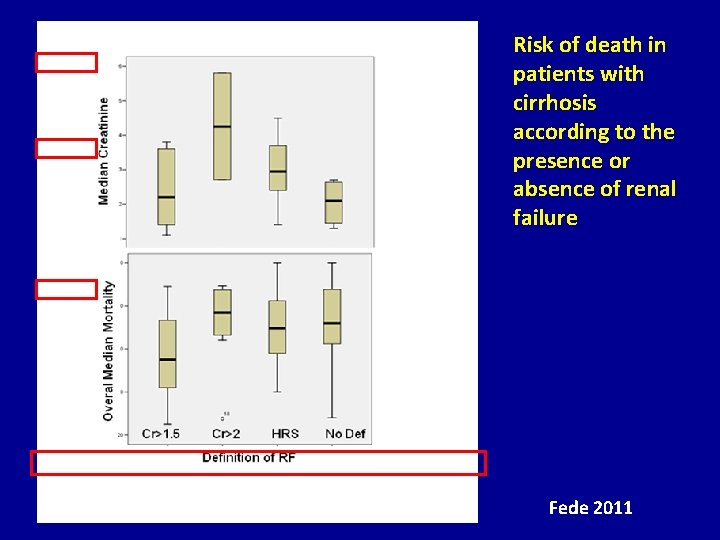
Risk of death in patients with cirrhosis according to the presence or absence of renal failure Fede 2011

Median creatinine and median overall mortality according to definition of renal failure Fede 2011

Protecting the kidney in cirrhosis 30% SBP renal failure Gines, 1997

RESULTS OF TWO RANDOMIZED CONTROLLED TRIALS COMPARING TERLIPRESSIN AND ALBUMIN (T+A) vs ALBUMIN ALONE (A) IN PATIENTS WITH HRS Martín-Llahí et al. Patients Reversal of HRS 3 months survival Sanyal A et al. T+A A 23 22 56 56 8 (34. 7%) 1 (4. 6%) 26% 18% * 2 months survival 19 (34%) 7 (13%) 48%*

LIVER SUPPORT DEVICES
Types of Liver Support • Detoxification techniques • Charcoal • Biologic DT • Dialysis techniques • MARS • SPAD • Prometheus • High volume haemofiltration / plasmapheresis • Extracorporeal organ perfusion • Baboons • Pigs • Humans • Bioartificial devices • MELS • AMC –BAL • ELAD

PROPERTIES OF ALBUMIN • 70% of total plasma oncotic activity • prolonged half life • high capacity molecule transport (aations/anions) • free radical scavenging (thiol groups) – also binds copper • modulatory effect on capillary permeability/rheology • modulatory effect on neutrophil adhesion/activation • nitric oxide binding • drug binding (Bertucci 2002)
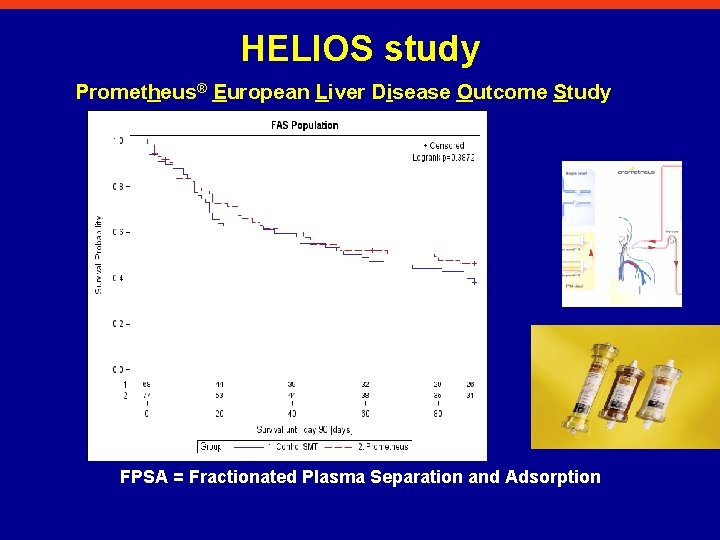
HELIOS study Prometheus® European Liver Disease Outcome Study FPSA = Fractionated Plasma Separation and Adsorption
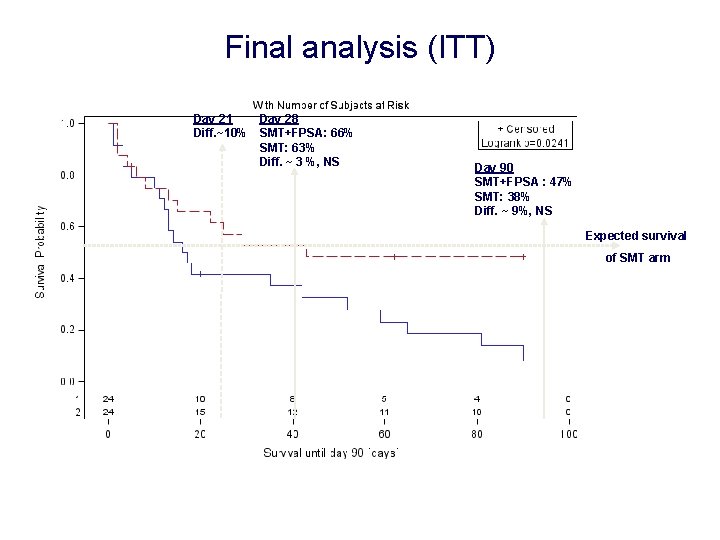
Final analysis (ITT) Day 21 Day 28 Diff. ~10% SMT+FPSA: 66% SMT: 63% Diff. ~ 3 %, NS Day 90 SMT+FPSA : 47% SMT: 38% Diff. ~ 9%, NS Expected survival of SMT arm
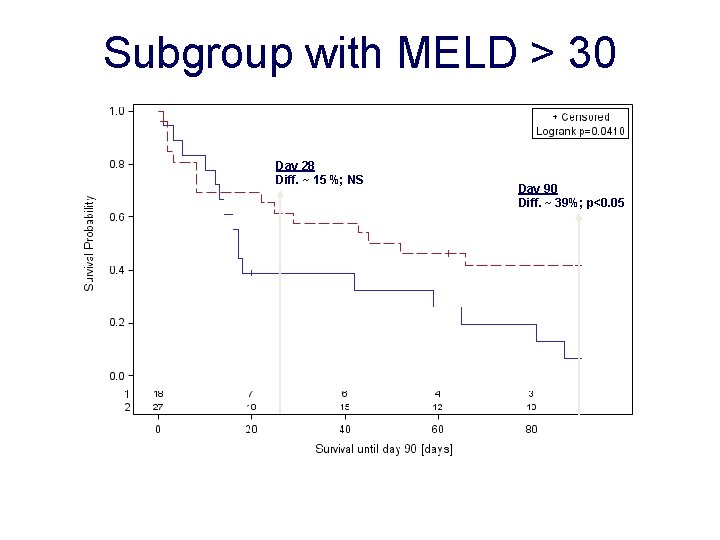
Subgroup with MELD > 30 Day 28 Diff. ~ 15 %; NS Day 90 Diff. ~ 39%; p<0. 05

Extracorporeal liver support with the Molecular Adsorbent Recirculating System (MARS) in patients with acute -on-chronic liver failure (ACLF). The RELIEF Trial.
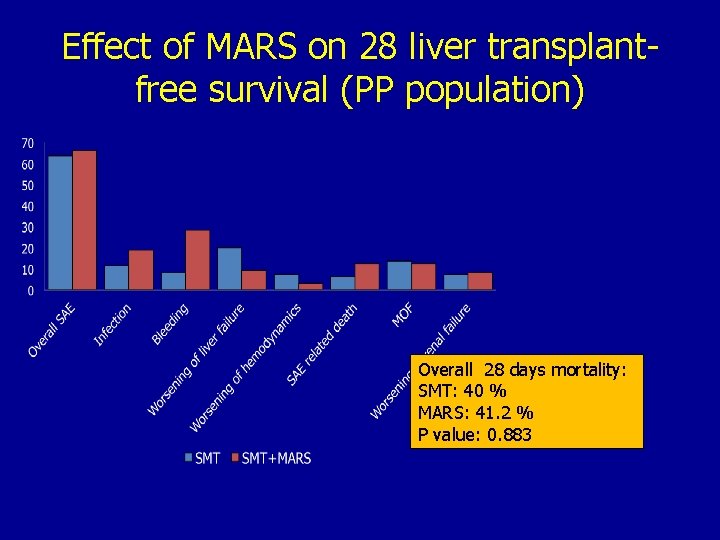
Effect of MARS on 28 liver transplantfree survival (PP population) Overall 28 days mortality: SMT: 40 % MARS: 41. 2 % P value: 0. 883

Adverse events NS NS p=0. 006 p=0. 04 NS NS

PREVENTION of CRITICAL ILLNESS in CIRRHOSIS v Prevention of renal failure • Avoid nephrotoxic drugs aminoglycosides, NSAIDS, ACE, ATII inhibitors, contrast media • Search for sepsis • Avoid depleting intravascular volume diuretics, post paracentesis, circulatory dysfunction, lactulose • • Use vasoconstrictors Volume replacement during sepsis

PREVENTION of CRITICAL ILLNESS in CIRRHOSIS ITU outreach TEAMS v Prevention and prompt therapy of sepsis 1º and 2º prophylaxis of spontaneous bacterial peritonitis ? Probiotics ? Non selective beta-blockers v. Rapid control of bleeding Prevention of aspiration Prevent renal impairment v Prevent severe encephalopathy Prevent aspiration Prevent need to intubate v “Bridge to transplantation”

PREVENTATIVE STRATEGIES IN CIRRHOSIS Tsochatzis, Bosch, Burroughs Gastroenterology 2010, Hepatology 2012
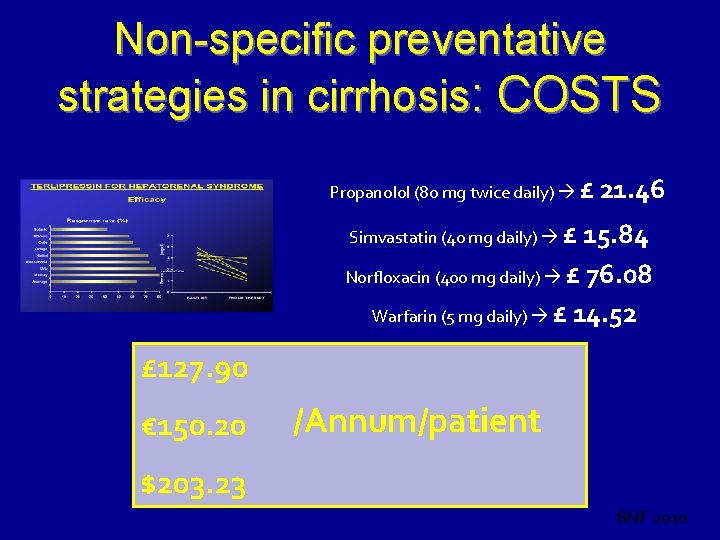
Non-specific preventative strategies in cirrhosis: COSTS Propanolol (80 mg twice daily) £ 21. 46 Simvastatin (40 mg daily) £ 15. 84 Norfloxacin (400 mg daily) £ 76. 08 Warfarin (5 mg daily) £ 14. 52 £ 127. 90 € 150. 20 /Annum/patient $203. 23 BNF 2010

CONCLUSIONS : CRITICALLY ILL PATIENTS with CIRRHOSIS § Think about sepsis Ø Empirical antibiotics – SBP § Short ACTH test Ø Adrenal function – steroids § Maintain circulation Ø Response vasopressors–terlipressin § Assess renal function Ø Colloid (albumin) § Bleeding Ø Antibiotics / terlipressin § Assess ITU / HDU care / referral Ø Out-reach team assessment § Renal failure Ø Trial of haemofiltration § Rule out HCC Ø Cross sectional imaging MRI / CT § Transplant possible? Ø Refer to transplant centre




Restuccia et al. J Hepatol 2004
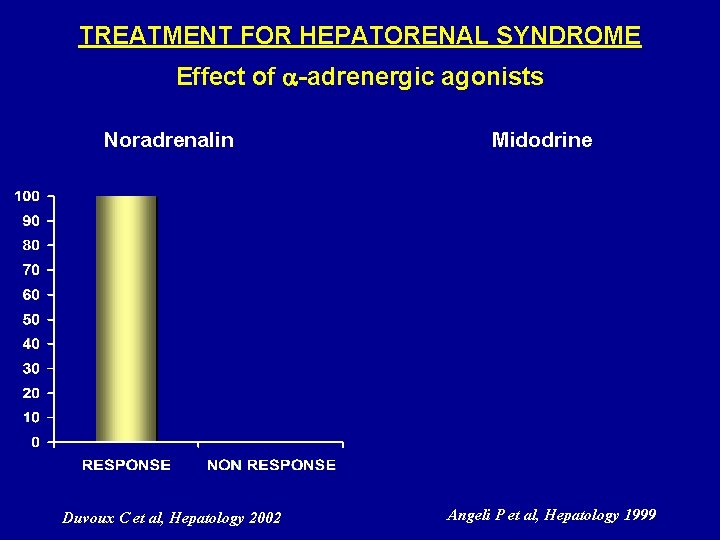
TREATMENT FOR HEPATORENAL SYNDROME Effect of -adrenergic agonists Noradrenalin Duvoux C et al, Hepatology 2002 Midodrine Angeli P et al, Hepatology 1999
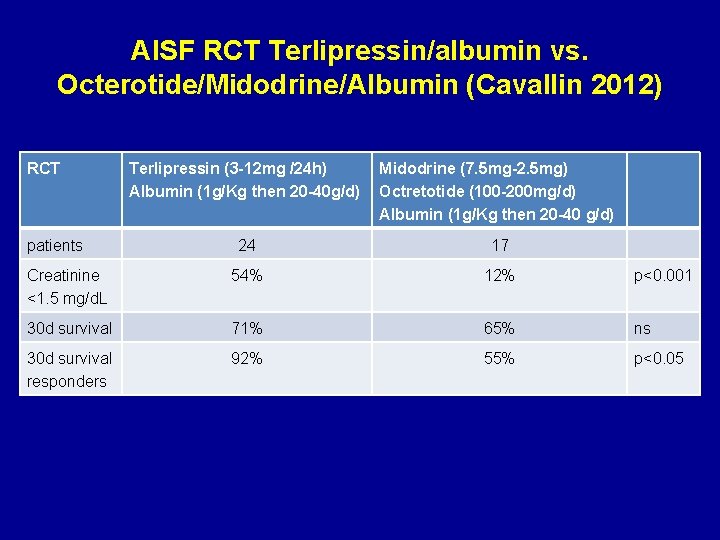
AISF RCT Terlipressin/albumin vs. Octerotide/Midodrine/Albumin (Cavallin 2012) RCT Terlipressin (3 -12 mg /24 h) Albumin (1 g/Kg then 20 -40 g/d) Midodrine (7. 5 mg-2. 5 mg) Octretotide (100 -200 mg/d) Albumin (1 g/Kg then 20 -40 g/d) 24 17 Creatinine <1. 5 mg/d. L 54% 12% p<0. 001 30 d survival 71% 65% ns 30 d survival responders 92% 55% p<0. 05 patients
- Slides: 91