PRADERWILLI SYNDROME Presented by The PraderWilli Syndrome Project

PRADER-WILLI SYNDROME Presented by: The Prader-Willi Syndrome Project for New Mexico

HISTORY 1956 3 Doctors from Switzerland A syndrome is a set of characteristics Incidence Rate: 1: 12 -15, 000 live births

GENETICS 15 th chromosome from father Paternal Deletion A band of genes 15 q 11 -q 13 is missing from the 15 th chromosome coming from the father 75% of people with PWS Maternal Dysomy the genetic material on the mother’s 15 th chromosome duplicates onto the father’s chromosome 25% of people with PWS

INHERITED PWS • Incidence – less than 1/10 of 1% • Mutation on father’s 15 th chromosome • Child can inherit the mutation • Mosaic PWS

MORE ON GENETICS • In Paternal Deletion there can be micro and macro deletions • Deletions may be influencing the other genes on chromosome 15 • Genes on chromosome 15 may be influencing a tendency toward depression and bi-polar disorders

AND MORE • In Maternal Dysomy the child receives a “double dose” of the mother’s genetic inheritance residing on chromosome 15 • Angelman’s Syndrome is a mirror image of PWS where deletions and duplications occur on the mother’s 15 chromosome - manifests as a different syndrome • Genetic research continues including treatment with gene therapy
DIAGNOSIS • PWS can now be diagnosed with a blood test called a protein mythelation assay. • Results can be obtained in a couple of weeks. • Test is 99% accurate.

HYPOTHALAMUS Regulates Body Processes & Functions Regulates Secretion of Hormones

HYPOTONIA. Delayed fetal movement. Weak cry & lethargy. Feeding difficulties. Delayed motor skills . Speech difficulties. Scoliosis/Hip Dysplasia. Myopia/Strabismus. Unbalanced , uncoordinated gait
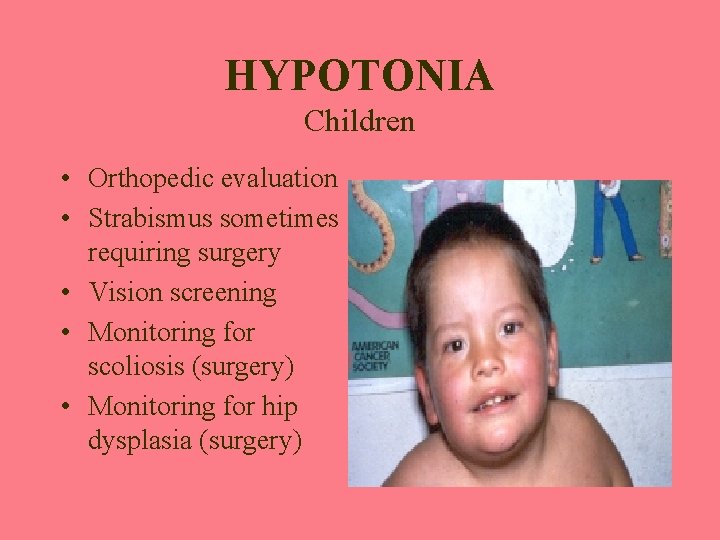
HYPOTONIA Children • Orthopedic evaluation • Strabismus sometimes requiring surgery • Vision screening • Monitoring for scoliosis (surgery) • Monitoring for hip dysplasia (surgery)

HYPOTONIA & OBESITY • The complications of morbid obesity (30% or more overweight) happen sooner for persons with PWS because of the hypotonia

HYPOGONADISM • Small genitals • Low levels of sexual hormone • Incomplete puberty due to hypothalamus not triggering the pituitary gland • Risk for premature osteoporosis • Low levels of Growth Hormone

MALE HYPOGONADISM • • Undescended testes Small penis Lack of growth spurt Lack of secondary sexual characteristics • Infertility usual

FEMALE HYPOGONADISM • Small genitalia • Absent/irregular menses • Lack of growth spurt • Lack of secondary sexual characteristics • Infertility usual

HYPOMENTIA • All have Learning Disabilities • Mental Retardation • IQ scores range from 35 -110, most testing around 70

HYPOMENTIA Cognitive Strengths • • • Fine Motor Skills Long Term Memory Visual Perceptional Skills Verbal Skills/Receptive Language Artistic Abilities

HYPOMENTIA Cognitive Challenges • • Abstract/Conceptual Thinking Auditory Short Term Memory Loss of Learned Information Set of Specific Learning Disabilities. Sequencing. Generalizing. Social Context. Meta-Cognition

LYING & PWS • Lying to get out of trouble • Lying to manipulate • Confabulations – the telling of tall tales for no apparent reason • Type of lying determines the response

BEST PRACTICES FOR THE CLASSROOM • Structure & consistency – is essential for management of PWS & needs to be visually presented • Activities – a full day moving from one to another with no “hanging out” • Individual attention – as much as possible • Positive reinforcement – as much as possible • Peer relationships – need to be encouraged • Visual learners

MORE BEST PRACTICES • Some children with PWS are easily overstimulated and have short attention spans – may need to make environmental accommodations • Concrete, hands-on learning style – learn by doing • Need to be weighed and measured weekly, same time and same scale • Therapies – often OT, SLP and PT

HYPERPHAGIA the food problem • • • Non-functioning Hypothalamus No feeling of fullness – satiety Always feeling hungry – insatiable appetite Slower metabolism – up to 1/3 slower Gain weight 3 times faster; need 1/3 fewer calories Can’t raise basal metabolic rate – little weight loss with exercise • Too much adipose tissue and not enough lean muscle mass – making them feel “mushy”

FOOD SEEKING • Incessant hunger makes person constantly think about food and how to get it • Body thinks it’s starving – survival instinct is stuck on ON • Person does whatever they have to do to obtain food • Out of their control – like you holding your breath and then body takes over and breathes for you

FOOD SEEKING AT SCHOOL • Should be expected • Most of it is opportunistic – result of failure of caretakers to follow rules • Forgive yourself & start again • Successful food stealing encourages food seeking • If occurring weekly, food security not established

FOOD STEALING • Ask for food – do not take it – let family know if child chooses to eat it • Establish consequence ahead of time – may require searches • Respond matter- offactly • Do not be angry, lecture or apologize • Once it’s over, it’s over

DANGERS OF MORBID OBESITY • Cardio-pulmonary Disease • Hypertension • Obstructive Sleep Apnea • Pickwickean Syndrome • Incontinence • Type II Diabetes – as early as 6 years old • Edema • Skin sores • Yeast Infections • Inability to walk • Right side heart failure

MORBID OBESITY

MORBID OBESITY Medical Implications • Growth charts with children • Regular weighing • Pulmonary functioning exams sometimes leading to sleep studies • Regular screening for Type II diabetes • Echocardiograms- right side heart failure • Care of skin and effects of self-abuse

DIETARY MANAGEMENT • • • Supervision around food & no food around Modified lunch menus No money at school Pre-plan parties & treats – do not exclude Watch for food trading & the generosity of children

SECONDARY MANIFESTATIONS • • • Almond-shaped eyes Tented upper lip Narrow temples Narrow jaw Larger space between nose and mouth • Straight ulnar border • • • Smaller hands & feet “Pear-shaped”torso Short stature Hypo pigmentation Thicker saliva leading to dental problems

FACIAL FEATURES
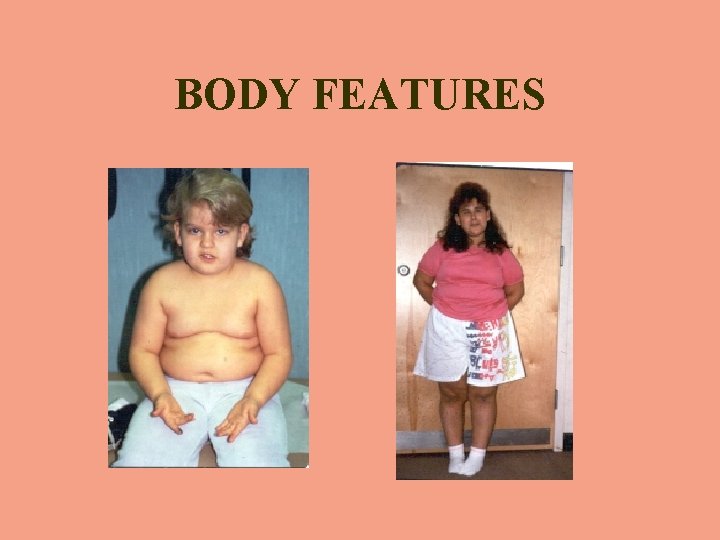
BODY FEATURES

HYPOTHALAMUS DYSFUNCTION • • • Brain arousal Internal body temperature High pain tolerance Difficulty with or inability to vomit Reactions to medications is different Symptoms of illness

EXPERIENCE OF ILLNESS • The body registers the pain or illness but the mind does not perceive it • The person acts out the pain or illness. Disorientation. Vomiting. Confusion. Memory loss. Fatigue. Odd behaviors. Loss of appetite. Loss of interest

RECENT MEDICAL ISSUES • • • Gorging Water Intoxication Rectal Digging Hernias Gastro-Intestinal Complaints • Aspiration • Thyroid Problems • Acute Idiopathic Gastric Dilation

CHECK THE BODY FIRST INTERNALLY • X-RAYS • ULTRASOUNDS • LAB WORK

THE HYPOTHALAMUS & EMOTIONS • • • Mood Swings Disproportionate emotional responses Temper tantrums Longer calming time Clinical depression Psychosis

• • THE HYPOTHALAMUS & BEHAVIOR Obsessive/compulsive Inflexibility Perseveration Stubbornness Hoarding Aggression/violence Self-trauma

STRESS & BEHAVIOR • Due to genetic reality people with PWS more vulnerable to stress • PWS itself is a stressor • Access to food and food itself is a stressor • Too much independence can be a stressor • Crisis for persons with PWS is the conflict between environment and their personalities and coping mechanisms

STRESS, BEHAVIOR & FOOD • Lack of food security = Hope = Disappointment = Stress = Behaviors • Food security = No hope = No disappointment = No stress = No behaviors

DEVELOPMENTAL DELAYS AND BEHAVIOR • Delay at the narcissistic stage of development – around 3 years of age • Delay at around 12 years of age in judgment

BEHAVIOR APPROACH • Look at underlying stressors not each individual behavior • Often stressors can be modified with environmental modifications • Reduction of stressors often leads to diminishment of behaviors without the need for medication

A WAY OF LOOKING AT BEHAVIOR When behaviors occur look at: 1. Physical illness 2. Stressors 3. Medications – SSRI’s can trigger the mood instability

3 MAIN WAYS TO MANAGE PWS BEHAVIORS • STRUCTURE • CONSISTENCY • PREDICTABILITY

THE THERAPEUTIC MILIEU • Structured daily plan • Rules • Reward Management System • Consequence System • Environmental Controls • Communication • Staff Supervision • Food Security

REWARD MANAGEMENT SYSTEM • Defined system of daily rewards & weekly reinforcers • Visual reminders – point sheet or chart • Reinforcers must be varied & interesting to the person • Individual needs to be involved in choosing reinforcers • Frequent random praise • Data sheets to document progress

BEHAVIOR CONTRACTS • • • Identify target behaviors – around 3 or 4 Write out what is expected Write out consequence Have person & team sign contract Give points on a set time frame for absence of target behaviors – differential reinforcement • Points translate into tokens

CONSEQUENCE SYSTEM • Defined system of consequence – initially thoroughly presented to person & then given low attention • Consequences given non-confrontationally • Not to be used as a threat • Must be consistently enforced and cannot be changed arbitrarily

INTERVENTIONS • Must have pre-planned interventions for the following PWS possibilities: . Elopement – running away. Removal to a quiet place to calm. Ability to have person remain in quiet place until they do calm down. Physical aggression against self or others requiring an intervention

FOOD SECURITY • All elements of meals need to be set in advance • No arbitrary changes • Planned & posted menus • Limit discussion about food – DON’T ARGUE • All staff trained on diet

SUGGESTED INTERVENTIONS FOR PWS BEHAVIOR • • Stubborn Opposition Negativism, Arguing, Defiance Perseveration Temper Tantrums Intermittent Explosiveness Physical aggression Skin Picking

STUBBORN OPPOSITION • Planned ignoring of harmless negativity and opposition – wait it out • Give praise immediately for positive behaviors as soon as exhibited • Do not comfort or cajole • Briefly restate request and then stop talking • Remain neutral

NEGATIVISIM, ARGUING & DEFIANCE • • Use prearranged prompts & cues Use low attention & redirection Do not continue to respond back Do not engage in arguing, simply restate the rule or expectation • Let the person have the last word • Show with your demeanor that you are calm and not going to change your mind.

PERSEVERATION • Planned ignoring – answer question once or explain once then STOP – to continue will give negative attention & reinforcement • Redirection – if person is truly stuck, reduce stimulus in environment & try to redirect • Give praise as soon as topic of perseveration changes

TEMPER TANTURMS • Control physical environment to ensure safety • Ignore behavior completely if actions not immediately dangerous • Give mild & neutral praise when person is calm and move on

PHYSICAL AGGRESSION • Control environment – remove objects that might be thrown; secure exits if person elopes • Give verbal prompts to calm • Intervene physically if there is imminent danger to person or others

SKIN PICKING • Low attention; Redirection • Do not punish – must live with natural consequences • Make a contract about picking. Take a picture of lesion. Put antibiotic on wound 4 or more times a day. Establish a small reward for healing – reward the healing, rather than the not picking. Expect picking at a new area

WELL MANAGED PWS

ANOTHER
A BABY

AND TWO OTHERS

OUT & ABOUT

AT THE PROM
- Slides: 62