Practice Guidelines for Obstetric Anesthesia An Updated Report


Practice Guidelines for Obstetric Anesthesia An Updated Report by the American Society of Anesthesiologists Task Force on Obstetric Anesthesia and the Society for Obstetric Anesthesia and Perinatology Anesthesiology, V 124 • No 2 270 February 2016

Purposes of the Guidelines �� quality of anesthetic care �� patient safety ��incidence/severity of anesthesiarelated complications �� patient satisfaction
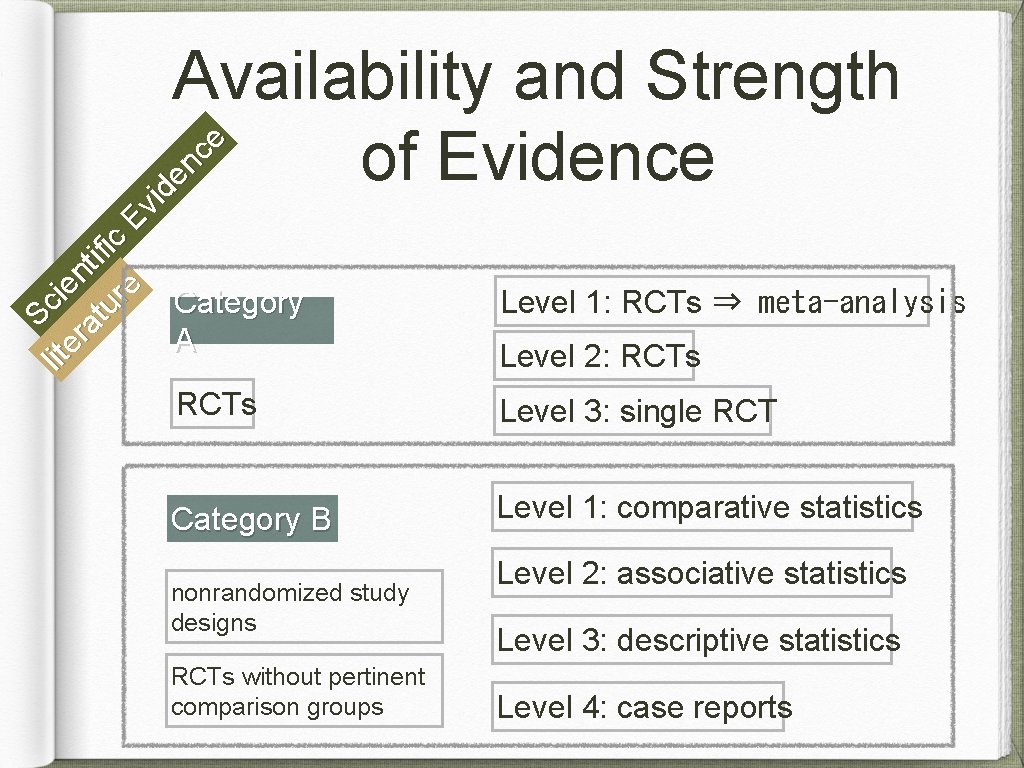

Sc lit er ien at tif ur ic e Ev id en ce Availability and Strength of Evidence Category A Level 1: RCTs ⇒ meta-analysis Level 2: RCTs Level 3: single RCT Category B Level 1: comparative statistics nonrandomized study designs RCTs without pertinent comparison groups Level 2: associative statistics Level 3: descriptive statistics Level 4: case reports

S Ev cie lit id nt er e ifi at nc c ur e e Availability and Strength of Evidence Insufficient Literature unavailable evidences beneficial (B) Evidence direction harmful (H) equivocal (E)

• O • su E pin In rve vid io • co tern y en n-b • let mm et dat ce as ed ed ter e -ba a ito s nts se ria d ls Availability and Strength of Evidence Category A • • • Strongly Agree Equivocal Disagree Strongly Disagree • • Membership Opinion • active ASA members • • Strongly Agree Equivocal Disagree Strongly Disagree Expert Opinion Task Force – appointed expert consultants Category B Category C Informal Opinion

Guidelines 2

Anesthetic Care for Labor and Vaginal Delivery • timing of neuraxial analgesia and outcome of labor • neuraxial analgesia and trial of labor after prior cesarean delivery • anesthetic/analgesic techniques Dr. Dariush Abtahi
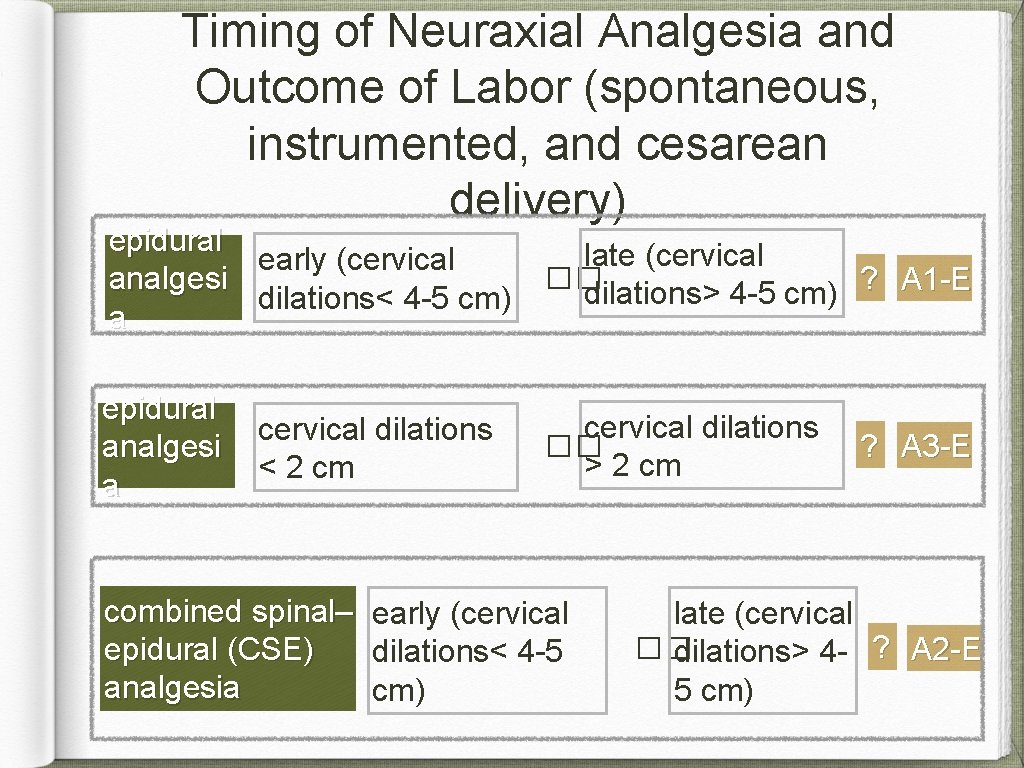
Timing of Neuraxial Analgesia and Outcome of Labor (spontaneous, instrumented, and cesarean delivery) epidural late (cervical early (cervical �� ? analgesi A 1 -E dilations> 4 -5 cm) dilations< 4 -5 cm) a epidural analgesi a cervical dilations < 2 cm combined spinal– epidural (CSE) analgesia cervical dilations �� > 2 cm early (cervical dilations< 4 -5 cm) ? A 3 -E late (cervical �� dilations> 4 - ? A 2 -E 5 cm)

Timing of Neuraxial Analgesia and Outcome of Labor Recommendations: Provide patients in early labor (< 5 cm dilation) the option of neuraxial analgesia. Offer neuraxial analgesia on an individualized basis regardless of cervical dilation. Reassure patients that the use of neuraxial analgesia does not increase the incidence of cesarean delivery.

Neuraxial Analgesia and Trial of Labor after Prior Cesarean Delivery { epidural analgesia mode of delivery duration of labor adverse outcomes ? B 1 -E Recommendations: Offer neuraxial techniques Consider early placement of a neuraxial catheter (labor analgesia/anesthesia in the event of operative delivery)

Anesthetic/analg esic techniques • early insertion of a neuraxial catheter for complicated parturients • CIE analgesia • epidural LAs + opioids • high vs. low concentrations of LAs • single-injection spinal opioids ± LAs • pencil-point spinal needles • CSE analgesia

Early Insertion of a Neuraxial Catheter for Complicated Parturients ? �� maternal / neonatal outcomes Recommendations: Consider early insertion of a neuraxial catheter for obstetric (twin gestation/preeclampsia) or anesthetic indications (anticipated difficult airway/obesity) to reduce the need for GA if an emergent procedure becomes necessary. In these cases, the insertion of a neuraxial catheter may precede the onset of labor or a patient’s request for labor analgesia.
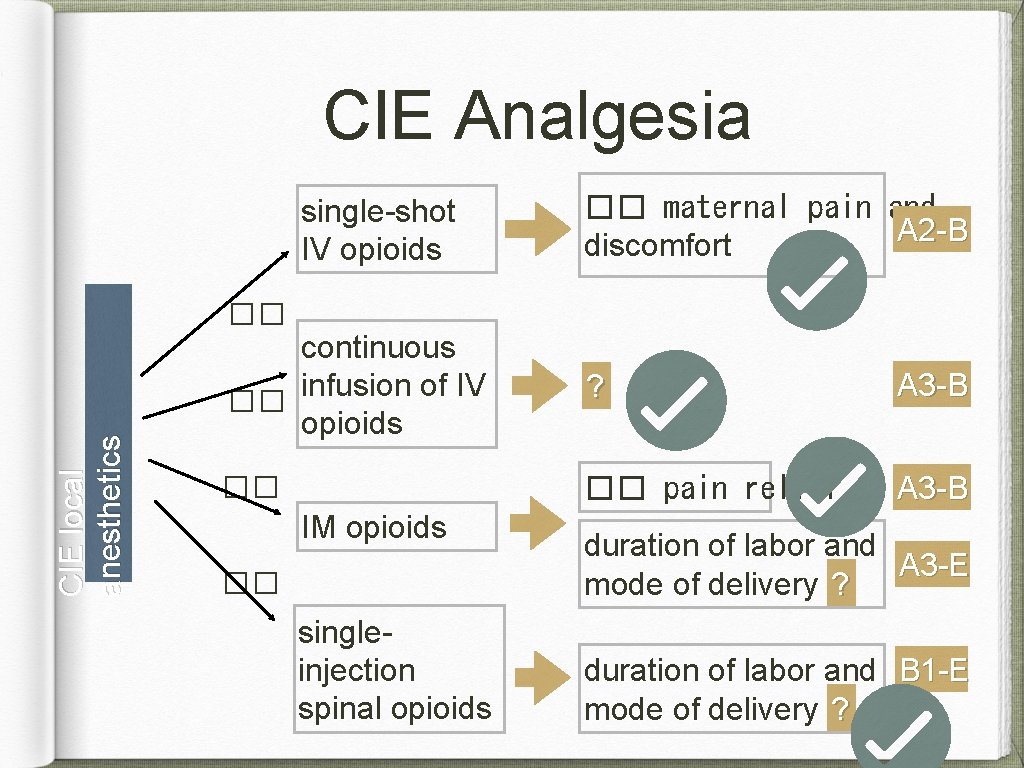
CIE Analgesia single-shot IV opioids �� maternal pain and A 2 -B discomfort CIE local anesthetics �� continuous infusion of IV �� opioids ? A 3 -B �� �� pain relief A 3 -B IM opioids �� singleinjection spinal opioids duration of labor and A 3 -E mode of delivery ? duration of labor and B 1 -E mode of delivery ?

CIE Analgesia Recommendations: Continuous epidural infusion may be used. When a continuous epidural infusion of local anesthetic is selected, an opioid may be added to: �� concentration of local anesthetic �� quality of analgesia �� motor block
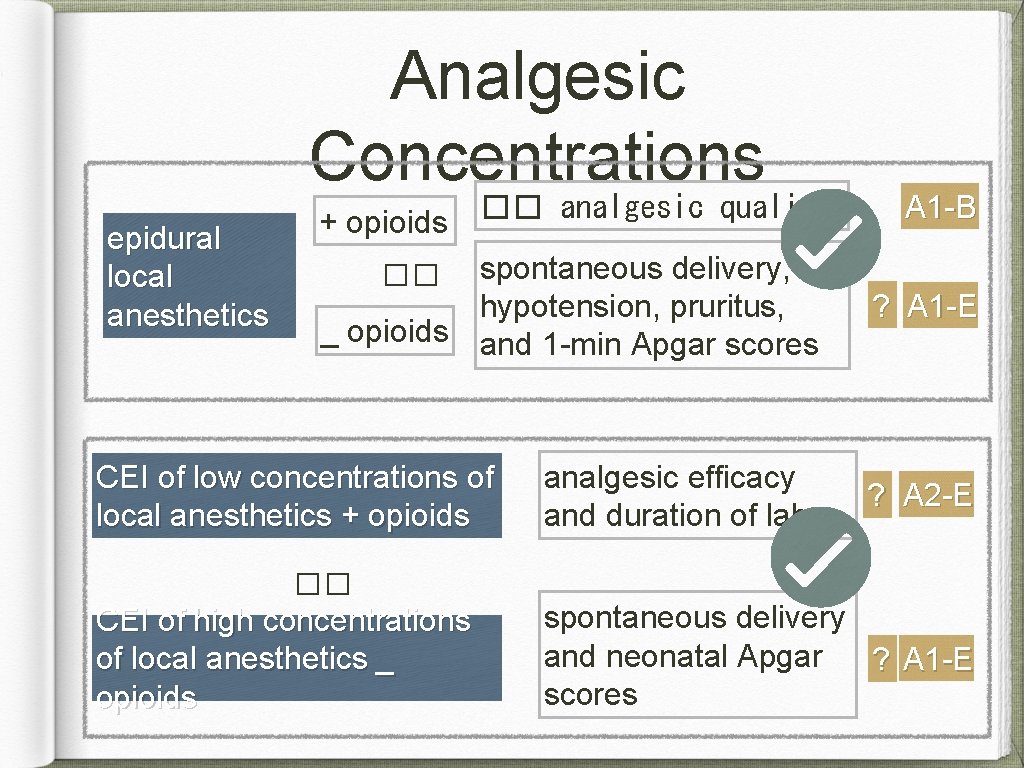

Analgesic Concentrations epidural local anesthetics �� analgesic quality + opioids �� spontaneous delivery, hypotension, pruritus, _ opioids and 1 -min Apgar scores CEI of low concentrations of local anesthetics + opioids A 1 -B ? A 1 -E analgesic efficacy ? A 2 -E and duration of labor �� CEI of high concentrations of local anesthetics _ opioids spontaneous delivery and neonatal Apgar ? A 1 -E scores

Analgesic Concentrations low concentrations of local anesthetics �� frequency of motor block A 1 -B epidural local anesthetics + opioids other maternal outcomes (hypotension, nausea, pruritus, respiratory depression, and urinary retention) Recommendations: Use dilute concentrations of local anesthetics with opioids to produce as little motor block as possible. ?
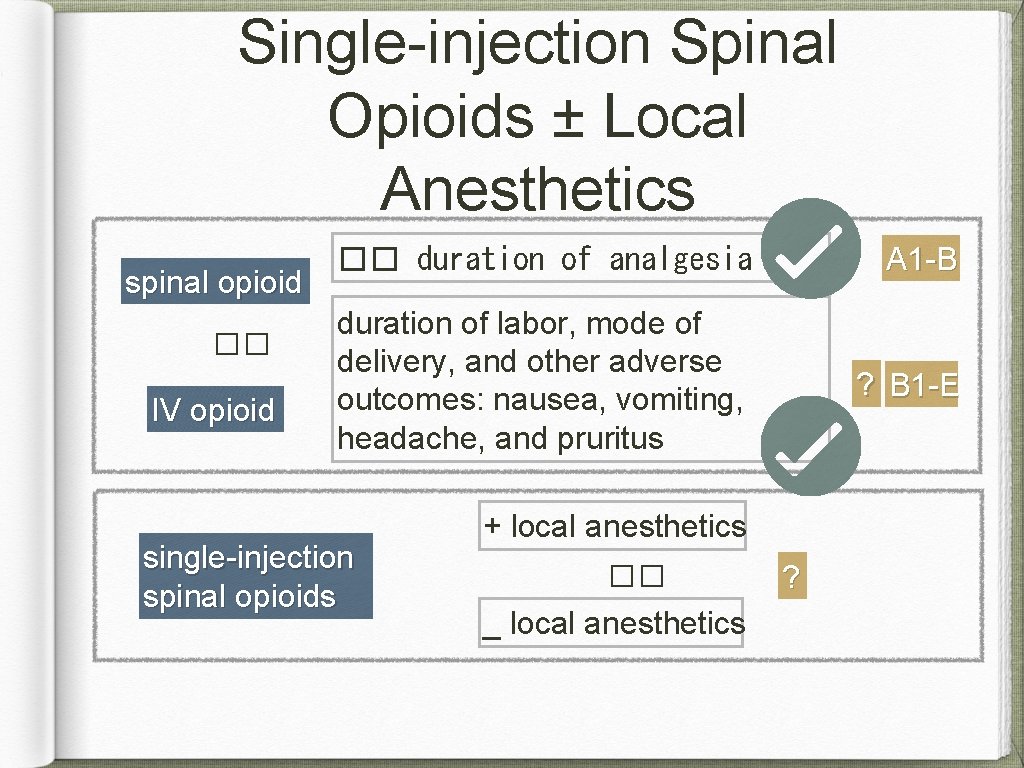
Single-injection Spinal Opioids ± Local Anesthetics spinal opioid �� IV opioid �� duration of analgesia A 1 -B duration of labor, mode of delivery, and other adverse outcomes: nausea, vomiting, headache, and pruritus ? B 1 -E single-injection spinal opioids + local anesthetics �� _ local anesthetics ?

Single-injection Spinal Opioids ± Local Anesthetics Recommendations: effective/time- limited, analgesia If labor duration is anticipated to be longer than the analgesic effects of the spinal drugs chosen, or if there is a reasonable possibility of operative delivery, then consider a catheter technique instead of a single-injection technique. A local anesthetic may be added to a spinal opioid to �� duration and �� quality of analgesia.
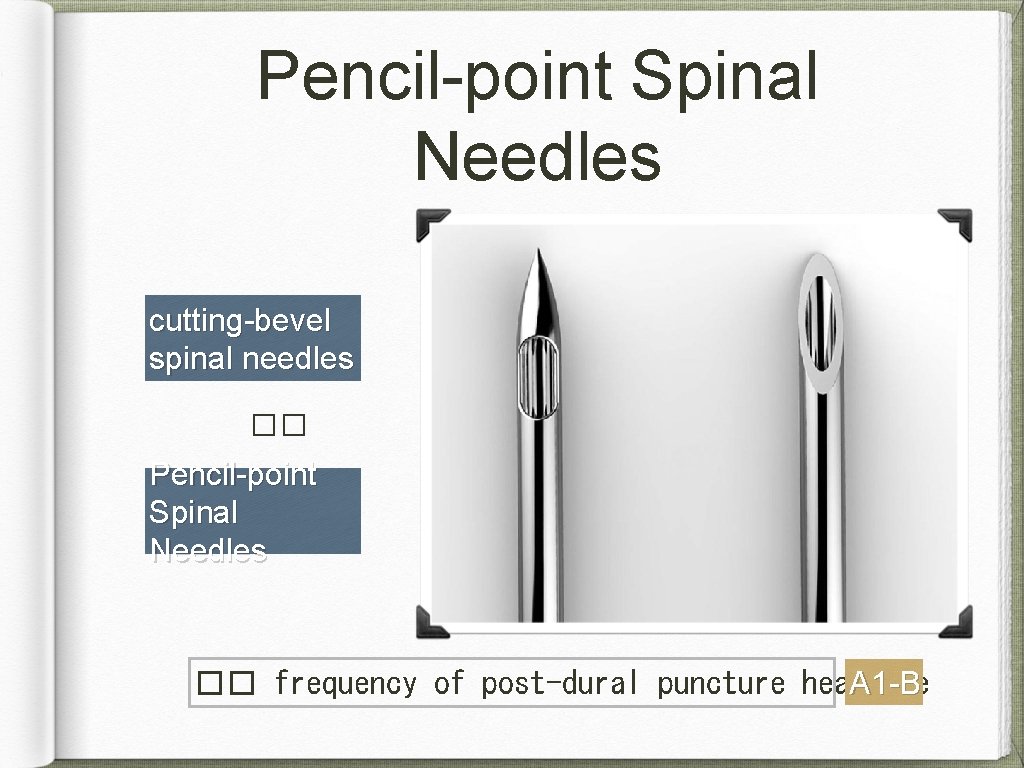
Pencil-point Spinal Needles cutting-bevel spinal needles �� Pencil-point Spinal Needles �� frequency of post-dural puncture headache A 1 -B
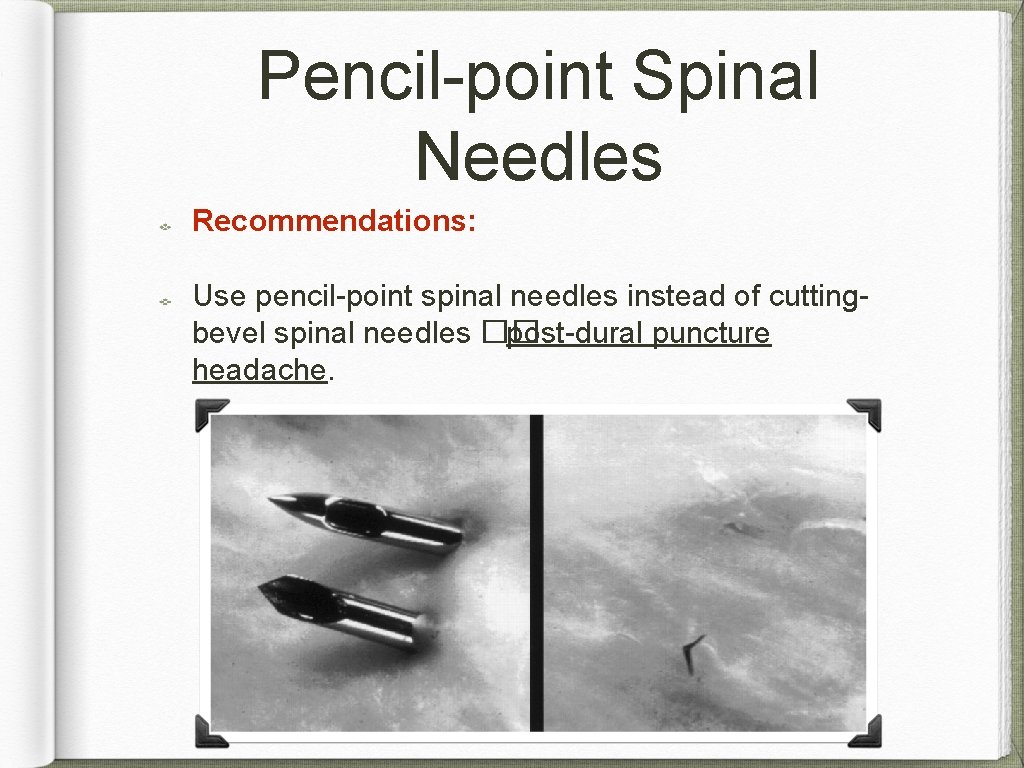
Pencil-point Spinal Needles Recommendations: Use pencil-point spinal needles instead of cuttingbevel spinal needles �� post-dural puncture headache.

CSE Analgesia CSE local anesthetics + opioids �� analgesia �� onset time A 2 -B epidural local anesthetics �� + opioids • • • analgesia mode of delivery hypotension pruritus 1 -min Apgar scores ? A 1 -E

CSE Analgesia Recommendations: If labor duration is anticipated to be longer than the analgesic effects of the spinal drugs chosen, or if there is a reasonable possibility of operative delivery, then consider a catheter technique instead of a single-injection technique. CSE techniques may be used to provide effective and rapid onset of analgesia for labor.
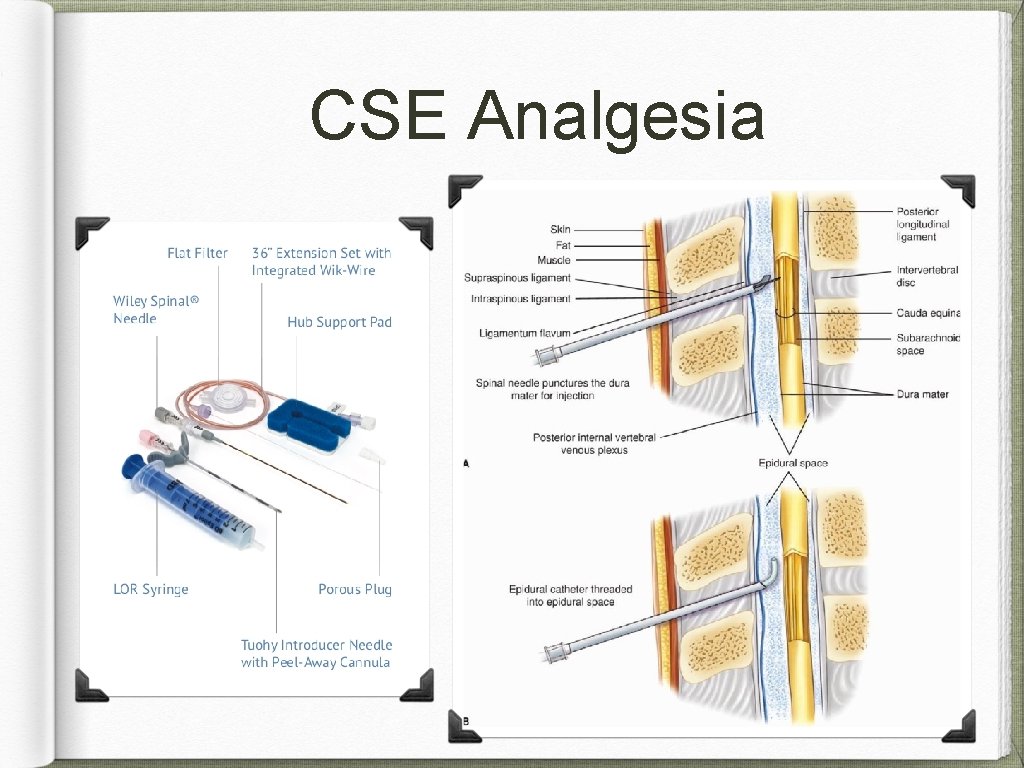
CSE Analgesia

Patient-controlled Epidural Analgesia �� analgesic consumption A 1 -B PCEA �� CIE • • duration of labor mode of delivery ? A 1 -E motor block 1 - and 5 -min Apgar scores PCEA + �� analgesic efficacy background infusion A 1 -B �� mode of delivery, PCEA _ background infusion frequency of motor block ? A 1 -E

Patient-controlled Epidural Analgesia Recommendations: An effective and flexible approach for the maintenance of labor analgesia. preferable to fixed-rate CIE, �� dosages of local anesthetics PCEA may be used ± background infusion
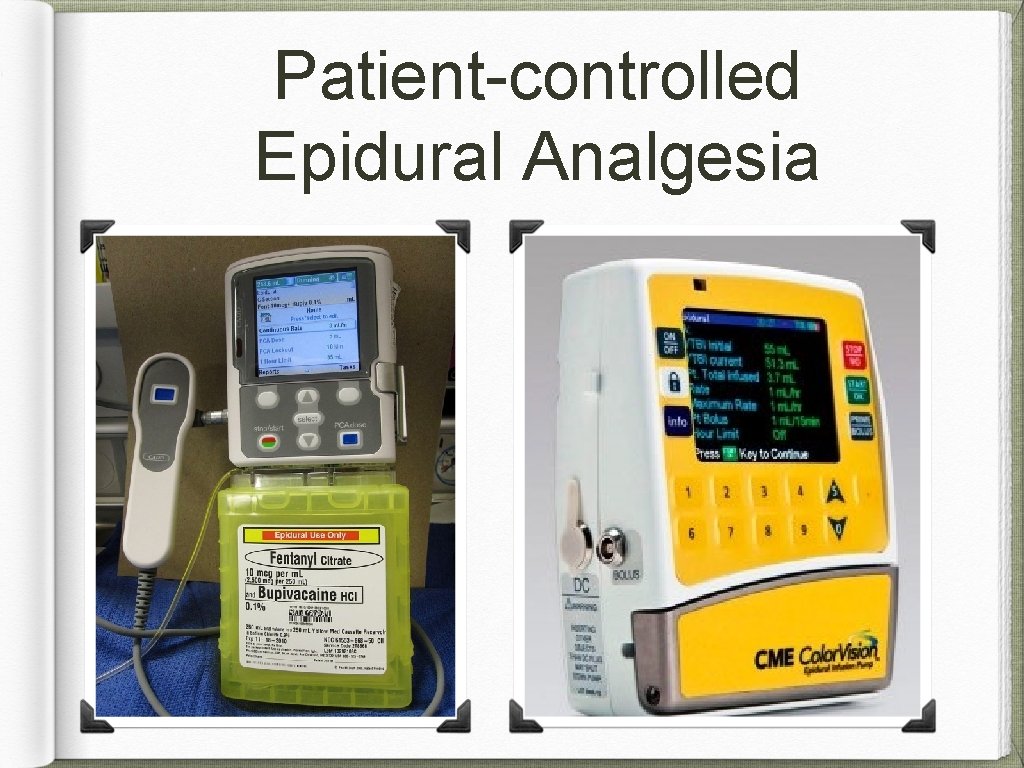
Patient-controlled Epidural Analgesia

Removal of Retained Placenta • anesthetic techniques for removal of retained placenta • nitroglycerin for uterine relaxation

Anesthetic Techniques Recommendations: No preferred anesthetic technique. If an epidural catheter in place + stable hemodynamics⇒ epidural anesthesia Assess hemodynamic status before neuraxial anesthesia Aspiration prophylaxis Titrate sedation/analgesia (respiratory depression/pulmonary aspiration) Major maternal hemorrhage + hemodynamic instability⇒ GA + endotracheal tube

Nitroglycerin for Uterine Relaxation inconsistent findings A 2 -E Successful uterine relaxation B 3/B 4 Recommendations: Alternate to terbutaline sulfate/GA + halogenated agents incremental doses (IV/sublingual) to sufficiently relax the uterus

Anesthetic Care for Cesarean Delivery • Equipment, facilities, support personnel • General, epidural, spinal, CSE anesthesia • IV fluid preloading/co-loading • Ephedrine/phenylephrine • Neuraxial opioids for postoperative analgesia after neuraxial anesthesia

Equipment, Facilities, and Support Personnel Recommendations: Equipment, facilities, support personnel available in the labor and delivery operating suite = main operating suite

Equipment, Facilities, and Support Personnel Resources for the treatment of potential complications: failed intubation inadequate analgesia/anesthesia hypotension respiratory depression local anesthetic systemic toxicity pruritus, and vomiting Equipment and personnel for obstetric patients recovering from neuraxial or GA.
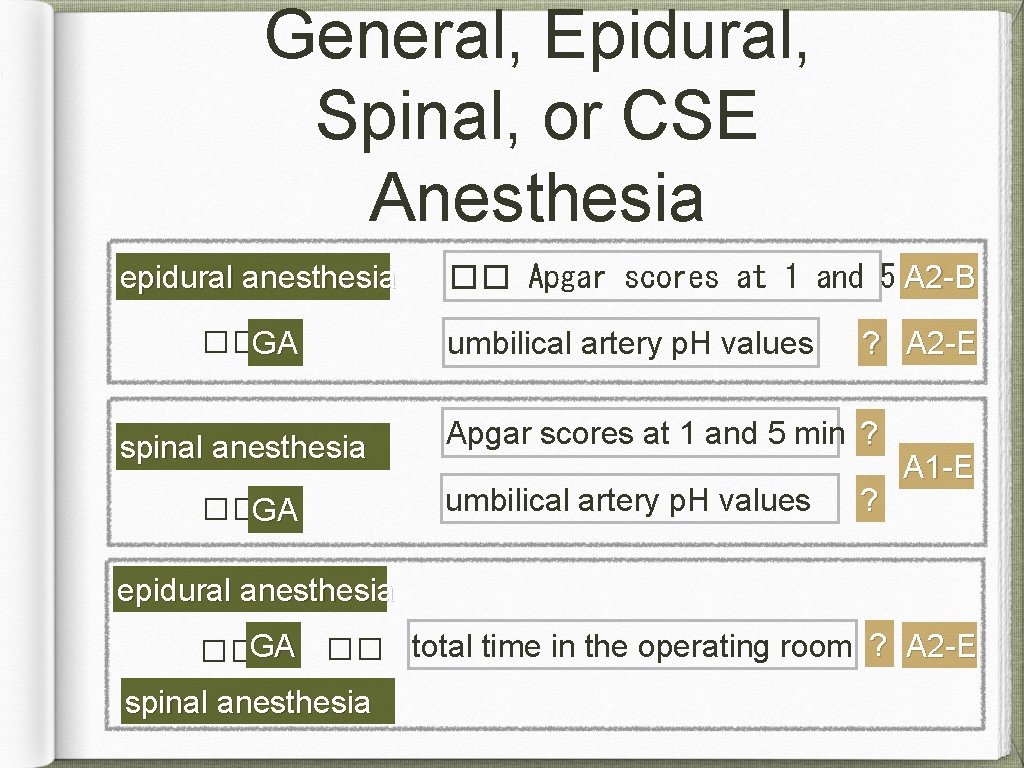
General, Epidural, Spinal, or CSE Anesthesia epidural anesthesia ��GA spinal anesthesia ��GA �� Apgar scores at 1 and 5 A 2 -B min umbilical artery p. H values ? A 2 -E Apgar scores at 1 and 5 min ? umbilical artery p. H values ? A 1 -E epidural anesthesia ��GA �� total time in the operating room ? A 2 -E spinal anesthesia

General, Epidural, Spinal, or CSE Anesthesia Recommendations: Anesthetic technique should be individualized: anesthetic, obstetric, fetal risk factors (elective vs. emergency), the preferences of the patient, and the judgment of the anesthesiologist. Uterine displacement should be maintained until delivery Neuraxial techniques in preference to GA for most cesarean deliveries

General, Epidural, Spinal, or CSE Anesthesia Pencil-point spinal needles instead of cuttingbevel spinal needles. For urgent cesarean delivery, an indwelling epidural catheter may be used as an alternative to initiation of spinal or GA. GA may be the most appropriate choice in some circumstances (profound fetal bradycardia, ruptured uterus, severe hemorrhage, and severe placental abruption).

IV Fluid Preloading or Co-loading IV fluid preloading or co-loading �� frequency of hypotension after SA ? A 2 -E frequency of ? hypotension after SA A 2 -E no fluids IV fluid preloading �� IV fluid co-loading

IV Fluid Preloading or Co -loading Recommendations: IV fluid preloading/co-loading: �� frequency of hypotension after spinal anesthesia Do not delay the initiation of spinal anesthesia in order to administer a fixed volume of IV fluid.
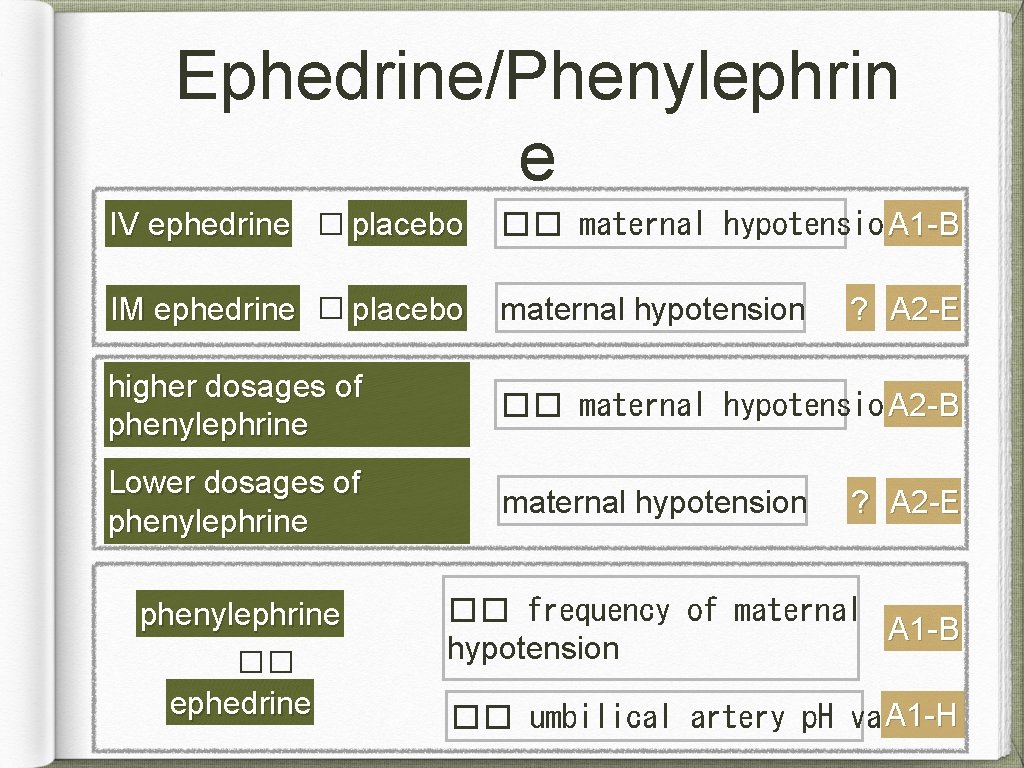
Ephedrine/Phenylephrin e IV ephedrine �� placebo �� maternal hypotension. A 1 -B IM ephedrine �� placebo maternal hypotension higher dosages of phenylephrine �� maternal hypotension. A 2 -B Lower dosages of phenylephrine maternal hypotension phenylephrine �� ephedrine ? A 2 -E �� frequency of maternal A 1 -B hypotension A 1 -H �� umbilical artery p. H values

Ephedrine or Phenylephrine Recommendations: Either IV ephedrine or phenylephrine may be used. In the absence of maternal bradycardia, consider selecting phenylephrine (improved fetal acid–base status in uncomplicated pregnancies).

Neuraxial Opioids for Postoperative Analgesia epidural opioids �� �� postoperative analgesia A 2 -B intermittent IV/IM opioids nausea, vomiting, pruritus ? A 1 -E �� postoperative analgesia A 2 -B PCEA �� PCA nausea, vomiting, pruritus, sedation ? A 2 -E

Neuraxial Opioids for Postoperative Analgesia Recommendations: For postoperative analgesia after neuraxial anesthesia, consider selecting neuraxial opioids rather than intermittent injections of parenteral opioids.

Postpartum Tubal Ligation

neuraxial anesthesia ��GA ? impact of the timing of a postpartum tubal ligation on ? maternal outcome Recommendations: NPO for solid foods (6 - 8 h), depending on the type of food ingested (fat content). Aspiration prophylaxis Timing of the procedure - anesthetic technique should be individualized: anesthetic and obstetric risk factors (blood loss), and patient preferences

Neuraxial techniques in preference to GA for most postpartum tubal ligations. Gastric emptying will be delayed in patients who have received opioids during labor. An epidural catheter placed for labor may be more likely to fail with longer post-delivery time intervals.

Management of Obstetric and Anesthetic Emergencies • resources for management of hemorrhagic emergencies • equipment for management of airway emergencies • cardiopulmonary resuscitation

Resources for Management of Hemorrhagic Emergencies �� maternal complications Recommendations: Resources available to manage hemorrhagic emergencies In an emergency, type-specific or O-negative blood is acceptable. Intractable hemorrhage + banked blood is not available ⇒ intraoperative cell salvage

Table 1. Suggested Resources for Obstetric Hemorrhagic Emergencies • Large-bore IV catheters • Fluid warmer • Forced-air body warmer • Availability of blood bank resources • Massive transfusion protocol • Equipment for infusing IV fluids and blood products rapidly. • hand-squeezed fluid chambers, hand-inflated pressure bags, and automatic infusion devices

Equipment for Management of Airway Emergencies �� maternal, fetal, and neonatal complications B 4 -B Recommendations: pulse oximeter and carbon dioxide detector. Basic airway management equipment should be immediately available during neuraxial analgesia. Portable equipment for difficult airway management

Equipment for Management of Airway Emergencies A pre formulated strategy for intubation of the difficult airway failed tracheal intubation⇒ ventilation with mask + cricoid pressure or a supraglottic airway device (laryngeal mask airway, intubating laryngeal mask airway, or laryngeal tube) Not possible to ventilate or awaken the patient, ⇒ surgical airway

Table 2. Suggested Resources for Airway Management during Initial Provision of Neuraxial Analgesia in a Labor Delivery Room Setting • Laryngoscope and assorted blades • Endotracheal tubes, with stylets • Oxygen source • Suction source with tubing and tonsil suction tip • Self-inflating bag and mask for positive-pressure ventilation • Medications for blood pressure support, muscle relaxation, and hypnosis

Table 3. Suggested Contents of a Portable Storage Unit for Difficult Airway Management for Cesarean Section Rooms • Rigid laryngoscope blades of alternate design and size • Videolaryngoscopic devices • Endotracheal tubes of assorted size • Endotracheal tube guides (semirigid stylets, light wands, …) • At least one device suitable for emergency nonsurgical airway ventilation- face mask/supraglottic airway device (laryngeal mask airway, intubating laryngeal mask airway, and laryngeal tube). • Equipment suitable for emergency surgical airway access (cricothyrotomy)

Cardiopulmonary Resuscitation Insufficient to evaluate the efficacy of cardiopulmonary resuscitation in the obstetric patient during labor and delivery. 4 to 5 min is the maximum time rescuers will have to determine whether the arrest can be reversed by Basic Life Support and Advanced Cardiac Life Support interventions.
Cardiopulmonary Resuscitation Delivery of the fetus may improve cardiopulmonary resuscitation of the mother by relieving aortocaval compression. The best survival rate for infants more than 24 to 25 weeks in gestation occurs when the delivery of the infant occurs no more than 5 min after the mother’s heart stops beating.

Cardiopulmonary Resuscitation Recommendations: Basic and advanced life-support equipment should be immediately available in the operative area of labor and delivery units. If cardiac arrest occurs, initiate standard resuscitative measures. Uterine displacement (usually left displacement) If maternal circulation is not restored within 4 min, cesarean delivery should be performed by the obstetrics team.

- Slides: 56