Practical Oncology Mast Cell Tumor Wendy Blount DVM

Practical Oncology Mast Cell Tumor Wendy Blount, DVM

Mast Cell Tumor • Mast cell granules contain histamine and heparin, among other things • Degranulation is largely responsible for symptoms • Release of histamine – Increased gastrin secretion (anorexia, ulcers, hematemesis) – Anaphylactoid reaction • Symptoms worse in CRF patients • Release of heparin – less clinically significant? ?
Mast Cell Tumor • Most often found on the skin or SC – Most common skin tumor in the dog (16 -21%) – Brachycephalics, Sharpeis & retrievers predisposed • Most common cancer in dogs • Also visceral & elsewhere – Gastrointestinal, Spleen, bone marrow • Less common sites – Oropharyngeal – Mediastinum – CNS – Nail bed, ocular & periocular

Mast Cell Tumor • Can have many different appearances • Can be infiltrated with fat – SC MCT resemble lipomas – Used to think more aggressive - false • Symptoms can be waxing and waning • Tumor gets bigger and smaller over time • 5 -15% have multiple masses at presentation • 20 -40% will have more MCT in the future, even if the first are cured (bully breeds)

Etiology • Allergic skin disease? • C-KIT mutation (aka SCFR, CD 117) – In “high risk MCT” (high grade II & all grade III) – These have decreased survival time – can be treated with tyrosine kinase inhibitors (Palladia® & Kinavet-CA 1® ) – C-KIT normally regulates proliferation, migration and differentiation – When C-KIT is mutated, it is constantly turned on, dysregulating cell growth an promoting malignancy

Clinical Signs • GI Signs – Anorexia, vomiting, melena • • • Pruritus and skin flushing Facial swelling Weakness, lethargy Delayed wound healing, bruising Darier’s Sign – swollen, itchy, red skin after scratching or stroking the skin
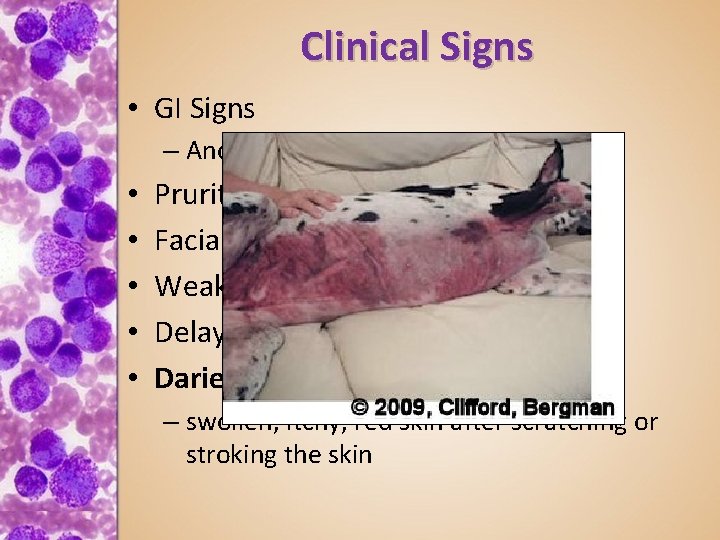
Clinical Signs • GI Signs – Anorexia, vomiting, melena • • • Pruritus and skin flushing Facial swelling Weakness, lethargy Delayed wound healing Darier’s Sign – swollen, itchy, red skin after scratching or stroking the skin

"A good leader takes a little more than his share of the blame, a little less than his share of the credit. " -- Arnold Glasow Attendee 12 – City TX "Surround yourself with the best people you can find, delegate authority, and don't interfere as long as the policy you've decided upon is being carried out. " -- Ronald Reagan

Diagnosis • FNA Cytology often diagnostic – Round cells + metachromatic granules – Granules intracellular or in background – Granules form a halo around the relatively pale nucleus (best seen at low power) – Eosinophils & basophils • Give diphenhydramine before or right after aspiration – FNA can cause degranulation – Dexamethasone as well if mass is visibly inflamed
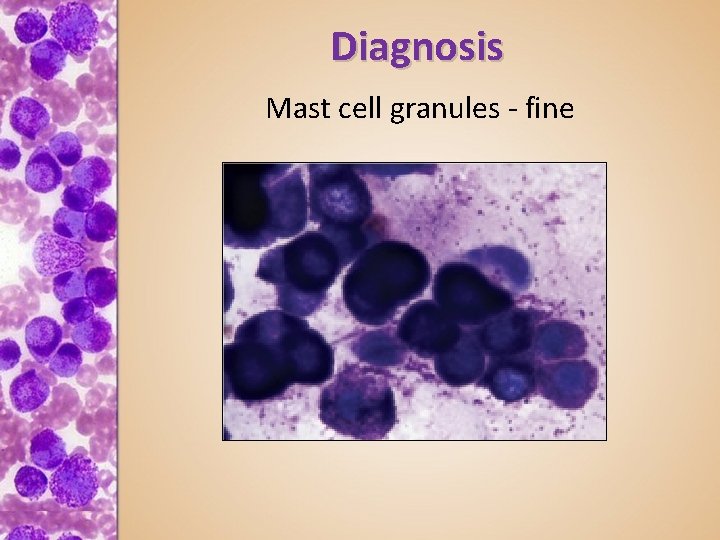
Diagnosis Mast cell granules - fine
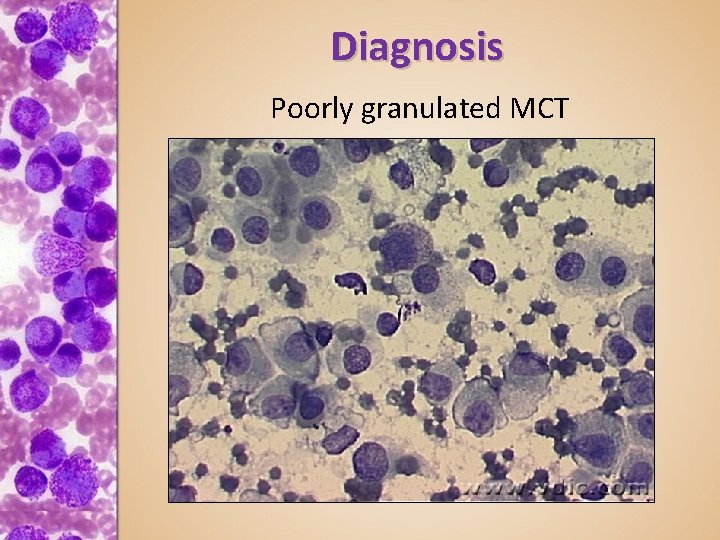
Diagnosis Poorly granulated MCT
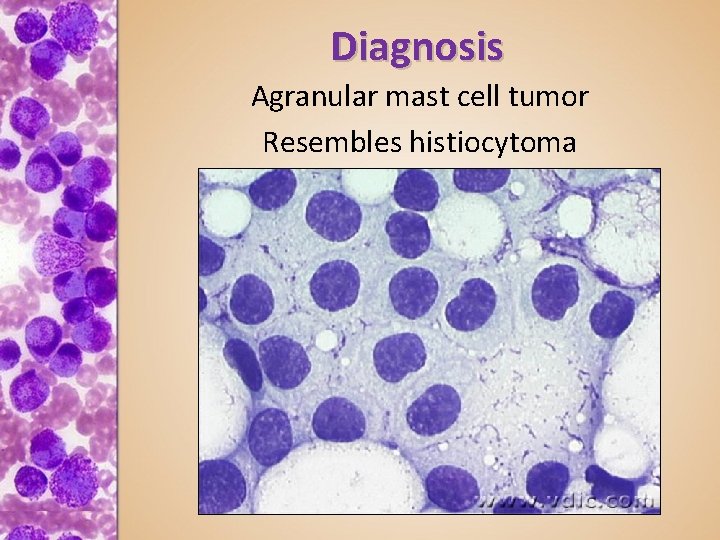
Diagnosis Agranular mast cell tumor Resembles histiocytoma
Sites of Metastasis • • Lymph node Liver & Spleen (Bone marrow) Almost never lungs

Staging for Metastasis 1. Histopathology for grading – Excisional if resectable – Incisional if not (May not heal well, Degranulation may be a problem) 2. FNA draining lymph node – Even if not large – some can have mets – Clusters of mast cells likely metastasis – Single mast cells likely not 3. Abdominal US + FNA liver and spleen – esp of MCT on rear of body – or abdominal rads – If US normal - Wright ways yes, Bergman says no 4. 2 view thoracic rads – esp if MCT on cranial body 5. CBC, panel, buffy coat in cats (poor man’s BM) 6. + Bone marrow in the dog (<8% +)
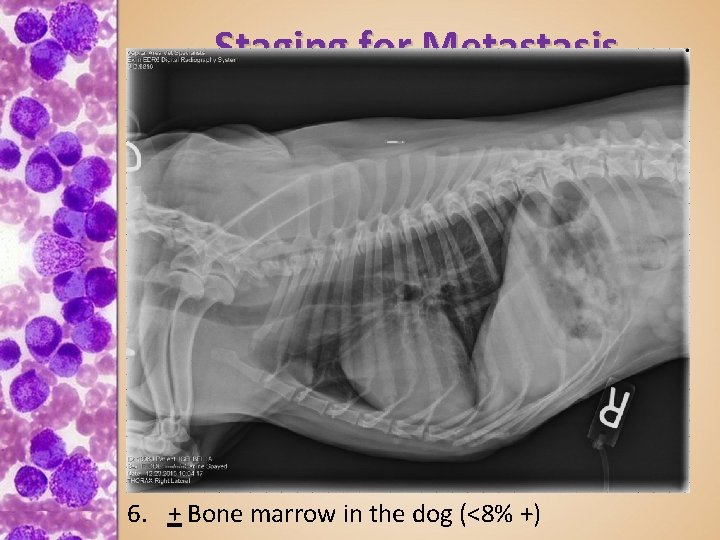
Staging for Metastasis 1. Histopathology for grading – Excisional if resectable – Incisional if not (May not heal well, Degranulation may be a problem) 2. FNA draining lymph node – Even if not large – some can have mets – Clusters of mast cells likely metastasis – Single mast cells likely not 3. Abdominal US + FNA liver and spleen – esp of MCT on rear of body – or abdominal rads – If US normal - Wright ways yes, Bergman says no 4. 2 view thoracic rads – esp if MCT on front body 5. CBC, panel, buffy coat in cats (poor man’s BM) 6. + Bone marrow in the dog (<8% +)

Staging for Metastasis • Staging not done for grade I MCT • Staging less important for high risk MCT – High grade II & Grade III – palliative treatment for best outcome • Palliative drugs, chemo, radiation – Cure is unlikely, especially for grade III (Maddie) • Staging most important for single local low grade II that is not resectable – If staging is clean for metastasis, then radiation can be curative (Sadie)
Staging for Metastasis • Consider partial staging for poor prognosticators, prior to surgery – Aggressive locations • • Scrotum nail bed Muzzle mucocutaneous junction – Visceral mastocytosis – Cytopenias (marrow)
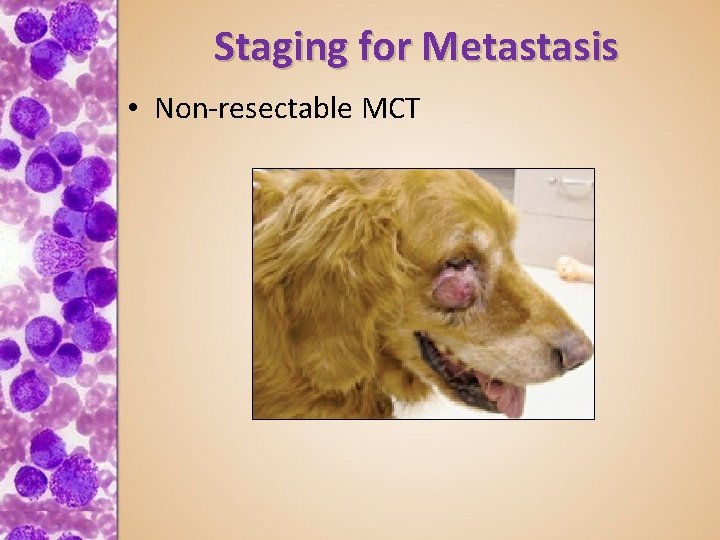
Staging for Metastasis • Non-resectable MCT
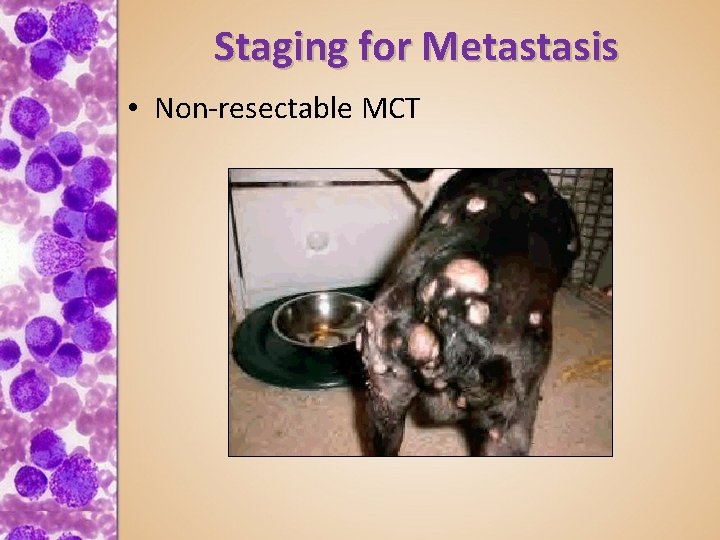
Staging for Metastasis • Non-resectable MCT
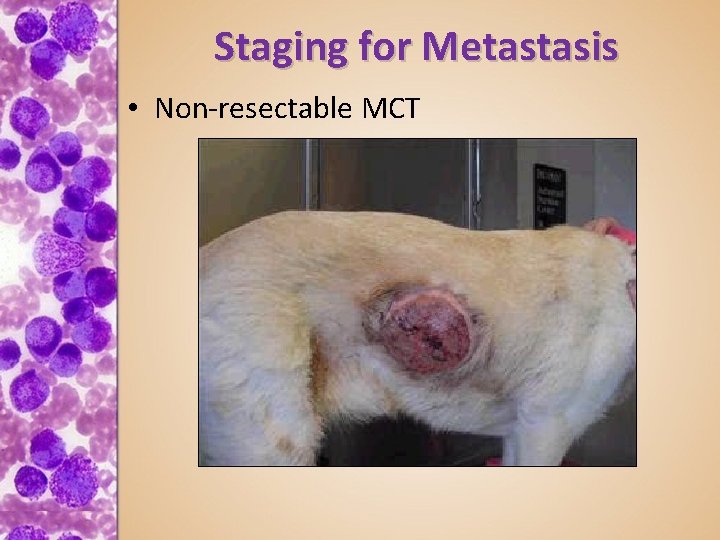
Staging for Metastasis • Non-resectable MCT
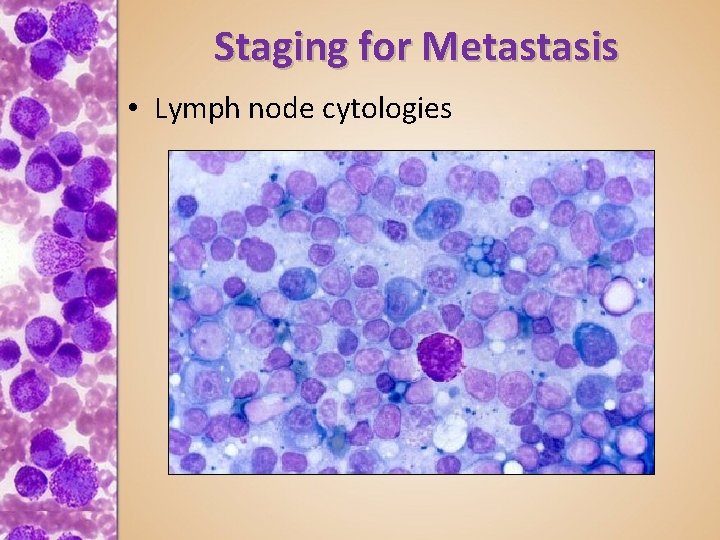
Staging for Metastasis • Lymph node cytologies
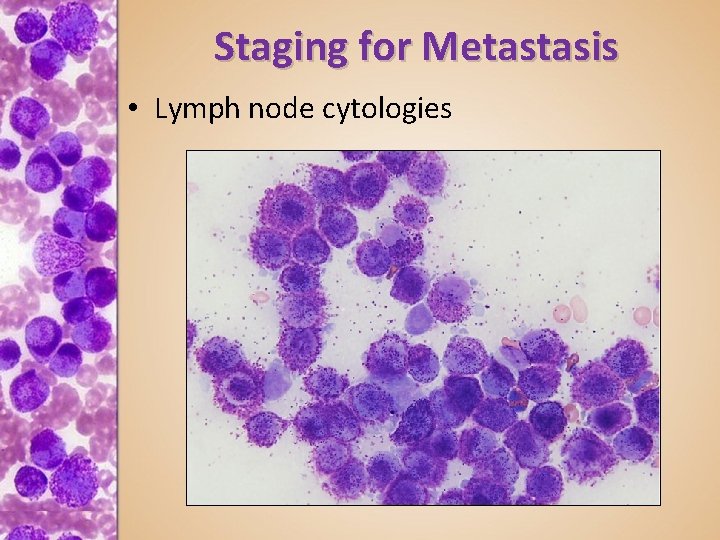
Staging for Metastasis • Lymph node cytologies
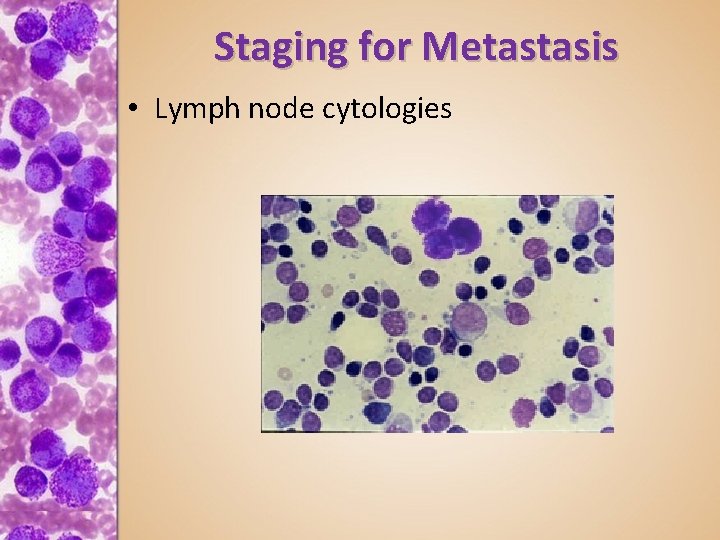
Staging for Metastasis • Lymph node cytologies
Tumor Stage (WHO) • Stage 0 – microscopic disease only • Stage I – tumor confined to the dermis • Stage II – tumor does not infiltrate subcutaneous tissues, lymph node metastasis • Stage III – large, infiltrating tumor (or multiple tumors) • Stage IV – distant metastasis Consideration is being given to reducing stage of multiple dermal tumors

Histopathology • • grade Mitotic Index (MI) Surgical margins – clean, narrow or dirty Invasiveness – dermal or invasive (subcutaneous/muscle) Histopathology tells a great deal about prognosis and treatment indicated for mast cell tumors Staging tells about prognosis but less about treatment, unless single unresectable low grade II

Histopathology • Are clean borders really clean? – Some MCT with dirty borders never recur • Normal mast cells attracted to the tumor by inflammation can be impossible to distinguish from neoplastic mast cells • Some 2 nd resections result in no tumor cells found in the resected tissue – In studies, as few <17 -38% of tumors with mast cells at the border recurred – studies do indicate that dirty borders adversely affect prognosis • Shorter survival times • Greater likelihood of local recurrence

"Too often we enjoy the comfort of opinion without the discomfort of thought. " -- John F. Kennedy Attendee 13 City TX "Men stumble over pebbles, never over mountains. " -- H. Emilie Cady

Histopathologic Grading • Grade I – well differentiated, behaves benignly (dermal in cats) • Grade II – intermediate differentiation, previously thought behavior widely variable – Low grade II – often behaves benignly – High grade II – may have C-kit mutation, often behaves malignantly • Grade III – anaplastic, aggressive behavior This is the Patnaik 3 Tier System, with high-low II (Kiupel – MSU 2 Tier) added – OPWG – Oncology Pathology Working Group 2013

Histopathologic Grading • Most path labs now give you high or low grade II in the report – Be sure to request Hi-Lo grade II *and* border reads • Mark borders – cranial and dorsal – Studies on same patients graded by each system & by multiple pathologists – 5 -10% histopath is errant
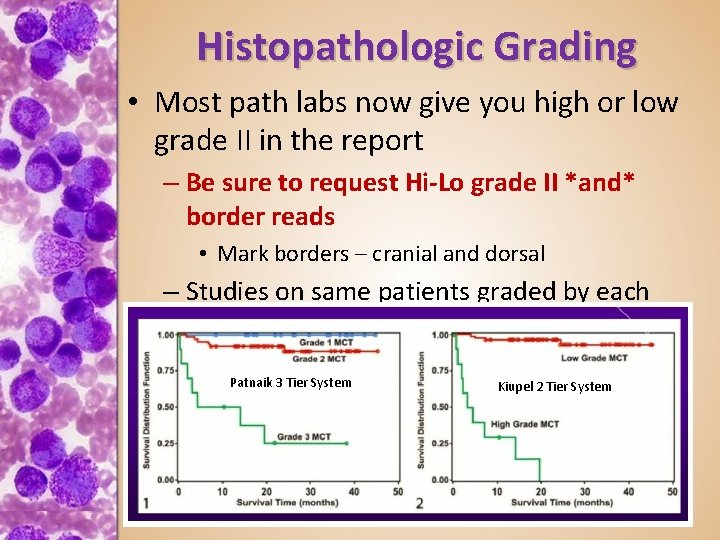
Histopathologic Grading • Most path labs now give you high or low grade II in the report – Be sure to request Hi-Lo grade II *and* border reads • Mark borders – cranial and dorsal – Studies on same patients graded by each system & by multiple pathologists – 5 -10% histopath is errant Patnaik 3 Tier System Kiupel 2 Tier System

MCT Prognostic Panel • MSU prognostic panel (form) – cost $200 -250 plus shipping • When to request the MCT prognostic panel – mixed message low grade II (after histopath) – Not indicated for grade I or III, and less important for high grade II – Grade II MCT with gray zone MI 4 -6/10 HPF – Rapidly growing mass that graded low – Low grade mass > 3 cm in size or not resectable – Location indicates poor prognosis, despite low grade – Low grade with clean but close margins (<4 -11 mm)

MCT Prognostic Panel • Facilitating the MCT panel – Send all MCTs for A+ clients to a lab that does the panel, so request is easy – Send tumor borders to your regular lab & keep the center of the tumor to send if MCT panel at another lab is needed – Use TVMDL - they are cooperative about forwarding paraffin sections for prognostic panel – Antech and Idexx are streamlined to provide the prognostic panel if requested after histopath

MCT Prognostic Panel • What to do if MCT prognostic panel says the tumor is an aggressive one – Supports radiation when borders are clean but close – Supports adjunctive chemo in addition to radiation for a grade II with dirty borders and no mets on staging – intent to cure • Maybe even when borders are clean (5 -10% local recurrence on clean borders) • Especially helpful for “clean but close” – 4 -11 mm – More aggressive follow ups for more aggressive tumors

Surgery • Mainstay of low grade MCT treatment (8090% cure with surgery) • Mast Cell Tumors often extend well beyond the visible mass • Diagnose by FNA before you excise!! • Lateral margins 2 -3 cm beyond visible mass – Small tumors <1 cm, 1. 5 -2 cm margins may be adequate (all these arbitrary) • One fascia layer deep to visible mass • Avoid manipulating the tumor • Intraoperative cytologies on 4 lateral and deep margins can be helpful
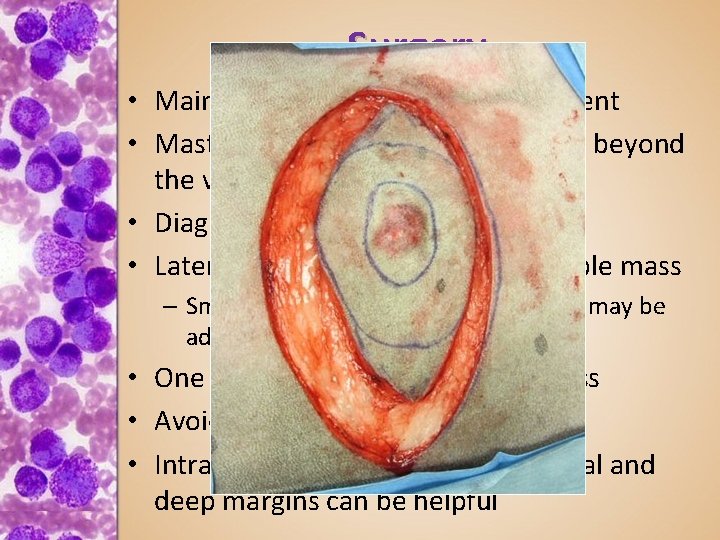
Surgery • Mainstay of low grade MCT treatment • Mast Cell Tumors often extend well beyond the visible mass • Diagnose by FNA before you excise • Lateral margins 2 -3 cm beyond visible mass – Small tumors <1 cm, 1. 5 -2 cm margins may be adequate • One fascia layer deep to visible mass • Avoid manipulating the tumor • Intraoperative cytologies on 4 lateral and deep margins can be helpful

Surgery – Neoadjuvant Prednisone for pre-surgical cytoreduction • Out of favor by some oncos at this time • I still like to use it (Wright also does) – Stabilizes lysosomal membranes – may prevent degranulation caused by surgery – Controls inflammation around the tumor so tumor borders are easier to see – Usually makes the dog feel better, so client perceives better toleration of surgery • Prednisone 40 mg/m 2 PO SID x 7 days, then 20 mg/m 2 PO SID x 7 days, then QOD
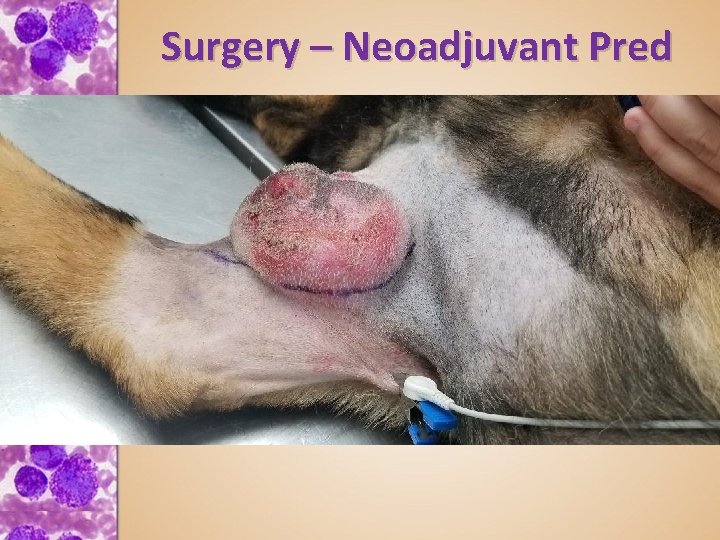
Surgery – Neoadjuvant Prednisone for pre-surgical cytoreduction • VCS 2018 – Klahn et al – 10 -14 days pred prior to surgery does not adversely affect histopathology grading • Doug Posey, DVM – “Shadow”
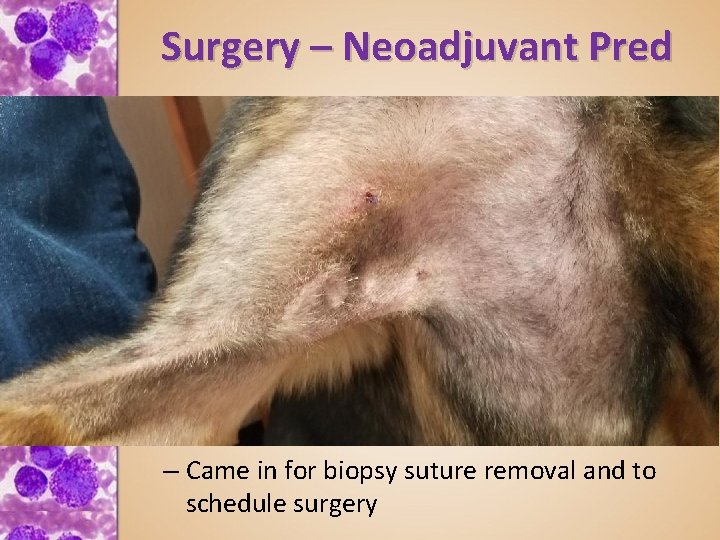
Surgery – Neoadjuvant Prednisone for pre-surgical cytoreduction • VCS 2018 – Klahn et al – 10 -14 days pred prior to surgery does not adversely affect histopathology grading • Doug Posey, DVM – “Shadow” – Incisional biopsy for grading – grade I – Post-biopsy neoadjuvant prednisone. amoxicillin and hydroxyzine, in preparation for cytoreductive surgery – Came in for biopsy suture removal and to schedule surgery

Surgery Re-excision where borders are dirty on grade I or II Grade III tumors considered systemic – More surgery only for local palliation • 2 -3 cm beyond original surgery • One fascia layer deeper than original surgery • Complete resection results in long survival • If clean borders, 95% cured with second excision, using these rules

Surgery Advanced Neo. Adjuvant Therapy • Given to a patient with non-resectable tumor in hopes of making it resectable • Chemotherapy and/or radiation • Best managed by medical and/or radiation oncologists • Need to understand effects of neoadjuvant therapy on healing and when and how to do surgery

Chemotherapy • Indications for MCT chemotherapy – MCT with clean borders -- palliation • high grade II and grade III MCT • Aggressive location – MCT with dirty borders + radiation • Radiation more likely to be curative – multiple dermal MCT when removing all becomes impossible *and* physical palliation is needed (e. g. , ulceration) – Non-resectable tumors – high or low grade

Chemotherapy • Indications for MCT chemotherapy – To palliate metastatic or systemic disease – Concurrent conditions precluding surgery or multiple sedations for radiation therapy

Chemotherapy • The bottom line – there are few studies to compare efficacy of various protocols – Dogs with low grade MCT with dirty borders can do very well long term with and even sometimes without chemo – Dogs with high grade tumors can enjoy significant palliation with chemo, but cures are not common • Objective Response rate (ORR) up to 64%
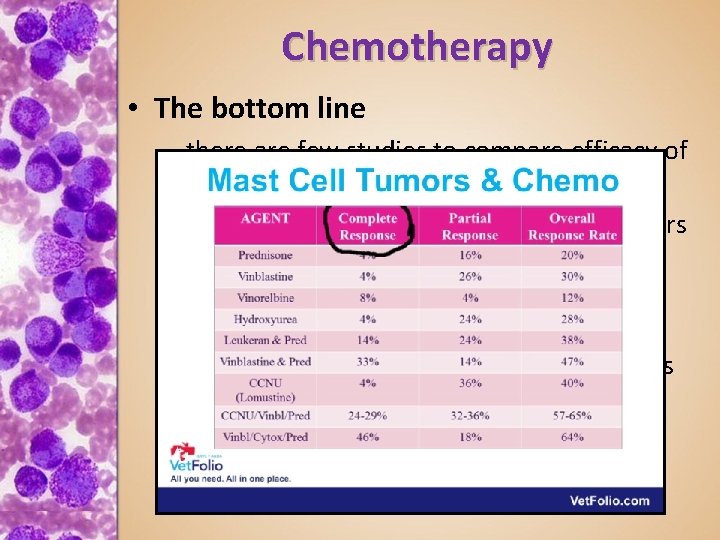
Chemotherapy • The bottom line – there are few studies to compare efficacy of various protocols – Dogs with low grade MCT with dirty borders can do very well long term with and even sometimes without chemo – Dogs with high grade tumors can enjoy significant palliation with chemo, but cures are not common • ORR up to 64%

Chemotherapy Two categories: 1. Traditional chemo – – VP – vinblastine prednisone CCNU – popular 20 -30 years ago Alternating VP and CCNU CVP – cyclophosphamide vinblastine pred 2. TKI – tyrosine kinase inhibitors – Palladia® - toceranib – Kinavet® - off the market in US, available in Europe – Gleevec® and about 20 others in people • $100 -150/pill, may be hepatotoxic to dogs

Chemotherapy Vinblastine, pred, cyclophosphamide • Study abstract claimed better response rate and longer survival times compared to other traditional chemo protocols • Analysis of data shows that long survival times were associated with tumors that typically do well even without adjunctive chemo • Despite abstract claims, adding cyclophosphamide is rarely done by oncologists

Chemotherapy Metronomic Therapy -- palliation • Chlorambucil and prednisone • Palladia® and Prednisone (alternating days) • Palladia® and piroxicam (alternating days)

"To live a creative life, we must lose our fear of being wrong. " -- Joseph Chilton Pearce Attendee 14 City TX "You gain strength, courage and confidence by every experience in which you really stop to look fear in the face. " -- Eleanor Roosevelt

Chemotherapy - Summary • Traditional chemo – VP or alternating VP & CCNU preferred to CCNU alone for grade III, high grade II and mixed message low grade II • TKI – Studies comparing traditional to TKI not available – many oncologists prefer TKI as first line therapy for high risk MCT – Others do traditional chemo, then follow with TKI – Many oncologists feel that if there is a good response to TKI, it is more durable than traditional chemo – Side effects of TKI are not common in the first 6 weeks, but eventually occur, can be significant and potentially life threatening

In a Nutshell “I've long ago decided that with MCT therapy, it's easier to assign protocols based on the day of the week than it is to actually figure out what's best for the tumor. On Tuesdays I really like to give Palladia®. ” --Zack Wright, ACVIM (Oncology)

Chemotherapy Palladia® • Palladia® = toceranib • Masivet® = Kinavet-CA 1® = masitinib • Tyrosine kinase (TKI) inhibitors • Prednisone and TKI are the chemo drugs with direct cytotoxicity for MCT – Probably the most effective chemo for high grade MCT A game changer for some high grade and very large MCT – palliative, not curative

Chemotherapy Palladia® • Indications for use: – All conditions mentioned earlier for first line MCT chemo – Post Chemo – VP x 4 -8 weeks, then Palladia for 6 months • Labeled for dogs >11 -15 lbs only – Oncologists compound for smaller pets, but this is an off-label use – Used off label for cats – Kinavet® has a failed conditional license, so off label use is illegal

Chemotherapy Palladia® • Response can take up to 2 -3 weeks • Palladia $600 -800 per month - 70 lb dog

Chemotherapy Palladia® Administration • 2. 5 -2. 75 mg/kg PO QOD (or MWF) – Dose chart on package insert is higher – With or without food • Dose reduction in response to adverse events – Stop Palladia® for 1 -2 weeks – 0. 5 mg/kg reduction when reduced – Minimum dose 2. 2 mg/kg PO QOD – label – Some see responses as low as 2. 0 mg/kg

Chemotherapy Palladia® Administration Monitoring: • Label: – Weekly CBC/panel for the first 6 weeks – Then every 3 weeks x 2 – Then every 6 weeks thereafter x 2 -3 • Oncologists: – CBC One month after starting – 60 days after that – Then every 3 months – Neutrophils stay between 2, 000 -3, 000/ul – Reduce dose if segs <1, 500/ul

Chemotherapy Palladia® Administration • GI side effects common – Make sure owner knows to STOP drug if anorexia, vomiting, diarrhea • Dispense Cerenia and metronidazole at the first visit to have on hand • Administer H 1 and H 2 blockers concurrently • Manufacturer says no prednisone concurrently

Chemotherapy Palladia® Study – Bergman & Clifford, 2009 • 40% did not respond at all • 60% overall response rate, 40 -50% CR • Among responders, median duration of response was 12 weeks (3 months) • Median time to non-response or death was 18 weeks (4 -5 months) • 82% of dogs with C-KIT mutation responded • 54% of dogs without mutation responded • There was a placebo response – Likely due to spontaneously resolving degranulation • Clin Cancer Res 2009; 15: 3856 -3865.
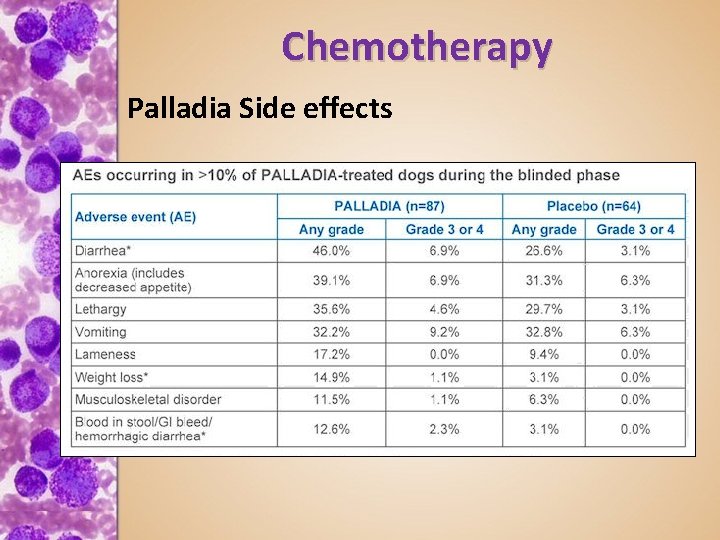
Chemotherapy Palladia Side effects

Chemotherapy Palladia Side effects • Dec. albumin – 13% Palladia, 8% Placebo • Palladia given long term leads to glomerular disease and renal failure • While this long term side effect is severe, it is balanced against the short term grave prognosis of high grade MCT
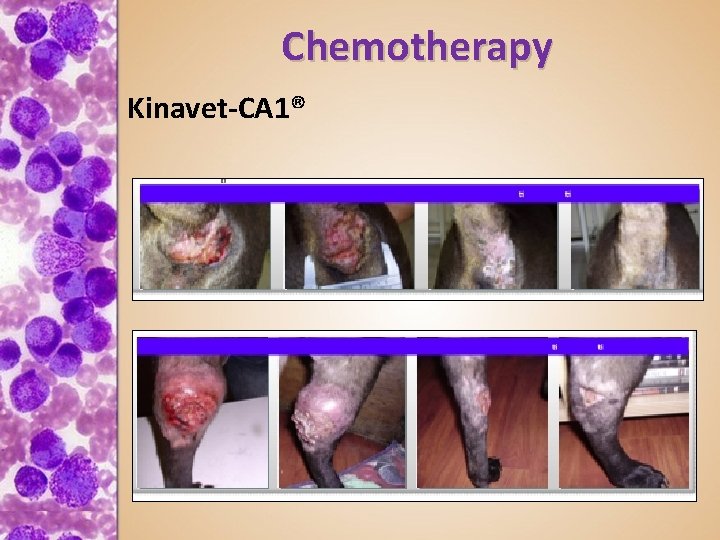
Chemotherapy Kinavet-CA 1®
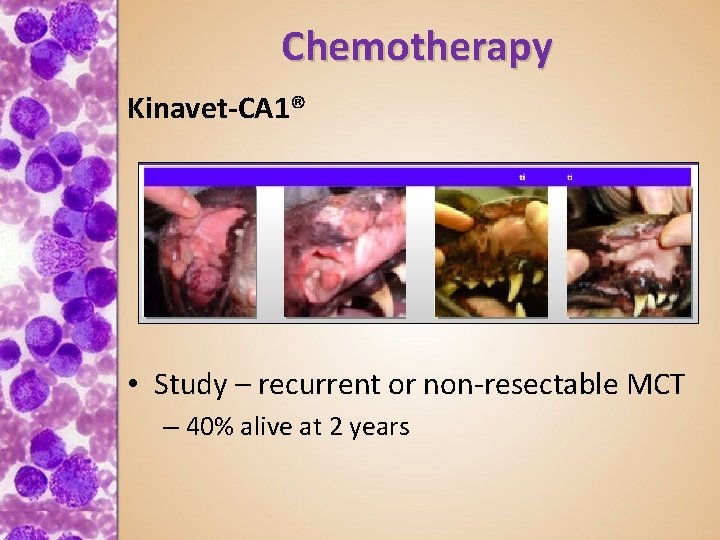
Chemotherapy Kinavet-CA 1® • Study – recurrent or non-resectable MCT – 40% alive at 2 years
Chemotherapy Palliative Drug Therapy • Alone, or accompanying chemo and/or radiation • Prednisone 40 mg/m 2/day – Wean gradually to 0. 5 mg/m 2/day • Antihistamines daily • H 2 blocker or proton pump blocker – Cimetidine, ranitidine, famotidine – Omeprazole, esomeprazole • sucralfate if GI ulceration – Hematemesis, melena

Radiation Therapy • 85 -95% Curative at 2 years under selective circumstances – Low grade II non-resectable MCT without distant metastasis • Including lymph node metastasis only – Grade II Stage 0 MCT with dirty or close (<3 mm) margins • Disease free interval is increased compared to no treatment • Similar outcome to re-excision (95% cure) – 16 Fraction @ 3 Gy administered M-F for a total of 48 Gy over 4 weeks • Come daily, go home weekends, or stay 4 weeks

Radiation Therapy • Palliative – Non-resectable high grade MCT – Regional lymph node metastasis – 4 -6 Fractions @ 6 -8 Gy administered once weekly – Alone or with chemo – 75 -80% respond to both, 55 -60% complete response • No indication to irradiate grade I-II MCT with clean borders >3 mm, unless mixed message low grade II

Prognosis • Histologic grade and stage are the most important prognostic factors for MCT – Grade I with clean borders are cured by surgery – Low grade II clean borders usually cured by surgery and/or radiation – High grade II clean borders should probably have adjunctive chemo and/or radiation – High grade II with dirty borders should definitely have adjunctive chemo and/or radiation and may have poor prognosis – Virtually all of grade III die of their disease, often within a few months, unless very small with clean borders

"The higher we are placed, the more humbly we should walk. " -- Cicero Attendee 15 City TX "Humility is not thinking less of yourself. It is thinking of yourself less. " --David Jeremiah

Prognosis • Local Recurrence – Dirty margins – only 20 -40% recur – But if it does recur, it can recur at a higher grade (grade jump) – MCT panel & staging can help sort this out when planning additional therapy – 90% of local recurrence happens within 1 year • Metastatic Rate – all MCT are malignant – Grade I - 1 -2% – Grade II - 10 -22% • 85% of grade II tumors are low grade II • 15% are high grade II – Grade III - 55 -96%

Prognosis • Mitotic Index – Not completely accurate alone, but along with grade can be highly predictive – Some false negatives with low MI (Lo-Hi) Lo-Hi – High MI correlates with high grade on MCT prognostic panel (poor man’s MCT panel) – MST MI <5 – 6. 7 years (false negatives) – MST MI >5 – 3 months • Other prognosticators on histopath – Infiltrative growth – Multinucleate cells – Other molecular factors on the MSU panel

Prognosis Indicators of poor prognosis • Dirty borders after re-excision • High grade, advanced stage, MI >5 • Breed- Shar pei • Systemic signs due to degranulation – Ishiguro et al 2003 – post-op plasma histamine level – but not offered • Size and growth rate - >3 cm worse prognosis • Patient age – geriatric worse

Prognosis Indicators of poor prognosis • Tumor Location – Aggressive – Muzzle – higher percentage of grade III here • Incisional biopsy encouraged – Scrotum, nail bed, mucocutaneous – perineum, inguinal – disproved Sfiligoil et al 2005 – histopath no less accurate here • Grave prognosis – visceral, bone marrow (metastasis) – rare but bad – 2% bone marrow + on 1 st MCT – 8% bone marrow + on 2 nd MCT – MST 43 days for bone marrow + MCT

Prognosis Indicators of poor prognosis • Lymph node metastasis is arbiter of prognosis – MST < 1 year if LN+, many years if LN– 25% of LN+ have distant mets, very few LN- • Systemic metastasis beyond LN at Dx – MST 194 days when LN+ and metastasis – MST 503 days when LN+ & no metastasis – Have to do staging in order to know this, but will detect metastasis only 10 -20% of the time

Prognosis Indicators of better prognosis • Skin tumor in location not associated with poor prognosis • Clean borders on excision • Low grade, low stage, MI <5 • Breed – Boxers and Pugs

Prognosis Indicators of better prognosis • Skin tumor in location not associated with poor prognosis • Clean borders on excision • Low grade, low stage, MI <5 • Breed – Boxers and Pugs

Prognosis Survival by Grade • Grade I – 83 -93% survival at 4 -5 years • Grade II – 44% survival at 4 -5 years – Low grade II - 85. 6% survival at one year – High grade II – 46% survival at one year • Grade III – most die within a year – 6% survival at 4 -5 years

Prognosis Multiple primary mast cell tumors do not necessarily worsen prognosis for distant metastasis • 11% of dogs who get one dermal MCT will get another later • Warn owners to look for more when you remove the first Some dogs can develop so many dermal MCT that surgery to keep up becomes impossible, and we are left with drugs

Bergman Treatment Buckets 1. Clean margins & staging, MI<5, low grade – Watch and wait for local recurrence (5 -10% will) – MCT panel if clean but close (4 -11 mm) 2. Clean margins & staging, MI>5, high grade – Chemotherapy, watch for local recurrence 3. Dirty margins, clean stage, MI<5, low grade – MCT panel is crucial + Additional surgery – watch and wait if low grade, radiation if high 4. Dirty margins, MI>5 + high grade – Chemotherapy, surgery/radiation 5. Distant Metastasis or c. KIT mutation – Chemotherapy indicated, palliative Sx/rad

Summary • Power. Point • . pdfs of Power. Point – 1 & 6 slides per page Laboratory Information: • MSU Forms - IHC Form; Pathology Form (MCT Prognostic Panel) • MSU Fees – Molecular Pathology Fees; MCT Pricing Flow Chart • MSU Info – List of Tumor Panels; MCT Prognostic Panel Info

Summary Vet Handouts: • Clifford - MCT Diagnostic Algorithm • Bergman – MCT Treatment Buckets • Strottner – MCT Diagnostic Algorithm • MSU - MCT Diagnostic Algorithm • MSU – MCT Panel Scientific Article: • VCS 2018 – Prednisone Neo. Adjuvant Therapy

Summary Chemotherapy Protocols: • Vinblastine and Prednisone • Vinblastine, Prednisone, CCNU • Palladia®
Summary Package Insert: Palladia® Client Handouts: • Blount - Mast Cell Tumor • MSU – Mast Cell Tumor Drug Handouts: • Prednisone • CCNU • Diphenhydramine • Toceranib • Vinblastine • Famotidine

Summary Hidden Slides: • Cytologic grading • MCT Diagnostic Algorithms • Northrup study on consistency of grading • Details on interpreting MCT Panel • Surgical borders study • Chemotherapy protocols (VP, CCNU, both) • Kinavet® administration • MOA Palladia®, Palladia® study • Treatments not recommended

Acknowledgements • Philip J. Bergman, DVM, MS, Ph. D, DACVIM (Oncology) VIN Consultant, CMO Bright. Heart Vet Centers • Louis-Philippe de Lorimier, DVM, ACVIM (Oncology) VIN Consultant, U of Ill Urbana-Champaign Visiting assistant professor, medical oncology • Karri A. Meleo, DVM, ACVIM (Oncology), ACVR VIN Consultant, Vet Onc Serv, Edmonds, WA

Acknowledgements • Robert C. Rosenthal, DVM, BS, MS, Ph. D VIN Consultant • Kurt R. Verkest, BVSc, BVBiol, MACVSc (Small Animal) VIN Associate Editor, Univ Queensland, Australia • Claudia Barton, DVM, ACVIM (Internal Medicine, Oncology) TAMU CVM

Acknowledgements • Craig Clifford, DVM, MS, ACVIM (Oncology) VIN Consultant • Zachary Wright, DVM, ACVIM (Oncology) Animal Diagnostic Clinic, Dallas TX • Gabi Strottner, DVM, ACVIM (Oncology) Capital Area Veterinary Specialists and Texas Veterinary Oncology (www. cavstvo. com )

Acknowledgements • Craig Clifford, DVM, MS, ACVIM (Oncology) Vet. Folio. com – Oncology Certificate Program – Mast Cell Tumors, Top Ten Trends In Oncology
- Slides: 85