Practical medical mycology Lab 8 Yeast Identification Introduction
ﺑﺴﻢ ﺍﻟﻠﻪ ﺍﻟﺮﺣﻤﻦ ﺍﻟﺮﺣﻴﻢ Practical medical mycology Lab 8 Yeast Identification

Introduction • Yeasts are considered normal flora of oropharynx and gastrointestinal tract and may therefore be recovered from sputum, throat swabs, bronchial washings, gastric washings, and stool specimens. • However, the repeated isolation of yeasts from a series of clinical specimens of urine, nail scrapings, and vaginal washings, from the same patient usually indicates infection with the organism recovered and identification of the isolates is necessary.

• Furthermore, the presence of yeast in normally sterile body fluids such as blood, cerebrospinal fluid (CSF), or fluids aspirated from the pleural cavity, or the pericardial sac, is also considered as a clinical situation in which species identification is justified. • Candida albicans is the species of yeast most frequently cultured from clinical specimens.

Principal Criteria and Tests for Identifying Yeasts 1. Culture characteristics - Colony color, shape, texture. 2. Asexual structures. a. Shape and size of cells. b. Bipolar, fission, multipolar or unipolar "budding“. c. Absence or presence of arthroconidia, ballistoconidia, blastoconidia, clamp connections, germ tubes, hyphae, pseudohyphae, or sporangia and sporgangiospores.
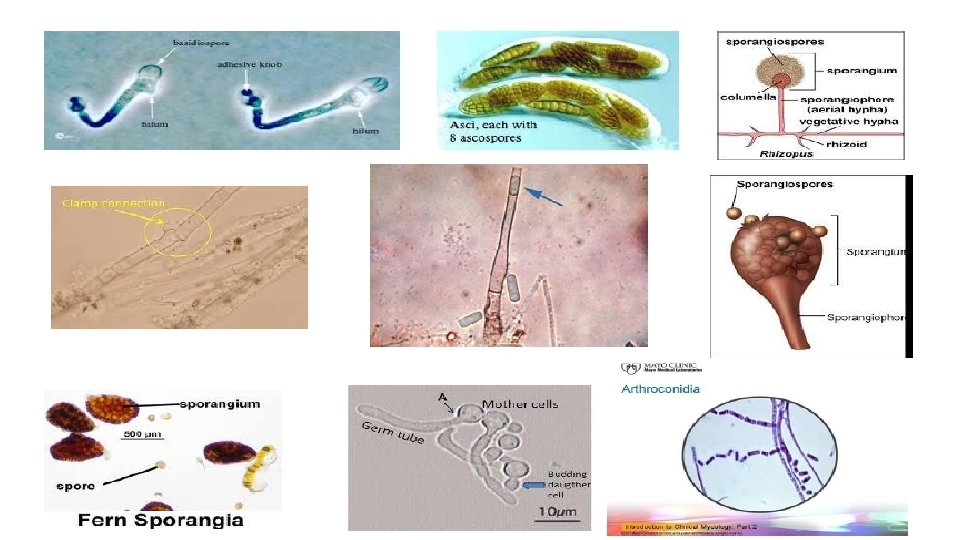

Principal Criteria and Tests for Identifying Yeasts 3. Sexual structures - Arrangement, cell wall ornamentation, number, shape and size of ascospores or basidiospores. 4. Physiological studies Assimilation, Cycloheximide resistance, Fermentation, Nitrogen utilization, Urea hydrolysis, Temperature studies, Citrate utilization test.

Microscopic examination of yeasts Yeasts are examined by microscope by one of these methods : 1 -Gram stain. 2 -Direct/ Wet mount. 3 -Germ tube test. 4 -India ink test. 5 - Lactophenol Mount. 6 - Production of chlamydospores on CMA-Tween 80: Corn Meal Agar with Tween® 80. 7 - Carbohydrate fermentation.

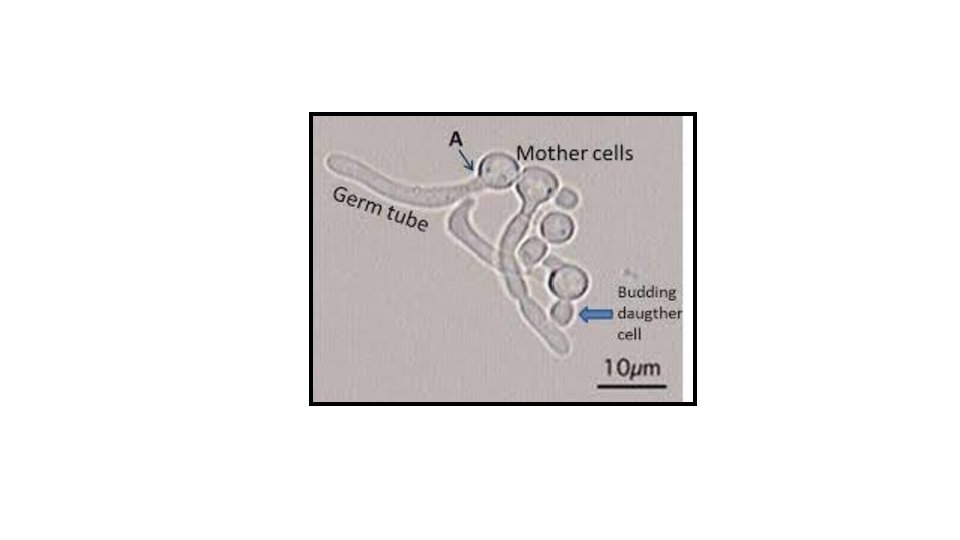
Germ tube test 1. Suspend a very small portion of an isolated colony of the yeast to be tested in a test tube containing 0. 5 ml of rabbit or human serum. 2. Incubate the test tube at 37 ºC for no longer than 3 hours. 3. Place a drop of the yeast-serum suspension on a microscope slide, and cover with a coverslip. 4. Examine under the microscope for the presence of germ tube.

Production of chlamydospores on CMA-Tween 80. 1. Using an inoculating needle, obtain visible paste of the organism. Draw the needle through the agar making two perpendicular lines in the shape of an "x". 2. Flame a coverslip and allow it to cool. Once coverslip has cooled, place over the central area of the "x" in order to reduce oxygen tension. Reduced oxygen tension stimulates chlamydospore production. Leave some growth uncovered. 3. Seal the plate with tape or Myco. Seals™ (Cat. no. SS 9225) and incubate aerobically at room temperature (25 -30ºC) for up to 72 hours in the dark. Examine daily for typical colonial growth and morphology.

4. Invert the plate and examine microscopically using a low power objective (10 X). View along the edge of the coverslip for detection of chlamydospore formation. 5. Follow steps one through four of the above procedure for the examination of sporulation of molds. Incubate until mold is visible and mount coverslip in glycine. Examine microscopically for characteristic structures.

Carbohydrate fermentation test for yeast identification • The principal tests for the identification of yeasts involve the investigation of isolates for their ability to ferment sugars and also to assimilate various sources of carbohydrates and nitrates. • However, commercial identification kits which give sufficient information to identify most isolates encountered in a medical laboratory are available.

Yeast fermentation in appropriate culture media containing a single carbohydrate source is detected by gas and acid production. a. To each of the yeast fermentation tubes (glucose, maltose, sucrose, and lactose) add 0. 2 ml of a yeast suspension in saline equivalent to a Mc. Farland No. 4 standard. b. Incubate at 37 ºC for 48 hours. c. Leave all negative test in incubator for 6 -10 days before discarding.

Note the presence of bubbles or a drop in the liquid level, in the inverted Durham’s tube, which indicates the fermentation.

The Urease test is useful in yeast identification. Cryptococcus species can be confirmed by a positive urease reaction, whereas most Candida and Saccharomyces species are urease negative.

Commercial Yeast Identification Systems • Two commercially available yeast identification systems are described: API 20 C Yeast Identification System (API Analytab Products, Plainview, NY) and the Biomerieux Vitek System (Hazelwood, MO). • These two yeast identification systems are easy to use. The API 20 C requires less preparation of reagents. The Vitek system is an automated system.

Yeasts of Medical Importance • Candida albicans • It is part of the normal respiratory, gastrointestinal, and female urogenital tract floras. • Under the proper circumstances, it may flourish and produce pathological conditions, such as thrush in the oral cavity, vulvovaginitis of the female genitals, and cutaneous candidiasis of the skin. • Systemic candidiasis may follow infection of the lungs, bronchi, or kidneys.

• Entry into the blood may result in endocarditis. Individuals most susceptible to Candida infections are diabetics, those with immuno - deficiency (e. g. , AIDS), catheterized patients, and individuals taking antimicrobial medications. • Budding results in chains of cells called pseudohyphae that produce clusters of round, asexual blastoconidia at the cell junctions. • Large, round, thick-walled chlamydospores form at the ends of pseudohyphae. • Presumptive identification of C. albicans can be made from a positive germ tube test.
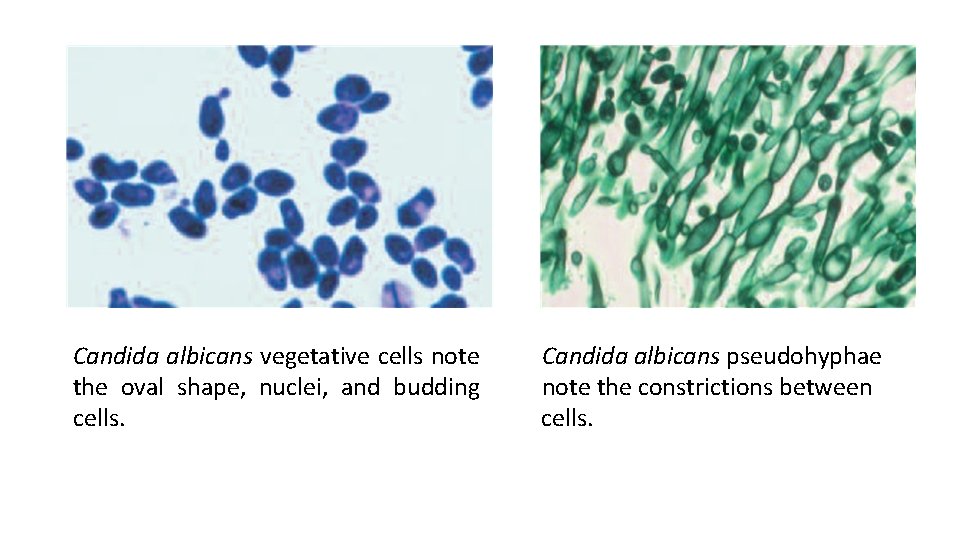
Candida albicans vegetative cells note the oval shape, nuclei, and budding cells. Candida albicans pseudohyphae note the constrictions between cells.
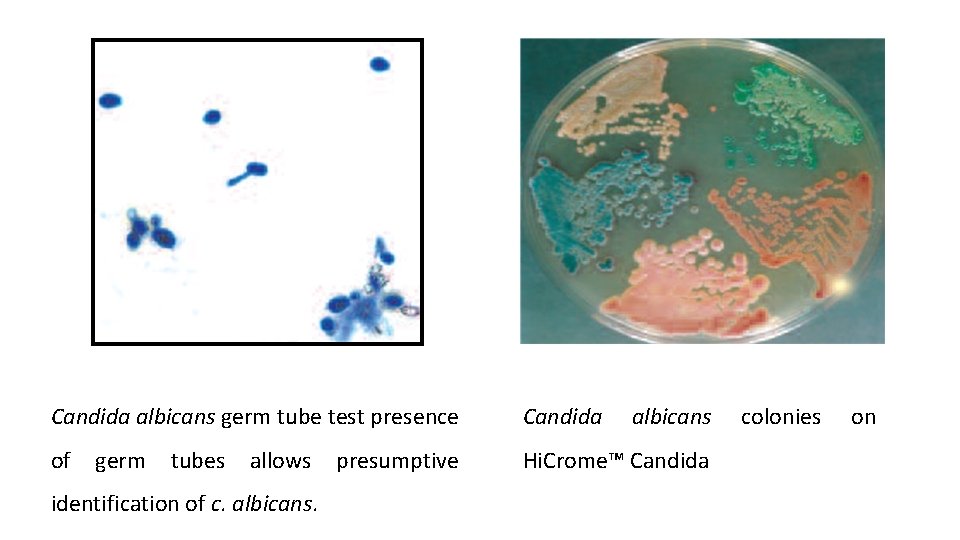
Candida albicans germ tube test presence Candida of Hi. Crome™ Candida germ tubes allows identification of c. albicans. presumptive albicans colonies on

• Hi. Crome™ Candida Differential Agar • It is recommended for rapid isolation and identification of Candida species from mixed cultures in clinical and non-clinical samples. • Composition • Ingredients Gms / Litre • Peptone, special 15. 000 • Yeast extract 4. 000 • Dipotassium hydrogen phosphate 1. 000 • Chromogenic mixture 7. 220

• Chloramphenicol 0. 500 • Agar 15. 000 • Final p. H ( at 25°C) 6. 3± 0. 2 **Formula adjusted, standardized to suit performance parameters

• Principle And Interpretation • Candida albicans produces an enzyme b -N-acetyl- galactosaminidase and incorporation of chromogenic or fluorogenic hexosaminidase substrates into the growth medium helps in identification of C. albicans isolates directly on primary isolation. • Hi. Crome™ Candida Differential Agar is a selective and differential medium, which facilitates rapid isolation of yeasts from mixed cultures and allows differentiation of Candida species namely C. albicans, C. krusei, C. tropicalis and C. glabrata on the basis of coloration and colony morphology.

• On this medium results are obtained within 48 hours and it is useful for the rapid and presumptive identification of common yeasts in Mycology and Clinical Microbiology Laboratory. • Peptone special and yeast extract provides nitrogenous, carbonaceous compounds and other essential growth nutrients. • Phosphate buffers the medium well. Chloramphenicol suppresses the accompanying bacterial flora. • C. albicans appear as light green coloured smooth colonies, C. tropicalis appear as blue to metallic blue coloured raised colonies. C. glabrata colonies appear as cream to white smooth colonies, while C. krusei appear as purple fuzzy

• Limitations 1. Variations in color intensity may be observed for Candida isolates depending on the presence of enzymes. 2. Other Candida species may produce light mauve colored colonies which is also produced by other yeast cells. This must be confirmed by further biochemical tests. 3. Other filamentous fungi also exhibit color on this medium

• Pneumocystis jirovecii • (formerly P. carinii) is an opportunistic pathogen whose taxonomy and natural history has been difficult to work out due to the inability to grow it outside of its mammalian host. • Comparison of ribosomal RNA and genome sequencing has led to the conclusion that Pneumocystis, long classified as a protozoan, is more closely related to certain ascomycete yeasts. • Its protozoan roots are still evident, however, in the terminology associated with it.

• Pneumocystis exists as a trophozoite (trophic stage) and a multinucleate cyst (spore case) (Figure 15 -7). • Asexual reproduction is by fission of the trophozoite, not budding as in most yeast. • Its sexual phase is thought to resemble yeast-like conjugation to form a zygote that produces four spores by meiosis. • These then undergo mitosis to produce a cyst with eight spores. • Most people become seropositive for Pneumocystis in childhood and humans—even immunocompetent individuals— are the apparent reservoirs for the organism.

• Transmission is through the air, with the primary infection occurring in the lungs. • Infection produces pneumocystis pneumonia (PCP) in AIDS patients and immunosuppressed individuals, and interstitial plasma cell pneumonitis in malnourished infants. • Identification is made by direct examination of the cyst (usually) using immunofluorescence. • Co-trimoxazole is given to immunocompromised patients whose CD 4 (T-helper) cell counts are less than 200/mm 3.
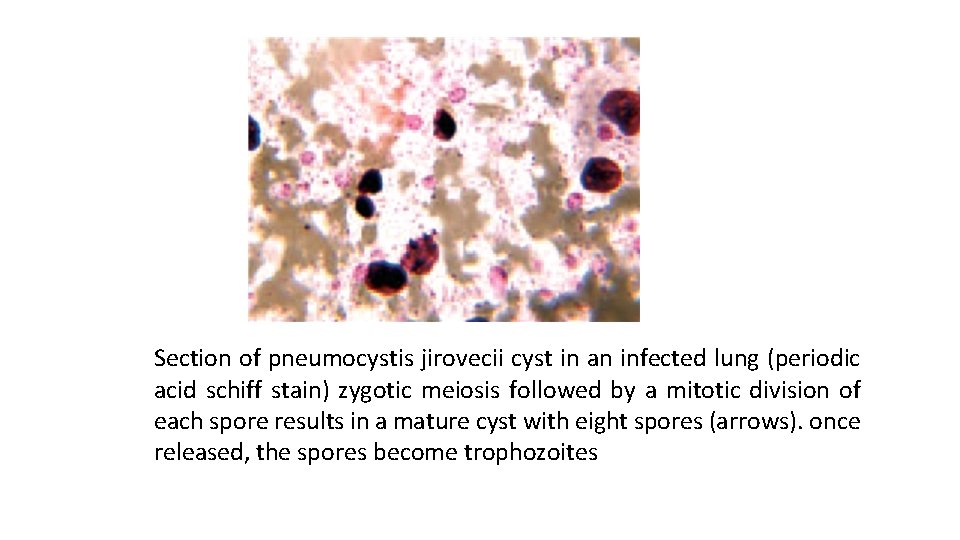
Section of pneumocystis jirovecii cyst in an infected lung (periodic acid schiff stain) zygotic meiosis followed by a mitotic division of each spore results in a mature cyst with eight spores (arrows). once released, the spores become trophozoites

Saccharomyces cerevisiae • Synonomy: Candida robusta • Saccharomyces cerevisiae, commonly known as Baker’s yeast, may be found as a harmless and transient digestive commensal and colonizer of mucosal surfaces of normal individuals. • The anamorphic state of S. cerevisiae is sometimes referred to as Candida robusta.

• This species is genetically closely related to Candida glabrata and shares many clinical and microbiological characteristics to this species. • S. cerevisiae may be involved in mucosal infections like vaginitis, and in bloodstream infections, particularly in fluconazole-exposed patients. • Note: Saccharomyces boulardii, a genetically similar species that is used as a probiotic for prevention and treatment of various sorts of diarrhea and recurrent Clostridium difficle -associated diarrhea should be avoided in immunocompromised hosts
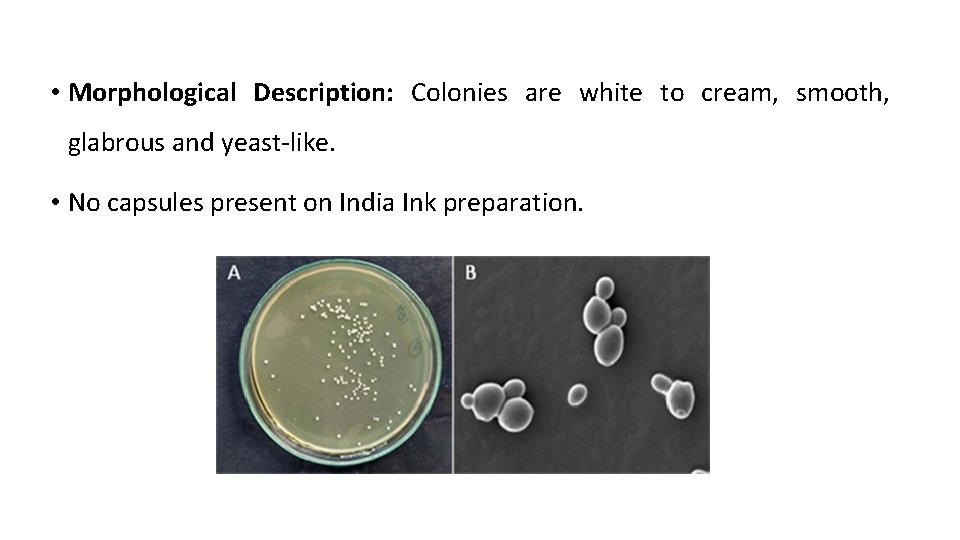
• Morphological Description: Colonies are white to cream, smooth, glabrous and yeast-like. • No capsules present on India Ink preparation.

The End
- Slides: 33