Practical Management of Common Cardiac Presentations CINDY STIVES





































- Slides: 45

Practical Management of Common Cardiac Presentations CINDY STIVES, APRN, CNP

Disclosures Prior speaker for Lantus, Apidra and Toujeo and Soliqua Insulins through Sanofi Pharmaceuticals On an advisory board for Sanofi regarding the real world use of their products last year. No disclosures for anything cardiac related

Objectives Discuss Understand Discuss the practical management of CHF including cases, common presentations, treatments, and red flags. Understand the management of heart failure with reduced and preserved ejection fractions Increase knowledge in the area of practical management of chest pain, including cases, EKG presentations, and red flags. Discuss clinical applications of medications used to treat and manage CHF, hypertension, atrial fibrillation, and chest pain.

CHF: Etiology / Triggers Colucci, 2018 Results from structural or functional cardiac disorders May be caused by disease of the myocardium, pericardium, endocardium, heart valves, vessels or by metabolic disorders. Heart failure due to left ventricular dysfunction are categorized according to the left ventricular ejection fraction (LVEF) • HFr. EF or systolic HF • HFp. EF or diastolic HF.

CHF Presentations Chest Pain: RED FLAG New Onset A fib: RED FLAG Borlaug & Collucci, 2018 Fluid Overload

Reduce morbidity Reduce mortality Colucci, 2018 Treatment of CHF: Goals of Therapy • Reducing symptoms • Improving health related quality of life and functional status • Decrease rate of hospitalization

Management of contributing factors and associated conditions Lifestyle modification Pharmacologic therapy Device therapy if indicated Preserved EF Borlaug & Colucci, 2018; Colucci, 2018 Treatment: Approach to Management Reduced Ejection Fraction (EF) Management directed toward associated conditions and symptoms Hypertension Edema

2013 American College of Cardiology/American Heart Association (with 2016 focused update) AHA, 2017 Systolic and diastolic HTN should be controlled in accordance with published clinical practice guidelines to prevent morbidity. Diuretics should be used to relieve symptoms due to volume overload.

Disease Management Program Advanced Care Mechanical circulatory support Cardiac transplantation Palliative Care Colucci, 2018 Approach to Management continued

Restrict sodium and alcohol consumption Annual influenza vaccine Pharmacologic therapy • Governed by associated conditions and symptoms • Diuretics: treats volume overload • ARBS, ACE inhibitors, Calcium Channel Blockers, B Blockers treat hypertension Borlaug & Colucci, 2018 General Management: HFp. EF (Diastolic Heart Failure) Pneumococcal vaccination

Flu and pneumococcal vaccine Serial assessment Cardiac rehab Heart failure disease management Smoking cessation Restrict sodium to 3 gm Fluid restriction (1. 5 -2 liters per day) Avoidance of obesity Daily Weights Pharmacologic therapy Colucci, 2018 General Management of HFr. EF (Systolic HF)

Primary cause of HF in many patients Increased hemodynamic load on failing ventricles Lowering systemic BP • reduces rate of development of HF • Reduces LV afterload Choice of antihypertensive must be individualized based on coexisting diseases (such as COPD and DM) Borlaug & Colucci, 2018 Management of Associated Conditions of CHF: Hypertension

B Blockers Angina relief in patients with ischemic heart disease and rate control in patients with A fib. Examples: metoprolol tartrate, metoprolol succinate, atenolol, sotalol, carvedilol, propranolol Side effects: hypotension, bradycardia, orthostasis **In COPD patients: better to use beta-1 (cardio-selective) blockers which are less likely to interact with albuterol (antagonistic effect) Atenolol, metoprolol, nebivolol, and bisoprolol. Borlaug & Colucci, 2018; Colucci, 2018 Treating hypertension with reduced ejection fraction (HFr. EF, systolic HF)

ACE Inhibitors, ARBs, or angiotensin receptorneprilysin inhibitor (ARNI) Patients still hypertensive after B Blocker, and ACE and MRA can be added (spironolactone). Ace inhibitors may prevent and control diabetic nephropathy and control diabetic retinopathy No need to be on both ACE inhibitor and ARB Examples: lisinopril, ramipril enalapril benazepril, and captopril Colucci, 2018 Treating hypertension with reduced ejection fraction

Colucci, 2018 Treating hypertension with reduced ejection fraction Mineralocorticoid receptor antagonist (MRA) Block actions of aldosterone Renal protection in CKD Example: spironolactone

Management of Associated Conditions of CHF: Atrial Fibrillation 3 settings in which rhythm control strategy should be considered: • Persistent symptoms (HF, dyspnea, light headed, angina, syncope) • Inability to attain adequate rate control • Patient preference Rhythm control strategies • Anti-arrhythmic medications • Cardioversion • Catheter ablation Borlaug & Colucci, 2018 Restoration and maintenance of sinus rhythm preferred in patients with HFp. EF

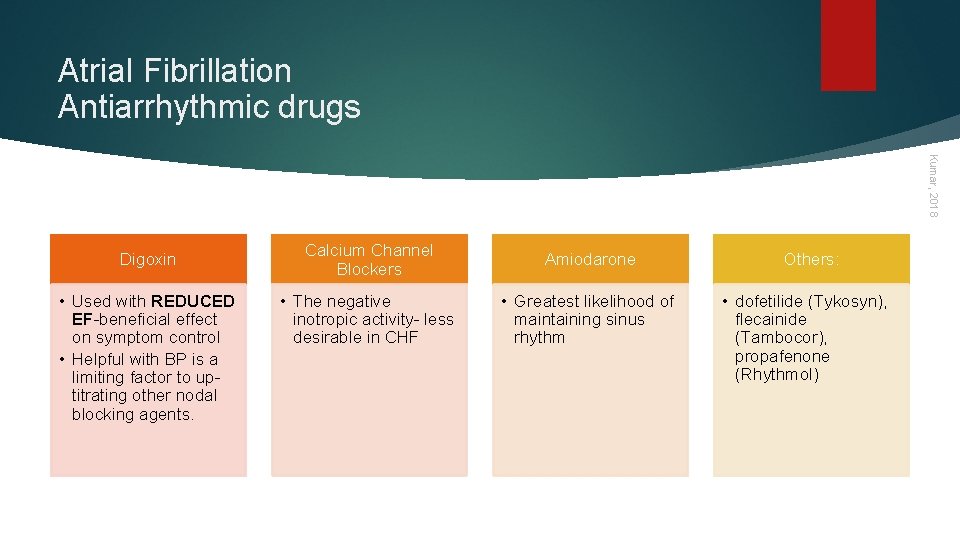
Atrial Fibrillation Antiarrhythmic drugs Kumar, 2018 Digoxin • Used with REDUCED EF-beneficial effect on symptom control • Helpful with BP is a limiting factor to uptitrating other nodal blocking agents. Calcium Channel Blockers Amiodarone • The negative inotropic activity- less desirable in CHF • Greatest likelihood of maintaining sinus rhythm Others: • dofetilide (Tykosyn), flecainide (Tambocor), propafenone (Rhythmol)

Atrial Fibrillation Treatment with B Blockers Protect against the recurrence of A fib Effective in maintaining sinus rhythm Decrease resting heart rate and blunt the heart rate response to exercise REDUCED EF: Carvedilol: improvement in left ventricular EF and decrease in death/hospitalization Kumar, 2018 Started before or simultaneously with an antiarrhythmic drug

Management of Associated Conditions of CHF: Atrial Fibrillation Kumar, 2018 Inpatient vs outpatient initiation of meds • 10 -15 % incidence of adverse cardiac events during initiation • Bradycardia • Proarrhythmia • QT prolongation • RVR • Hypotension • Stroke • Conduction abormalities

Outpatient initiation of may be considered Flecainide or propafenone Sinus rhythm with no structural heart disease Amiodarone No other risk factors for torsades (hypokalemia, hypomagnesemia) Kumar, 2018 Inpatient vs outpatient initiation of meds (continued)

Management of Associated Conditions of CHF: Myocardial Ischemia Borlaug & Colucci, 2018 2/3 of HF with preserved EF have CAD Independent predictor of increased mortality and deterioration in LV systolic function over time Standard therapy includes B blockers, calcium channel blockers, nitrates May need coronary revascularization by PCI or CABG

Recommended for the primary and secondary prevention of cardiovascular disease 2 large randomized trials found: Statins have no beneficial effect in patients with reduced EF Statins may be of benefit in patients with preserved EF Borlaug & Colucci, 2018 Management of Associated Conditions of CHF: Hyperlipidemia

Bradycardia Abrupt severe elevations of blood pressure Ischemia Atrial fibrillation Borlaug & Colucci, 2018 Avoid common precipitants of HF Tachycardia

Borlaug & Colucci, 2018 Cardiac rehab improves exercise capacity and quality of life Weight loss Other Management Serial Assessments with each visit • Ability to perform ADL’s • Volume status and weight • Current use of meds, alcohol, tobacco, illicit drugs, alternative therapies • Diet and sodium intake

OUTPATIENT EVALUATION OF ADULT WITH CHEST PAIN

Chest Pain: etiology/presentation Benign to life threatening 1/3 to ½ have musculoskeletal chest pain 10 -20% have Gastrointestinal (GI) causes 10% have stable angina 5% have respiratory condition causing the CP 2 -4% have acute myocardial ischemia including myocardial infarction (MI) Yelland, 2018

Myocardial Ischemia Yelland, 2018 Angina: CP attributed to myocardial ischemia • Symptoms at rest could be ACS • New onset, not stable: ACS • Progressive symptoms: ACS • Refer to ED urgently Classic Symptoms • • Pressure Heaviness Tightness Constriction in the center or left of chest

Other symptoms of myocardial ischemia Radiation Dyspnea Nausea and vomiting Diaphoresis Presyncope Palpitations Yelland, 2018 Provocation with emotional stress

• Acute chest/back pain: severe, sharp, ripping quality Heart Failure • Acute decompensated HF can present with CP Non-ischemic cardiac causes Pericarditis • Pleuritic CP that is improved by sitting up and leaning forward Stress cardiomyopathy • Physical/emotional stress or critical illness Mitral valve disease • CP likely from pulmonary hypertension and RVH Yelland, 2018 Aortic dissection

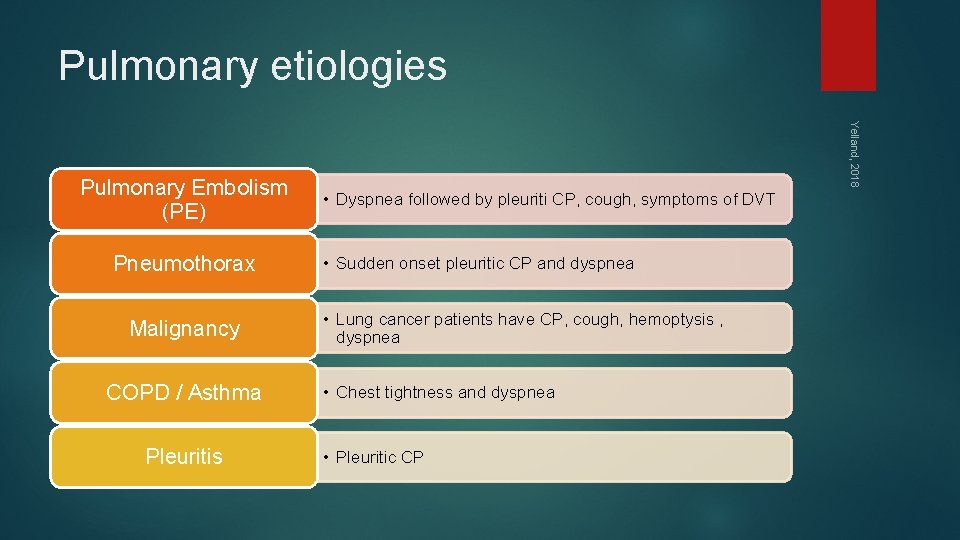
Pulmonary etiologies Pneumothorax Malignancy COPD / Asthma Pleuritis Yelland, 2018 Pulmonary Embolism (PE) • Dyspnea followed by pleuriti CP, cough, symptoms of DVT • Sudden onset pleuritic CP and dyspnea • Lung cancer patients have CP, cough, hemoptysis , dyspnea • Chest tightness and dyspnea • Pleuritic CP

GI etiologies Yelland, 2018 GERD Esophageal pain • Can mimic angina (squeezing, burning) • Substernal, radiating to back, neck, jaw, or arms • Can last minutes to hours • Will resolve with antacids or GI cocktail • Food bolus, GERD, esophagitis, esophageal rupture.

Musculoskeletal CP Yelland, 2018 Regional tenderness without other symptoms Can usually be traced back to an injury or strain The pain can be reproduced

Other causes of CP Yelland, 2018 Psychiatric / Panic attack Herpes Zoster Spontaneous, discrete episodes of intense fear, usually recurrent Hyperventilation can result in nonanginal CP and occasionally EKG changes CP may precede the characteristic rash (present in the effected dermatome

Quality Location / radiation Evaluation of Chest Pain Abrupt onset Pneumothorax, aortic dissection, esophageal rupture, PE Provocation Ischemic pain is often diffuse and difficult to localize Exertion / eating/ movement Palliation Abated with rest / antacids / nitroglycerin Yelland, 2018 Sharp, dull, tearing, reproducible, pressure, tightness

Evaluation of CP continued Risk factors Age HTN Hyperlipidemia Diabetes Obesity Smoking Family history Atherosclerotic disease Yelland, 2018

Physical Exam Yelland, 2018 Vital signs and oxygen saturation Cardiac exam Pulmonary exam Musculoskele tal and skin exam Abdominal exam Labs: troponin, CBC, CMP, lipase, CXR

EKG Yelland, 2018 Unless obvious cause, get EKG, consider keeping on continuous monitoring STEMI: new ST elevation in 2 consecutive leads Hx of ACS, but normal EKG: still send to ED Non. STEMI: ST depression or T wave inversion in 2 consecutive leads • T waves always upright in leads I, II, V 3 -6 • T waves always inverted in lead a. VR Initial EKG often NOT diagnostic in patients with ACS True or False: EKG obtained while patient having CP that fails to show evidence of ischemia rules out the possibility of ACS.

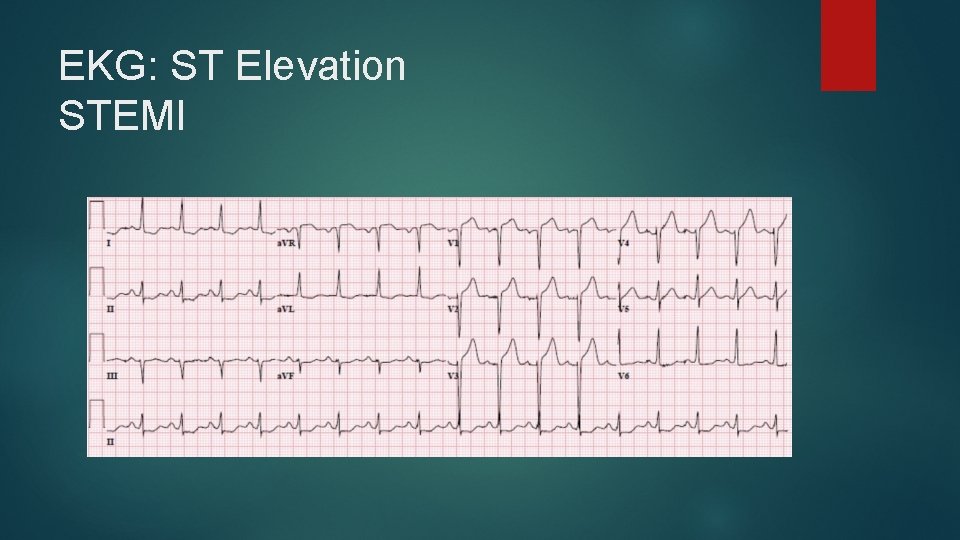
EKG: ST Elevation STEMI

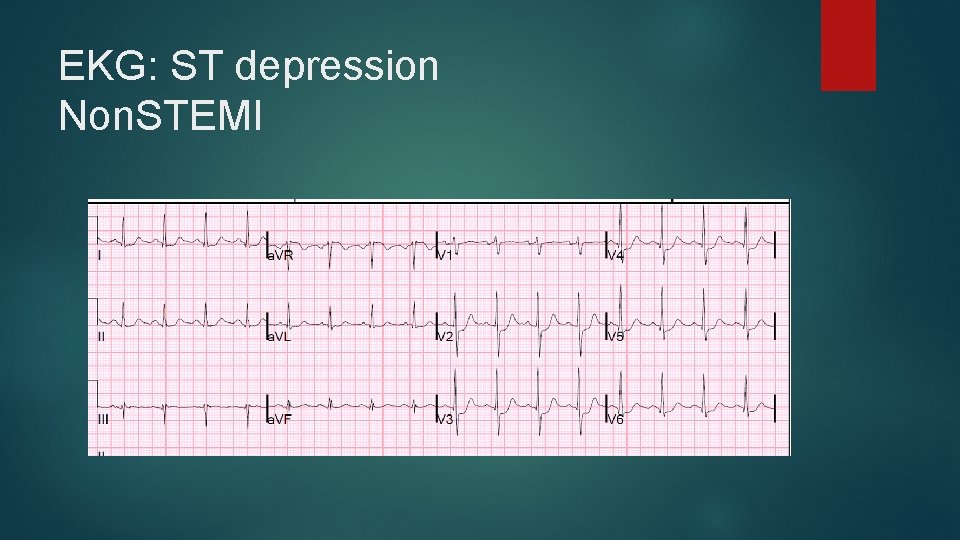
EKG: ST depression Non. STEMI

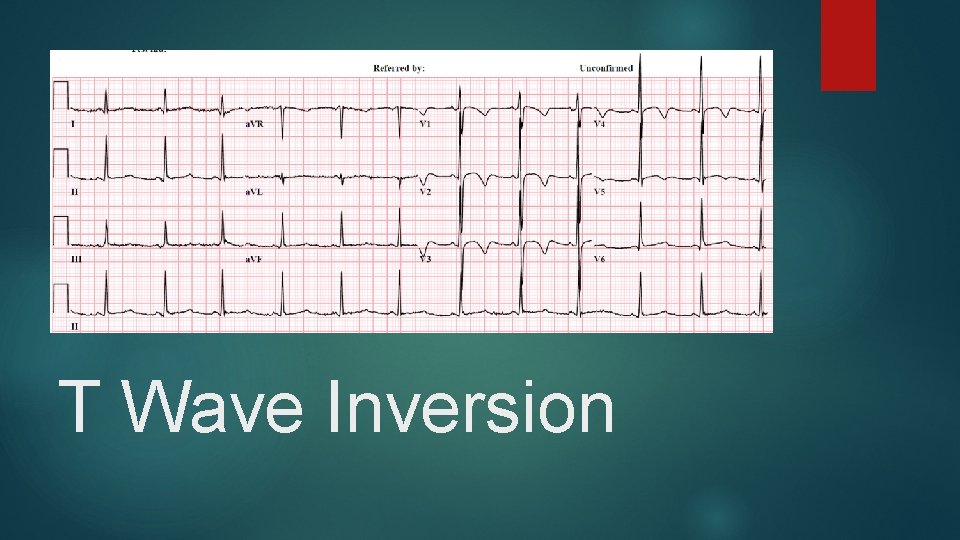
T Wave Inversion

Stress Test to evaluate cause Schedule Stress Test for patients not currently having CP, but reporting intermittent CP in the office Nuclear stress test Treadmill stress test

Risk Assessment https: //www. heartscore. nl/

ASA 325 mg chewed Oxygen Treatment of CP Continuous telemetry Establish IV access IV morphine (2 mg) Observation unit Cardiology consultation Reeder, Awtry & Mahler, 2018 Nitroglycerin SL (0. 4 mg q 5 min x 3)

Antianginal therapy Beta Blockers First line therapy Reduce anginal episodes and improve exercise tolerance Calcium Channel Blockers Used in combination with B Blockers Long acting diltiazem or verapamil or amlodipine preferred Nitrates Used for acute episodes or prophylaxis Newer therapy: ranolazine Late sodium channel blocker Used in combination with B Blocker or as substitute Kannam et al. , 2019

References Borlaug, B. A. & Colucci, W. (2018). Treatment and prognosis of heart failure with preserved ejection fraction. In S. Yeon (Ed. ), Up. To. Date. Retrieved from https: //www. uptodate. com/contents/treatment -and-prognosis-of-heart-failure-with-preserved-ejection-fraction? source=history_widget Colucci, W. (2018). Overview of therapy of heart failure with reduced ejection fraction. In S. Yeon (Ed. ), Up. To. Date. Retrieved from https: //www. uptodate. com/contents/overview-of-therapy-ofheart-failure-with-reduced-ejection-fraction? source=history_widget Kumar, K. (2018). Antiarrhythmic drugs to maintain sinus rhythm in patients with atrial fibrillation: recommendations. In G. Saperia (Ed. ), Up. To. Date. Retrieved from https: //www. uptodate. com/contents/antiarrhythmic-drugs-to-maintain-sinus-rhythm-in-patientswith-atrial-fibrillation-recommendations? source=history_widget Reeder, G. , Awtry, E. , & Mahler, S. (2018). Initial evaluation and management of suspected acute coronary syndrome in the emergency department. In J. Grayzel (Ed. ), Up. To. Date. Retrieved from https: //www. uptodate. com/contents/initial-evaluation-and-management-of-suspected-acutecoronary-syndrome-myocardial-infarction-unstable-angina-in-the-emergencydepartment? source=history_widget Yelland, M (2018). Outpatient evaluation of the adult with chest pain. In J. Givens (Ed. ), Up. To. Date. Retrieved from https: //www. uptodate. com/contents/outpatient-evaluation-of-the-adult-with-chestpain? source=history_widget