Practical Hematology Lab 1 Blood Smear Preparation of
Practical Hematology Lab 1 Blood Smear

Preparation of blood smear n There are three types of blood smears: q q q n The cover glass smear. The wedge smear. The spun smear. The are two additional types of blood smear used for specific purposes q q Buffy coat smear for WBCs < 1. 0× 109/L Thick blood smears for blood parasites.

Wedge blood smear n Specimen : EDTA blood within 2 to 3 hours & collected to the mark on tube. Not's : Changes to RBCs morphology such as Speculated (crenated) cells may occur if : q q q Excessive amount of anticoagulant to specimen Old blood - long standing. Warm environment (room temperature) may hasten changes.

Procedure 1. Placing a drop of blood from mixed sample on a clean glass slide. 2. Spreader slide using another clean glass slide at 30 -40 degree angle. 3. Control thickness of the smear by changing the angle of spreader slide 4. Allow the blood film to air-dry completely before staining. (Do not blow to dry. The moisture from your breath will cause RBC ). Note: Increased the angle of the spreader will decrease the length of the slide The faster the blood is spread on the slide thicker the film will be.
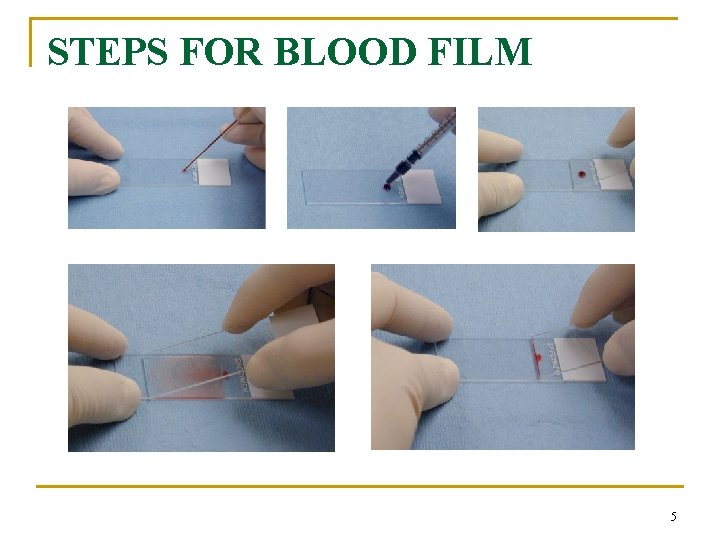
STEPS FOR BLOOD FILM 5


Artifacts n n n Poor spreading techniques. Slow drying (humidity). Insufficient or late fixation. Water contaminating fixation solution (>3%). Certain cell types can be easily damaged by blood film preparation: q q q n Large Number of Atypical lymphocytes. CLL. Acute Leukemia. Degenerative Changes: prolonged or inadequate storage.

Characteristics of a Good Smear Ø Thick at one end, thinning out to a smooth rounded feather edge. Ø Should occupy 2/3 of the total slide area. Ø Should not touch any edge of the slide. Ø Should be margin free, except for point of application.
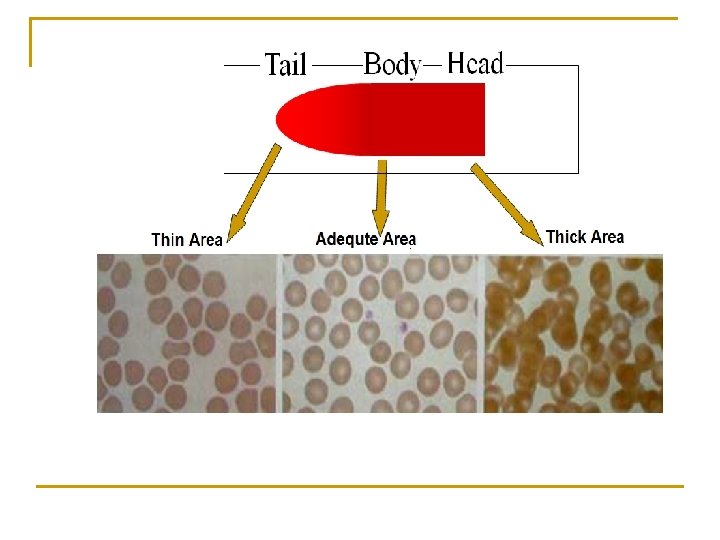
tail body head
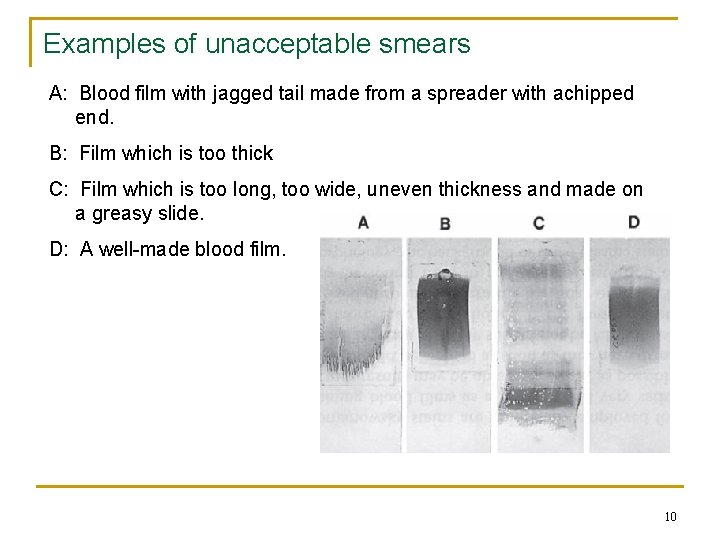
Examples of unacceptable smears A: Blood film with jagged tail made from a spreader with achipped end. B: Film which is too thick C: Film which is too long, too wide, uneven thickness and made on a greasy slide. D: A well-made blood film. 10

Examples of unacceptable smears 11

MORPHOLOGIC CHANGES DUE TO AREA OF SMEAR n Thin area- Spherocytes which are really "spheroidocytes" or flattened red cells. True spherocytes will be found in other (Good) areas of smear. n Thick area - Rouleaux, which is normal in such areas. Confirm by examining thin areas. If true rouleaux, twothree RBC's will stick together in a "stack of coins" fashion. .

Common causes of a poor blood smear n Drop of blood too large or too small. n Spreader slide pushed across the slide in a jerky manner. n Failure to keep the entire edge of the spreader slide against the slide while making the smear. n Failure to keep the spreader slide at a 30° angle with the slide. n Failure to push the spreader slide completely across the slide.

n Irregular spread with ridges and long tail: Edge of spreader dirty or chipped; dusty slide n Holes in film: Slide contaminated with fat or grease n Cellular degenerative changes: delay in fixing, inadequate fixing time or methanol contaminated with water.

Biologic causes of a poor smear n n n Cold agglutinin - RBCs will clump together. Warm the blood at 37° C for 5 minutes, and then remake the smear. Lipemia - holes will appear in the smear. There is nothing you can do to correct this. Rouleaux - RBC’s will form into stacks resembling coins. There is nothing you can do to correct this

g n i tain S & n o i t a n i x i a t F S e s d ’ i t h Sl g i r W

Principle like Romanowsky n Wright’s stain : a metachromatic stain made by Principle mixing old or specially treated stain Methylene blue dye with eosin in a methanol diluent q q Methanol : fixes cells to slide methylene blue stains RNA, DNA blue-grey color Eosin stains hemoglobin, eosin granules orange-red color p. H value of phosphate buffer is very important (6. 4 – 6. 7)

Staining Procedure 1. 2. 3. 4. 5. 6. 7. 8. Thin smear are air dried. Fix the smear with methanol by dip the slide 10 times Flood the smear with stain. Stain for 1 -2 min. Experience will indicate the optimum time. Add an equal amount of buffer solution and mix the stain by blowing an eddy in the fluid. Leave the mixture on the slide for 2 -4 min. Wash off by running water directly to the centre of the slide to prevent a residue of precipitated stain. Stand slide on end, and let dry in air.
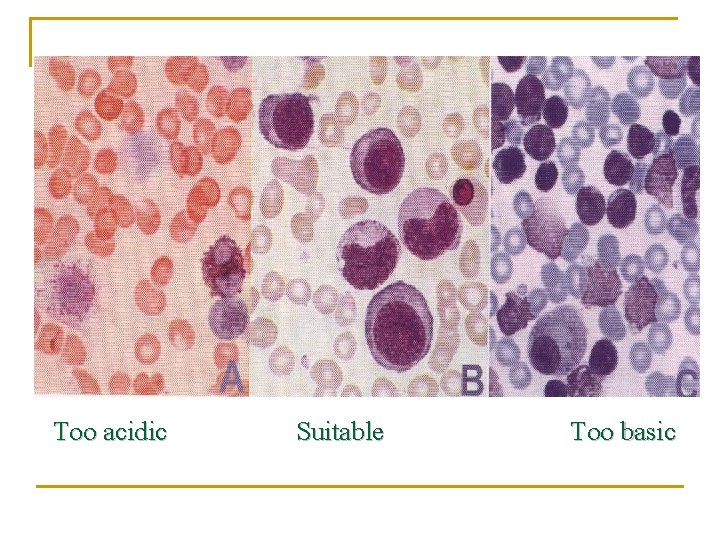
Too acidic Suitable Too basic

Causes & correction n n Too Acid Stain: 1. Insufficient staining time 2. Old stain 3. Acid p. H of stain components Correction: 1) Lengthen staining time 2) Check stain and buffer PH n n Too Alkaline Stain: 1. Thick blood smear 2. Prolonged staining 3. Insufficient washing 4. Alkaline p. H of stain components Correction : 1) Check p. H 2) Shorten stain time 20

d n A l a i t n e r e f f i d y l g a o u l n o a h p M r o A M g n i C B m r R o f g r n e i s P s e s s a
Purposes n White Blood Cells. 1. n Check for distribution and estimate the number present 2. Perform the differential count. 3. Examine for morphologic abnormalities. Platelets. n Red Blood Cells, 1. Size and shape. 2. Relative hemoglobin content. 3. Polychromatophilia. 4. Inclusions. 5. Rouleaux formation or agglutination 1. Estimate number present. 2. Examine for morphologic abnormalities. 22

Observations Under × 10 1. Check to see if there are good counting areas 2. 3. 4. 5. available free of ragged edges and cell clumps. Check the WBC distribution over the smear. Check that the slide is properly stained. Check for the presence of large platelets, platelet clumps, and fibrin strands. Check the presence of any abnormal large cells (megakaryocyte) and parasites.

Observing direction: Observe one field and record the number of WBC according to the different type then turn to another field in the snakeliked direction *avoid repeat or miss some cells

Observations Under 40 x (WBC Estimate) 1. 2. 3. 4. Using the × 40 high dry with no oil. Choose a portion of the peripheral smear where there is only slight overlapping of the RBCs. Count 10 fields, take the total number of white cells and divide by 10. To do a WBC estimate by taking the average number of white cells and multiplying by 2000.

Observations Under 100 x (Platelet ) Estimates 1. Use the oil immersion lens estimate the 2. 3. 4. q number of platelets per field. Look at 5 -6 fields and take an average. Multiply the average by 20, 000. Note any macroplatelets. Platelets per oil immersion field (OIF) q <8 platelets/OIF = decreased q 8 to 20 platelets/OIF = adequate q >20 platelets/OIF = increased

Evaluate WBC Morphology n Note if any abnormal white cell morphology is present q q q Hypersegmented poly's (5 or more lobes) Vacuolation of neutrophils Toxic granulation of neutrophils Dohle bodies Atypical Lymphocytes Smudge cells

Manual Differential Counts n n n These counts are done in the same area as WBC and platelet estimates with the red cells barely touching. This takes place under × 100 (oil) using the zigzag method. Count 100 WBCs including all cell lines from immature to mature. Reporting results Absolute number of cells/µl = % of cell type in differential x white cell count

Observing and Recording Nucleated Red Blood Cells (n. RBCs) n If 10 or more nucleated RBC's (NRBC) are seen, correct the White Count using this formula: Example : If WBC = 5000 and 20 NRBCs have been counted Then 5, 000 × 100/120 = 4166. 65 The corrected white count is 4166. 65 29

Tips on Diff's n Do not count cells that are disintegrating q q Smudge cells Eosinophil with no cytoplasmic membrane and with scattered granules Pyknotic cell (nucleus extremely condensed and degenerated, lobes condensed into small, round clumps with no filaments interconnecting). Basket cells

ABNORMAL DIFFERENTIALS n Count 200 Cell differential: q q q n n n WBC > 15. 0 (>20. 0 for babies under 1 month and labor unit) Three or more basophils seen. If more than five immature WBC's are seen (or any blasts) let someone else diff slide and average results. Correct WBC for NRBC's if you seen ten or more NRBCs/100 WBC. Always indicate number of cells counted on diff. If any cell type is extremely elevated (such as bands, monocytes, or eosinophils > 20) indicate that you are aware of the abnormality by circling or checking on the card next to the results.

Recording RBC Morphology n n n Scan area using × 100 (oil immersion). Observe 10 fields. Red cells are observed for size, shape, hemoglobin content, and the presence or absence of inclusions. Abnormal morphology: Red cell morphology is assessed according to See the following sample grading system. Note that red cell morphology must be scanned in a good counting area. Two questions should be asked q q n Is the morphology seen in every field? Is the morphology pathologic and not artificially induced? Next Table represents a system derived to determine a quantitative scale.
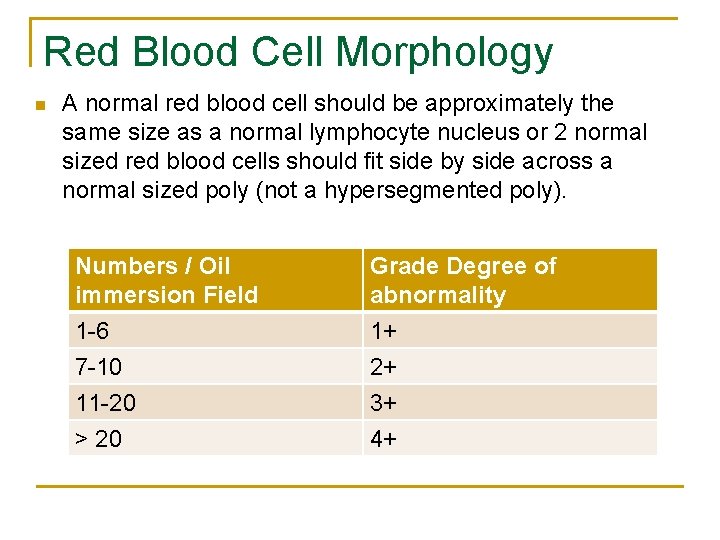
Red Blood Cell Morphology n A normal red blood cell should be approximately the same size as a normal lymphocyte nucleus or 2 normal sized red blood cells should fit side by side across a normal sized poly (not a hypersegmented poly). Numbers / Oil immersion Field 1 -6 7 -10 11 -20 > 20 Grade Degree of abnormality 1+ 2+ 3+ 4+

Reporting results n n Where possible use macrocytic and microcytic, rather than simply anisocytosis alone, when describing red cell morphology. Use specific cell morphology when possible, rather than simply reporting poikilocytosis. When red cells are normocytic, normochromic, report out as NORMAL. When abnormal morphology has been noted, DO NOT indicate normal on the report form. EXAMPLE: 7 -10 microcytic RBC's/OIF is reported out as: 2+ microcytosis or Moderate microcytosis.

determine a quantitative scale 1
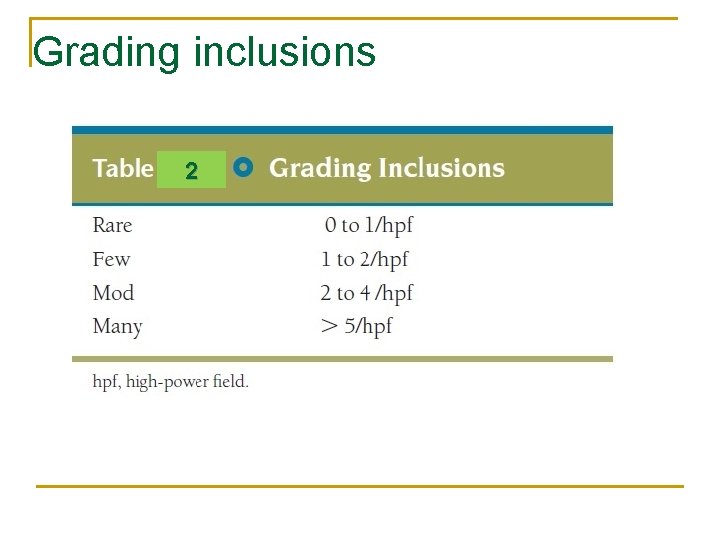

Grading inclusions 2

C B W f o y g o l o h d p o r o l b Mo l a r e h p i r e in p

Normal peripheral blood smear

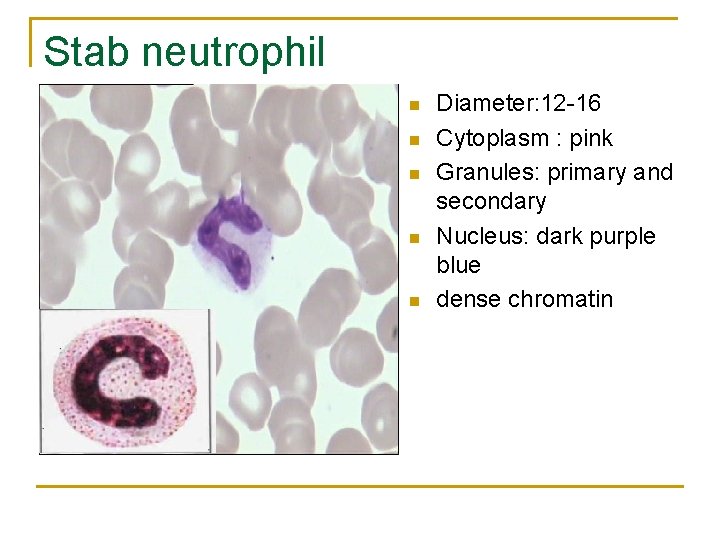
Stab neutrophil n n n Diameter: 12 -16 Cytoplasm : pink Granules: primary and secondary Nucleus: dark purple blue dense chromatin
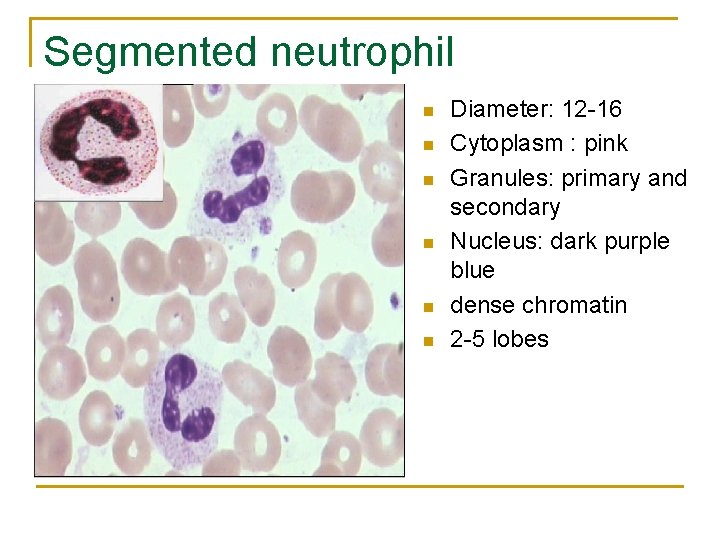
Segmented neutrophil n n n Diameter: 12 -16 Cytoplasm : pink Granules: primary and secondary Nucleus: dark purple blue dense chromatin 2 -5 lobes
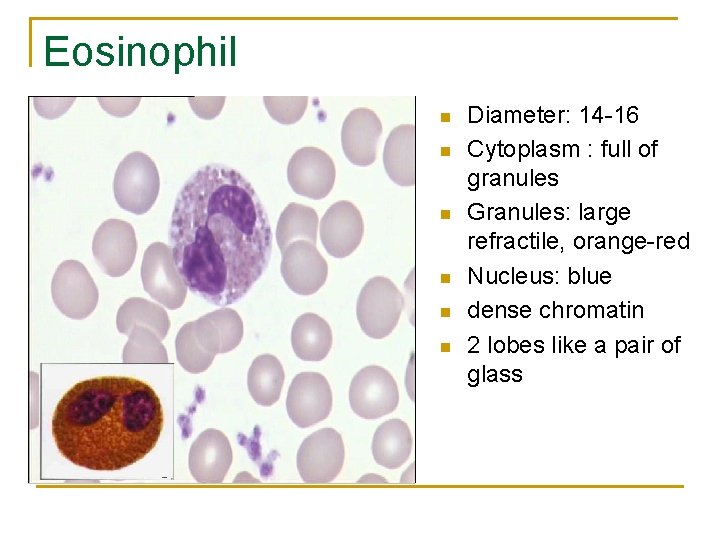
Eosinophil n n n Diameter: 14 -16 Cytoplasm : full of granules Granules: large refractile, orange-red Nucleus: blue dense chromatin 2 lobes like a pair of glass
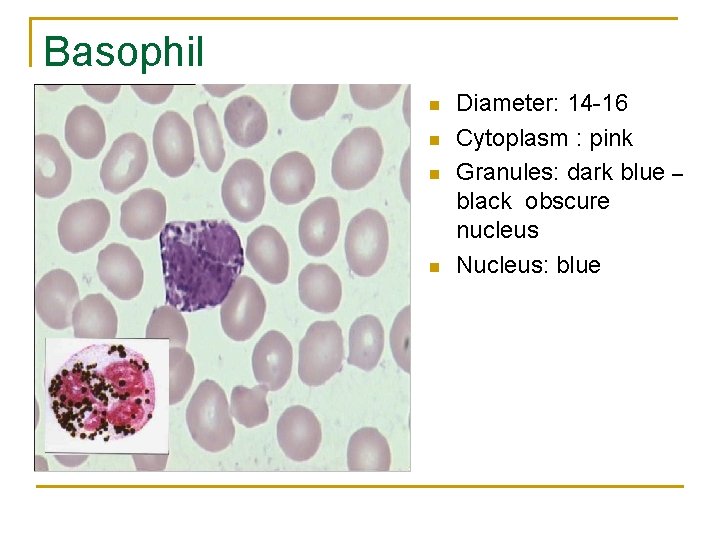
Basophil n n Diameter: 14 -16 Cytoplasm : pink Granules: dark blue – black obscure nucleus Nucleus: blue
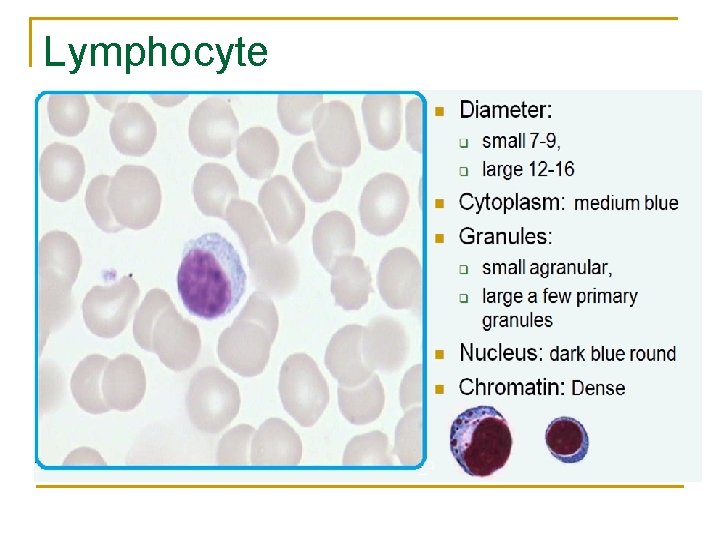
Lymphocyte
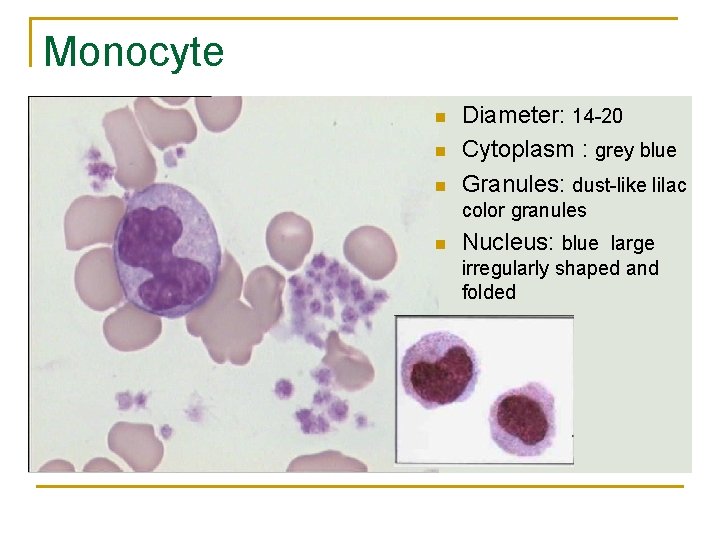
Monocyte n n n Diameter: 14 -20 Cytoplasm : grey blue Granules: dust-like lilac color granules n Nucleus: blue large irregularly shaped and folded

s e g n a h y c g l o a l o m h r p o r n o b m A C B W f o

Left-shift and right-shift of neutrophil: n n Left-shift: non-segmented neutrophil > 5% Right-shift: hypersegmented neutrophil >3%
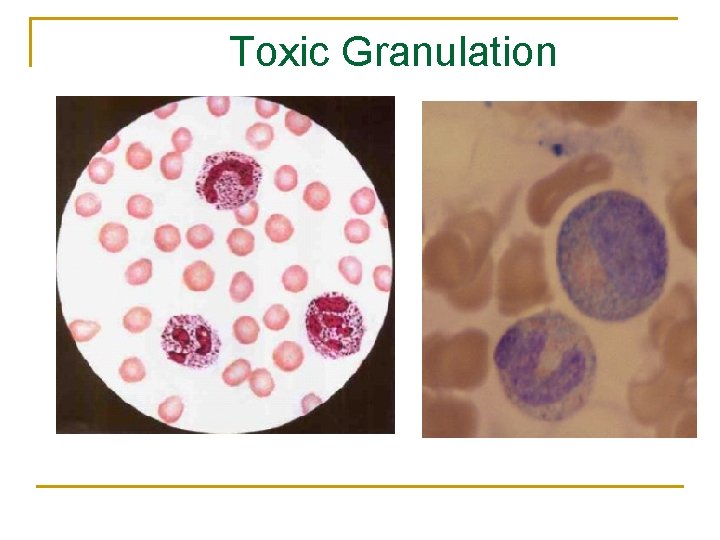
Toxic Granulation
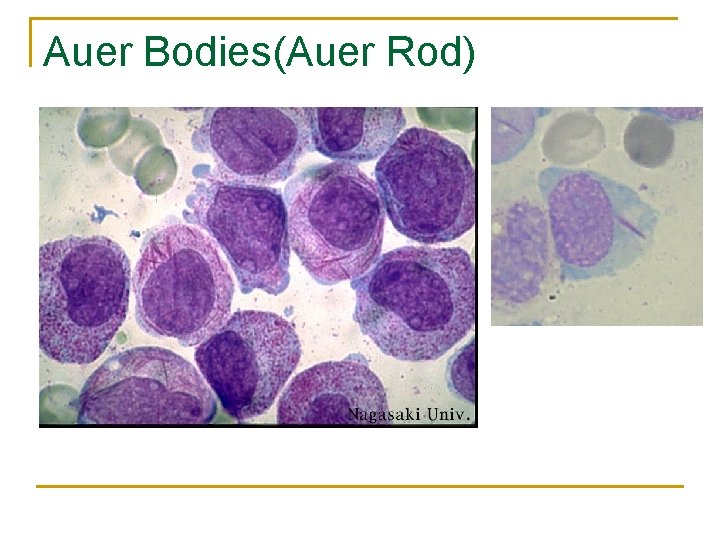
Auer Bodies(Auer Rod)
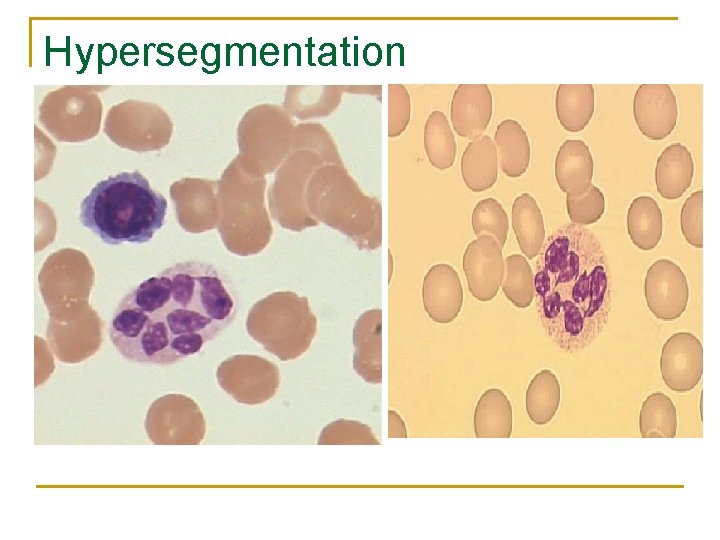
Hypersegmentation
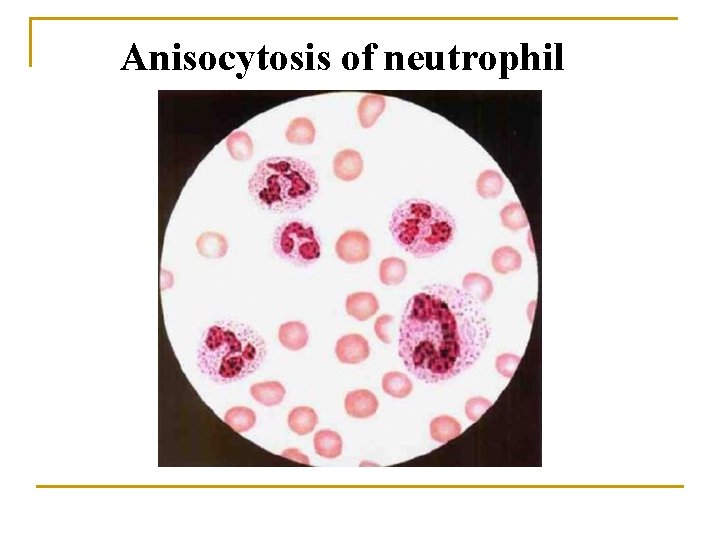
Anisocytosis of neutrophil
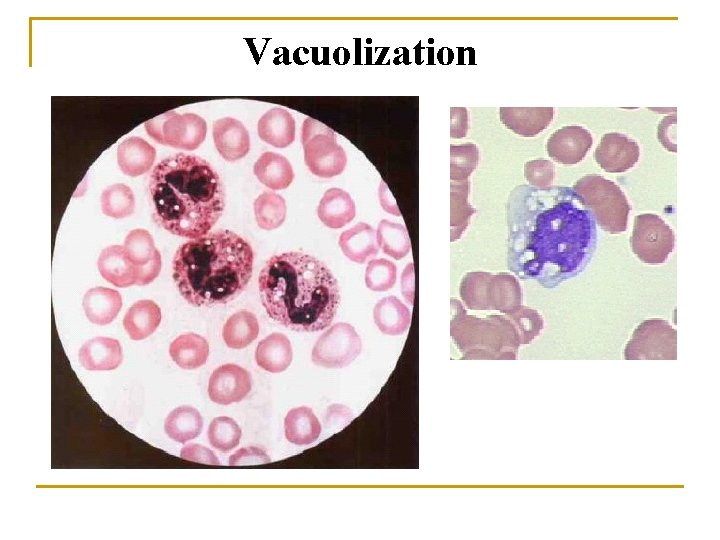
Vacuolization
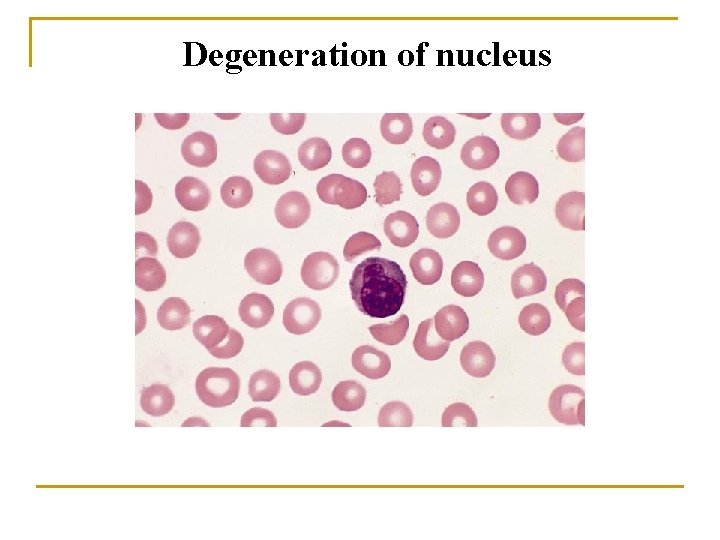
Degeneration of nucleus
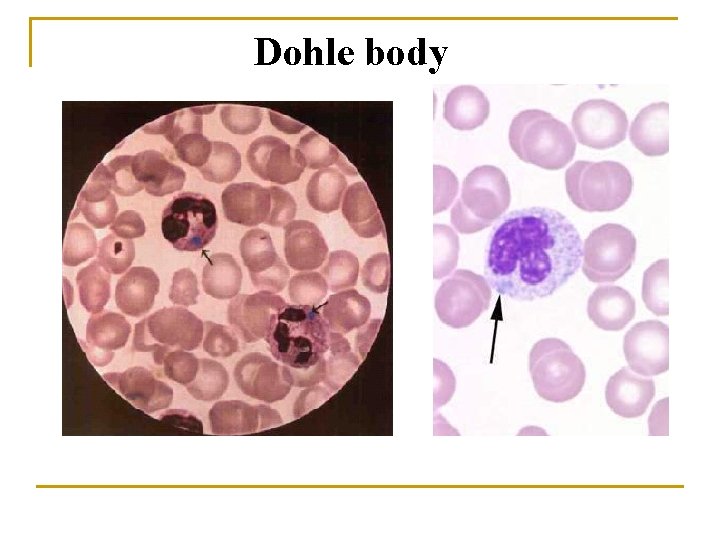
Dohle body

Thank you
- Slides: 55