Practical Clinical Pathology Blood Proteins Lipids Wendy Blount

Practical Clinical Pathology Blood Proteins & Lipids Wendy Blount, DVM
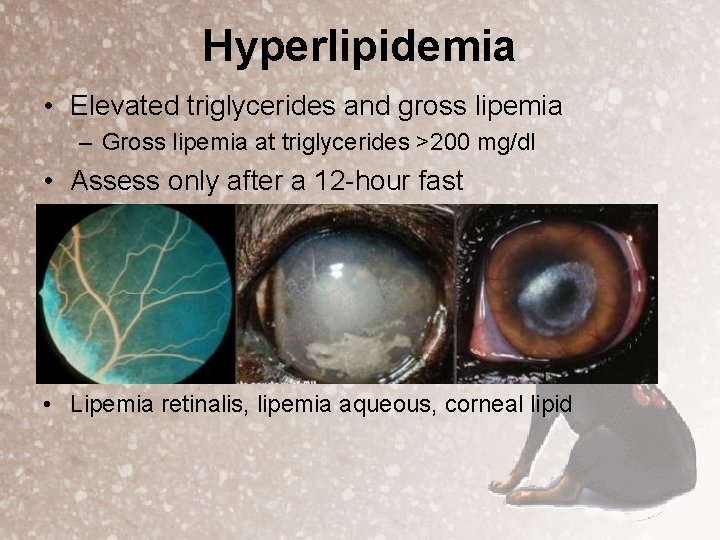
Hyperlipidemia • Elevated triglycerides and gross lipemia – Gross lipemia at triglycerides >200 mg/dl • Assess only after a 12 -hour fast Clinical Signs • GI upset, abdominal pain, pancreatitis • PU-PD • Ataxia, weakness, behavioral changes, seizures – Danger value - >1000 mg/dl • Lipemia retinalis, lipemia aqueous, corneal lipid

Hyperlipidemia • Elevated triglycerides and gross lipemia – Gross lipemia at >200 mg/dl • Assess only after a 12 -hour fast Clinical Signs • GI upset, abdominal pain, pancreatitis • PU-PD • Ataxia, weakness, behavioral changes, seizures – Danger value - >1000 mg/dl • Lipemia retinalis, lipemia aqueous, corneal lipid • Xanthoma
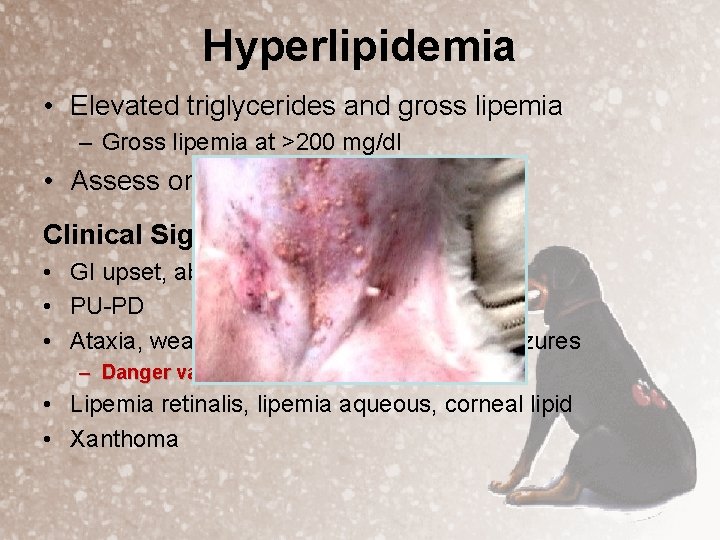
Hyperlipidemia • Elevated triglycerides and gross lipemia – Gross lipemia at >200 mg/dl • Assess only after a 12 -hour fast Clinical Signs • GI upset, abdominal pain, pancreatitis • PU-PD • Ataxia, weakness, behavioral changes, seizures – Danger value - >1000 mg/dl • Lipemia retinalis, lipemia aqueous, corneal lipid • Xanthoma

Hyperlipidemia DDx High Triglycerides • Post-prandial elevation • Primary hyperlipidemia – miniature schnauzers, shelties >> cats • Secondary hyperlipidemia – Endocrine – hypothyroidism, hyperadrenocorticism, diabetes – Pancreatitis, cholestasis – Liver disease, nephrotic syndrome • Drugs – Glucocorticoids, estrogens – Phenobarbital, bromide – Megace in the cat

Hyperlipidemia

Hyperlipidemia Diagnostic work-up • First Tier Tests – CBC, serum profile with electrolytes, UA – c. PL or CPLI – Thyroid panel: canine TSH, TT 4, f. T 4; feline TT 4, f. T 4 • Second Tier Tests – If signs of hyperadrenocorticism - Low Dose Dexamethasone Test and/or ACTH Stim – If hyperglycemia needs further investigation – fructosamine – If proteinuria – Urine P: C ratio x 3 days – If signs of liver disease – bile acids • Trial Therapy for primary hyperlipidemia (handout) handout (Client Handout)

Hypercholesterolemia DDx high cholesterol • • • Hypothyroidism Hyperadrenocorticism Diabetes mellitus Liver Disease Protein losing nephropathy Drugs – corticosteroids, methimazole – phenothiazines – phenytoin, thiazide diuretics
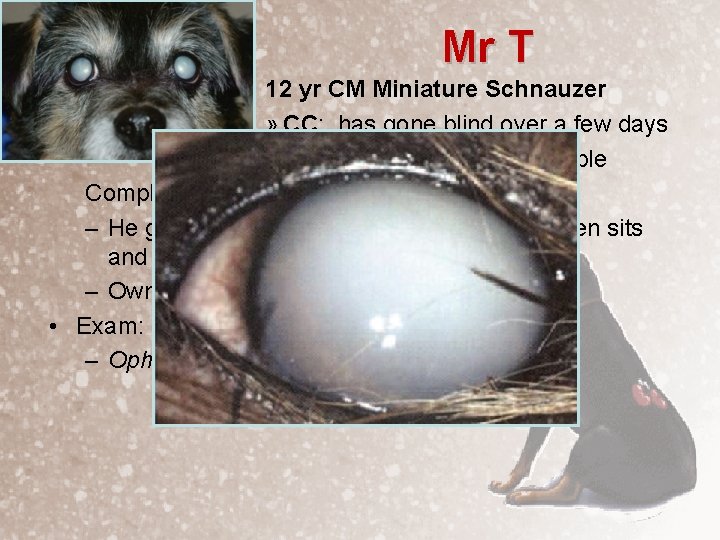
Mr T 12 yr CM Miniature Schnauzer » CC: has gone blind over a few days » Hx: Mr T also has had trouble Completing his evening walks for a few weeks – He gets weak in the rear end and twitchy, then sits and refuses to continue. – Owner carries him home • Exam: the eyes appear white – Ophthalmic exam

Mr T 12 yr CM Miniature Schnauzer » CC: has gone blind over a few days » Hx: Mr T also has had trouble Completing his evening walks for a few weeks – He gets weak in the rear end and twitchy, then sits and refuses to continue. – Owner carries him home • Exam: the eyes appear white – Ophthalmic exam – the anterior chamber is opaque – can’t see the lenses, irises are obscured – Scleral injection, lipemia aqueous – Neurologic exam – no abnormalities in gait, posture, postural responses, or cranial/spinal nerve reflexes, normal pain sensation

Mr T CBC: NSAF » panel: bili 8. 2, phos 9. 3, glu 187 ALKP 1122 U/L (Idexx Catalyst) • Send triglycerides to TVMDL: 4400 mg/dl • All abnormalities on panel may be artifact • Mr T has not eaten since last night • DDx: – – Diabetes mellitus, hypothyroidism, Cushings Severe glomerular disease Pancreatitis, liver disease Familial hyperlipidemia

Dx Plan: » Mr T Thyroid Panel – TSH, TT 4, f. T 4 normal Urinalysis – SG 1. 032, protein neg – – c. PL – normal – Fasting and 2 hr post-prandial bile acids – normal – Fructosamine - normal – Abdominal US – sludge in GB, no evidence of HAC Tx Plan: – High fiber, low fat diet – Purina OM – Other options: r/d, w/d, RC Diabetic, Purina DCO, Eukanuba Glucose Control, Eukanuba Reduced Fat – Fish Oil 500 -700 mg EPA/DHA daily – Recheck fasting triglycerides 30 days

Mr T 30 Days Later: » Fasting Triglycerides – 1254 mg/dl eyes clear, symptoms resolved Tx Plan: – Increase Fish Oil to 1000 -1500 mg EPA/DHA daily – Niacinamide 250 mg once daily – Recheck fasting triglycerides 30 days 30 Days Later: doing well – Fasting Triglycerides – 567 mg/dl

Attendee 6 – City TX

Hypocholesterolemia DDx low cholesterol • • • Liver Disease – portacaval shunt, cirrhosis Lymphangiectasia Selected neoplasias Starvation Addison’s Disease Drug therapy – – L-asparaginase, azathioprine Colchicine Cholestyramine Oral aminoglycosides

Serum Proteins TP = albumin + globulins Albumin • provides 75 -80% of the colloid oncotic pressure (COP) • COP is the force that keeps water from escaping the intravascular space • Acts as a protein carrier of many endogenous and exogenous substances

Serum Proteins TP = albumin + globulins Albumin • provides 75 -80% of the colloid oncotic pressure (COP) • COP is the force that keeps water from escaping the intravascular space • Acts as a protein carrier of many endogenous and exogenous substances • Nutrition for healing and microvascular integrity • Acts as a buffer and prevents hypercoagulation

Serum Proteins TP = albumin + globulins Albumin • Danger values - <1. 0 g/dl – Major fluid shifts – pulmonary and peripheral edema, third space accumulation – Simultaneous loss of AT 3 – thromboembolic disease • Pulmonary thromboembolism (PTE) • mesenteric thrombus • portal vein thrombus • If portal hypertension, ascites can occur at albumin <1. 5 g/dl
Serum Proteins DDx increased Albumin • Dehydration • Falsely increased (refractometer) – – – Lipemia severe hyperglycemia Azotemia Hyperchloridemia, hypernatremia Severe hyperbilirubinemia
Serum Proteins DDx hypoalbuminemia 1. Not making/assimilating enough albumin – – liver failure anorexia, hyporexia maldigestion, malabsorption (Protein Losing Enteropathy) Severe malnutrition (starvation) 2. Albumin Loss – – – Protein losing enteropathy (PLE) Protein losing nephropathy (PLN) – glomerular disease Exudative wounds and lesions External hemorrhage – including GI loss Addison’s disease
Serum Proteins DDx hypoalbuminemia 3. Albumin Consumption – – Sepsis Pancreatitis 4. Sequestration – body effusions - can cause or be caused by hypoalbuminemia • – Due to increase hydrostatic pressure, decreased oncotic pressure or leaky vessels (mild to moderate changes) Vasculitis – immune mediated, infectious (bacteria, rickettsial) 5. Secondary to hyperglobulinemia – mild to moderate 6. Dilution from aggressive IV fluid therapy – mild to mod 7. Lab error – Human labs give falsely low values for canine albumin – Abaxxis also had problems for awhile

Addison’s and Hypoalbuminemia • Hypoalbuminemia can be the primary presenting symptom of Addison’s (15%) • Hypocholesterolemia is present in 10% of Addisonians • Both can be caused by GI malabsorption • GI blood loss also contributes to hypoalbuminemia
Serum Proteins Stepwise work-up for low albumin 1. If no exudative skin lesions, do first tier tests • CBC, panel, UA, fecal flotation • K 9 HW Test, Feline Fe. LV/FIV tests 2. Then indicated second tier tests • If liver pattern on panel – bile acids, blood ammonia • If proteinuria without pyuria or hematuria – Urine P: C • If profuse diarrhea, consider PLE – GI diagnostics – GI panel, intestinal biopsies – Or confirm with fecal alpha-1 proteinase inhibitor assay • If effusions, sample fluid – Transudate indicates effusion is likely due to hypoproteinemia – Modified transudate or exudate means other factors are in play
Serum Proteins Stepwise work-up for low albumin 2. Then indicated second tier tests • Imaging – thoracic rads + abdominal US or Global. FAST® • Tick disease panel or Rx doxycycline • ACTH stimulation Test 3. Then indicated third tier tests for vasculitis • Skin biopsy • If vasculitis and no apparent cause, consider immunosuppression

Alpha-1 Proteinase Inhibitor • • • TAMU GI Lab 1 g (<1/4 teaspoon) naturally passed feces Collect daily for three days, and freeze Ship overnight, on ice Normal ranges do not apply to puppies and kittens

Serum Proteins Drugs that alter albumin Increased albumin: Decreased albumin: • Long term high dose corticosteroids • Estrogens • Anticonvulsants (if liver disease) • Acetaminophen • Antineoplastics - CCNU The most common causes of albumin <2. 0 g/dl are liver failure and PLE and/or GI hemorrhage are possible even when owners think stools are normal
Serum Proteins Look at serum proteins together! • Very high globulins and mild hypoalbuminemia (>2 g/dl) – Work up hyperglobulinemia first • Low albumin and low globulin – panhypoproteinemia Non-selective protein loss – – External hemorrhage (including GI loss) – also low PCV Exudate skin wounds Protein losing enteropathy (PLE) Hemodilution – aggressive IV fluid therapy • Low albumin and normal globulin – Selective loss or sequestration of albumin – effusions, vasculitis, PLN – Poor albumin production (Liver disease)

Serum Proteins Look at serum proteins together! • Low globulins and normal to increased albumin – – – Immunodeficiency – congenital or acquired Congenital immunodeficincies result in neonatal death which is difficult to definitively diagnose Acquired immunodeficiencies often due to lymphoproliferative disease or cancer chemotherapy • High albumin and globulin – nonselective hyperproteinemia – dehydration

Serum Proteins • DDx high globulins – Increased acute phase proteins cause a mild increase – Chronic antigenic stimulation – plasma cells in lymph nodes and bone marrow making antibodies • • Heartworm disease FIP, acromegaly in cats Severe dermatitis Other chronic infection – Immune mediated disease – systemic lupus erythematosis and is many variations – Paraproteinemia – multiple myeloma and other neoplasia

Serum Proteins Acute Phase Proteins – alpha & beta globulins • indications – Need specific information about inflammation or coagulation • Examples: – – – Fibrinogen (Cornell) Cornell Haptoglobin (Kansas State U) U C-reactive protein (TAMU GI Lab) Lab Complement c 3 a Serum amyloid A • Alpha-1 -acid glycoprotein • Alpha-1 antiproteinase (TAMU GI Lab) Lab • Alpha-2 macroglobulin • Ceruloplasmin (KSU) KSU • Hemolysis and lipemia can interfere • Negative acute phase proteins decrease w/ inflammation – albumin, transferrin (KSU), KSU antithrombin 3 (Cornell) Cornell

Serum Proteins Acute Phase Proteins – alpha & beta globulins • High Fibrinogen – indicates acute inflammation – In house meters are available • Low Fibrinogen – consumptive coagulopathy such as DIC – Rare congenital deficiencies

Serum Proteins Diagnosis of Hyperglobulinemia 1. Rule out most common causes: • Severe dermatitis – find and treat cause • Heartworm disease in dogs, FIP in cats • Exudative body cavity effusions, including polyarthritis – Global. FAST® ultrasound • Lymphadenopathy – FNA lymph nodes 2. First Tier Tests • CBC, panel/lytes, UA • Fe. LV/FIV in cats • UPC if proteinuria on dipstick
Serum Proteins Diagnosis of Hyperglobulinemia 3. Second Tier Tests • thoracic rads and abdominal ultrasound - FNA liver/spleen + abnormal organs • Tick disease panel or Rx doxycycline 4. Third Tier Tests – • ANA – mediocre screen for immune mediated disease • Whole body rads, protein electrophoresis, Bence Jones protein for myeloma • Consider fungal/protozoal antigen, antibody tests • Blood, urine, macerated tissue biopsy cultures • Last resort – diagnostic surgery for multiple biopsies

Summary Power. Point – Proteins and Fats • . pptx • . pdfs – 1 and 6 slides per page Vet Handouts • Blount – Hyperlipidemia • Willard – Algorithm for Dx of Hyperglobulinemia • Willard – Algorithm for Dx of Hyperlipidemia • Willard – Algorithm for Hypoalbuminemia

Summary Client Handouts • Blount – Hyperlipidemia Laboratory Information • KSU – Haptoglobin, ceruloplasmin, transferrin assays • TAMU GI Lab – C Reactive Protein Cornell (fibrinogen) – Submission Form, Guidelines, Shipping, Fees, Patient Sample Labels, Blood Collection Guidelines, Credit Card Form

Acknowledgements • Richard Nelson. Small Animal Clinical Diagnosis by Laboratory Methods, 5 th Edition. Ch 8 – Endocrine, Metabolic and Lipid Disorders. Eds. Michael Willard, Harold Tvedten. • Mark C Johnson. Small Animal Clinical Diagnosis by Laboratory Methods, 5 th Edition. Ch 12 – Immunologic and Plasma Protein Disorders. Eds. Michael Willard, Harold Tvedten.

Acknowledgements J Catharine Scott-Moncrief. Canine & Feline Endocrinology, 4 th Edition. Ch 12 – Canine Hypoadrenocorticism. Lathan & Thompson. Management of hypoadrenocorticism (Addison’s Disease) in dogs. Vet Med Res & Rpts. 2018: 9 1– 10. CAVMA presentation on Hypoalbuminemia
- Slides: 37