Practical Cardiology Case Studies Wendy Blount DVM Nacogdoches
Practical Cardiology Case Studies Wendy Blount, DVM Nacogdoches TX

Ginger Signalment • 12 year old SF cocker spaniel Chief complaint • Several episodes of collapse during the past month • Description matches partial seizure • Rear legs get weak on walks • Lethargic and dull in general
Ginger Exam • Dark maroon oral mucous membranes • Rear foot pads cyanotic (heart sounds) • Split S 2 • Neurologic exam normal, except dull mental status

Ginger Differential Diagnosis – Split S 2 • Pulmonic and aortic valves don’t close at the same time – Pulmonary hypertension – Normal variation in giant dogs – Reverse PDA Differential Diagnosis - cyanosis • Respiratory hypoxia • Cardiac hypoxia

Ginger Initial Diagnostic Plan • CBC, GHP, electrolytes • Arterial blood gases, Pulse oximetry • ECG • Thoracic radiographs Bloodwork • Tech couldn’t get enough serum for serology • CBC – PCV 73% • GHP and electrolytes - normal

Ginger DDx Differential Cyanosis • FATE – Femoral Artery Thrombo. Embolism – Lack of femoral pulses – Feet cool to the touch • Right to Left shunt – ductus is distal to the brachiocephalic trunk – Reverse PDA – AV fistula with pulmonary hypertension – Tetralogy of Fallot
Ginger Arterial blood gases • p. O 2 – 52 mm. Hg • p. CO 2 – 36 mm. Hg • all else normal Pulse oximetry • Lip – O 2 sat 89% • Vulva - O 2 sat 67%
Ginger
Ginger

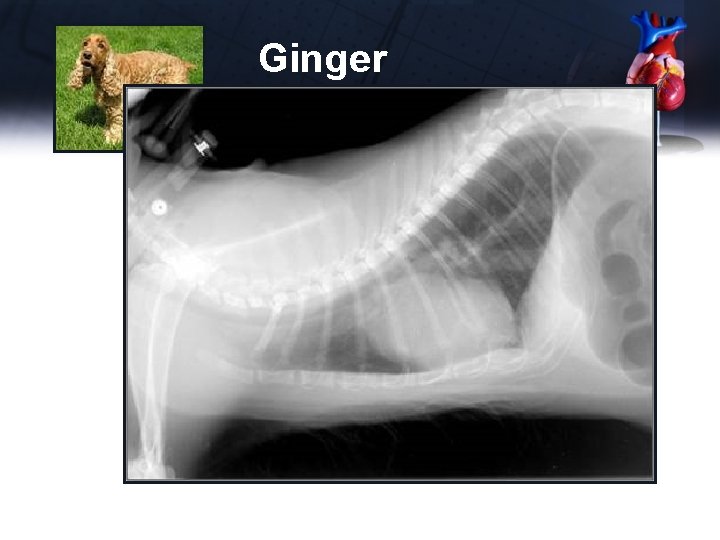
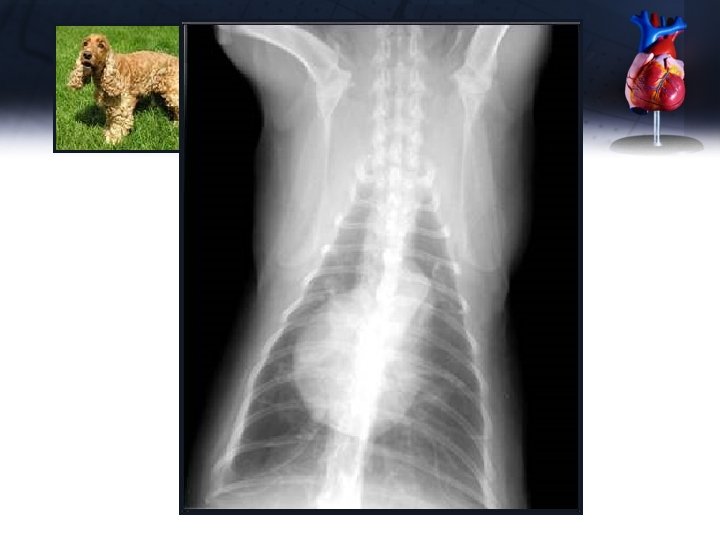
Ginger Thoracic radiographs • Normal great vessels • Normal heart size (VHS 9. 5) • aortic bulge on VD, PA bulge on VD • No evidence of severe respiratory disease which might cause hypoxia • No evidence of heart failure
Ginger ECG

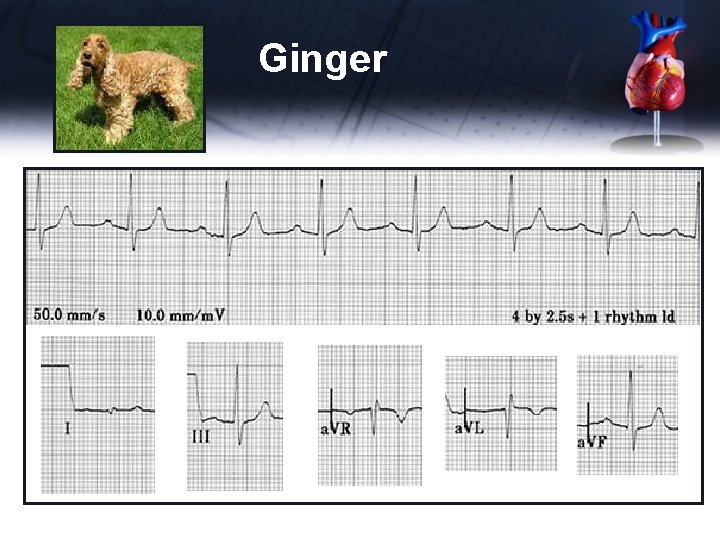
Ginger ECG • S wave mildly deep in leads II, III, a. VF • MEA 90 o • Arrhythmia doesn’t seem likely Differential Diagnoses • Right to left shunt • Pulmonary hypertension • Severe respiratory disease and anemia ruled out
Ginger

Ginger Right to Left Shunt • Reverse PDA (right to left) – Eisenmeinger’s physiology • Tetralogy of Fallot • AV fistula with pulmonary hypertension Echocardiogram
Ginger Right to Left Shunt • Reverse PDA (right to left) – Eisenmeinger’s physiology • Tetralogy of Fallot • AV fistula with pulmonary hypertension Echocardiogram
Ginger Right to Left Shunt • Reverse PDA (right to left) – Eisenmeinger’s physiology • Tetralogy of Fallot • AV fistula with pulmonary hypertension Echocardiogram

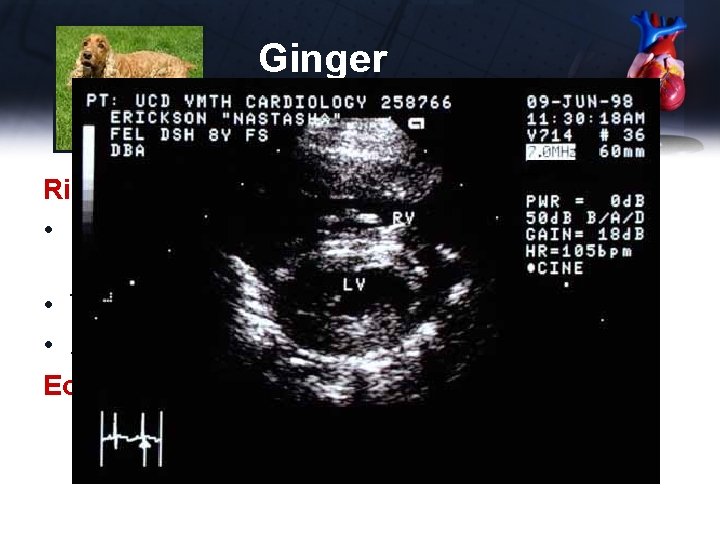
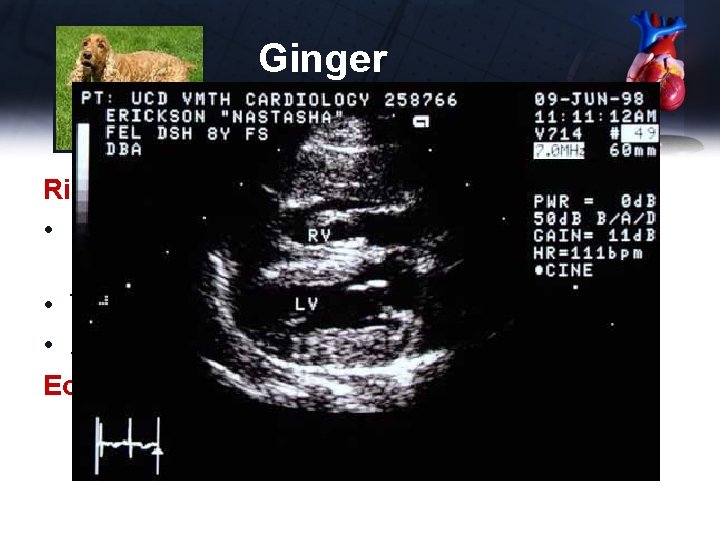
Ginger Right to Left Shunt • Reverse PDA (right to left) • Tetralogy of Fallot • AV fistula with pulmonary hypertension Echocardiogram • RV thickening, flattening of the IVS • RV normally thinner than LV • No PDA seen without Doppler

Ginger Bubble Study • Place venous catheter • Shake 5 -10 cc saline vigorously • Place US probe where you can look for shunting – Long 4 chamber view – Abdominal aorta • Inject IV quickly • Bubbles normally appear on the right (video) • Watch for bubbles on the left (this means R to L shunt) • False negatives when bubbles disperse quickly

Reverse PDA • Reverse PDAs are usually large, providing no resistance to blood flow – Ductus is often as large in diameter as the great vessels it connects • increase in pulmonary artery pressure combined with the increase in pulmonary blood flow creates pathologic responses in the pulmonary arteries over time • a continuous murmur is heard during the first days to weeks of life but disappears before the eighth week • Often do well until polycythemia develops late in life

Reverse PDA Treatment • Ligation of right to left shunting PDA results in death due to pulmonary hypertension – Has been ligated in stages without causing death – Cyanosis and symptoms usually persist • Managed Medically by periodic phlebotomy – – – Remove 10 ml/lb and replace with IV fluids Eliminate hyperviscosity without inducing hypoxia Goal for PCV is 60 -65% Excellent blood for RBC transfusion ; -) Repeat when clinical signs return

Reverse PDA Treatment • Hydroxyurea – 30 mg/kg/day for 7 to 10 days followed by 15 mg/kg/day. – CBC q 1 -2 weeks – D/C when Bone marrow suppression – Resume lower dose – Some dogs require higher doses – side effects – GI and sloughing of the nails

Reverse PDA Prognosis • Can do well short term • Poor prognosis long term – Survival months to a year or two • Phlebotomy interval is progressively shorter, and then eventually the phlebotomies become minimally effective to ineffective

Hank Signalment • 10 week old male schnauzer Chief Complaint • Loud heart murmur heard on examination for routine vaccinations • Suspect congenital heart defect

Hank Exam • mm pink, CRT 2 sec • 4/6 ejection murmur loudest at left heart base (audio) • Mild superficial pyoderma

Hank Initial Differential Diagnoses • Pulmonic stenosis • Aortic Stenosis Initial Diagnostic Plan • Chest x-rays • EKG • Echocardiogram
Hank
Hank

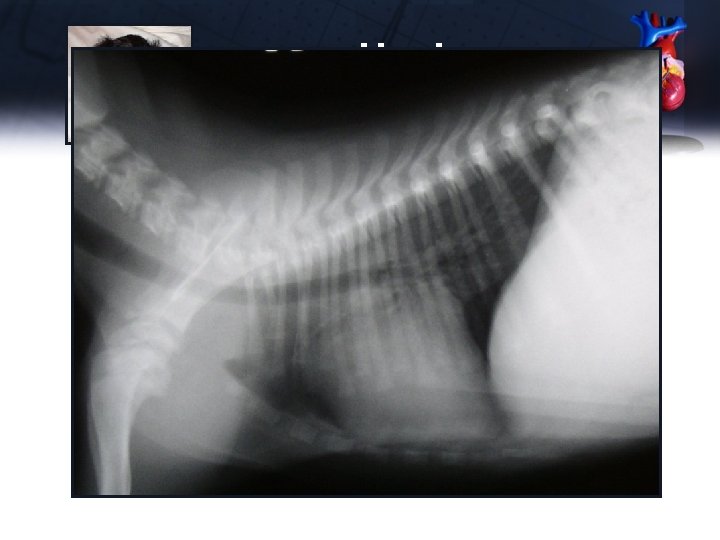
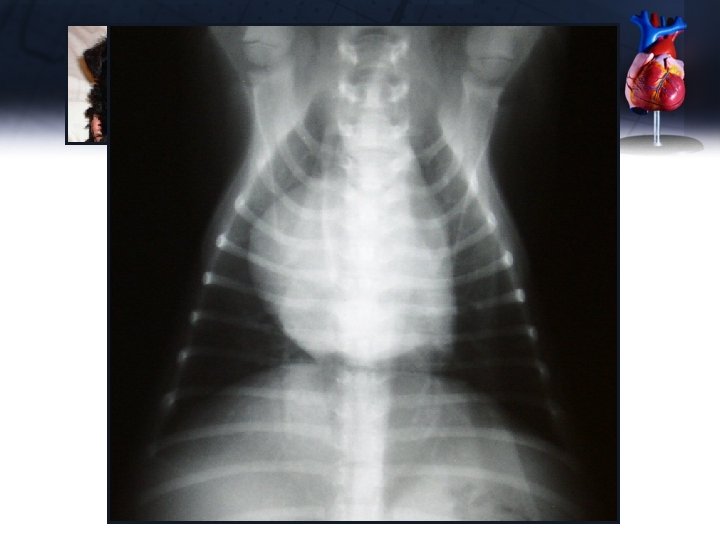
Hank Thoracic radiographs • Dorsally elevated trachea • Vertebral heart score 9. 5 • Right heart enlargement • Right auricular/atrial enlargement • Distended caudal vena cava • Bulge at main pulmonary artery
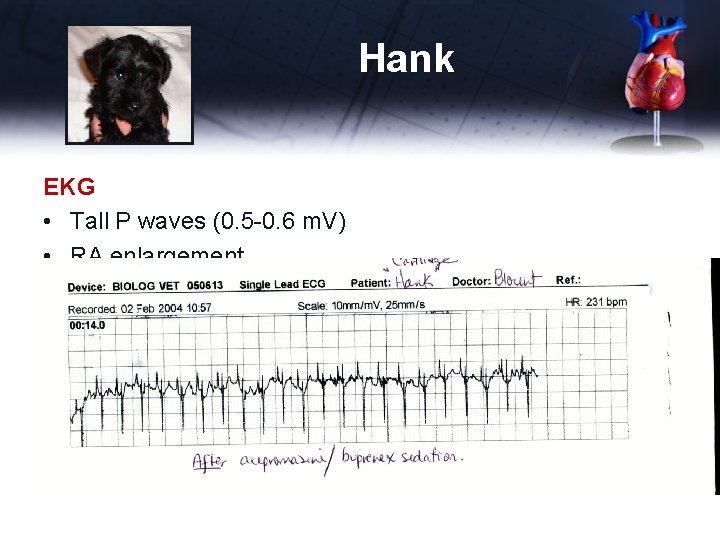
Hank EKG • Tall P waves (0. 5 -0. 6 m. V) • RA enlargement • Deep S waves in leads I, II and III (-13 to -15 m. V) • RV enlargement • Tachycardia 200 -210 bpm • Under Buprenex-ace sedation
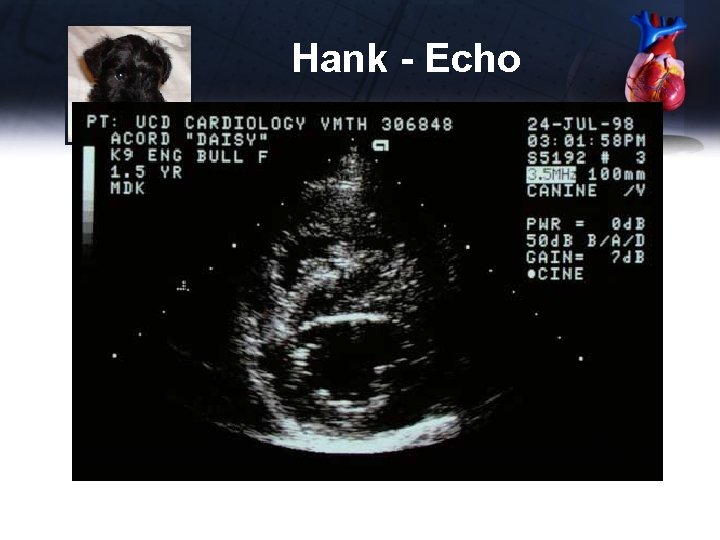
Hank - Echo

Hank - Echo Short Axis – LV Apex • RV seems thickened Short Axis – LV PM, MV, Ao/RVOT • RV as thick as LV – markedly thickened • IVS is flattened
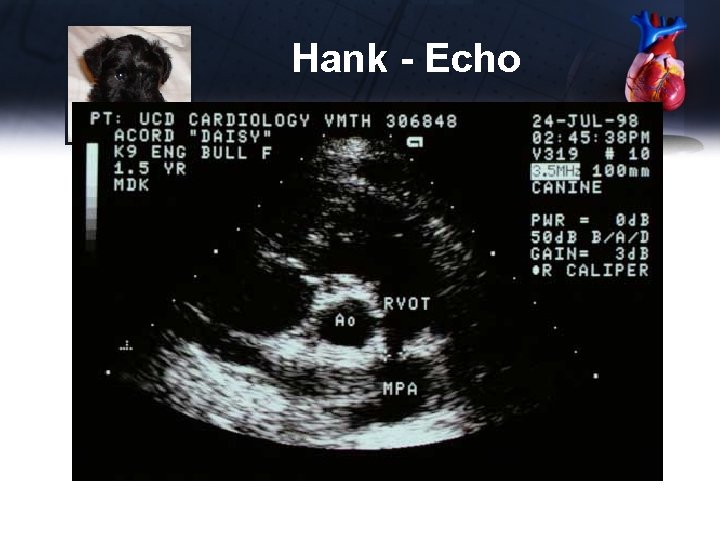
Hank - Echo

Hank - Echo Short Axis – PA • MPA dilated • RV as thick as LV – markedly thickened Long Axis – 4 Chamber • Aberrant septum dividing RA into 2 chambers – cranial and caudal Long Axis – LVOT • RV as thick as LV – markedly thickened
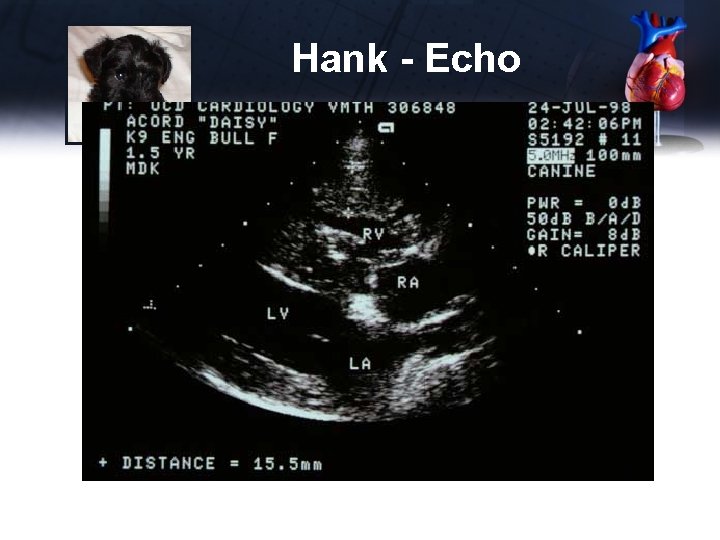
Hank - Echo

Hank - Echo Diagnosis • Likely Pulmonic Stenosis • DDx RV thickening – Heartworms impossible in a 10 week old puppy – Pulmonary hypertension rare in a 10 week old puppy • Need Doppler to confirm, and to determine gradient • Cor triatum dexter

Hank - Echo Plan – updated • Referral to TAMU for balloon valvuloplasty • Atenolol 0. 5 mg/kg PO BID (monitor weight to increased dose PRN until cath procedure)

Pulmonic Stenosis Clinical features • Many breed predispositions – Bulldog, chihuahua, Beagle, Cavalier • Often valvular and subvalvular • Valvular defect can be corrected by valvuloplasty • Prognosis varies, depending on severity – Mild – less than 50 mm Hg gradient – Moderate – 50 -100 mm Hg – Severe - >100 mm Hg • Can be progressive

Pulmonic Stenosis Clinical features • Bulldogs and Boxers can have left coronary artery anomaly, which can preclude balloon valvuloplasty • Arrhythmia is much more common than RHF • May be part of Tetralogy of Fallot – – PS RV hypertrophy VSD Overriding aorta
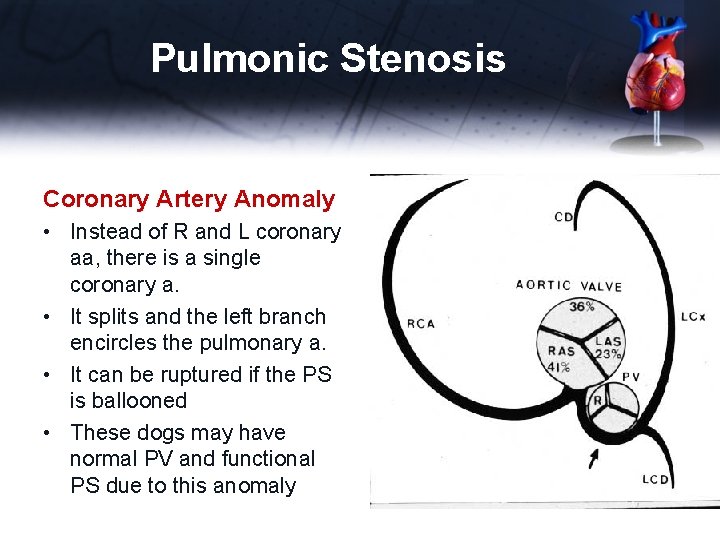
Pulmonic Stenosis Coronary Artery Anomaly • Instead of R and L coronary aa, there is a single coronary a. • It splits and the left branch encircles the pulmonary a. • It can be ruptured if the PS is ballooned • These dogs may have normal PV and functional PS due to this anomaly

Pulmonic Stenosis Echocardiographic abnormalities • RV thickening • Post-stenotic dilatation of MPA • Pulmonic valve may be thickened with poor movement • Paradoxical septal motion may be noted in severe cases • Tricuspid dysplasia is a common concurrent malformation – RHF is rare in dogs with PS alone – Many PS dogs that develop RHF also have tricuspid dysplasia (Client Handout)

Suzie Signalment • 2 year old female chihuahua mix Chief Complaint • Loud heart murmur heard on free examination for shelter pup

Suzie Exam • Left apex (audio) – holosystolic murmur PMI left apex (MR murmur) due to left volume overload • Left axilla (audio) – Continuous machinery murmur at the left base (left armpit) • Hyperkinetic pulses • Left apical heave on precordial palpation
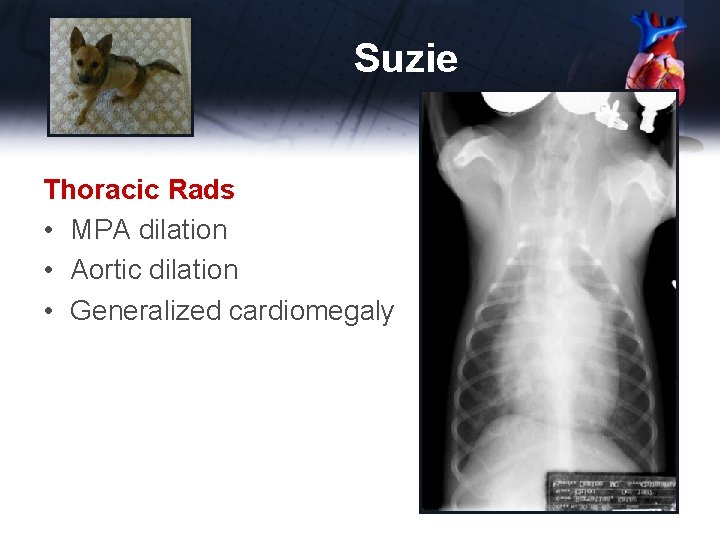
Suzie Thoracic Rads • MPA dilation • Aortic dilation • Generalized cardiomegaly
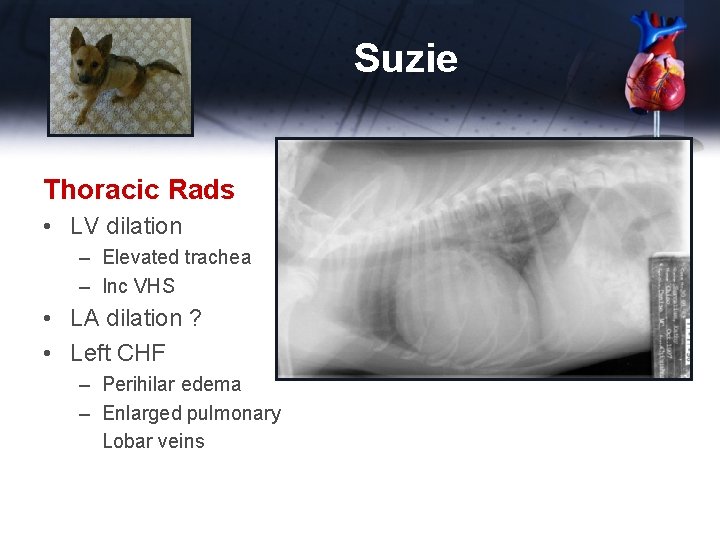
Suzie Thoracic Rads • LV dilation – Elevated trachea – Inc VHS • LA dilation ? • Left CHF – Perihilar edema – Enlarged pulmonary Lobar veins

Suzie Treatment • Furosemide 12. 5 mg PO BID • Enalapril 2. 5 mg PO BID • Pimobendan 1. 25 mg PO BID 2 week recheck • CHF controlled – resolution of edema

Suzie Echocardiogram • • IVSd 8. 0 (n. 6. 2 -7. 8) LVIDd 35. 1 (n. 21. 3 -25. 8) LVWd 7 (n. 5. 0 -6. 3) IVSs 11. 0 (n. 9. 4 -11. 2) LVIDs 15. 1 (n. 11. 9 -15. 2) IVDs 9. 3 (n. 8. 3 -10. 0) LAd 18 (n. 13. 4 -16. 1) Ao. S 14. 1 (n. 13. 5 -15. 5) • • LA: Ao – 1. 3 (n. 0. 8 -1. 3) FS = 57% MPA jet dilation Can see PDA at transverse MPA view Eccentric hypertrophy LV overload, CHF controlled No Myocardial failure Dx - PDA
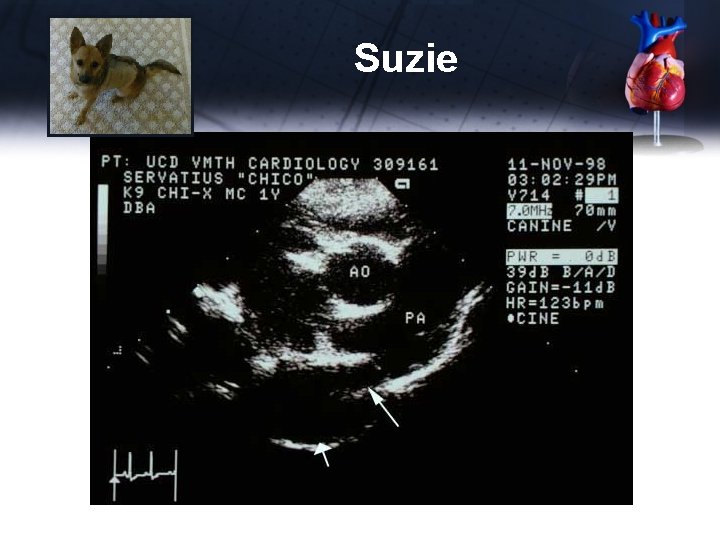
Suzie

Patent Ductus Arteriosus Echocardiographic Features • Can see PDA at transverse MPA view • Doppler can find PDAs that aren’t easily visualized • FS hyperdynamic unless myocardial failure

Suzie Treatment • Surgical ligation

Suzie 2 week recheck • CHF controlled – weaned off meds • Still doing well 60 days later • But…. Murmur returned – left axillary area (audio) • No mitral murmur Treatment • Cath procedure for coil placement
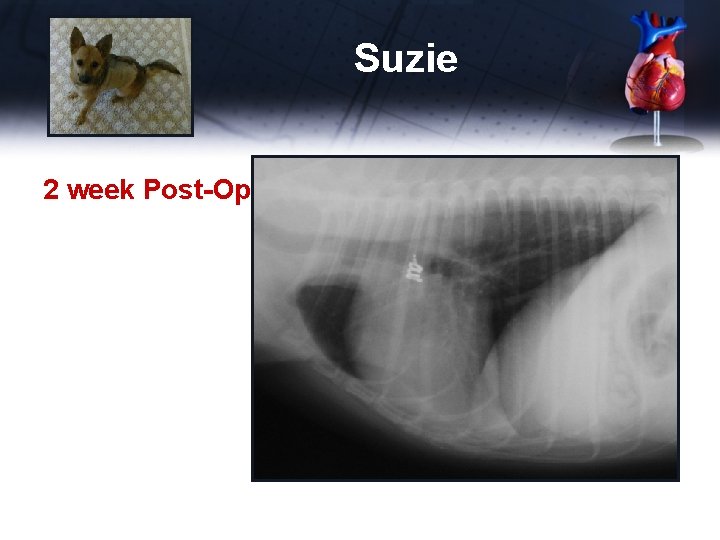
Suzie 2 week Post-Op Rads
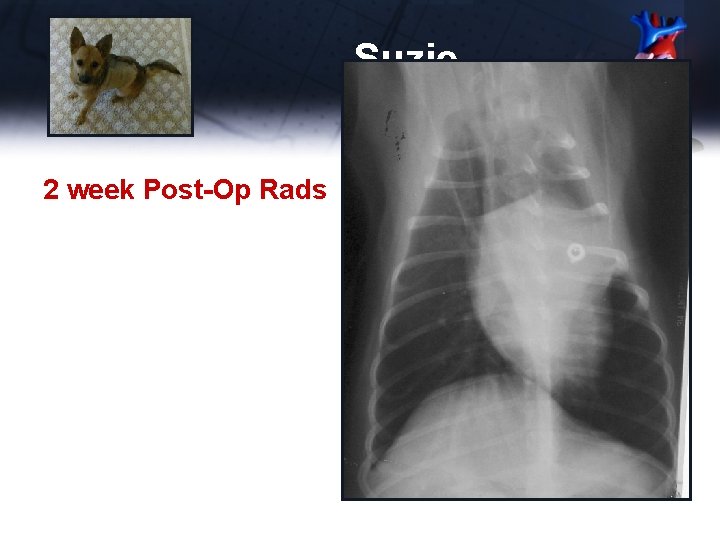
Suzie 2 week Post-Op Rads
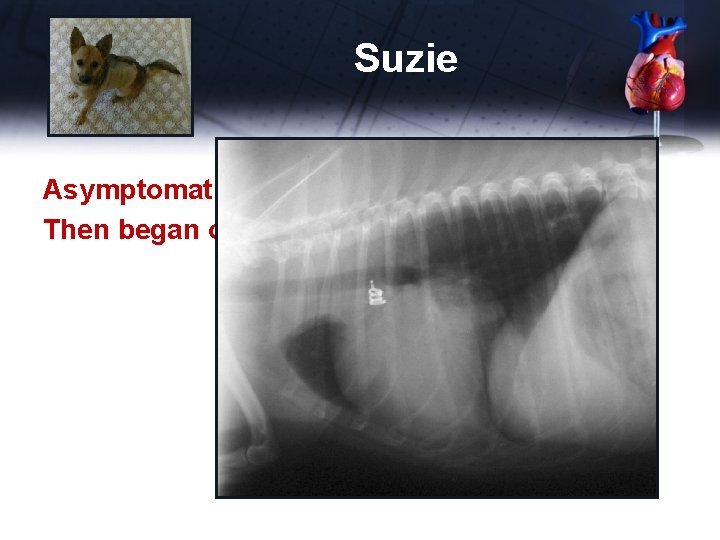
Suzie Asymptomatic for 8 yrs Then began coughing
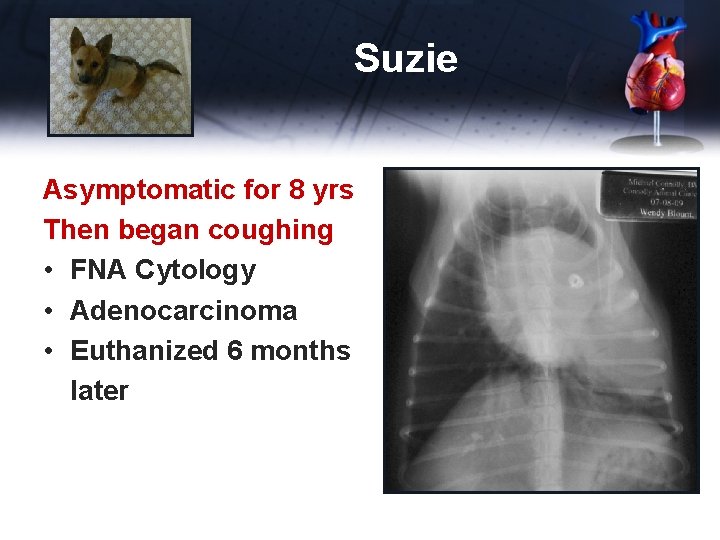
Suzie Asymptomatic for 8 yrs Then began coughing • FNA Cytology • Adenocarcinoma • Euthanized 6 months later

Sub-Aortic Stenosis Clinical Features • Large breeds more common than small • Valvular and supravalvular stenosis very rare • Does not lend itself to balloon valvuloplasty • Patch grafts are being tried at TAMU • Anatomic expression may not occur until several weeks to months old • Disease can be progressive or regressive

Sub-Aortic Stenosis Clinical Features • Doppler is required to determine severity • Prognosis depends on severity – Mild – 0 -50 mm Hg – Moderate – 50 -100 mm Hg – Severe - >100 mm Hg

Sub-Aortic Stenosis Echocardiographic Features • LV (IVS and LVPW) thickening • An echodense ridge or band may be seen on the long LVOT view, especially if severe • Aortic valve may be abnormal – – Thickened (rare) Decreased movement (rare) Delay in opening of AV after systole Excessive systolic fluttering

Sub-Aortic Stenosis Echocardiographic Features • Doppler can identify those SAS which can not be visualized directly • FS usually normal to slightly increased (Video 1) Shiloh-Lion (Video 2) Shiloh-Lion

Sub-Aortic Stenosis Treatment • Treat arrhythmia if present – Atenolol 0. 5 mg/kg PO BID • Treat left heart failure if present • Treat aortic regurgitation if present – Hydralazine 0. 5 mg/kg PO BID – Titrate up to 2 mg/kg PO BID to reduce systolic BP by 10 -20 mm Hg
Sub-Aortic Stenosis Treatment • Treat arrhythmia if present – Atenolol 0. 5 mg/kg PO BID • Treat left heart failure if present • Treat aortic regurgitation if present – Hydralazine 0. 5 mg/kg PO BID – Titrate up to 2 mg/kg PO BID to reduce systolic BP by 10 -20 mm Hg
Sub-Aortic Stenosis Treatment • Treat arrhythmia if present – Atenolol 0. 5 mg/kg PO BID • Treat left heart failure if present • Treat aortic regurgitation if present – Hydralazine 0. 5 mg/kg PO BID – Titrate up to 2 mg/kg PO BID to reduce systolic BP by 10 -20 mm Hg
Sub-Aortic Stenosis Treatment • Treat arrhythmia if present – Atenolol 0. 5 mg/kg PO BID • Treat left heart failure if present • Treat aortic regurgitation if present – Hydralazine 0. 5 mg/kg PO BID – Titrate up to 2 mg/kg PO BID to reduce systolic BP by 10 -20 mm Hg
Sub-Aortic Stenosis Treatment • Treat arrhythmia if present – Atenolol 0. 5 mg/kg PO BID • Treat left heart failure if present • Treat aortic regurgitation if present – Hydralazine 0. 5 mg/kg PO BID – Titrate up to 2 mg/kg PO BID to reduce systolic BP by 10 -20 mm Hg

ASD and VSD Clinical Features • Disease is a result of left to right shunting • This causes pulmonary hypertension and right heart failure – – – caudal caval distension, hepatic vein distension jugular vein distension/pulses/reflux Ascites Pericardial effusion Pleural effusion

ASD and VSD Echocardiographic Features - VSD • In dogs and cats, most VSDs occur in membranous IVS, at the top of the LV near the atria • Need to be 1 cm to reliably seen on echo • Doppler can find those that can not be seen directly • May see abnormal septal motion due to conduction interruption • Occasionally can see right cusp of AV prolapsing, creating aortic regurgitation • Huge RA and MPA; RV dilation

ASD and VSD Echocardiographic Features - ASD • ASD much less likely to cause clinical signs than VSD • Do not confuse with drop-out of fossa ovalis • Doppler can confirm • If large enough, may see right volume overload – Enlarged RA and RV – Enlarged MPA

Summary • Power. Point – Cases – Congenital Heart Defects • . pdf of Power. Point – Cases - Congenital Heart Defects • Client Handouts – – PDA Subaortic Stenosis Pulmonic Stenosis VSD
- Slides: 67