Practical Blood Bank Lab 7 Antibody Identification Antibody

Practical Blood Bank Lab 7 Antibody Identification

Antibody Presence of an antibody may be indicated by the following serological tests: 1. A discrepancy in the results of cell and serum ABH grouping. 2. A positive test for unexpected antibodies. 3. A positive direct Coomb’s test. 4. An incompatible major cross match.

The Basics…. . n As we said in the previous lecture, q q Antibody Screens use 2 or 3 Screening Cells to “detect” if antibodies are present in the serum If antibodies are detected, then they should be identified…

Why do we need to identify? n n n Antibody identification is an important component of compatibility testing It will identify any unexpected antibodies in the patient’s serum If a person with an antibody is exposed to donor cells with the corresponding antigen, serious side effects can occur (i. e. transfusion reactions).

Key Concepts n In blood banking, we test “knowns” with “unknowns”: Known: Reagent RBCs + Reagent antisera + n Unknown: patient serum patient RBCs When detecting/screening and/or identifying antibodies, we test patient serum (unknown that contain blood bank antibodies) with reagent RBCs (known)

Reagent RBCs n Screening Red Cells and Panel Red Cells are the same with minor differences: q Screening red cells n n q Antibody detection/screening Sets of only 2 or 3 vials Panel red cells n n Antibody identification At least 10 vials/set
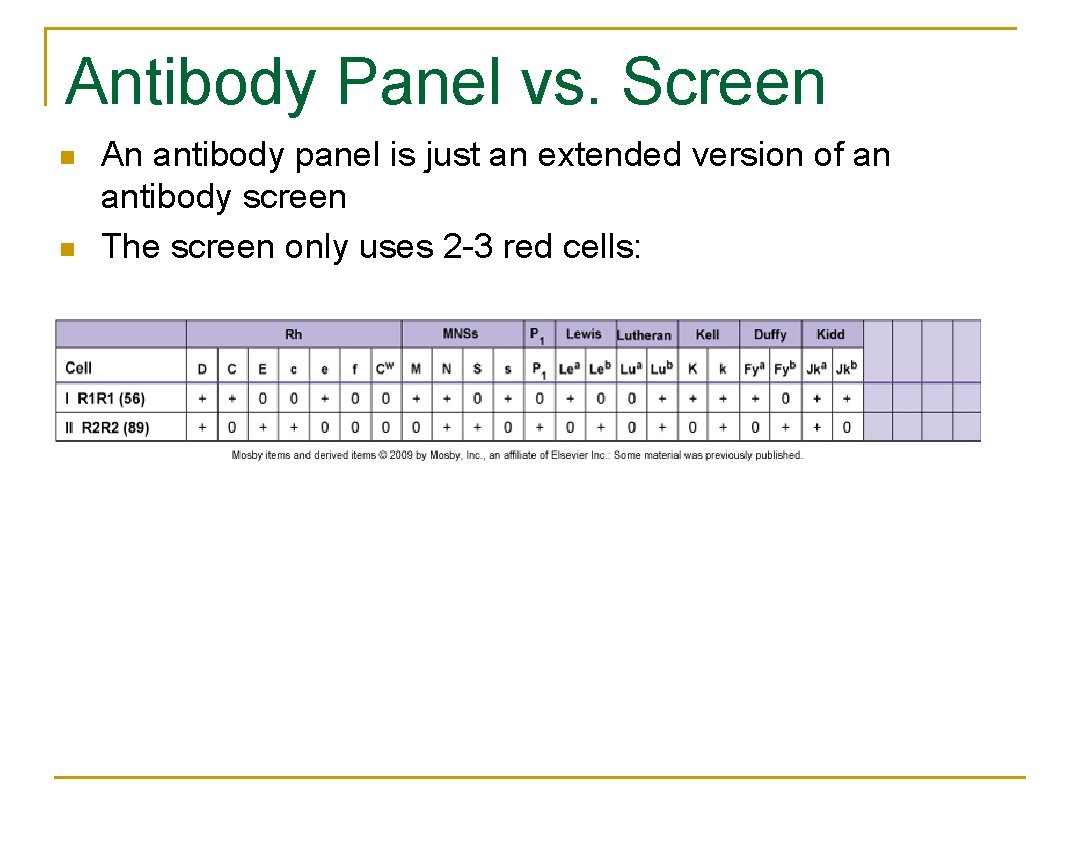
Antibody Panel vs. Screen n n An antibody panel is just an extended version of an antibody screen The screen only uses 2 3 red cells:
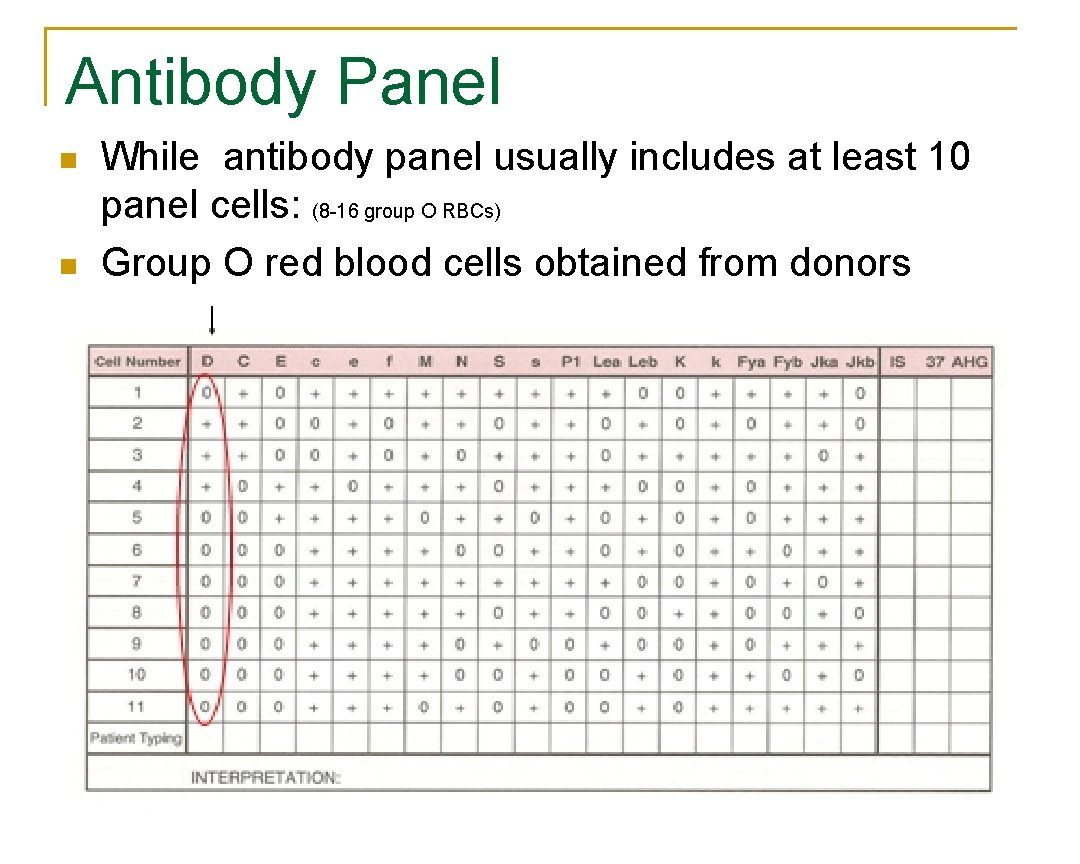
Antibody Panel n n While antibody panel usually includes at least 10 panel cells: (8 16 group O RBCs) Group O red blood cells obtained from donors
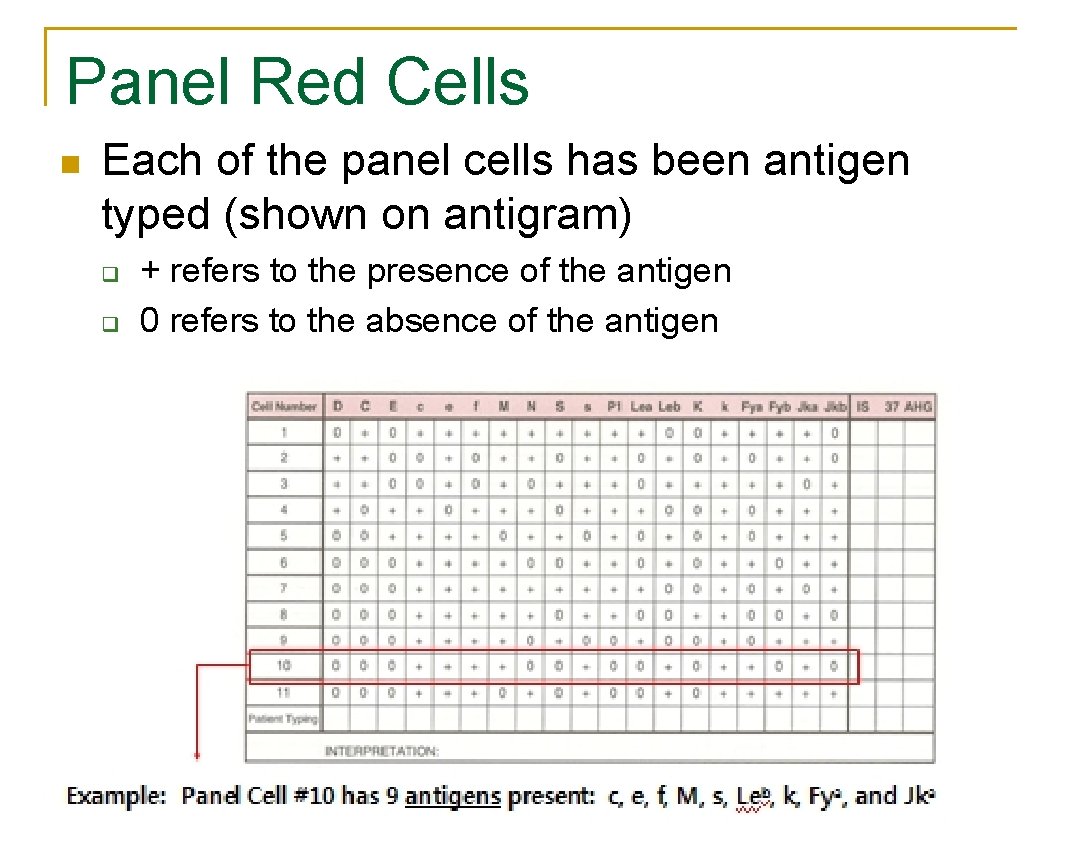
Panel Red Cells n Each of the panel cells has been antigen typed (shown on antigram) q q + refers to the presence of the antigen 0 refers to the absence of the antigen

Panel Red Cells n An autocontrol (AC) should also be run with panels
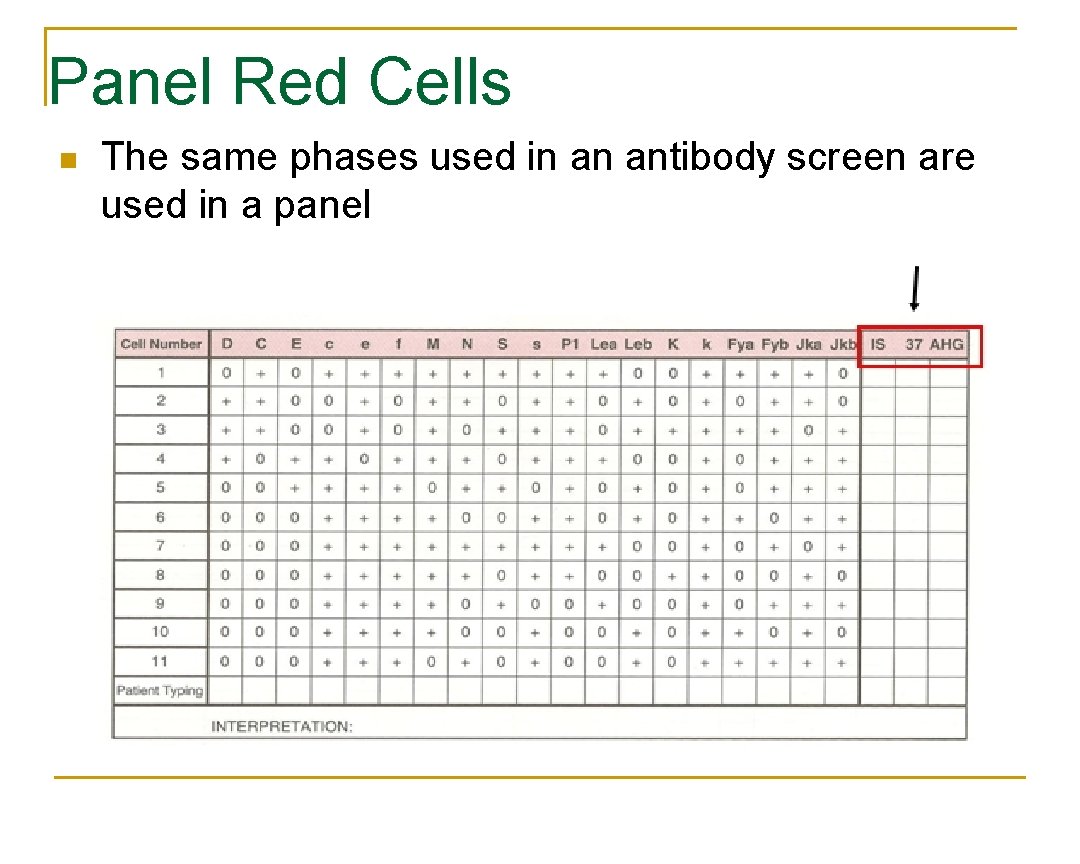
Panel Red Cells n The same phases used in an antibody screen are used in a panel
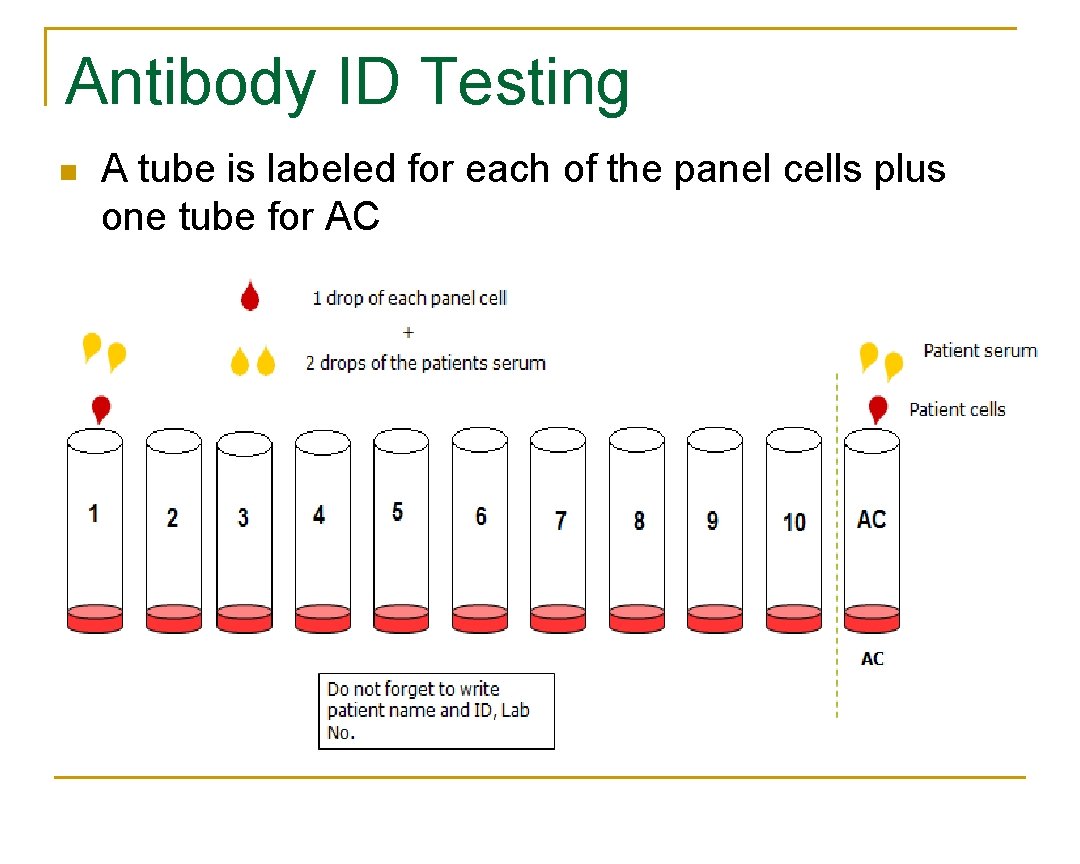
Antibody ID Testing n A tube is labeled for each of the panel cells plus one tube for AC

IS Phase n n Perform immediate spin (IS) and grade agglutination; inspect for hemolysis Record the results in the appropriate space as shown.

(LISS) 37°C Phase n n n 2 drops of LISS are added, mixed and incubated for 10 15 minutes. Centrifuge and check for agglutination Record results as previous but now fill the 37°C lane. Agglutination Viewer
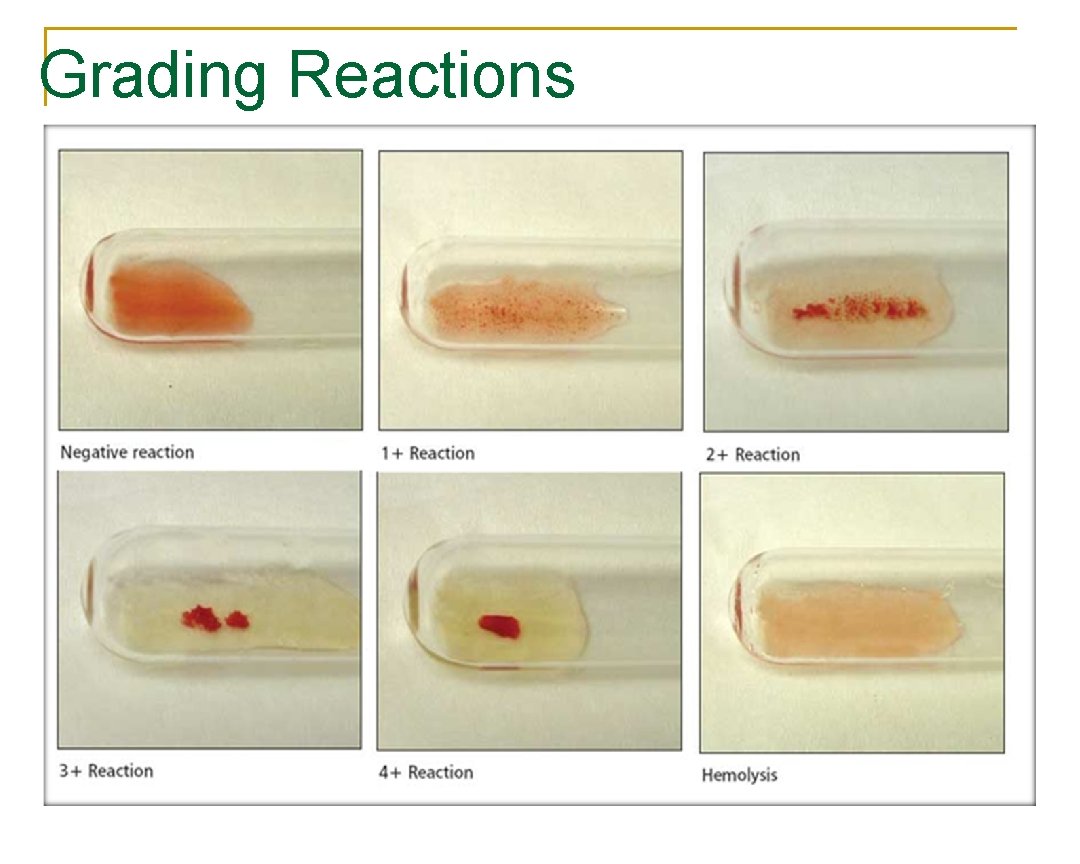
Grading Reactions
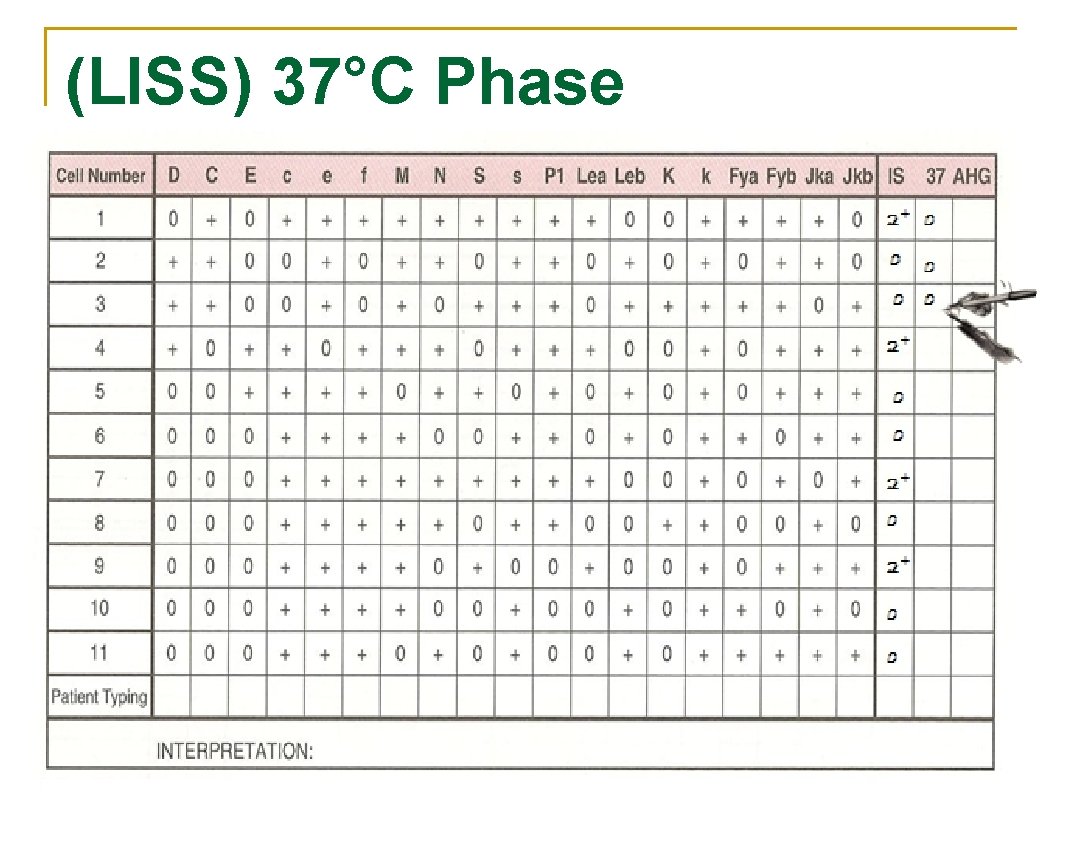

(LISS) 37°C Phase

IAT Phase (or AHG) n n Indirect Antiglobulin Test (IAT) – we’re testing whether or not possible antibodies in patient’s serum will react with RBCs in vitro To do this we use the Anti Human Globulin reagent (AHG) q q q Polyspecific AHG Monospecific Anti Ig. G Monospecific Anti Complement

IAT (AHG) Phase n n Wash red cells 3 X with saline (manual or automated (cell washer)) Add 2 drops of AHG and gently mix q q q Centrifuge Read for agglutination Record reactions
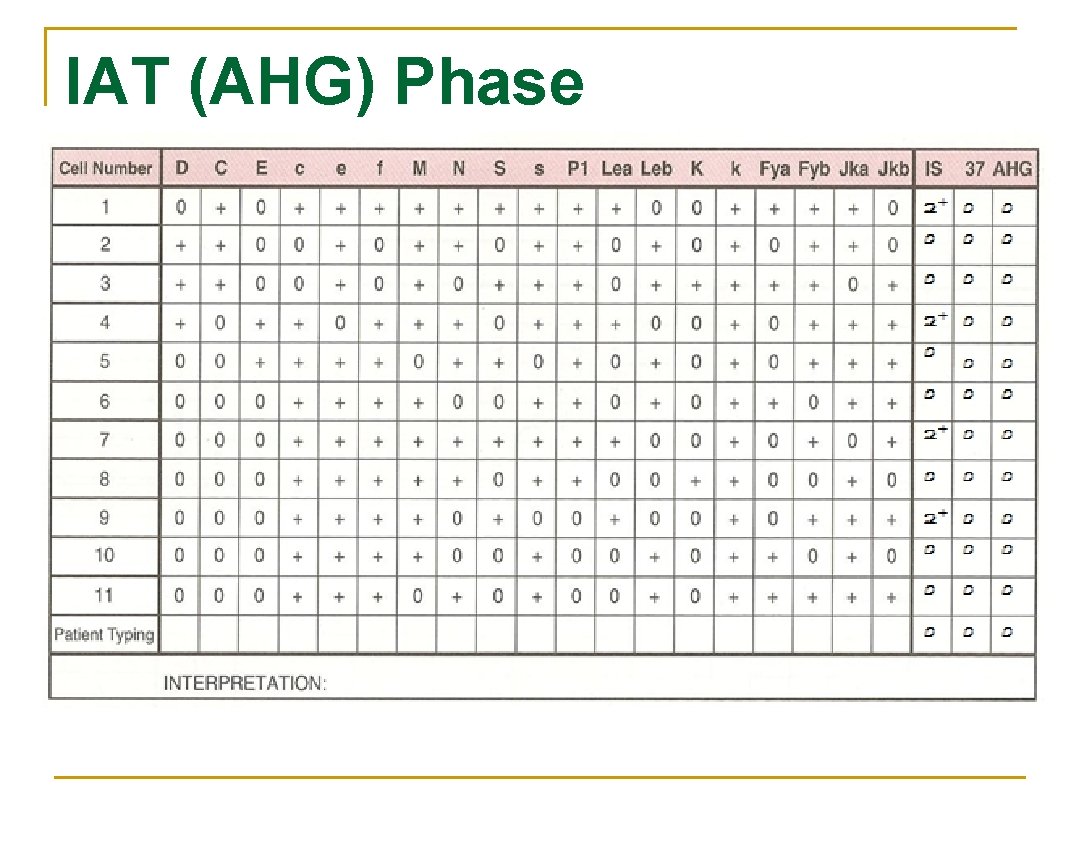
IAT (AHG) Phase

And don’t forget…. …. add “check” cells to any negative AHG !
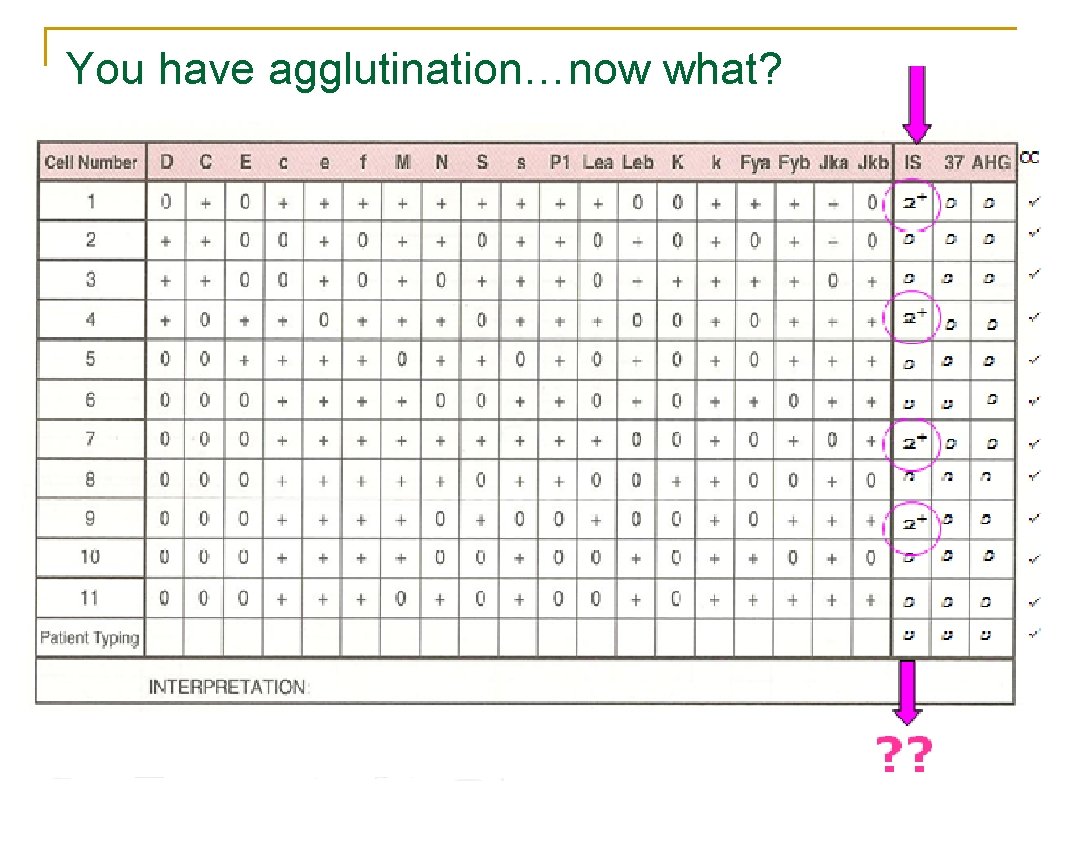

You have agglutination…now what?

Guidelines n Again, it’s important to look at: q Autocontrol n n q Phases n n n q IS – cold (Ig. M) 37° cold (some have higher thermal range) or warm reacting AHG – warm (Ig. G)…significant!! Reaction strength n n n Negative alloantibody Positive – autoantibody or DTR (i. e. alloantibodies) 1 consistent strength – one antibody Different strengths – multiple antibodies or dosage Matching the pattern q q Single antibodies usually shows a pattern that matches one of the Multiple antibodies are more difficult to match because they often show mixed reaction strengths
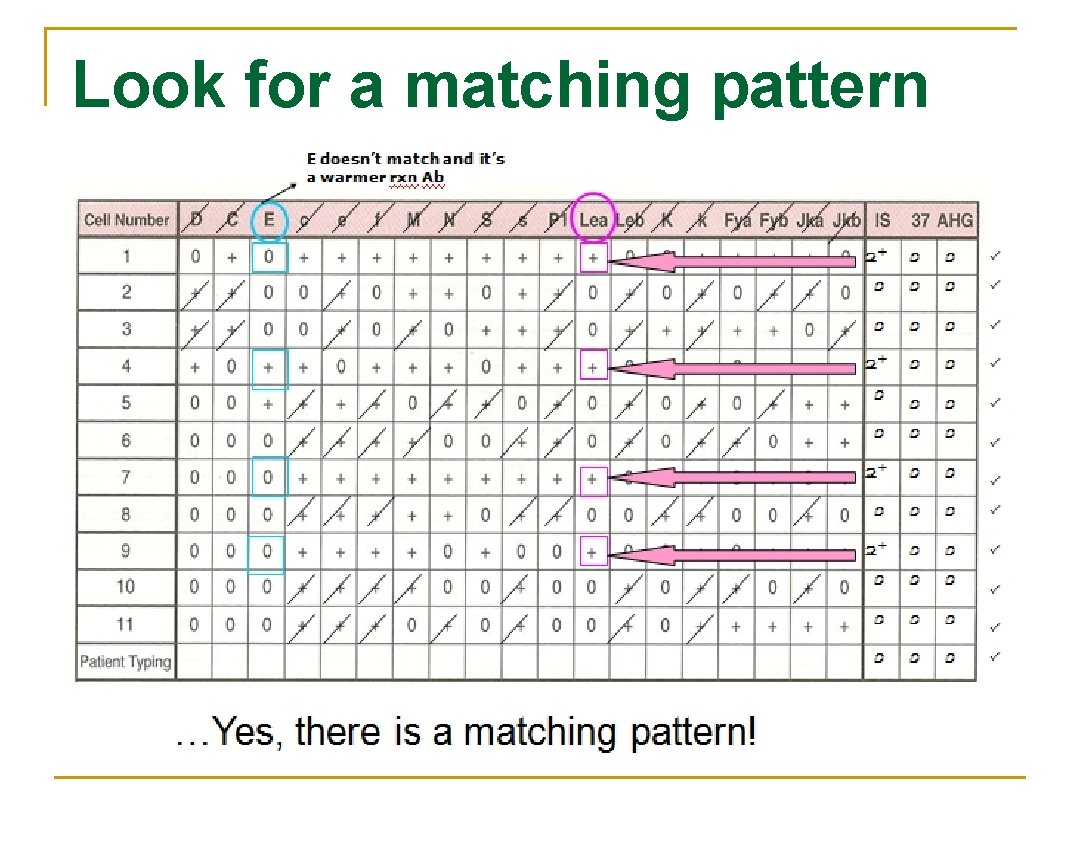
Look for a matching pattern

Rule of three n The rule of three must be met to confirm the presence of the antibody q How is it demonstrated? n Patient serum MUST be: q Positive with 3 panel cells with the antigen, +ve reaction. q Negative with 3 cells without the antigen and should not be reacting.
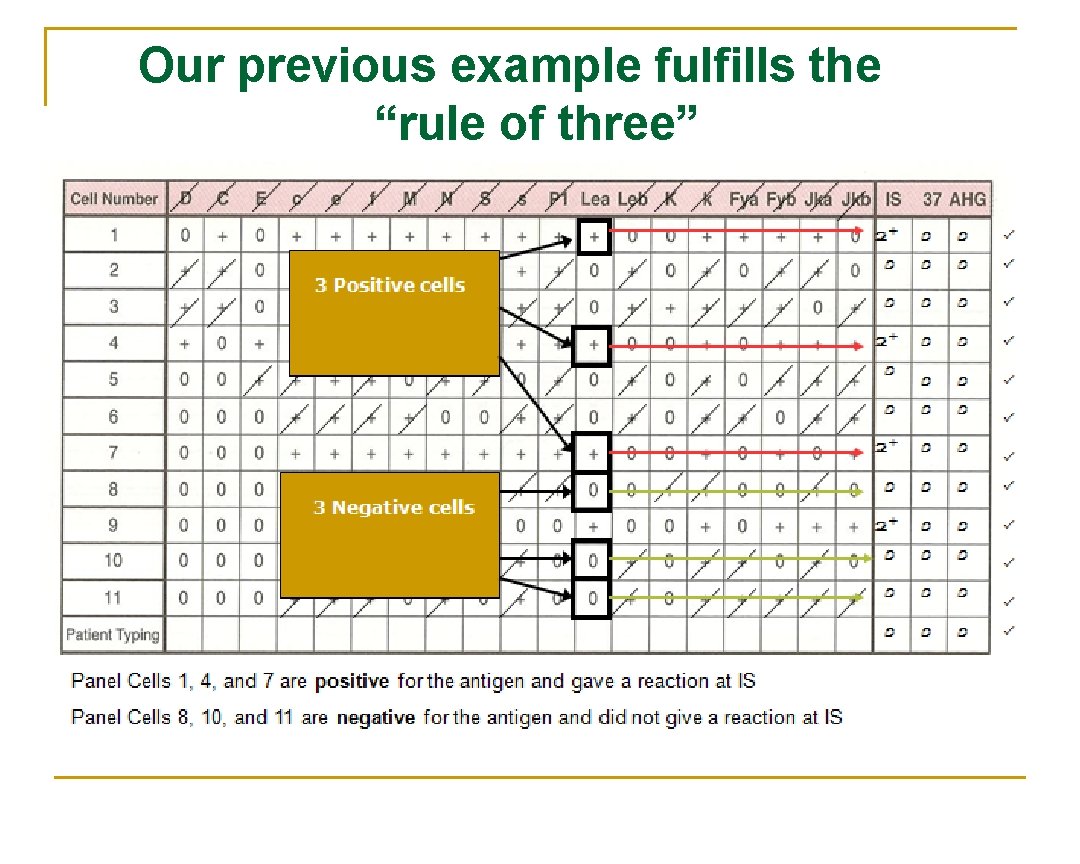
Our previous example fulfills the “rule of three”

What if the “rule of three” is not fulfilled? n n If there are not enough cells in the panel to fulfill the rule, then additional cells from another panel could be used Better to carry different lot numbers of panel cells

Patient Antigen Typing (Phenotyping) n n In addition to the rule of three, antigen typing the patient red cells can also confirm an antibody How is this done? q q Only perform this if the patient has NOT been recently transfused (donor cells could react (chimera)). If reagent antisera (of the suspected antibody) is added to the patient RBCs, a negative reaction should result…Why?

Remember Landsteiner’s Rule Individuals DO NOT make allo-antibodies against antigens they have

Multiple antibodies n n Multiple antibodies may be more of a challenge than a single antibody Why? q q Reaction strengths can vary Matching the pattern is difficult

So what we have to do? n Several procedures can be performed to identify multiple antibodies q q q Selected Cells Neutralization Chemical treatment n n Proteolytic enzymes Sulfhydryl reagents

1 - Selected Red Cells n n n Selected cells are chosen from other panel or screening cells to confirm or eliminate the antibody. The cells are “selected” from other panels because of their characteristics. The number of selected cells needed depends on how may antibodies are identified. Every cell should be positive only for each of the antibodies and negative for the remaining suspicious antibodies For example: q Let’s say you ran a panel and identified 3 different antibodies (you cannot rule out): anti-S, anti-Jka, and anti-P 1 q Selected cells could help…
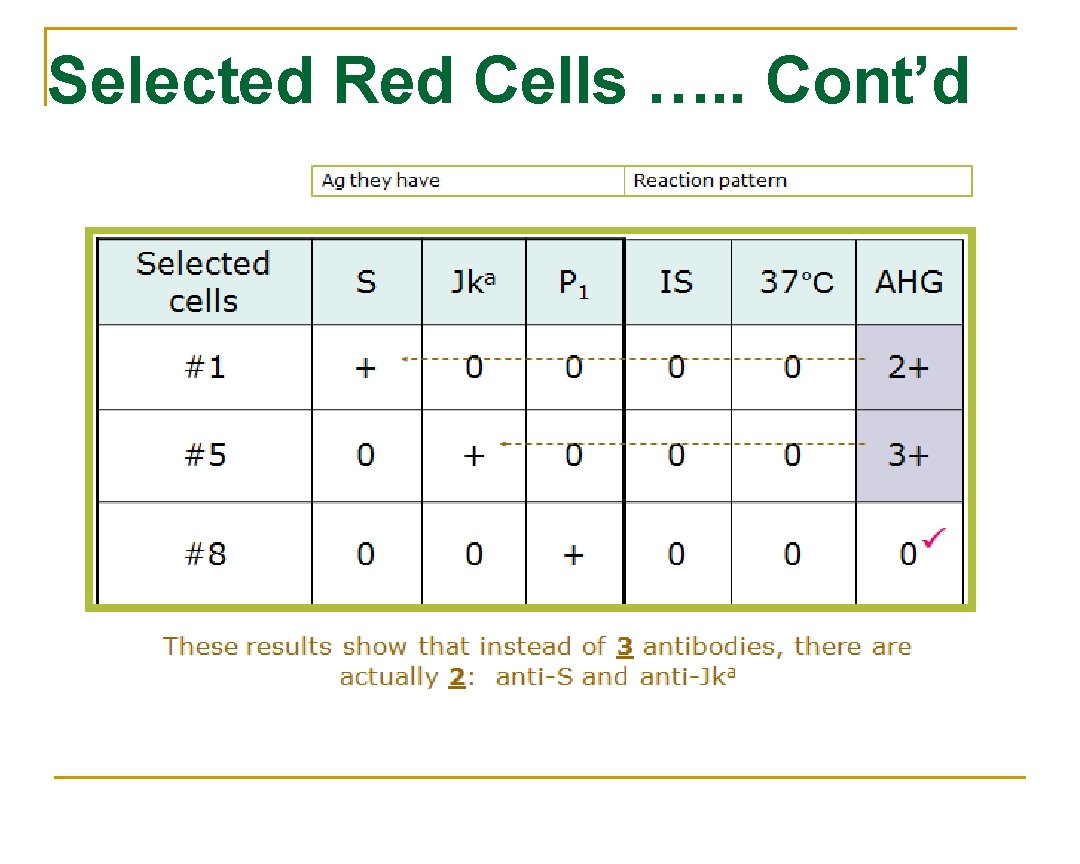
Selected Red Cells …. . Cont’d

2 - Neutralization n Some antibodies may be neutralized as a way of confirmation Commercial “substances” bind to the antibodies in the patient serum, causing them to show no reaction when tested with the corresponding antigen (in panel) Common substances q q q P 1 substance (derived from hydatid cyst fluid) Lea and Leb substance (soluble antigen found in plasma and saliva) I substance can be found in breast milk **you should be aware that many of these substances neutralize COLD antibodies; Cold antibodies can sometimes mask more clinically significant antibodies (Ig. G), an important reason to use neutralization techniques

3 - Again: Proteolytic Enzymes n n Can be used to enhance or destroy certain blood group antigens Several enzymes exist: q q q n Ficin (figs) Bromelin (pineapple) Papain (papaya) In addition, enzyme procedures may be q q One step Two step

Enzymes n Enzymes remove the sialic acid from the RBC membrane, thus “destroying” it and allowing other antigens to be “enhanced” q q Antigens destroyed: M, N, S, s, Duffy Antigens enhanced: Rh, Kidd, Lewis, I, and P n One stage q Enzyme is added directly to the serum/panel cell mixture n Two stage q Panel cells are pre treated with an enzyme, and washed q Patient serum is added to treated panel cells and tested n If there is no agglutination after treatment, then it is assumed the enzymes destroyed the antigen

Sulfhydryl Reagents n n Cleave the disulfide bonds of Ig. M molecules and help differentiate between Ig. M and Ig. G antibodies Good to use when you have both Ig. G and Ig. M antibodies (warm/cold) q q Dithiothreitol (DTT) is a thiol and will denature Kell antigens 2 mercaptoethanol (2 ME)

Autoantibodies…. Warm & Cold Reacting

Autoantibodies n Autoantibodies can be cold or warm reacting n A positive autocontrol or DAT may indicate that an auto antibody is present n Sometimes the autocontrol may be positive, but the antibody screening may be negative, meaning something is coating the RBC

Getting a positive DAT n We have focused a lot on the IAT used in antibody screening and ID, but what about the DAT? n The direct antiglobulin test (DAT) tests for the in vivo coating of RBCs with antibody (in the body) n AHG is added to washed patient red cells to determine this

What can the DAT tell us? n Although not always performed in routine pretransfusion testing, a positive DAT can offer valuable information q q If the patient has been transfused, the patient may have an alloantibody coating the transfused cells If the patient has NOT been transfused, the patient may have an autoantibody coating their own cells

Identifying autoantibodies Auto antibodies can sometimes “mask” clinically significant allo antibodies, so it’s important to differentiate between auto and allo antibodies

Cold autoantibodies n n n React at room temperature with most (if not all) of the panel cells and give a positive autocontrol The DAT is usually positive with anti-C 3 AHG (detects complement) Could be due to Mycoplasma pneumoniae, infectious mono, or cold agglutinin disease

Avoiding reactivity n Cold Autoantibodies can be a trouble at times. Here a few ways to avoid a reaction: q q q Use anti Ig. G AHG instead of polyspecific. Most cold antibodies react with polyspecific AHG because they fix complement Skipping the IS phase avoids the attachment of cold autoantibodies to the red cells Use 22% BSA instead of LISS

Other techniques n If the antibodies remain, then prewarmed techniques can be performed: q n Red cells, serum, and saline are incubated at 37° before being combined Autoadsorption is another technique in which the autoantibody is removed from the patients serum using their own red cells The serum can be used to identify any underlying alloantibodies

Warm autoantibodies n n n More common that cold autoantibodies Positive DAT due to Ig. G antibodies coating the red cell Again, the majority of panel or screening cells will be positive

Warm autoantibodies n n Cause warm autoimmune hemolytic anemia (WAIHA)… How do you get a warm autoantibody? q q q n Idiopathic Known disorder (SLE, RA, leukemias, pregnancy, infectious diseases, etc) Medications Several techniques are used when warm autoantibodies are suspected…
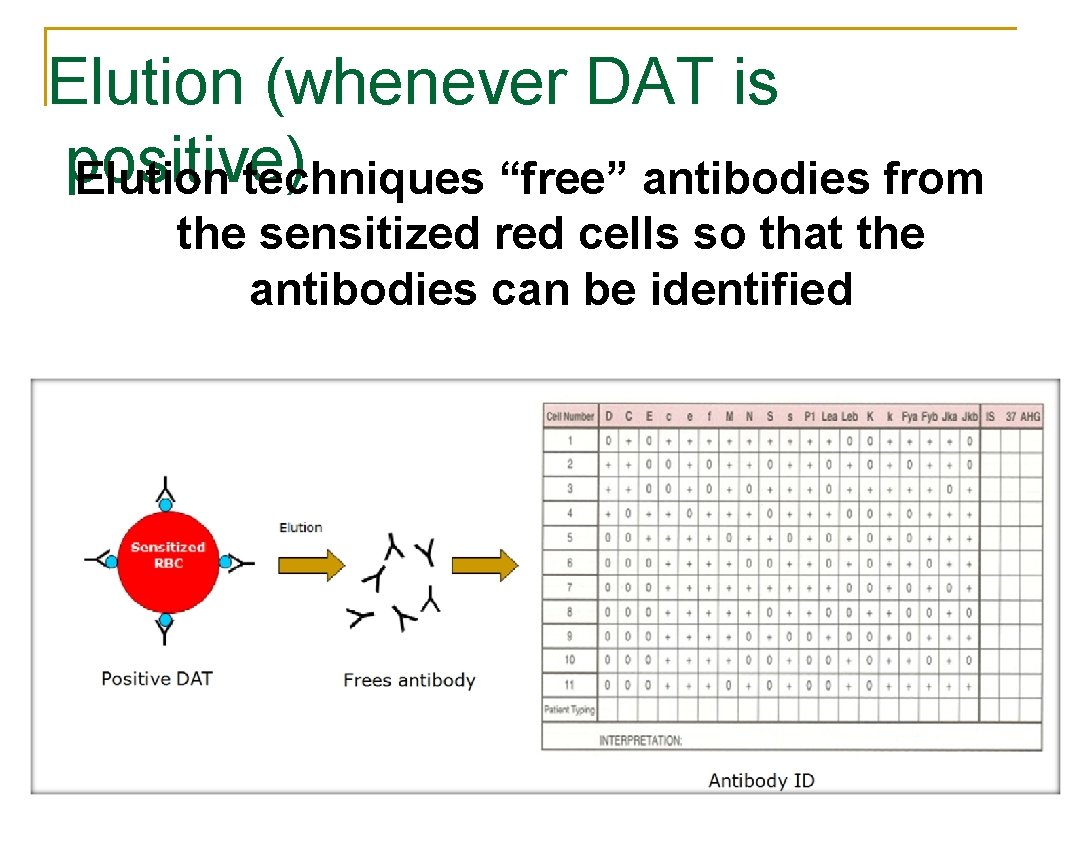
Elution (whenever DAT is positive) Elution techniques “free” antibodies from the sensitized red cells so that the antibodies can be identified

Elution n n The eluate is a term used for the removed antibodies Testing the eluate is useful in investigations of positive DATs q q q n n HDN Transfusion reactions Autoimmune disease The red cells can also be used after elution for RBC phenotyping if needed When tested with panel cells, the eluate usually remains reactive with all cells if a warm autoantibody is present

Elution Methods n Acid elutions (glycine acid) q q n Organic solvents (ether, chloroform) q n n Most common Lowers p. H, causing antibody to dissociate Dissolve bilipid layer of RBC Heat (conformational change) Freeze Thaw (lyses cells)

Adsorption n n Adsorption procedures can be used to investigate underlying alloantibodies After the patient RBCs are incubated, the adsorbed serum is tested with panel cells to ID the alloantibody (if present)

Adsorption n Two types: q Autoadsorption n n q No recent transfusion Autoantibodies are removed using patient RBCs, so alloantibodies can be identified Allogenic (Differential) adsorption n n If recently transfused Uses other cells with the patients serum


Summary n n If an unexpected antibody is detected in a patient’s serum or plasma it must be identified. Once identified the clinical significance must be determined.

Summary n n If the antibody is clinically significant antigen negative donors must be found and crossmatched for the patient, a Coomb’s crossmatch must be done. If the antibody is not clinically significant it is not necessary to provide antigen negative blood, but the donors must be compatible by the Coomb’s crossmatch.

Providing Compatible Donor Units n Once an antibody has been identified, the next task is to provide appropriate units of RBCs for transfusion. n When clinically insignificant antibodies are detected, use of crossmatch compatible RBCs is appropriate.

Providing Compatible Donor No further testing is needed to confirm compatibility when Units the antibody is anti M, anti N, anti Pi. Le , or Le. n a n b However, when a clinically significant antibody is identified, the blood must be cross match compatible and confirmed as antigen negative with reagent antisera.

Example n n Knowledge of the incidence of antigens is useful for determining how many units of blood to screen or cross match for patients with antibodies. If a patient with an anti Jk(a ) needed 4 units of blood, how many units would need to be tested to find them? Jk (a+)= 0. 77 Jk (a ) = 0. 23 4 units Jk(a ) blood needed = 17. 4 units 0. 23 incidence of Jk(a ) In this case, testing 17 or 18 random units should yield 4 Jk(a ) units.

Example 2 n n The same calculations can be used when multiple antibodies are present if the antigen frequencies are first multiplied together. E. g. a patient with an anti K and anti Jka, 10 random units would need to be tested to find 2 that are compatible. Jk(a+) = 0. 77 K positive = 0. 09 Jk(a ) = 0. 23 K negative = 0. 91 Jk(a ) (0. 23) X K negative (0. 91) = 0. 20 Jk(a ) and K negative 2 units needed = 10 units 0. 20 Jk(a ) and Kell negative

h T k n a u o y
- Slides: 59