Practical Blood Bank Lab 2 ABO Discrepancies ABO

Practical Blood Bank Lab 2 ABO Discrepancies

ABO Discrepancy n n When the results of the forward grouping (patient cells) is not matching the results of the reverse grouping (patient serum) or abnormal reactivity is present (i. e. Mixed Field) then we called this ABO discrepancy. The Discrepancy will be noticed by: q Strength of reaction n q q Weak or missing. Additional reactions Abnormal reactions

HINT n ABO forward and reverse reactions are typically very strong: 3+ to 4+. Weaker reactions should immediately send up red flags indicating that something is wrong. n Since production of ABO antigens is genetically controlled they are less vulnerable to problems than does the production of ABO antibodies. Therefore we see more problems in which grouping: Forward or Reverse?
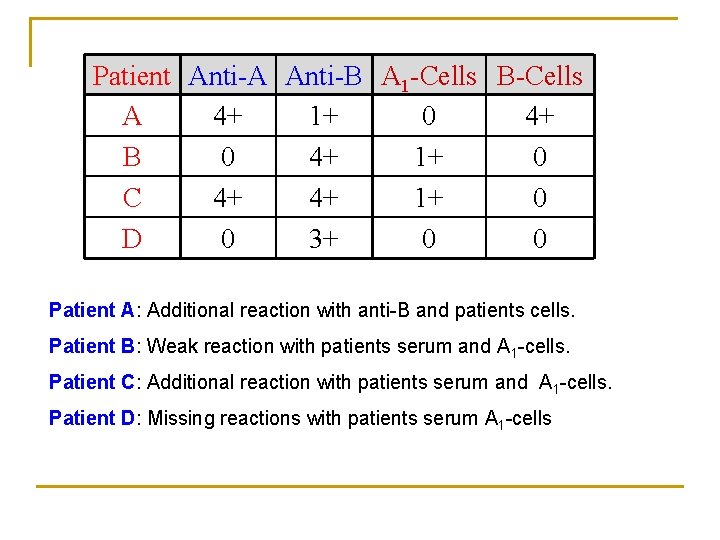
Patient Anti-A Anti-B A 1 -Cells B-Cells A 4+ 1+ 0 4+ B 0 4+ 1+ 0 C 4+ 4+ 1+ 0 D 0 3+ 0 0 Patient A: Additional reaction with anti-B and patients cells. Patient B: Weak reaction with patients serum and A 1 -cells. Patient C: Additional reaction with patients serum and A 1 -cells. Patient D: Missing reactions with patients serum A 1 -cells

n i p u o r G d r a w r Fo s m e l b o r P g
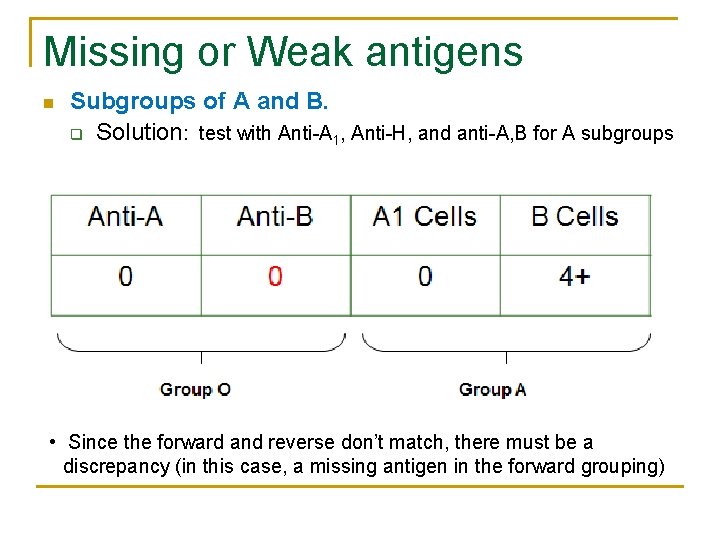

Missing or Weak antigens n Subgroups of A and B. q Solution: test with Anti-A 1, Anti-H, and anti-A, B for A subgroups • Since the forward and reverse don’t match, there must be a discrepancy (in this case, a missing antigen in the forward grouping)

Extra Antigens n n n Acquired B B(A) phenotype Rouleaux Polyagglutination Wharton’s Jelly Anti-A Anti-B 4+ 1+ A 1 Cells 0 EXAMPLE B Cells 4+

Solutions: n Acquired B q q q n B(A) phenotype q n n Check patient diagnosis: Infection? Some manufacturers produce anti-B reagent that does not react with acquired B Test patients serum with their own RBCs n The patients own anti-B will not react with the acquired B antigen on their red cell (autologous testing) Test with another anti-A reagent from another manufacturer Polyagglutination, Rouleaux, Wharton’s Jelly q Wash red cells or request new sample from heel, etc
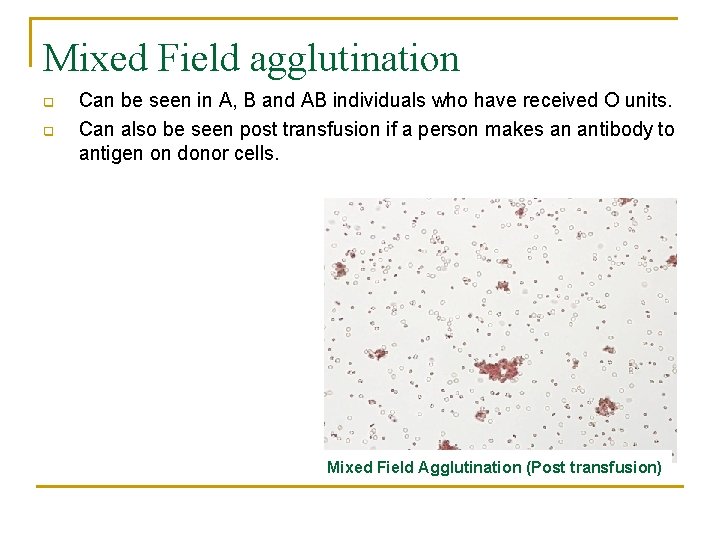
Mixed Field agglutination q q Can be seen in A, B and AB individuals who have received O units. Can also be seen post transfusion if a person makes an antibody to antigen on donor cells. Mixed Field Agglutination (Post transfusion)

n i p u o r G e s r e v Re s m e l b o r P g

Unexpectedly Weakened Antibodies Immunodeficient due to therapy or disease q q Immunosuppressive drugs Certain leukemia’s (CLL) or lymphoma’s (malignant lymphomas) have hypogammaglobulinemia (Little or no antibody production) Age related q Very young: <6 months of age (Newborns) q Very old: >65 years of age (Weakened Abs Activity) Dilutional Effect q Plasma Exchange, Transfusion, etc. dilutes out patient antibodies

Resolving Weak or Missing antibodies n Determine patients age, diagnosis n n Incubate serum testing for 15 minutes (RT) to enhance antibody reactions If negative, place serum testing at 4°C for 5 minutes with autologous control (a. k. a. Autocontrol, AC) q This is called a “mini-cold” panel and should enhance the reactivity of the antibodies

Extra Antibodies n n n Cold antibodies (allo- or auto-) q Cold antibodies may include anti-I, H, M, N, P, Lewis q The autocontrol will be positive. q Resolution: warming tube to 37° and washing red cells can disperse agglutination; breaking the Ig. M bonds with 2 -ME will also disperse cells Rouleaux q Stronger at IS and weak reaction at 37° C and no agglutination at AHG phase q Solutions Anti-A 1 in an A 2 or A 2 B individual

Resolving Rouleaux n If the forward grouping is affected, wash cells to remove protein and repeat test n If the reverse grouping is affected, perform saline replacement technique (more common) q q q Cells (reagent) and serum (patient) centrifuged to allow antigen and antibody to react (if present) Serum is removed and replaced by an equal volume of saline (saline disperses cells)* Tube is mixed, centrifuged, and reexamined for agglutination (macro and micro)

Anti-A 1 n n Sometimes A 2 (or A 2 B) individuals will develop an anti-A 1 antibody A 2 (or A 2 B) individuals have less antigen sites than A 1 individuals The antibody is a naturally occurring Ig. M Reacts with A 1 Cells, but not A 2 Cells

Resolving anti-A 1 discrepancy n 2 steps: q q q Typing patient RBCs with Anti-A 1 lectin Repeat reverse grouping with A 2 Cells instead of A 1 Cells Both results should yield NO agglutination Anti-A Anti-B 4+ 0 A 1 Cells 2+ B Cells 4+

Others… n n The Bombay phenotype (extremely RARE) results when hh is inherited These individuals do not have any antigens and naturally produce, anti-A, anti-B, anti-A, B, and anti-H Basically, NO forward reaction and POSITIVE reverse Resolution: test with anti-H lectin (Bombay’s don’t have H and will not react)

Popular LAB CAUSES Of ABO Discrepancies 1. 2. 3. 4. 5. 6. 7. Poorly labeled specimen OR test tubes Patient RBC suspension too heavy or light Wrong specimen put in Patient’s labeled test tubes Oh? Is hemolysis really a Pos. Rx’n? Wrong results recorded on Pt. Form Didn’t follow manufacturer’s instructions Poor centrifugation: over or under!

Popular LAB CAUSES Of ABO Discrepancies Didn’t add: 1. 2. 3. Patient Serum Reagents Correct Reagent Reaction Reading: 1. 2. 3. Shaking tubes while looking elsewhere Shaking tubes too hard Shaking tubes too gently or not completely resuspending cell button

ABO Discrepancy When an ABO Discrepancy is encountered: 1. 2. 3. Results must be recorded, but interpretation of the ABO group must be delayed until the discrepancy is resolved…by you! Begin follow up by getting an accurate patient history – age, medications, diagnosis, etc. Repeat testing to rule out tech errors such as mislabeling, adding reagents, wrong patient sample, etc.

Resolving ABO Discrepancies 1. Repeat testing on the sample… 2. Repeat testing using saline suspended and/or washed patient red blood cell’s. Saline Replacement. 1. From the beginning: re-label tubes, re-drop patient and reagent drops, etc. 1. Many labs make the patients red blood cell suspension with the patient’s serum/plasma. If the patient has increased plasma proteins it can cause non-specific red cell aggregation.

3. 4. Weak or missing reactions? Mislabeled or contaminated specimen: 3. 4. Incubate test system at room temperature for 1530 minutes! Get patient history. Redraw Patient!! a) ALL of the above: any labeling error may account for the problem and needs to be redrawn. b) Drawn above an IV?

5. Test patient cells with anti-A 1 (Dolichos biflorus), anti-A, B or anti-H (Ulex europaeus) 6. Test patient serum with A 1 or A 2 cells 5. For suspected subgroups of A 6. Ditto!

7. Review Antibody Screening tests 1. 8. 7. Can react with reagent A 1 and B cells 8. Should strengthen weakened ABO antibody reactivity! WHY? Allo antibody or cold reactive allo or auto Ab Incubate tests and controls for 10 -30 minutes room temperature
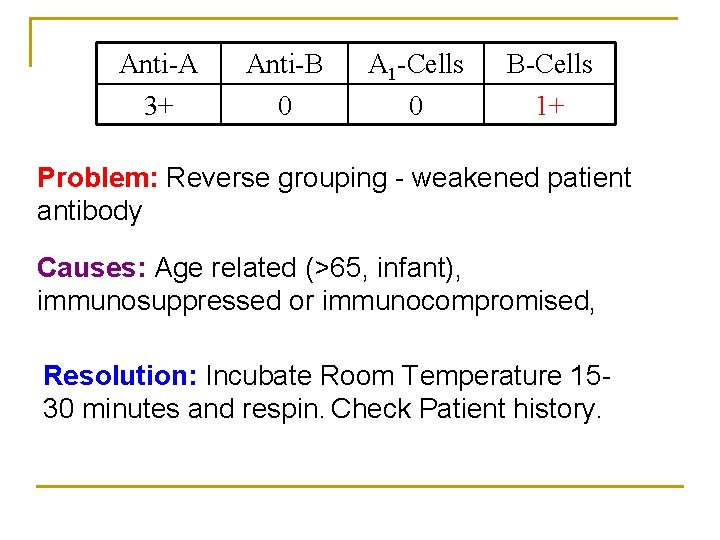
Anti-A 3+ Anti-B 0 A 1 -Cells 0 B-Cells 1+ Problem: Reverse grouping - weakened patient antibody Causes: Age related (>65, infant), immunosuppressed or immunocompromised, Resolution: Incubate Room Temperature 1530 minutes and respin. Check Patient history.
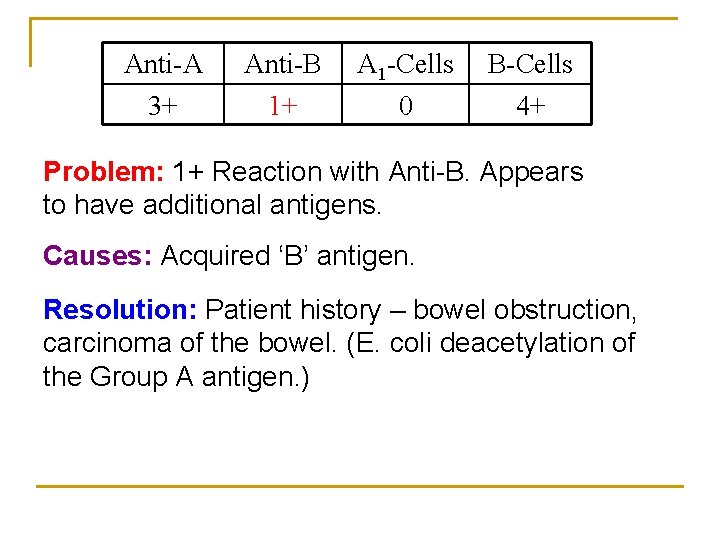

Anti-A 3+ Anti-B 1+ A 1 -Cells 0 B-Cells 4+ Problem: 1+ Reaction with Anti-B. Appears to have additional antigens. Causes: Acquired ‘B’ antigen. Resolution: Patient history – bowel obstruction, carcinoma of the bowel. (E. coli deacetylation of the Group A antigen. )
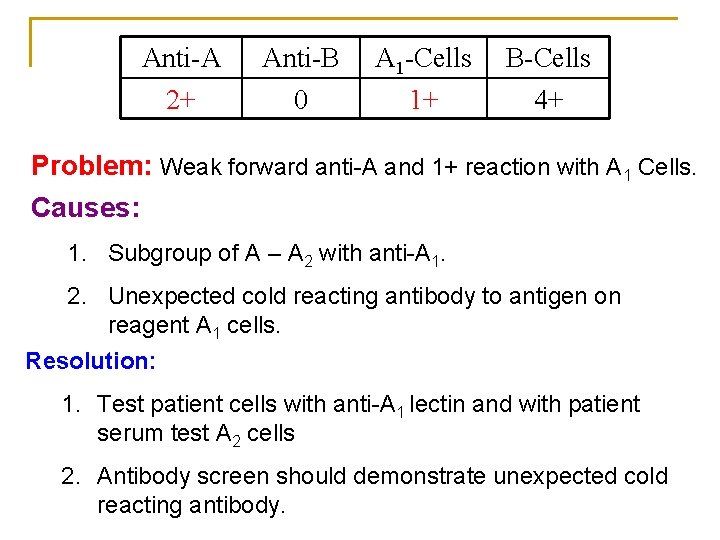
Anti-A 2+ Anti-B 0 A 1 -Cells 1+ B-Cells 4+ Problem: Weak forward anti-A and 1+ reaction with A 1 Cells. Causes: 1. Subgroup of A – A 2 with anti-A 1. 2. Unexpected cold reacting antibody to antigen on reagent A 1 cells. Resolution: 1. Test patient cells with anti-A 1 lectin and with patient serum test A 2 cells 2. Antibody screen should demonstrate unexpected cold reacting antibody.

Le ! r p t’s e c i act
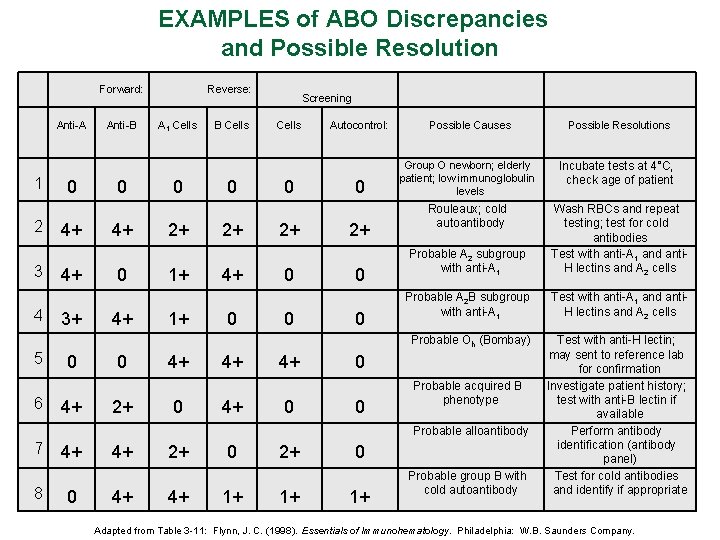
EXAMPLES of ABO Discrepancies and Possible Resolution Forward: Anti-A 1 2 3 4 5 6 0 4+ 4+ 3+ 0 4+ Anti-B 0 4+ 0 2+ Reverse: A 1 Cells 0 2+ 1+ 1+ 4+ 0 B Cells 0 2+ 4+ 0 4+ 4+ Screening Cells 0 2+ 0 0 4+ 0 Autocontrol: Possible Causes Possible Resolutions 0 Group O newborn; elderly patient; low immunoglobulin levels Incubate tests at 4°C, check age of patient 2+ 0 0 Rouleaux; cold autoantibody Probable A 2 subgroup with anti-A 1 Wash RBCs and repeat testing; test for cold antibodies Test with anti-A 1 and anti. H lectins and A 2 cells Probable A 2 B subgroup with anti-A 1 Test with anti-A 1 and anti. H lectins and A 2 cells Probable Oh (Bombay) Test with anti-H lectin; may sent to reference lab for confirmation Investigate patient history; test with anti-B lectin if available Perform antibody identification (antibody panel) Test for cold antibodies and identify if appropriate 0 0 Probable acquired B phenotype Probable alloantibody 7 8 4+ 0 4+ 4+ 2+ 4+ 0 1+ 2+ 1+ 0 1+ Probable group B with cold autoantibody Adapted from Table 3 -11: Flynn, J. C. (1998). Essentials of Immunohematology. Philadelphia: W. B. Saunders Company.
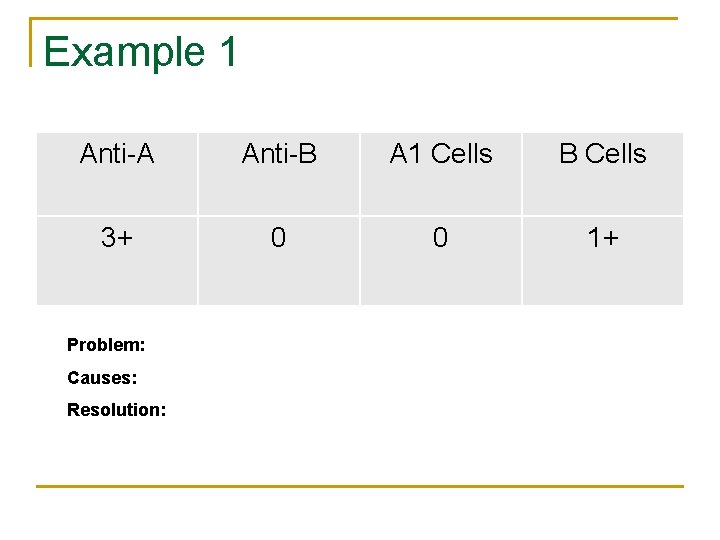

Example 1 Anti-A Anti-B A 1 Cells B Cells 3+ 0 0 1+ Problem: Causes: Resolution:
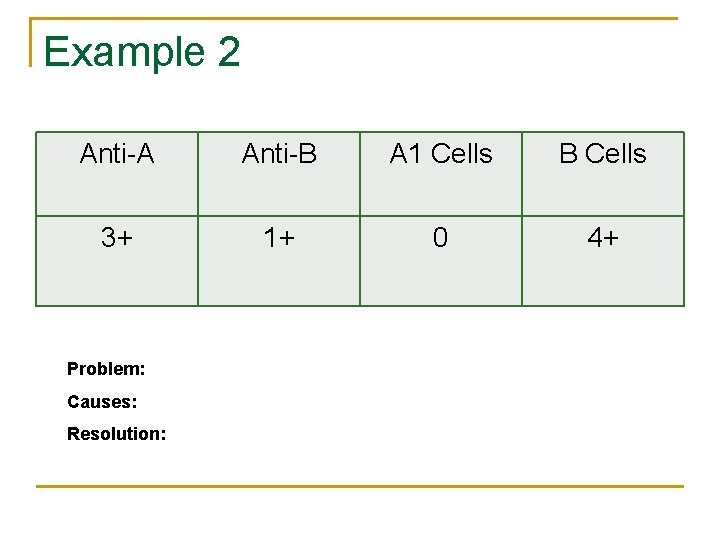

Example 2 Anti-A Anti-B A 1 Cells B Cells 3+ 1+ 0 4+ Problem: Causes: Resolution:
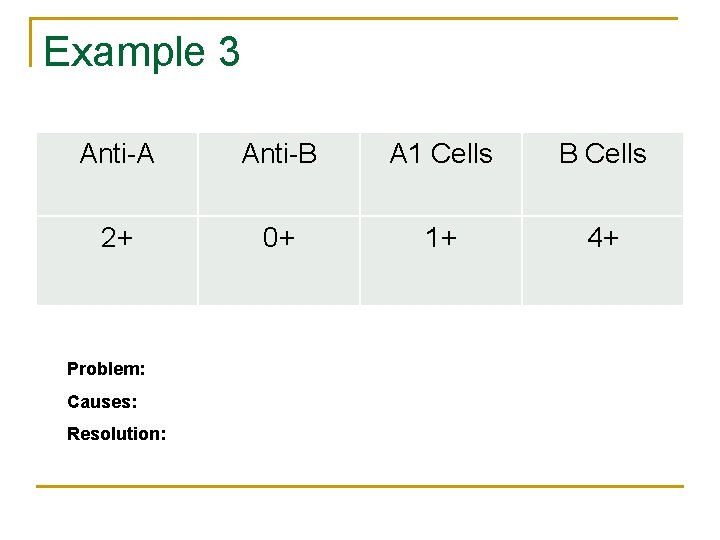

Example 3 Anti-A Anti-B A 1 Cells B Cells 2+ 0+ 1+ 4+ Problem: Causes: Resolution:
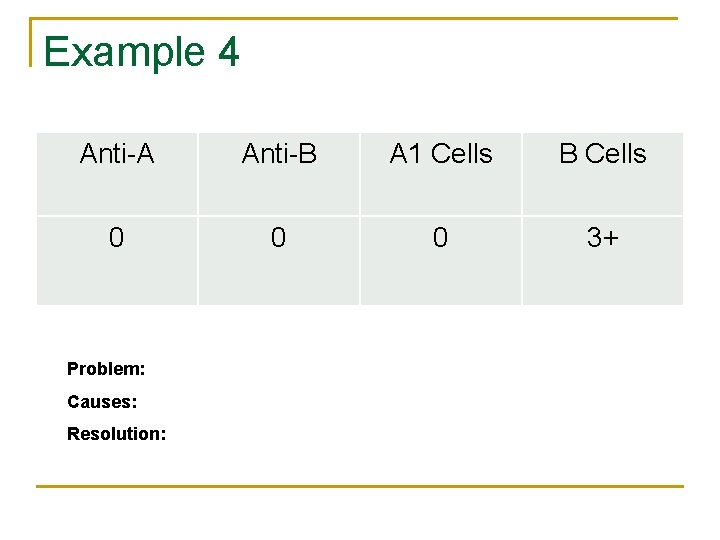

Example 4 Anti-A Anti-B A 1 Cells B Cells 0 0 0 3+ Problem: Causes: Resolution:
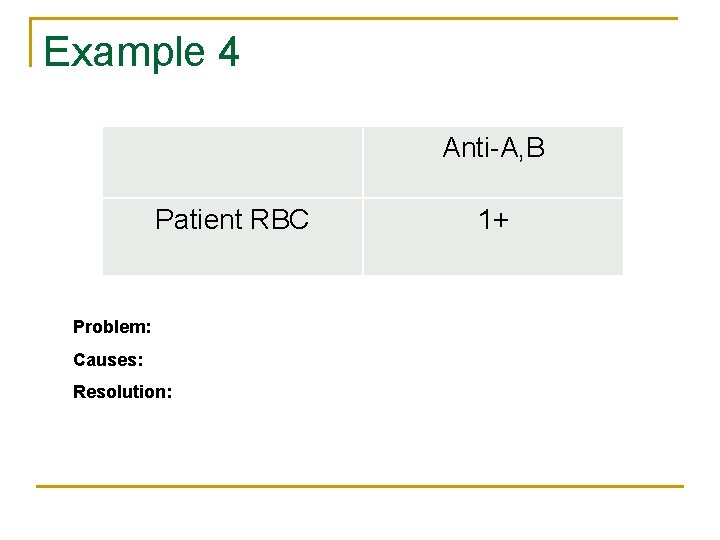

Example 4 Anti-A, B Patient RBC Problem: Causes: Resolution: 1+
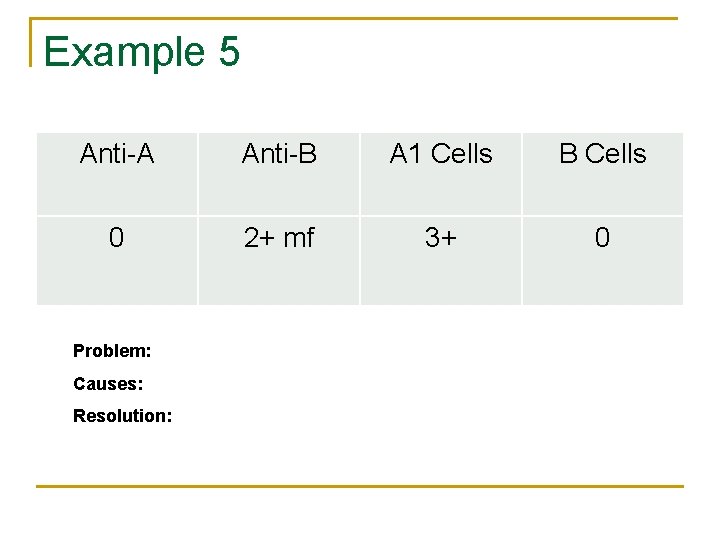

Example 5 Anti-A Anti-B A 1 Cells B Cells 0 2+ mf 3+ 0 Problem: Causes: Resolution:
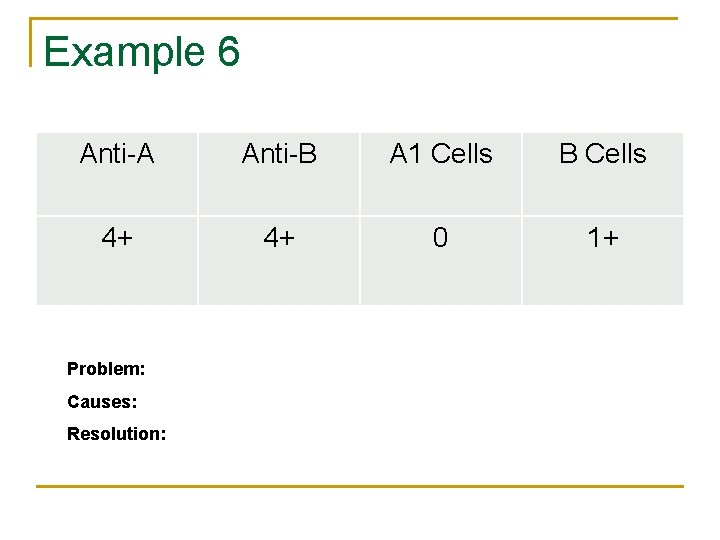

Example 6 Anti-A Anti-B A 1 Cells B Cells 4+ 4+ 0 1+ Problem: Causes: Resolution:
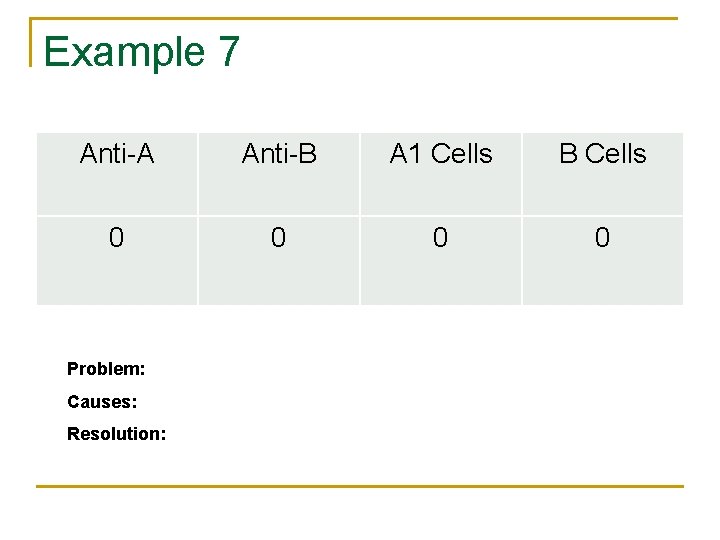
Example 7 Anti-A Anti-B A 1 Cells B Cells 0 0 Problem: Causes: Resolution:
- Slides: 37